Abstract
With the growing senior citizen population, crimes such as elder abuse are on the rise. In India, individuals over 60 years are considered senior citizens. Medico-legal challenges stem from under-reporting and the overlap of abuse-related injuries with natural aging processes. A literature review explored elder abuse, forensic markers, legal frameworks, and case studies shaping protective laws in India and globally. Elder abuse includes physical, emotional, and sexual abuse, neglect, and psychological harm. Identifying abuse-related trauma, such as spiral fractures or injuries to the head, face, or neck, is crucial. Due to limited literature and under-reporting, circumstantial evidence plays a significant role in legal proceedings. Research on forensic markers can help in clinical detection, while a multidisciplinary approach, involving geriatricians, forensic experts, dermatologists, and odontologists, ensures a comprehensive assessment. Strengthening guidelines and raising awareness will enhance the identification and management of elder abuse cases.
Introduction
India’s aging population is rapidly increasing, creating unique healthcare, social, and medico-legal challenges, with elder abuse remaining under-recognized and under-reported.1, 2
The term “granny battering,” coined by G. R. Burston in 1975, was a significant early attempt to highlight the hidden problem of elder mistreatment within domestic settings. Despite increasing recognition, elder abuse remains grossly under-reported due to factors such as emotional dependence on caregivers, cognitive impairments, fear of abandonment, and lack of accessible reporting mechanisms. 3 It is defined as “a single or repeated act, or lack of appropriate action, occurring within any relationship where there is an expectation of trust, which causes harm, or distress to an older person.” 4
Elder abuse in India remains a significantly under-recognized medico-legal problem with major forensic implications. Most cases go unreported due to dependence on caregivers and misinterpretation of inflicted injuries as age-related changes. The absence of standardized medico-legal proformas, limited forensic training for healthcare professionals, and a lack of a forensic databank hinder accurate identification. Inadequate autopsies often label suspicious deaths as “natural,” while minimal research and case law obscure the forensic differentiation between senile degeneration and trauma from assault. There are no standardized medico-legal proformas for elder abuse comparable to those for child abuse or sexual assault, and healthcare providers receive limited training in recognizing suspicious injury patterns in older adults. Injury markers unique to elder abuse are poorly studied in the Indian setting, and there is no forensic databank to help distinguish between natural senile changes (such as osteoporosis-related fractures or senile purpura) and trauma caused by assault.5–7
The doctor’s role in both clinical and post-mortem settings is critically important. Recognition, diagnosis, treatment, and ongoing follow-up are essential. Elder abuse should always be considered as a differential diagnosis rather than being overlooked. Physicians are responsible for reporting suspected cases to the police. Medico-legal examinations must be conducted with the same rigor as any other case, and any abnormalities should be meticulously documented with relevant photographs or diagrams. In cases of uncertainty, consultation with senior colleagues is recommended. Common obstacles to reporting include concerns about missing a treatable condition, fear of damaging family relationships, potential breaches of confidentiality, and doubts regarding the benefits of reporting.1, 2, 7–12
Highlighting and addressing this gap is essential to enhance the accuracy of forensic assessments, ensure proper legal redressal, and ultimately protect one of the most vulnerable sections of society.
Methodology
This systematic review discusses the literature on forensic markers of elderly abuse.
The research questions in our study were
Are there forensic markers of elderly abuse? When should an alarm be raised for elderly abuse, as signs overlap between signs of aging and abuse?
Search Strategy
A systematic review was conducted following the PRISMA guidelines, using electronic databases such as PubMed, Google Scholar, government websites, and elderly non governmental organisations (NGOs) such as HelpAge India and Annapurna Yojna, up to 2023. Textbooks on forensic and geriatric medicine were also referenced. Keywords included: Offenses against the elderly, age criteria, promulgation of guidelines, pioneers of guidelines globally and locally, and relevant case studies. The study was done over a year in 2023. This review included studies that specifically investigated elder abuse, including its types and associated forensic markers. Eligible sources encompassed original research articles, book chapters, theses, dissertations, systematic reviews, literature reviews, meta-analyses, and conference papers reporting primary research findings. Only publications available in English and published up to and including 2023 were considered. Studies were excluded if they did not focus on elder abuse or its forensic markers, or if they were not available in English.
The quality of the included studies was independently assessed by the first two authors using the Critical Appraisal Skills Program checklists. Differences in opinion between the authors were resolved by consensus.
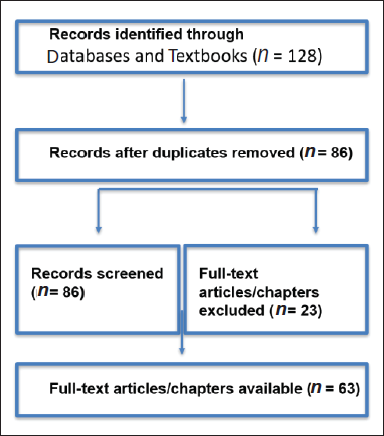
The extracted data included authors, titles, the type of abuse reported to be prevalent, forensic markers, and other markers. The data extraction was implemented by two researchers and was checked for accuracy by a third researcher. This is summarized in Figure 1.
PRISMA Flowchart of the Records Identified and Screened.
Discussion
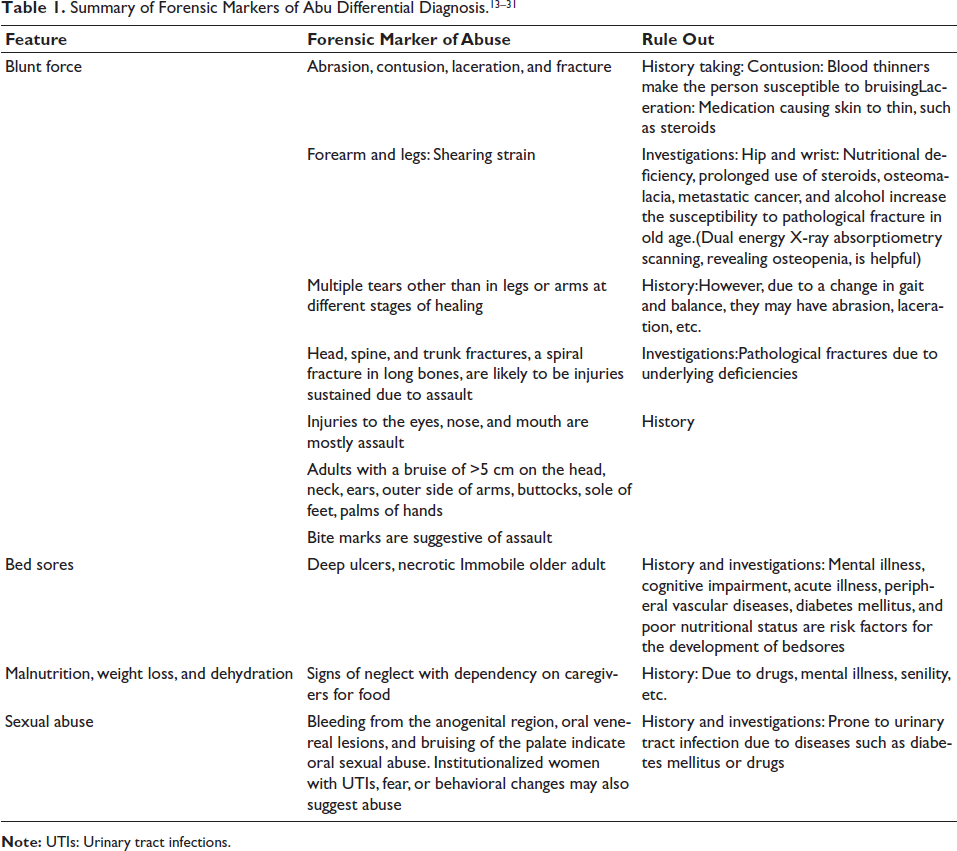
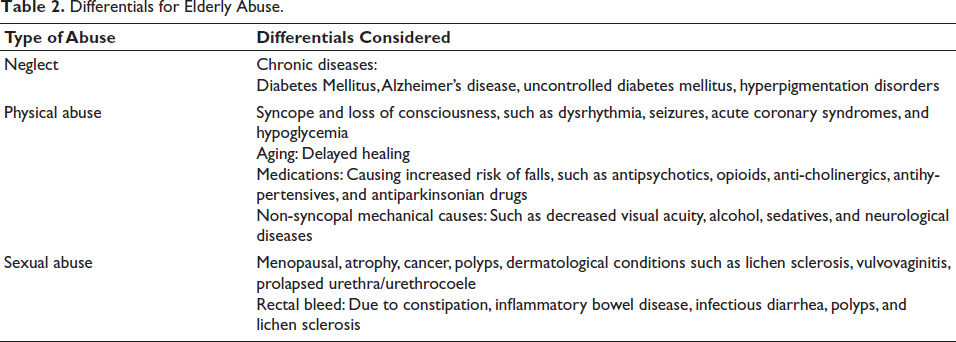
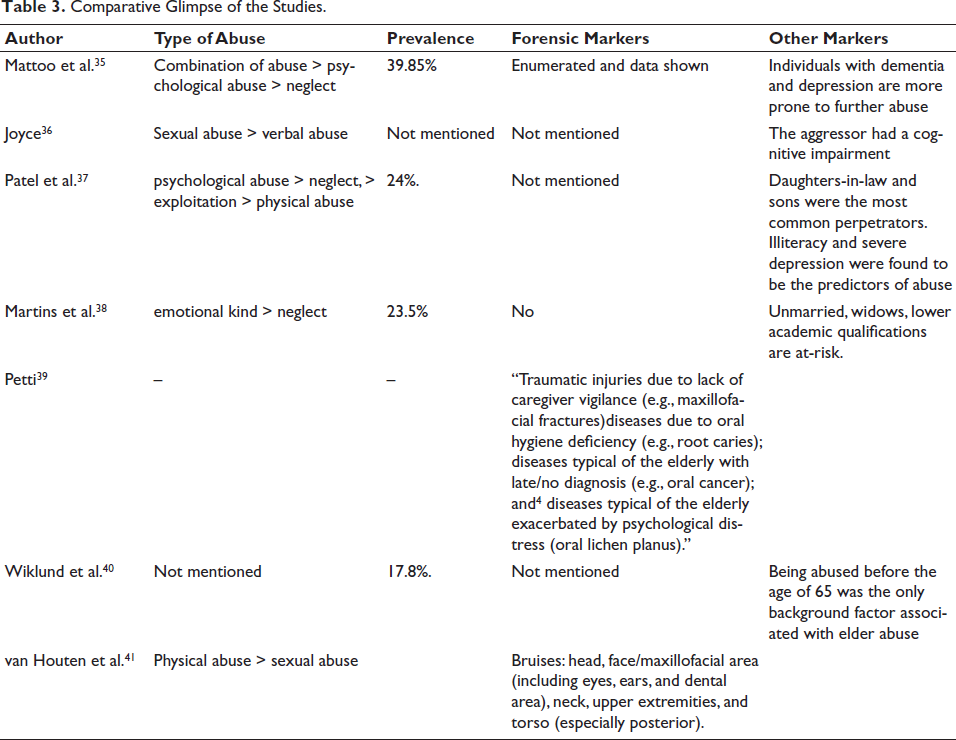
Elderly individuals may exhibit signs of abuse such as weight loss, dehydration, injuries, and behavioral changes, leading to malnutrition and depression.12, 13 Abuse includes physical harm, neglect, and sexual exploitation. Recognizing subtle signs is crucial for accurate diagnosis and identifying forensic markers of abuse.13–31 A comparative of features of elderly abuse are as depicted in Table 1 with differentials enlisted in Table 2. Comparative glimpse of the studies are mentioned in Table 3.
Differentials for Elderly Abuse.
Comparative Glimpse of the Studies.
Blunt Force Injury and Old Age
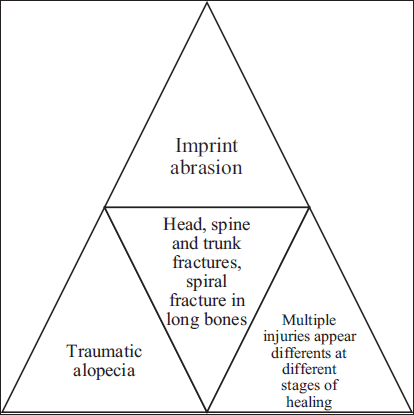
Aging skin is prone to abrasions, contusions, and lacerations. Malnutrition, steroid use, and bed rest increase fracture risk. Medico-legal implications include documenting imprint abrasions, multiple tears, traumatic alopecia, and spiral fractures, which may suggest physical abuse or neglect.14–16 The features are as depicted in Figure 2.
Markers of Physical Abuse in the Elderly.
Bedsores
Bedsores result from interrupted blood flow, with risk factors such as cognitive impairment, diabetes, and poor nutrition. Preventive strategies include repositioning and nutrition. Deep bedsores and necrotic ulcers may indicate neglect due to poor hygiene.17–19
Malnutrition
Dental issues, medications, and impaired cognition in older adults lead to weight loss and nutritional deficiencies, suggesting neglect.14, 15, 21
Dehydration
Hydration status in older adults is hard to assess. Confusion, somnolence, weight changes, or vital fluctuations may indicate neglect.14, 20, 21
Bone fractures by radiological exams, coagulation profile, liver tests, and bone densitometry help evaluate fractures and neglect signs. 22
Negligence
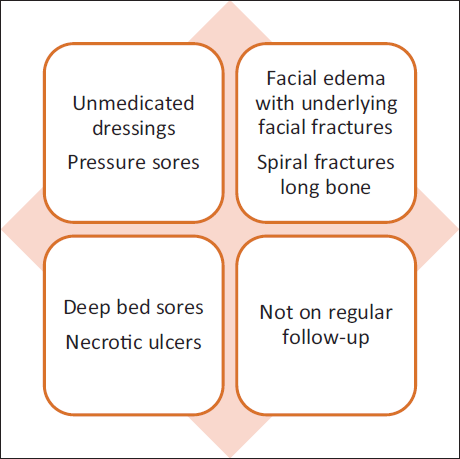
Inadequate care in elderly patients, such as untreated wounds and pressure sores, raises suspicion of negligence.23, 24 The features are as depicted in Figure 3.
Markers of Neglect in the Elderly.
Sexual Abuse
Sexual abuse includes non-consensual contact. Anogenital bleeding, oral lesions, and recurrent urinary tract infections (UTIs) in elderly women suggest possible abuse or victimization. 25
Elders often hesitate to report abuse, blaming themselves and choosing silence. In clinical settings, the Hwalek–Sengstock Elder Abuse Screening Test assesses psychological factors. The Conflict Tactics Scale is modified for elders, while the Vulnerability to Abuse Screening Scale helps identify at-risk individuals, aiding early detection and intervention. 27
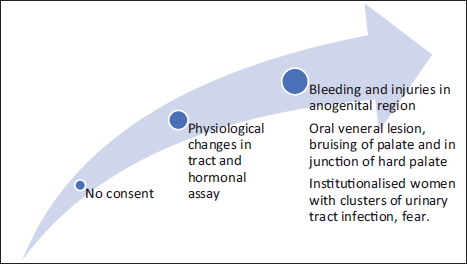
Physicians are legally obligated to report suspected elder abuse under the Married Women Protection Act, Indian Penal Code Criminal Procedure Code Sec. 44, and CrPC Sec. 125; however, under-reporting persists, often due to fear, uncertainty, and limited awareness. The medico-legal challenges in proving abuse are significant: Age-related physiological changes, delayed disclosure, and incomplete documentation can obscure trauma or mimic injury, complicating both clinical assessment and legal proceedings. While an autopsy can reveal critical evidence—such as malnutrition, pressure ulcers, untreated injuries, and fractures inconsistent with history—the interpretation of findings requires careful consideration to distinguish neglect or abuse from natural age-related conditions.11, 26–28, 31–34 The features are as depicted in Figure 4.
Markers and Reasons of Sexual Abuse in the Elderly.
Structured screening tools such as the Hwalek–Sengstock Elder Abuse Screening Test, Elder Abuse Suspicion Index, and Vulnerability to Abuse Screening Scale show promise in enhancing early detection, systematic documentation, and generation of legally admissible evidence. Yet, their routine implementation remains limited, raising questions about feasibility, clinician training, and integration into workflow.
Post-mortem examinations offer important insights into abuse-related deaths, but reliance on autopsy alone is insufficient. Forensic evaluation—including nutritional assessment, examination of skin and soft tissue injuries, skeletal analysis, and toxicology—must be interpreted alongside clinical history, caregiver interviews, and comorbidity profiles. Even then, distinguishing neglect from natural deterioration is often ambiguous, highlighting the need for rigorous standards and multi-disciplinary input.
Forensic markers—unexplained bruises, fractures, burns, rope marks in varying stages of healing, unusual pressure ulcers, and behavioral changes—provide important clues, yet overlap with age-related or iatrogenic changes, complicating interpretation. Effective detection requires pattern recognition, comprehensive assessment, and consistent professional training. Critically, delayed reporting not only worsens patient outcomes but also undermines the legal process, emphasizing that meticulous documentation and early intervention are as essential as the forensic findings themselves.
Conclusion
Elderly abuse is under-researched and under-reported, forcing authorities to rely on circumstantial evidence. Research on forensic markers aids healthcare professionals in identifying abuse. A multidisciplinary approach, including geriatricians, forensic experts, dermatologists, and odontologists, is crucial for accurate evaluations, considering aging-related changes that may obscure abuse signs.
Recommendations
Further studies are needed to amend laws, mandate reporting of elder deaths in care homes, and develop evidence-based screening tools for abuse.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Not applicable.