Abstract
Background
The use of assisted reproductive technology (ART) in individuals with intellectual disabilities raises significant ethical tensions between reproductive autonomy and the welfare of future offspring. Global guidelines addressing this dilemma remain absent. In China, nurses frequently encounter these dual responsibilities without clear operational frameworks.
Aim
To explore how nursing interventions can support ethical decision-making and reproductive safety for an intellectually disabled patient undergoing ART.
Design
A qualitative, exploratory single-case study.
Methods
The study followed a 27-year-old woman with mild intellectual disability through an in vitro fertilization (IVF) pathway. A nurse-led dual-intervention strategy was implemented: (1) cognitively adaptive decision-making tools (pictogram-based IVF guides, emoji risk charts, visual medication calendars); and (2) government-integrated perinatal care services, including prenatal registration, structured follow-up, and postpartum home visits.
Ethical Considerations
Ethical approval was obtained, and the study adhered to strict ethical standards, including a tailored informed consent process and robust guarantees of confidentiality.
Findings
The intervention ensured informed consent completion, medication adherence without errors, and comprehensive prenatal tracking via the national maternal health system. The patient delivered a healthy infant (Apgar score = 10). These outcomes demonstrate that nurse-designed cognitive adaptations, combined with systemic safeguards, enhance patient autonomy and reproductive safety.
Conclusion
This study illustrates an ethical and practical paradigm for reconciling reproductive justice and cognitive equity in ART. Nurse-led innovations, supported by institutional governance, may inform global frameworks for ethically complex fertility care.
Keywords
Introduction
The application of assisted reproductive technology (ART) in individuals with intellectual disability (ID) remains mired in ethical dilemmas balancing reproductive self-determination and offspring welfare protection, amid the absence of globally standardized practice guidelines. This regulatory void imposes dual practice dilemmas on nursing professionals: upholding reproductive self-determination rights under the CRPD while addressing parenting risk assessments complicated by impaired decision-making capacity. 1 International practices diverge sharply, ranging from mandatory parenting assessments in some nations to outright treatment bans in others,2,3 exposing fundamental cultural conflicts between individual rights and social responsibilities. Within China’s tiered healthcare system, nurses serve as pivotal executors translating ethics committee directives into clinical practice, establishing end-to-end ethical governance from treatment decision-making to postpartum care through cognitive accessibility innovations.
Although ART has provided fertility solutions to hundreds of millions globally, its application in intellectually disabled (ID) individuals ignites fundamental ethical tensions between reproductive self-determination (Article 23, CRPD) 4 and children’s right to appropriate care (CRC). 5 Affecting 1% of the global population 6 ID reproductive health needs remain neglected 7 —a persisting gap even after the CRPD’s ratification by 185 countries. This dilemma embodies the philosophical clash between Nussbaum’s capabilities justice (prioritizing reproduction as core human capability for dignity) and Rawlsian intergenerational equity (advocating “just savings” for future generations),8,9 manifesting in polarized practices: mandatory parenting competency assessments in the UK/Australia,10–12 whose ethical foundation emphasizes maximizing offspring welfare and risk prevention, but which in practice may constitute procedural barriers to the reproductive rights of individuals with ID, implicitly reflecting an assumption of ableism; legislative reproductive restrictions for severe ID in Nordic states,13,14 which reflect strong elements of social paternalism and utilitarianism, explicitly limiting individual rights for the sake of collective or intergenerational interests—an approach that directly conflicts with the equal-rights principles enshrined in the CRPD; and autonomy-focused social support systems in the US,15,16 which emphasize individualistic autonomy supported by legal protections and community-based services, yet face implementation challenges due to inequities in the social safety net. 17 These international differences reveal the core ethical tension between individual rights (autonomy) and social responsibilities (protection) in the context of ART for individuals with ID, with each country’s policy effectively seeking a different balance point along this spectrum.
China’s unique approach, grounded in the Revised Disabled Persons Protection Act and spousal guardianship priority (Civil Code Article 34), provides robust legal protection for ID reproductive rights, yet confronts three implementation barriers: standardized assessment gaps, professional bias, and insufficient social supports. Innovative practices at Guangzhou Women and Children’s Medical Center demonstrate how nurses, serving as cultural mediators between familial expectations and bioethical requirements, establish ethical equilibrium through leadership in continuous cognitive assessment, decision-support provision, and interdisciplinary coordination—repositioning nurses as central ethical agents in clinical decision-making and offering a novel paradigm for global nursing ethics.
Case scenario
This case was purposefully selected for in-depth analysis because it typifies the multidimensional challenges faced by women with mild intellectual disability when seeking assisted reproductive technologies (ART). Specifically, it illustrates the interplay of cognitive limitations, ethical deliberations, and systemic support mechanisms. As such, the case provides an information-rich and illustrative exemplar for exploring a nurse-led, dual-pathway intervention framework that integrates cognitive adaptation with system-level safeguards. Ms L is a 27-year-old married woman who has been struggling with primary infertility for 6 years. Diagnosed with mild intellectual disability in childhood, she can manage basic self-care and communicates fluently in Mandarin and her local dialect. Despite these abilities, her cognitive limitations sometimes make complex decisions difficult.
In May 2023, hospital assessments confirmed her condition: her WAIS-IV test showed a full-scale IQ of 52, with verbal and performance scores of 54 and 57, respectively. She scored 19 on the Activities of Daily Living (ADL) scale, indicating a slight decline in daily functioning, and five on the Social Disability Screening Schedule (SDSS), confirming mild social impairment. Genetic testing later revealed no hereditary cause of her disability.
Her husband, however, faced severe oligoasthenospermia, leaving the couple with little chance of natural conception. The medical team proposed intracytoplasmic sperm injection (ICSI) as the only viable option. Before proceeding, geneticists ruled out significant genetic risks and decided that preimplantation genetic testing was unnecessary.
The case was presented to the hospital ethics committee and received unanimous approval (12:0), as it reflected a critical question: how can healthcare providers balance Ms L’s right to become a mother with concerns about her capacity for parenting? To support her, nurses and specialists worked together, using simplified explanations and repeated counseling sessions to ensure she understood each step. The team also created a personalized prenatal care plan to safeguard both maternal and fetal well-being.
Method
We implemented a nurse-led dual-pathway framework designed to safeguard informed decision-making and continuity of care for patients with intellectual disability undergoing ART. Given the patient’s cognitive limitations, ensuring truly informed consent was paramount. We therefore implemented an ongoing, adaptive consent process. First, specially designed pictogram-based guides and emoji-based risk charts were used to repeatedly explain treatment steps, potential risks, and patient obligations in an accessible manner. Second, nurses continuously assessed the patient’s comprehension throughout the treatment course and reconfirmed her consent at critical decision points (e.g., initiation of ovarian stimulation, pre-embryo transfer). Third, in accordance with the Civil Code of the People’s Republic of China, her spouse, as the legal guardian, was fully engaged in all communications and co-signed the written informed consent documents. Regarding the publication of this study, the same adaptive communication strategies were applied, and both the patient and her spouse provided permission for the anonymized case details to be reported.
Ethical considerations
This study was conducted in accordance with the ethical standards outlined in the Declaration of Helsinki and received formal approval from the Institutional Review Board of Guangzhou Women and Children’s Medical Center Liuzhou Hospital (Approval No.: Expedited-Research-2025-144). Ethical considerations, particularly regarding informed consent and confidentiality, were paramount given the vulnerable nature of the participant.
Informed Consent: An ongoing, adaptive consent process was implemented, tailored to the patient’s cognitive abilities. Specially designed pictogram-based guides and emoji-based risk charts were used to repeatedly explain the treatment steps, potential risks, and benefits in an accessible and comprehensible format. The patient’s understanding was continuously assessed by the nursing team, and her consent was reaffirmed at all critical decision points. In line with the Civil Code of the People’s Republic of China, her spouse, acting as her legal guardian, was fully involved in all communications and co-signed the written informed consent documents for both the medical treatment and the publication of this anonymized case study.
Confidentiality: To safeguard privacy, all personal identifiers were removed from the data collected. The patient is referred to by a pseudonym (“Ms L”) throughout the manuscript. All research data, including interview transcripts, clinical notes, and ethics committee documents, are securely stored on password-protected institutional servers accessible only to the core research team. The anonymity and confidentiality of the patient and her family have been rigorously maintained throughout the research and publication process.
Phase 1: Cognitive-adaptive decision-support tools
Recognizing the patient’s limited cognitive capacity, reproductive nurses developed tailored tools to transform complex ART information into cognitively accessible formats, thereby enhancing understanding, reducing anxiety, and promoting shared decision-making. Key tools included: 1. Pictogram-Based IVF Process Guide (“IVF Theme Park Map”), which restructured IVF stages into a sequential, visually engaging storyline to improve memory retention (Figure 1). 2. Emoji-Based Risk Alert System, enabling the patient to self-report symptoms and interpret ART-specific risks through an intuitive three-tier emoji scale (Figure 2). 3. Visual Medication Calendar, which combined graphical drug identifiers with a structured schedule to ensure medication adherence under caregiver supervision (Figure 3). Pictogram-based IVF process guide (“IVF theme park map”). Note. Visual tool depicting the multi-step IVF process through a theme-park narrative to facilitate patient comprehension and reduce procedural anxiety. Icons represent each treatment stage sequentially, enabling recall for patients with cognitive limitations. Emoji-based alert system. Note. Three-tier emoji scale used to communicate ART-specific risks and symptom severity (Smiling Face: safe; Frowning Face: vigilance required; Crying Face: urgent care). Designed to support patient self-reporting and caregiver-assisted monitoring. Visual medication calendar Note. Color-coded calendar integrating graphical identifiers for each drug and scheduled administration times, ensuring accurate medication adherence under family supervision with remote nurse guidance.
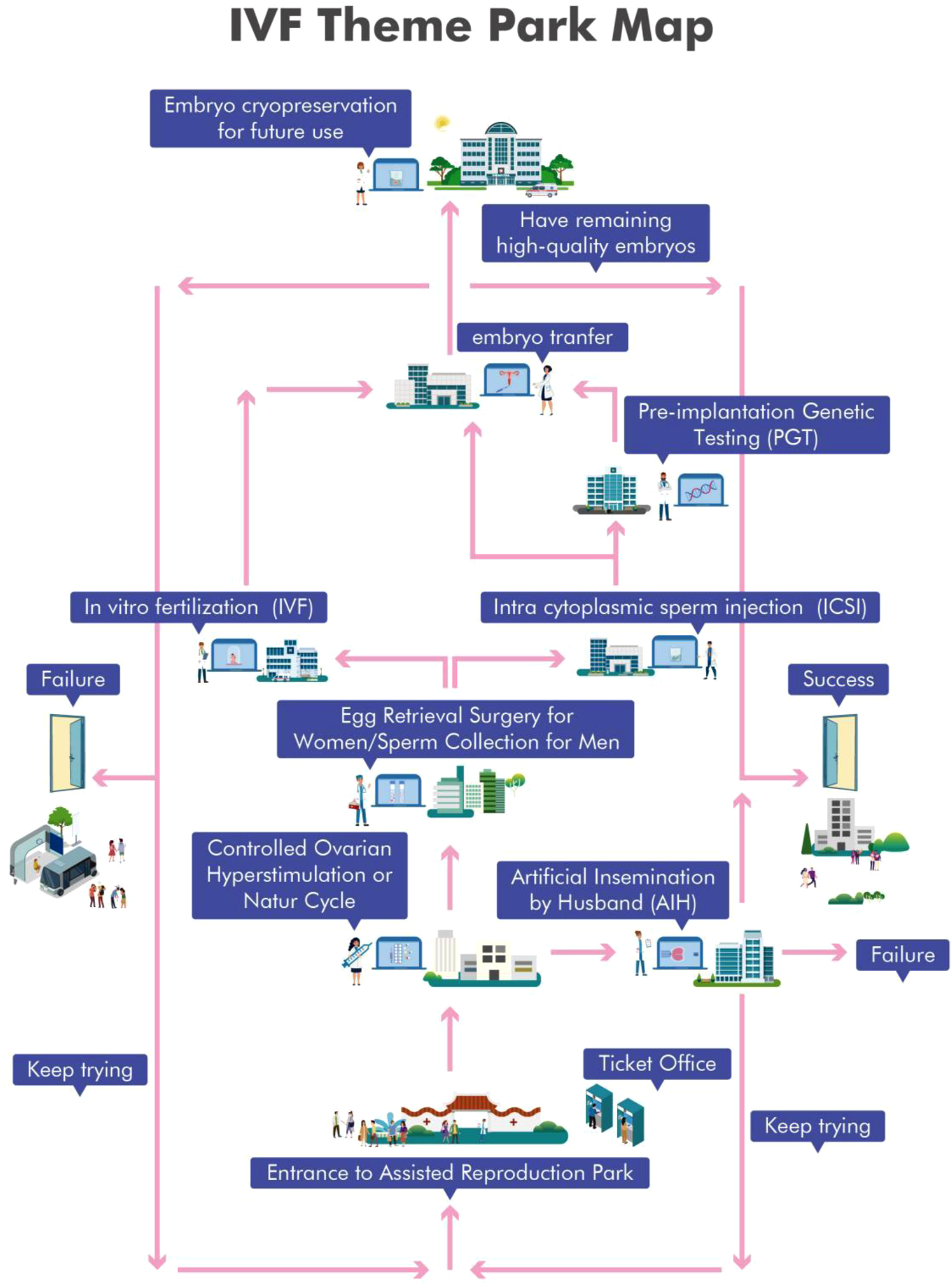

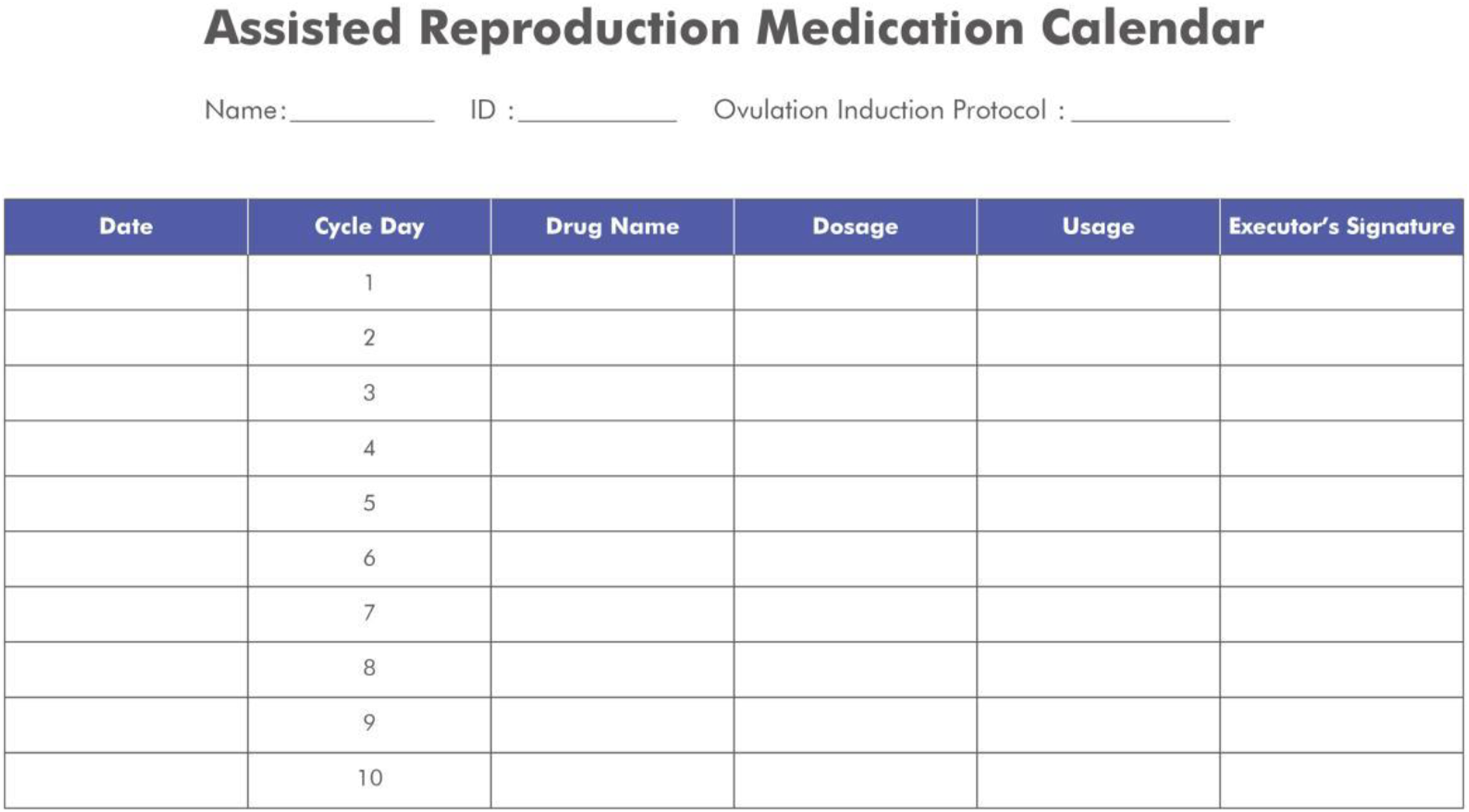
These innovations supported autonomy within the patient’s cognitive limits while minimizing safety risks and reducing nursing burden.
Phase 2: Integration with government-funded perinatal care
Following embryo transfer and confirmation of fetal cardiac activity, care transitioned to a government-funded perinatal closed-loop system in line with China’s National Basic Public Health Service Specifications. Reproductive nurses initiated an electronic referral to the local maternal and child health network, ensuring continuity of antenatal and postnatal care.
A risk assessment classified the pregnancy as Level II (“yellow”) due to factors including ART conception and mild intellectual disability, triggering enhanced supervision and tailored follow-up. Designated nurses coordinated high-risk monitoring and provided caregiver education to ensure adherence to recommended check-ups and interventions.
The patient completed standardized antenatal visits, underwent targeted risk-based assessments, and ultimately delivered a healthy infant at term via spontaneous vaginal delivery. Postnatal follow-up, including home visits and community-based evaluations, confirmed satisfactory maternal recovery, adequate newborn care, and strong family support, closing the care loop.
Multiple data sources were triangulated to enhance methodological transparency and validity. These included: (1) semi-structured interviews with the patient and her spouse to capture their decision-making process and subjective experiences; (2) clinical observation records documented by the primary nursing staff, detailing comprehension, medication adherence, and emotional fluctuations; (3) meeting minutes and related deliberation documents from the hospital ethics committee; and (4) the patient’s electronic medical records, encompassing the entire ART treatment process and perinatal healthcare data.
Results
Ethical deliberations and resolution
The ethics committee identified several critical tensions in this case: concerns that reduced parenting capacity could compromise child development under the “protection of offspring” principle; the dichotomy between fulfilling reproductive autonomy and mitigating potential long-term caregiving burdens; societal considerations regarding resource allocation for special education and social services under the principle of social beneficence; and questions regarding the validity of informed consent given possible limitations in understanding ART-related risks and maternal responsibilities. Additional issues included balancing reproductive rights with diminished decision-making capacity and ensuring distributive justice in healthcare resource allocation.
Grounded in the ethical principles outlined in China’s Regulations on Human Assisted Reproductive Technology and following multiple rounds of rigorous deliberation, the committee unanimously concluded that the patient’s reproductive autonomy should be upheld under strict conditions. These conditions include verified informed consent, structured family education, and the establishment of formal social support systems.
To ensure ethical integrity during implementation, the committee mandated: (1) the use of accessible and visual consent tools to enhance patient comprehension and participation; (2) continuous capacity assessment and dynamic risk monitoring throughout treatment; (3) an emergency response protocol to address unforeseen complications; and (4) adherence to a tiered maternal health management system after conception, consistent with national standards. Collectively, these measures aim to safeguard patient rights, protect offspring welfare, and provide humane, ethically sound care for individuals with intellectual disability seeking ART.
Validation of collaborative intervention outcomes
The nurse-led dual-pathway framework—combining cognitively adaptive decision-making tools with China’s tiered perinatal service system—effectively mitigated ethical challenges in ART implementation for individuals with intellectual disability. At the cognitive support level, pictogram-based treatment guides, emoji-based risk alerts, and visual medication calendars enhanced procedural understanding and adherence across the ART continuum, from ovarian stimulation to embryo transfer and luteal support. These strategies enabled consistent medication compliance and reduced decisional anxiety, while ensuring guardian-informed consent through structured, accessible communication.
At the systemic level, integration with a closed-loop perinatal care pathway facilitated continuous high-risk pregnancy monitoring via regional health information platforms, supported by government-funded antenatal services. This collaborative approach safeguarded maternal and neonatal health while maintaining equity in service access.
Together, these interventions illustrate how cognitive empowerment strategies, combined with institutional safeguards, can uphold reproductive autonomy and minimize risks associated with cognitive limitations, offering a scalable model for ethically responsible ART in vulnerable populations.
Discussion
Persistent gaps in reproductive rights for women with ID
Globally, women with intellectual disabilities experience structural inequities in reproductive health, including inadequate information, coercive practices, and sociocultural biases that undermine autonomy.18–22 These barriers persist within healthcare systems through communication failures and provider bias,23,24 restricting access and violating dignity. 25 Our case illustrates how these challenges can be addressed through structured decision-support and integrated care pathways.
Operationalizing public health ethics
China’s tiered maternal health system exemplifies how reproductive rights can move beyond declarative principles toward actionable safeguards. By coupling universal service packages with differentiated high-risk management, the system operationalizes justice principles by prioritizing vulnerable populations, thereby embodying a practical application of Rawls’ difference principle, which requires that inequalities benefit the least advantaged. 8 Classifying the patient into the yellow high-risk category and providing intensified follow-up concretely illustrates this institutional redistribution toward vulnerable groups, aiming at reproductive justice through structured differentiation. Integration with digital monitoring further reduces implementation gaps, ensuring continuity of care while protecting offspring welfare. Beyond clinical care, the closed-loop model redefines autonomy as supported decision-making, embedding structured ART access within state-funded maternal health services. By transforming ethics committees from restrictive gatekeepers to facilitators of informed care, this approach shifts reproductive rights from abstract concepts to practical empowerment.
While China’s institutionalization of reproductive rights is effective, the deeper value of the “nurse-led dual-pathway framework” lies in its two core principles—cognitive adaptation and systemic integration—which possess global relevance. Its applicability depends on local adaptation rather than replication. For example, in the UK, 26 systemic integration could connect ART care with community learning disability nurse services; in the US, 27 cognitive-adaptive tools could be advanced by digital health enterprises and incentivized via insurance; in resource-limited settings, intra-hospital multidisciplinary ART ethics teams could simulate integration. Thus, the framework offers a modular approach: cognitive adaptation can independently enhance informed consent quality, while systemic integration can inspire context-sensitive strategies that anchor ART within existing public health or social infrastructures.
Reconstructing nursing ethics: From compliance to moral agency
This case highlights a shift from proxy decision-making toward relational, cognition-sensitive care. Pictogram guides and emoji-based alerts reframe informed consent as an interactive process, reflecting care ethics’ emphasis on contextual responsiveness and substantive autonomy. 28 The cognitive-adaptive tools also resonate with Nussbaum’s capabilities approach, 9 which stresses enabling individuals to realize basic human capabilities. For women with intellectual disabilities, reproductive capability is often constrained by communication barriers. These tools dismantle such barriers, empowering patients to understand and participate, thus supporting reproductive dignity in practice. Nurses assumed an active moral role—bridging cognitive gaps, fostering tripartite consensus, and embedding ethical principles into every clinical step—illustrating ICN’s mandate for advocacy and justice in vulnerable populations.29,30 This repositioning transforms nurses from procedural implementers into ethical agents capable of shaping systemic equity in reproductive healthcare. Throughout the process, nurses embodied the essence of care ethics, 28 acting not as passive implementers but as moral agents who built supportive relationships and ensured that ethical principles were applied in a contextualized and compassionate manner.
Study limitations and future directions
Despite positive outcomes, several limitations remain. First, the intervention relied heavily on spousal support, raising concerns about applicability to patients lacking stable family support. Second, the effectiveness of cognitive-adaptive tools may be culturally constrained, as visual symbols require local adaptation. Third, China’s tiered maternal health system provided unique institutional support; in regions without such infrastructure, intra-hospital multidisciplinary teams may be needed to approximate integration. Finally, as a single-case study, generalizability is limited, requiring validation in larger, comparative samples.
Conclusion
This study demonstrates that integrating cognition-adaptive tools with system-level safeguards can uphold reproductive autonomy without compromising offspring welfare. By embedding ethical principles into communication and care continuity, nurse-led frameworks offer a scalable model for equity in ART for intellectually disabled populations. This case therefore contributes not only to the Chinese context but also to a broader global dialogue on reproductive justice for women with intellectual disabilities. Future research should include multi-center, multi-sample case studies to validate generalizability, and cross-national comparative studies to examine contextual adaptation across diverse healthcare systems. Cognitive-adaptive tools (e.g., pictograms, calendars) also hold potential for digital translation into interactive applications, whose usability and effectiveness should be systematically evaluated. Finally, embedding such strategies into nursing education and policy frameworks will be essential for advancing reproductive health equity at systemic levels.
Footnotes
Acknowledgments
We are grateful for the clinical support provided by all medical staff at Guangzhou Women and Children’s Medical Center and Liuzhou Maternal and Child Healthcare Hospital. We also sincerely appreciate the trust and dedication of the patient and her family participating in this study toward the scientific research endeavor.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
