Abstract
Background
Healthcare workers are increasingly subject to violence, aggression, and discriminatory requests from patients and families, reflecting broader societal biases within healthcare settings. In response, some institutions have developed policies and decision-making tools to guide leaders in addressing these situations ethically, consistently, and in accordance with human rights obligations.
Aim
This paper describes the revision of a previously published Caregiver Preference Algorithm to guide healthcare leaders in managing discriminatory patient requests. The goal was to create a more robust, accessible, and contextually sensitive tool to support decision-making.
Research design
The algorithm was revised through a multi-phase quality improvement project aimed at enhancing support for both frontline clinicians and leadership.
Participants and research context
The project was conducted at a large, multisite tertiary care hospital in Ontario, Canada. Interviews were completed with 27 healthcare workers from various clinical areas. Stakeholder consultations included clinical and operational leadership, legal counsel, patient relations, equity offices, patient partners, and frontline staff.
Ethical considerations
This project was approved by the University Health Network’s Quality Improvement Review Committee [ID: QIRC 22-0378].
Findings
The updated algorithm is structured around six key decision points: (1) patient acuity and capacity; (2) consideration of religious, cultural, or trauma-informed needs; (3) relevance of trainee or learner status; (4) whether the request violates the Human Rights Code; (5) the identity of the requester; and (6) the clinician’s willingness to continue care.
Discussion
The revised algorithm integrates legal and ethical principles to help healthcare leaders navigate complex situations. It offers structured guidance while allowing flexibility to respond sensitively to diverse clinical contexts.
Conclusion
This work contributes a practical, rights-based framework that can support healthcare institutions in ethically and consistently responding to discriminatory patient requests while protecting healthcare workers.
Keywords
Introduction
Healthcare workers are facing increasing levels of violence and aggression in the workplace, ranging from physical assault to verbal abuse and harassment.1–5 While this crisis has been widely acknowledged,6–9 less research and scholarly attention has been paid to the ways in which racism and other forms of discrimination are embedded within these encounters. Racialized healthcare workers, particularly those who are Black, or Indigenous are subjected not only to heightened aggression but also to racial slurs, stereotyping, and exclusion.10–13 In some cases, patients and their families go beyond verbal abuse, making discriminatory requests or refusals of care based on the healthcare worker’s race, ethnicity, or religious background. These situations surface profound ethical tensions and questions; for example, should healthcare institutions accommodate such requests when they appear to be grounded in strongly held patient preferences or values, or does doing so promote discrimination and infringe on the rights and well-being of healthcare workers?
Under the Ontario Human Rights Code (OHRC), healthcare workers have the right to work in an environment free from discrimination, harassment, and harm. 14 Furthermore, healthcare institutions have legal and ethical obligations to ensure that their policies and practices do not expose employees to toxic work environments.14,15 When hospitals and healthcare organizations fail to address or, worse, condone discrimination from patients or their families—whether this takes the form of racial slurs, exclusionary treatment requests, or other forms of bias—they undermine their staff members’ dignity, safety, and well-being. 7 In addition, they send a troubling message that patient preferences, including those that are rooted in bias, take precedence over the rights of healthcare workers. 7 Historically, some hospitals have accommodated racist patient requests, allowing discrimination to persist, perhaps under a belief that doing so recognizes patients’ rights to self-determination.16–18 However, legal challenges have demonstrated that such actions are indefensible. In cases where staff members have sued their employers for failing to protect them from racial discrimination, courts have ruled in favor of the workers, affirming that institutions must actively prevent and address workplace discrimination.19–21 Protecting healthcare workers from racism, and other forms of discrimination, is not only a legal duty but an ethical obligation that healthcare managers and leaders cannot ignore given their responsibilities to provide safe working conditions for all who fall under their care and jurisdiction. Fulfilling this duty requires clear policies, an acknowledgement of institutional accountabilities, and a commitment to fostering workplaces that truly are inclusive and supportive. 7
While patients have the right to make decisions about their own care, there are limits to the extent of their autonomy. 7 These limits are defined by the need to maintain a safe, respectful, and professional environment for both staff members and other patients. 7 In Ontario, Canada, healthcare workers navigating challenging workplace incidents often turn to hospital policies, their professional colleges or regulatory bodies, or relevant legislation—such as the OHRC 14 and workplace safety laws—for guidance and support. Regulatory colleges, tasked with protecting the public interest, provide evidence-based practice standards to help professionals manage complex clinical issues, and the codes of conduct, or codes of ethics, applicable to members of self-regulating healthcare professions generally emphasize duties owed to patients, the public, and to other professionals. However, many have not explicitly acknowledged patient bias and discrimination as a practice issue that falls within their mandate. Consequently, healthcare workers are left without clear, profession-specific guidance on how to respond to discriminatory behavior. Instead, they must interpret and apply broader policies, such as those addressing the termination of therapeutic relationships due to violence or abuse, or guidelines on patient referrals. These resources, while helpful in some cases, do not adequately address the nuances of discrimination in clinical settings. In the absence of explicit direction from regulatory bodies, healthcare workers must rely on institutional policies or legal frameworks (e.g., OHRC) to navigate these difficult situations. This lack of standardized guidance creates inconsistencies in how discrimination is handled within and across health systems, and places the burden on individual workers, managers, and organizations to determine appropriate responses. Inconsistent responses within clinical contexts and across organizations can leave healthcare workers feeling unprotected, isolated, and devalued.4,11,22–24 The continued absence of institutional accountability may exacerbate feelings of anger, abandonment, and moral distress, especially among those with lived experiences of bias and exclusion.6,18,25–27
A growing body of research has examined this issue through the lens of organizational policy and guidelines, highlighting key recommendations for institutions seeking to navigate discriminatory requests arising in care provision.28–34 Anstey and Wright, 29 for example, introduced a Caregiver Preference Guideline and accompanying decision making algorithm (Caregiver Preference Algorithm) at the University Health Network (UHN), a multi-site tertiary care academic hospital in Toronto, Canada. Their work offers a structured approach to managing patient requests for or refusals of care based on discriminatory preferences. The current paper builds on Anstey and Wright’s foundational work, outlining the changes in the local context that necessitated a revision of their algorithm and detailing the process taken to refine and implement the updated guideline. We present here the revised Patient Bias and Preferences Algorithm, which replaces Anstey and Wright’s Caregiver Preference Algorithm in our local context.
In this paper, we use the term algorithm to refer specifically to clinical decision support algorithms (CDS) as defined by Oxholm et al. 35 CDS algorithms are intended to aid clinical problem-solving and improve both patient care and healthcare systems. Typically presented as flow diagrams or decision trees, CDS algorithms outline potential pathways for addressing a problem or guiding decision-making. Unlike logic-based automated algorithms rooted in the computational sciences, CDS algorithms are structured guides designed to support human judgment in complex, often context-sensitive situations, and are intended to help healthcare teams think through a problem systematically.
The UHN context: The Caregiver Preference Guideline (2007) versus the Patient Bias and Preferences Guideline (2024)
The Caregiver Preference Guideline was developed to address patient requests for and refusals of specific healthcare workers at the University Health Network (UHN), a large research and teaching hospital network in Toronto, Ontario, Canada. The Bioethics Program, now the Department of Clinical and Organizational Ethics, in collaboration with what was then called the Office of Diversity and Mediation—now renamed the Inclusion, Diversity, Equity, Accessibility, and Anti-Racism (IDEAA) Office—created this tool to provide recommendations to managers on whether and how to respond to patient requests that could conflict with the institution’s anti-discrimination policies. It was prompted by numerous reported incidents, particularly cases of racism and other forms of discrimination, directed at staff members by patients and their family members or visitors. The tool was primarily created for use by managers to provide them with a starting point in addressing or navigating these scenarios, but it also provided them with a resource that delineates the multiple steps they need to take to ensure a thoughtful and safe response to distressing incidents. Clinical contexts in which these cases frequently emerged included the emergency department, the dialysis unit, specialized dementia unit, and geriatric care. For further information on how the Caregiver Preference Algorithm was designed and could be applied, see Anstey and Wright. 29 The guideline was designed for UHN as it existed in 2007. Since then, UHN has expanded significantly, encompassing not only acute care but also rehabilitation and specialized cancer care spanning multiple sites. Additionally, the sociopolitical landscape has shifted dramatically, further highlighting the urgent need for a robust approach that is attentive to context, the complexity, and frequency of cases involving discriminatory patient requests, and the impact on staff well-being. In 2022, we launched a quality improvement (QI) project designed to ensure that the guideline would be comprehensive, responsive, and better equipped to support staff navigating complex ethical and discriminatory challenges in today’s healthcare environment.
Our quality improvement project used an evidence-informed approach to revising the Caregiver Preference Guideline. This included conducting: (1) a scoping review of the literature, 7 (2) qualitative interviews with 27 healthcare workers from diverse clinical backgrounds across UHN, (3) a critical review of comparable health system policies, and (4) consultations with UHN representatives from various clinical departments, leadership groups, and support services.
Interviews
Semi-structured interviews were conducted with 12 nurses (bedside and leadership), 5 occupational therapists, 2 social workers, 1 physiotherapist, 1 recreational therapist and 6 physicians (4 staff and 2 learners) from acute care, rehabilitation medicine, cancer care, and specialized clinics. Of the 27 interviews, 26 were virtual, and 1 was in-person.
Policy review
The reviewed policies included: Mayo Clinic’s 5-Step Policy for Responding to Patient Bias, 36 Penn State Health’s Patient Caregiver Preferences and Refusal of Care Based on Aspect of Diversity Policy, 37 and Johns Hopkins’ Prohibiting Discrimination by Patients against Employees Policy. 38
Consultations
Consultations were conducted with representatives from the following departments and stakeholder groups across UHN: Legal Affairs, Labor Relations, Clinical Education, Medical Affairs, ED Physician Leadership, Internal Medicine Leadership, Clinical Directors from the ED & ICU, Psychiatric Nursing and Behavioral Specialists, Social Work Leadership and Practitioners, Patient Relations, Occupational Health & Safety Services, UHN Security Services, Patient Partners, the IDEAA office, and the Indigenous Health Program.
Ethical Considerations
This project was reviewed and granted approval by UHN’s Quality Improvement Review Committee (QIRC) - ID#: 22-0378. Participants were provided with a written preamble outlining the project’s purpose, methods, and the voluntary nature of participation. They were assured that participation would not be connected to their employment status (i.e., their decision to participate or decline would remain confidential and would not be disclosed to supervisors, colleagues, or their employer). Information was provided regarding how data would be used, who would have access to it, and the measures in place to ensure confidentiality. All data were de-identified, coded, and stored securely, with access limited to the project team. Only the first author (CB) had access to identifiable participant information.
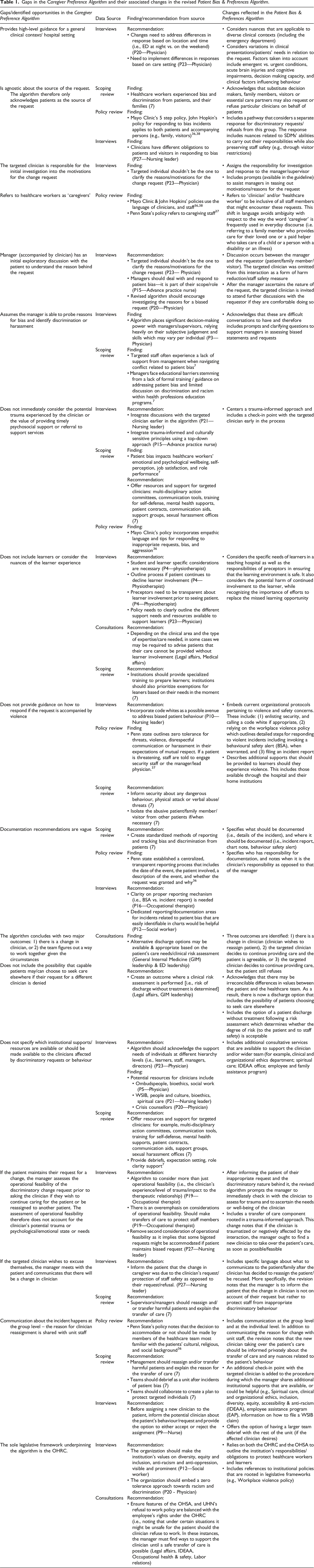
Gaps in the Caregiver Preference Algorithm and their associated changes in the revised Patient Bias & Preferences Algorithm.
Applying the Patient Bias and Preferences Algorithm
The Patient Bias & Preferences Algorithm is a five-page decision-making tool with six key decision points, designed to guide responses when a patient’s request or refusal of a specific healthcare worker is tied to consent to treatment. The process begins with the affected clinician informing their manager of the request, thereby initiating a discussion to clarify the requestor’s values, beliefs, and reasoning. To minimize harm or retraumatization of the affected healthcare worker, the manager—rather than the clinician—leads further discussions with the requestor. This ensures that explicit concerns about care can be addressed while also offering the requestor an opportunity to reconsider and withdraw their request if it is discriminatory in nature. In cases where requests or refusals involve slurs, epithets, or violent behaviour, the discussion focuses less on exploring rationale and more on reinforcing the institution’s anti-discrimination policies and expectations for respectful conduct.
At this stage, the manager, with input from the clinician, reaches the first decision point, assessing the requestor’s preference in light of their clinical presentation:
Acuity and capacity: Does the patient have urgent or emergent medical needs? Are they capable of refusing treatment or imposing conditions on their care?
Assessing a patient’s acuity is critical to determining whether immediate health-related needs take precedence. While healthcare workers are not expected to tolerate discriminatory behaviour, they also have ethical duties to provide care, particularly in emergencies. In crisis situations, the obligation to deliver treatment can override the need for discussions about the request, with priority being placed on stabilizing the patient.
The updated algorithm explicitly ties the refusal of a specific healthcare worker—or the request for a particular provider—to consent to treatment. This requires assessing the patient’s capacity to make treatment decisions and considering whether they understand the implications of their request or refusal. Importantly, capacity is assessed in relation to a specific treatment decision and is not treated as a global determination. This decision point also considers how a patient’s stability and capacity intersect, evaluating whether clinical factors (e.g., cognitive impairment, delirium, or mental health crisis) are influencing their ability to appreciate both the clinical and psychosocial consequences of their preferences—including potential harm to themselves or staff.
Religious, cultural, and trauma-related needs: Are there reasonable, non-discriminatory reasons for the request/refusal?
The second key decision point involves an exploration of reasonable, non-discriminatory, concerns that may affect the patient’s care experience directly. If the requestor has not yet articulated specific care-related needs, this step provides an opportunity to clarify whether their request is linked to accommodations protected under human rights legislation such as the Ontario Human Rights Code. These may include cultural, spiritual, or religious considerations, as well as past traumatic experiences, that could influence their degree of comfort with certain providers. The goal is to determine whether the request aligns with trauma-informed or culturally sensitive care, which can enhance patient safety, trust, and overall well-being. However, it is also recognized that some religious, cultural, or trauma-related requests may still be shaped by implicit bias or discriminatory beliefs, meaning that not all such requests automatically warrant accommodation.
If a request is determined to be rooted in a traumatic experience or religious-based need, the manager can communicate this to the affected healthcare worker, clarifying that the decision is not based on discriminatory grounds but rather on a request that supports the patient’s care journey in a meaningful way. Likewise, the patient is to be informed that the request is being accommodated due to legitimate clinical or psychosocial factors rather than personal preferences alone.
Learner status—is the refusal based on the clinician’s “trainee” status?
As a teaching hospital, UHN has a responsibility to protect and support the education of its diverse cohort of health professions learners. Learners may experience refusals of care based solely on their trainee status, aspects of their identity, or both. This decision point ascertains whether the refusal is primarily due to the learner’s status as a learner and requires a check-in with the learner to evaluate their level of harm, comfort, and willingness to proceed. The patient’s interest in directing their own care must be weighed against (1) the institution’s obligation to provide teaching and learning opportunities to those in training and (2) its duty to ensure that future patients have a well-prepared workforce available to meet their needs. While capable patients may exercise their rights to refuse care, or care from specific healthcare providers, teaching hospitals must establish clear boundaries regarding the treatment of learners, ensuring that necessary support systems are in place to foster their success and well-being. Although nuances exist across various contexts, disciplines, and professions, in cases where a patient refuses care from a learner, it is still the capable patient’s right to wait for a fully licensed provider, even if this results in delayed treatment. Institutions should take steps to determine whether these refusals are rooted in discriminatory biases and ensure that learners are protected from harm and exclusion while training in a clinical environment.
Discrimination or harassment—does the request/refusal discriminate against or harass the clinician?
This decision point determines whether the patient’s request or refusal is rooted in bias or discrimination under any of the 14 protected grounds of the OHRC (which references race, ancestry, place of origin, color, ethnic origin, citizenship, creed, sex, sexual orientation, age, record of offenses, marital status, family status, and disability). The OHRC legally protects individuals from discrimination based on these grounds, which determine the institution’s legal and ethical obligations in responding to such requests. Appendix B of the Patient Bias and Preferences Guideline includes prompts and guiding questions to help managers and decision-makers tease out the particulars of the request or refusal. The goal is to differentiate between reasonable, patient-centered, concerns (e.g., trauma-informed needs, religious accommodations) and discriminatory requests that violate institutional policies and obligations.
Source of the request—who is the requestor and how do our obligations change in reference to the source of the request?
The next decision point clarifies who is making the request or refusal—the patient, a family member, or another party—as this helps determine the legal and ethical obligations of the institution. While healthcare workers have clear duties of care with respect to their patients, this obligation does not extend in the same way to family members or visitors. However, complexities arise when a family member serves as a substitute decision-maker (SDM) or when they hold Power of Attorney for Personal Care, as they then are legally authorized decision-makers (LARs) for incapable patients. In these cases, the institution must both uphold and respect their decision-making rights, even if their behaviors or attitudes are problematic. This requires careful navigation; respect for the SDM’s role must be balanced against the institutional and leadership responsibility to ensure that discriminatory behavior does not go unaddressed. If the request or refusal comes from a non-decision-making family member or visitor, the institution has greater flexibility to take corrective action, including setting firm boundaries on unacceptable conduct. Depending on the situation, responses may range from education and dialogue to removing privileges for disruptive visitors if their behaviour creates a toxic or unsafe environment for healthcare staff members.
Agency of the clinician—does the clinician wish to excuse themselves/reassign patient or to continue providing care?
An important goal of the algorithm is to ensure that affected healthcare workers have agency in deciding how they wish to proceed. At this decision point, the clinician is given the choice to: (a) Continue providing care, or (b) Request reassignment (if operationally feasible)
Irrespective of their choice, the manager must express solidarity and support for the clinician. If the clinician opts to continue care, the manager should reinforce the institution’s commitment to a safe and discrimination-free workplace and affirm the clinician’s competence and professionalism to both the staff member and the requestor. This ensures that the decision is not seen as validating the discriminatory request, but rather as the result of clinician’s autonomous choice to continue to support the patient. If the clinician requests reassignment, the institution should facilitate the transition without validating the bias underlying the request. The manager must explicitly communicate to the requestor that the change is not a concession to their discriminatory demand, but rather a protective measure to safeguard the well-being of the staff member. Additionally, the affected clinician should be provided with access to institutional supports to help process the emotional and psychological impact of the incident. This may include referral to an Employee Assistance Program or other resources. By emphasizing a commitment to both agency and support, this approach ensures that healthcare workers are empowered rather than burdened by these challenging encounters, and it reinforces the organization’s commitment to equity, safety, and professional dignity.
Discussion
This paper describes the revisions made to Anstey and Wright’s 29 algorithm and the processes available to respond to discriminatory requests or refusals of care in a Canadian tertiary care academic hospital. In this paper, we note important contextual factors that are relevant to the assessment of whether, how, and when one should respond to, or accommodate, a request or refusal that is discriminatory in nature. The algorithm was designed specifically for adult inpatient care environments. Establishing institutional practices and recommendations for responding to patient bias in other care contexts (e.g., in pediatric or outpatient settings) requires consideration of population-specific factors and clinical nuances. Notably, what UHN has instituted, and what has historically existed, is a guideline not a policy. A guideline was chosen during the revision due to considerations about what is enforceable, and what is recommended. Organizational accountability and responsibility differ depending on whether a policy or a guideline is adopted. For example, if an institution were to establish a policy, there would be an obligation to inform patients and families about the existence of that policy, as well as the parameters under which a decision to accommodate or not to accommodate was made. Some clarity would be gained, but significant context-specific flexibility and adaptability would be lost.
The Patient Bias and Preferences Algorithm incorporates recommendations from the literature regarding the importance of the agency of the clinician, especially learners,39–44 the need for learner-specific guidance and resources,28,40,42,45 clear documentation processes,29,32,43,46–48 and better communication with respect to the existence of these guidelines with patients.29,43,48,49 In addition, our quality improvement project identified the following 7 needs: (1) specific documentation based on the type of request or refusal made (i.e., incident reports, clinician notes in the electronic medical record); (2) data collection on the various types of requests/refusals and resolution, frequency of occurrence, identity of the requestor, clinical setting in question and impact on the clinician; (3) clear escalation pathways (including when to escalate and to whom); (4) identification of key organizational supports (such as Clinical and Organizational Ethics, Spiritual Care, Administrators on Site, Division Heads); (5) identification of the role of the preceptor and learner-specific resources; (6) context specific scripts and speaking prompts to support conversations with patients and family members at different points in the process; and (7) information on related organizational policies and processes (e.g., Workplace Violence and Harassment, Refusal to Work).
Whereas Anstey and Wright’s 29 foundational work is grounded primarily in human rights legislation, the revised guideline and algorithm incorporate both human rights legislation and occupational health and safety legislation as fundamental legal considerations with implications for the quality of staff experiences, employee well-being, and workforce retention. New federal legislation provides additional legal grounding to protect healthcare workers from violence. Bill C-3, which received royal assent in December 2021 created a new intimidation offence for behaviour intended to provoke fear in a healthcare professional in order to impede the performance of their duties. 50 Although not included in the revised guideline or algorithm, this new legislation includes legal ramifications for discriminatory behaviour from patients and families, beyond visitor restrictions.
The revised algorithm serves both informational and instructional purposes, enabling point-of-care healthcare workers to easily identify available procedural options and relevant resources. It is also intended to support managers and healthcare leaders in guiding their responses in ways that are sensitive to the needs and capacities of their patients and staff members. While the academic literature on this topic is expanding, there remains a significant need for increased knowledge dissemination and skill building in this area, particularly as interpersonal tensions continue to escalate.
Importantly, we do not intend the algorithm to be directly transposed to different healthcare contexts, but rather to prompt reflection, recognizing the shared challenges while respecting local differences. For settings outside of Ontario, we recommend that institutions draw on their own occupational health and safety legislation, anti-discrimination laws, and relevant human rights frameworks (which in many Canadian provinces, and in other countries reflect the protections outlined in Ontario’s policies), to develop equivalent approaches tailored to their specific regulatory and institutional contexts. Additionally, other hospitals often have comparable functions, even if named differently, such as committees to address violent behaviors or offices addressing health and safety, as well as anti-discrimination. Furthermore, many codes are standardized across institutions (e.g., Code Blue).
Conclusion
Healthcare workers, and the patients they serve, come from diverse backgrounds and it is impossible for healthcare institutions to be insulated entirely from the disturbing expressions of bias and interpersonal violence that occur in the wider community. This has always been true; but what has changed in recent years, perhaps in recognition of increasing incidents of aggression toward healthcare workers and the increased complexity of patient circumstances, is the expectation that healthcare leaders pay greater attention to the wellbeing of the workforce. In addition, it is now understood that employee recruitment and retention is linked inextricably to efforts to attend to staff members’ well-being, and that efforts to reduce non-physical harms are essential components of sustainable and ethically attuned institutions. Patient declarations of values, professional and institutional codes of ethics, and codes of conduct, are worthy, but insufficient, tools for advancing what is now described as the quadruple aim of healthcare.51,52 Put another way, an ethical workplace is one which strives for safety for all, and that entails a commitment to psychological as well as physical safety and respect for cultural diversity.
Our hope is that UHN’s revised and expanded Patient Bias and Preferences Guideline will assist those who struggle to find a practical, intuitive, and inclusive way of balancing patient and family requests with the responsibility to ensure a safe and respectful environment in which all are free to do their best work and where patients receive the highest quality of care.
Supplemental Material
Supplemental Material —Navigating discriminatory requests and refusals of healthcare workers: A Canadian-based inpatient hospital algorithm
Supplemental Material for Navigating discriminatory requests and refusals of healthcare workers: A Canadian-based inpatient hospital algorithm by Claudia Barned, Akosua Nwafor, and Ann Heesters in Nursing Ethics.
Supplemental Material
Supplemental Material —Navigating discriminatory requests and refusals of healthcare workers: A Canadian-based inpatient hospital algorithm
Supplemental Material for Navigating discriminatory requests and refusals of healthcare workers: A Canadian-based inpatient hospital algorithm by Claudia Barned, Akosua Nwafor, and Ann Heesters in Nursing Ethics.
Footnotes
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
