Abstract
Background
Schisandra chinensis is widely applied in the prevention and treatment of asthma in China, but the material basis for the anti-asthmatic effect of S. chinensis is unclear. Our previous studies found that the lignans from S. chinensis can relax tracheal smooth muscle in rats. Schisandrol A (SCA) is a representative monomer of S. chinensis lignans with high content and activity.
Purpose
This study was aimed at further exploring the relaxation effect of SCA and its mechanism on the isolated tracheal smooth muscle of rats through tracheal perfusion experiments.
Materials and Methods
The isolated rat tracheal ring was precontracted with acetylcholine (ACh). Then, the impact of SCA on the tension of precontracted tracheal ring was studied. Verapamil (L-type calcium channel blocker) and four potassium channel blockers, including glibenclamide, tetraethylamine, 4-aminopyridine (4-AP), and barium chloride (BaCl2), as well as propranolol (β-adrenergic receptor antagonist), were respectively used to precontract the tracheal ring for investigation.
Results
SCA could dose-dependently reduce the ACh-induced contraction of the tracheal ring, and the verapamil and 4-AP could weaken this effect, while BaCl2, glibenclamide, tetraethylamine, and propranolol did not show this effect.
Conclusion
SCA can significantly relax the effect of tracheal smooth muscle of rats, and the underlying mechanism might be involved in the blocking of L-type Ca2+ channels and activating the voltage-dependent potassium channels (KV).
Keywords
Introduction
Asthma is a chronic disease that seriously endangers human health. Due to the unclear pathogenesis and the lack of curable drugs, it has always been an urgent problem faced by the global medical community (Chakaya & Ait-Khaled, 2022; Dharmage et al., 2019). The main pathological features of asthma are bronchiectasis, tracheal hyperresponsiveness, and chronic nonspecific inflammation. Tracheal hyperresponsiveness refers to the too-early or excessive contraction response of trachea to the various stimuli such as allergens, physical and chemical factors, and drugs (Chapman & Irvin, 2015). Nowadays, for the clinical treatment of asthma, anti-inflammatory anti-asthmatic drugs, adrenal glucocorticoid, and bronchodilator β2 adrenergic receptor agonists, as well as theophylline, are mainly used. Although they can alleviate asthmatic symptoms, their long-term use can result in serious adverse reactions (Alsaeedi et al., 2002; Cazzola et al., 2013; Tao-Tao & Yan-Lin, 2014). Therefore, safer and more effective asthma medicines are needed. Encouragingly, Traditional Chinese Medicine (TCM), with the advantages of high safety, multitarget, and remarkable therapeutic effect, is expected to be an alternative or adjuvant drug for asthma treatment (Bo-Wen et al., 2022).
Schisandra chinensis was first recorded in “Shennong Herbal Classic” as the top herb, with an acidic taste and convergence of lung and kidney. Zhang Zhongjing, in the Han Dynasty, “Synopsis of Golden Chamber,” recorded that S. chinensis can restrain lung qi and cough, and it was used as the main medicine to treat cold cough and asthma. In the Song Dynasty, “Taiping Huimin Pharmaceutical Bureau” recorded that S. chinensis can control lung qi and asthma cough. By using data mining techniques, Wang Jiaran sorted out prescriptions in the “Chinese Prescription Database” and screened out 631 prescriptions with S. chinensis, most of which were used for lung-related diseases, accounting for 55.9% (Jiaran et al., 2019). S. chinensis is among the top 10 TCMs used in the treatment of asthma, so it is the vital medicine that ancient and modern doctors choose to cure asthma (Yu-Zhen et al., 2017).
However, the material basis for the anti-asthmatic effect of S. chinensis is unclear. Schisandrol A (SCA), with a higher content and activity in the active component lignans of S. chinensis, is listed as a component used to identify S. chinensis in Chinese Pharmacopoeia (Figure 1). In TCM for asthma, Bufei Pill, Zhike Pingchuan Mixture, and Yinhuang Qingfei Decoction, SCA is the symbolic component for quality standards. Modern pharmacological research has revealed that SCA has actions of anti-inflammation, antioxidation, and relaxation of smooth muscle (Li et al., 2022; Lun et al., 2017; Qiu et al., 2023). Our preliminary experiments have shown that among the six Schisandra lignans, SCA was the most effective in relaxing the smooth muscle of isolated rat trachea. It is speculated that SCA may be the essential ingredient of S. chinensis to play the anti-asthmatic role. Accordingly, in the present study, an isolated tracheal perfusion experiment was employed for further proving the relaxation of SCA on rat-isolated tracheal rings, and the underlying mechanism was explored by using drugs that could affect calcium and potassium channels. All this work was expected to lay a foundation for the research and development, as well as the clinical use, of SCA as an ingredient for anti-asthmatic drugs.
(A) Fresh Schisandra chinensis (Turcz.) Baill. Fruit. (B) Dried Fruits of Schisandra chinensis. (C) The Chemical Structure of Schisandrol A.

Materials and Methods
Chemicals and Reagents
SCA, with a purity of ≥98% and prepared with dimethyl sulfoxide (DMSO), was obtained from Chengdu Pfizer Technology Co. Ltd, Chengdu, China. Verapamil (Ver), propranolol (Pro), glibenclamide (Gli), tetraethylamine (TEA), and 4-aminopyridine (4-AP) were obtained from Sigma Aldrich, St. Louis, MO, USA. Acetylcholine (ACh) and barium chloride (BaCl2) were obtained from Sinopharm Group Chemical Reagent Co., Ltd., Shanghai, China.
Animals
Male Wistar rats [250–300 g, license No.: SCXK (Ji)-2018-0007, Changchun Yisi Experimental Animal Technology Co. Ltd., Changchun, China] were used. The rats were raised in separate cages, and they freely consumed water and food.
Isolated Rat Tracheal Ring Preparation
The method used in our previous study was employed to prepare the isolated tracheal ring (Lin et al., 2021). Rats were anesthetized in intraperitoneal injection of urethane (4 mg/kg), and then all tracheae from the lower thyroid cartilage to the bifurcated part of the lower trachea were removed and put into a nutrient solution at 4℃. The trachea was prepared into a 2–4 mm tracheal ring after removing the surrounding tissues on the surface of the trachea. The tracheal ring was fixed through its lower end, and the tension sensor was connected to its upper end. The resting tension was 1.0 g. The tracheal ring was incubated in 10 mL of the nutrient solution at 37℃ for 60 min, and the nutrient solution was replaced by the fresh one every 15 min. The incubator was continuously added with a mixed gas (95% O2 and 5% CO2) (Kajioka et al., 2012). A BL-420F Biolab System (Chengdu Taimeng Biotechnology Co. Ltd., China) was used to record the rat tracheal ring tension signals. The subsequent experiments were not carried out until the tracheal ring tension was stable.
Observation on Isolated Rat Tracheal Ring Resting Tension
To detect the influence of SCA on tracheal ring tension in a resting state, the final concentrations of 10–5–10–3 M of SCA were added cumulatively when the tracheal ring tension was stable, and an equal volume of DMSO (10 µL) was added every time in the control group. Changes in the tension were recorded, and the inhibition rate (% of tension changes) was calculated according to the following formula: (tension after adding SCA – resting tension)/resting tension × 100% (Shu-Zhi et al., 2012).
Study on the Effect of SCA on the Isolated Tracheal Ring Precontracted by ACh
To examine the relaxing action of SCA on the isolated tracheal ring, the ring’s precontraction was induced by adding ACh (10–3 M). When the tracheal ring tension was stable, SCA at cumulative concentrations (10–5–10–3 M) was added into the bath continuously, and changes in the tension were observed and recorded. Vehicle (DMSO) at the corresponding concentrations was applied in normal control group. Then, the relaxation rate (% of the change in the tension) following by adding SCA was determined according to the formula: (ACh-induced maximal tension – SCA-induced minimal tension)/(ACh-induced maximal tension – resting tension) × 100%.
Investigating the Role of Verapamil in SCA-induced the Relaxation of the Tracheal Ring
For investigating whether the relaxing action induced by SCA on airway smooth muscle is mediated by L-type Ca2+ channels, verapamil (10–5 M), an L-type Ca2+ channel blocker, was used for the preincubation of tracheal ring for 15 min, and an equal volume of distilled water was used in the control group, then ACh was used, and finally, SCA (10–5–10–3 M) was accumulatively added into the bath.
Intracellular calcium release is required during the constriction of tracheal smooth muscle. For examining the effect of SCA on this intracellular release, the sample was placed in a Ca2+-free nutrient solution [0.5 mM ethylene glycol-bis(2-aminoethyl ether)-N,N,N′,N′-tetraacetic acid] for 30 min for the equilibrium of solution, then verapamil (10–5 M) was added into the bath for preincubating for 15 min, and SCA (10–3 M) was added into it (DMSO was added in the control group) for another 15 min. The bath solution was added with ACh (10–3 M) to induce the ring contraction when the tension was stable, and then the concentration of Ca2+ was recovered at 2 mM. The experimental results were observed, recorded, and calculated according to the method described above (Müller-Schweinitzer & Fozard, 2010).
Investigating the Impact of Potassium Channel Inhibitors on the Ring Relaxation Produced by SCA
It is believed that calcium channels and potassium channels are both involved in the regulation of smooth muscle relaxation and constriction. In order to explore the role of potassium channels in the airway smooth muscle relaxation produced by SCA, potassium channel inhibitors, including KATP inhibitor Gli (10–5 M), BKCa inhibitor TEA (10–2 M), Kv inhibitor 4-AP (10–5 M), and KIR inhibitor BaCl2 (10–3 M), were employed to preincubate the rat tracheal ring for 15 min, respectively; then, it was precontracted with ACh, and finally, SCA (10–5–10–3 M) was accumulatively added into the bath. The experimental results were observed, recorded, and calculated according to the method described above.
Investigating the Role of β-Adrenoceptor Antagonists in SCA-induced the Relaxation of Tracheal Ring
To examine whether β receptors participate in SCA-induced relaxation of tracheal smooth muscle, propranolol (10–5 M) was used to preincubate the tracheal ring for 15 min, followed by ACh and SCA. The tension changes were observed, recorded, and calculated.
Statistical Analysis
All experimental data were presented as mean ± standard deviation (SD), and “n” denoted the sample number in each group. The data were analyzed with SPSS software (Windows 20.0 version). Student’s t-test was used for the comparison of the statistical significance between the two groups, and p < 0.05 indicated a significant difference.
Results
Effects of SCA on the Tracheal Ring Precontracted by ACh
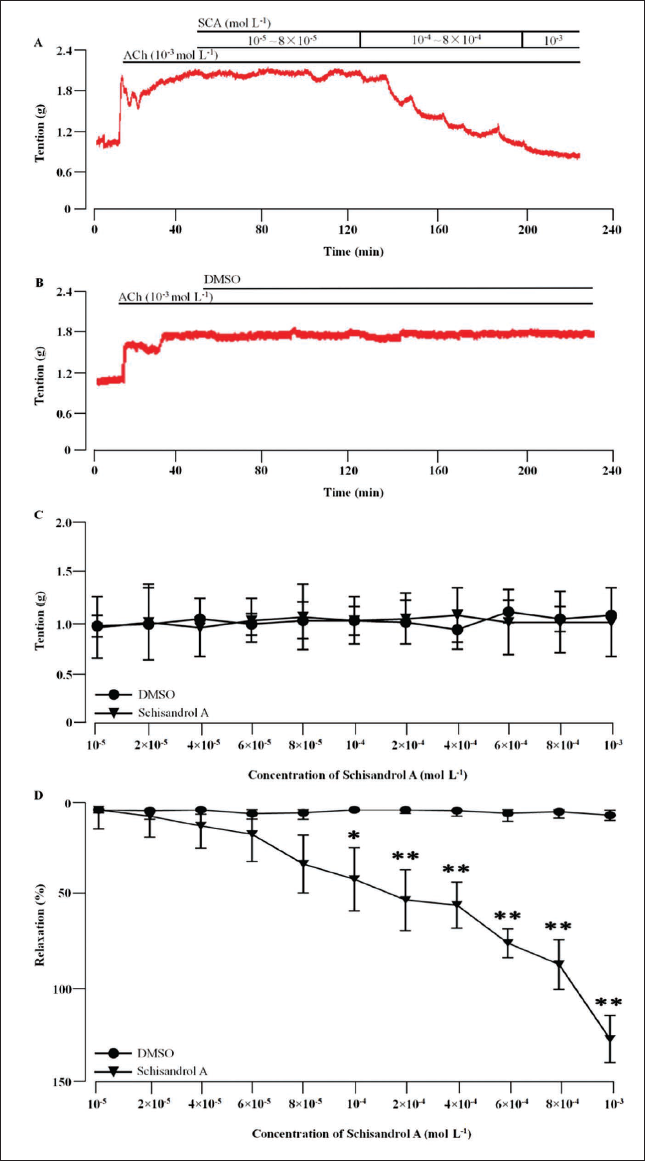
Tracheal rings from normal rats were used for observing the roles of SCA in relaxation of airway smooth muscle. The results (Figure 2) showed that SCA at 10–5–10–3 M final concentration could not significantly affect the tracheal ring tension under the condition without the precontraction with ACh (Figure 2C), but it had a significant inhibition on the tension with ACh precontraction (Figure 2A), and the maximum relaxation rate was 120.86 ± 13.85% (Figure 2D). This suggests that airway smooth muscle relaxation can be induced by SCA at its contraction state but not at its resting state.
Effect of SCA on ACh-induced Influx of Extracellular Ca2+
ACh constricts tracheal smooth muscle through opening L-type Ca2+ channels and promoting extracellular Ca2+ influx (Wei et al., 2015). To study whether Ca2+ influx is involved in the relaxation effect of SCA, we preincubated the sample with L-type Ca2+ channel blocker verapamil (10–5 M) for 15 min. The results showed that the relaxation effect induced SCA was significantly decreased, with the maximum relaxation rate decreased to 91.8 ± 22.42% in comparison to 119.75 ± 10.35% in the control group (Figure 3, p < 0.01). This suggests that the relaxation effect of SCA may be partly caused by blocking L-type Ca2+ channels and preventing extracellular Ca2+ influx.
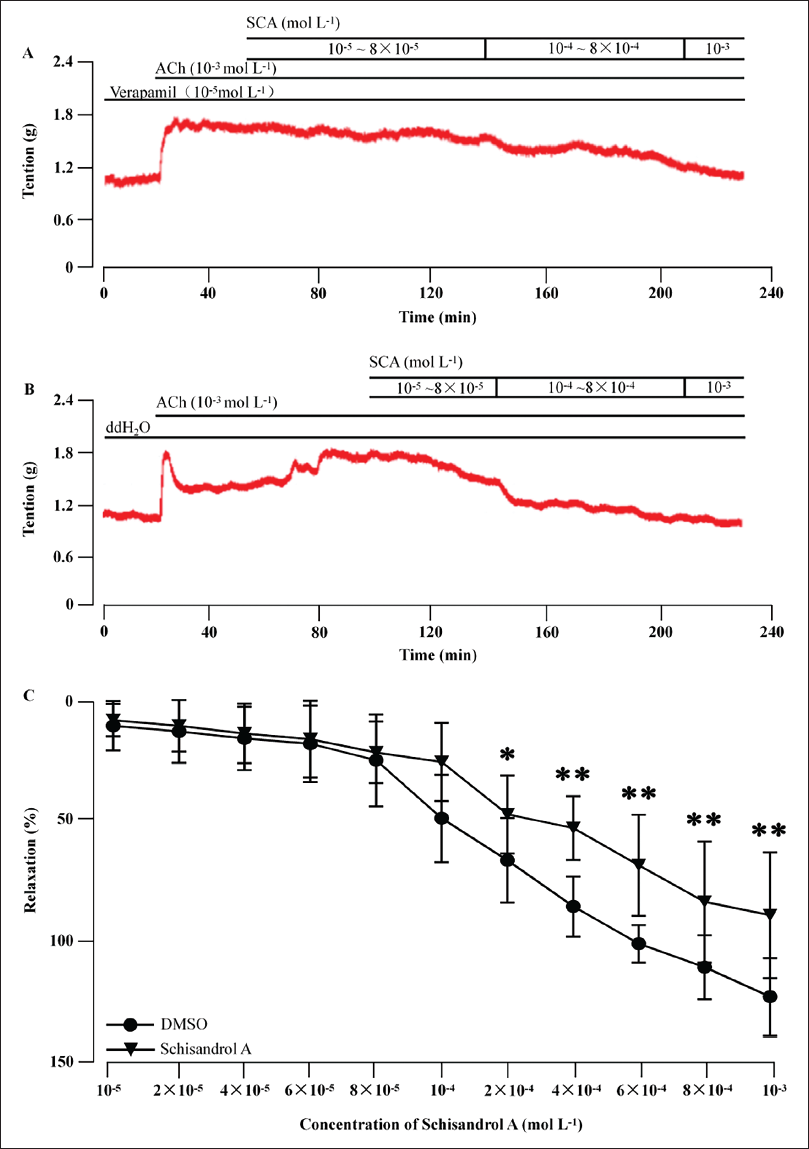
The contraction of tracheal smooth muscle can be caused by ACh through its opening of L-type Ca2+ channels and promoting extracellular Ca2+ influx (Wei et al., 2015). In order to confirm if the relaxation induced by SCA could be related to Ca2+ influx, the tracheal ring was preincubated with verapamil (10–5 M), an L-type Ca2+ channel blocker, for 15 min. It was found that the relaxation effect of SCA was significantly reduced with the decrease in the maximum relaxation rate to 91.8 ± 22.42% in comparison to 119.75 ± 10.35% in the control group (Figure 3, p < 0. 01), indicating that the effect of SCA may be partly related to its blocking of L-type Ca2+ channels and preventing extracellular Ca2+ influx.
Effect of SCA on ACh-induced Release of Intracellular Ca2+ in Tracheal Smooth Muscle
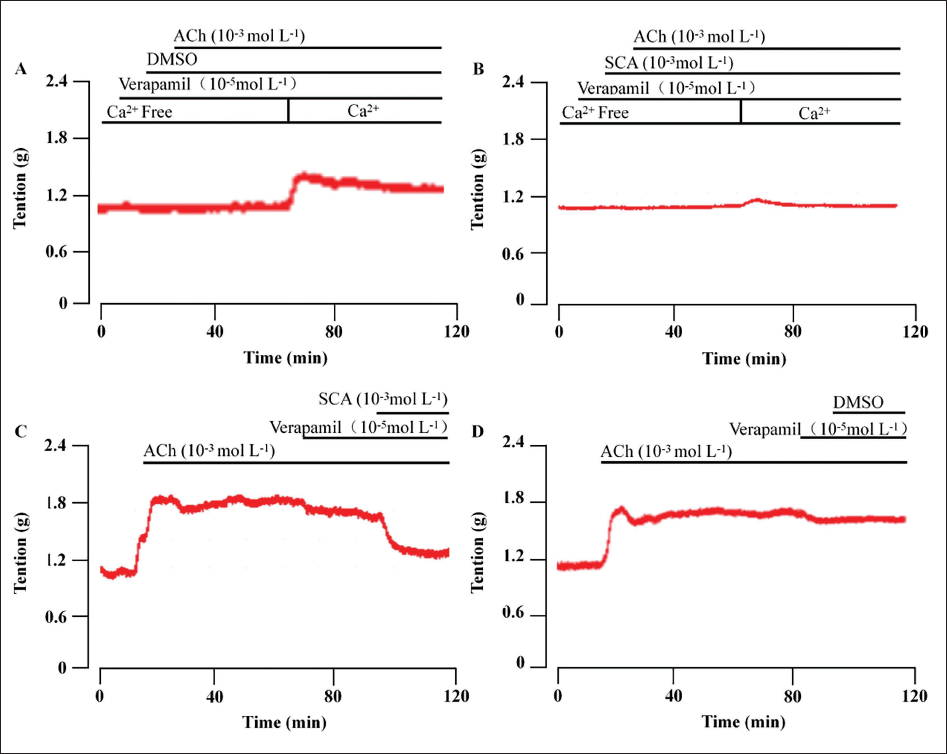
Besides Ca2+ influx, intracellular Ca2+ release is required during the airway constriction. The results (Figures 4A and B) showed that with Ca2+-free perfusion, ACh did not cause tracheal ring contraction but caused significant contraction after restoring the Ca2+ perfusion in the control group. However, SCA, just before ACh, prevented its contraction. In addition, we also tested the relaxation effect of SCA (10–3 M) after ACh precontraction and verapamil (10–5 M) relaxation. As shown in Figure 4C, verapamil reached a relaxation rate of 18.74 ± 5.63%, whereas SCA got a further relaxation rate of 66.93 ± 9.48%. Therefore, it is reasonable to speculate that SCA may inhibit the Ca2+ release from the intracellular sarcoplasmic reticulum and/or the extracellular calcium influx via calcium channels and other L-type Ca2+ channels on cell membrane.
Effect of Potassium Channel Blockers on the Relaxation of the Rat Tracheal Smooth Muscle by SCA
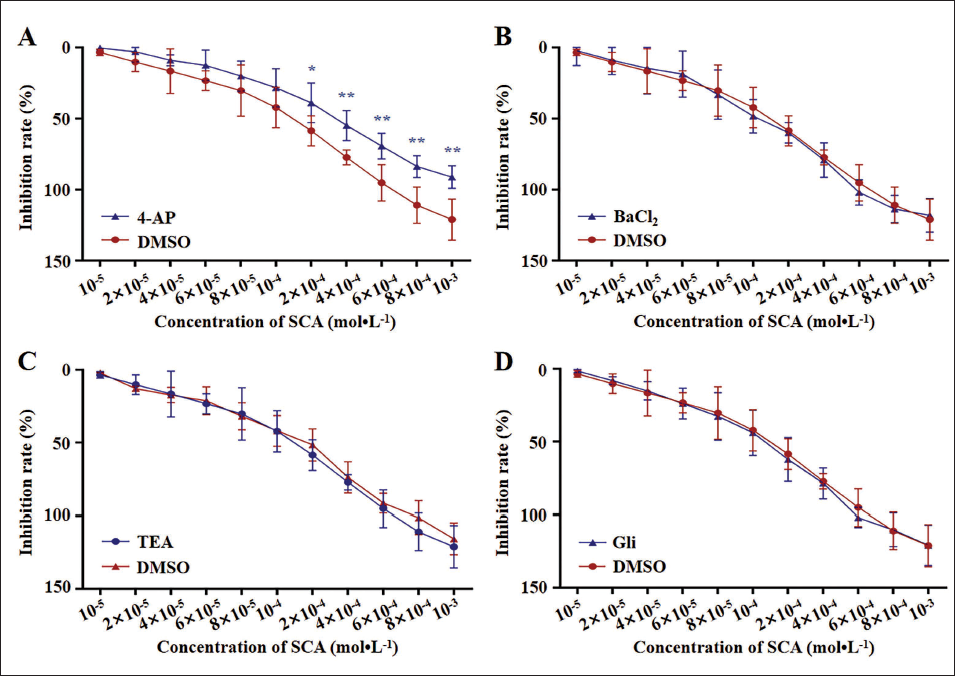
Four kinds of K+ channel inhibitors, KATP inhibitor Gli (10–5 M), BKCa inhibitor TEA (10–2 M), Kv inhibitor 4-AP (10–5 M), and KIR inhibitor BaCl2 (10–3 M), were applied to observe if K+ channels participate in the tracheal dilation induced by SCA. The results showed that the inhibition of SCA on the precontraction of ACh was weakened by the preincubated 4-AP, with a maximum relaxation rate down to 91.75 ± 17.92% (p < 0. 01), but not significantly affected by Gli, TEA, and BaCl2 (Figure 5). These results indicate that the activation of the Kv channel might be involved in the relaxation of airway smooth muscle by SCA.
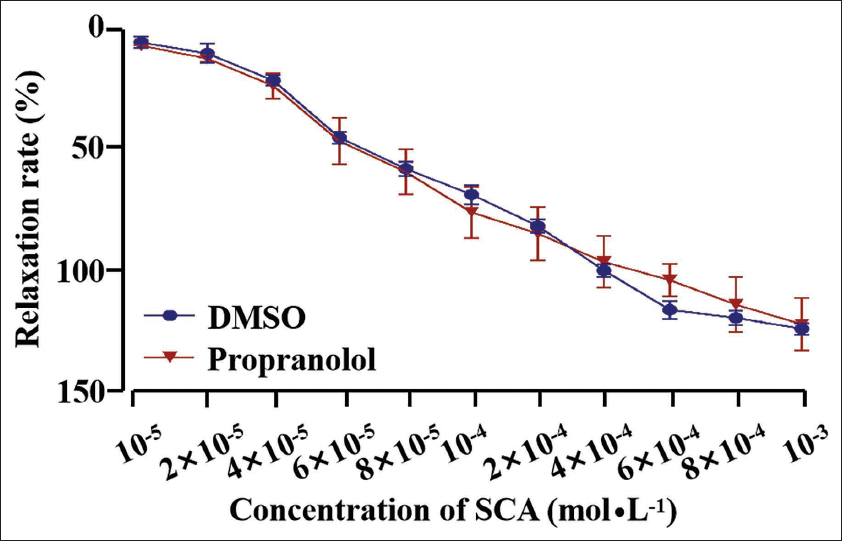
Effect of β-Adrenoceptor Antagonist on the Rat Trachea Smooth Muscle Relaxation Produced by SCA
Beta-receptor is also involved in the bronchial smooth muscle dilation, and its agonists are commonly used as bronchodilators (Deshpande et al., 2008). After preincubation with propranolol (10–5 M) for 15 min, SCA still had a significant dose-dependent relaxation of the sample, but without significant difference in comparison to it in normal control group where the sample was not preincubated with propranolol (Figure 6), suggesting that SCA-induced trachea smooth muscle relaxation may be not β receptor-dependent.
Discussion
S. chinensis is an important drug in the treatment of cough and asthma in both traditional and modern medicine. It is often used to treat respiratory diseases, but its effective components are not clear. Some advanced separation and analysis methods have been used for separating and identifying bioactive components from natural world, and lignans have been considered representative bioactive components in S. chinensis, containing a higher content of SCA, schisandrin A, schisandrin B, schisandrin C, schisandrol B, schisantherin A, etc. (Chen et al., 2001; Zhang et al., 2009). Our previous research suggested that total lignans and several monomers from S. chinensis could induce the rat trachea relaxation, of which, SCA (119.12 ± 15.35%) and schisandrol B (78.23 ± 10.20%) had a stronger effect, followed by schisandrin A (62.95 ± 12.93%) and schisandrin B (46.58 ± 4.92%), while schisantherin A and schisandrin C did not produce such an effect (Chen et al., 2021; Lin et al., 2021). In this study, by tracheal perfusion experiment, we further confirmed that SCA could relax isolated rat tracheal smooth muscle precontracted by ACh in vitro. Furthermore, the SCA-induced trachea smooth muscle relaxation was inhibited by verapamil, an L-type Ca2+ channel blocker, and 4-AP, a voltage-dependent potassium channel inhibitor.
Tracheal smooth muscle spasm is a main factor in inducing asthma, which is mainly manifested in the excessive contraction of the trachea when stimulated. The factors affecting smooth muscle relaxation and contraction of the trachea include nerve reflex, signal transmission pathway, receptor status on the smooth muscle of the trachea, and open status of the ion channel. The muscarinic receptor family is widely expressed in tracheal smooth muscle, which contains M1–M5 subtypes of the muscarinic receptor family (Yu-Zhen et al., 2017). Among them, G protein-coupled M3 receptors were believed to be involved in constriction of airway smooth muscle (Kovacevic et al., 2015). ACh was used to preincubate the tracheal ring, and it bonded to and activated the M3 receptors in the smooth muscle, causing the influx of calcium ions and ultimately inducing the trachea smooth muscle contraction. SCA significantly inhibited this effect of ACh and induced tracheal ring relaxation.
It is well known that cell membrane potential affects the calcium sensitivity of contractile proteins and regulates intracellular Ca2+ concentration. L-type Ca2+ channels on cells of tracheal smooth muscle are the most pharmacologically significant calcium channels, and their activation of them is the main way for calcium to enter the cell when the cell is excited (Chen et al., 2019). The present study demonstrated that the trachea smooth muscle relaxation effect of SCA could be attenuated by the preincubation with verapamil, suggesting that SCA may inhibit the tracheal smooth muscle contraction by inhibiting the extracellular Ca2+ influx through the transmembrane L-type Ca2+ channel. Intracellular Ca2+ release is mainly regulated by inositol triphosphate and calcium. To test whether SCA affects intracellular Ca2+ release, we preincubated the tracheal ring with verapamil to block calcium ion channels and inhibit extracellular Ca2+ influx to activate intracellular sarcoplasmic reticulum Ca2+ release, and then added SCA and ACh. It was observed that under either Ca2+ or Ca2+-free conditions, ACh did not cause a significant contraction of the ring. In addition, after verapamil partially inhibited ACh-induced tracheal ring contraction, SCA could produce further relaxation. Therefore, we speculated that SCA may inhibit the release of intracellular Ca2+. This result is similar to that in the study on S. chinensis lignans, in which the lignans could relax tracheal smooth muscle by inhibiting the release of intracellular Ca2+ (Lin et al., 2021).
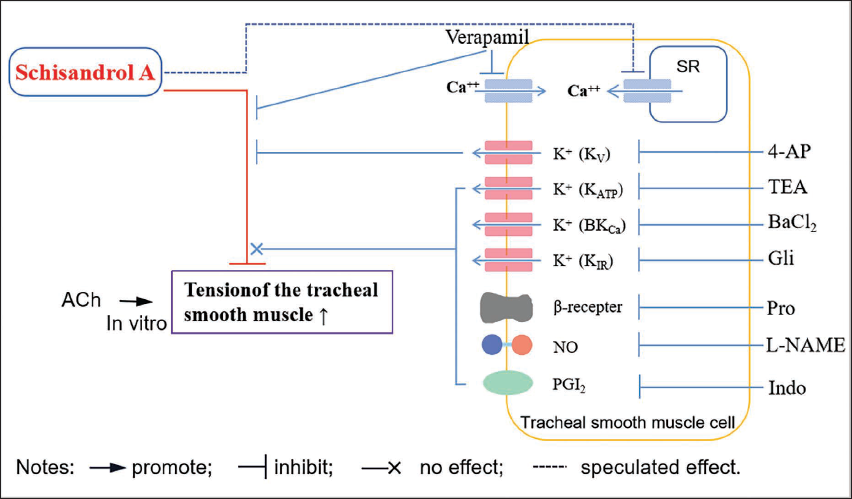
Potassium channels are also important for the relaxation and contraction of smooth muscles. At least four potassium channels have been found in trachea smooth muscle: KCa (Ca2+-activated K+ channel), KATP (ATP-sensitive K+ channel), BKCa (large conductance Ca2+-activated K+ channel), Kv (voltage-dependent K+ channel), and KIR (inward rectifier K+ channel) (Emami et al., 2020; Kakad et al., 2012). In this experiment, Kv inhibitor 4-AP significantly reduced the relaxation effect of SCA, while TEA, Gli, and BaCl2 did not, verifying that the Kv channel activation may participate in the relaxation produced by SCA. Besides ion channels, β2 receptor activation is also a main pathway to mediate the trachea smooth muscle relaxation. However, propranolol, a β-adrenergic receptor blocker, could not significantly affect the relaxation of SCA, suggesting that β-adrenergic receptors may not be involved in it (Figure 7).
Conclusion
SCA can significantly relax ACh-precontracted isolated rat trachea smooth muscle, which may be related to its regulation of intracellular Ca2+ concentration and KV channel, confirming that SCA should be an effective component in S. chinensis for relieving asthma. SCA is one of the highest content lignan monomers in S. chinensis, with great development value. However, we have noticed that the dose of SCA in relaxing isolated tracheal smooth muscle is relatively high in the present experimental system. In vivo effects of SCA on airway tension in rats or mice need to be further evaluated, and the structure–effect relationship regarding SCA and other monomers in S. chinensis, as well as pathways related to their calcium and potassium channel blocking, remain to be verified. An ideal asthma animal model needs to be established to explore the antiasthma effect and its mechanism of SCA.
Abbreviations
ACh: Acetylcholine; 4-AP: 4-Aminopyridine; BaCl2: Barium chloride; DMSO: Dimethyl sulfoxide; Gli: Glibenclamide; KV: Voltage-dependent potassium channels; TCM: Traditional Chinese medicine; TEA: Tetraethylamine; SCA: Schisandrol A; S. chinensis: Schisandra chinensis.
Footnotes
Acknowledgments
We appreciate all coworkers who participated in this study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
All animal experiment procedures were in line with the national regulations regarding the use and welfare of laboratory animals, and were approved by the Animal Ethics Committee of Beihua University (Jilin, China).
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article. The present study was supported by the Health Technology Innovation Project of Jinlin Province (No. 2023JC034) and the Jilin Province Industrial Innovation Special Fund Project (No. 2023C037-9).
