Abstract
Nasal bone fractures are among the most prevalent indications for referral to forensic medicine centers for examination and certification. The objective of this study was to ascertain the frequency of diagnostic discrepancies in nasal bone fractures between public hospitals and forensic medicine experts in East Tehran zfrom 2018 to 2019. In this prospective quantitative study, 200 patients referred to the East Tehran Forensic Medicine Center in 2018 were selected based on available files. A survey was conducted to assess the frequency of unconfirmed nasal fracture diagnoses from public hospitals. These diagnoses were then analyzed in conjunction with the opinions of forensic experts. The results indicated that fractures were not confirmed in 59 patients (29.5%), suggesting a substantial discrepancy (p < .05). The underlying causes for non-confirmation included an initial diagnosis that was either incorrect or missing (55.9%), the presence of old fractures (35.6%), and post-rhinoplasty conditions (8.5%). The study’s findings indicate that approximately one-third of nasal bone fracture diagnoses from public hospitals were not in accordance with the evaluations of forensic experts. The primary etiologies of these discrepancies were identified as diagnostic errors, pre-existing fractures, and post-surgical alterations. To address these concerns, it is advisable to place greater emphasis on the following: (a) the utilization of early and precise radiographic imaging, (b) comprehensive clinical documentation, and (c) the prompt referral of patients to forensic centers for expert evaluation.
Introduction
Nasal bone fractures represent the most prevalent type of facial fracture, often resulting from sports-related accidents, physical altercations, and other forms of trauma. 1 Although often regarded as inconsequential, an accurate diagnosis is imperative for two primary reasons. First, it serves as a crucial guide for determining the most suitable clinical management approach. Second, it plays a pivotal role in medico-legal contexts, ensuring the appropriate handling of medical cases in legal proceedings.2, 3 In numerous legal jurisdictions, the corroboration of a fracture by a forensic expert is a prerequisite for legal claims, compensation, and criminal prosecution.
The forensic significance of the nasal and midfacial anatomy is well-established, as structures such as the nasal septum and frontal sinus exhibit unique morphological patterns that can aid in human identification in forensic investigations, a fact highlighted in studies published in the Journal of Indian Academy of Forensic Medicine. Furthermore, the resilience of structures like the maxillary sinus, which often remains intact despite severe trauma to the skull, underscores their critical value as stable anthropological markers for identity verification in complex cases.4, 5
However, a significant challenge arises from discrepancies between initial diagnoses made in emergency departments or public hospitals and the subsequent evaluations conducted by forensic medicine specialists.6, 7 These diagnostic inconsistencies can lead to serious consequences, including unjust legal outcomes, loss of public trust in the healthcare system, and the financial burden of unwarranted claims on insurance and judicial systems. This phenomenon has garnered significant attention within the domain of medico-legal systems on a global scale, extending to regions such as India and the Middle East.
Despite the global recognition of this problem, there is a paucity of robust data quantifying the frequency and causes of these discrepancies, particularly in the Iranian context. A review of the extant literature reveals a prevalence of two notable limitations. First, the sample sizes of existing studies are often inadequate, and second, the majority of these studies are designed in a manner that is limited to a single center. Therefore, the specific research gap pertains to the absence of concrete, evidence-based analyses of mismatch rates and their etiologies in our region.1, 3, 6, 7
The present study aims to address this gap by investigating the frequency of non-confirmation of nasal bone fracture diagnoses initially made in public hospitals by forensic experts in East Tehran. In addition, a thorough analysis of the underlying causes of these discrepancies is conducted. The results of this prospective study will provide valuable insights to help minimize misdiagnosis, improve referral practices, and enhance the reliability of medico-legal certifications.
Materials and Methods
This prospective quantitative study was conducted at the East Tehran Forensic Medicine Center from 2018 to 2019.
The study population comprised all individuals who were referred to the center for medico-legal assessment of suspected nasal bone fractures during the study period.
The inclusion criteria for the study were as follows: The patient must have been referred from a public hospital in East Tehran with an initial diagnosis of acute nasal bone fracture. The patient must be at least 18 years of age and must have complete medical and forensic records. The following criteria were used to determine exclusion from the study: The presence of other major facial fractures that could complicate the assessment is the first consideration.
Second, referral from private clinics or other cities is to be taken into account.
Finally, the availability or completeness of radiographic images must be ascertained. Due to the specific and consecutive nature of the referrals during the study period, a convenience sampling method was employed. The annual caseload was used to calculate the sample size, which was determined to be 200 participants, with a margin of error of approximately 7% and a 95% confidence level. This size was deemed sufficient for the study’s objectives.
Data Collection and Diagnostic Confirmation
The data were collected using a structured form to record demographic information, mechanism of injury, medical history (including previous fractures, rhinoplasty, or nasal deviation), time intervals between trauma and assessments, and clinical findings.
Diagnostic Confirmation Protocol
The definitive diagnosis (confirmation or non-confirmation of an acute nasal bone fracture) was made by two senior forensic medicine specialists. The diagnosis was based on a standardized protocol:
Physical Examination: The specialists assessed the patient for objective signs of acute trauma, including crepitation, deformity, swelling, and bruising over the nasal bridge, as well as periorbital ecchymosis (raccoon eyes).
Imaging Review: All available imaging (nasal bone radiographs and, if available, computed tomography (CT) scans) was reviewed. The experts looked for definitive radiographic evidence of an acute fracture, carefully distinguishing it from signs of old healed fractures or post-surgical changes (e.g., from previous rhinoplasty).
A case was categorized as “confirmed” only if both specialists agreed on the presence of an acute fracture based on a combination of positive clinical and radiographic findings. Cases where the initial diagnosis could not be verified based on these objective criteria were categorized as “unconfirmed.”
Data Analysis
Data analysis was performed using SPSS software version 24. Descriptive statistics are presented as mean ± standard deviation for quantitative variables and frequency (percentage) for qualitative variables. The Chi-square test was used to compare categorical variables. A p value of less than .05 was considered statistically significant.
Results
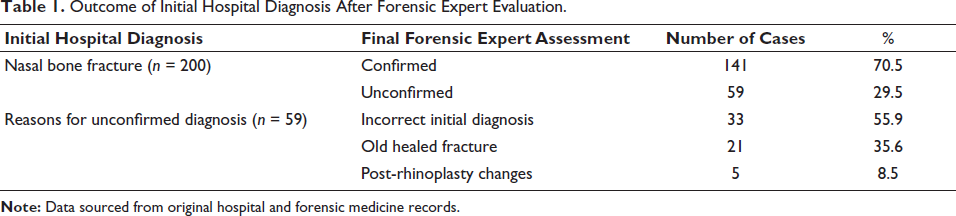
A total of 200 cases with an initial diagnosis of nasal bone fracture from public hospitals were referred for forensic evaluation. As demonstrated in Table 1, the forensic experts corroborated the diagnosis in 141 cases (70.5%), yet did not substantiate it in 59 cases (29.5%), thereby unveiling a substantial discrepancy rate of 29.5%.
Outcome of Initial Hospital Diagnosis After Forensic Expert Evaluation.

The demographic factors examined (see Table 2) demonstrated that age, gender, and education level were not significantly associated with fracture confirmation (p > .05). However, a significant association was identified with occupation (p = .019). The largest group with unconfirmed fractures was the self-employed individuals, which may be related to specific work-related risks or motivations for seeking certification.
Association Between Demographic Characteristics and Fracture Confirmation by Forensic Experts.
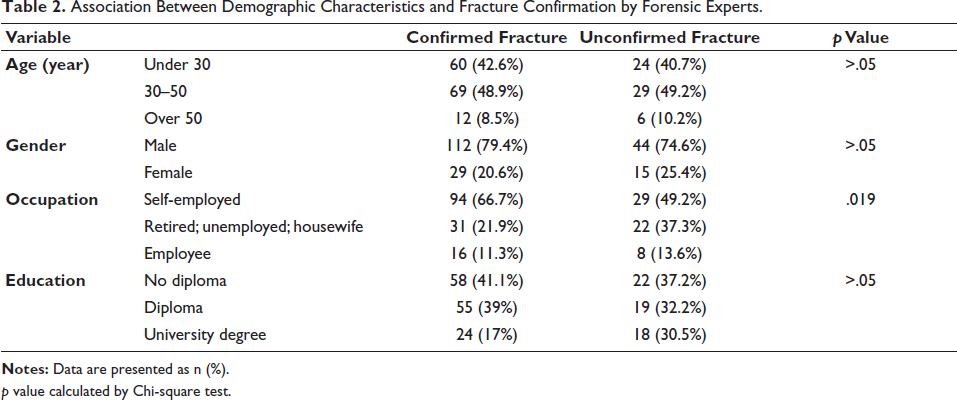
p value calculated by Chi-square test.
Analysis of clinical history factors showed that a prior history of nasal fracture or rhinoplasty was not significantly associated with the current fracture confirmation status (p > .05 for both). A clear difference was observed in symptom presentation: 22.0% of unconfirmed cases were asymptomatic, compared to only 8.5% of confirmed cases. The distribution of reported symptoms (swelling, nosebleeds, bruising) is presented descriptively in Table 3; however, as patients could present with more than one symptom, formal statistical comparison for individual symptoms is not appropriate.”
Clinical History Factors and Fracture Confirmation.
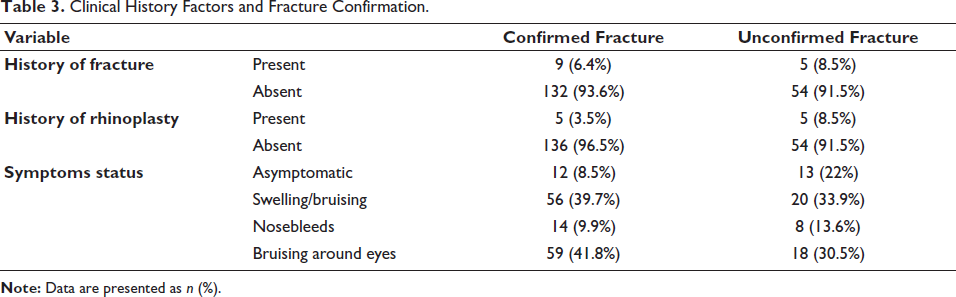
As demonstrated in Table 4, neither the mechanism of injury nor the primary method used for the initial diagnosis exhibited a significant relationship with the final confirmation outcome (p > .05).
Association of Injury Mechanism and Diagnostic Method with Fracture Confirmation.
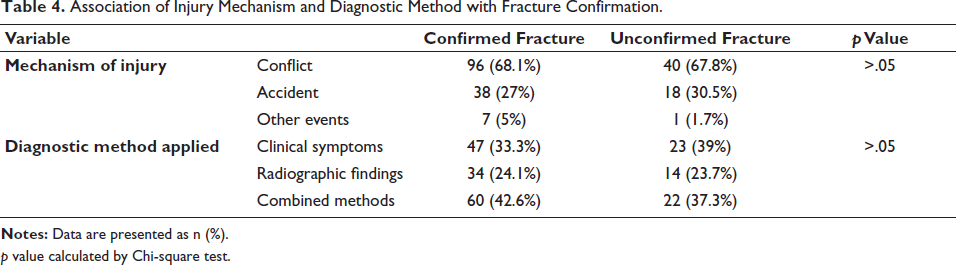
p value calculated by Chi-square test.
The predominant reasons for forensic non-confirmation included incorrect interpretation of imaging or symptoms (55.9%) and the failure to distinguish acute trauma from pre-existing conditions such as old fractures (35.6%) or post-surgical changes (8.5%).
This synthesis delineates a clear target for intervention, namely the enhancement of diagnostic accuracy. This enhancement is contingent upon the implementation of heightened scrutiny for specific patient profiles and a more critical evaluation of imaging to rule out old injuries.
Discussion
The primary objective of this study was to investigate the critical issue of diagnostic discrepancies in nasal bone fractures between public hospitals and forensic medicine experts. This is a problem with profound medico-legal consequences. The findings indicate that 29.5% of initial diagnoses were not corroborated by forensic experts, thereby underscoring a substantial gap in the accuracy of injury documentation. This documentation is fundamental to legal claims, compensation awards, and criminal justice outcomes.
The underlying causes of non-confirmation, namely an inaccurate diagnosis (55.9%), the presence of old fractures (35.6%), and post-rhinoplasty alterations (8.5%), underscore specific domains that necessitate intervention. The high rate of incorrect diagnoses indicates a necessity for enhanced training in acute fracture recognition for emergency physicians. This issue has also been identified in studies focusing on initial clinical assessments.8, 9 The prevalence of old fractures being misclassified as acute cases is a well-documented pitfall in forensic practice. This phenomenon underscores the indispensable role of a detailed patient history and the forensic expert’s ability to distinguish radiographic signs of healing. This is an area where specialized training is crucial.9, 10 A thorough understanding of the normal morphological variations of the nasal bone, including differences related to sex, is fundamental for accurately identifying pathological fractures. For instance, a study in the Journal of Indian Academy of Forensic Medicine highlighted significant differences in pyramidal angle and linear distance of the nasal bone between genders using CT imaging, underscoring the detailed anatomical knowledge required for precise forensic assessment. 11 These discrepancies are not merely clinical errors; they directly impact the judicial process. Unconfirmed claims may signify either honest diagnostic errors or, in a subset of cases, potential attempts to seek unwarranted compensation. This is a challenge that medico-legal systems face globally.12, 13
A particularly intriguing finding of our study is the significant association between occupation and fracture confirmation status (*p* = .019), with self-employed individuals showing a higher rate of unconfirmed fractures. The present socio-demographic variable has the potential to be associated with the motivations individuals have for seeking certification. One such motivation may be the necessity of documentation to support claims for financial compensation. This factor has the capacity to influence the manner in which patients present themselves and the information they provide in their histories.12, 13 This finding moves the discussion beyond pure diagnostic accuracy and into the complex interplay between socio-economic factors and the medico-legal system.
Furthermore, the markedly elevated incidence of unconfirmed fractures in asymptomatic patients (*p* = .044) offers a compelling clinical-forensic correlation. The absence of acute signs, such as swelling or bruising, upon physical examination serves as a significant indication that the initial diagnosis may be inaccurate or that the alleged acute injury is not recent. This finding is consistent with established forensic principles that prioritize objective clinical findings, a standard practice in expert evaluation.8, 9, 14
Our results strongly resonate with the work of Sener et al., 15 who found that overdiagnosis of nasal fractures (24.5%) was far more common than missed diagnoses (1.9%). This pattern suggests that a major component of the discrepancy problem is not a failure to detect fractures, but a tendency to label soft tissue injuries or old changes as acute fractures, particularly when examinations are conducted without specialist consultation and rely solely on plain radiography.
While the overall discrepancy rate in our setting appears higher than that reported in some studies, 9 it is consistent with the known variability in diagnostic accuracy across different contexts.12, 14 This variation can be attributed to differences in study settings, the experience level of the initial diagnosticians, and the specific protocols used by forensic centers. For instance, the diagnostic accuracy can be influenced by the imaging modality used. In our study, a majority of initial assessments included CT scans, yet discrepancies persisted. This underscores that while advanced imaging is crucial, as seen in the study by Hosukler et al. 16 where 76.5% of cases had CT scans, its interpretation by non-specialists remains a vulnerability. The consistent theme across all studies, including ours, is that a reliance solely on the initial hospital diagnosis without expert forensic verification is prone to error, potentially leading to significant legal and financial repercussions. 13
The practical implications of our findings are threefold. First, the high rate of misdiagnosis underscores the necessity for advanced training in the interpretation of nasal radiographs for emergency physicians, particularly to differentiate acute fractures from old or post-rhinoplasty changes. This is critically important as general practitioners and emergency physicians have been shown to have a significantly higher tendency to overdiagnose non-depressed fractures. Second, it is imperative to exercise caution when diagnosing fractures in asymptomatic patients, and to promptly refer them for forensic evaluation when necessary. Third, clinicians should consider socio-demographic factors, such as occupation, which may influence motivations for filing claims. They should maintain objective and meticulous documentation in doing so. Ultimately, as concluded by Hosukler et al., the most reliable solution may be for the final forensic report in cases of nasal trauma to be issued by a Forensic Medicine Specialist, who can integrate clinical, radiological, and contextual findings into a holistic and objective assessment. The implementation of these measures has the potential to mitigate diagnostic discrepancies.
A limitation concerns the analysis of symptoms. As clinical signs were recorded as non-exclusive categories, it was not statistically valid to compare them directly using a single Chi-square test. Unfortunately, the original dataset is no longer available to permit a re-analysis using mutually exclusive categories or individual binary variables. Therefore, the symptom analysis is presented descriptively, and the primary robust finding is the significant difference in confirmation rates between asymptomatic and symptomatic patients.
Recommendations and Conclusion
To address these discrepancies, a multifaceted approach is proposed: Enhanced Training: It is imperative that emergency physicians partake in obligatory workshops that focus on the acute and chronic radiographic characteristics of nasal fractures. Standardized Protocols: The development of clear guidelines for when to suspect an old injury or a post-surgical state and when referral to a forensic specialist is warranted or is essential. Forensic Vigilance: The present study offers evidence to assist forensic practitioners in recognizing the potential impact of socio-demographic factors, including occupation, on the legitimacy of claims.
In summary, the present study advances beyond the mere quantification of diagnostic error to underscore its substantial medico-legal ramifications. A discrepancy rate of nearly one-third calls into question the reliability of initial diagnoses for legal purposes. By identifying incorrect diagnoses as the primary cause and examining the roles of asymptomatic presentations and occupational status, a roadmap is provided for improving diagnostic accuracy and safeguarding the integrity of the medico-legal process. This roadmap is based on evidence.
Footnotes
Data Availability Statement
Data will be available upon request from the corresponding author.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This study will be conducted in accordance with the ethical principles of the Declaration of Helsinki. The study protocol was reviewed by the Ethics Committee of the Forensic Medicine Organization and approved with the code (IR.LMO.REC.1398.002). Patient information will remain confidential and will only be accessible to the research tea.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from all individual participants included in the study.
