Abstract
Background
Obsessive-compulsive disorder (OCD) is considered frequent, unnecessary thoughts that lead to repetitive actions to lessen the apprehension provoked by thoughts; this repetitive sequence may further influence trouble in one’s daily activities. The remedial procedure for OCD includes medication (such as SSRIs, anxiolytics, and antidepressants) with psychotherapy [such as cognitive behavioral therapy (CBT) and exposure response prevention (ERP)]. Previous investigations indicated that regardless of the trend of adopting CBT and ERP to treat OCD, only around half of the patients experienced a full reduction in symptoms.
Purpose
The ERP component in CBT has been termed as a challenging treatment as it contains threatening anxiety-provoking indications, and it has been reflected that between 25–30% of OCD patients reject the ERP treatment, and the refusal and dropout rates for ERP in OCD are higher than other interventions. Thus, in the present investigation, researchers developed a proposed therapy that includes neuropsychoeducation, intrinsic motivation, and metaphoric content integrated with CBT in addition to regular pharmacological management to treat OCD patients and validated the efficacy of the proposed therapy through psychometric ratings (Y-BOCS).
Method
In this pilot study, 10 cases of OCD received a 12-week proposed therapy program. The primary outcome was the Yale-Brown Obsessive-Compulsive Scale (Y-BOCS), which was assessed at baseline and post-treatment.
Results
The present study’s results revealed a significant decrease in scores on the obsessions and compulsions domains and overall total scores on Y-BOCS among OCD patients.
Conclusion
The findings show that this proposed therapy, which includes neuropsychoeducation, intrinsic motivation, and metaphors contents integrated with CBT in combination with pharmacological management, is effective in the treatment of OCD. Therefore, the proposed therapy may be beneficial in the treatment of OCD. It has far-reaching implications in the areas of clinical, psychiatry, and mental health.
Introduction
Obsessive-compulsive disorder (OCD) highlights an example of undesirable thoughts and worries (obsessions) that lead to tiresome ways of behaving (compulsions). These obsessions and compulsions obstruct everyday exercise and are a source of huge trouble. According to the ICD-10 Classification of Mental and Behavioral Disorders, “The essential feature is recurrent obsessional thoughts or compulsive acts. Obsessional thoughts are ideas, images, or impulses that enter the patient’s mind again and again in a stereotyped form. They are almost invariably distressing, and the patient often tries, unsuccessfully, to resist them. They are, however, recognized as his or her own thoughts, even though they are involuntary and often repugnant. Compulsive acts or rituals are stereotyped behaviors that are repeated again and again. They are not inherently enjoyable, nor do they result in the completion of inherently useful tasks. Their function is to prevent some objectively unlikely event, often involving harm to or caused by the patient, which he or she fears might otherwise occur. Usually, this behavior is recognized by the patient as pointless or ineffectual, and repeated attempts are made to resist. Anxiety is almost invariably present. If compulsive acts are resisted, the anxiety gets worse.” As OCD interferes in one’s life and troubles their daily routine, there is a need for an effective treatment that gives relief from these symptoms; if these symptoms are left untreated, they may lead to unfortunate consequences and a poor prognosis. 1 With legitimate treatment, individuals with OCD can recapture command over their lives and feel critical alleviation from their side effects. A review of the literature suggested that two therapies, namely, drug therapy (SSRIs, antidepressants, and anxiolytic) and psychotherapies [such as cognitive behavioral therapy (CBT) and exposure response prevention (ERP)] worked together effectively to treat OCD.2, 3 van der Heiden et al. found that regardless of the remarkable viability of ERP for OCD, with 60% of patients recovering and 25% effectively treated and relieved, the dropout rate was 25%, which is pretty high. 4 In ERP, exposure to disturbing thoughts represents a certain threat, and elevated degrees of emotional arousal and uneasiness might represent high dropouts. 5 In contrast to traditional CBT with ERP therapy, the present investigation aimed to study the proposed psychotherapy, which includes an integrated blend of three components, namely, neuropsychoeducation, 6 intrinsic motivation, and metaphoric contents with CBT (without using direct ERP) in combination with regular pharmacological management to treat OCD patients and validate the efficacy of the proposed therapy through psychometric ratings using the Yale-Brown Obsessive-Compulsive Scale (Y-BOCS).
Methods
Procedure
All the participants in the present investigation were from the NHS hospital in Jalandhar, Punjab. Purposive sampling was done as the participants meeting the inclusion and exclusion criteria were taken into the sample. Scores of patients (pre- and post-intervention) were procured through Y-BOCS. The intervention given to OCD patients has been explained below.
Statistical Analyses
Means, standard deviations, and paired t-tests for within-group comparisons (pre- and post-intervention) were computed to make the comparisons based on the Y-BOCS scores of patients at pre- and post-intervention.
Results
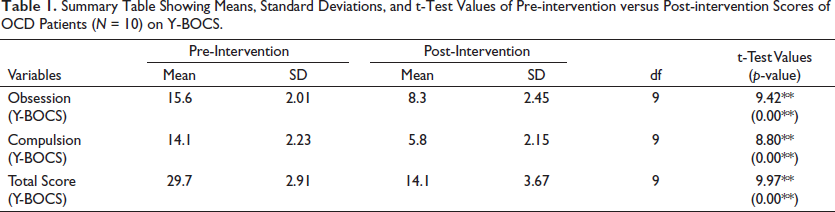
Results of the t-test (Table 1 and Figure 1) revealed that OCD patients showed significantly lesser post-intervention scores on Y-BOCS, namely, obsessions domain (t = 9.42; p < 0.00), compulsions domain (t = 8.80; p < 0.00), and total score on Y-BOCS (t = 9.97; p < 0.00) as compared with their pre-intervention scores without any drop-outs. These findings revealed that OCD patients showed significant improvement after OCD the proposed therapy in combination with pharmacotherapy.
Summary Table Showing Means, Standard Deviations, and t-Test Values of Pre-intervention versus Post-intervention Scores of OCD Patients (N = 10) on Y-BOCS.
Differences Between Means of Pre- and Post-Intervention Scores of OCD Patients (N = 10) on Y-BOCS.
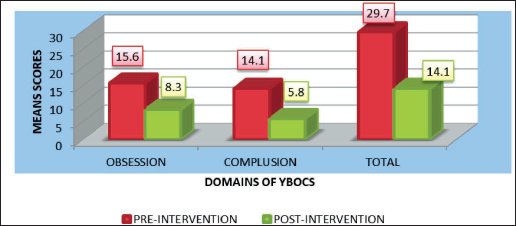
Discussion
In the present investigation, the results of the t-test revealed that OCD patients scored lesser post-intervention as compared to pre-intervention scores on the Y-BOCS rating scale. These findings revealed that the proposed therapy, in combination with regular pharmacotherapy, was well accepted by the clients, as evident by the lack of attrition, and was effective in reducing OCD symptoms among patients in ten sessions. The reason could be that the proposed therapy is based on an established CBT approach, which is itself the gold-standard therapy. The effectiveness of CBT is linked with ERP, which is anxiety-provoking and distressing, and for some patients, it is not suitable, which may lead to high attrition rates during the treatment of OCD. A similar study was conducted by Chasson, 15 on the topic of exposure and response prevention (ERP), discussing that it is an effective intervention for OCD but is often accompanied by significant patient dropouts. This proposed therapy is a blend of neuropsychoeducation, intrinsic motivation, and extensive use of metaphoric content integrated with the basic framework of CBT. Furthermore, the reason could be that the proposed therapy excluded the direct ERP exercises and made patients self-sufficient to ignore their obsessions with intrinsic motivation. In ERP, the stress is mainly on getting exposed and preventing the response in the clinical settings under the direction of a therapist. Whereas the proposed therapy concentrated more on making the client confident enough to ignore the obsessions and restrict compulsive acts on their own. Similar to the constructs of habituation and extinction as explained by ERP in the process of treatment, the proposed therapy also used the same constructs but without clinical setting-based exposure methods. Rather, the clients were empowered by making them knowledgeable about the fundamental theories behind the process of obsessions and compulsions. Furthermore, neuropsychoeducation was delivered to the patients, which made them understand the biological basics of this disorder. At this point, patients could recognize that negative or unwanted thoughts were caused by an imbalance in neurotransmitters or hormones and not by any other factor and that these biological imbalances in the body could be treated with medication. It thus empowered them to tolerate the anxiety and ignore the obsessive thoughts, leading to response prevention. This sense of empowerment intrinsically motivated the clients toward self-directed behavioral changes, which included restricting compulsive acts. Along with intrinsic motivation and neuropsychoeducation, the extensive use of metaphoric language helped patients accomplish difficult goals like learning in the least restrictive way possible, surpassing the opposition, and reaching the unaware. Leeuwerik et al. also reported that a strong emphasis on psychoeducation in ERP might lay the groundwork for subsequent success in performing challenging and anxiety-evoking exposures. 16 Hence, in totality, the integration of these three components, namely, neuropsychoeducation, intrinsic motivation, and metaphoric language, served as a blend in the basic framework of CBT; in every session, they worked together and empowered the client to handle their obsessions and compulsions on their own without the need of excessive external support from the therapist, even during the therapy. To conclude, it can be said that the proposed therapy offers a fair substitute for ERP and shows promising results in overcoming the symptoms of this disorder.
Conclusion
In a nutshell, it can be concluded that neuropsychoeducation equips the clients with an understanding of the basic mechanisms of OCD, which results in increased knowledge and hopes to recover and also reduces fear and myths regarding their suffering. Intrinsic motivation helps the clients regulate their obsessions and compulsions on their own. Metaphoric language leads to easy comprehension of complicated biological and psychological constructs and also makes the treatment procedure pleasant and interesting. The results showed that the proposed therapy is effective in reducing the symptoms of OCD without using many anxiety-provoking techniques. The proposed therapy is based on the principle “Knowledge Is Confidence,” implying that knowledge empowers the person to manage their own issues. Overall, when neuropsychoeducation, intrinsic motivation, and metaphoric language are integrated with CBT, it empowers clients to understand and treat their disorder with their own efforts. Thus, it is suggested that the proposed therapy be named Client Empowerment Therapy (CET).
Limitations
The current study has a few but significant limitations. First, the sample size was small, and the sample population came from a small geographic area; thus, the results could not be generalized to the entire population of OCD patients. To compare the effectiveness of the proposed psychotherapy, a comparative study with another group of samples receiving gold-standard CBT with ERP therapy is required. Also, a follow-up evaluation should have been done after a few months to assess the sustainability of the effect.
Footnotes
Authors’ Contribution
First author: Conception of the study, manuscript preparation, data collection, and analysis.
Second author: Supervision, data analysis, and editing.
Third author: Manuscript preparation and data collection.
Statement of Ethics
Ethical clearance for the study was obtained from the ethics committee of the NHS Hospital, Jalandhar, Punjab. Written informed consent was obtained from all the subjects.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
