Abstract
Background
Although mandated inpatient mental healthcare is initiated on a therapeutic premise, consumers’ autonomy, safety and recovery are often compromised. Mandated inpatient mental healthcare is ethically complex and the therapeutic basis of inpatient mental healthcare must be clearly established.
Research aim
The aim of this study is to understand the perspectives of consumers in relation to the ethical merits and demerits of mandated inpatient mental healthcare.
Research design
This study was a qualitative descriptive study, involving semi-structured interviews with 12 consumers. The data were analysed using reflexive thematic analysis, whereby significant themes were constructed and reported with supporting quotes.
Participants and research context
Participants were adults who had experienced involuntary inpatient mental healthcare. Participants were recruited from social media special interest groups.
Ethical considerations
Free and fully informed consent was sought from all participants. This study was approved by a university human research ethics committee.
Findings
Mandated inpatient mental healthcare was regarded as ethical to the extent that it ensured safety in circumstances that could not be managed without mandated intervention. However, the perceived ethical merit of mandated care was challenged by recurring violence and unwanted sexual interactions, as reported by the participants of this study. Furthermore, mandated inpatient mental healthcare involved the routine and unnecessary suspension of participants’ autonomy, without regard for their preferences or individual needs.
Conclusions
Mandated inpatient mental healthcare is ethical to the extent that it is necessary for ensuring therapeutic outcomes. However, the hazardous environment and incursions to autonomy described by participants compromise perceived ethical integrity. This study demonstrates the necessity of a clear therapeutic basis for all aspects of mandated inpatient mental healthcare, and that greater consideration for consumer safety and autonomy is needed.
Introduction
Inpatient care is often mandated during treatment for high acuity mental illness. A variety of terms are used to describe the practice of mandating inpatient care, such as ‘involuntary treatment’, 1 ‘involuntary commitment’ 2 or ‘sectioning’. 3 Although a common practice, the ethical defensibility of mandated inpatient mental healthcare is subject to considerable scrutiny due to its inherently coercive nature. O'Brien and Golding 4 have previously defined coercion as ‘any use of authority to override the choices of another’ (p. 168). Mandated inpatient care is coercive by definition, and typically involves non-negotiated treatments, loss of privacy and personal autonomy. Contrary to the therapeutic premise of mandated inpatient mental healthcare, coercive practices such as seclusion and restraint are common and regarded as harmful by both nurses and consumers. 5 Furthermore, consumers report that coercive practices are liable to hinder mental health recovery. 6 The World Health Organization (WHO) and United Nations (UN) jointly published guidelines advocating for a mandate on fully informed consensual mental healthcare, as well as the elimination of involuntary care. 7 Mandated inpatient mental healthcare is clearly incompatible with contemporary principles of mental healthcare.
Despite clear denunciation, mandated inpatient mental healthcare is arguably ethically viable in certain circumstances. Incursions to autonomy from mandated inpatient mental healthcare are justified on the premise of therapeutic necessity; mandated inpatient mental healthcare may be necessary for immediate safety and stabilisation. 8 The NSW Mental Health Act clearly establishes that involuntary inpatient care is defensible on condition that such measures are necessary to secure immediate safety, and on proviso that restrictive practices are limited to the minimum necessary in the circumstances. 9 According to research of consumer perspectives, coercive care can be justified in certain circumstances.10–14 The use of force is justified when used to diminish proximal threats to physical safety. For example, the use of force without consent to interrupt violent or suicidal behaviour is regarded as justifiable, 15 which is itself common grounds for mandated inpatient mental healthcare. According to consumer perspectives, the use of force-in a manner that is ostensibly coercive-can be warranted by situational ethical mandates, suggesting that mandated inpatient mental healthcare can be ethically defensible.
The conflicting assertions made regarding the ethics of mandated inpatient mental healthcare must be addressed. In order to maintain the therapeutic merit of the power differential, consumers must be consulted about their views of the ethics of mandated inpatient mental healthcare. 8 Consumer insights regarding mandated inpatient mental healthcare are necessary for developing and maintaining the ethical integrity of practice and the safety of both consumers and healthcare professionals. The aim of this study is to understand the perspectives of consumers in relation to the ethical merits and demerits of mandated inpatient mental healthcare.
Methods
This study was a qualitative descriptive investigation of consumer perspectives. In-depth, semi-structured interviews were conducted with people who have experienced mandated inpatient mental healthcare. The design of this study and process of analysis was primarily informed by guidance from Braun and Clarke and Doyle et al.16–18 The COREQ checklist was used to ensure comprehensive transparency in reporting. 19 There were no reported adverse events from this study. This study was conducted with close consideration for consumer perspectives and interests. A listed co-author (KG) is a consumer advocate and was involved in the design and procedures of the study and data analysis. All authors were involved in the development of the interview questions to ensure completeness and sensitivity. The interview questions were determined with consideration for issues established in the broader literature, as well as with consideration for the experience of the authors.
Sample
This study relied on non-probability purposive sampling, of people who had experienced mandated inpatient mental healthcare. All participants were required to be 18 years of age or older and reside in Australia. The participants were required to have experienced mandated inpatient care in Australia; however, people who were currently receiving inpatient care were excluded.
Recruitment and data collection
Recruitment and data collection commenced February 2024 and was finalised in May 2024. Recruitment was conducted on two social media community sites for people with psychotic illness in Australia. A post advertising the study was made on the social media pages, and potential participants contacted the Principal Investigator (PI) to express interest. An information sheet detailing the study was provided to those who made enquiries. The information sheet provided details about the research team, research aims and requirements of participation. Interviews were conducted by the PI over an online audiovisual conferencing service (Zoom). Recruitment and data collection continued until data saturation occurred, the point at which no new information or themes were observed. 20 However, it was anticipated that 12–15 interviews would be required to address the aims of the study, consistent with other relevant qualitative investigations. 21 The investigators had no prior relationship with any of the participants.
Data management
Upon completion of data collection, audio recordings were deidentified with software (Audacity), and the deidentified audio files were dispatched for transcription to a service compliant with the Australian Privacy Principles within the Australian Privacy Act 1988 and the Guidelines on Privacy in the Private Health Sector issued by the Federal Privacy Commissioner under the National Health Act 1953. 22 Data will be stored for 5 years post-publication and will then be permanently deleted in accordance with university institutional ethical guidelines.
Analysis
Process of thematic analysis (adapted from Braun and Clarke 17 ).

Ethical considerations
This study was ethically approved by the University of Wollongong Human Research Ethics Committee (2023/207). Participants were required to be able to read, speak and understand English for the purposes of consent and participation. Upon meeting, participants were first asked questions to determine their suitability for participation, followed by a verbal consenting process. With suitability and fully informed consent established, the interview questions commenced. All data was deidentified, and pseudonyms are used for reporting results. Data was stored securely in accordance with institutional guidelines.
Findings
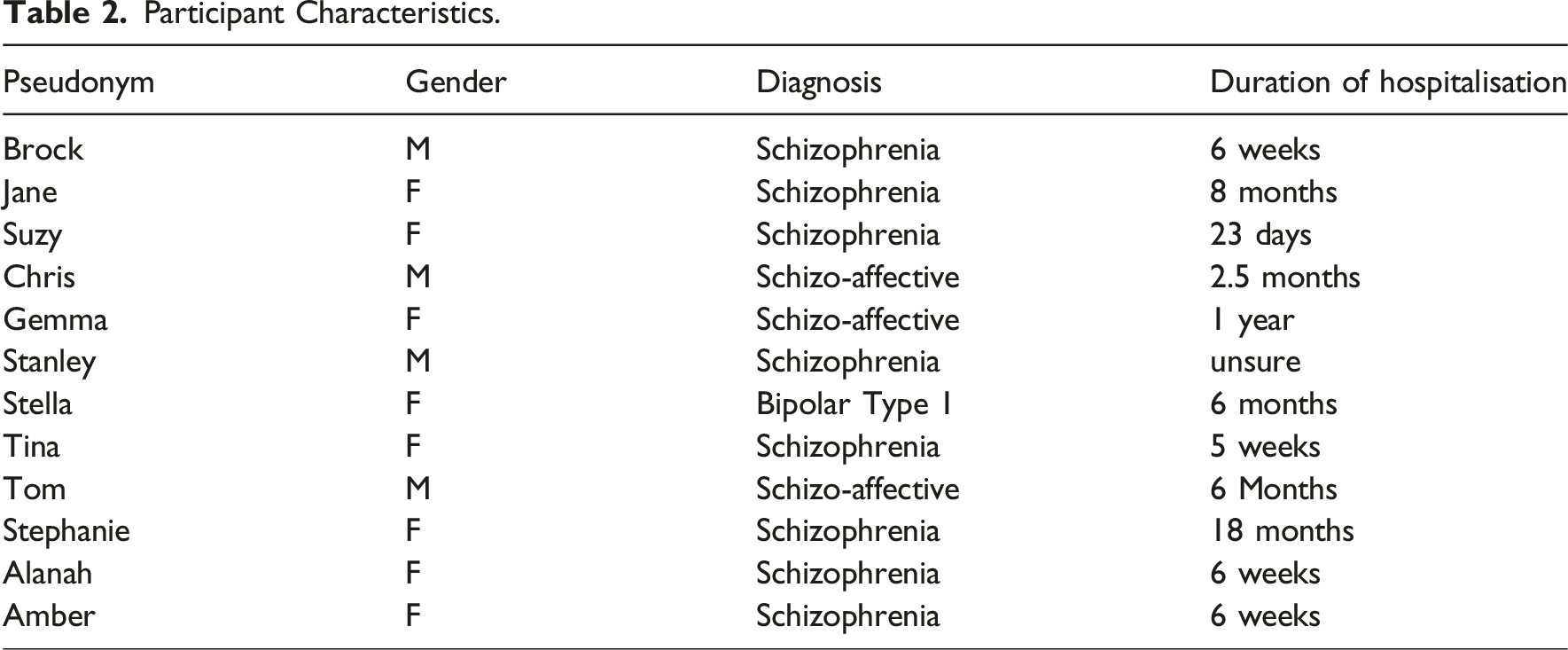
Participant Characteristics.
Themes.
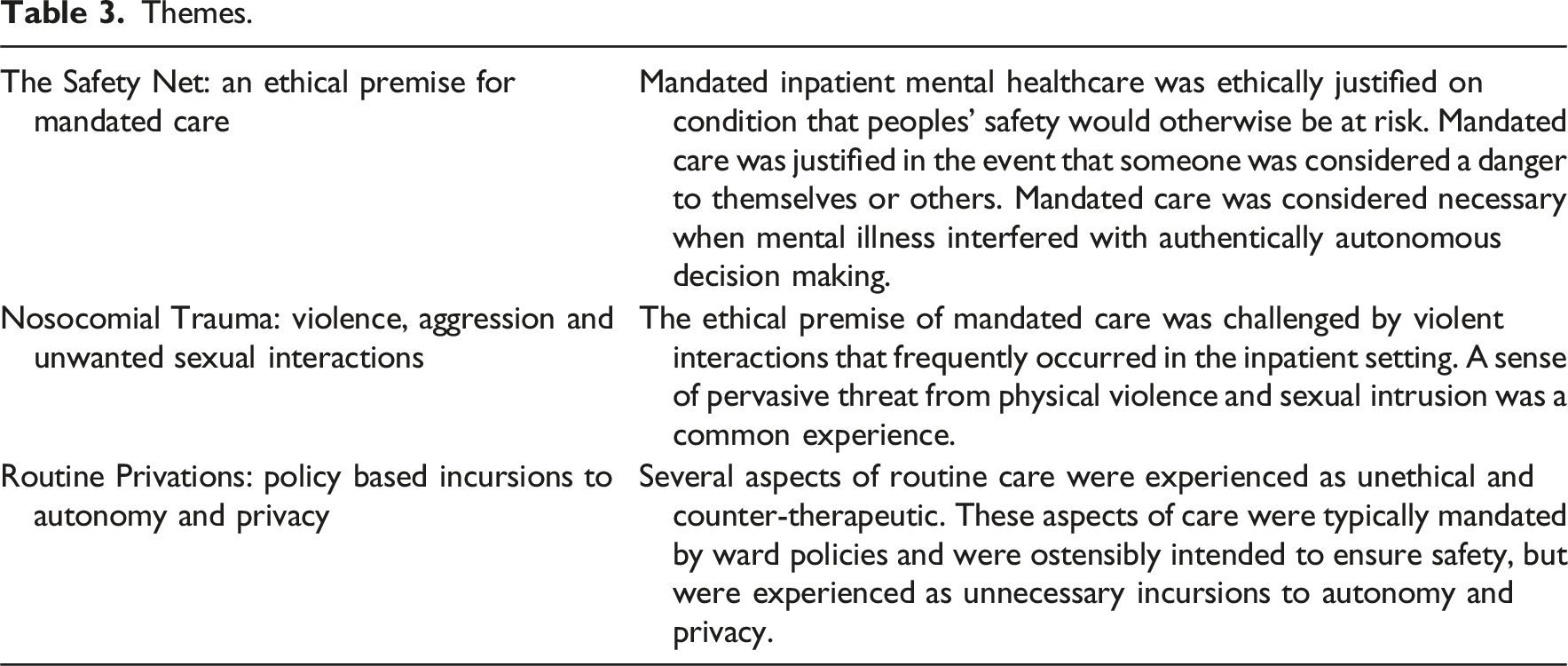
The safety net: An ethical premise for mandated care
Participants reported that mandated inpatient care was a necessary measure, justified by particular circumstances and conditions. Acute psychotic illness, suicidal behaviour and reputational destruction were described as justifications for mandated inpatient care. Brock described a situation where he became acutely psychotic and paranoid, convinced that his life was in danger. Consequently, he drove his car recklessly at high speeds, and he was ultimately involved in a serious motor-vehicle accident: ‘After having that experience, I know that involuntary treatment is a real necessary thing. I 100 per cent support it. Not only did I nearly die, other people nearly died. There was nearly head on crashes and all sorts of stuff. That all came about basically because I wasn't getting treatment and stuff’, Brock.
Recognising the harm he could have caused to himself and others, Brock was grateful for the mandated care he received, and strongly believed that his inpatient mandated admission was a necessary and therapeutic measure. In addition to describing circumstances threatening physical harm, the participants also described situations of reputational injury. In the course of a manic episode, Stella recounted the reputational harms she self-inflicted from her ill-considered interactions: ‘…but I definitely – I needed something. I needed to be somewhere safe. I needed to be, I suppose, somewhere where I wasn’t getting myself into more trouble, because I was also going out on Facebook and going out on text messages and like very – and that kind of stuff you can actually – you can destroy your own life very, very quickly’, Stella.
Stella relayed that she relied on her reputation for her livelihood, and how mandated care was a necessary and protective intervention. In addition to relaying their own accounts, participants described circumstances that should be generally considered ethical grounds for mandated inpatient care. Most participants agreed that credible risk of suicide was reasonable grounds for mandated inpatient care: ‘That is a tricky question and, yes, I have been – I’ve been suicidal many times. But I think someone might need to step in, like they take all your wires and shoelaces and stuff like that to try and prevent – minimise the risk of you committing suicide. But I think – I think, if someone has a history of suicide behaviour, then it’s all right to take measures to prevent that’, Stanley.
In addition to validating mandated admissions to the inpatient setting, participants also expressed that the mandated use of medication was justified. Jane described how mandated medication was justified by the impaired decision-making capacity that acute mental illness induced: ‘This is really hard because people who really need medication often really don't want it. I know it's taken me a really long time. Yes, I think it's justifiable to give people medication when they don't want it. Yes, I do. That's purely because when you're not in the right frame of mind, you can't make those decisions. That's a decision - there's something weird that happens with us schizophrenics. We have this paranoia against people who give us medication, we have paranoia against medication itself. There's all this weird psychology around it. It's taken me a really long time to accept the fact that I have to have medication and that I'm happy to have medication. Yeah, I do think it's justifiable’, Jane.
Overall, the participants’ justifications for mandated inpatient care were based on the understanding that mental illness had the potential to corrupt the capacity for authentic autonomy, with consequences that posed significant threat of harm to self and others. The participants described how, whilst acutely unwell, their wellbeing – as well as the wellbeing of others – could not be ensured outside of the safety and containment of mandated inpatient care.
Nosocomial trauma: Violence, aggression and unwanted sexual interactions
The therapeutic and ethical premise of mandated inpatient care was challenged by a pervasive sense of threat from violence and aggression from fellow inpatients. A mandated inpatient admission often involved co-habitation with people who were frequently violent and people who offered unwelcome sexual interactions. Brock described his experiences with violent inpatients, and Jane described unwelcome sexual interactions. ‘The last time I was in the ward a few years ago, it was quite violent in there because of the patients. The patients were quite violent and they needed to be restrained. They were a risk to people's safety… Somebody tried to pick a fight with me on the first day that I was in there and they were sedated. It's a dangerous place in my opinion’ Brock. ‘It also put me in a vulnerable position because I had a guy wrap his arms around me and being really flirtatious and stuff… I was vulnerable so I didn't know how to navigate that situation… My dad actually saw him, and he complained to the nurses. The nurses weren't doing anything about it… There was another, in the same period of time in the same seclusion ward, there was an old man that was masturbating. I threw my slipper at him’ Jane.
The participants of this study felt aggrieved by staff who made little attempt to intervene in such situations, compounding their sense of vulnerability. Participants disclosed that they felt threatened to the extent that they seriously countenanced the need to physically defend themselves. Furthermore, the threat of physical violence validated restrictive measures, such as seclusion and restraint, as a means of managing the threat of violence. ‘Absolutely. Absolutely. I felt very intimidated in my last stay. I thought I was going to have to have a physical altercation on more than one occasion. I could probably stand up for myself; I had a very rough upbringing with an older sister, but I definitely felt like I was probably going to have to protect myself at one point’ Jane. ‘One of the patients was violent a number of times and had to be sedated, and I think that that's the best thing they could've done with him… I think seclusion can be part of treatment. If somebody is posing a risk to others and themselves, seclusion can be a valid option’ Brock.
It is important to note that the threat of physical violence and unwanted sexual interactions were more clearly described by the female participants of this study (most of the participants in this study were female). This led to a recurring suggestion that men and women be separated, or that inpatients be separated with consideration for their degree of vulnerability. It was considered an injustice – and an absurd irony – to be mandated into inpatient care on a therapeutic premise, only to be subjected to the most threatening circumstances. ‘I didn’t feel safe sleeping in a hallway full of mixed gender people, and particularly there was one night I got moved from acute to sub-acute, for misbehaving. They separated me from other people that I guess I was being rowdy with. It was like – oh, it’s probably like 70 per cent men, and lots of young men that had come in from night clubbing or something, like peaking, and I felt really afraid of them and I said to the nurse, I feel really afraid; I’m scared I’m going to get raped. She said, I’ll check on you every 30 minutes and I was like 30 minutes is a really long time to get raped’ Stella. ‘I definitely think splitting male and female would be more safer for the young women. Probably not just young women, it would be all age women… Like in a perfect world, yes, it would be split up probably diagnosis and genders. You probably wouldn't put - someone in a psychosis that has violent tendencies, you probably wouldn't put that person with someone who's really vulnerable’ Jane. ‘The fact that they put people who are violent and people who are terrified in the same ward is absolutely ludicrous… I would definitely split people who are terrified with people who are violent. It’s not fair on the people who are terrified’ Suzy.
Routine privations: Policy based incursions to autonomy and privacy
Inpatient care involved mandated routine measures that were often experienced as unwelcome incursions to autonomy and privacy. These routines were implemented as standard precautions mandated by policy, and could not be amended or ceased. Participants expressed frustration that they were not permitted to sleep, attend to hygiene and toileting without interruption. Furthermore, personal property was often confiscated and only returned briefly on request. Gemma described her frustration at the privations she experienced, that seemed to lack any therapeutic basis. ‘I had to go to the nurses' station to ask for deodorant, for moisturiser, for a… it's not a very nice feeling to feel like a 30 year old woman who can't even handle… a hairbrush, you know? It's pretty dehumanising… I don't think it's okay. What can you do to yourself? I don't like being on the toilet and having someone come in and do a check on me while I'm on the toilet and like - it's yuck’ Gemma.
‘My mum was sneaking tampons in for me, because I had to use the hospital issued enormous pads and I was like, well, why? They said, once there was this woman who forgot to change her tampon because she was manic and she got toxic shock so we don’t let anybody use tampons. I was like, really?... That – for me that felt like a loss of dignity. To have to go to the nurse and be issued with like three hospital grade pads, that made me feel really terrible’ Stella.
The non-negotiable deprivation of basic autonomies and rudimentary privacy was ill-experienced. The privations were compounded by the absence of any perceived therapeutic justification, and the standardised mandated application of such measures represented a refusal to provide person-centred care on an individual basis. In this way, care in the inpatient setting was unethical.
Discussion
O’Brien and Golding 4 stipulate that practices that meet the criteria for being coercive are only justified when the harms from coercion are less than the harms of failing to act coercively when necessary. Furthermore, they also stipulate that coercive practices should involve the least force necessary to secure the consumer’s wellbeing. 4 The principle of ‘least restrictive practice’ is endorsed as convention in mental health policy and law.1,9 Despite the defensibility of the guiding principle of ‘least restrictive practice’, the distinction between beneficent use of force and maleficent coercion is poorly demarcated. Evincing this poor demarcation, a recent meta-ethnography demonstrates the sense of tension mental health nurses experience when providing involuntary mental healthcare 25 ; mental health nurses acknowledge that involuntary care has the potential for both therapeutic and harmful outcomes, and this tension is a source of internal conflict and moral distress. 25 Mandated inpatient mental healthcare is ethically complex, and the findings of this study demonstrate the importance of a nuanced examination of the ethical premise of mandated inpatient mental healthcare. The participants of this study, as well as previous consumer perspective research, indicate that mandated mental healthcare is ethically viable under certain circumstances.10–14 Specifically, mandated mental healthcare is justified when physical safety is at risk, or when mental illness substantially interferes with autonomous decision making. The injunction to involuntary inpatient mental healthcare recommended by the WHO and UN is inconsistent with the nuanced perspectives of consumers. Rather than an injunction, mental health policy should make clear indications about how and when mandated, involuntary mental healthcare is to be conducted. Furthermore, clinicians must have a clear and well substantiated procedure for the escalation of force developed with close reference to consumer perspectives.
Physical aggression and sexual harassment are recurring issues in the inpatient mental health setting.26–29 Whilst physical aggression and sexual harassment are not inherent aspects of mandated inpatient mental healthcare, the participants of this study reported that these events undermined the therapeutic and ethical premise of mandated mental healthcare. This finding demonstrates the need for clear strategies that prevent and manage these events. Some of the participants of this study suggested sex-based segregation as a means of mitigating unwelcome sexual interactions. Bowers et al. 29 indicates that sex-based segregation does not necessarily offer greater protection from unwanted sexual interactions. However, in contrast, Mezey, Hassell 28 reports that sex-based segregation minimizes the likelihood of sexual transgression for women. The absence of staff intervention in response to violence or sexual transgressions compounded participants’ sense of vulnerability. Dismissive responses from staff and feeling unprotected is reported in other research of consumer perspectives. 28 In order to ensure the ethical implementation of mandated inpatient mental healthcare, staff must be prepared and properly trained to intervene in events of physical aggression and sexual harassment. The ethical integrity of mandated inpatient mental healthcare is dependent on the maintenance of a safe environment.
Mandated inpatient mental healthcare involves the implementation of standard precautions that constrain autonomy and privacy. These policy driven routine measures are implemented in the absence of individualised preference or consideration, and to this extent undermined participants’ perception of the therapeutic basis of mandated hospitalisation. This finding demonstrates the importance of authentically integrating person-centred mental healthcare in the inpatient setting. Person-centred mental healthcare lays emphasis on the recognition of consumers’ personhood and empowering self-determination in decision-making. 30 Ethical mental healthcare will account for personal preferences and maximise autonomy. Strategies such as shared decision making and the use of advanced directives are viable means of protecting consumer autonomy. 31 Furthermore, service design and research of mental healthcare must be co-designed, 32 and services must espouse the principles of consumer directed care (CDC). 33 CDC is a concept of care that lays emphasis on giving individuals greater decision-making capabilities over the care they receive. 33 Service modelled on CDC has demonstrated advantages, with enhanced recovery prospects and greater satisfaction with services. 34
Limitations
The study’s use of purposive sampling through social media platforms presents both strengths and limitations. Whilst this approach successfully recruited suitable participants, it may have inadvertently over-represented participants who were more digitally literate, socially connected, or comfortable engaging online. This sampling strategy could therefore limit the representativeness of findings, particularly regarding individuals who may be more marginalised or less technologically engaged. Furthermore, all data were self-reported and gathered from people with psychotic illness from one country. The findings therefore are relatively localised, and inferences may be limited to this extent. The geographical specificity to Australia, whilst providing contextual depth relevant to the Australian mental health system, limits the transferability of findings to other healthcare contexts with different legislative frameworks, service delivery models, or cultural approaches to mental health treatment. Future research incorporating multiple jurisdictions and diverse cultural perspectives would strengthen the generalisability of findings regarding mandated mental healthcare experiences. Additionally, the requirement for English proficiency excluded potentially valuable voices from culturally and linguistically diverse communities, which may be particularly significant given the disparities in mental health service experiences among these populations.35,36 Future research should investigate how consumer and staff perspectives can be better integrated to address the ethical issues of involuntary inpatient mental healthcare established in this study.
Conclusion
The perceived ethical validity of mandated inpatient mental healthcare was for the most part determined by its perceived therapeutic merit. That is, mandated inpatient mental healthcare was ethical to the extent that it was necessary for ensuring therapeutic outcomes. However, the perceived therapeutic merit of mandated inpatient mental healthcare was threatened by events that were perceived as harmful or events that involved unnecessary loss of autonomy and privacy. This study demonstrates the necessity of a clear therapeutic basis for all aspects of mandated inpatient mental healthcare, and that greater consideration for consumer safety and autonomy is needed. Authentic integration of consumers’ perspectives is imperative for maintaining the ethical integrity of mandated inpatient mental healthcare. 8
Footnotes
Acknowledgements
The research team would like to thank all participants of this study for their time and for sharing their experiences.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by an internal grant from the University of Wollongong.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The dataset generated and analysed during the current study is not publicly available. The data contains sensitive information that could compromise participant privacy and confidentiality.
