Abstract
‘Moral resilience’ is a concept whereby individuals sustain and restore their integrity in the face of moral distress. While the key aspect of this concept is the individual’s integrity, some indicate that personal and professional integrity differ. In clinical practice, a phenomenon is observed where nurses demonstrate resilience and behave ethically in accordance with their professional values. However, this phenomenon cannot be fully explained by moral resilience. This study proposes the concept of ethical resilience, a phenomenon in which resilience and ethical behaviour are demonstrated towards ethical issues, by undertaking concept synthesis. Articles that mention ethical resilience were selected from among those released on PubMed and CINAHL and Web of Science and Eric (up to 20 January 2024). Walker and Avant’s method was used for the concept synthesis. Four attributes were extracted for ethical resilience: (1) grasping ethical issues, (2) integrity as a nurse, (3) flexible and tenacious approach, and (4) collaboration to resolve ethical issues. Based on the results of concept synthesis, nurses’ ethical resilience was defined as the ability to sustain or restore professional competence when facing ethical issues while assessing the situation and collaborating with others. This concept describes a positive approach to ethical issues oriented towards professional ethical behaviour. The concept of ethical resilience was derived from previous studies accumulated to this date. Research on resilience to ethical issues and moral distress is still in its infancy, and thus it must be examined further. It is expected that discussion on these matters will advance further along with the concept of ethical resilience.
Introduction
Moral resilience is a concept that refers to the ability to recover from the moral distress 1 that arises from ethical issues. This idea has existed since 2005 in the global psychological community. 2 It was initially defined as follows: ‘Moral resilience means to be good (and prove one’s integrity and character) under conditions of risk’. The concept, which was subsequently adopted in nursing science, drew attention when Rushton 3 defined it as the ‘capacity of an individual to sustain or restore their integrity in response to moral complexity, confusion, distress or setbacks’. Its key aspect as defined by Rushton 3 is to sustain or restore integrity and mitigate moral distress by being faithful to one’s own values and convictions.3–5 Some researchers view moral resilience as a virtue, highlighting it as a character trait. 6 In addition, according to experts, ‘personal integrity’ is a key component. 7 Personal integrity and the underlying character traits are the main elements of moral resilience, which is based on one’s own judgement of right and wrong, good or bad, and not on professional ethical perspectives. Another argument posits that nurses must build moral resilience by managing their own emotions before trying to help others. 8 This emphasises it as the ability to restore or sustain one’s values and convictions when they are, or are about to be, undermined by distress related to moral adversity. However, it seems that the concept and usage of resilience, especially in nursing, are ambiguous.
Background
Resilience
Examining conceptual analyses of resilience in general, one previous study 9 introduced Rutter’s 10 definition of resilience attributes, namely, ‘rebound and continuity’, ‘self-awareness’, ‘determination’, and ‘sociable attitudes’, with the antecedent requirement of ‘adversity’ and consequent being ‘coping effectively’ through a ‘toughening effect’. A subsequent similar conceptual analysis 11 also cites Rutter’s 10 definition. A 2013 study 12 indicates the attributes of resilience. These three conceptual analyses differ in the expression of attributes, but individual factors such as flexibility, optimism, and confidence are examined with a view toward ‘getting back on one’s feet’, which includes self-reflection. In addition, relationships are suggested as environmental factors, including ‘support from others’.
The most recent conceptual analysis of resilience among nurses was by Cooper et al., 13 which proposed similar attributes as those described earlier. If differences exist, the inclusion of the term ‘as a professional’ in the antecedent requirements and indications of ‘achieving better care’ or ‘improving the quality of patient care’ in the consequences or outcomes are characteristics of resilience in nursing.
Moral resilience
In moral resilience, the focus is on sustaining or restoring personal integrity without compromising personal values and conviction. However, the term ‘resilience’ is used not only to denote sustaining or restoring one’s integrity as an individual but also including elements related to the perspective of ethics as a nurse. The latter includes expressions such as ‘resilience to ethical issues’ and ‘organising and clarifying ethical issues to enhance moral resilience’.3,7,14,15 For example, when discussing moral resilience, some studies identify the need to distinguish personal and professional integrity, recognise the difference between personal and professional moral distress, and examine whether there is any inconsistency between personal and professional values.16,17 Using words such as ‘occupational’ and ‘professional’, these studies argue that nurses must make decisions based on their professional opinions, that is, professional ethics, rather than personal moral views. However, they all use the word ‘moral’ to refer to matters concerning ethics.
The aforementioned points also apply to the study of nursing ethics. Terms such as ‘moral practice’ and ‘moral issues’ are often used in cases involving issues that nurses may face in their profession or those involving professional practice, even if these issues relate to ethics,1,6,18,19 not personal moral views. It has been highlighted that painful experiences and problematic situations for nurses that involve ethical issues are often framed as moral issues in international academic circles. 20 This may partly be because studies of issues related to ethics did not spread widely until Jameton 1 proposed the concept of ‘moral distress’.
Ethical resilience
Ethical resilience is not treated as a separate concept from that of moral resilience in previous studies. As of 20 January 2024, articles containing the term ‘ethical resilience’ were not found on a search of medical databases using this term. A search of PubMed and CINAHL using the term ‘ethical resilience’ returned 13 articles targeting nurses, medical students, and those in medical-related professions. However, these articles did not use the term ‘ethical resilience’ but included ‘ethical issues’ and ‘ethical behaviour’. On the other hand, four articles appeared in a Web of Science search using the term ‘ethical resilience’ across all disciplines: one in the field of law, one in education, and two in social anthropology. These four articles described resilience as phenomena, but no accounts were found regarding ethical resilience as a concept. Thus, the concept of ethical resilience has not been addressed in nursing science. Furthermore, no clear definition or structure of the concept has been provided in other disciplines. As noted, ethics and morality tend to be treated as the same concept in medical disciplines. Studies on moral resilience include those that refer to ethical resilience, that is, those that argue that nurses demonstrate resilience with respect to ethical issues from a professional perspective. Therefore, this study undertakes conceptual synthesis of ethical resilience to advocate for the use of the concept. The distinction between morality and ethics in the study of nursing ethics may prevent confusion, broaden the scope of discussion, and contribute to future research endeavours.
Methods
Concept synthesis is a concept development method and useful way to develop standardised terminology for practice. 21 It involves examining related concepts for similarities and differences and observing new phenomena that have not been described before. As in previous studies, the method in this study followed the literature synthesis method of Walker and Avant, 21 which combines phenomena that represent a concept through careful reading of the literature to extract its underlying attributes and define it. 22
Data collection and analysis
We conducted literature collection by using PubMed, CINAHL, Web of Science, and Eric databases, which all index literature on nursing science. Among the search terms were ‘ethical issues’ or ‘ethical dilemma’ or ‘ethical concerns’ or ‘ethical distress’, each of which indicates a situation that requires ethical resilience. This facilitated searching for articles that may contain accounts related to the phenomenon. One search term was ‘(ethical issues or ethical dilemma or ethical concerns or ethical distress) AND (resilience or resiliency or resilient) AND (nurse or nurses or nursing)’. Therefore, the terms ‘resilience or resiliency or resilient’ and ‘nurse or nurses or nursing’ were added to the search. In addition, the following search term was used: ‘(moral issues or moral dilemma or moral concerns or moral distress) AND (resilience or resiliency or resilient) AND (nurse or nurses or nursing)’. In this term, the word ‘ethical’ was changed to ‘moral’ because some previous studies discuss ethical issues, ethical dilemmas, and ethical distress in terms of moral issues, moral dilemmas, and moral distress. In addition, the search term ‘moral resilience’, a similar concept, was used to search for articles because ethical resilience may have been mentioned in these articles. The concept to be considered would be developed for the first time, but moral resilience (a similar concept) is also evolving. Thus, timeframes were not set for either of these terms.
Criteria for literature selection.

Data synthesis for conceptualisation of ethical resilience and virtual cases
The selected literature was then re-read in its entirety, and elements suggesting ethical resilience were coded. The coded content was then scrutinised, and commonalities were qualitatively and inductively categorised into higher-level concepts. This process was carried out through a back-and-forth way and confirmation between the researchers until consensus was reached. Furthermore, advice was sought separately from the researchers on the extracted codes, categories, and attributes from three doctoral researchers with achievements in nursing ethics, philosophy/ethics, and resilience research, respectively, to ensure their validity.
Then, we developed virtual cases using the attributes that make up the concept of ethical resilience, by partially using Walker and Avant’s concept analysis method. The exemplary case represents a model of ethical resilience as a practical case study and to distinguish it from the similar concept of moral resilience.
Results
On 20 January 2024, the literature was searched for ‘(ethical issues or ethical dilemma or ethical concerns or ethical distress) AND (resilience or resiliency or resilient) AND (nurse or nurses or nursing)’. Consequently, 44 articles were found on CINAHL, 24 on PubMed, 24 on Web of Science, and 3 on Eric. The literature was further searched using ‘(moral issues or moral dilemma or moral concerns or moral distress) AND (resilience or resiliency or resilient) AND (nurse or nurses or nursing)’. As a result, 102 articles were found on CINAHL, 140 on PubMed, 204 on Web of Science, and 1 on Eric. Simultaneously, a search for ‘moral resilience’ yielded 81 articles on CINAHL, 97 on PubMed, and 107 on Web of Science. Furthermore, one for ‘ethical resilience’ yielded 4 articles on Web of Science and 3 on Eric. From these 834 articles, 342 were selected after removing duplicates, articles that only contained symposium rosters or photos, and dissertations and theses. From the selected articles, 90 were extracted after the titles and abstracts were screened according to the inclusion and exclusion criteria (Table 1). Finally, 49 articles were extracted (Figure 1). Subsequently, the articles were read carefully and repeatedly. As a result, contents that constitute the attributes of ethical resilience were extracted from 40 of the 49 articles. Search and retrieval process.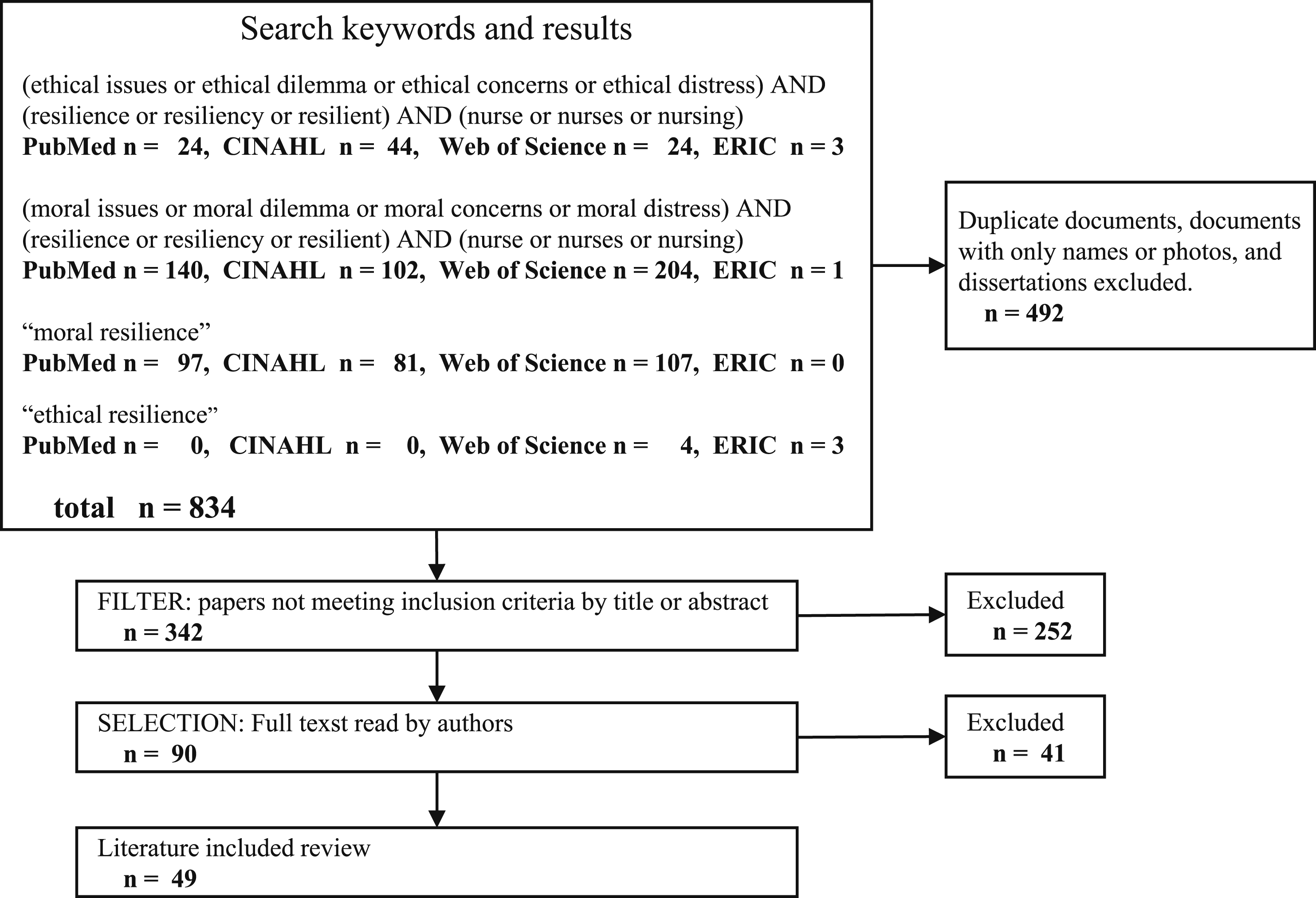
Attributes of ethical resilience
Attributes of the concept of ethical resilience for nurses.
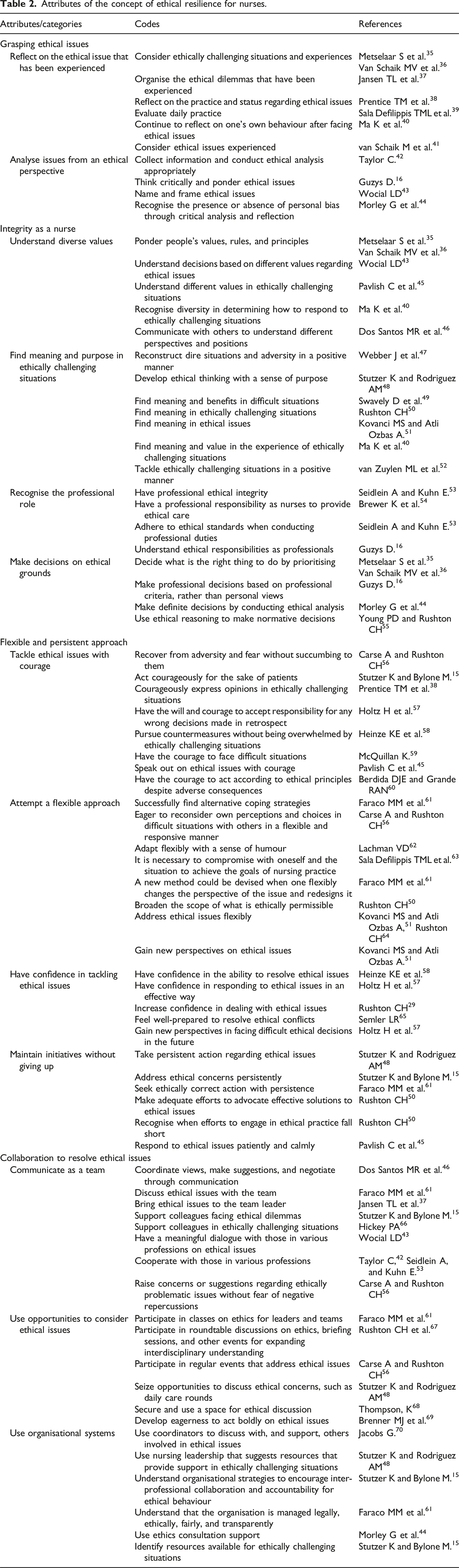
Grasping ethical issues
This attribute was synthesised from the following two categories: ‘Reflect on the ethical issue experienced’ and ‘Analyse issues from an ethical perspective’. The first category consisted of the following six codes: ‘Consider ethically challenging situations and experiences’; ‘Organise the ethical dilemmas that have been experienced’; ‘Reflect on the practice and status regarding ethical issues’; ‘Evaluate daily practice’; ‘Continue to reflect on one’s own behaviour after facing ethical issues’; and ‘Consider ethical issues experienced’. The second category consisted of the following four codes: ‘Collect information and conduct ethical analysis appropriately’; ‘Think critically and ponder ethical issues’; ‘Name and frame ethical issues’; and ‘Recognise the presence or absence of personal bias through critical analysis and reflection’.
Integrity as a nurse
This attribute was synthesised from the following four categories: ‘Understand diverse values’; ‘Find meaning and purpose in ethically challenging situations’; ‘Recognise the professional role’; and ‘Make decisions on ethical grounds’. The first category consisted of the following five codes: ‘Ponder people’s values, rules, and principles’; ‘Understand decisions based on different values regarding ethical issues’; ‘Understanding different values in ethically challenging situations’; ‘Recognise diversity in determining how to respond to ethically challenging situations’; and ‘Communicate with others to understand different perspectives and positions’. The second category consisted of the following seven codes: ‘Reconstruct dire situations and diversity in a positive manner’; ‘Develop ethical thinking with a sense of purpose’; ‘Find meaning and benefits in difficult situations’; ‘Find meaning in ethically challenging situations’; ‘Find meaning in ethical issues’; ‘Find meaning and value in the experience of ethically challenging situations’; and ‘Tackle ethically challenging situations in a positive manner’. The third category consisted of the following four codes: ‘Have professional ethical integrity’; ‘Have a professional responsibility as nurses to provide ethical care’; ‘Adhere to ethical standards when conducting professional duties’; and ‘Understand ethical responsibilities as professionals’. The fourth category consisted of the following four codes: ‘Decide what is the right thing to do by prioritising’; ‘Make professional decisions based on professional criteria, rather than personal views’; ‘Make definite decisions by conducting ethical analysis’; and ‘Use ethical reasoning to make normative decisions’.
Flexible and persistent approach
This attribute was synthesised from the following four categories: ‘Tackle ethical issues with courage’; ‘Attempt a flexible approach’; ‘Have confidence in tackling ethical issues’; and ‘Maintain initiatives without giving up’. The first category consisted of the following eight codes: ‘Recover from adversity and fear without succumbing to them’; ‘Act courageously for the sake of patients’; ‘Courageously express opinions in ethically challenging situations’; ‘Have the will and courage to accept responsibility for any wrong decisions made in retrospect’; ‘Pursue countermeasures without being overwhelmed by ethically challenging situations’; ‘Have the courage to face difficult situations’; ‘Speak out on ethical issues with courage’; and ‘Have the courage to act according to ethical principles despite adverse consequences’. The second category consisted of the following eight codes: ‘Successfully find alternative coping strategies’; ‘Eager to reconsider own perceptions and choices in difficult situations with others in a flexible and responsive manner’; ‘Adapt flexibly with a sense of humour’; ‘It is necessary to compromise with oneself and the situation to achieve the goals of nursing practice’; ‘A new method could be devised when one flexibly changes the perspective of the issue and redesign it’; ‘Broaden the scope of what is ethically permissible’; ‘Address ethical issues flexibly’; and ‘Gain new perspectives on ethical issues’. The third category consisted of the following five codes: ‘Have confidence in the ability to resolve ethical issues’; ‘Have confidence in responding to ethical issues in an effective way’; ‘Increase confidence in dealing with ethical issues’; ‘Feel well-prepared to resolve ethical conflicts’; and ‘Gain new perspectives in facing difficult ethical decisions in the future’. The fourth category consisted of the following six codes: ‘Take persistent action regarding ethical issues’; ‘Address ethical concerns persistently’; ‘Seek ethically correct action with persistence’; ‘Make adequate efforts to advocate effective solutions to ethical issues’; ‘Recognise when efforts to engage in ethical practice fall short’; and ‘Respond to ethical issues patiently and calmly’.
Collaboration to resolve ethical issues
This attribute was synthesised from the following three categories: ‘Communicate as a team’; ‘Use opportunities to consider ethical issues’; and ‘Use organisational system’. The first category consisted of the following eight codes: ‘Coordinate views, make suggestions, and negotiate through communication’; ‘Discuss ethical issues with the team’; ‘Bring ethical issues to the team leader’; ‘Support colleagues facing ethical dilemmas’; ‘Support colleagues in ethically challenging situations’; ‘Have a meaningful dialogue with those in various professions on ethical issues’; ‘Cooperate with those in various professions’; and ‘Raise concerns or suggestions regarding ethically problematic issues without fear of negative repercussions’. The second category consisted of the following six codes: ‘Participate in classes on ethics for leaders and teams’; ‘Participate in roundtable discussions on ethics, briefing sessions, and other events for expanding interdisciplinary understanding’; ‘Participate in regular events that address ethical issues’; ‘Seize opportunities to discuss ethical concerns, such as daily care rounds’; ‘Secure and use a space for ethical discussion’; and ‘Develop eagerness to act boldly on ethical issues’. The third category consisted of the following six codes: ‘Use coordinators to discuss with, and support, others involved in ethical issues’; ‘Use nursing leadership that suggests resources that provide support in ethically challenging situations’; ‘Understand organisational strategies to encourage inter-professional collaboration and accountability for ethical behaviour’; ‘Understand that the organisation is managed legally, ethically, fairly, and transparently’; ‘Use ethics consultation support’; and ‘Identify resources available for ethically challenging situation’.
Definition of ethical resilience
Based on the concept synthesis, nurses’ ethical resilience, a concept that represents a positive initiative regarding ethical issues oriented towards professional ethical behaviour, is defined as follows: the ability to sustain or restore professional practice competence in response to ethical issues while grasping the situation and working with others.
Virtual cases with the attributes of ethical resilience
According to the above four attributes of ethical resilience for nurses, we organised virtual cases. An exemplary case serves as a typical example of the application of the concept of ethical resilience, encompassing all of its defining attributes. Three additional types of cases are presented: a borderline case, containing most of the concept’s essential attributes but differing significantly in one attribute; a related case, including the concept under study but not containing all of the defining attributes and being connected in some way to the primary concept; and a contrary case, demonstrating that the concept is not the one being studied. 36 Each virtual case is explained based on the attributes of ethical resilience listed in Table 2.
Model case
Nurse A, aged in their 20s and in their third year of working as a nurse, felt there were issues with a certain situation. Deteriorating cognitive ability had been observed in Patient X, a male patient aged 70 years. He tended to sleep during the day, staying awake during the night, and had been using sleeping medication. To facilitate wakefulness during the day, Patient X was to sit in a wheelchair in the staff room for two hours after lunch. Nurse A had heard from Patient X that he found it excruciating to do so. Moreover, being in the staff room placed Patient X in an environment where the records of other patients, both electronic and on paper, were visible to him. Furthermore, Patient X’s sleeping pattern did not improve as he continued to be administered sleeping medication and asked to sit in a wheelchair. Nurse A considered the above situation problematic and brought up the matter with a senior nurse working in the same ward. This senior nurse responded that sitting in the wheelchair was to facilitate wakefulness in Patient X and that there was no problem with this as it was a decision made by the ward team. While Nurse A was unable to say anything at the time, they felt this was not the best nursing care to provide to Patient X and that the issue had to be handled professionally; thus, they did not ignore the problem but worked towards its resolution. First, they considered the situation to identify what constituted the problem based on their nursing experience thus far. Following this, they felt that the situation was problematic in light of the ethical code of conduct for nurses, which requires them to act in ways that support patient decisions in line with their wishes and values, handle personal information in appropriate ways, protect patients while guaranteeing their safety, and provide high-quality nursing care. They then proceeded to raise the issue at a team meeting in the ward. However, during this first meeting, Nurse A was met with the same opinion as when they previously raised the issue with the senior nurse; thus, no improvements were made to the situation. However, without giving up, Nurse A made adjustments to when they took their lunch break with the help of colleagues on days when they were in charge of Patient X so they could take the patient to places other than the staff room. They also made efforts to record the activities of Patient X during the day in great detail, including the use of sleeping medications and their effects. Furthermore, Nurse A participated in a training programme organised by the ethical consultation team at the hospital, where they brought up the case of Patient X. At this point, Nurse A adjusted the prescription of sleeping medication for Patient X while discussing it with doctors and pharmacists, and attempted to remedy the plan for the patient by bringing up the issue a second time at a team meeting where the ward managers would be present.
In the model case, Nurse A, in a situation where a plan for Patient X had been decided at the organisational level, did not follow the plan. Instead, she ‘grasped ethical issues’ based on her ‘integrity as a nurse’ to understand why the situation was problematic and implemented a solution. Nurse A initially raised the issue at a team meeting as a ‘collaboration to resolve ethical issue’, but no results were achieved. However, with her ‘integrity as a nurse’, she took a ‘flexible and persistent approach’, starting by intervening in areas where change could be brought about, and continued to work on resolving the problem. After utilising the department within the organisation that handles ethical issues and collaborating with other professionals, she again raised the issue at a meeting as a ‘collaboration to resolve the ethical issue’. In this way, she attempted to improve the plan decided for Patient X.
Borderline case
Nurse B, aged in their 20s and in their second year of working as a nurse, considered a certain situation problematic. Deteriorating cognitive ability had been observed in Patient X, a male patient aged 70 years. He tended to sleep during the day, staying awake during the night, and had been using sleeping medication. To facilitate wakefulness during the day, Patient X was to sit in a wheelchair in the staff room for two hours after lunch. Nurse B had heard from Patient X that he found it excruciating to do so. Moreover, being in the staff room placed Patient X in an environment where the records of other patients, both electronic and on paper, were visible to him. Furthermore, Patient X’s sleeping pattern did not improve as he continued to be administered sleeping medication and asked to sit in a wheelchair. Nurse B considered the above problematic and adjusted the prescription of sleeping medication for Patient X while discussing it with doctors and pharmacists. The nurse also attempted to remedy the plan for Patient X by bringing up the issue at a team meeting. However, during this meeting, Nurse B was met with the same opinion as when they previously raised the issue with the senior nurse, and thus, feeling unmotivated with the situation at hand, stopped trying to deal with the plans for Patient X.
In the borderline case, Nurse B, based on her ‘integrity as a nurse’, understood the ethical issues and implemented solutions, explaining why the situation was problematic. Then, as part of her ‘collaboration toward resolving the ethical issue’, Nurse B contacted the organization’s ethical affairs department, coordinated with other experts, and raised the issue at a meeting. However, because she did not receive support from others for her proposed changes to Patient X’s treatment plan, Nurse B was unable to ‘find meaning and purpose in the difficult situation’ and demonstrate ‘flexible and persistent approach’ in her ‘integrity as a nurse’, and gave up on further changes. Therefore, in this case, Nurse B was unable to sustain her ‘integrity as a nurse’ and demonstrate ‘flexible and persistent approach’. This does not demonstrate the resilience essential to this concept.
Related case
Nurse C, aged in their 20s and in their first year of working as nurse, was worried they were unable to perform interventions satisfactorily regarding a certain patient. Deteriorating cognitive ability had been observed in Patient X, a male patient aged 70 years. He tended to sleep during the day, staying awake during the night, and had been using sleeping medication. To facilitate wakefulness during the day, Patient X was to sit in a wheelchair in the staff room for two hours after lunch. Nurse C had heard from Patient X that he found it excruciating to do so and felt they were unable to follow through with the patient’s wishes. They brought up their concerns with a senior nurse working in the same ward. This senior nurse responded that sitting in the wheelchair was to facilitate wakefulness in Patient X and that this could not be helped as it was necessary. While this did not alleviate Nurse C’s concerns, they felt somewhat relieved after consulting their senior. However, they continued to feel sorry for Patient X, and at a multidisciplinary meeting, they brought up the patient’s treatment plan, asking if it were possible to reduce the two hours spent in a wheelchair by an hour and allow the patient to lie in bed depending on the situation.
In the related case, Nurse C sympathised with Patient X and was disappointed that she could not prioritise the patient’s wishes. This indicates that ‘personal integrity’ took precedence over ‘nursing integrity’.5,7,9 Although her feelings were temporarily alleviated by consulting with a colleague to resolve the situation, Nurse C did not give up. Instead, she used a ‘flexible and persistent approach’ to raise the issue again at the interprofessional meeting and attempted to intervene to accommodate Patient X’s request to remain in bed. This approach to the interprofessional meeting was based on ‘relational integrity’ rather than ‘collaboration to resolve ethical issues’ because it lacked ‘grasping ethical issues’. In this case, Nurse C demonstrated resilience and persistence in responding, but it was based on ‘personal integrity’ rather than ethical considerations.5,7,9
Contrary case
Nurse D, aged in their 30s and in their 15th year of working as a nurse, was in charge of Patient X, a male patient aged 70 years who tended to sleep during the day and stay awake at night. The patient was prescribed sleeping medication and had been observed as having deteriorating cognitive ability. Patient X was to sit in a wheelchair for two hours after lunch in the staff room to facilitate wakefulness. Even when Patient X expressed to Nurse D that it was excruciating to sit in the wheelchair, they told the patient that it was a decision made by ward staff and because it was necessary, they hoped he could endure it. Nurse D continued to administer the said treatment plan.
In the contrary case, Nurse D was observed to have lacked ‘nursing integrity’ and not interacted appropriately with Patient X. Nurse D also did not appear to have ‘grasping ethical issues’ regarding the patient’s treatment plan. Because Nurse D was unable to identify the ethical issues, no steps were taken to address the issues, and the treatment plan continued without any further approach.
Discussion
This study undertook conceptual synthesis of ethical resilience to advocate for the use of the concept in nursing. We synthesised the four attributes of ethical resilience: ‘Grasping ethical issues’; ‘Integrity as a nurse’; ‘Flexible and persistent approach’; and ‘Collaboration to resolve ethical issues’.
The first attribute, ‘Grasping ethical issues’ has the following categories: ‘Reflect on the ethical issue experienced’ and ‘Analyse issues from an ethical perspective’. These categories consist of experiential learning that becomes necessary when addressing ethical issues, including codes that indicate theoretical analysis based on the knowledge and framework of ethics. These codes incorporate elements such as self-reflection and the accompanying situational awareness necessary for resilience. They also indicate the need to recognise and examine ethical issues, explaining their structure, and responding to them with evidence as means of demonstrating resilience to ethical issues. Therefore, ‘grasping ethical issues’ means that one must not only understand them but also grasp and judge them so that they can be revisited and analysed.
The second attribute, ‘Integrity as a nurse’, included the following categories: ‘Understand diverse values’, ‘Find meaning and purpose in ethically challenging situations’, ‘Recognise the professional role’, and ‘Make decisions on ethical grounds’. Nurses are aware of their professional role and responsibility to provide care to patients. When they face ethical problems in practice, they find meanings and purposes as professional nurses. In addition, the ethical issues nurses encounter are a mixture of medical and patient values, which require professional and objective understanding. These values must be organised and addressed from an ethical perspective as a nurse. Therefore, ‘integrity as a nurse’ suggests that nurses find meanings in ethical issues and approach them with professionalism and responsibility.
The third attribute, ‘Flexible and persistent approach’, contained the categories of ‘Confront ethical issues with courage’, ‘Attempt a flexible approach’, ‘Have confidence in tackling ethical issues’, and ‘Maintain initiatives without giving up’. Maintaining initiatives without giving up and being flexible are important elements of resilience. The core element of resilience is the power to rebound or the ability to continue as planned. This power is also described as ‘adapting well’ or ‘bouncing back’, processes that characterise resilience.17–19 Note that nurses’ resilience describes the resilience of individuals with a nursing background. 21 This presents a sustained, rather than temporary, force. Simultaneously, flexibility indicates suppleness or the ability not to concede. These are important elements as nurses continue to respond to issues. Flexibility in handling ethical issues is also expressed in the codes; it involves finding ways to cope, changing responses to various issues, and at times compromising in certain situations. Therefore, ‘flexible and persistent approach’ means not only persistent and continuous efforts but also skilful initiatives from diverse perspectives, performed in clinical settings by nurses as a professional.
The fourth attribute, ‘Collaboration to resolve ethical issues’, had the following categories: ‘Communicate as a team’, ‘Use opportunities to consider ethical issues’, and ‘Use the organisational system’. This attribute serves as a reminder that sociable attitudes and positive relationships/social support are also among the requirements of resilience. This category includes codes such as ‘Support colleagues in ethically challenging situations’, ‘Understand different perspectives and positions’, and ‘Communicate through appropriate dialogue and interaction’. The nature of ethical issues is such that many remain unresolved and few can be handled by individual nurses. Hence, support is needed from colleagues and those in various other professions. Furthermore, communication is required to deepen understanding within the team based on sociable attitudes and positive human relations. Other codes include ‘Participate in roundtable discussions on ethics, briefing sessions, and other events for expanding interdisciplinary understanding’, ‘Use coordinators to discuss with and support others involved in ethical issues’, and ‘Identify resources available for ethically challenging situations’. Since few ethical issues can be handled by individual nurses alone, as mentioned, it would be easier to work as a team if the organisation offers regular ethics training, hosts ethics conferences, and provides resources that allow members to discuss ethical issues. Seizing and utilising such opportunities would facilitate social support, which is an attribute of resilience. Thus, ‘collaboration to resolve ethical issues’ means that ethical issues are addressed through communication with people from various professions, such as team discussions and using organisational systems.
In the process of conceptual integration concerning ethical resilience of nurses, it was also found out that nurses’ ethical resilience is part of the basic concepts of resilience in general and moral resilience, especially in terms of ‘flexible and persistent approach’. Based on this underlying concept of resilience, ethical resilience can be considered a higher-level concept than moral resilience, as a type of resilience shown by professionals (Figure 2). Relational model of resilience, moral resilience, and ethical resilience.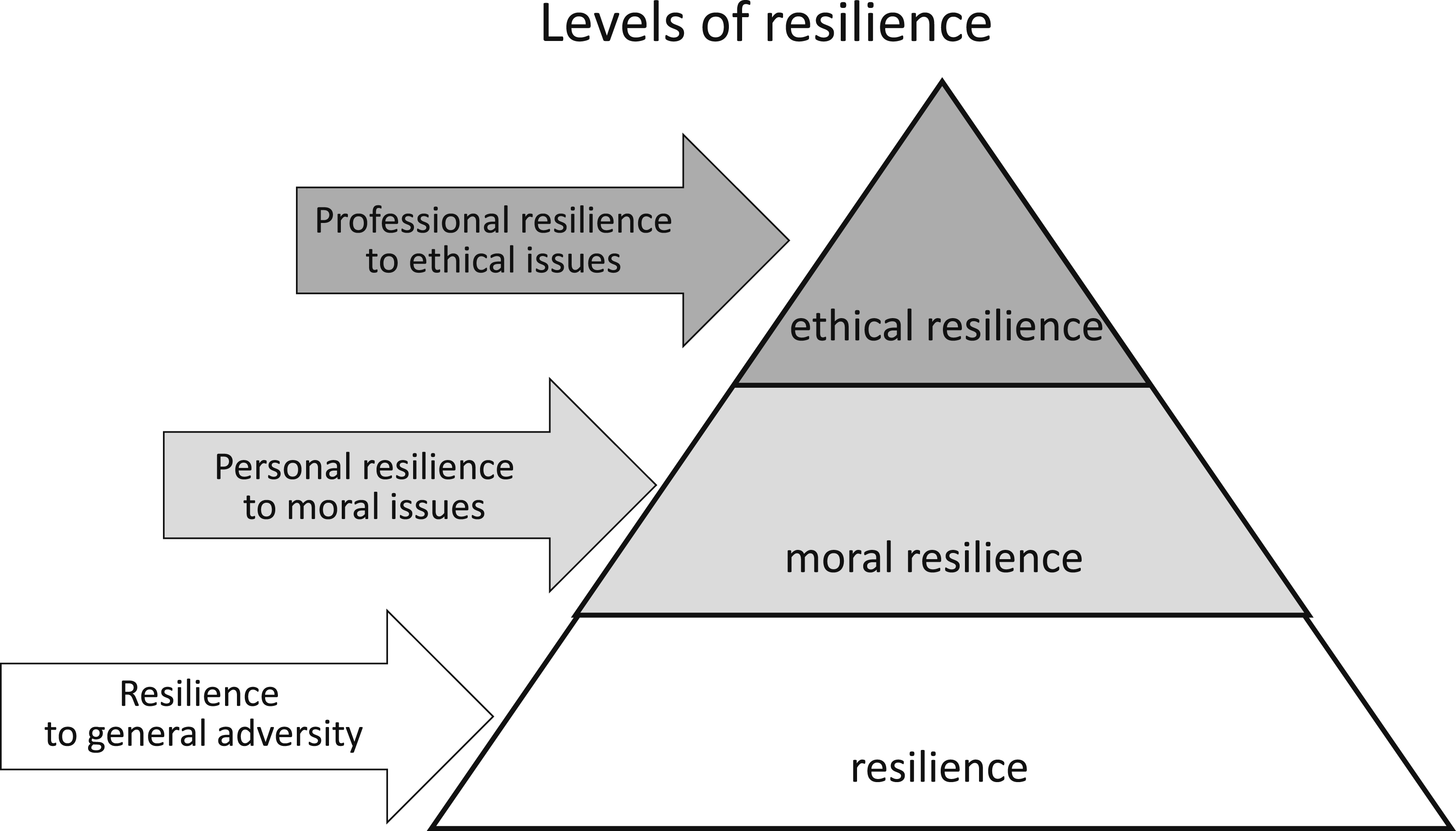
Using the four attributes, we wrote four types of virtual cases. These cases describe clinical situations with ethical problems in detail, which could help actual nurses in practice to understand and judge what they performed was ethical or not as a professional. For example, as shown in the related case, if nursing is practiced solely based on personal integrity, it becomes difficult to clarify the ethical issues inherent in the situation. Nurses are professionals, and nursing practice is the practice of ethics. Therefore, nurses must address the ethical issues they encounter in various clinical experiences. Unless they demonstrate ‘integrity as a nurse’ as professionals and recognise and persistently address ethical issues, as shown in the related and contrary cases, the quality of nursing cannot be guaranteed. This is why specialised ethics education is provided. Ethical resilience can be enhanced through ethics education. In this respect, the four attributes in this study, including the 13 categories, could be criteria for judging what ethical resilience is like, which may protect nurses in practice from collapsing due to heavy burden of duty with various ethical issues in clinical settings.
So far as we have performed searches for literature, this study is the first attempt to conduct concept synthesis of ethical resilience in nursing. Thus, the present study has limitations. Research on resilience related to ethical issues and moral distress is still in its infancy. Similar to moral resilience, ethical resilience requires further exploration. Since its introduction, studies on ethics abound; however, there is confusion between morality and ethics because few researchers clearly distinguish the two. For example, one study discusses the difference between morality and ethics, stating that ‘moral sensitivity’ is a genuine concern for the other person while ‘ethical sensitivity’ relates to the knowledge of ethical theories and principles. 23 Essentially, the term ‘ethics’ is more appropriate when used in relation to the professional values held by individual nurses or organisations. Therefore, it is important to clarify the meaning of these terms and concepts to eliminate confusion in academic research. These issues, along with the concept of ethical resilience, require further discussion and empirical research, such as collecting narratives of nurses in practice with experiences of ethical problems. Cultural aspects should also be examined and considered to evaluate and validate the concept of ethical resilience with the four attributes. For example, in Japan, there is a cultural background in which morality is used in an individual capacity and ethics is considered the way and order between people.24,25 The Japanese Nursing Association 26 further stated that ‘morality is often used for small groups such as individuals and families, whereas ethics is used more broadly, spanning from individual relationships to society’ and that ‘morality is often used as a standard for behaviour in daily life, but it cannot be a standard for decisions such as the direction of treatment in medical settings’. Morality is important in nursing, but it is a standard of value that we hold as worldly individuals, and when we make various decisions as professional nurses, we need to consider ethics as a standard of value that we hold as an organisation. This perspective may also support the idea that it is more appropriate to use the term ‘ethical resilience’ than ‘moral resilience’ when discussing nurses’ efforts to tackle ethical issues in their professional capacity or when aiming for the acquisition of resilience in ethics education for nurses.
When one demonstrates ethical resilience, one can maintain ethical behaviour without being overwhelmed by ethical issues. Ethical behaviour prevents one from acquiescing to ethical issues, compels one to manage them appropriately, and allows one to maintain this ethical behaviour.27–29 Accordingly, the distress caused by ethical issues is mitigated,5,29,30 enabling one to avoid burnout.28,31 Simultaneously, ethical behaviour, if maintained, can lead to the resolution of ethical differences with those in other professions and help achieve organisational harmony.27,32 This facilitates an environment conducive to ethical behaviour.3,33 Thus, resilience is regarded as a positive concept in handling adversity, and ethical resilience enables positive practices in a challenging situation and helps improve it.
An individual must be a good person to become a good nurse. It has been argued that the nature of the profession is such that individual personality traits are strongly reflected in one’s nursing practice.6,34 However, while general moral education improves individual character, it cannot be considered professional education. Professional ethical education is necessary to encourage nurses to confront ethical issues and act ethically. It is hoped that this ethical education for nurses may prevail and contribute to equipping them with ethical resilience, protecting them in practice and producing quality of care to patients.
Footnotes
Acknowledgement
I would like to express my gratitude to Associate Professor Shinji Miyauchi of the Linguistics Laboratory at Oita Prefectural University of Nursing and Health Sciences for his advice on the linguistic structure of this paper.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by JSPS KAKENHI Grant Number JP 24K13584.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
