Abstract
Rodenticides or ‘rat poisons’ are mixture of compounds to eradicate rodents. They are the most toxic compounds with various chemical compositions, mechanisms of action, toxic doses and lethal effects. Coumarins, aluminium phosphide, zinc phosphide and yellow phosphorous are the commonly used rodenticides for deliberate self-harm (DSH). The use of pesticides as agents of deliberate self-poisoning (DSP) is on the rise, with more than 500,000 cases reported worldwide annually. The National Poison Information Centre (NPIC) is a round-the-clock telephone service meant for the dissemination of information regarding the symptoms and management of various poisonings. It is managed by the Department of Pharmacology at the All India Institute of Medical Sciences. In a retrospective study, data over 13 years were analysed from the NPIC. Of 14,867 cases reported to the NPIC, 17.06% were due to rodenticides. Rats are the most destructive pests damaging crops and for preventing these pests, rodenticides are commonly used in agricultural sector and homes. In the absence of a definite antidote, mortality in patients with rodenticide consumption is high. The rapid action, easy availability and high toxicity for the target species at an economic deal have made this compound an ideal agent with misuse for suicidal poisoning. This case series presents four cases of rat poisoning admitted to a tertiary health care hospital which helped us in identifying the clinical features of certain rat poisons and diagnosing the rat poison by means of poison detection centre and which will help the treating physician to reduce the mortality in future.
Introduction
Rodenticides, commonly referred to as ‘rat poisons’, are chemical agents aimed at eliminating small rodents. The common targets for their use are household rodents, that is, rats/mice, squirrels and gophers. Controlling rodents is imperative as they are vectors for the spread of disease, destroy crops/grains and multiply rapidly. In India, being a primarily agrarian country, rodenticides are widely used and also commonly available in almost every household, to prevent their stored grains from rodents. They are available in various formulations, such as powders, pastes, pellets, cereal baits or blocks. 1 Since it is easily available and cheaper than other pesticides in the market, it is often taken with suicidal intent or ingested accidentally by children. 2
Deliberate self‑harm (DSH) is a problem that is increasing in prevalence with time. Since the ancient times to the postmodern era, people have deliberately tried and at many instances succeeded in taking their own life. The population is varied and not restricted to any socioeconomic class of people. Various methods of DSH are used across the world with rodenticides being one of the most common methods used in the Indian subcontinent. 3 The global burden of rodenticide poisoning varies from region to region. In the United States, as per the American Association of Poison Control Centres, rodenticides accounted for 0.3% of 2.3 million human exposures as reported to the regional poison control centres. There are no definite data from Asia describing the prevalence of the various rodenticide poisonings. However, the National Poison Information Centre (NPIC) is a round-the-clock telephone service meant for dissemination of information regarding the symptoms and management of various poisonings. It is managed by the Department of Pharmacology at the All India Institute of Medical Sciences (AIIMS). In a retrospective study, data over 13 years were analysed from the NPIC. Of 14,867 cases reported to the NPIC, 17.06% were due to rodenticides. 1
Rodenticides are of following common types—anticoagulants, metal phosphides (aluminium phosphide, zinc phosphide) and yellow phosphorus. Other types include calciferols, barium carbonate and alpha-naphthylthiourea (ANTU). Each one of them has different methods of action. Hence, they have different toxicological profiles with variable fatality rates in humans when consumed by accident or intentionally. 3 As a result, the toxidrome produced by one rodenticide is largely different from that produced by another rodenticide. In addition, there is also a vast difference in the immediate and long‑term outcomes based on the type of rodenticide consumed. 1 Since almost every system is affected in rodenticide poisoning and also there in no definite treatment guidelines available, we have taken up this study to identify the specific clinical features, and course and to diagnose the poisoning using 1,2-dichloropropane (PDC) as soon as possible to start the specific treatment.
Materials and Methods
We present a case series of four patients, consecutively admitted to the medical ward with rat poisoning in a tertiary care hospital over a period of six months from May 2023 to November 2023. After obtaining approval from the institutional ethical committee and written informed consent of patients’ relatives, the case records of patients with rodenticide poisoning were retrieved from the medical records department. The diagnosis was made from the patient’s clinical signs and symptoms, local examination, investigations like laboratory parameters and most importantly from PDC as well as history from patient bystanders. Treatment histories from other hospitals were obtained from reference letters. After the death of the patient, we have involved the findings of post-mortem examinations, histopathology and Regional Forensic Science Laboratory (RFSL) report.
Results
There was a total of four patients who were admitted with rodenticide poisoning during the one-year study period. The age of the patients ranged between 20 and 30 years of age and the gender of all four patients was female. Among four cases, case 1, 2 and 3 were referred from other hospitals. The intent for ingestion of rodenticide in all four cases was suicide and we were able to find the exact quantity of ingested rodenticide only in two cases based on the history. Soon after the ingestion, patients developed gastrointestinal symptoms like nausea, vomiting and diarrhoea. Despite treatment like Ryle’s tube aspiration and other non-specific treatments since there is no specific antidote available, patients progressed to hepatic, renal and pulmonary dysfunction.
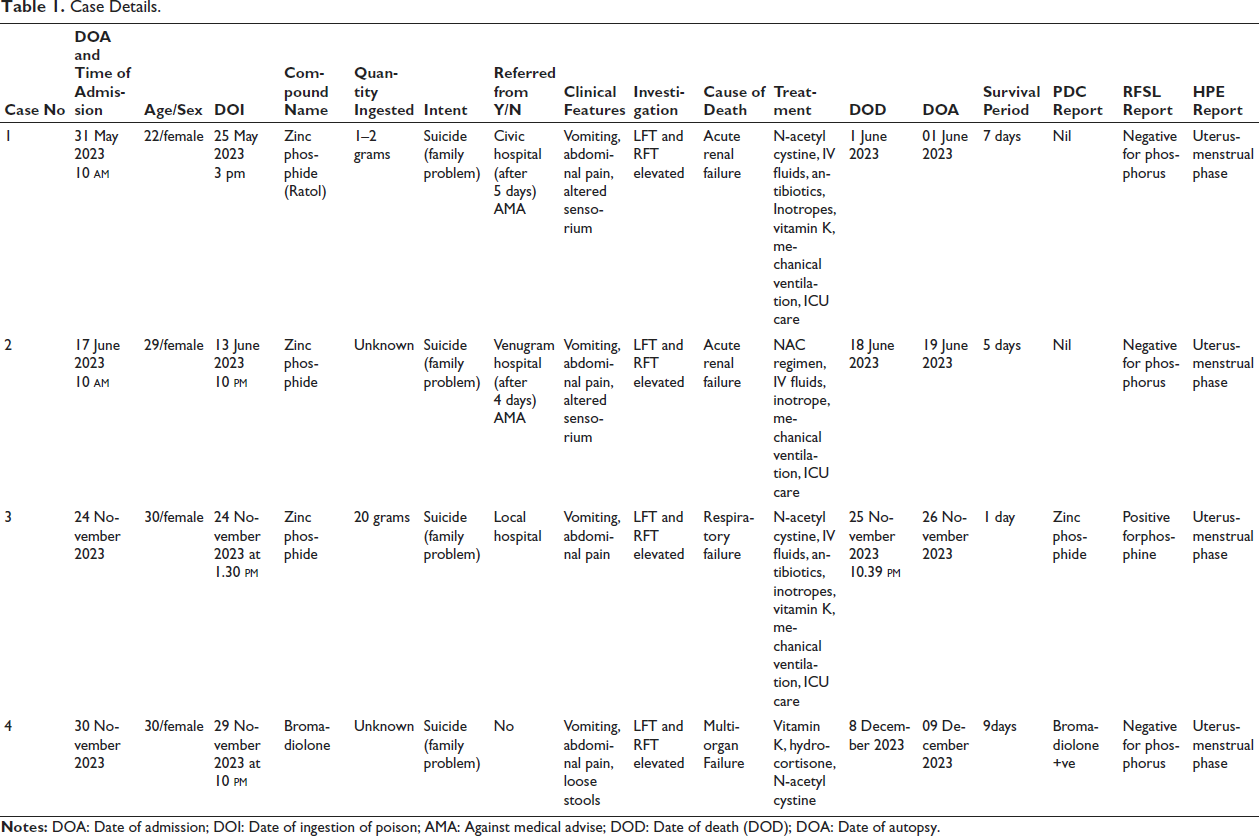
Based on the PDC reports, case 4 consumed a rodenticide called bromadiolone and case 1, 2 and 3 had consumed zinc phosphide. Investigations were undertaken and all the cases had raised liver function test (LFT), renal function test (RFT) levels suggesting multiorgan dysfunction with severe hypoglycaemia and metabolic acidosis. Treatments like N-acetyl cysteine regimen, vitamin K, sodium bicarbonate and other supportive care and treatment were given according to patient’s symptoms. Cases 1 and 2 ended up with acute renal failure, case 3 with respiratory failure and case 4 with multiorgan dysfunction. All the four cases expired despite the required treatment. The survival period of these patients ranged from 24 hours to 9 days (Table 1 and Figure 1).
Case Details.
Distribution of Types of Poisons, Dosage, and the Survival Days.
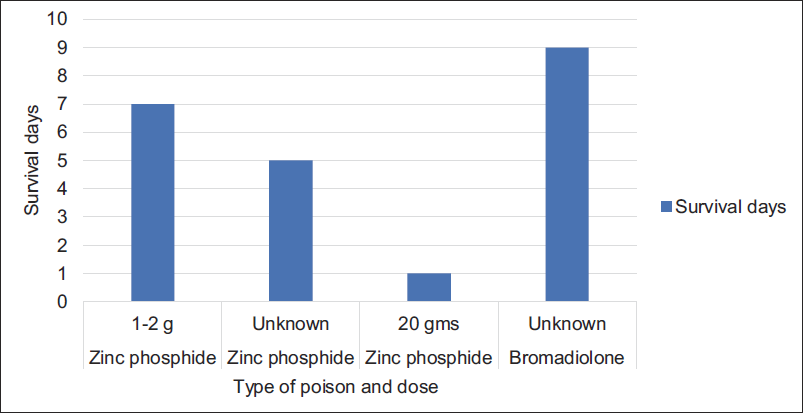
Discussion
Rodenticides have a wide range of toxicity, fatality and modes of action. Studying each poison independently and examining its different modes of action, organ involvement, toxicity and deadly effects will provide you the most thorough understanding of the rodenticides. Compounds with a single-dose LD50 less than 50 mg/kg of body weight are included in this group. This group of compounds consists of zinc phosphide and aluminium phosphide. The poison that causes both types is phosphine, which has been considered hazardous due to its inhibition of cytochrome c oxidase. Zinc phosphide toxicity has a few days latent phase, but aluminium phosphide toxicity manifests as systemic poisoning right away. Appropriate treatment with necessary antidote must be given as early as possible within 12 hours. 4
Due to its extended half-life, bromadiolone, which is categorized as a ‘super coumarin’, may need to have the prothrombin time (PT) and international normalized ratio (INR) monitored often for several days. 5 Even though the risk of bromadiolone poisoning has increased, only limited number of published articles are available till now. Early supportive treatment would definitely help to recover sooner.
Intentional self-harm through the use of rodenticide is a serious global health issue that has a significant influence on family and societal dynamics. So, the need to study about the rodenticide poisoning plays a significant role. In our study, all the patients who consumed poison were in the age group of 20–30 years. A study was conducted by Vignesh et al. in Chidambaram also had the majority of 20–30 age group. 6 Our case series was female predominant and mode of poisoning was suicidal. Another study conducted by Lokesh et al. in Mandya, Bangalore, with found majority of females had suicidal intension. 7 In our case series, all the four patients were females and the histopathological examination of these four patients had revealed they were in their menstrual phase. This reveals there was a significant association between suicidal attempts and menstrual cycle. The menstrual cycle is associated with nonfatal suicidal behaviour; attempts at suicide tend to happen more frequently during the cycle’s lowest oestrogen (and serotonin) stages. A study conducted by Leenaars et al. revealed that women who had committed suicide were menstruating at the time of event. 8
PDC plays a vital role in detecting type of poison ingested which helps the treating physician to provide appropriate treatment with specific antidote and helps in reducing the mortality. Treatment for each case of rat kill poisoning involves a thorough clinical examination, progressive monitoring of the coagulation profile and LFTs. 9 Due to the abundant availability of rodenticides and for the rural population involved in agriculture, it is accessible at a lower cost. For the peripheral hospitals treating a case of rodenticide poisoning without the proper availability of antidote poses a great challenge.
Conclusion
Rodenticide poisoning is an important health problem with a high case fatality rate especially with metal phosphides. Easy availability, over-the-counter or on e-commerce websites and a lack of antidotes for rodenticides in our country pose an important health problem. Early gastric lavage and symptomatic treatment were key in the management of rodenticide poisoning. Still, universal guidelines are needed for proper management. Prognosis mainly depends upon the type of chemical compound and amount of compound consumed, the time interval between intake and first aid treatment and early treatment with magnesium sulphate and acetylcysteine. Early magnesium sulphate therapy may be useful in aluminium phosphide poisoning patients and acetylcysteine therapy may prevent hepatic complication. In our case series, PDC helped us in confirming the diagnosis and we started treatment at the earliest. However, delayed presentation, an unknown quantity of ingestion and no specific antidote are the drawbacks which led to the patient’s demise. It was also observed that all four cases in our case series were females between the ages of 20 and 30 years old who committed suicide during or near their menstruation period, as evidenced by an HPE examination of the uterus, implying that the patients may have had premenstrual dysphoric disorder (PMDD). People with PMDD will have PMS symptoms (bloating, headache and breast tenderness) along with extreme irritability, anxiety or depression. Therefore, family issues, PMMD, easy access and availability to rodenticide could all have contributed to the suicides in these four cases. Therefore, improving public awareness regarding the lethality of rodenticides, strict monitoring of sales and usage of rodenticides, family support, proper counselling against suicide and awareness on PMMD will help to avoid indiscriminate use and poisoning with rodenticides, as well as potentially lowering suicidal rates in the near future.
Footnotes
Acknowledgement
We express our deep sense of gratitude to all the relatives and MRD department.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
The study was conducted after obtaining the ethical clearance from the Jawaharlal Nehru Medical College, Belagavi.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
The study was conducted after obtaining the informed consent from patient’s relatives.
