Abstract
Background
Individuals with intellectual and developmental disabilities (IDD) face significant health disparities, often exacerbated by ethical and legal complexities in nursing care. Nurses are frequently challenged to balance autonomy, informed consent, patient safety, and human rights, especially in settings with unclear guidelines or insufficient training. This narrative review explores the ethical and legal considerations in nursing care for individuals with IDD, aiming to highlight challenges and propose best practices.
Methods
A narrative review methodology was employed to synthesise evidence from qualitative, quantitative, mixed-methods studies, theoretical articles, and grey literature. A comprehensive search was conducted across PubMed, EBSCO, Embase, Scopus, and Web of Science, using keywords related to ethical issues, legal rights, nursing, and intellectual disability. Studies were included if they addressed the ethical or legal dimensions of nursing care for people with IDD. Data were synthesised narratively and visually mapped using conceptual mapping techniques. Quality was assessed using the SANRA scale.
Results
Eighteen studies met the inclusion criteria. The findings reveal ethical tensions in obtaining informed consent, maintaining autonomy, and ensuring dignity against communication barriers and behavioural challenges. Nurses reported experiencing an emotional burden and ethical uncertainty when institutional constraints limit person-centred care. The overuse of restrictive practices and limited access to tailored healthcare were recurrent concerns. Legal challenges included complexities in guardianship, consent to treatment, and discriminatory practices. Emerging issues, such as the ethical use of artificial intelligence in care planning, were also noted.
Conclusion
Nursing care for individuals with IDD requires ethically grounded, legally informed, and person-centred approaches. Best practices include accessible communication, interdisciplinary collaboration, tailored education, and advocacy. Nurses must receive support through training and organisational frameworks to navigate complex ethical decisions and uphold the dignity and rights of individuals with IDD. These findings have direct implications for nursing practice and policy, offering actionable guidance to improve ethical decision-making, communication, and inclusive care delivery for individuals with intellectual disabilities.
Keywords
Introduction
Individuals with intellectual and developmental disabilities (IDD) experience significant health disparities and often face challenges in accessing appropriate and equitable healthcare.1,2 These disparities are compounded by ethical and legal complexities that arise in the provision of nursing care. 3 Nurses, who are at the forefront of healthcare delivery, require a strong understanding of these dimensions to ensure optimal and ethical care for this vulnerable population.4,5 This understanding is particularly crucial given the increasing lifespan of individuals with IDD and the corresponding rise in chronic illnesses. 6
Ethical considerations in nursing care for individuals with IDD encompass a wide range of issues, including informed consent, decision-making capacity, respect for autonomy, and the balancing of beneficence and non-maleficence.3,7,8 Legal frameworks further shape the landscape of care, with regulations and guidelines impacting areas such as guardianship, advocacy, and the protection of rights. 9 Navigating these ethical and legal dimensions can be challenging for nurses, particularly in acute care settings where they may feel underprepared and face communication barriers. 10
The experiences of nurses caring for individuals with IDD are shaped by various factors, including their education, training, attitudes, and the availability of resources.4,11,12 Understanding these experiences is vital for developing effective strategies to support nurses and improve the quality of care. 1 Furthermore, exploring the impact of intellectual disability nursing interventions is essential to inform best practices and promote positive outcomes. 13
The narratives of caregivers offer essential perspectives on the ethical complexities inherent in supporting individuals with intellectual and developmental disabilities. Caregivers often grapple with moral dilemmas and ethical challenges related to autonomy, informed consent, and quality of life for the individuals they support.14,15 Understanding these narratives provides a framework for addressing these intricate issues. Centring on the stories and experiences of patients and caregivers highlights the significance of acknowledging each individual’s viewpoint and encourages person-centred care. Additionally, it recognises the concept of “disabled authorship” that individuals with IDD often encounter and aims to empower them in crafting their narratives. 16 Disabled authorship refers to the challenges individuals with IDD face in expressing themselves and creating their narratives, while also emphasising efforts to empower them in this area. 17
This paper presents a narrative review of the literature exploring the ethical and legal dimensions of nursing care for individuals with intellectual disabilities. By synthesizing existing research, this review aims to: (1) identify key ethical and legal challenges faced by nurses; (2) examine the experiences of nurses in providing care; (3) explore the role of narrative ethics in promoting ethical practice; and (4) highlight strategies for improving nursing education and support to ensure equitable and ethical care for individuals with IDD. This review contributes to a deeper understanding of the complexities within this field. It provides a foundation for future research and practice development to promote the well-being and rights of individuals with intellectual disabilities. 18 Furthermore, the increasing application of Artificial Intelligence (AI) in healthcare, including nursing,19,20 introduces new ethical considerations that must be addressed in caring for individuals with IDD. The potential benefits and risks of using AI to support nursing care for this population warrant careful examination.
Methods
This narrative review aims to synthesise existing literature on the ethical and legal considerations of nursing care for individuals with intellectual disabilities. A narrative approach was chosen to allow for a broad and flexible synthesis of diverse perspectives and study designs. 21 Unlike systematic reviews with strict inclusion/exclusion criteria, a narrative review allows for the inclusion of a broader range of evidence, including qualitative studies, theoretical papers, and expert opinions.
Search strategy
Search terms and strategy used to identify literature on ethical and legal dimensions of nursing care for individuals with intellectual disabilities.

Inclusion and exclusion criteria
Studies were included if they explored ethical or legal dimensions related to individuals with intellectual disabilities in nursing care. Studies were excluded if they: (a) were not available in English; (b) did not directly address the research question.
Study selection
Retrieved articles were initially screened based on their titles and abstracts to determine their relevance to the research question. Full-text articles of potentially eligible studies were retrieved and assessed against the inclusion and exclusion criteria. A PRISMA flow diagram
22
was used to document the study selection process, see Figure 1. The PRISMA 2020 flow diagram shows the selection process of included studies.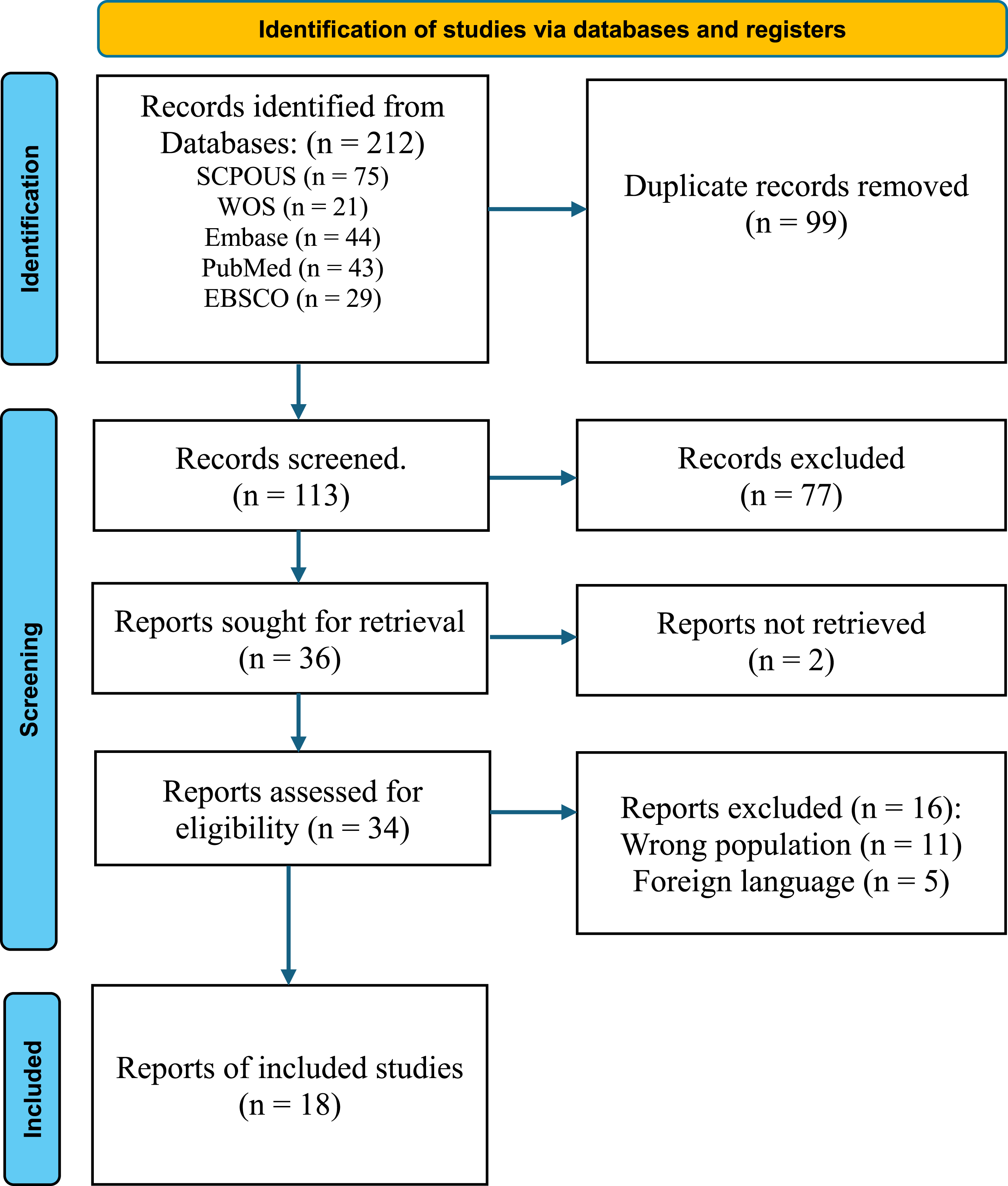
Data extraction and synthesis
Data were extracted from the included studies using a standardised data extraction form. The extracted data included study design, sample characteristics, key findings, and relevant conclusions. The extracted data were then synthesised using a narrative approach. This involved identifying common themes, patterns, and contradictions across the studies and developing a coherent narrative that addresses the research question. As part of this synthesis process, a conceptual mapping technique was employed to visually represent the thematic connections within the ethical and legal dimensions of nursing care for people with intellectual disabilities. Key concepts were derived from the thematic analysis of the included literature, focusing on topics related to nursing ethics, care delivery, health equity, and patient rights. The central concept, “Ethical and Legal Dimensions in Nursing Care,” was placed at the core, with branches extending to thematically related areas such as nurse-patient relationship, care planning, health inequality, and human rights. This visual representation, Figure 2, supported the narrative synthesis by clarifying the multidimensional nature of ethical considerations in nursing care and highlighting their relevance to the care of individuals with intellectual disabilities. Special attention was paid to the methodological rigour of the included studies, and limitations were noted. Conceptual map of ethical and legal dimensions in nursing care for people with intellectual disabilities: Thematic linkages to key nursing and healthcare topics.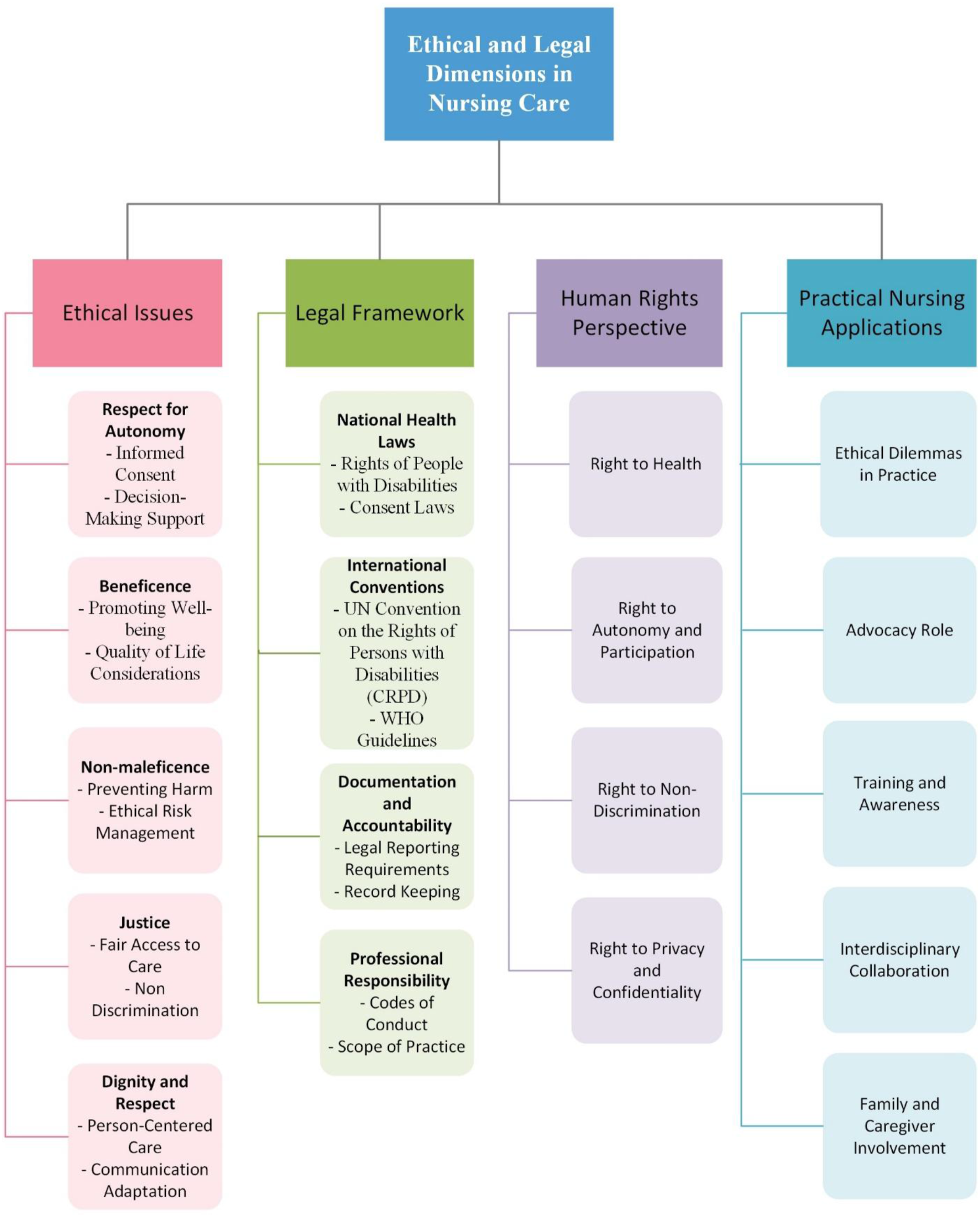
Quality assessment
Given the nature of a narrative review, the Scale for the Assessment of Narrative Review Articles (SANRA) was used. 23 The strengths and weaknesses of different study designs were acknowledged, and the potential for bias was considered. We acknowledge that the inclusion of studies with varying designs (e.g., qualitative, quantitative, and mixed methods) introduces the potential for methodological bias. Although a formal appraisal of study quality was not conducted, we sought to manage this limitation by carefully describing the characteristics and contexts of each included study. During the synthesis process, we paid close attention to differences in study design, data collection methods, and scope, and we interpreted the findings with caution to avoid overgeneralization. This reflective approach was intended to enhance transparency and support a balanced interpretation of the evidence.
Results
Search outcomes
A total of 212 papers were identified through databases and grey literature searches. After removing duplicates using EndNote, 113 articles remained and were screened by title and abstract. This screening led to the exclusion of 77 articles, leaving 36 for further review. Of these, 2 articles could not be retrieved, so 34 articles were screened for eligibility. After full-text screening, 16 articles were excluded for the following reasons: wrong population 11, and 5 foreign language articles. Ultimately, 18 articles were included in the study: four quantitative, seven qualitative, and one mixed methods study. Figure 1 illustrates the study screening and selection process.
Narrative synthesis
Summary of ethical and legal challenges in nursing care for individuals with intellectual and developmental disabilities: Findings from 18 included studies.

The persistent misuse or overuse of restrictive practices, such as physical restraints or sedation, is reported in studies,27,30,31,34,39 raising critical concerns about human rights and the ethical use of power in caregiving relationships. Restrictive practices are intentional interventions that limit a person’s freedom or autonomy, often employed to manage risk or maintain order.46–51 A lack of formal education and ethical training specific to IDD populations is a barrier noted in several studies,25,28,35,40,41 leaving practitioners feeling underprepared and unsupported. Structural limitations, including poor access to specialised palliative care or healthcare tailored to the needs of people with IDD, are further documented in studies.29,32,38,40,41 Collectively, these studies call for ethically grounded, person-centred care frameworks that integrate narrative, relational, and human rights-based approaches. They also highlight the necessity for training, ethical leadership, and policy reforms to support nurses and midwives in advocating effectively for this marginalised population.
Thematic synthesis
In Figure 2, the conceptual map developed in this study illustrates the core ethical and legal dimensions relevant to nursing care for individuals with intellectual disabilities. It comprises four interrelated domains: ethical issues, legal framework, human rights perspective, and practical nursing applications. Under ethical issues, key principles include respect for autonomy, emphasising informed consent and decision-making support; beneficence, which focuses on promoting well-being and quality of life; non-maleficence through harm prevention and ethical risk management; justice, encompassing fair access to care and non-discrimination; and the promotion of dignity and respect via person-centered care and communication adaptation.
The legal framework comprises multiple layers, beginning with national health laws that govern the rights of people with disabilities and consent-related matters. This is supported by international conventions such as the UN Convention on the Rights of Persons with Disabilities (CRPD) and WHO guidelines. Furthermore, legal dimensions extend to documentation and accountability, which cover legal reporting requirements and record keeping, as well as professional responsibility, defined by codes of conduct and scope of practice standards.
The human rights perspective highlights key entitlements, including the right to health, the right to autonomy and participation, the right to non-discrimination, and the right to privacy and confidentiality. Finally, the practical nursing applications encompass ethical dilemmas encountered in clinical practice, the advocacy role of nurses, the importance of ongoing training and awareness, interdisciplinary collaboration, and the engagement of families and caregivers. This conceptual framework serves to guide ethical decision-making and ensure legally compliant and rights-based care for individuals with intellectual disabilities.
The results reveal multifaceted ethical and legal challenges faced by nurses caring for individuals with intellectual disabilities, highlighting tensions between autonomy, safety, and legal responsibilities. Building on these findings, the following discussion explores their practical implications for nursing practice, education, and policy, and proposes strategies to address identified gaps and promote person-centred, rights-based care.
Discussion
Nursing care for individuals with intellectual developmental disabilities (IDD) encompasses complex ethical and legal dimensions. These are essential for ensuring that care is both effective and respectful of the rights, autonomy, and individual needs of this vulnerable population. 8 This discussion outlines key ethical and legal challenges, along with best practices to guide nursing professionals.
Ethical challenges
Informed consent and autonomy
Obtaining informed consent from individuals with IDD can be challenging due to potential cognitive impairments.25,35 Nurses must communicate information in accessible formats, using simplified language, visual aids, or alternative communication strategies. 35 Respecting autonomy means supporting individuals in making their own decisions, even when these differ from caregivers’ or professionals’ views.25,52 Balancing autonomy with patient safety is a central ethical concern. 25 Caregivers’ long-term relationships with individuals with intellectual and developmental disabilities (IDD) provide unique insights into their needs and preferences, especially for non-verbal individuals. 53 Recognising and valuing caregivers is critical for person-centred care.54–56 Simultaneously, empowering individuals with IDD to express their own choices is essential for promoting autonomy and respecting their rights.57–59 Balancing caregiver insights with individual empowerment is a key challenge in providing holistic and rights-based care.
Best interests decision-making
When individuals lack decision-making capacity, healthcare professionals must act in their best interests. 33 This requires consideration of the individual’s values, preferences, and overall well-being, with input from family members, caregivers, and interdisciplinary teams.33,60
Access to services
Individuals with IDD often face systemic barriers in accessing general and specialised healthcare, including palliative care.2,61 Addressing issues such as provider bias, communication challenges, and transportation barriers is an ethical imperative to promote health equity. 2 The COVID-19 pandemic significantly impacted access to healthcare services for individuals with intellectual disabilities (IDD), exacerbating existing health disparities and creating new challenges.62–64 In the United States, the COVID-19 pandemic has had a particularly severe impact on individuals with intellectual disabilities. Studies have found that having an intellectual disability was one of the strongest independent risk factors for receiving a COVID-19 diagnosis, and, aside from older age, was also one of the highest risk factors for COVID-19-related mortality. 65
End-of-life care
Palliative and end-of-life care for individuals with ID demands attention to their unique physical, emotional, and spiritual needs. 61 Ethical considerations include pain management, respecting individual preferences, and making life-sustaining treatment decisions in line with the patient’s expressed wishes or, when unavailable, their best interests. 3 Literature reviews have highlighted key barriers to equitable end-of-life care for individuals with intellectual disabilities, including diagnostic overshadowing, delayed recognition of symptoms, and inadequate healthcare adjustments. 66 Studies emphasise the importance of tailored communication, emotional sensitivity, and the active inclusion of individuals with intellectual disabilities in care planning. 67 Additionally, there is an ethical imperative to embed equity, dignity, and cross-national standards into palliative care for this population. 68
Ethical competence
Nurses’ ability to navigate ethical challenges is deeply influenced by their ethical competence, which encompasses not only attitudes toward ethical behavior, perceived behavioural control, and social norms, 69 but also a foundational understanding of professional codes of ethics. Documents such as the ICN and ANA Codes of Ethics provide essential guiding principles for clinical integrity and professional conduct.70,71 Ethical competence also involves knowledge of ethical theories, such as deontology, utilitarianism, and principlism, which offer structured perspectives for resolving moral dilemmas. 72 In practice, decision-making frameworks like Robichaux’s Four-Component Model or integrative models reviewed by Mallari 73 support nurses in applying ethical reasoning systematically. As Lechasseur et al 74 emphasise, ethical competence is not static; it evolves with education, experience, and moral reflection, shaping the intention and capacity to deliver patient-centred, ethically sound care.
Self-determination versus protection
While self-determination is a fundamental health law principle, it may not always serve individuals with IDD adequately. Alternative principles, such as the right to receive appropriate care and developmental support, may provide better protection in certain situations. 75
Contraceptive choices
Decisions regarding contraception for women with IDD involve complex ethical and legal considerations. Informed consent is essential, and any decision, especially irreversible methods such as sterilisation, must not be made for eugenic reasons, which are both ethically and legally unacceptable.76,77
Legal challenges
Guardianship
Legal guardianship allows a designated person to make decisions for individuals who lack capacity. 33 While it serves to protect vulnerable individuals, it may also restrict autonomy. Therefore, guardianship should be applied only when absolutely necessary, ensuring that the individual’s rights and preferences are upheld. 33
Consent to treatment
Valid consent is a legal requirement, but assessing and obtaining it from individuals with IDD can be particularly challenging. 35 Legal frameworks must guide the evaluation of decision-making capacity and establish procedures for substitute decision-making when needed. The use of psychotropic medication also raises legal and ethical concerns, necessitating careful oversight to avoid misuse and ensure informed consent. 78
Discrimination and inequity
Individuals with IDD are protected against discrimination under various laws and regulations. 79 Despite these protections, many experience health disparities due to systemic inequities. Nurses have a critical role in advocating for reasonable adjustments, promoting inclusion, and ensuring equitable access to healthcare services.37,79,80
Emerging legal-ethical considerations
With advances in healthcare technologies, new legal-ethical considerations are emerging. For example, the use of large language models (LLMs) in clinical decision-making raises concerns around data privacy, consent, and transparency—issues particularly sensitive in the care of individuals with cognitive impairments.52,81
Best practices for nurses
Person-centered care
Providing individualised, person-centred care is fundamental. This approach requires nurses to understand each patient’s unique preferences, values, and goals, and to tailor interventions accordingly. 79
Effective communication
Clear, simple language and alternative communication strategies are essential. Nurses must also be attentive to nonverbal cues and involve family members or caregivers when appropriate to support understanding and decision-making. 35
Collaborative practice
Interdisciplinary collaboration, including healthcare teams, caregivers, and family members, supports comprehensive care planning and ethical decision-making. Coordination of services enhances care quality and helps resolve ethical and legal dilemmas.2,7,82
Education and training
Nurses require ongoing education to address ethical, legal, and practical challenges in caring for individuals with IDD. Training should focus on capacity assessment, legal frameworks, communication techniques, and strategies for resolving ethical dilemmas.10,25,35,83
Advocacy
Nurses play a vital role in advocating for the rights, dignity, and needs of individuals with ID. This includes challenging discriminatory practices, improving service accessibility, and influencing policy development.37,84
Resilience and support
Working with individuals with IDD can present emotional and professional challenges. Developing resilience and ensuring organisational support for nurses are essential to sustaining ethical, compassionate care. 10 As life expectancy for individuals with intellectual and developmental disabilities (IDD) continues to increase, many are now outliving their family caregivers, raising significant ethical and practical challenges for long-term care planning. 85 This demographic shift underscores the urgent need for sustainable support systems to ensure continuity of care when aging parents or relatives are no longer able to provide caregiving support. 86 The absence of adequate future planning can result in crises in placement, caregiver burnout, and diminished quality of life for the person with IDD. 87 To address this, healthcare providers, social services, and policymakers must work collaboratively to develop person-centered care plans that incorporate legal guardianship arrangements, supported living pathways, and the proactive engagement of alternative caregivers or formal support systems. 88 Responding to these needs is a vital step toward providing ethically sound, equitable, and sustainable care for individuals with IDD.
Limitations
This narrative review has several limitations that should be acknowledged. First, although the review included a broad range of sources, including grey literature, the search was limited to articles published in English, which may have excluded relevant studies published in other languages and introduced a language bias. Second, as a narrative review, the study did not follow a formal systematic review protocol or meta-analytic procedures, which may limit the reproducibility and objectivity of the findings. While quality assessment was conducted using the SANRA scale, no standardised tool was used to appraise the methodological quality of the empirical studies included, which may affect the robustness of the conclusions drawn.
Furthermore, the inclusion of diverse study designs (qualitative, quantitative, and mixed methods) and theoretical papers led to a heterogeneous body of literature, making it difficult to compare findings directly or generalise outcomes. The review also primarily reflects the perspectives of nurses and healthcare professionals, with limited representation of the voices of individuals with intellectual disabilities and their families. This may result in an incomplete understanding of ethical and legal challenges from the service user’s standpoint.
Lastly, while conceptual mapping was used to illustrate key themes, the subjective nature of this technique may influence interpretation. Future studies should adopt more rigorous synthesis methods and incorporate stakeholder perspectives, especially those of individuals with intellectual disabilities, to ensure a more comprehensive and inclusive understanding of ethical and legal issues in nursing care.
Conclusion
Nursing care for individuals with intellectual disabilities involves navigating intricate ethical and legal landscapes. By adhering to best practices, such as person-centred care, effective communication, interdisciplinary collaboration, ongoing training, and advocacy, nurses can uphold the rights and dignity of individuals with IDD. Continued education, ethical competence, and systemic support are key to delivering high-quality, equitable care. Future research should prioritise the inclusion of first-person perspectives from individuals with intellectual disabilities to ensure that their voices and lived experiences shape ethical and legal frameworks in nursing care. Methodological strategies to support this include the use of accessible language, visual aids, simplified consent processes, and participatory research approaches such as inclusive interviews, photovoice, or involving individuals with ID as co-researchers. These approaches not only promote ethical integrity but also help bridge the gap between theory and lived experience, ensuring that care models are both rights-based and person-centred.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
This study did not involve the generation or analysis of primary data. All data presented in this paper are derived from publicly available sources, including published literature, legal documents, and international guidelines. Further information regarding the sources is available from the corresponding author upon reasonable request.
