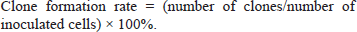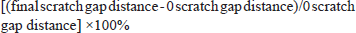Abstract
Background
Scutellaria baicalensis is an important medicinal plant used in China. Several compounds have been extracted from S. baicalensis using modern techniques. Baicalin, an active ingredient of S. baicalensis, is widely used clinically. However, its clinical use is limited owing to poor oral bioavailability and intestinal absorption.
Objectives
To evaluate the anti-tumor effect of baicalin magnesium salt (BA-MG, a novel magnesium salt form of baicalin with superior water solubility) on the human hepatocellular carcinoma cell line, HepG2.
Materials and Methods
Seven groups were established, including three dosages of BA-MG (200, 250, and 300 µg/mL), baicalin, dimethyl sulfoxide (DMSO) (negative control), magnesium sulfate (negative control), and control groups. Cell proliferation was determined using the cell counting kit-8 (CCK-8) assay. Cell cycle and apoptosis were detected by flow cytometry. Cell migration was determined using a cell scratch assay. Protein expression was determined using western blotting.
Results
In vitro, BA-MG inhibited proliferation, reduced cell cloning and migration abilities, induced cell cycle arrest, and promoted apoptosis of HepG2 cells (all p < 0.05). The effects of baicalin and BA-MG on proliferation and migration, cell cycle, and apoptosis may be attributed to decreasing the expression of Bcl-2, ROCK-1, proliferating cell nuclear antigen (PCNA), and cyclin E, as well as increasing the expression of Bax and caspase-9. The efficacy of BA-MG is superior to that of baicalin at the same dose.
Conclusion
BA-MG showed superior effects on inhibiting cell proliferation and inducing apoptosis in liver cancer cells.
Introduction
Liver cancer is a malignant tumor that seriously endangers human health. It is characterized by a high recurrence rate and uncontrolled growth. 1 Because the early symptoms of liver cancer are hardly observed, patients are generally diagnosed with liver cancer that developed to a late stage and lose the best treatment opportunity. Chemotherapeutic drugs are effective for patients to some extent. However, their side effects impair the survival status of the patients, leading to more complications, such as irreversible liver and kidney damage, severe vomiting, fever, and reduced immunity. 2 Therefore, it is crucial to discover novel anticancer drugs with fewer adverse effects. Natural medicines and natural compounds play an increasingly important role in the treatment of cancers.3, 4
In China, the traditional Chinese medicine, Scutellaria baicalensis, has long been used to treat liver and gall diseases. It has the functions of clearing heat and dampness, relieving fire, detoxifying, stopping bleeding, and placing the fetus. S. baicalensis and its active ingredients play important hepatoprotective roles.5, 6 Baicalin, an active ingredient of S. baicalensis, has the highest content as a standard for quality control. Baicalin has bacteriostatic, diuretic, anti-inflammatory, spasmolytic, and anti-cancer effects.7, 8 The commonly used dosage forms of baicalin in clinics include decoctions, tablets, and capsules. However, owing to its poor water solubility, the absorption and utilization of baicalin after oral administration are low, and the expected efficacy cannot be achieved. This limits the clinical application of baicalin. Baicalin magnesium salt (BA-MG) overcomes the above shortcomings, because it is completely soluble in water and easily absorbed, which greatly improves the bioavailability of the drug. 9
In this study, we verified that BA-MG promotes apoptosis and inhibits the proliferation of HepG2 cells in vitro. The objective is to provide an experimental basis for further development and application.
Materials and Methods
Cell Culture
The hepatocellular carcinoma cell line, HepG2, was purchased from Shanghai Saibaikang Biotechnology Co., Ltd. Cells were cultured in DMEM under conditions of 5% CO2, 37°C temperature, and 70% humidity. After culturing, the cells were counted and diluted for subsequent experiments.
Cell Counting Kit (CCK)-8 Assay
Two 96-well plates were inoculated for 24 or 48 h for each drug-treatment group. The groups were zero adjustment (cell-free), blank control, BA-MG 50, 100, 150, 200, 250, and 300 µg/mL. The cells cultured to the logarithmic growth phase were counted and diluted into a uniform single-cell suspension, and 500 cells were inoculated into each well. The zero-adjustment and blank control groups only added a complete medium. The same batch was used for all other groups. A spectrophotometer was used to detect the absorbance at 450 nm, taking the average optical density (OD) value of the remaining multiple holes and excluding outliers. The inhibitory rate and half-maximal inhibitory concentration (IC50) were calculated to determine the optimal time for drug action.
Experimental Grouping
Seven groups were used in this study: control, dimethyl sulfoxide (DMSO) (negative control, baicalin solvent), magnesium sulfate (negative control, 67µg/mL magnesium sulfate heptahydrate (MgSO4·7H2O)), baicalin (237 µg/mL), low, medium, and high doses of BA-MG (200, 250, and 300 µg/mL, respectively).
Three doses of BA-MG (200, 250, and 300 µg/mL) near the IC50 were selected in this study. The purities of the BA-MG, MgSO4·7H2O, and baicalin standards were 82.6%, 99%, and 98%, respectively. To ensure comparability, the concentrations of baicalin (237 µg/mL) and MgSO4·7H2O (67 µg/mL) were calculated based on the highest concentration (300 µg/mL) of BA-MG.
Colony Formation
Forty-eight hours after treatment, trypsin was used to digest the adherent cells, and digestion was terminated at any time according to the cell status. A complete culture medium was then added to prepare the cell suspension. The cell suspension of each group was diluted, and the small cell culture dishes of the new group were renumbered. A total of 600 cells were collected from each group and placed in new dishes for further culture. The cells were gently mixed and cultured for 15 days. Most groups had more than 30 colonies, and the culture was terminated. Photographs were obtained after fixation. Cells in each image were counted with ImageJ software to calculate the clone formation rate according to the following equation:
Cell Cycle Detection by Flow Cytometry
All cells in each dish were collected 48 h after treatment, and the cell counts were determined. The number of cells in each group ranged from 2.0 × 10 5 to 1.0 × 10 6 . Phosphate buffered saline (PBS) (2 mL) was dropped twice for repeated cleaning, and 1 mL of PBS-suspended cells was added. Then, a new set of flow tubes was renumbered A–G, and 3 mL of anhydrous ethanol was added to each tube. Anhydrous ethanol was kept for 24 h in advance at −20°C. One milliliter of the cell suspension was added drop by drop into anhydrous ethanol corresponding to the tube number, so that the cells contacted the anhydrous ethanol to ensure complete cell fixation. Seven groups of cells were kept at −20°C refrigerator and frozen overnight (fixed time ≥24 h). After fixation for 24 h, cells were rewarmed and fully hydrated at room temperature for 15 min. The fixed cells were centrifuged (1700 revolutions per minute (rpm), 7 min), ethanol was discarded, and the cells were washed twice with PBS. One milliliter of the DNA staining solution was taken from the kit, the cells were re-suspended and vortexed for 5–10 min to ensure full contact with the reagent. The reaction was carried out for 30 min at room temperature in the dark. Owing to the high viscosity of the periodic reagent, after passing the screen, the flow tube had to be re-plucked before the machine was tested, so that the cells were completely dispersed and suspended by an external force to avoid clogging the machine.
Apoptosis Detection by Flow Cytometry
After 48 h of cell dosing, all the cells in the dish were collected, including floating cells killed by dosing and cells washed with PBS. Adherent cells were digested with trypsin-free ethylene diamine tetra acetic acid (EDTA). The suspension was collected into the corresponding A–G centrifuge tube and resuspended after centrifugation. After counting, appropriate amounts of cells were added to flow tubes numbered A–G, respectively (the number of cells in each group was ≤5 × 10 5 ). The solution was discarded, the cells were cleaned, centrifuged at 1200 rpm for 5 min, and the cleaning procedure was repeated twice. Next, the binding buffer in the flow apoptosis kit was added to the flow tubes according to the specification of 500 µL/tube, and the cells were re-suspended. The suspension was filtered through a 300-mesh screen. Then, 5 µL of fluorescein isothiocyanate (FITC) and propidium iodide (PI) reagents were added to the flow tube, reacted under light for 30 min, and allowed for detection. From the remaining cells, one group of normal cells and two groups of cells that could undergo apoptosis after drug administration were selected. A total of 1–5 × 10 5 cells were selected. Cells in the three groups were counted and cleaned according to the above steps, and binding buffer (500 µL) was added to the normal group. The flow tube was pulled before the up-flow cytometer to fully suspend the cells and to avoid clogging the instrument.
Cell Scratch Test
On the back of the six-hole plate, three straight lines were equidistantly drawn using a ruler across each hole. After 48 h of treatment (dosing method was the same as that described above), the cells were washed and removed with PBS. Cells were counted, diluted, and inoculated into plates at a density of 5×10
4
/well. The rats were placed in an incubator and observed. The fluid was normally changed during this period, and the cells were scratched after they grew into a dense monolayer. Three straight lines were drawn perpendicular to the backside of the adherent cells in the dish with a 10-µL spear tip compared to a ruler. The spear tip remained vertical without tilting. The PBS cleaned the floating cells and exposed the scratches to prevent the line of scratches from affecting sight and disturbing the results when capturing photos. The scratch condition at 0 h was recorded under a microscope for the convenience of subsequent analysis. At 12, 24, 36, and 48 h after the scratch, the same location was selected to capture photos and record. The intersection point was used for positioning, and the same position was selected for observation and longitudinal analysis. The cell scratch healing rate was calculated using the following equation:
Western Blotting
Seven groups of A–G cells were treated with different doses for 48 h. The concentration of bicinchoninic acid (BCA) was measured, and all seven histones were diluted to the lowest concentration in the seven groups. After mixing in the blender, the protein was boiled at 100°C for 10 min for denaturation. To avoid protein degradation caused by repeated freezing and thawing in subsequent experiments, the proteins were stored at −80°C after packaging. The obtained images were analyzed using ImageJ software, and GraphPad Prism 8.0 was used to draw diagrams.
Statistical Analysis
Statistical analyses were performed using SPSS 25.0, and statistical charts were drawn using GraphPad Prism 8.0. Data are expressed as mean ± standard deviation (X ± S). If the data met the criteria of normal distribution and homogeneity of variance, one-way ANOVA was used to compare means between groups. The Newman–Keuls Q test was used to compare means between multiple samples in pairs. Otherwise, the Games–Howell test was performed. Statistical significance was set at p < 0.05.
Results
BA-MG Inhibited Cell Viability and Clonal Formation of HepG2 Cells
The cell counting kit-8 (CCK-8) results showed that BA-MG inhibited the growth of HepG2 cells. The effect of BA-MG on the growth of HepG2 cells showed a time- and dose-dependent relationship (Figure 1A). The IC50 of BA-MG in HepG2 cells was 297.901 and 237.9 µg/mL at 24 and 48 h, respectively. The drug effect was more evident when the action time was 48 h. Thus, 48 h was selected as the follow-up experiment time, and 200, 250, and 300 µg/mL were selected as the follow-up experimental concentrations.
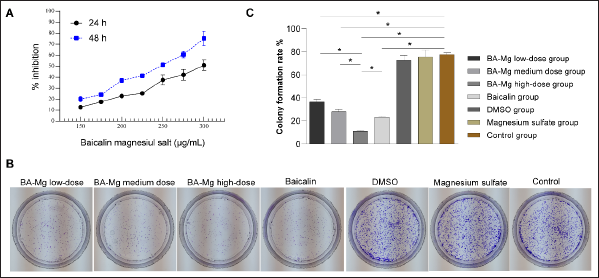
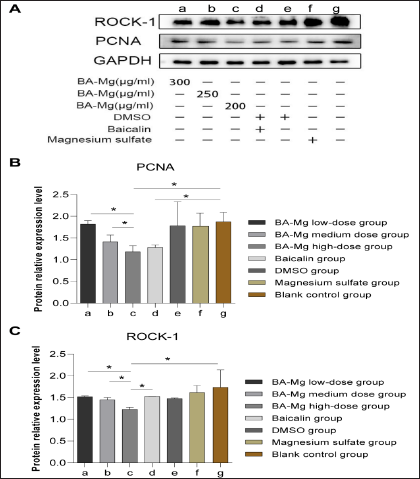
Clonal formation results revealed that both BA-MG and baicalin inhibited the clonal formation ability of HepG2 cells (p < 0.05, Figure 1B–C). The inhibitory effect of BA-MG on clonal formation in HepG2 cells was concentration-dependent. Compared to that of the baicalin group, the colony formation inhibitory effect of the high-dose BA-MG group was more significant (p < 0.05), indicating that the magnesium salt of baicalin had a more obvious inhibitory effect at the same dose as baicalin. We further investigated the expression of proliferating cell nuclear antigen (PCNA) using western blotting. The results showed that both high-dose BA-MG and baicalin decreased the expression of PCNA (Figure 2A and B).
BA-MG Inhibited Migration of HepG2 Cells
The cell scratch test detected changes in the migratory ability of each group (Figure 3). The results of the scratch test showed that BA-MG and baicalin inhibited the migration of HepG2 cells. The higher the concentration of BA-MG, the more obvious the inhibitory effect on cell migration (p < 0.05). BA-MG inhibited cell migration better than baicalin did at the same dose (p < 0.05).
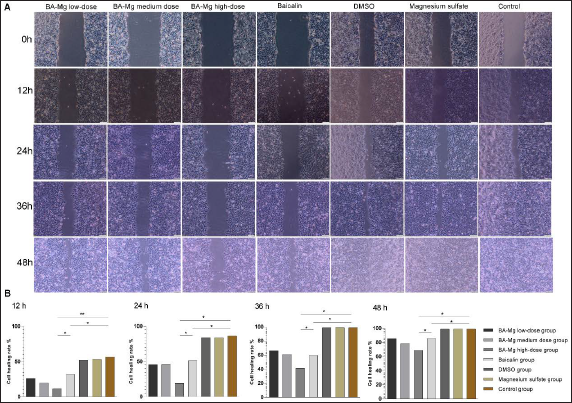
We then detected the protein expression of Rho-associated protein kinase 1 (ROCK-1) using western blotting (Figures 2A and C1). Compared to that of the control group, high-dose BA-MG significantly inhibited the expression of ROCK-1. Additionally, the inhibitory effect of BA-MG on ROCK-1 expression was dose-dependent.
BA-MG Induced Cell Cycle Arrest
Cell cycle changes in each group were analyzed using flow cytometry (Figure 4A–B). Compared with that of the control group, the proportion of G2 phase in the BA-MG and baicalin groups significantly decreased (p < 0.05); however, no significant difference was detected between the DMSO and the magnesium sulfate groups (p > 0.05). The cell cycle arrest gradually became more obvious with the increase in drug dose, showing dose-dependent characteristics. The high-dose BA-MG group showed the lowest G2 phase ratio compared with that of the baicalin group (p < 0.05). Additionally, the expression of the cell cycle-related protein, cyclin E, was determined by western blotting (Figure 4C). Compared to that of the control group, BA-MG and baicalin treatment significantly inhibited the expression of cyclin E (p < 0.05). The decrease in cyclin E expression in the three BA-MG groups was dose-dependent (p < 0.05). Moreover, the high-dose BA-MG group showed a marked decrease in cyclin E expression compared to that in the baicalin group (p < 0.05).
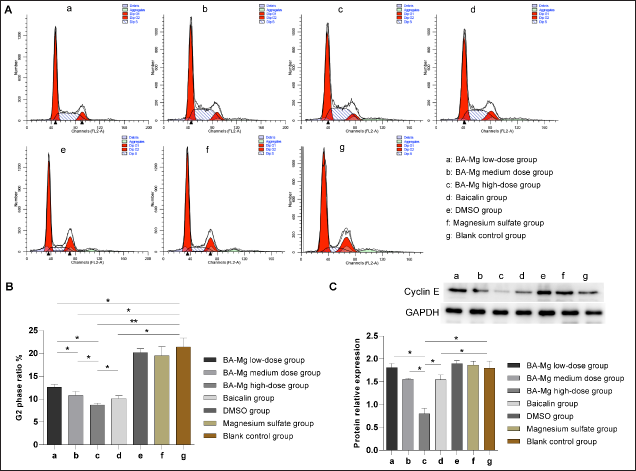
BA-MG Induced Apoptosis of HepG2 Cells
Apoptosis in each group was analyzed using flow cytometry (Figure 5A–B). The low-, medium-, and high-dose BA-MG, as well as baicalin groups significantly promoted apoptosis when compared with control group (p < 0.05). A significant difference was detected between the BA-MG low- and medium-dose groups (p < 0.05). Moreover, a significant difference was detected between the BA-MG low- and high-dose groups (p < 0.05). The apoptosis rate in the high-dose BA-MG group was significantly higher than that in the baicalin group (p < 0.05). The results of cell apoptosis showed that baicalin and BA-MG promoted cell apoptosis. The apoptotic effect of BA-MG increased with increasing the drug dose. The results showed that BA-MG exhibited a higher apoptotic effect than that of baicalin at the same dose.
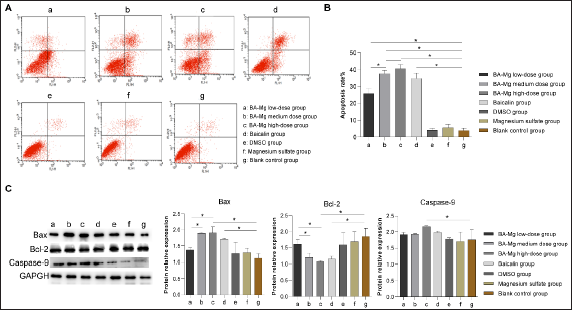
We then determined the expression of several apoptotic proteins using western blotting (Figure 5C). Both high-dose BA-MG and baicalin decreased Bcl-2 expression and increased Bax expression (p < 0.05). However, no significant differences were detected between the high-dose BA-MG and baicalin groups (p > 0.05). In addition, high-dose BA-MG increased caspase-9 expression compared to that of the control group, but this change was not observed in the baicalin group.
Discussion
In addition to surgical resection, ablation, intervention, targeted therapy, immunotherapy, and combination therapy have been used for liver cancer. However, liver cancer remains an unsolved problem.10, 11 Traditional Chinese medicine can improve the therapeutic effects in liver cancer. In our study, we focused on S. baicalensis, which is traditionally used to treat pneumonia, diarrhea, jaundice, and so on, and has been recently proven to exert an anti-tumor effect. To date, many researchers have carried out a large number of studies on the anticancer effects of S. baicalensis and its extracts, and have proven that S. baicalensis and its extracts are potential anticancer drugs.12–14 Baicalin, an extract of S. baicalensis, inhibits a variety of tumors. For example, baicalin showed anti-tumor activity in bladder cancer by inducing FTH1-dependent ferroptosis. 15 Baicalein and baicalin could inhibit ovarian cancer cells viability by inhibiting the expression of multiple cancer-promoting genes, while showing less effect on normal cells. 16 Baicalin could inhibit cell viability, migration, and invasion while inducing apoptosis of breast cancer cells through the regulation of miR-338-3p and MORC4 expression. 17 Baicalin inhibited epithelial–mesenchymal transition and cell cycle progression while inducing apoptosis in lung cancer.18, 19 In hepatocellular carcinoma, baicalein and baicalin are demonstrated to contribute anti-tumor immunity by inhibiting PD-L1 expression. 13
BA-MG is a highly water-soluble baicalin. In this study, we used baicalin as a positive control and confirmed that the anticancer effect of BA-MG was superior to that of baicalin in vitro. Baicalin can substantially reduce the proliferation level of pancreatic cancer SW1990 cells. 20 In addition, baicalin can block the PBK/TOPK pathway, thus inhibiting the proliferation of lung cancer cells. 21 Baicalin inhibited the migration and invasion of HeLa and SiHa cells in a dose-dependent manner. 22 We detected the survival of the cells in each experimental group after drug addition using the CCK-8 method to analyze cell proliferation, evaluated the inhibitory effect of BA-MG on HepG2 cells by cell colony formation assay, and detected the molecular markers related to proliferation at the molecular level. Both BA-MG and baicalin inhibited HepG2 cell proliferation. At the same dose, the inhibitory effect of BA-MG on HepG2 cells was more pronounced than that of baicalin. Baicalin can remarkably increase the apoptosis of pancreatic cancer SW1990 cells. 20 By promoting the expression of Dickkopf (Dkk1), an important antagonist of the Wnt signaling pathway, BA-MG inhibited Mir-217/Dkk1 signaling pathway and induced apoptosis of colon cancer cells. 23 Sui et al. found that baicalin plays an anti-tumor role in lung cancer by regulating the Akt/mTOR signaling pathway, leading to apoptosis and inducing cycle arrest. 19 Further study by Yu et al. proved that baicalin can regulate the expression of CyclinD, CyclinE, CDK2, and apoptosis-related proteins, caspase-3, caspase-9, Bcl-2, and Bax in HepG2 and SMMC-7721 cells to induce apoptosis. 24 In addition, baicalin can induce apoptosis of HepG2 cells by activating the p38MAPK signaling pathway and interfering with the mitochondrial pathway.25, 26 Flow cytometry results showed that both BA-MG and baicalin induced apoptosis in HepG2 cells. At the molecular level, apoptotic star molecules include anti-apoptotic molecules, such as Bcl-2, pro-apoptotic molecules, such as Bax, and a series of molecules in the caspase family. The star molecules identified in this study are Bcl-2, Bax, and caspase-9. Baicalin and BA-MG changed the expression of these proteins, and BA-MG had a stronger effect on cell apoptosis than that of baicalin at the same dose. Based on the antitumor effect of S. baicalensis and its extract, this study investigated whether BA-MG has the same antitumor effect. Through this study, we verified the effects of BA-MG on promoting apoptosis, inhibiting proliferation, and influencing the cancer cell cycle.
As the developer of BA-MG, Dr. Liu Cuizhe has confirmed through full experiments that BA-MG has many advantages over baicalin: magnesium salt is the original and stable form of baicalin, the water solubility of BA-MG is 300 times higher than that of baicalin, its stability is better than that of baicalin, and pharmacokinetics showed that BA-MG had a longer residence time in the body.27−29 In vivo experiments showed that BA-MG had a higher intestinal absorption. Owing to the advantages of BA-MG, the efficacy of BA-MG in vivo is more remarkable than that of baicalin. In this study, the anticancer effects of BA-MG were verified from multiple perspectives. According to the results of in vitro experiments, BA-MG had a more substantial inhibitory effect on HepG2 cells than that of baicalin, which may be attributed to the high-water solubility and good stability of BA-MG.
Conclusion
Both baicalin and BA-MG can inhibit proliferation, cell cloning, and migration of HepG2 cells. In addition, they can induce cell cycle arrest and promote cell apoptosis. These effects may be attributed to decreasing the expression of Bcl-2, ROCK-1, PCNA, and cyclin E and increasing the expression of Bax and caspase-9. The application of BA-MG in treating tumors is promising, and its efficacy is superior to that of baicalin.
Footnotes
Abbreviations
Acknowledgment
We thank Chengde Medical College for providing us with the experimental platform. This study was funded by the Science and Technology Project of the Hebei Education Department (Project No. ZD2021003), the Detail Project of Precision Medicine Joint Fund of the Natural Science Foundation of Hebei Province (Project No. H2021406066), Research Start-up Fund for High-level Talents of Chengde Medical College (Project No. 202002), and Key Discipline Construction Projects of Hebei Province Higher School (Grant/Award Number: [2013]4).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This study was funded by the Science and Technology Project of Hebei Education Department (Project No. ZD2021003); Detail Project of Precision Medicine Joint Fund of Natural Science Foundation of Hebei Province (Project No. H2021406066); Research Start-up Fund for High-level Talents of Chengde Medical College (Project No. 202002); Key Discipline Construction Projects of Hebei Province Higher School (Grant/Award Number:[2013]4).
Statement of Informed Consent and Ethical Approval
Necessary ethical clearances and informed consent were obtained before initiating the study from all the participants.