Abstract
Background
After hypovolemic shock caused by severe burns, lipid peroxidation is an important factor in tissue edema and multiorgan dysfunction syndrome (MODS). Many studies have shown that valproic acid (VPA) inhibits lipid peroxidation and reduces tissue and organ injury.
Objectives
This study investigated whether the VPA treatment of scalded rats reduced tissue edema by inhibiting lipid peroxidation, thereby improving organ function and survival rate.
Materials and Methods
A total of 60 male Sprague-Dawley rats (weighing: 280–300 g) with a 50% total body surface area (TBSA) full-thickness dermal burn were randomly assigned to the following 3 groups (with 20 rats per group): (I) the no infusion resuscitation (NR) group; (II) the sodium lactate Ringer’s solution (LR) group; and (III) the sodium valproate Ringer’s solution (VR) group. After scalding, the following hemodynamic parameters were measured: Copper2+-Zinc2+-superoxide dismutase (Cu2+-Zn2+-SOD) activity, thiobarbituric acid reactive substances (TBARSs), oxidized glutathione (GSSG), reduced glutathione (GSH), and antioxidant enzyme activities. Organ function parameters and water content were also measured. Another 60 male Sprague-Dawley rats were used to observe the 24-h survival rate of the rats using the same scald model and fluid resuscitation.
Results
VPA significantly increased the mean arterial pressure (MAP) and cardiac output (CO), and significantly decreased the pulmonary vascular permeability index (PVPI) and extravascular lung water index (ELWI). VPA also increased plasma Cu2+-Zn2+-SOD activity and decreased the plasma TBARS level. VPA reduced the TBARS level and GSSG in various tissues and increased the concentration of GSH. VPA decreased glutathione peroxidase (GPx) and catalase (CAT) activity, but significantly increased glutathione reductase (GR) activity in various tissues. VPA significantly improved organ functions and decreased water content. VPA significantly improved the survival rate, and the 24-h survival rate of the VR group was double that of the LR group.
Conclusion
Resuscitation with VPA reduced tissue edema, protected visceral functions, and improved the survival rate of rats with severe burn shock (BS) by alleviating lipid peroxidation.
Introduction
Burn shock (BS) is a severe injury that induces considerable morbidity and mortality (Liu et al., 2016a, 2018, 2022). The current treatment for BS includes timely fluid resuscitation to replenish the circulating blood volume, restore tissue perfusion, and improve cell metabolism. Traditional crystal solutions include normal saline (0.9% sodium chloride, NaCl; NS) and sodium lactate Ringer’s solution (LR). NS and LR are still the basic solutions used in fluid resuscitation, but there are serious shortcomings in their application. NS is often complicated by hyperchloric acidosis, and LR can induce cell pseudohypoxia and aggravate intracellular acidosis, and neither contains energy substrates as previously described (S. Liu et al., 2019; Young et al., 2014). Previous studies have shown that LR aggravates tissue edema and multiorgan dysfunction syndrome (MODS) through lactic acidosis, inflammation, and peroxidation (Matsuo et al., 2021; Wagner et al., 2018). Currently, sodium acetate Ringer’s solution is one of the alternatives for crystal fluid resuscitation. It avoids the above shortcomings as described by Matsuo et al. (2021). However, as Keitel et al. (2015) reported, it cannot protect organ function and correct lactic acidosis. Thus, it is necessary to develop a novel resuscitation fluid to replace NS and LR for use in critical care. Patients with critical polytrauma, in addition to primary and secondary trauma, exhibit a range of molecular catastrophes. Dysfunctional biochemical pathways and molecular damage exacerbate the deterioration of the clinical state of these patients, one of the best-known molecular phenomena being oxidative stress (OS), leading to an escalating inflammatory state, multiple infections, and MODS (Horhat et al., 2016).
Previous studies have shown that valproic acid (VPA) exerts a protective effect in multiple organs (Gąssowska-Dobrowolska et al., 2021; Soria-Castro et al., 2019, 2020). It has been shown to improve organ function, lactic acidosis, and the survival rate of rats with hemorrhagic shock in various models (T. Liu et al., 2019; Tang et al., 2018; Tian et al., 2019). Additionally, previous research suggested that intraperitoneal injections of VPA significantly increase the blood flow of intra-abdominal organs, reduce the water content in organs, decrease ischemia-reperfusion injury, protect abdominal organ function, and reduce the risk of MODS as described by Williams et al. (2019). Some clinical trials have shown that VPA exerts a protective effect on multiple organ function (Felice et al., 2021; Kühne et al., 2021). Superoxide dismutase (SOD) activity was positively correlated with the duration of VPA treatment. In conclusion, patients with primary idiopathic epilepsy have an impaired oxidant-antioxidant status and the scavenger system is activated to reduce lipid peroxidation. VPA, often used in childhood epilepsy, may alter the balance between the oxidant and antioxidant systems (Yiş et al., 2009). VPA is a histone deacetylase inhibitor. It can improve the survival rate of animals with lethal hemorrhagic shock, septic shock, and BS, and reduce heart, brain, lung, liver, kidney, and other organ dysfunction caused by ischemia and inflammation; however, the specific mechanism by which this occurs is not yet known.
In this study, we tested the hypothesis that LR with an intraperitoneal injection of VPA would reduce tissue edema. To do this, we inhibited lipid peroxidation in scalded rats and detected the tissue water content and organ injury. To detect the level of lipid peroxidation, we measured the concentration of thiobarbituric acid reactive substances (TBARSs) and the activities of antioxidant enzymes, including oxidized glutathione (GSSG), reduced glutathione (GSH), glutathione peroxidase (GPx), glutathione reductase (GR), and catalase (CAT), in plasma and tissues.
Materials and Methods
Animal Ethics
All animal experiments were approved by our hospital, in compliance with Chinese national guidelines for the care and use of animals.
Experimental Animals
A total of 120 male Sprague-Dawley rats (Specific pathogen Free, SPF grade; aged: 80–100 days; weighing: 280 ± 20 g) were reared in a constant temperature and humidity animal laboratory for 2 weeks to adapt to the environment. The rats were fasted for 12 h before the experiment with free access to drinking water. The rats were provided by Beijing Huafukang Biotechnology Co. Ltd. (License: SCXK (Beijing) 2019-0008).
Burn Procedures
The skin of the rats was prepared, and the rats were anesthetized with 50 mg/kg of sodium pentobarbital. The back and lower limbs of the rats were immersed for 15 s in boiling water, and the abdomen was immersed for 8 s to induce a 50% total body surface area (TBSA) full-thickness third-degree scalding injury as described previously (Young et al., 2014). Dry the surface of the scalded skin with gauze immediately after the burn and disinfect with iodophor cotton balls. A protocol was prepared before the study without registration.
Surgical Procedures
At the time points of 0, 4, 8, 12, and 16 h post-scalding, the following operations were performed to measure the hemodynamic parameters. The hemodynamic parameters were monitored by pulse index continuous cardiac output (CO) (PiCCO-PLUS; Pulsion, Germany). After anesthesia, each rat was fixed in the supine position on the operating table, the lower limb and neck skin were sterilized, the unilateral femoral vein was separated from the lower limb, the right carotid artery and jugular vein were exposed, and the rat was intubated with a PE-50 catheter. The femoral vein cannula was used for whole-body heparinization and fluid replacement. A temperature sensor was inserted into the jugular vein to the superior vena cava, and a pressure fiber sensor was inserted into the carotid artery to the aorta to measure hemodynamic parameters. The 2 sensors were led out through the subcutaneous channel and fixed at the skin exit.
Experimental Protocols
A total of 60 Sprague-Dawley rats (weighing: 280–300 g) were randomly assigned to the following three groups (with 20 rats per group): (I) the no infusion resuscitation (NR) group; (II) the sodium LR (LR; Kelun Pharmaceutical Co. Ltd., Guizhou, China) group, which was immediately given fluid resuscitation after scalding; and (III) the sodium VR group, which was given VPA (300 mg/kg in 0.25 mL NS) intraperitoneally immediately after scalding. Sodium valproate solution: Take 1000 mg of sodium valproate and dissolve it in 10 mL of saline at a concentration of 100 mg/mL, ready to use. Another 60 rats were used to measure the survival rate after BS, and the Kaplan-Meier curve was used for the survival analysis. Fluid resuscitation was calculated using the Parkland formula (4 mL/kg/1% TBSA), and the total fluid rehydration was calculated. Half of the total fluid replenishment was added in the first 8 h (every 30 min), and the other half in the next 16 h (every 1 h).
Measurements
Hemodynamic parameters, such as the mean arterial pressure (MAP), CO, pulmonary vascular permeability index (PVPI), and extravascular lung water index (ELWI), were detected by pulse index continuous CO (PICCO-PLUS). The plasma concentration of TBARSs was measured by spectrophotometry to assess the oxidation as described by Dos Santos Chemelo et al. (Dos Santos Chemelo et al., 2021). The activity of plasma Cu2+-Zn2+-SOD was determined to evaluate antioxidant capacity as described by Guijarro et al. (2017). At various time points in the experiment, tissue samples of the heart, lung, liver, kidney, and jejunum were removed; the concentration of TBARSs, GSSG, GSH, GPx, GR, and CAT in various tissues was detected as described by Hafez et al. (2021), and changes in water content in various tissues were measured as previously described (Nong et al., 2021; Zhao et al., 2021). Changes in plasma creatine kinase (CK-MB), arterial partial pressure of oxygen (PaO2), alanine aminotransferase (ALT), diamine oxidase (DAO), and creatinine (Cr) were measured to determine the level of organ function as described by Cheng et al. (2021).
Statistical Analysis
The data were analyzed using SPSS version 17.0. The continuous variables are presented as the mean ± standard deviation. The t-test was used for intragroup comparisons, the F test was used for between-group comparisons, and the Student-Newman-Keuls test was used for between-group pairwise comparisons. A p-value < 0.05 indicated a statistically significant difference. The Kaplan-Meier method was used to analyze the survival of the rats.
Results
VPA Improved the Hemodynamic Parameters in BS
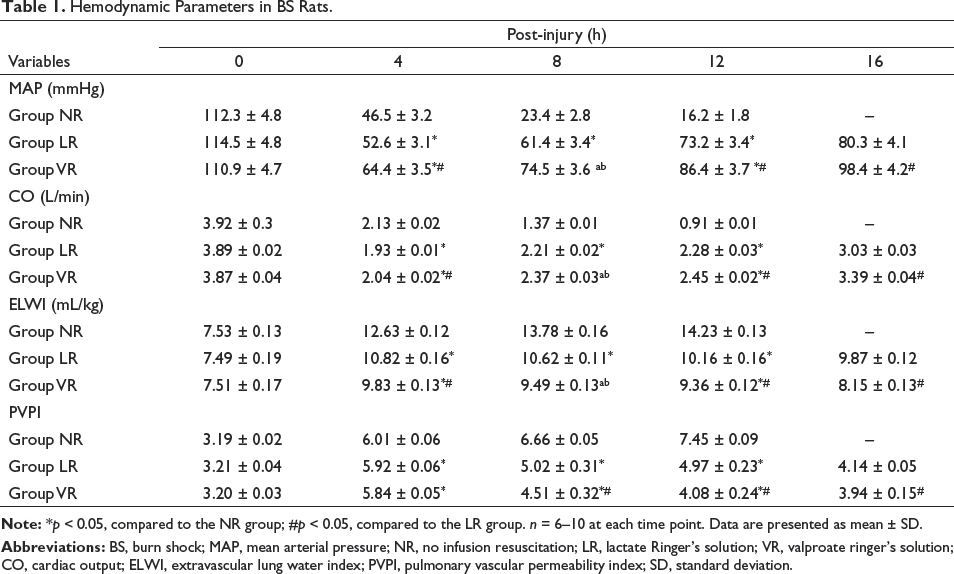
In the LR and VR groups, MAP and CO at 4 h post-BS decreased significantly, and then slowly increased. In the NR group, MAP and CO continued to decrease over time. At 4 h post-BS, the parameters of MAP and CO in the LR and VR groups gradually increased compared to those in the NR group (p < 0.05). However, the PVPI and ELWI parameters of the NR group were significantly higher than those of the LR and VR groups. In the LR and VR groups, the PVPI and ELWI significantly increased at 4 h post-BS, and then gradually decreased. The PVPI and ELWI parameters of the VR group were significantly lower than those of the LR group (p < 0.05; Table 1).
Hemodynamic Parameters in BS Rats.
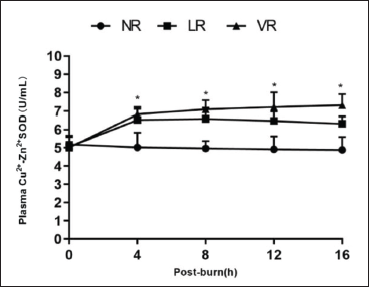
Effects of VPA on the Plasma Cu2+-Zn2+-SOD Activity
The plasma Cu2+-Zn2+-SOD activity gradually increased with fluid resuscitation. The plasma Cu2+-Zn2+-SOD activity was significantly higher in the LR and VR groups than in the NR group. The plasma Cu2+-Zn2+-SOD activity was higher in the VR group than in the LR group, but there were no significant differences in the plasma activity of Cu2+-Zn2+-SOD between the two groups (Figure 1).
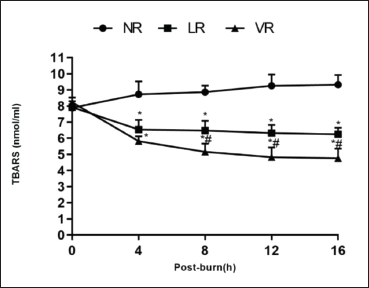
Effects of VPA on TBARS Concentration
The plasma concentration of TBARS decreased significantly after BS in the LR and VR groups but increased in the NR group. Compared to the NR group, the TBARS concentration in the LR and VR groups was significantly reduced after BS (p < 0.05). The plasma concentration of TBARS was significantly lower in the VR group than in the LR group (p < 0.05; Figure 2).
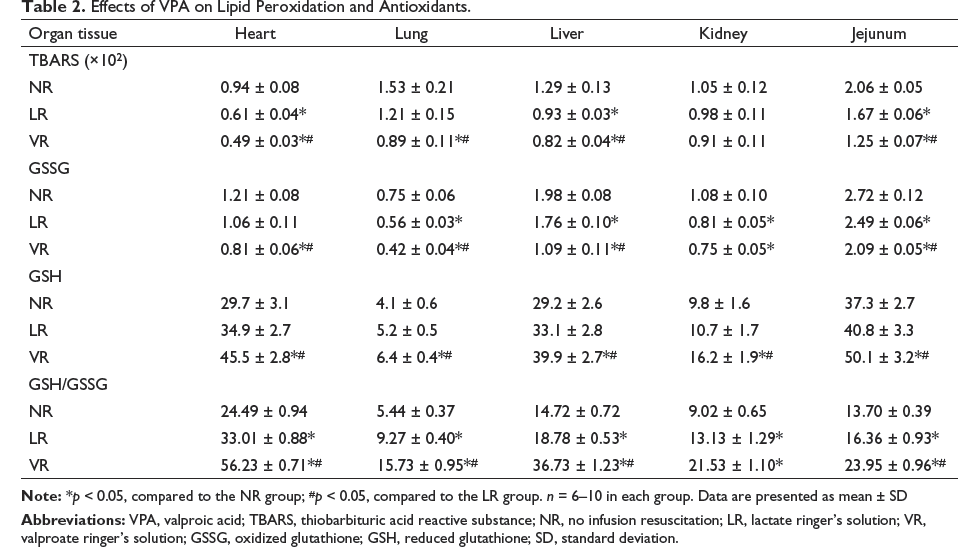
Effects of VPA on Lipid Peroxidation and Antioxidants
Compared to the NR group, TBARS concentration in various tissues in the LR and VR groups decreased significantly, but there was no significant difference in the kidney tissue. Compared to the LR group, the TBARS concentration significantly decreased in various tissues (with the exception of the kidney tissue) in the VR group (p < 0.05). The concentration of GSSG in the LR and VR groups was lower than that in the NR group, but the concentration of GSH and GSH/GSSG ratio in the LR and VR groups was significantly higher than that in the NR group. Compared to the LR group, the concentration of GSSG in the VR group was significantly decreased in the heart, lung, liver, and jejunum tissues, but the concentration of GSH and GSH/GSSG ratio was significantly increased. (p < 0.05; Table 2).
Effects of VPA on Lipid Peroxidation and Antioxidants.
Effects of VPA on Antioxidant Enzyme Content
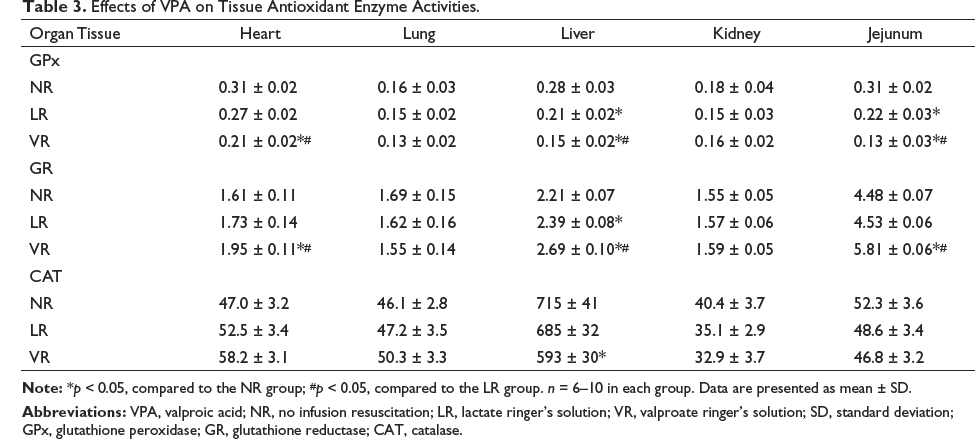
The GPx content in various tissues in the LR and VR groups was significantly lower than those in the NR group. Compared to the LR group, the content of GPx in the VR group was significantly decreased, but the activity of GR was significantly increased (p < 0.05; Table 3). The CAT content in most tissues (with the exception of the liver tissue) was similar in all the groups, and no significant inter-group differences were found (Table 3).
Effects of VPA on Tissue Antioxidant Enzyme Activities.
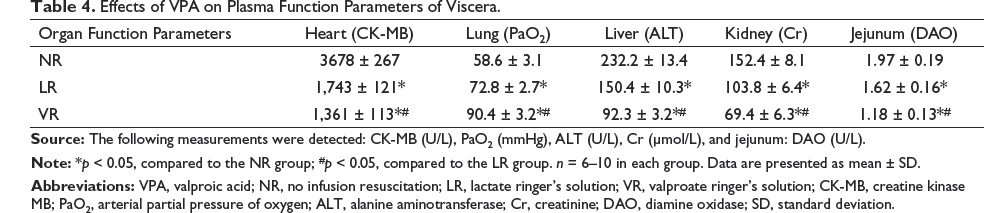
Effects of VPA on the Plasma Function Parameters and Viscera Water Concentration
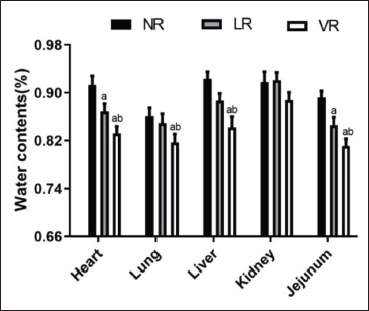
Compared to the NR and LR groups, PaO2 was significantly increased in the VR group, while the activities of ALT, CK-MB, DAO, and Cr in the VR group were significantly decreased (p < 0.05; Table 4). The water content of various tissues (with the exception of the kidney tissue) of the VR group was significantly lower than that of the LR group (p < 0.05), and there were no significant differences in the kidney tissues between the two groups (Figure 3).
Effects of VPA on Plasma Function Parameters of Viscera.

Effect of VPA on the 24 h Survival Rate
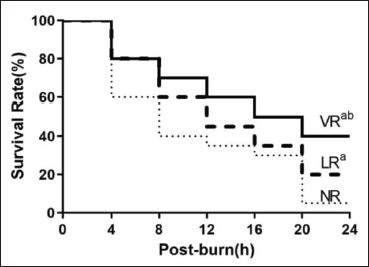
There was no significant difference in the survival rate at 4 h post-BS among all the groups (p > 0.05). The survival rates at 8, 16, and 24 h post-BS were 40% (8/20), 30% (6/20), and 5% (1/20), respectively, in the NR group; 60% (12/20), 40.0% (8/20), and 20% (4/20), respectively, in the LR group; and 70% (14/20), 50% (10/20), and 40% (8/20), respectively, in the VR group. Thus, VPA significantly improved the survival rate of the BS rats compared to the LR group (p < 0.05; Figure 4).
Discussion
Capillary permeability increases after severe burn and trauma shock and leads to severe edema and complex changes in tissues and organs. Ischemia and hypoxia in tissues and organs can induce tissue edema and organ injury, which can lead to sepsis and even MODS. The goal of BS treatment is to provide early and timely fluid resuscitation to maintain blood perfusion of tissues and important organs. A combination of colloidal and crystalloid fluid resuscitation is often used in the treatment of BS or sepsis and hypovolemic shock. Currently, NS and LR are widely used for crystalloid fluid resuscitation; however, neither represents an ideal choice. A large amount of normal saline can cause perchloric acidosis. While lactate infusion may result in intracellular pseudohypoxia, metabolic inhibition, and inflammatory response. Acetate-containing solutions can eliminate both the above-mentioned defects, but such solutions are still not optimal because of their inability to metabolize in anoxia, protect against glycolysis, and correct lactic acidosis (Liu et al., 2016b). Thus, there is a need to develop a novel fluid treatment to improve resuscitation efficiency in patients with severe shock.
Recent research has shown that lipid peroxidation is a key factor in increased vascular permeability after severe BS (Idrovo et al., 2021). The application of VPA in the early stage of shock can play a role in cell protection, antioxidation, and anti-inflammatory activity. A new method has been developed for the treatment of severe burns, septic shock, and MODS (T. Liu et al., 2019; Tang et al., 2018). It has also been reported that inhibiting the activities of myeloperoxidase and malondialdehyde reduces lipid peroxidation (Emekli-Alturfan et al., 2015; Oztopuz et al., 2020). However, it is not yet known whether VPA reduces tissue edema and protects multiple organ functions by alleviating lipid peroxidation in a BS rats model. Multiple studies have shown that VPA improves glucose metabolism disorders, protects multiple organ function, and maintains cell stability (Dos Santos Chemelo et al., 2021; T. Liu et al., 2019; Luo et al., 2013; Soria-Castro et al., 2019; Williams et al., 2019; Yiş et al., 2009). The stress response and catabolism of the body are quite intense after extensive burns, and the body undergoes a complex series of changes that cause excessive inflammation of tissues and organs. It has been shown that VPA improves the tolerance of shock-induced tissue and organs to the ischemic, hypoxic, and inflammatory responses of the body (Liu & Wang, 2022). In this research, we studied the effective mechanism of VPA on lipid peroxidation and edema in various tissues in rats with 50% TBSA third-degree scalding. The results clearly showed that VPA significantly attenuated lipid peroxidation, vascular permeability, and tissue edema, and improved organ function and the survival rate.
The hemodynamic parameters of fluid resuscitation after burn injury have been reported previously (Liu et al., 2016a; Luo et al., 2013; Young et al., 2014). Our results showed that the MAP and CO parameters in the LR and VR groups were significantly higher than those of the NR group at 4–24 h post-BS. Compared to the LR group, the MAP and CO parameters were significantly increased in the VR group. The 2 resuscitation solutions restored the circulating plasma volume, but VR was superior to LR in the BS rats. Conversely, the PVPI and ELWI parameters in the LR and VR groups were significantly lower than those of the NR group at 4–24 h post-BS. Additionally, the PVPI and ELWI parameters were significantly lower in the VR group than in the LR group. This shows that VPA can reduce tissue edema, which is similar to the results reported by other studies (Kühne et al., 2021; Kasotakis et al., 2017). However, it should be noted that a low blood volume is one of the disadvantages of the PiCCO system; thus, as other studies (Luo et al., 2013; Obata et al., 2016) have shown, the PiCCO system may overestimate ELWI and PVPI.
The free radical scavenging system can eliminate the harmful effects on the tissues and organs that are caused by oxygen-free radicals. Under normal conditions, the production and clearance of cellular free radicals and reactive oxygen species are in a dynamic equilibrium. SOD is a scavenger of oxygen-free radicals and plays an important role in oxidative damage (Simon-Szabo et al., 2021). Our results showed that the activities of plasma Cu2+-Zn2+-SOD gradually increased with fluid resuscitation. The activities of plasma Cu2+-Zn2+-SOD in the LR and VR groups were significantly higher than those in the NR group. Compared to the LR group, the activity of plasma Cu2+-Zn2+-SOD in the VR group increased, but there were no significant differences between the two groups. This suggests that VPA alleviated lipid peroxidation, which is supported by other studies (Chaudhary & Parvez, 2018; Ourique et al., 2016). The level of TBARS can be used to measure the level of lipid peroxidation as previously described (Liu et al., 2021; Naspolini et al., 2021). In this study, the plasma concentration of TBARS decreased significantly after BS in the LR and VR groups but increased in the NR group. The TBARS concentration in various tissues (with the exception of the kidney tissue) in the LR and VR groups was significantly decreased. These results are consistent with those of previous studies (Liu et al., 2016b; Luo et al., 2013).
SOD, GPx, and GR are the fundamental antioxidant enzymes, which are the markers of antioxidant status. SOD catalyzes the dismutation of O2− to H2O2, which would later be transformed into H2O and O2 by CAT. GPx, on the other hand, contributes to the disintegration of H2O2 and other organic peroxides. GPx is another important antioxidant. It can scavenge lipid peroxides induced by reactive oxygen-free radicals, which specifically reduces GSH to GSSG by using GPx. GR can catalyze GSSG with GPx to produce GSH, which prevents the lipid peroxidation chain reaction, which plays a positive role in protecting tissues and organs by minimizing the degree of lipid peroxidation. We evaluated the effects of VPA on these enzyme activities in rats who underwent BS followed by resuscitation. VPA reduced the concentration of GSSG in various tissues and increased the concentration of GSH and GSH/GSSG ratio as described previously (Lapehn et al., 2021; Salimi et al., 2022). Our findings about the content of antioxidant enzymes with VPA on the resuscitation of the scalded rats were consistent with those reported previously (Koroglu et al., 2021; Lapehn et al., 2021; Simon-Szabo et al., 2021). In summary, VPA markedly alleviated lipid peroxidation, thereby improving visceral function in the scalded rats.
Compared to the NR and LR groups, most organ function parameters in the VR group were significantly decreased, with the exception of PaO2, which was significantly increased. Thus, the VPA resuscitation of the scalded rats improved organ function. The water content of various tissues (with the exception of the kidney tissue) was significantly lower in the VR group than in the LR group. This is consistent with our previous research and other research (Deckmann et al., 2021; Liu et al., 2016b), indicating that VPA decreases vascular permeability. Thus, the VPA resuscitation of the scalded rats was found to reduce tissue edema and protect organ function.
A comparison of the survival rates confirmed that VPA was superior to LR in the resuscitation of the scalded rats. In this experiment, the NR group had a lower survival rate of 5% than the LR and VR group. Resuscitation with VR doubled the 24-h survival rate of the LR group (40% vs. 20%), which further demonstrated that VR provided superior fluid resuscitation from BS than LR as previously reported (Kühne et al., 2021).
One limitation of this research was that it did not evaluate the activity of key enzymes in the glucose metabolism pathway. This study aimed to investigate whether the use of VPA in the resuscitation of scalded rats reduced tissue edema by inhibiting lipid peroxidation, thereby improving organ function and the survival rate.
VPA significantly increased the MAP and CO and significantly decreased the PVPI and ELWI. It also increased the activity of plasma Cu2+-Zn2+-SOD and decreased the plasma TBARS level. VPA reduced the TBARS concentration and the content of GSSG in various tissues and increased the concentration of GSH. VPA also decreased the activity of GPx and CAT but significantly increased the activity of GR in various tissues. VPA significantly improved various organ functions and decreased water content. VPA significantly improved the survival rate. The protective effects of VPA may be achieved by inhibiting lipid peroxidation.
Abbreviations
LR: Lactate Ringer’s solution; VR: Valproate ringer’s solution; NR: No infusion resuscitation; CK-MB: Creatine kinase-MB; PaO2: Partial pressure of oxygen; ALT: Alanine aminotransferase; Cr: Creatinine; DAO: Diamine oxidase; VPA: Valproic acid; MODS: Multiorgan dysfunction syndrome; PVPI: Pulmonary vascular permeability index.
Authors’ Contribution
(I) Conception and design: RL, SMW; (II) Administrative support: RL, YTF; (III) Provision of study materials or patients: RL, SMW; (IV) Collection and assembly of data: RL, YTF, FQJ; (V) Data analysis and interpretation: RL, SMW, FQJ, YJY; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research was supported by the Special Fund of the Heilongjiang Provincial Academy of Science and Technology Cooperation Project of China (No. YS20C02) and the Heilongjiang Provincial Health Bureau Fund, China (No. 20211010000021).
Animal Ethics
All animal experiments were approved by the Animal Ethics Committee of Heilongjiang Provincial Hospital, China (No. 2021-099), in compliance with Chinese national guidelines for the care and use of animals.
