Abstract
Background
With technological advancement and economic competitiveness there is an exponential rise in the number of shift workers. Worldwide, healthcare workers constitute the single largest proportion of workers who work on shift duty in order to provide round-the-clock healthcare services to patients. Various studies have demonstrated an association between circadian cycle disturbance due to shift work and adverse health impacts.
Purpose
The purpose of the study was to investigate the impact of night shift work on the brainstem-evoked auditory potentials in nursing interns who had been assigned to their first night shift after working day shifts.
Methods
A longitudinal, self-case-control study was designed with a sample of 67 nursing interns. Brainstem evoked response audiometry (BERA) had been done after completion of their first posting in Day-shift and then after completion of Night-shift. The paired t-test was used for data analysis.
Results
The findings of the study showed significant changes in latencies of wave II (p < .0001), wave IV (p < .0001), wave V (p = .012 & .30), interpeak latency III-V (p = .009 & .003) and V/I ratio (p < .0001) for both ears.
Conclusions
BERA is an objective non-invasive test to evaluate hearing ability by measuring increased latency and interaural latency difference. After night shift, there were significant changes in auditory acuity which was highly suggestive of delayed transmission in auditory pathway. Hearing impairment has a cascading effect on cognition which may affect night-shift workers’ daily activities and may lead to medical error and risk to patient safety.
Introduction
In present time, there is a growth in the number of shift workers and the most evident cause is technological advancement, economic competitiveness and social pressure. In developed nations, about 20% of the workforce is working in shifts, out of them one-third is engaged in night shifts.1, 2
In many countries, healthcare workers constitute the single largest proportion of shift workers. To facilitate the provision of round-the-clock health care services for sick patients, shift schedule is widely adopted. 3
Night-shift workers have many health-related problems due to disturbed circadian rhythms like insomnia, anxiety, unable to concentrate, irritable behaviour, indigestion etc. Many studies have been done to investigate the impact of night shift work on various health-related issues. In hospital set-up, studies on night-shift workers have been done to assess the effect of various factors on their health in order to improve their performance owing to their significant responsibilities towards patients admitted to hospital. In this study, we included the nursing staff who have to take care of admitted patients during odd hours, especially at night and sometimes in the absence of consultants/specialists.
Out of these significant duties of the nursing staff, one of the most important is to listen carefully and to respond immediately to the call of in-patients during odd hours of the night. During these odd hours, nursing staff are also in a state of reduced response to any stimuli or command because of altered circadian patterns. Keeping these facts in mind, we search for studies related to hearing and decision-making abilities in a hospital setup. We found studies related to cognition in night-shift workers, but there were no studies to show the effect of night-shift working on hearing ability per se. Some researchers have discovered that particularly on the night shift, there is poorer work performance and an increase in accidents. 4
The auditory brainstem response (ABR) is an auditory evoked potential. ABR is recorded from ongoing electrical activity in the brain using electrodes placed on the scalp. The resulting recording is a series of vertex waves. These waves which are seven in number (I–VII) are usually recorded in the first 10 milliseconds following broad-band and high-intensity clicks.
Night shift working affects circadian rhythm which in turn affects various physiological responses in comparison to day-time workers like- psychosomatic disturbances (impaired arousal, alertness and decision making), delayed reflexes, raised stress hormone (cortisol) levels. BERA is a useful method to assess the responses to auditory signals. So, we conducted this study to find out effect of such working conditions on the hearing ability, which is necessary for a proper cognitive response. 5
Methods
In this study, we included 67 subjects of age group 20–27 years (Mean 22.46 ± 1.41). The subjects in the study were nursing students completing their internship in one of the tertiary care hospitals in North India. These students had two shifts of posting in the hospital; Day-shift of eight hours and then Night-shift of eight hours on a rotation basis during internship. First of all, we have taken brainstem evoked auditory potentials (BEAPs) recordings after completion of their first posting in Day-shift and then after completion of Night-shift. This was a longitudinal, self-case control, interventional study. This study was done after seeking approval from the ethical committee of the institution and getting written, informed consent from the participants.
Inclusion Criteria
Hospital health workers on rotational shifts (Day-time and Night-shift) including male and female.
Exclusion Criteria
Subjects: a) With known neurodegenerative diseases. b) With hearing disorders. c) On treatment with ototoxic and sedative drugs. d) With sleep disorders. e) With psychiatric disorders.
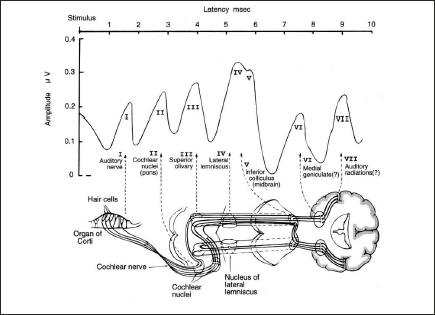
Usually two-channel recordings are made: vertex (Cz) to ipsilateral ear and Cz to contralateral earlobe derivation. Common parameters evaluated for assessing clinically relevant abnormalities of Brainstem Evoked Auditory Potentials were:
6
a) Latencies (the speed of transmission) of waves I (1.4–1.8 msec.), III (3.6–4.1 msec.), and V (5.5–6 msec.), b) Inter-peak latencies of I–III (2.0–2.6 msec.), III–V (1.8–2.5 msec.), and I–V (3.8–4.4 msec.), c) Amplitude (the number of neurons firing) ratio of wave V to wave I (Normal: 50%–300%) d) Inter-aural latency (the difference in wave V latency between ears) (Normal ≤ 0.5 msec.)
Data Analysis
Data analysis was performed using the Statistical Package for Social Sciences (SPSS 16.0). Paired t-test was used for the inferential analysis. The level of significance was calculated at p value <.05.
Results
In this study, a total of 67 subjects had been enrolled. Their distribution according to age is given below in Table 1 .
Agewise Distribution of the Subjects.
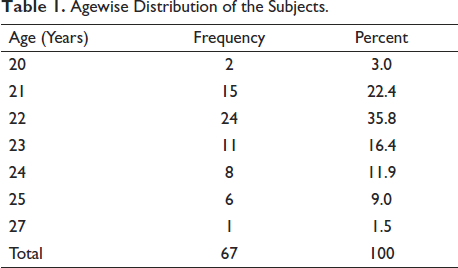
Table 1 showed that age group ranges from 20 to 27 years. Total of 50 (74.6%) subjects were in age group from 21 to 23 years.
Wave latencies of wave I to V, interpeak latencies of I–III, I–V, and III–V and V/I ratios have been given in Tables 2, 3 and 4, respectively.
Waves Latencies.
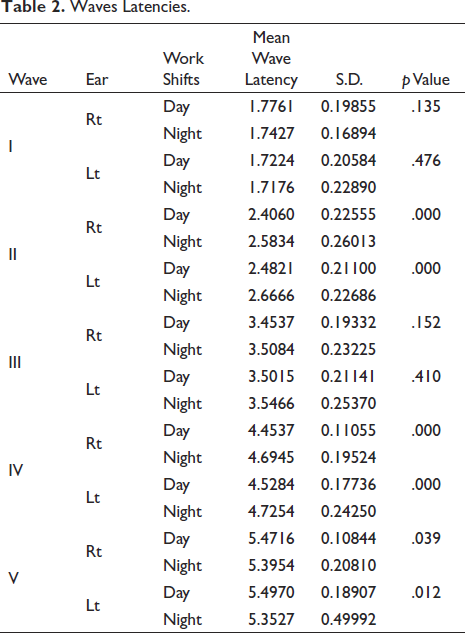
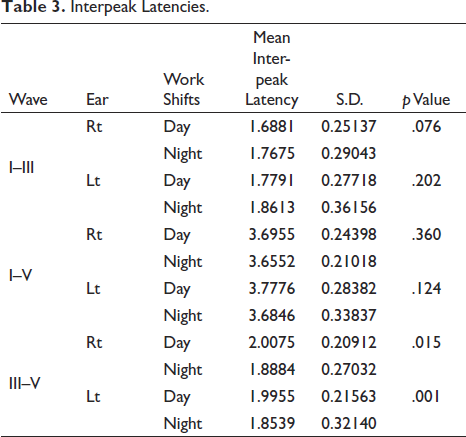
Interpeak Latencies.
V/I Ratio.
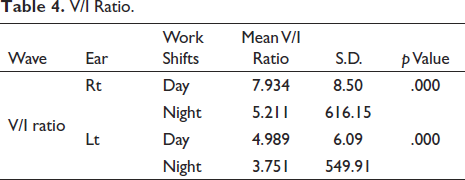
On analysing the data, the paired t-test showed that after night shift of working, significant changes in latencies of wave II (p < .0001), wave IV (p < .0001), wave V (p = .012 & .30), interpeak latency III–V (p = .009 & .003) and V/I ratio (p < .0001) were found for both ears.
Discussion
This study explored the characteristics of Auditory Brain Stem Response in Nursing students who worked during Night shift. Findings from the current study further our knowledge about how night shift affects the latency of wave II, wave IV, and wave V as well as the interpeak latency III–V and V/I ratio in both ears.
The result showed that the mean wave latency in Wave II of day shift was 2.406 ± 0.225 and in night shift was 2.583 ± 0.260 in right ear whereas in left ear the mean wave latency in day shift was 2.482 ± 0.211 and in night shift was 2.666 ± 0.226. The difference in mean wave latency of day and night shift in both ears was found to be highly significant at p < .05.
In Wave IV, the mean wave latency on day shift was 4.453 ± 0.110 and on night shift was 4.694 ± 0.195 in right ear whereas in left ear the mean wave latency on day shift was 4.528 ± 0.177 and on night shift was 4.725 ± 0.242. The difference in day and night shift latency in both ears was found to be highly significant at p < .05.
In wave V also, the difference in mean wave latency in both the shift and in both the ears was found significant among study group.
The findings indicated that there is delayed transmission of auditory pathway after night shift among study group. In other words, the night shift work effects the hearing acuity of the night-shift workers.
One of the studies conducted by Park et al. to find out the relationship between long working hours and hearing impairment in unexposed workers to occupational and environmental noise showed that long working hours have a significant association with hearing impairment in both low and high frequencies among Korean female workers with an exposure-response relationship. The findings of this study support the result of present study as long working hours like in night shift also lead to a level of fatigue which may have affected the auditory acuity among the workers. 7
Another prospective observational study conducted to assess the slowing of sensorimotor and executive function after overnight work among anaesthesia residents showed a similar result. This study involved 30 anaesthesiology residents working day shifts and 30 of their peers working overnight call shifts at the University of Texas Health Science Centre in Houston. The Pro Point and Anti Point tablet-based tasks were used to assess the sensorimotor function. Call residents displayed increased response time across their shifts on both Pro Point (p = .002) and Anti Point (p < .002) tasks, when they were compared to Routine residents. These findings suggest that overnight Call residents showed both sensorimotor and cognitive slowing compared to routine daytime shift residents. 8
The research study by Peelle JE et al. has suggested that impaired hearing ability has a cascading effect on the neural processes which support both perception and cognition. The researchers employed structural MRI images to study the relationship between hearing ability and regional grey matter volume and the results showed a significant correlation between individual differences in hearing capacity and grey matter volume in the auditory cortex. The people with impaired hearing ability had lower grey matter volume in auditory cortex region. So, it was clearly evident from the study that hearing ability has detrimental effects on perception and cognition. 9
The term cognition refers to the internal mental operations that underlie how people perceive, remember, speak, think, make decisions, and solve problems. 10 The deterioration of cognitive performance has serious consequences on working life, especially in carrying out hazardous/safety-sensitive working activities like the work of nurses in health care sector.
In the healthcare setting, a group of 100 nurses engaged in patient care in shift schedule showed poorer scores in general intellectual ability, mental speed, response inhibition, attention, simple reaction time, and working memory tests, after performing a night shift compared to a day shift. Such impairment could be brought on by the qualitative-quantitative alterations of sleep that could affect the frontal and prefrontal cortex executive functions by changing the sleep–wake rhythm. 11 In the same professional group, Esmaily et al. administered different cognitive tests before and after different work shifts and they found that nurse’s working memory and interference scores were significantly reduced at the end of each work shift, though the level of decrease was greater after a night shift than after morning and evening shifts. 12 This implies that night work has a significant effect on cognitive processes.
Age has been shown to affect electrophysiological thresholds, increase latencies and/or reduce wave amplitude in humans and animals.13, 14 So, in the present study nurses within the age group of 20–27 years were considered to avoid age as a confounding factor.
The results of the abovementioned studies are in sharp contrast with those obtained by Chang et al. They assessed cognitive performance of nurses working two, three, and four consecutive night shifts in Taiwan using the State-Trait Anxiety Inventory, Stanford Sleepiness Scale, Wisconsin Card Sorting Test, Taiwan University Attention Test, Digit Symbol Substitution Test, and Symbol Searching Test. The finding of the study was that a greater impairment of perceptual and motor ability was perceived among subjects who worked two consecutive night shifts compared with those who worked four consecutive night shifts. This difference was explained in the light of the participants’ circadian rhythm adaptability. 15 In the present study, the participants of the study were nursing students who had never performed night shift work before. They were afresh with this pattern of shift schedule. The question of night shift adjustments which would have altered the findings was avoided.
Limitations
Firstly, the selection bias was there as we recruited a particular group of hospital health workers and did not include all the cadre of hospital workers who have shift schedules of work.
Secondly, our sample was from young age group. The range was from 20 to 27 and other hospital workers with different age groups were not included in the study.
Thirdly, the hospital workers who were working in night shift for longer periods were also not included in the study.
The findings of this study are reliable as the study was conducted in laboratory settings using BERA technique and factors like age and circadian adaptability were also taken care off. The further study can be done to see the effect of night shift on cognition using P300 for the individual showing changes in hearing ability.
Conclusion
BERA is an objective non-invasive test to evaluate hearing ability by measuring increased latency and interaural latency difference. After night shift there were significant changes in mean latency wave and interpeak latency and V/I ratio of both ears which was highly suggestive of delayed transmission in auditory pathway. Hearing impairment has a cascading effect on cognition which subsequently impacts understanding of speech, problem-solving and decision-making ability which may affect night-shift workers’ daily activities. The hospital administrators are recommended for a better organisation of shift work that takes into consideration the opportunity to reduce night shift working hours and number of consecutive night shift, and ensure adequate relaxation periods between work shifts. This might limit hearing impairment, cognitive impairment, thus contributing to improvement of the psychophysical well-being of health workers and minimise the risk to patient safety.
Footnotes
Acknowledgements
We are thankful to the student nurses for their active participation in the research study. We are also grateful to Professor Vinita Gupta, Professor In charge, College of Nursing for her kind support.
Authors’ Contribution
Author 1: Concept; literature review; clinical studies; Data acquisition and analysis; Manuscript preparation, editing and review.
Author 2: Concept; Literature review; Data acquisition and analysis; Manuscript preparation, editing and review.
Author 3: Clinical studies and data acquisition.
Author 4: Clinical studies and data acquisition.
Author 5: Data analysis.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Statement of Ethics
The study was conducted after seeking approval from the Institutional Ethical Committee (Ethics No. Dean/2018/EC/846).
