Abstract
Background
Stroke is the fourth leading cause of death in India. Data on long-term outcomes of patients with stroke in India are relatively sparse.
Objective
To document survival and long-term functional outcomes of patients with acute stroke and to assess the measures taken for secondary prevention of stroke.
Methods and Material
A five-year retrospective cohort study involving 118 patients with acute stroke was conducted. Details about five years’ survival, functional outcomes (modified Rankin Scale [mRS], Barthel index [BI], and Hamilton Depression Rating Scale [HDRS]), and secondary prevention measures were investigated.
Results
Among the patients, 38.1% were diagnosed with ischemic stroke and 61.8% were diagnosed with hemorrhagic stroke. Hypertension was observed to be the predominant risk factor in a majority of the admitted patients. About 30.5% of patients died in the hospital within zero to four weeks after the index event, while 27.1% died during the follow-up period of five years. Approximately 21.1% of patients experienced a recurrent stroke over the next five years which turned out fatal. The quality of life was seriously affected in 32.4% of survivors. It was seen that 40.5% of survivors were fully independent and 45.9% were able to return to their occupation after five years poststroke. Prevalence of severe and very severe depression was observed in 3.4% and 1.7% of survivors, respectively. The majority of the survivors (93.9%) were aware of the risk of recurrent stroke. Physical activities as measures for the prevention of stroke were undertaken by 60.6% of survivors.
Conclusion
Effective strategies for secondary prevention and also for long-term survival after stroke should be initiated as early as possible after the onset of the initial stroke. Stroke survivors should be closely monitored for their functional recovery and behavioral and emotional improvement poststroke.
Introduction
Stroke, a major noncommunicable disease, is a serious public health problem. Globally, it is the second most common cause of death and the fourth leading cause of disability.1–4 In 2016, a study conducted by the Indian Council of Medical Research (ICMR) entitled “India: Health of the Nationʼs Statesˮ reported that stroke is the fourth leading cause of death and the fifth leading cause of Disability-Adjusted Life Years (DALY) in India. Stroke as such has become a major burden on the health care system of India. Risk factors that are associated with stroke comprise modifiable risk factors that include alcoholism, diabetes, diet, hypertension, lack of physical activity, obesity, and smoking, while age, family history, gender, and race/ethnicity are the nonmodifiable risk factors. 5 Prevention of stroke mainly focuses on the identification and management of these risk factors, use of antiplatelet drugs and/or anticoagulant therapy, and lifestyle modifications. Mostly eating a healthy diet, regular physical exercise, and avoiding smoking and heavy drinking can be the best means to prevent a stroke. In India, major advances have been made in the treatment, care, and rehabilitation of stroke patients over the last few years. There is always a need to have updated long-term data for the proper treatment and rehabilitation of stroke patients. However, such long-term cohort data that describe both survivality and functional outcomes are relatively sparse.
Therefore, this single-centric hospital-based retrospective cohort study was designed to investigate the survivality of patients diagnosed with acute stroke and to document their long-term functional outcomes. The study also focuses on the secondary prevention measures adopted by stroke patients.
Methods
Study Design and Participants
A single-centric retrospective cohort study was performed that involved GNRC super specialty hospital which is situated in Guwahati, Assam, India. Guwahati lies in the northeast region of India and is located at an altitude of 55 m above sea level. GNRC is the first super specialty tertiary health care center in Northeast India. The study included stroke cases that were registered in the year 2005 in GNRC hospital. A total of 572 cases of possible acute stroke were registered. Inclusion criteria were (a) acute ischemic and hemorrhagic stroke patients, (b) patients who were from Guwahati city and resided within a radius of 25 km from the hospital, and (c) only those patients who were admitted to the hospital. The exclusion criteria of the study were (a) patients who were from a radius >25 km from the hospital and (b) patients who were not admitted to the hospital. Thus, 118 stroke patients who were primarily from Guwahati city and admitted to the hospital were considered for a retrospective five years follow-up study. The remaining 454 patients came from a radius of 500 km from the study hospital. It was difficult to contact all these patients and their family members personally because of limited resources, poor connectivity, hostile environment, and invalid contact information, and hence, they were excluded from the study. Ethical clearance for the study was obtained from the ethics committee of the hospital.
Data Collection
Data from the year 2005 registered stroke cases were collected retrospectively. Patients were identified from the Medical Records Department (MRD) of the hospital. Medical records of all the 118 stroke patients from MRD were reviewed to retrieve baseline information that included sociodemographics and comorbidities. The sociodemographics of patients that were considered included age, gender, smoking, and alcohol habit. Information about comorbidities such as hypertension, diabetes mellitus, hyperlipidemia, and elevated serum uric acid levels was retrieved from MRD. Duration of hospital stay and time of death for the patients who died in hospital were also extracted. Communication addresses and contact numbers of the patients were collected from MRD. A pro forma that included patient demography, clinical parameters, any disabilities, activities of daily living (ADL), presence/absence of depression, and secondary prevention measures was predesigned. At five years poststroke, the survivors were interrogated individually based on the structured pro forma. To ascertain the time and possible cause of death in the case of deceased patients, the primary caregivers were directly consulted.
Functional Outcome
Data on the functional status of patients were assessed using the modified Rankin Scale (mRS).6, 7 The mRS is a widely used 6-point disability scale to measure the degree of disability in patients who were diagnosed previously with a stroke. A score of 0 indicated the patient had no symptoms, while a score of 1 indicated that the patient despite symptoms had no significant disability and was able to carry out all activities without any assistance. Patient with mild disability and unable to carry out all previous activities but able to look after themself without any assistance was given a score of 2. Moderate disability in a patient who required some help but was otherwise able to walk on their own was scored as 3. A score of 4 implied that the patient had a moderately severe disability and was unable to walk and attend to bodily functions without assistance. A patient with severe disability, who was bedridden and required continuous care was given a score of 5, while a patient who had expired was scored 6. The Barthel index (BI) was used to evaluate the ability of patients to perform different ADLs following discharge from the hospital.8–10 Ten variables that included the presence or absence of fecal and urinary incontinence, grooming, toilet use, feeding, transfer, mobility, dressing, climbing chairs, and bathing were scored. Each item was then rated and given a score that ranged from 0 (totally dependent), 5 (major help), 10 (minor help), and 15 (independent). The sum of all the points for each of the items gave the final score. The presence or absence and severity of depression in patients and their recovery following hospital discharge were measured using the Hamilton Depression Rating Scale (HDRS).11, 12 The scale consisted of 17 items and each item was scored on a 3-point or a 5-point Likert scale. A score of 0–7 was considered to be normal; 8–13, mild; 14–18, moderate; 19–22, severe; and >23 indicated very severe depression. Evaluation parameters as measures of secondary prevention of stroke that included lifestyle modifications, control of risk factors, use of antiplatelet drugs, and anticoagulant therapy were recorded.
Statistical Analysis
All statistical analyses were performed using SPSS software version 17 (SPSS Inc., Chicago, IL, USA). 13 Multivariate regression analysis was performed to determine the effect of age, gender, and stroke type on the survival of the stroke patients. Data on the category-wise responses in the predesigned pro forma were either represented as frequency and percentage or assigned scores following the mRS, BI, or HDRS rating system.
Results
Baseline Characteristics
Table 1 describes the baseline attributes of the 118 patients involved in the study. The cohort included 28% (n = 33) females and 72% (n = 85) males. The mean age of the cohort was 64 ± 12.9. In 2005, 38.1% (n = 45) admitted patients had ischemic stroke and 61.9% (n = 73) had hemorrhagic strokes. Hypertension was found to be the predominant associated risk factor in 83.9% (n = 99) followed by diabetes mellitus in 32.2% (n = 38) of patients. Smoking and alcohol consumption also contributed significantly in prevalence of stroke in 11.9% (n = 14) and 13.6% (n = 16) of patients respectively. Elevated levels of blood cholesterol or fats (lipids) also known as hyperlipidemia was observed only in 1.7% (n = 2) of patients. At least 0.85% (n = 1) had elevated serum uric acid levels. About 70.3% (n = 83) were admitted for one week and only 0.85% (n = 1) had a hospital stay of more than six weeks.
Baseline Attributes of Stroke Patients Included in This Study.

Five Years Survival Analysis
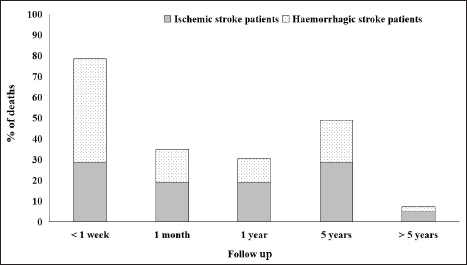
During the five years follow-up, it was found that 57.6% (n = 68) of patients died, among them, 30.5% (n = 36) died at the hospital and the rest 27.1% (n = 32) died at home. Stroke/stroke-related complications was the probable cause of death in 76.5% (n = 52), while 5.8% (n = 4) died because of myocardial infarction. Miscellaneous or unrelated causes accounted for 10.3% (n = 7) deaths and cause of death for 7.4% (n = 5) could not be determined. As shown in Figure 1, 28.6% of the ischemic stroke patients expired within a week after stroke, 19.0% within a month, 19.0% within a year, 28.6% within five years, and 4.8% expired after five years. Whereas 50% of the hemorrhagic stroke patients expired within a week after stroke, 15.9% within a month, 11.4% within a year, 20.5% within five years, and 2.3% expired after five years. The cumulative five years survival rate was found to be 34% among females (37%) showing slightly better survival than males (33%). Patients with >70 years of age showed decreased survival (31%) as compared to those whose age was <70 years (35%). Survival of ischemic stroke patients (45%) was higher than hemorrhagic stroke patients (27%). However, on multivariate analysis, factors such as age, gender, and stroke type were not significantly associated with the survival rate as seen in Table 2.
Five Years Follow-Up of Death Rates in Ischemic and Hemorrhagic Stroke Patients.
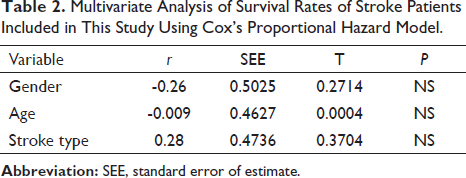
Multivariate Analysis of Survival Rates of Stroke Patients Included in This Study Using Cox’s Proportional Hazard Model.
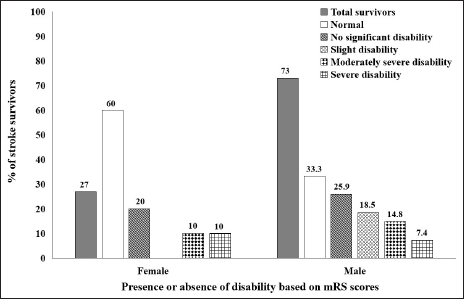
Five Years of Functional Outcomes
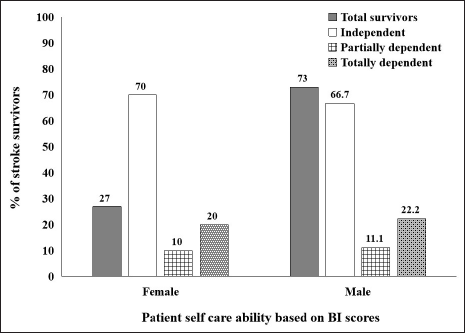
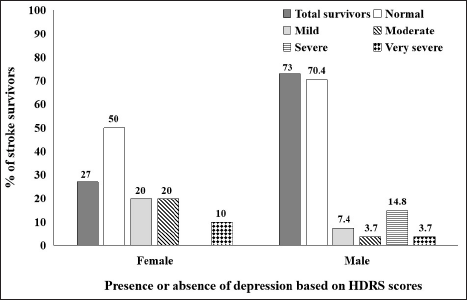
Among the survivors (n = 50), information could not be retrieved for seven patients, two patients moved out of Guwahati, and four patients did not give satisfactory responses during the study. Therefore, the total number of survivors who participated in the follow-up study was 37. Among them 73% (n = 27) were in a fully conscious state, 18.9% (n = 7) exhibited stroke-related disabilities, and 8.1% (n = 3) were found to be bedridden at the five years follow-up study. Further from the mRS scores, 40.5% (n = 15) survivors were fully independent, 24.3% (n = 9) showed no significant disabilities despite symptoms, 13.5% (n = 5) had mild disabilities but did not require any assistance, 13.5% (n = 5) had moderate disabilities and required assistance, and 8.1% (n = 3) showed severe disabilities and was totally bedridden (Figure 2). The BI scores for the presence of different social activities are shown in Figure 3. It describes the proportion of those survivors who participate in various ADLs after five years poststroke. Patient self-care ability based on BI scores revealed that 10.8% (n = 4) and 21.6% (n = 8) survivors were partially and completely dependent on their primary caregivers, respectively (Figure 4). Interestingly, 45.9% (n = 17) survivors could completely resume their occupation as before the occurrence of a stroke, while 43.2% (n = 16) were unable to resume their previous occupation and 10.8% (n = 4) could partly go back to their occupation. The presence of poststroke pain and its effect on normal living is of considerable concern in stroke recovery. About 51.5% (n = 17) of survivors complained of having poststroke pain and it was found to be more common among males (70.6%) than females (29.4%) and it was also found prevalent in survivors whose age was more than 70 years. The prevalence of poststroke depression was evaluated using HDRS scores. Very severe depression was found in 1.7% (n = 2) survivors, while 18.9% (n = 7) survivors exhibited moderate to severe depression. About 10.8% (n = 4) survivors reported mild depressive symptoms and 64.9% (n = 24) were normal with no depressive thoughts (Figure 5). Thus, 39.4% (n = 13) of survivors were found to have intermittent to persistent depressive thoughts, were emotionally unstable, and showed signs of social withdrawal.
Modified Rankin Scale (mRS) Based Disability in Stroke Survivors.
Proportion of Stroke Survivors Regularly Carrying Out Social Activities.
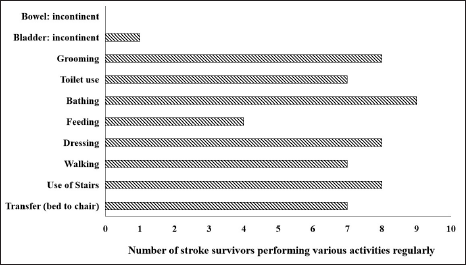
Barthel’s Index (BI) Based Self-Care Ability in Stroke Survivors.
Hamilton Depression Rating Scale (HDRS) Based Depression in Stroke Survivors.
Prevention Measures
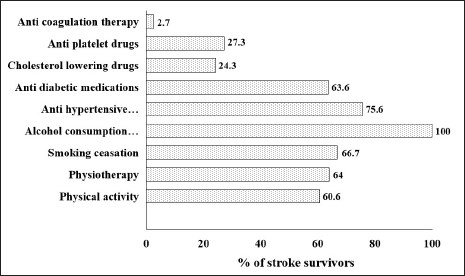
Among the survivors, 93.9% (n = 31) took adequate steps as a measure for secondary prevention of another stroke. During the follow-up it was seen that 54% (n = 20) regularly underwent physical activities, while 27.3% (n = 9) occasionally carried out some forms of physical exercises. At the time of discharge from the hospital, 67.6% (n = 25) were advised physiotherapy of which only 64% (n = 16) regularly followed it, 32% (n = 8) practiced occasionally, and 4% (n = 1) completely discontinued. About 8.1% (n = 3) had a history of smoking during hospital admission. Among them 66.7% (n = 2) had quit smoking, while 33.3% (n = 1) still continued. Alcoholism was seen in 18.9% (n = 7) patients at the time of hospital admission. However, the five years follow-up revealed that all the survivors gave up on liquor consumption. A history of hypertension was seen in 81.1% (n = 30) and among them 90% (n = 27) were still on antihypertensive medications, 10% (n = 3) discontinued, while 3.3% (n = 1) latterly started on antihypertensives poststroke. Diabetes mellitus was reported in 29.7% (n = 11) and 72.7% (n = 8) were advised medicines at the time of discharge. Only 62.5% (n = 5) continued medications, 37.5% (n = 3) discontinued, and 28.6% (n = 2) started medications for controlling diabetes mellitus poststroke. During discharge time, 18.9% (n = 7) were advised medicines for controlling cholesterol, and among them, 57.1% (n = 4) continued, 42.8% (n = 3) quit medicines, while 13.5% (n = 5) freshly started taking medicines for cholesterol control poststroke. Only 27.3% (n = 9) were taking antiplatelet drugs out of which 44.4% (n = 4) were on aspirin, 33.3% (n = 3) on clopidogrel, and 22.2% (n = 2) took both aspirin and clopidogrel. One of the survivor (2.7%) reported of having cardioembiolic stroke and was on anticoagulant therapy. An overall secondary prevention measures adopted by the stroke patients during the follow-up study is described in Figure 6.
Secondary Prevention Measures Followed by Stroke Survivors.
Discussion
To our knowledge, this is the first study from Northeast India that examined the long-term significance of stroke including survival, functional, and emotional outcomes. In the year 2005, 118 patients from Guwahati were admitted to the hospital with acute stroke. At the baseline, the majority of the admitted patients belonged to the 40 to 79 age group and more males were affected by acute stroke than females. Hemorrhagic stroke was found to be more common among admitted patients. Various studies have reported that both hypertension and diabetes mellitus are prognostic risk factors for stroke.14–17 Hypertension is well known to be the most predominant modifiable risk factor for people with stroke. 14 The likelihood of having a stroke and high death rates increases 1.5 to 3 fold in people who are already diagnosed with long-term chronic diabetes. 14 In our study, hypertension and diabetes mellitus were also found to be the two risk factors associated with a majority of stroke patients. Smoking and alcohol consumption were found to be the other two risk factors. Many studies have also reported that both smoking and heavy drinking are independent risk factors for stroke.18–22 Heavy drinking increases the risk for all subtypes of stroke including intracerebral hemorrhage (ICH) and subarachnoid hemorrhage (SAH). 18 Weakened or impaired metabolism and hypertension induced by alcohol are responsible for ICH in people with heavy alcohol consumption. 18 Whereas the risk for SAH because of occasional alcohol intake significantly increases as episodic drinking causes a sudden increase in the blood pressure which results in aneurysm or bleeding in the cerebral arteries. 18
During the follow-up of five years, 68.6% of death cases were reported. Thus, only about 31.3% of the patients could survive at least five years after stroke. The overall cumulative survival rate in this study was found to be 34% for all types of stroke. Immediate mortality was seen in the first seven days after the initial event of index stroke with stroke itself being the underlying cause of death in most of the cases. Within zero to four weeks after the initial onset, 52.9% of the patients died at the hospital and 47% of the patients died at home during the four weeks to five years follow-up duration. Long-term survival for females was found to be slightly better than that for males. Also, the survival rates for patients with <70 years of age were marginally higher than the >70 years age group. Also, the ischemic patients showed somewhat superior long-term survival as compared to the hemorrhagic patients. Other studies have found that the long-term survival of stroke patients is in general shorter than those without any history of stroke. 23
This study showed that a few of the survivors had some levels of physical disabilities and were in residential care. Although the majority of the patients were fully independent, some were dependent on their caregivers. Because of the restricted lifestyle, the majority of the survivors and also their carers reportedly showed constant emotional difficulties. In this study, we have also observed that the stroke survivors reported having depressive thoughts, emotional disturbances, and feelings of social isolation. The survivors likely suffered from substantial emotional strain even after five years poststroke. Thus, proper care for the mental well-being of stroke survivors is of utmost importance and should be taken into consideration during the rehabilitation program.
Prevention of stroke primarily focuses on either reducing the risk factors that increase the likelihood of having a stroke or reducing the chances of developing any of the risk factors associated with stroke. In this study, the majority of the stroke survivors were aware of the risk of recurrent stroke and adhered to strict secondary prevention measures. Physical activities and physiotherapy were regularly practiced. Blood pressure and blood sugar were also regularly monitored. The findings on the consumption of antihypertensive, antidiabetic, cholesterol-lowering medications; antiplatelet drugs; and cessation of smoking and alcohol consumption were reassuring and supported the fact that the stroke survivors were taking adequate measures for the prevention of the disease.
In India, awareness of the warning symptoms of stroke among the general population is far from satisfactory. This lack of awareness leads to a delay in receiving medical advice from physicians and a delay in hospitalization, which are setbacks for providing the necessary treatment. From the study, it is clear that even though functional improvement and mental well-being are seen in many of the survivors, however, a few still faced consistent functional and emotional challenges even five years after stroke. The limitation of the study includes the small size of the sample. In general, the data were collected retrospectively. Because of a lack of information and published data on long-term follow-up of stroke in Northeast India, there is a frequent need for such kinds of studies. In the near future, GNRC Hospitals aims to take a holistic approach to conduct the same.
Conclusion
This retrospective cohort study showed that after the index stroke, death rates were significantly high during the first few days. In subsequent years, deaths because of stroke or stroke-related complications were on the rise. Although many survivors could function on their own, a few of them showed severe functional dependency and major emotional disturbances after stroke. Appropriate care, advice, and support for stroke survivors are therefore important.
Footnotes
Authors’ Contribution
MN contributed to study concept and design; data acquisition, analysis, and interpretation; statistical analysis; and literature overview and discussion. RD contributed to study concept and design; data interpretation; critical revision of the manuscript; and provided scientific guidance. ARB contributed to data analysis and interpretation; critical revision of the manuscript; and provided scientific guidance. PD contributed to study design; data analysis and interpretation; and provided scientific guidance. ApB contributed to statistical analysis; literature review; discussion; and critical revision of the manuscript. NB contributed to study concept and design; data acquisition, analysis, and interpretation; critical review of the manuscript; and provided scientific guidance and supervision. NC contributed to data acquisition, data analysis, and interpretation; statistical analysis; and critical revision of the manuscript. AB contributed to study design; data analysis and interpretation; statistical analysis; and literature review and discussion.
Statement of Ethics
Ethical clearance for the study was obtained from the ethics committee of GNRC Hospitals, Assam.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
