Abstract
Introduction
Headache is one of the most frequent neurological symptoms in SLE; however, its definition and relationship with the disease remain unclear. Distinguishing whether a headache is attributable to lupus or represents a primary headache disorder can be challenging. This preliminary study aimed to investigate the prevalence, frequency, and associated clinical factors of primary headaches in juvenile-onset SLE (jSLE) compared to healthy peers.
Methods
This cross-sectional case-control study included 32 children with jSLE and 38 age- and sex-matched healthy controls, who were evaluated between July and September 2025. Headache characteristics were assessed using a standardized questionnaire and classified according to the International Classification of Headache Disorders, 3rd edition (ICHD-3). All participants underwent neurological and fundoscopic examinations. Clinical, laboratory, and treatment-related parameters including disease activity (SLEDAI-2K), cumulative dose of systemic corticosteroids, and autoantibody profiles were compared between jSLE patients with and without primary headache.
Results
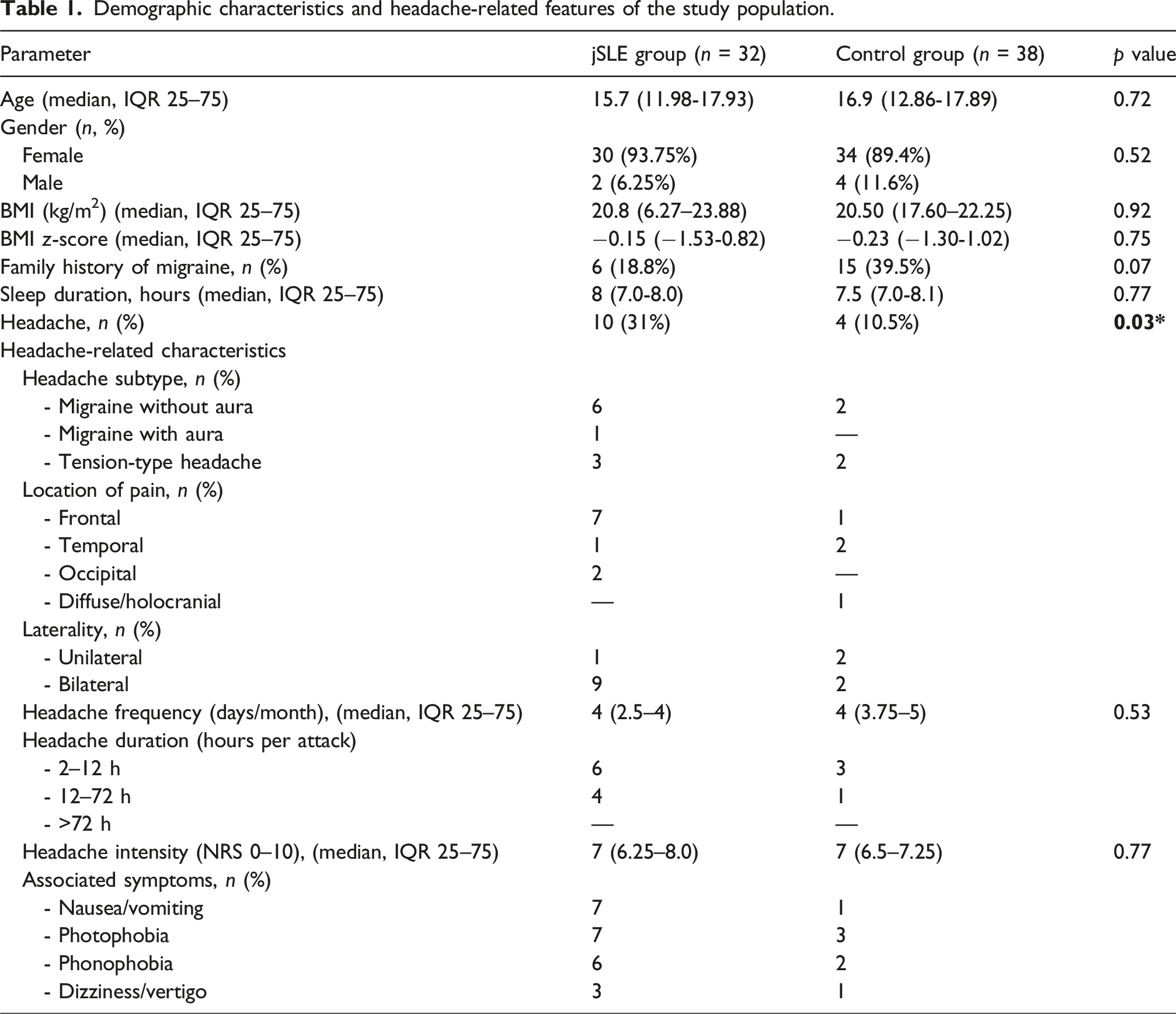
Primary headache was observed in 31.3% of jSLE patients (10/32) and 10.5% of controls (4/38) (p = 0.03). Among jSLE patients with headache, migraine without aura (60%) and tension-type headache (40%) were the predominant subtypes. Compared with those without headache, patients with headache had higher BMI z-scores (p = 0.03), shorter sleep duration (p = 0.03), more frequent antiphospholipid antibody positivity (p = 0.04), and higher cumulative corticosteroid doses (p = 0.02). Disease activity and duration did not differ significantly.
Conclusion
Primary headaches, particularly migraine, are more frequent in pediatric lupus compared to healthy controls. Their associations with BMI, sleep, antiphospholipid antibodies, and corticosteroid exposure suggest multifactorial origins rather than direct links to disease activity. These findings highlight the need for larger, prospective studies to clarify underlying mechanisms.
Introduction
Juvenile-onset systemic lupus erythematosus (jSLE) is a rare but severe multisystem autoimmune disease characterized by chronic inflammation, which may involve virtually any organ system and is associated with considerable morbidity and mortality. 1 Neuropsychiatric involvement in systemic lupus erythematosus (SLE) is reported more frequently in pediatric-onset cases than in adult-onset, with prevalence in children ranging from 14% to 75%, reflecting heterogeneity in diagnostic approaches and cohort composition.2,3 Previous cohort studies have also demonstrated that pediatric-onset SLE may present with more severe systemic involvement compared with adult-onset disease, including higher frequencies of renal involvement, hematologic abnormalities, and neuropsychiatric manifestations. 4 In addition, long-term follow-up studies have shown that a substantial proportion of children with SLE develop irreversible organ damage, particularly affecting renal and neuropsychiatric domains, highlighting the significant disease burden in this population. 5
Neuropsychiatric involvement represents one of the most complex manifestations of SLE and encompasses a broad spectrum of neurological and psychiatric syndromes affecting both the central and peripheral nervous systems. The American College of Rheumatology has defined 19 neuropsychiatric syndromes associated with SLE, including seizures, cerebrovascular disease, cognitive dysfunction, psychosis, mood disorders, and headache. 6 Although neuropsychiatric manifestations are not included as individual items in the 2019 European Alliance of Associations for Rheumatology/American College of Rheumatology (EULAR/ACR) classification criteria, 7 they remain clinically important features of the disease and are widely recognized as part of the neuropsychiatric SLE spectrum.
Headache is one of the most frequently reported neurological features in SLE. The American College of Rheumatology has included “lupus headache” among the case definitions of neuropsychiatric SLE, describing it as a severe, persistent headache, often migrainous in nature, and unresponsive to narcotic analgesics. 6 However, this definition remains controversial, and distinguishing disease-related headache from primary headache disorders such as migraine or tension-type headache continues to be a clinical challenge.
The pathophysiology of headache in SLE is complex and likely multifactorial. Proposed mechanisms include immune-mediated neuronal injury, small-vessel vasculopathy, blood–brain barrier disruption, and cytokine-driven neuroinflammation. 8 Additional factors such as antiphospholipid antibody–related vascular dysfunction, increased intracranial pressure, and treatment-related effects may also contribute to headache development in patients with SLE.
The objective of this study was to delineate the prevalence and phenotypic features of primary headaches in pediatric SLE relative to healthy peers, and to investigate clinical and laboratory correlates of headache within the jSLE population.
Methods
Study design and participants
This cross-sectional, case control study was performed at a tertiary pediatric rheumatology center between July 2025 and September 2025. The study compared jSLE patients with age- and sex-matched healthy controls and further examined within-cohort differences between jSLE patients with and without primary headache.
Children diagnosed with SLE before 18 years of age who fulfilled either the 2019 EULAR/ACR classification criteria or the 2012 Systemic Lupus International Collaborating Clinics classification criteria, and who were in regular follow-up at pediatric rheumatology outpatient clinic, were included in the study.7,9,10 Exclusion criteria for the jSLE group were a history of or current neuropsychiatric SLE, seizures attributed to SLE, cerebrovascular events, demyelinating disease, abnormal brain MRI findings related to SLE, uncontrolled hypertension, or other neurological conditions that could cause secondary headache. Healthy children without chronic medical conditions or neurological diseases were recruited from general pediatric clinics. Children with abnormal neurological examination, neurological disorders, uncontrolled hypertension, or secondary cause were excluded.
For all participants, demographic and clinical characteristics were collected, including age, sex, height, weight, body mass index, average sleep duration, and family history of headache. The Body Mass Index (BMI) of participants was calculated by dividing body weight (kg) by height squared (m2), and the standard deviation score (SDS) was determined using national reference data. 11
Disease-related variables (jSLE cohort)
Additional disease-specific data, comprising age at onset, disease duration, and measures of activity and damage assessed by the Systemic Lupus Erythematosus Disease Activity Index 2000 (SLEDAI-2K) and the Systemic Lupus International Collaborating Clinics/American College of Rheumatology Damage Index (SDI) were retrieved from patient files.12,13 The diagnosis of lupus nephritis was based on either kidney biopsy findings classified according to the International Society of Nephrology/Renal Pathology Society (ISN/RPS) 2003 criteria. 14
Treatment data encompassed current and cumulative corticosteroid exposure (expressed as milligrams per kilogram and milligrams per day), as well as the use of hydroxychloroquine, mycophenolate mofetil, azathioprine, methotrexate, rituximab, cyclophosphamide, and other immunosuppressive agents.
Laboratory results closest to the headache assessment date (±14 days) included antinuclear antibody, anti-double-stranded DNA antibody, complement C3 and C4 levels, erythrocyte sedimentation rate, and C-reactive protein. The antiphospholipid antibody profile, which included lupus anticoagulant, anticardiolipin immunoglobulin G and M, and anti-β2-glycoprotein I immunoglobulin G and M, was also documented.
Headache assessment and classification
All participants were interviewed using a standardized questionnaire that assessed the presence of headaches, frequency (number of days per month), laterality, character, intensity on a 0–10 numerical rating scale, associated symptoms (such as nausea, vomiting, photophobia, and phonophobia), and impact on daily activities. Headache duration was classified into three categories according to the International Classification of Headache Disorders (ICHD-3) criteria: short duration (2–12 h per attack), intermediate duration (12–72 h per attack), and prolonged duration (>72 h per attack). 15 Headaches were classified as migraine with aura, migraine without aura, tension-type headache, or other primary headache syndromes according to ICHD-3.
All participants were also evaluated by a pediatric neurologist and those with headache underwent fundoscopic examination to exclude intracranial hypertension or other secondary causes.
Statistical analysis
Continuous variables were summarized as mean ± standard deviation or median (interquartile range), and categorical variables as counts and percentages. The primary analysis compared the prevalence of primary headache between SLE patients and healthy controls using chi-square or Fisher’s exact tests, with risk ratios and 95% confidence intervals reported.
Secondary analyses examined the distribution of headache subtypes within the SLE cohort and compared patients with and without primary headache regarding demographic, clinical, treatment-related, and laboratory characteristics. Continuous variables were compared using Student’s t-test or Mann–Whitney U test, and categorical variables using chi-square or Fisher’s exact tests, as appropriate. Statistical significance was set at p < 0.05. Analyses were conducted using SPSS software (version 26.0, IBM Corp.).
Ethical considerations
The study was conducted in accordance with the ethical standards of the Declaration of Helsinki. Written informed consent was obtained from all participants or from the parents/guardians of underage children. The study protocol received approval from the Institutional Ethics Committee of Istanbul University, Istanbul Faculty of Medicine (approval date: 25.06.2025; approval number: 3429685).
Results
Demographic characteristics and headache-related features of the study population.
Comparative analysis of juvenile-onset systemic lupus erythematosus patients according to presence of headache.
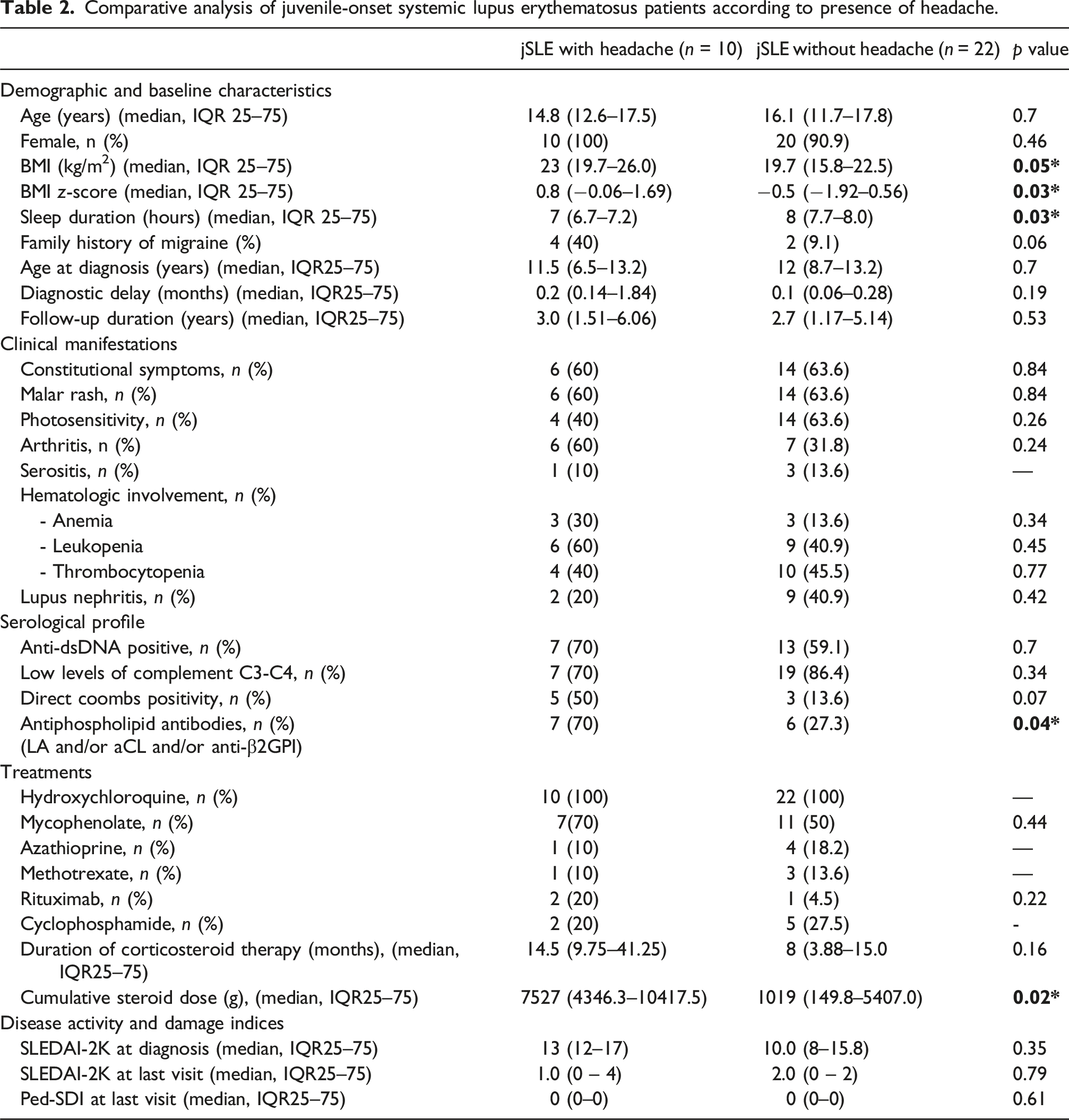
Discussion
To our knowledge, this is the first study to systematically evaluate primary headache disorders in a juvenile-onset SLE cohort using standardized ICHD-3 criteria, and uniquely incorporating a comparison with healthy controls. Primary headaches were observed in about one-third of jSLE patients, significantly more frequent than in healthy controls. Within the jSLE cohort, patients with headache had a higher BMI z-score, shorter sleep duration, more frequent positivity for antiphospholipid antibodies, and a higher cumulative exposure to corticosteroids compared with those without headache, whereas disease activity and organ involvement did not differ between the groups.
In a recent meta-analysis of adult SLE patients, Feld et al. reported a pooled prevalence of 26.8% for primary headaches, with rates comparable to healthy controls. 16 Although the prevalence in our jSLE cohort was similar (31.3%), it was significantly higher than that of healthy peers, possibly reflecting the lower baseline prevalence of headache typically observed in pediatric populations. The most common headache subtype in our cohort was migraine without aura, followed by tension-type headache. Cajado et al. evaluated 34 jSLE patients, equally divided into those with and without headache, and similarly reported migraine as the most frequent subtype, highlighting its predominance in the headache profile of this population. 17 However, a recent meta-analysis of primary headaches in the general pediatric population revealed tension-type headache as the most common subtype. 18 These findings suggest that the headache profile in jSLE may be influenced, at least in part, by disease-specific mechanisms such as systemic inflammation or treatment exposures, rather than fully mirroring the distribution observed in the general pediatric population.
Although a family history of migraine was more frequently reported among jSLE patients with headache than among those without (40% vs 9.1%, p = 0.06), this difference did not reach statistical significance. This trend is consistent with evidence that family history is a strong and well-established risk factor for migraine in the pediatric population, but our sample size may have been insufficient to demonstrate a significant association.19,20
The median BMI z-score in our jSLE cohort was within the normal range in both subgroups but was significantly higher in patients with headache (p = 0.03). A recent systematic review by Quispe-Vicuña et al. suggested that excess weight may increase the risk of migraine in pediatric populations, although the certainty of the evidence was low due to methodological limitations. 21 Our findings may indicate that even modest differences in BMI could contribute to headache susceptibility in jSLE, but this needs to be confirmed in larger, longitudinal studies.
Sleep disturbance is a well-known trigger and aggravating factor for both migraine and tension-type headaches in children and adolescents. 22 In our study, jSLE patients with headaches reported shorter sleep duration compared to those without headaches (p = 0.03). In chronic conditions such as SLE, optimizing sleep may be a simple yet important strategy to reduce headache burden.
Disease activity scores at diagnosis and at the time of evaluation (SLEDAI-2K), as well as the frequency of major organ involvement, were similar between jSLE patients with and without headache in our cohort. Previous studies have shown that most headaches in SLE are not directly linked to active neuropsychiatric disease, and systemic activity markers such as SLEDAI, anti-dsDNA, and complement levels are not consistently correlated with neuropsychiatric symptoms.23,24 In our cohort, patients with headache showed a higher frequency of antiphospholipid antibody positivity. A recent large multicenter Turkish study including 1,107 children with jSLE identified antiphospholipid antibody positivity as an independent predictor of neurological damage. 25 Although headaches in our cohort fulfilled the ICHD-3 criteria for primary headache after excluding overt neuropsychiatric involvement and structural abnormalities, their higher prevalence in jSLE compared with healthy peers suggests that disease-related factors may still contribute. In our cohort, cumulative corticosteroid exposure was higher in patients with headache than in those without, while hydroxychloroquine use did not differ between groups. This finding may indicate that patients with headache required higher cumulative steroid doses to achieve comparable disease control despite similar disease activity scores.
Previous studies have reported conflicting findings regarding treatment-related factors. In a large SLICC cohort of 1,732 SLE patients, Hanly et al. found no significant association between corticosteroid use and the presence of headache, 9 whereas Weder-Cisneros et al. reported that hydroxychloroquine treatment was associated with a reduced risk of headache. 26 In addition, the observed associations with antiphospholipid antibody positivity and higher BMI in our cohort further support the possibility that both disease-related and treatment-related mechanisms may influence headache susceptibility. Consequently, some headaches classified as primary may still reflect underlying disease processes rather than purely idiopathic disorders.
The relatively small size of the jSLE cohort represents an important limitation of this study and reduced the ability to perform multivariable analyses to disentangle the potential effects of corticosteroid exposure from other variables such as BMI z-score, antiphospholipid antibody positivity, and sleep duration. In addition, sleep duration was assessed through self-report rather than objective measurements, which may have introduced recall bias. Therefore, the proposed multifactorial origin of headache in jSLE should be considered hypothesis-generating. Larger prospective and multicenter studies with appropriate multivariable modeling are needed to confirm these observations and better clarify the clinical determinants and mechanisms of headache in jSLE. 27 A major strength of this study is that it is the first to systematically characterize primary headache disorders in jSLE using standardized ICHD-3 criteria and to directly compare findings with age- and sex-matched healthy controls.
In conclusion, primary headaches appear to be more common in jSLE than in healthy peers, with migraine representing the most frequent subtype. The observed associations with higher BMI, shorter self-reported sleep duration, antiphospholipid antibody positivity, and greater cumulative corticosteroid exposure suggest that headache occurrence in jSLE may have a multifactorial background involving both general pediatric risk factors and disease-related mechanisms. These findings highlight the potential importance of considering headache symptoms in the clinical evaluation of patients with jSLE and support the need for larger prospective and multicenter studies to further clarify the underlying mechanisms and their implications for patient management.
Footnotes
Acknowledgements
Authors are grateful to all patients and their families.
Ethical considerations
The study protocol was approved by the Ethics Committee of Istanbul University (Approval No: 3429685).
Consent to participate
Informed consent was obtained from all individual participants included in the study. Patients’ data were treated to guarantee confidentiality.
Author contributions
BM and GKK conceptualized the study and drafted the initial manuscript. BM, SDA, and AD contributed to data collection and clinical evaluation of patients. AD, ÖA, CB, FGD, and FÇ contributed to patient recruitment, data acquisition, and clinical database management. HMG and EPY provided neurological evaluation and contributed to headache classification. AD and ÖA participated in the statistical analysis and data interpretation. NAA supervised the study design, data analysis, and manuscript revision. All authors reviewed and approved the final version of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
