Abstract
Background
The shortage of skilled healthcare workers, intensified by demographic change, has stimulated interest in robotic solutions for elderly care. While assistive robots typically perform practical tasks, socially assistive robots (SARs) are increasingly taking on communicative and relational roles, raising ethical concerns. Critics fear that SARs will disrupt the professional caregiver–client relationship and replace, rather than complement, human workers.
Aim
This study explores how SARs influence the professional care relationships and the professional self-understanding.
Research design
A qualitative interpretive study design.
Participants and research context
Using a constructivist grounded theory approach, we analyzed twelve semi-structured interviews with professional caregivers experienced in using SARs in Germany and four additional interviews with stakeholders involved in their development and implementation (2023–2024).
Ethical considerations
The study was approved by the Ethics Committee of the University of Potsdam (No. 84/2022).
Results
Caregivers initially feared that SARs would replace the relational and emotional dimensions of care. However, practical experience changed their perspective. Instead of seeing SARs as substitutes, caregivers came to view them as part of a triadic care model involving the caregiver, the client, and the robot. This model reinforces the central role of caregivers in integrating SARs while maintaining emotional and relational care. SARs were accepted as tools to reduce physical workload, but caregivers emphasized that emotional support and relationship-building must remain human tasks.
Conclusion
Using SARs reshapes the perspective of caregivers, fostering a triadic relationship in which they remain central. They act as mediators, ensuring that SARs function as supportive tools rather than substitutes. Caregivers set ethical boundaries, prioritizing human empathy and relational care. This evolving role highlights the continued importance of the human presence in care, even as robotic technologies advance.
Introduction
Care and nursing are commonly associated with “tender love,” a deeply human and emotional practice that is often contrasted with the perceived rationality and coldness of technology. 1 Nonetheless, technology has always played an important role in healthcare, facilitating medical interventions, monitoring patients, and improving the efficiency of care.2–4 However, the introduction of robotic technology raises new ethical and philosophical questions about the relationship between care and technology within human interaction. This is particularly relevant in elderly care, where socially assistive robots (SARs) are designed to provide not only practical assistance but also companionship and emotional interaction.
The aim of this study is to explore the impact of SARs on caring relationships and professional self-perception in inpatient elderly care. Specifically, it analyzes how professional caregivers perceive SARs, how they conceptualize their own roles and those of the SARs within their caring relationships, and how they establish ethical boundaries around the use of such technologies. Our findings reveal a transition from a dyadic to a triadic model of care. Understanding this shift is important, as it reveals how care practices and professional self-perception evolve alongside technological innovation.
Background
SARs are embodied tools aimed at assisting older adults through companionship and daily activity support.5,6 Their design often incorporates anthropomorphic or zoomorphic features to increase user acceptance. 7 The increasing presence of SARs in elderly care has sparked intense debate as it challenges conventional notions of “good care.” The International Council of Nurses' 8 Code of Ethics states that nursing is inextricably linked to respect for human rights, dignity, and autonomy. Likewise, according to the German Ethics Council, 9 an essential part of nursing is interpersonal connection that cannot be fully replaced by technology. This foundation raises important questions about the impact of SARs on professional–client relationships and on how caregivers understand themselves.
Coeckelbergh 2 identifies ten aspects of “good care” and links them to two philosophical traditions: (1) care ethics, as formulated by Fisher and Tronto, 10 and (2) phenomenological-hermeneutic approaches. Two key aspects of “good care” are particularly relevant when assessing SARs in elderly care: first, care inherently includes psychological and relational dimensions, such as emotional support; second, “good care” requires skilled engagement that goes beyond formal expertise to include practical know-how and caregiving craftsmanship. 2 This distinguishes the integration of robots in care from other domains, such as industry or transportation, where efficiency and automation are paramount. 11 Caring for the elderly involves work for, with, and on people, with an emphasis on emotional connection and comfort that cannot be fully reconciled with the logic of technological efficiency.12,13
Because of this perceived tension between the essence of care and the use of machines, the introduction of SARs in elderly care has sparked extensive ethical and philosophical debates.2,14–16 Much of the discussion revolves around concerns about the reduction of human contact in robotic care, a critique that is particularly pronounced in contexts involving vulnerable individuals such as the elderly.17–19
Vandemeulebroucke et al. 15 identify two dominant perspectives in these debates: First, the “care-romantic” perspective argues that SARs dehumanize eldercare, objectify elders, and promote a dystopian future where technology replaces human interaction.17,19–21 Rooted in the belief that caring is a natural, deeply human activity, this view holds that machines can never meaningfully replicate care.19,21 However, this view tends to overlook the already deeply technological nature of modern elderly care and risks equating the natural with the morally good. It can lead to overly restrictive and unjustified policies. Second is the “techno-deterministic” perspective, which argues that SARs provide necessary solutions to current and future challenges in elderly care, such as workforce shortages and rising care demands.22–24 This perspective assumes that SARs represent an inevitable stage of technological development and presupposes a structural need for their implementation in the elderly care sector.20,22,23,25,26 Yet, it risks legitimizing overly permissive guidelines that fail to reflect the complexity of care relationships. Empirical studies highlight the ambivalence of these technologies: while they may improve the identification of care needs and reduce physical strain, they may also introduce new complexities and burdens for caregivers. 27 We argue that these studies point to a third stance towards technology in elderly care. 3 As Verbeek 28 has outlined, this approach focuses on how technologies help to shape actions, decisions, and practices, while reflecting on the ethical implications. Using this epistemic lens, which focuses on the relationships between humans and technical artifacts, we examine how technology acts as a mediator that shapes and is shaped by social practices.1,28 From this perspective, integrating SARs in care facilities can transform the configuration of care relationships beyond the classic dyad. This open concept of technology also allows us to examine how people adopt and adapt to technologies.
Traditionally, caregiving has been conceptualized as a dyadic interaction between caregiver and care recipient. However, by implementing SARs, they become part of the care process, thereby changing this relationship. This shift requires a rethinking of roles, responsibilities, and professional self-understanding in care. 29 Consequently, it is crucial to facilitate interpretive dialogue with stakeholders 6 and encourage the active involvement of caregivers in these discussions. 30
Research design
To develop a model of how care interactions change with SAR use, a qualitative design following a constructivist grounded theory approach 31 was chosen. This approach was particularly well-suited to this exploratory research, as well as to the varied implementation of SAR in Germany. The absence of a standardized national policy on SAR use resulted in a highly diverse field in terms of stakeholders, funding, technologies, and institutional logics. Constructivist grounded theory allowed us to adapt to this complexity, respond to emerging patterns, and ultimately develop a theoretically informed conceptual model based on the lived experiences of caregivers. Twelve semi-structured interviews 32 were conducted with care professionals experienced in employing SARs in Germany. Four interviews with other stakeholders were included to cover multiple perspectives. The interview study is part of the mixed-methods project “Ethics Guidelines for Socially Assistive Robots in Elderly Care: An Empirical-Participatory Approach (E-cARE),” which includes a literature review, 33 a citizens’ conference, 34 and ethics guidelines for using SARs. The COREQ criteria were used to guide the writing of this section. 35
Participant selection and recruitment
The sampling strategy was purposive. In light of the ongoing debate about integrating technology into care settings and the lack of empirical research on how care professionals experience and respond to this transformation, the focus of the study was on the perspectives of those employing SARs in inpatient elderly care and how this might impact relationships between caregivers and recipients. This group included (geriatric) nurses and care assistants who organize social interactions. We aimed for maximum variation of perspectives in terms of work setting, work experiences, time spent working with robots, and type of robots used. Institutions using SARs were identified through web searches. Snowball sampling was also used as a recruitment strategy.
Participants were contacted by email and telephone to arrange an interview. Before the interview, the participant received an email containing study information, an informed consent form, and a short socio-demographic questionnaire. A total of 16 interviews were conducted with 18 participants, as 1 interview involved 3 people from different organizational levels.
To understand how SARs are used today (and in line with a grounded theory approach), we included four people who were not directly involved in care but shape SAR integration. Specifically, they were from the fields of applied science, technical support, management, and caregiver training. In the German context, it is important to note that SARs remain largely piloted and are mostly introduced in the context of funded (research) projects.
Requests to participate were declined for a variety of reasons (by twelve institutions), including lack of personnel resources, high interest but commitments to other studies (and media engagements), because SARs were no longer in use due to practical barriers (e.g., unstable Wi-Fi), the termination of a funded project, or lack of technical support.
Data collection
The interview guide was developed using the process established by Helfferich 32 and discussed in a workshop with other qualitative researchers for validation. The guide focused on the practical experiences, implementation process, perceptions, and reflections of participants (see appendix). Due to the small number of interviewees available, it was not pre-tested but continually adapted. Interviews were conducted by CK (4 interviews) and MB (12 interviews). Interviews were audio-recorded using a voice recorder and lasted between 25 and 90 min. They were then transcribed, and all personal or identifiable information was pseudonymized. Initial notes and thoughts were collected during the interviews, followed by the production of a postscript.
Data analysis
Data analysis followed a constructivist grounded theory approach. 31 Inductive coding was the first stage of analysis: The data was read and re-read and then analyzed to identify units of meaning. Conceptual labels (codes) were used to divide the data (into words, phrases, or lines). Codes that related to or represented similar concepts in respondents’ experiences were combined into groups. The categories and the overall analytical framework were developed using codes. To deepen the analysis, the data were condensed in a second round to extract and refine the main categories and to highlight their relationship (focused coding). Additionally, theoretical coding was employed to contextualize the findings within existing concepts in Science and Technology Studies as well as nursing ethics, such as technological mediation, 28 “good care,”2,10 and critical perspectives on care technology. This enabled an analytical process that was both theoretically informed and empirically grounded. Therefore, it was possible to consider the transformation of caregiving in terms of the participants’ experiences and the broader relational and socio-material complex.
Data were coded by MB, CVK, and CK. In joint coding groups, codes were compared and relationships between categories were mapped (MB and CK, MB and CVK). In addition, categories were presented in interpretation groups (e.g., with nurses) and team meetings. MAXQDA24 was used to code the data.
Setting
The interviews took place in Germany between April 2023 and April 2024. Five interviews were conducted in person at the institutions, seven by video call and four by telephone. The interviewees mostly preferred the latter two formats, as they were less time-consuming. To get a feeling for the care setting, both interviewers carried out at least one interview at the interviewee’s workplace. One interview was conducted with three people as this provided the perspectives of the institution, the local caregiver, and the supporting academic institution.
Sample characteristics
The participating institutions were located across Germany and varied in type, from open day centers to closed institutions that specialized in dementia care.
Information about the sample.
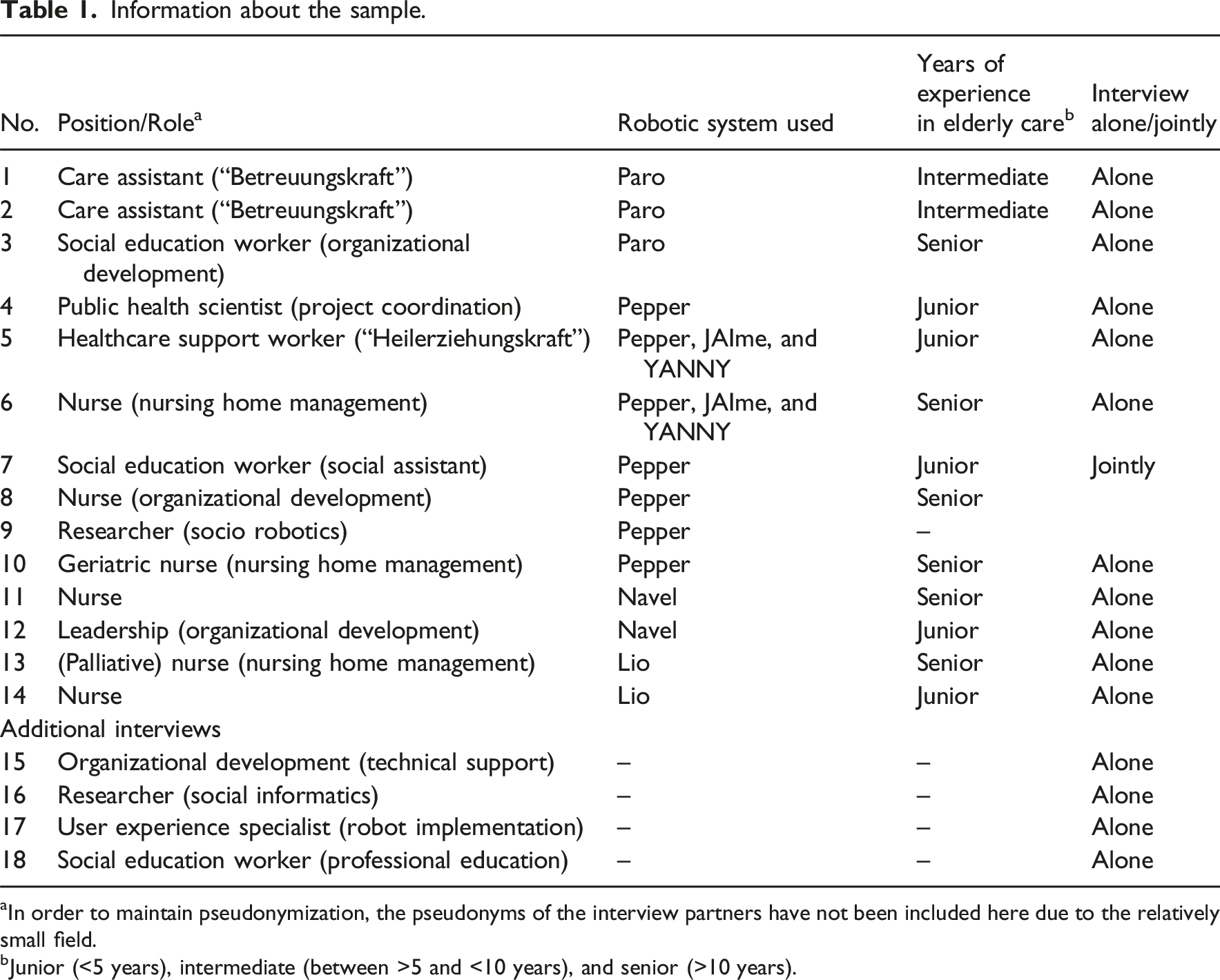
aIn order to maintain pseudonymization, the pseudonyms of the interview partners have not been included here due to the relatively small field.
bJunior (<5 years), intermediate (between >5 and <10 years), and senior (>10 years).
The robotic systems used by participants included Lio (2x), Navel (2x), Paro (3x), Pepper (7x), JAIme (2x), and YANNY (2x). As some facilities employed more than one system, the total number of systems is higher than the number of interviews conducted.
Reflexivity
Data collection and analysis were mainly undertaken by CK and MB. CK was the co-project lead and is an interdisciplinary health scientist with a focus on empirical bioethics. MB worked as a researcher on the project and is a sociologist specializing in interpretive research methods. Both researchers had previous experience of conducting qualitative research, particularly semi-structured interviews with health professionals. In addition, CVK, a research assistant trained in life sciences, coded all the interviews. The project and parts of the analysis were discussed in internal team meetings, colloquiums, and in an interdisciplinary interpretation group that included among others nurses and physicians. Their practical insights greatly enriched the interpretations.
Ethical considerations
The study was approved by the Ethics Committee of the University of Potsdam (No. 84/2022). Written informed consent was obtained from each participant prior to inclusion in the study. Data were pseudonymized, and original audio recordings were deleted after transcription to protect participants.
Results
The findings highlight the complex transition caregivers experience when integrating SARs. This shift is marked by a transformation from a dyadic (human-to-human) to a triadic (human–robot–human) care relationship model (Figure 1). The integration process unfolds in three distinct phases, each representing a key stage in this transformation. Illustration of the described three different phases. In each phase the care relationship model changes.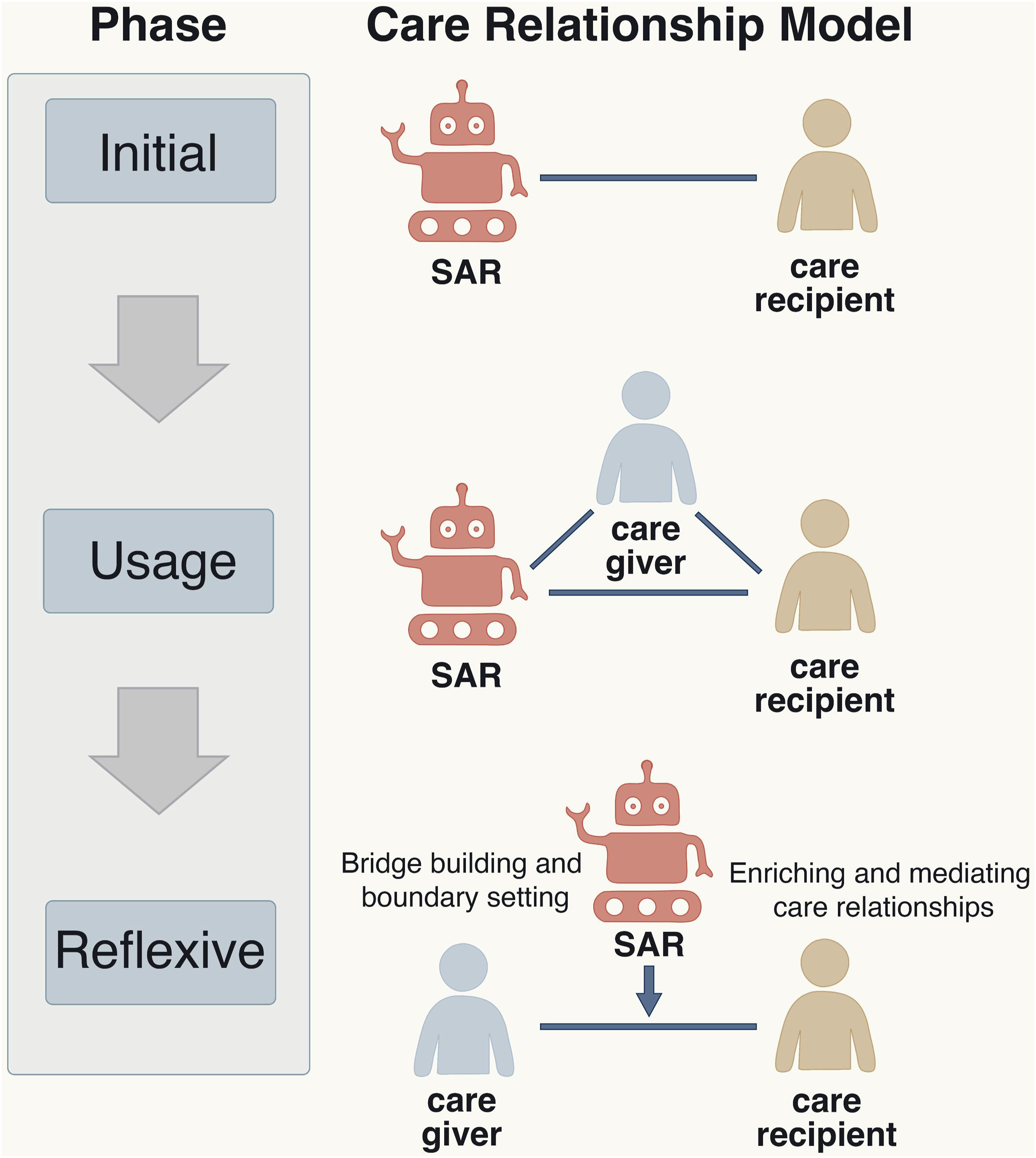
In the initial phase, caregivers tend to be skeptical and cautious when it comes to SARs, preferring to rely on a traditional dyadic care model that prioritizes direct interpersonal relationships between the caregiver and recipient. Within this framework, SARs are often viewed as external elements, raising concerns about the replacement of human caregivers and the subsequent erosion of professional values. As caregivers begin to engage with SARs in practice, relationship models gradually become recalibrated during the usage phase. Through repeated interactions, SARs become integrated into care routines. Throughout this process, caregivers remain pivotal figures, selectively appropriating SARs’ capabilities and adapting their role to suit the situation and care objectives. These practices facilitate new relational configurations in which caregivers, care recipients, and SARs interact within a more dynamic, triadic constellation. Finally, in the reflexive phase, caregivers actively consider the ethical and professional implications of this triadic relationship. Caregivers reassess their responsibilities and adapt SAR use to their normative frameworks. This shows that caregivers are active participants in constructing new care models that respond to technological change while upholding professional commitments.
Initial phase: Fears of displacing the human element of care
Initially, caregivers expressed concern about SAR implementation, which they perceived as a potential threat to relational care. This resistance is rooted in a dyadic model of caregiving, in which the caregiver–recipient relationship is seen as fundamental to providing “good care.” From the caregivers’ perspective, both they and care recipients alike expressed concern about the erosion of the human connection.
A recurring theme in the interviews was the fear that SARs could replace human caregivers, undermining interpersonal relationships: “Sure, the question always comes up in the second sentence [with caregivers]: ‘Are they going to replace us living people?’ And we always answer: ‘We hope not’. (…) Because of course the biggest fear of the seniors is that the human connection will disappear altogether” (Mehl).
1
Underlying such concern is the conceptualization of the SAR as a potential new partner in a dyadic relationship. Such a development is feared, as it implies substituting the human element with a robotic one.
Furthermore, concerns were raised about the economic motivations behind the implementation. Caregivers feared that SARs would be used as a cost-saving measure, prioritizing efficiency over quality of care: “I'm worried about robots being misused - residents being left with robots just because it's cheaper. That would be a nightmare. Care is about human warmth, about seeing what someone needs in the moment. A robot can't do that, no matter how many sensors or cameras it has” (Stein).
Caregivers’ relational understandings of care were contradicted by this supposed economic rationale. They believed that maintaining care as relational work with a “human connection” (Mehl) is a normative obligation that political and ethical institutions should address: “I'm just afraid that more and more people will say, ‘Yeah, we've got a robot here. So we don't need a human’. And that is a political decision (...). That's why I think it's really a matter for the German Ethics Council (...) that care remains human. (...) As I said, I'm a fan of all this, but as an addition and not as a replacement” (Nau).
This skepticism was associated with the previously mentioned ethical commitment to “good care.” Other narratives referred to further reasons, such as fear of job loss or an increased workload, a lack of interest in and inability to cope with modern technology, and concerns about fundamental changes to the nursing profession: “Care has changed – suddenly you also must watch out for the robot and incorporate it into your work. You're no longer just a care assistant working with people. Suddenly, it all becomes technical. Some were very skeptical, saying: ‘Technology – that's just not my thing’” (Palm).
In addition, caregivers were skeptical about the ability of SARs to authentically emulate emotional and social behaviors. They feared that artificial emotional engagement could create misleading or inauthentic connections with care recipients, ultimately damaging trust. Nevertheless, all interviewees were open to try the new technology, but only a few were starting with a positive view: “From the beginning, I was very excited. ‘Oh, a robot! I really want to try that out’” (Kaya). Additionally, caregivers saw the potential for improving the status of the nursing profession through SAR implementation: “Robots are already versatile and can be used in many different ways. They are definitely interesting, and even attractive, to young people as a way of learning the profession” (Stein).
In summary, most caregivers were skeptical in the early stages of SAR implementation for various reasons. While they recognized the potentials of SARs, they emphasized the irreplaceability of human empathy, warmth, and judgment in caregiving. Their reservation was rooted in a dyadic model of care, which views the human relationship as fundamental for the notion of “good care.” Implementing SARs in their view runs the risk of replacing human caregivers with robotic ones, which also triggers fears of job loss and fundamental shifts in the nursing profession. However, as the next phase shows, this view begins to shift with practical experience in working with SARs.
Usage phase: Integrating SARs and recalibrating the relationship model
In retrospect, the professionals described how their initial expectations changed as they began to work with SARs. They observed that SARs had limited autonomy, could not fully engage with care recipients, and required constant supervision. This realization led to a recalibration of the relationship model: instead of replacing caregivers, SARs became part of a collaborative triad in which their effectiveness depended on caregivers’ ability to adapt and integrate them into daily practices: “At first, we thought that if we just put Pepper in the room, something might happen. But we learned that if you just put the robot in the dining room, it will be ignored. It just doesn't work that way. As a person, you really must build a bridge to the elderly” (Pieper).
SARs were primarily used for “communication and memory training, and to promote physical activity” (Pieper). They therefore facilitate social interaction and assist with specific routine tasks. There was some debate as to whether they relieve caregivers. While they could free up time when used for routine tasks, at the same time they often require the presence and supervision of caregivers: “It's important that robots don't replace staff. Robots should only support us, like reading recipes to seniors who want to cook, while I provide one-on-one care to someone who really needs it” (Dorn). “Someone must be there with the resident. If this person is with Navel […], then they are not elsewhere” (Heinrich).
After understanding the limited functionality of SARs, professionals had to adapt their conceptualization of them as a replacement technology. Instead, SARs were reinterpreted as a tool to support certain care tasks that were then carried out by a triad constellation. While the care relationship was mediated by SARs, effectively turning it into a triad, the roles within the care constellation are marked by power and responsibility differentials. Professional care providers, and to a lesser extent care recipients, need to make an effort to integrate SARs into the care relationship. It is often up to the caretaker to decide when and how to use it and when to end the interaction. For example, the task of calming down an agitated dementia patient can be realized by three entities working together: the care recipient interacting with a robotic seal Paro and the care professional who facilitates this interaction: “The seal [Paro] has a calming function. (…) The care recipients can stroke and can practically get rid of everything they have inside them for a moment. Then the facial expression relaxes, the body relaxes” (Nau).
However, in the end it is up to the care professional to place Paro in the lap of an agitated person. Other tools or the help of care provider (his/her voice etc.), can also be employed. In this triadic model, caregivers maintained their relationships with care recipients because they facilitated interactions with SARs. Their role ensured that SARs were perceived as a tool to enhance, rather than replace, human connection. SARs thereby broadened the care-toolkit but did not fundamentally change care or professional identities.
While SARs are mostly conceptualized as tools, it is still a relationship that is formed as the following statement illustrates: “In the beginning we also had to deal with some prejudice: now Pepper comes and replaces the caregivers. No, he doesn't. He is an addition. But now he really is an integral part, and somehow, he belongs. Well, that had to develop. It wasn't like that from the beginning” (Pieper).
Unlike traditional care objects (books or memory games), SARs were perceived as social agents capable of eliciting attachment. As such, their integration into care facilities required intentional effort from staff to foster a sense of familiarity and connection among both caregivers and residents. For example, in one case, the SAR was introduced as a “new trainee” (Erich) and then gradually became part of the team: “But now he’s just part of the team and that’s a good thing” (Erich). Care recipients formed bonds with the SARs, often treating them more like companions than tools: “The seniors like to shake his hand, just say hello and then he says something. (…) The dementia patients react very positively to this and then talk to him or are simply happy that he looks cute and comes” (Pieper).
While initial concerns focused on job displacement which could be dissolved by experience, these fears often gave way to disappointment with the SARs’ functional limitations. Many caregivers found it frustrating that SARs lacked autonomy and required constant human intervention to perform effectively. For example, they needed to manage technical issues, such as software errors. One participant contrasted the limited capabilities of SARs with inexpensive consumer technologies: “The need for constant supervision was a recurring theme. (…) With Pepper, there always must be someone with him – a caregiver or a housekeeper – to do something with him. It's a bit of a disappointment, because you'd expect it to be able to do more, you know? When I think about Alexa at home, it costs 30 euros, and you can almost have a conversation with it. With Pepper you can't” (Kaya).
This comparison between low-cost consumer technology and the expensiveness of SARs led to skepticism about whether robotics in their current state could meaningfully reduce workload or improve quality of care.
Our findings show that through their SAR experiences, caregivers gradually adjust their view of how care relationships with SAR will look from a traditional dyadic structure to a more flexible triadic one.
Reflective phase: Establishing normative boundaries for SAR use
Caregivers consistently emphasized the need to establish boundaries for the SAR use. While some boundary-making practices were rooted in ethical reasoning, such as maintaining human-centered values that define their profession, others were more pragmatic, such as acknowledging the unreliability and lack of contextual sensitivity of SARs. Both can be morally relevant, not because of their intent but because of their impact on care practices and values.
As mentioned in the first phase, the fundamental principle articulated by caregivers was that SARs should augment, but never replace, human caregiving. This belief shaped how caregivers integrated and used SARs. When used for social tasks, such as displaying images during biographical work or group gymnastics, they fostered social interaction and indirect conversation, as well as group identity building. However, they were firmly excluded from roles requiring emotional depth or relational care, which seems to drive some tension between the imagination of designers and policy makers and the expectations of caregivers.
2
Therefore, one caregiver explained the importance of maintaining a balance between technological integration and human presence: “And that could be the limit, because sometimes individuality can get lost in the daily grind. But that is our task and our challenge for the future, to ensure that this is the norm in care. (...) When it comes to educating people about data protection and how to handle it, I really don't think there are any major barriers. It's more about how you deal with it, how you implement it, how you integrate it. So that you don't feel like there are just robots running around and they can't really talk to anybody. So, the social aspect must continue” (Dorn).
Caregivers consistently established normative boundaries. They did this in situations that required responsibility, empathy, or direct human involvement. This could include administering medication or assisting with personal hygiene. Such scenarios are not currently feasible with existing robotic systems, highlighting the discrepancy between caregivers’ ethical concerns and the actual capabilities of present-day SARs: “But I always think that wherever responsibility or human affection is involved, I think that robotics simply cannot and should not, in my opinion, replace humans. So, when it comes to giving pills or food or going to the toilet or things like that, I think a robot has no place there” (Pieper).
This boundary setting underscores the belief that while SARs can play a supportive role, they must not compromise the relational and ethical core of caregiving. However, caregivers recognized that these boundaries are not fixed.
Despite this, end-of-life care emerged as a normative boundary seemingly non-negotiable: “I would never use [a robot] in a palliative setting. It's a time when you need human closeness. A dying person or someone in palliative care needs so much care and attention that no robot can provide. Palliative care and end-of-life care, I always do myself” (Erich).
Another caregiver expressed similar sentiments but acknowledged potential future challenges that might make a shift in attitudes necessary: “In the last phase of life, like end-of-life care, there is so much empathy needed. I think if there's ever a situation where we don't have enough staff, maybe a robot would be better than nothing. But for now, these moments require a human presence” (Mehl).
These quotes show that caregivers negotiate the normative boundaries of SAR use. While SARs were welcomed for certain routine and logistical tasks, caregivers maintained firm limits regarding relational and emotional aspects of care, particularly in palliative and end-of-life settings. However, their awareness of future challenges suggests that ethical boundaries are not static but require ongoing dialogue as both the challenges and the role of technology in care continue to evolve.
In the reflective phase, professionals critically evaluated the triad. They sought to ethically allocate professional responsibilities and maintain relational integrity.
Discussion
Our study contributes to current debates on the SAR integration in elderly care by showing how caregivers’ relationship models are shifting from a dyadic to a triadic model. This shift does not follow a linear technological logic but emerges through a dynamic interplay between the affordances of SARs and how caregivers use and adapt to them. Initially, caregivers often exhibit reluctance towards SARs based on a dyadic understanding of care, fearing the replacement of relational dimensions by technology. However, through practical engagement, these assumptions are recalibrated. Our findings show that SARs provide certain social affordances—opportunities for engagement, stimulation, or comfort—but these affordances are not automatically realized. Instead, caregivers selectively take up or resist them, depending on their professional values, experiences, and normative considerations. 36 This highlights the mediating role of technology in care, where meaning and practice emerge through use. 28 The emerging triadic model of care reflects not only a functional response to technological limitations but also a normative negotiation of what constitutes “good care.”
As the empirical study has shown, the “care-romantic perspective,” which emphasizes the interpersonal dimension of care, is of central importance to professionals. However, it is important to address the divide between humans and technology, and to avoid judging the former as inherently good and the latter as inherently bad. After all, care has long been technology-mediated. 1 Caregivers recognize their role as “bridge builders,” integrating SARs into their work and using them to shape the caregiver–care recipient relationship.
Rather than being a technical solution, it is a complex social interaction in which design decisions and the actual application of care can be distinguished. It is also necessary to address the error-prone nature and technical limitations of current developments, which require professionals to do more work. Therefore, it is crucial to critically discuss the promises of the “techno-deterministic perspective,” such as efficiency and workload reduction. Our study confirms concerns that SARs introduce new responsibilities for caregivers, potentially increasing their workload. 27 Caregivers must address technical challenges, adapt their interactions with, and ensure that SAR practices adhere to professional standards. These findings align with observations that users often adjust their behavior to align with the SARs’ capabilities. 7 These observations raise questions about the implications for user autonomy and the extent to which SARs influence caregiving practices. The extent to which further developments through AI and generative language models will emerge requires further research.
Caregivers maintain a strong sense of responsibility for preserving the relational and moral integrity of care. They actively mediate human–robot interactions, redirecting them in a way that supports, rather than replaces, the human-centered essence of care. Their actions demonstrate that SAR integration is never purely technological; rather, it is shaped by how professionals understand the technology in relation to their ethical and professional values. Thus, the triadic model is not a passive outcome but rather a situated and reflexive achievement.
This highlights tensions embedded in SAR affordances: while they are designed to support care, they inevitably create new demands and expectations. Caregivers resist some of these demands, for example, by restricting SARs to routine tasks. Professionals establish boundaries that are not solely dictated by technical capacity but rather reflect a broader professional ethos. This selective acceptance raises important questions for care policy and design: should future SARs be built to afford only what professionals are willing to accept? Or should they more deliberately challenge existing care practices?
As demonstrated by our study and others,37,38 the successful implementation of SARs depends on involving care professionals. However, we argue that the caregivers’ self-understanding is reconfigured as they interact with SARs. This process of negotiation and boundary setting is central to how ethical frameworks are enacted in practice. 39
Finally, our findings highlight a shift in professional identity. Caregivers increasingly see their role not only as maintaining good relationships with recipients but also as curating meaningful human–technology interactions. They are becoming “bridge builders”—mediating between technological innovation and the emotional, ethical, and practical needs of elderly care. To fulfill this role, caregivers need ongoing support, reflection, and professional development to ensure that technological integration enhances rather than undermines the human essence of care.
Our study has the following limitations: (1) a small sample size and potential bias arising from the self-selecting processes of institutions and caregivers and possible effects on participants’ answers by positioning our research within the field of bioethics; (2) the cross-sectional nature of the study, whereby caregivers’ experiences were interpreted retrospectively; (3) not including the perspective of care recipients. Therefore, future research should employ longitudinal or ethnographic methods to examine how professional moral orientations are expressed in everyday practice and evolve over time. Nevertheless, our findings are consistent with broader empirical research, while illuminating gaps in the existing literature. Our study takes a retrospective approach on SAR integration and changes of the caregivers’ relationship model.
Conclusion
The SAR implementation into elderly care can challenge professionals’ understanding of “good care” as well as their self-understanding. As empirically shown, caregivers’ perspectives are changing from a dyadic to a triadic model where they act as bridge builders between technology and relational care. While SARs support practical tasks and social engagement, caregivers do not see them as replacing the emotional depth, adaptability, and moral agency that are central to human caregiving. Our findings show that caregivers actively mediate SARs interactions to ensure that they enhance rather than diminish relational care.
Caregivers emphasize that SARs should complement, not replace, their work, thus preserving the human-centered character of caregiving. This highlights the need for structured training and participatory implementation to empower caregivers to integrate SARs effectively.
Ultimately, the success of SARs depends on their recognition as supportive tools rather than substitutes for human care. The bridge-builder metaphor encapsulates how caregivers navigate technological change to ensure that relational care remains at the heart of elder support. As care becomes increasingly technologized, maintaining this balance is critical for both care recipients and caregivers’ professional identities.
Supplemental Material
Supplemental material - An interview study on socially assistive robots and professional care relationships
Supplemental material for “An interview study on socially assistive robots and professional care relationships” by Marc Bubeck, Clara V. Keusgen, Joschka Haltaufderheide, Corinna Klingler, and Robert Ranisch in Nursing Ethics
Footnotes
Acknowledgments
We would like to thank Dr. Laura Gawinski (for writing the ethics committee application and developing the interview guide) and Marianne Leineweber (for her extensive insights into the state of research and discussion of links to the empirical data). Thanks also for the collegial and productive interpreting session with the “Qualitative Forschungswerkstatt des Netzwerks Qualitative Forschung der Charité – Universitätsmedizin Berlin.” Special thanks go to all the interviewees and field contacts who, despite limited time, allowed us to gain a deeper insight into their work.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by German Federal Ministry of Health (Grant Number. BMG2521FSB008).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Supplemental Material
Supplemental material is available online.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
