Abstract
Intracranial saccular (berry) aneurysms often remain asymptomatic until rupture, posing considerable diagnostic and medico-legal challenges when sudden death occurs outside healthcare facilities. We report the case of a 30-year-old female police officer who collapsed suddenly at home, with a history of occupational stress and recurrent headaches. Autopsy revealed diffuse subarachnoid hemorrhage, a 0.8 cm saccular aneurysm on the left posterior communicating artery, and a collapsed aneurysmal sac with multiple rupture sites on the left anterior communicating artery, with approximately 200 g of intracranial blood and cerebral edema. The findings confirmed a fatal aneurysmal rupture. Neither toxicological analysis nor histopathological examination was undertaken in this case, and other organs were unremarkable. This case underscores the risk of sudden death from multiple aneurysms in young adults and highlights the medico-legal significance of missed sentinel symptoms, emphasizing the necessity of timely neuroimaging in at-risk individuals.
Keywords
Introduction
Saccular aneurysms constitute the majority of intracranial aneurysms and typically manifest only upon rupture, resulting in subarachnoid hemorrhage (SAH) with high mortality.1–3 Although their prevalence in the general population is low, multiple aneurysms are reported in a significant minority of cases, particularly among females. 1 The present case is noteworthy for the coexistence of multiple aneurysms in a young adult, with acute occupational stress serving as a possible temporal trigger preceding sudden collapse. This raises important pathogenetic and medico-legal considerations concerning asymptomatic disease and unexpected death in the community. The case also highlights that recurrent headaches may represent sentinel events preceding rupture, and failure to investigate such warning symptoms may have legal implications when sudden death ensues. Previous medico-legal studies published in the Journal of Indian Academy of Forensic Medicine have also reported patterns of sudden unexpected natural deaths, including cases involving intracranial hemorrhage and neurovascular pathology.4, 5
Case History
On September 27, 2024, the body of a 30-year-old married female police officer was brought to the mortuary of our institute with an alleged history of sudden, unexpected death of unknown cause. The deceased had no known comorbidities or history of substance abuse and was reportedly carrying out her routine activities until the terminal event. She had a history of recurrent headaches for which she had consulted general practitioners. From the evening of September 25, 2024, until late night on September 26, 2024, she remained continuously on duty. After returning home and having dinner around 11:30
Autopsy Findings
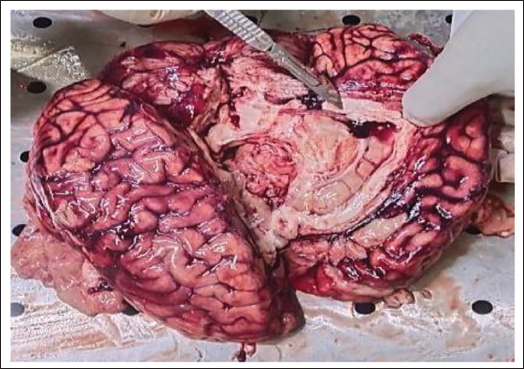
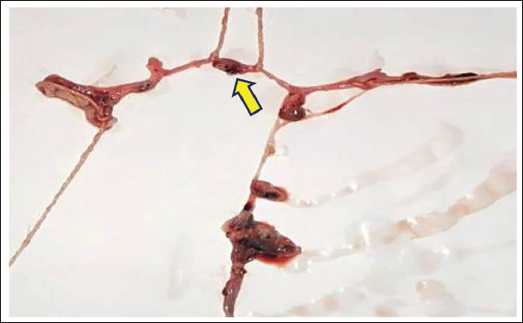
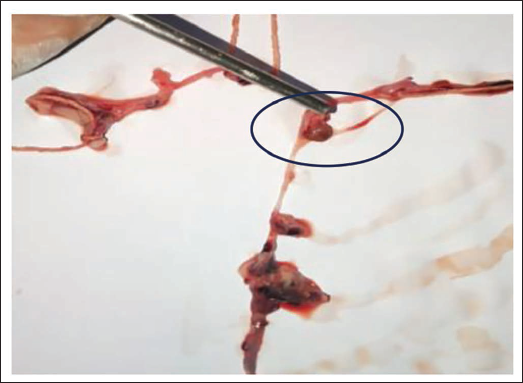
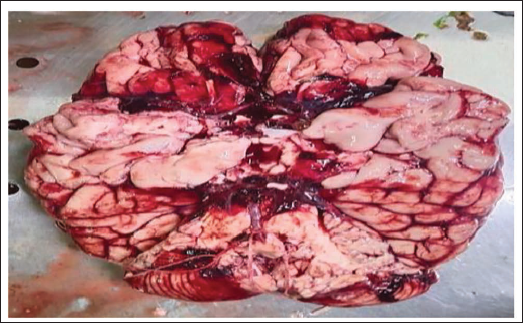
The eyes and mouth were closed; the corneas were hazy; the tongue was inside; and the nostrils were clear. The extremities were straight with semi-open fists; rigor mortis was present throughout the body; and hypostasis was fixed over the back. Faint cyanosis was noted on the ear lobules and nose. A petechial hemorrhage (1.0 × 0.5 cm) was observed on the mid-left upper eyelid. Multiple old, healed hesitation cut marks were noted on the left wrist, consistent with remote self-harm, without active inflammation or fresh hemorrhage. Petechial hemorrhages were present on both parietal scalp regions; the skull and neck vertebrae were intact and healthy; and the meninges were tense. SAH was present over the cerebrum and cerebellum, with clotted and fluid blood in the posterior aspect of the lateral ventricles (Figure 1). A collapsed saccule with multiple bleeding points was found on the left anterior communicating artery (Figure 2). A 0.8 cm saccule was present on the left posterior communicating artery near its junction with the left middle cerebral artery (Figure 3). The base of the brain showed ruptured arterial branches and ecchymosis, mainly laterally; the brain was congested and edematous (Figure 4). The cranial cavity contained approximately 200 g of fluid and clotted blood. Pinkish froth was present in the trachea. The heart weighed 247 g with grossly patent coronaries. The other internal organs were grossly normal and congested, and the stomach contained yellowish, pasty material with normal mucosa. Neither toxicological analysis nor histopathological examination was undertaken.
Discussion
Death in this case was due to cardiorespiratory failure consequent to rupture of an intracranial saccular aneurysm with diffuse SAH, in the presence of multiple aneurysms. Although the heart was anatomically normal, systemic hypertension cannot be fully excluded.
The mean age of incidence of intracranial saccular aneurysms is approximately 50 years. 1 Rupture leading to sudden death in the third decade of life is uncommon and poses diagnostic challenges because of its often silent antecedent course.
Common sites of intracranial saccular aneurysms include the anterior communicating artery, posterior communicating artery, internal carotid artery, middle cerebral artery, and basilar artery bifurcation. 6 These findings correspond with the observations in the present case.
The pathogenesis of intracranial aneurysms is multifactorial. Hemodynamic stress and associated inflammatory responses cause maladaptive vascular remodeling, which weakens the arterial wall and predisposes it to aneurysm formation. 7 Risk factors include female sex, smoking, hypertension, and genetic predisposition.1, 6, 8, 9 Multiplicity of aneurysms is frequently associated with a familial component, 8 although such a history was unavailable in this case. While a genetic contribution remains possible, it cannot be confirmed in the absence of specific genetic or syndromic markers.
The presence of aneurysms in the anterior and posterior communicating segments of the circle of Willis in the present case is consistent with observations reported by Koutsothanasis GA et al. 1
Psychological or physical stress has been shown to precipitate aneurysmal rupture by transiently increasing transmural pressure and wall stress in predisposed vessels.10–12 In this case, prolonged duty, occupational stress, and a thunderclap headache preceding collapse strongly suggest that acute stress may have acted as a precipitating trigger. This finding aligns with the work of Cooke DL et al., 10 Hoyer C et al., 11 and Müller-Forell W and Bohl J, 12 who described associations between psychiatric comorbidity, stress, and cerebrovascular events.
Healed hesitation cuts were observed over the left wrist, consistent with a prior episode of self-harm. They showed no evidence of recent hemorrhage or vital reaction and had no causal relationship with the terminal event. Although unrelated to death certification, documentation of such findings is essential for comprehensive medico-legal evaluation and may provide insight into psychosocial background, particularly in cases where psychiatric comorbidity may influence cerebrovascular vulnerability. Similar associations between psychiatric conditions and cerebrovascular events have been reported by Cooke DL et al. 10 and Hoyer C et al. 11
No gross autopsy findings or circumstantial evidence suggested ingestion of any toxic substance; therefore, viscera were not preserved for chemical analysis. The coronary arteries were patent on gross examination, and the heart, as well as other visceral organs, appeared normal and healthy. Consequently, tissues were not retained for histopathological examination to avoid unwarranted use of laboratory resources in the absence of specific diagnostic indications.
This case demonstrates that fatal rupture of previously silent intracranial aneurysms can occur even in young adults, an age group considerably below the mean incidence of approximately fifty years reported in population studies. 1 The aneurysms in this patient involved the anterior and posterior communicating arteries, the sites most frequently described in published literature, 6 and their coexistence supports the established role of hemodynamic stress and inflammatory remodeling in aneurysm formation. 7 The presence of multiple aneurysms further indicates a potential genetic or familial predisposition. 8 Although no hereditary disorder was identified in this case, previous studies have shown that inherited conditions such as autosomal dominant polycystic kidney disease are associated with an increased risk of intracranial aneurysm formation. 13 From a medico-legal perspective, these findings underscore the importance of promptly recognizing sentinel headaches and ensuring appropriate neuroimaging in symptomatic individuals. Furthermore, therapeutic experiences reported by Mitsuhashi et al. 14 emphasize that early identification and timely management of posterior communicating artery aneurysms are vital to prevent catastrophic rupture.
Conclusion
Fatal rupture of undiagnosed intracranial aneurysms reinforces the necessity for heightened clinical vigilance in individuals presenting with unexplained or recurrent headaches. Early recognition of such warning symptoms and appropriate diagnostic evaluation are essential to prevent missed diagnoses and potential allegations of medical negligence. It further underscores the necessity of meticulous autopsy examination and accurate death certification to ensure precise determination of the cause of death and to uphold the integrity of medico-legal adjudication.
Footnotes
Authors’ Contribution
All authors have contributed to this manuscript.
Availability of Data and Materials
Data sharing are not applicable.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable as a Medico-legal autopsy does not require consent.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Authors declare consent for publication.
