Abstract
Introduction
The Omicron variant of SARS-CoV-2 (COVID-19) became the global community’s third major cause of worry. In the current study, we deployed a self-reported survey questionnaire to investigate the degree of comprehension, awareness and perception of the Omicron variant of COVID-19 in patients with Parkinson’s disease (PD) and their respective caregivers (CGs).
Materials and Methods
Using a standardised questionnaire, we conducted a prospective study on PD patients attending the neurology outpatient department prior to and during the COVID-19 pandemic. The study period was between February and August of 2022.
Results
A total of 114 CGs and 134 disease-affected patients were evaluated. Approximately 1.8% of the CGs and 4.5% of the patients contracted the Omicron-COVID-19. Over half of the patients (77.6%) were aware of the Omicron variant, and approximately 40.3% of them were aware of its symptoms. After receiving the Covid immunisation, patients (94.02%) reported no change in symptoms. The percentage of patients and CGs who had no symptoms of the viral infection and were not even got tested ever was 95.5% and 98.2%, respectively. Further, patients (95.5%) opted for the ‘offline’ as a preferred mode of consultation, citing the precision of treatment being the main reason.
Conclusion
No definite correlation between the Omicron variant infection and symptoms of PD could be established. The awareness regarding Omicron variant was largely unknown. More patient-centred research on larger population groups, incorporating literate and urban groups would unravel the knowledge gaps.
Introduction
The SARS-CoV-2 Omicron variant was reported approximately two years following the appearance of COVID-19. It emerged at a time when the majority of the world’s population was living with exasperation and frustration due to the devastation unleashed by COVID-19 and its accompanying sequalae. This had a widespread negative impact on social, psychological and economic well-being. Although significant research is being conducted worldwide to gain an insight into the pathophysiology, symptomatology and genetics about the Omicron variant, various aspects of the virus still remain cryptic and unexplored. This has led to a misinformation and panic in the population, resulting in a threatening situation in the healthcare sector. Isolation and social alienation were the important measures to be taken and that could be attempted only via lockdown.1, 2 This led to the origin of complications in patients with serious disorders like Parkinson’s disease (PD), who are primarily dependent on their caregivers (CGs) and doctors for routine medical check-ups, assistance with everyday tasks, and medication administration and dose changes. Cognitively impaired PD patients are especially susceptible to these social limitations and possible loss of access to regular support networks. The Omicron variant of COVID-19 could potentially limit the access of the patient to medical health facilities, thereby negatively impacting their physical and mental health. In a global poll of healthcare workers, a significant majority said that their PD patients had trouble in getting regular medicines, thereby increasing their disability. 3
The Omicron variant is less severe than previous variants of COVID-19. Despite this, the rapid transmissible nature of this variant continues to have an impact on handling of healthcare services for other illnesses, resulting in an overburdened health system worldwide. Although compared to the Delta virus, there are less chances of death, admission to an intensive care unit, and hospitalisation in the case of Omicron, they do significantly impact the unvaccinated population. 4 Importantly, existing vaccines offer the best protection against the Delta form, including some against the Omicron variant as well, particularly against severe symptoms necessitating hospitalisation. 5 A longer time interval between the first and second doses was linked to a higher likelihood of symptomatic COVID-19. 6 While additional research and data are needed to comprehend this, evidence in some contexts does suggest that the booster dose is useful in reducing Omicron’s influence.5, 7
The Omicron variant had a variable impact on the PD patients and their CGs on various parameters such as the activities of daily living (ADLs), follow-up visits, aggravation of PD symptoms, availability of medications and perceptions on vaccinations. However, there is a paucity of data worldwide, reporting the overall impact of the current Omicron variant on PD patients and their CGs. The present study aimed to identify the perception of patients with PD and their CGs regarding the Omicron variant of COVID-19, using a self-reported survey questionnaire. 8
Material and Method
The tertiary care multi-specialty university teaching and research institute was the place where this study was conducted. The study was ethically approved by the institutional review board (2020/EC/1924). The survey was done on patients diagnosed with PD (n=134) who were under follow-up treatment in the neurology/movement disorder outpatient department (OPD) and their respective CGs (n=114). The research was conducted from 1 February 2022 to 31 August 2022. Questions (n=15) in the questionnaire were related to the awareness, knowledge about the Omicron variant of COVID-19 and interpretation about its association with their disease. A summary of questions and obtained data is detailed in Table 1. Patients and CGs were contacted via telephone and interviewed. Questions were asked in Hindi, the language understandable by the rural population of North India. Each patient gave written consent at the time of visit to the hospital. Patients who died at the time of call and who did not have any CGs were excluded from the study.
Characteristics, Attitudes and Consequences of COVID-19 (Omicron) Among Patients with Parkinson’s Disease and Their CGs.
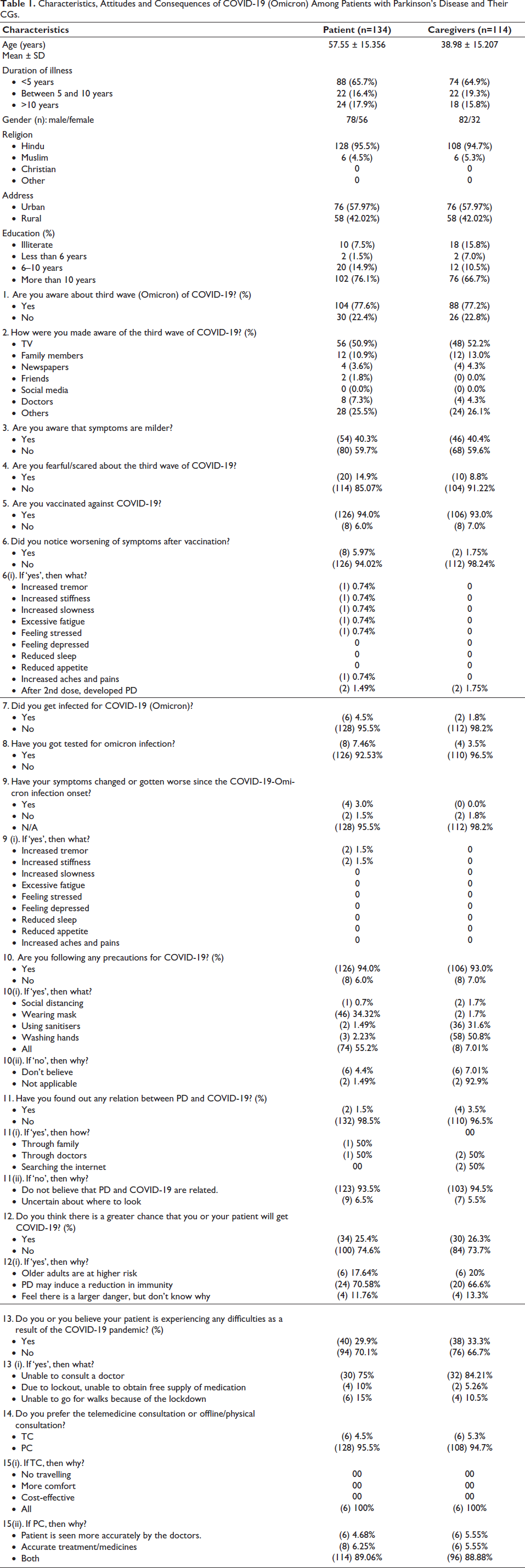
Statistical Analysis
The final data recorded, entered and summarised using MS Excel. All statistical data for categorial variables (i.e., gender, religion, education, etc.), numbers (percentages) and for continuous variables, descriptive statistics (mean and standard deviation) were given. Data analysis was done using IBM SPSS Statistics 21.0 software.
Results
A total of nearly 200 patients were in the follow-up group, out of which only 134 patients having PD and their 114 CGs could be contacted and recruited. All of them were taking the treatment and were in follow-up at the neurology OPD. Few patients were independent in all their ADLs and hence did not have a CG (n=10). Based on telephonic conversation, detailed information was collected and recorded. A total 77.6% patients (n=104) and 77.2% of CGs (n=88) were aware about the third wave (Omicron) of COVID-19 but were not fearful of the same. More than half of the patients (59.7%) and CGs (59.6%) were unaware about the symptoms. Television was the primary source of awareness in almost half of the patients (50.9%) and CG (52.2%). A significant number of patients (94.02%) and CGs (98.24%) vaccinated against COVID-19 did not notice any worsening of symptoms related to the disease after vaccination. The majority of patients (92.53%) and their CGs (96.5%) did not choose to undergo testing or have any symptoms suggestive of Omicron. So, the question of worsening of PD symptoms does not arise.
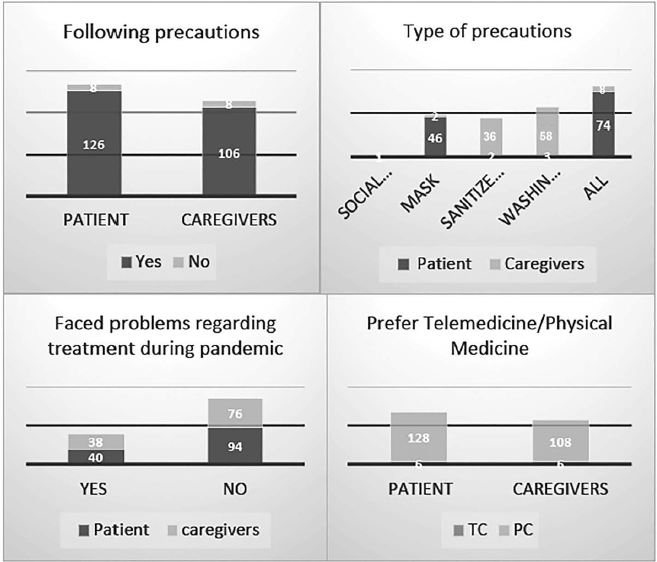
About 94% of patients and 93% of CGs were taking precautions for COVID-19 infection and wearing mask along with using sanitisers were two of the most commonly followed precautions. Most of the patients (98.5%) and CGs (96.5%) found no relation between PD and COVID-19 and did not feel (74.6% patients and 73.7% CGs) that the patient is at a higher risk of getting the Covid infection.
Inability to consult the doctor during pandemic was one of the most commonly faced problems by patients (75%) and their CGs (84.21). Physical/offline consultation was the preferred choice in maximum patients (95.5%) and CGs (94.7%), citing the accuracy of patient assessment and treatment prescription being the main reason.
Relevant data are also shown graphically in Figures 1–4.
Basic Features of the Patient Population and Their Caregivers Shown Graphically.
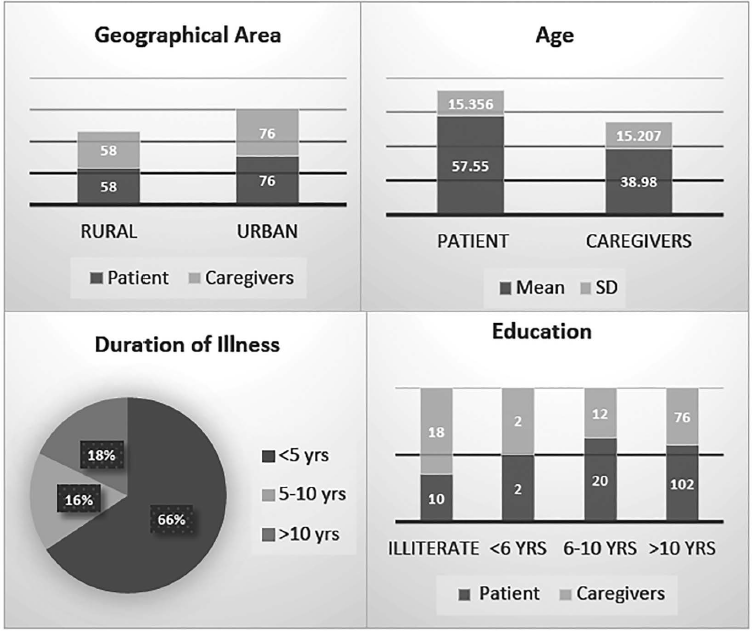
Patients’ and Caregivers’ Thoughts about Relation between Covid Vaccination and Parkinson’s Disease Shown Graphically.
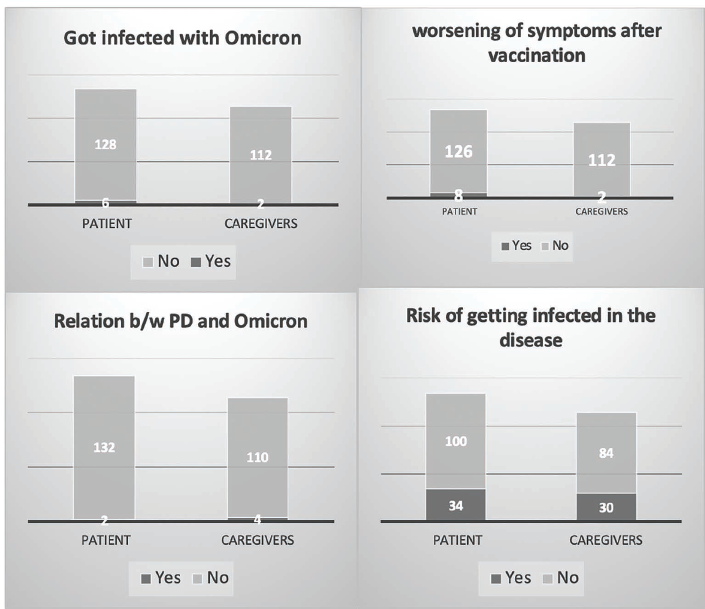
Awareness Regarding Omicron Infection Show Graphically.
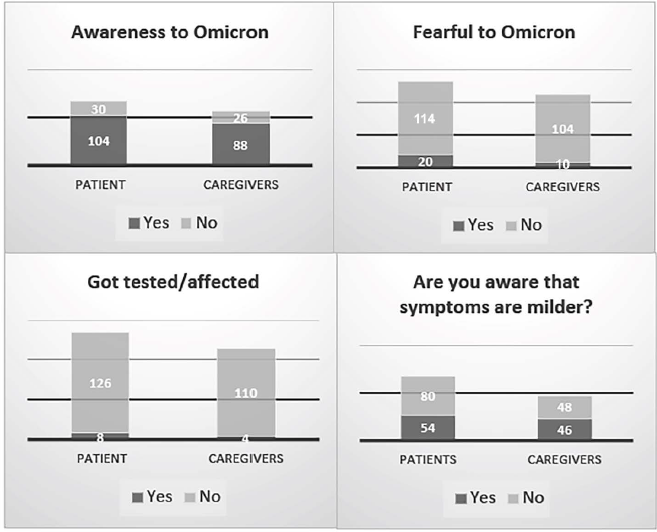
Thoughts Regarding Precautions Against Infection and Pandemic Shown Graphically.
Discussion
This cross-sectional study is one of the first to investigate the awareness of the Omicron variant regarding its occurrence, vaccination, symptoms aggravation on vaccination, vulnerability of acquiring the infection and various other factors, in patients with PD and their respective CGs. Their perception and interpretation of the Omicron variant has been aptly elucidated through the self-reported survey questionnaire. 8
Severity of the Omicron variant was less than the earlier variants. Hospitalisation, intensive care, mortality and ventilatory assistance were strikingly less than the other previous variants with life-threatening consequences. This perhaps best explains the probable reason for lesser fear and panic amongst the PD patients and CGs, even after contracting the symptoms. There was a similar perception about the disease and its relation to the Omicron variant in both patients and their CGs. Certain misconceptions about the COVID-19 infection and its variants were noted. The majority of the patients and CGs belonged to the rural and countryside areas, were uneducated and did not have access to social media. This could also be the reason for the ignorance about the Omicron variant.
For the aforesaid reasons, patients were not familiar with the existence of covid variants, making them ignorant about the preventive precautionary practices against COVID-19 infection. Maximum caregivers and patients felt that they had not acquired the infection and neither were they at a higher risk of contracting the infection. Also, a majority of them did not face any problem in patient care in terms of consultation or availability of medications during the lockdown as the lockdown was short and not on very strict rules like the first one.
Despite in small number, 82% of patients in our study completed their telephonic evaluation satisfactorily, demonstrating its viability and utility during the COVID-19 pandemic. Telemedicine thus emerged as an important tool for patient management and continuity of regular follow-up during the pandemic. Reduced social congregations and the use of face masks and sanitisers were commonly used precautions, especially for people with moderate to severe PD until an optimal control of the pandemic was attained.
According to our study, PD patients were not at a greater risk of developing COVID-19 Omicron infection. Very few studies have been conducted on the Omicron variant of COVID-19 and investigating its relation to PD are even lesser. Falla et al. 7 evaluated the lockdown effects on PD during the COVID-19 pandemic. Patients showed worsening of non-motor symptoms during the COVID-19 lockdown. A study in 2022 9 demonstrated significant difference in healthcare workers’ knowledge and significant misconceptions regarding the Omicron variant of COVID-19. This supports the findings of our study, indicating the misconceptions and ignorance about the Omicron variant among general population. Many supported the viability and necessity of telemedicine for managing and tracking the symptoms of PD patients during the COVID-19 pandemic.9–11 Similar studies on the COVID-19 pandemic and PD have been conducted in India, 8 which reported the worsening of the motor and non-motor symptoms in PD and other movement disorders. 11
This study has few limitations. It was a single centre study with small sample size, with lack of face-to-face questionnaires used for the follow-up evaluation. An online survey was used for the research, and the evaluation was based on the telephonic conversation. These reports might not accurately reflect patients’ and CGs’ perception regarding the Omicron variant. Second, there is little information on the COVID-19 vaccine’s efficacy and safety in PD patients. Third, other factors, such as vaccination attitudes, the presence of other chronic conditions and vaccination histories were not examined and might have affected patients’ willingness to accept the COVID-19 vaccine.
Conclusion
Through this study, the knowledge, awareness and perception of PD patients and their CGs about various aspects of the Omicron variant of COVID-19 regarding its severity, vaccination, precautions and effects on PD patients have been addressed. The Omicron variant remained unnoticed and was unknown to many people of rural northeastern areas of India. As of now, there is no conclusive evidence linking the pandemic, Omicron variant infection, COVID-19 vaccine and PD symptoms. Further studies with large sample size, enrolling urban and literate population, would perhaps elucidate the knowledge gaps and implications of the Omicron infection.
Footnotes
Acknowledgements
The authors are thankful to the Institute of Eminence, SRICC and Banaras Hindu University, Varanasi, Utter Pradesh, India.
Authors’ Contribution
NRD and DJ: Planning and conception, data collection and initial draft writing
VG: Data collection and statistical analysis
AK: Supervision, statistical analysis and final draft editing
All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Ethics
The study was ethically approved by the institutional review board (2020/EC/1924).
