Abstract
Background:
Synthetic cathinone abuse is a global health issue. Synthetic cathinones emerged in Taiwan in 2009, and their prevalence rapidly rose. They are usually made into “instant coffee packets,” and these so-called “toxic coffee packets” may also contain psychoactive drugs other than synthetic cathinones. Due to the diversity of the ingredients, clinical presentations can be complex.
Methods:
Retrospective analysis of emergency department (ED) patients who reported ingesting toxic coffee packets at three Chang-Gung Memorial Hospitals located in northern Taiwan between January, 2015 and December, 2019.
Results:
Sixty patients were included. Their mean age was 28.85 ± 9.24 years and 47(78.33%) were male. The most common presentations were palpitation, agitation, hallucination, and altered consciousness. Tachycardia and hypertension were common, while hyperthermia was observed in only three patients. Three patients (5%) developed rhabdomyolysis, and one underwent transient hemodialysis. Most patients were discharged from the ED, but 15(25%) were admitted, of whom nine (15%) were admitted to the intensive care unit (ICU), and one eventually died. Confirmation tests (mass-spectrometry-based analysis) were available in 10 patients; all reported positive for at least one type of synthetic cathinone. Polysubstance exposure was common. In multivariate logistic regression analyses, Glasgow coma scale ≤13 and the presence of seizure were associated with ICU admission.
Conclusion:
Patients who report ingesting toxic coffee packets are very likely to have been exposed to synthetic cathinones. Polysubstance exposure is common following ingestion. Cardiovascular and neurological symptoms are the main presentations, and severe complications such as rhabdomyolysis and life-threatening dysrhythmia can occur.
Introduction
New psychoactive substances (NPS), usually considered to be substances with stimulant properties that are not controlled by the Single Convention on Narcotic Drugs of 1961 or the Convention on Psychotropic Substances of 1971, have become a threat to public health in many countries.1,2 NPS involve several classes of drugs, of which synthetic cathinones are a major type used for recreational purposes.3,4 By mid-2019, the United Nations Office on Drugs and Crime (UNODC) listed a total of 964 substances on their NPS database, of which 169 were cathinone derivatives. 5
Cathinone is a naturally occurring β-ketone analog of amphetamine found in the leaves of khat (Catha edulis), a plant indigenous to northeast Africa and the Arabian Peninsula. 6 Synthetic cathinones are human-made cathinone derivatives that directly and indirectly activate the sympathetic nervous system resulting in pharmacological effects similar to those of amphetamine and 3,4-methylenedioxy-methamphetamine (MDMA). The first synthetic cathinone, methcathinone, was synthesized in 1928, followed by the synthesis of mephedrone in 1929. 7 Methcathinone was initially used in the former Soviet Union as an antidepressant in the 1930s but was removed from the market due to its strong addictive potential. 8 In 2007, reports of mephedrone use emerged, first in Israel and then in four other countries. 7 In 2009 and 2010, the abuse of synthetic cathinones (especially mephedrone) became prevalent in Western Europe. 9 Abuse of synthetic cathinones also appeared in the United States in 2010, mainly methylenedioxypyrovalerone (MDPV) and methylone, and increased rapidly over the next few years. 6
In Western countries, synthetic cathinones are frequently sold as “bath salts” despite having no such purpose. 6 They can also be made into other products, such as traditional tablets/pills, plant food/fertilizer, insect repellant, pond cleaner, and vacuum fresheners, 10 and may be sold as different products in different countries. 11 They are usually insufflated or swallowed in powder or crystal form but can also be administered by smoking, mucosal delivery, or injection via intramuscular or other routes. 12
Synthetic cathinones emerged in the Taiwan illicit drug market in 2009, 13 and their prevalence rapidly rose.14,15 They were made or mixed into various products, 16 and among them, instant coffee packets (psychoactive substances mixed with instant coffee powder) were the most popular.14,16,17 In Taiwan, illicit ketamine was the most popular NPS from the early 2000s until 2016. Since early 2010, an increasing number of drug-laced instant coffee packets have been seized. Synthetic cathinones have replaced ketamine as the most predominant NPS in the illicit drug market since 2017. 14 These so-called “toxic coffee packets” include various packaging (Figure 1) and may contain psychoactive drugs other than synthetic cathinones.18,19 Although these products have been popular in Taiwan for a few years, only small numbers of synthetic cathinone poisonings have been identified in the medical system.15,18 Clinical studies regarding synthetic cathinone poisoning from instant coffee packets are also limited.

“Toxic coffee packets” in various packaging. The photos were adapted with the approval of the National Police Agency, Minister of Interior, Republic of China (Taiwan). Retrieved June 26, 2020 from URL: https://www.cib.gov.tw/Drup/Detail/76.
Synthetic cathinones represent a broad class of pharmacologically active compounds that induce numerous effects with different mechanisms of action. 20 Additionally, due to the diversity of the ingredients of toxic coffee packets, the clinical presentation following ingestion can be complex and unpredictable. In this study, we aimed to evaluate the demographics and clinical features of patients who ingested toxic coffee packets and presented to an emergency department (ED).
Materials and methods
We retrospectively reviewed the medical charts of ED patients who reported ingesting toxic coffee packets at three Chang-Gung Memorial Hospitals located in northern Taiwan between January, 2015 and December, 2019. Exposure history could have been self-reported by the patient or provided by any of the relevant personnel including family members, friends, paramedics, or the police. The three hospitals were Linkou Chang-Gung Memorial Hospital (medical center; annual ED visits approximately 180,000), Taipei Chang-Gung Memorial Hospital (local hospital; annual ED visits approximately 5000), and Keelung Chang-Gung Memorial Hospital (regional hospital; annual ED visits approximately 6000). This study was approved by the Chang-Gung Medical Foundation Institutional Review Board (No. 202000882B0).
The exposure history, time of ingestion, age, sex, initial vital signs, initial Glasgow coma scale (GCS) score, clinical symptoms, laboratory data, urine drug screening results (by immunoassay), confirmation test results (qualitative mass-spectrometry-based analysis for commonly abused drugs in patients’ urine samples), hospital flow, severity of toxicity (recorded as Poison Severity Score), 21 poisoning-related therapies, and outcomes were recorded for descriptive analysis. A comparative analysis was conducted between patients who were or were not admitted to the intensive care unit (ICU). We also performed a multivariate analysis to evaluate the factors associated with the ICU admission.
Statistical procedures
The Mann–Whitney U test was used to compare continuous variables between groups, and the chi-square or Fisher’s exact test was used to compare categorical variables between groups, as appropriate. A p-value <0.05 was considered statistically significant. Baseline characteristics highly associated with ICU admission (p < 0.1) were then fitted into both univariate and multivariate logistic regression analyses. The odds ratios (ORs) and relevant 95% confidence intervals (CIs) were calculated. All analyses were performed using SAS Enterprise Guide 9.4.
Results
In total, 60 patients who reported ingestion of “toxic coffee packets” were included in the analysis: 47 (78.33%) were male and 13 (21.67%) were female. The majority (43 patients, 71.7%) of patients reported ingesting instant coffee packets only, while the other 17 patients reported ingesting other drugs simultaneously (Table 1). Their mean age was 28.85 ± 9.24 years. In general, case numbers increased from 2015 through 2018 and decreased slightly in 2019 (Figure 2). The most common presentation was palpitation (41.7%), followed by agitation (31.7%), hallucinations (31.7%), and altered mental status (25%, defined as GCS score <15). Four patients (6.7%) had a seizure episode and six patients (10%) presented with a concomitant trauma. Tachycardia (63.3%) and hypertension (36.7%) were common, while hyperthermia with a body temperature (BT) >38°C was observed in only three patients (5%). Laboratory testing revealed creatine kinase (CK) elevation in 16 patients; three of these patients had CK levels above 10,000 U/L. All three patients developed acute kidney injury (AKI), and one underwent transient hemodialysis. Ten patients had an abnormal serum creatinine level in their admission laboratory data. Hyponatremia was found in five patients, of whom only one had significant hyponatremia, at 120 meq/L (Table 1).
Demographic and clinical data of patients. Data represent case numbers of the parameter and its percentage. Continuous data are presented as mean values ± SD; laboratory parameters are shown as number of positive results/number of tests done.

GCS, Glasgow Coma Scale; HR, heart rate; SBP, systolic blood pressure; BT, body temperature; RR, respiratory rate; Cr, serum creatinine level; CK, creatine kinase, Na, serum sodium level; MDMA, 3,4-methylenedioxymethamphetamine; ED, emergency department; AMA, against medical advice; ICU, intensive care unit; PSS, Poisoning Severity Score.

Case numbers over the years.
Most patients had mild to moderate toxicity and were discharged from the ED after symptom relief. Fifteen patients (25%) were admitted, of whom nine (15%) were admitted to an ICU. More than half were treated with benzodiazepines, and four were intubated. The only fatality was a 37-year-old male who developed agitation, seizure, and ventricular tachycardia following ingestion of toxic coffee packets and unknown sedatives. He was admitted to the ICU and eventually died from the poisoning. Confirmation tests (by mass-spectrometry-based analysis) were available in 10 patients (including the fatal case), and all these patients’ urine samples tested positive for at least one kind of synthetic cathinone. Detailed test results and analytical methods applied are shown in Table 2. Polysubstance exposure following toxic coffee packet ingestion was common; seven of these 10 patients were exposed to more than one kind of synthetic cathinone, and the most frequently detected illicit drug other than synthetic cathinones was ketamine.
Clinical presentations and confirmation test results in 10 patients. The admission urine samples of these patients were sent to a regional reference laboratory unit and tested qualitatively for commonly abused drugs using the standard mass spectrometry at that time.

M, male; F, female; AKI, acute kidney injury; AMS, altered mental status; Na, serum sodium level; ICU, intensive care unit; Am, amphetamine; MDMA, 3,4-methylenedioxymethamphetamine; K, ketamine; P, positive; N, negative; 4-CMC, 4-chloromethcathinone; 4-CEC, 4-chloroethcathinone; 4-MEAP, 4-methyl-α-ethylaminopentiophenone; 4-chloro-N,N-DMC, 4-chloro-N,N-dimethylcathinone; LC-MSMS, liquid chromatography–tandem mass spectrometry; GCMS, gas chromatography–tandem mass spectrometry; LC-TOF, liquid chromatography–time of flight mass spectrometry.
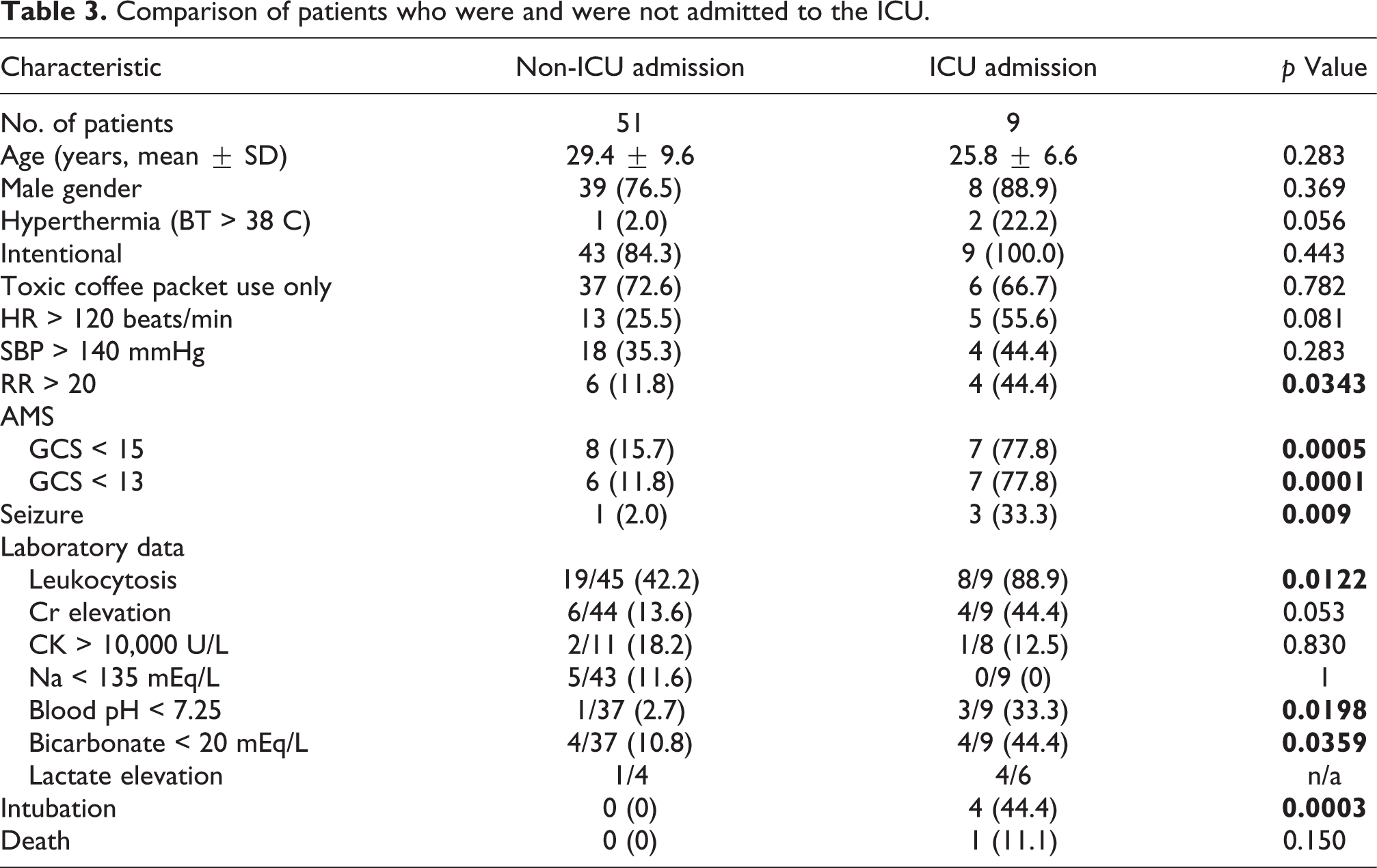
To identify the potential risk factors associated with ICU admission after toxic coffee packet ingestion, we further compared demographic and clinical characteristics between patients who needed ICU care and those who did not (Table 3). Patients who needed ICU care had a worse initial GCS score, higher respiratory rate, higher rate of experiencing seizures, higher white blood cell count, lower bicarbonate level, and higher intubation rate and were more likely to have significant acidemia (pH < 7.25). To evaluate the predictive role of each parameter, we used a receiver operating characteristic (ROC) curve to find the best cutoff value that predicted ICU admission. A GCS score ≤13 was found to have the best predictive value (sensitivity, 77.8%; specificity, 88.2%), and the area under the curve was 0.86 (95% CI 0.69–1.0). When all variables with a p-value less than 0.1 in univariate analysis were fitted into a multivariate logistic regression model, only GCS score ≤13 (OR 29.4, 95% CI 2.9–297.3) and the presence of seizure (OR 32.3, 95% CI 1.3–784.1) were significantly associated with ICU admission.
Comparison of patients who were and were not admitted to the ICU.
Discussion
In this study, we report clinical characteristics, presentations, and outcomes of ED patients who reported ingestion of toxic coffee packets, a new pattern of synthetic cathinone use in Taiwan. Patients ingesting toxic coffee packets usually presented with sympathomimetic symptoms, which were mainly neurologic and cardiovascular symptoms and combative behavior. Mortality was rare in our series, but it did occur. Based on the confirmation test results in 10 patients, we considered that patients who reported ingesting these products were very likely to be exposed to synthetic cathinones. Multiple psychoactive substances exposure after toxic coffee packet ingestion was common.
Individuals who ingested toxic coffee packets tended to be young and predominantly male. This finding is similar to some reports of synthetic cathinone poisoning from other countries.11,22–24 According to data from the Taiwan Food and Drug Administration (TFDA), the most predominant illicit drug used by people older than 40 years old in Taiwan is heroin, followed by amphetamine/methamphetamine. Illicit ketamine and other NPS are more popular in young people aged less than 30 years. 15 A single-center study from Taiwan showed that lab-confirmed NPS users (mean age, 27.0 ± 9.9 years) were significantly younger than traditional drug (heroin or amphetamine/methamphetamine) users (37.0 ± 9.1 years). 19 A possible explanation is that ketamine and toxic coffee packets cost less (10–20 USD for each packet) and are more affordable for young people and students. 13 Another potential reason is that ketamine and some popular synthetic cathinones (e.g., mephedrone, methylone, chloromethcathinone, methyl-α-ethylaminopentiophenone, 4-chloroethcathinone, and ethylone) are classified as Schedule III drugs in Taiwan. Illicit narcotics and psychoactive agents are divided into four categories (Schedule I to Schedule IV) in Taiwan based on their addictive potential, illicit use liability, and social harm liability.25,26 Unlike Schedule I or II drugs, illicit use of these Schedule III drugs does not involve criminal responsibility and is punished only with an administrative fine. 26 First-time users, usually young people, might feel less guilty and be more willing to use these drugs and share them with friends.
According to the confirmation test results in some of our patients, multiple substance exposure is common among toxic coffee packet users. Previous case series from Taiwan demonstrated the same finding.17–19 A recent study from Taiwan further reported that polysubstance exposure was more common in NPS users than in traditional drug users. 19 Polysubstance use was also a common phenomenon in “bath salt” users in the United States and Europe.27–29 Since the majority of our patients reported ingesting only toxic coffee packets, our findings indirectly imply that patients who ingested this product in fact simultaneously ingested various psychoactive substances. Both consumers and sellers, most likely unknowingly, are confronted with the risk of criminalization and potential harm. Some evidence showed that concurrent exposure to other stimulants with synthetic cathinones may enhance toxicity.30–32 The only fatality in our series (case no. 1 in Table 2) was exposed to a mixture of NPS including N-ethylpentylone and 25B-NBOMe (a phenethylamine derivative) following ingestion of toxic coffee packets. This new pattern of polysubstance exposure caused by toxic coffee packets has brought new threats to public health in Taiwan. Moreover, this phenomenon may have occurred in some of the other Southeast Asian countries despite not being formally reported in the literature.
Synthetic cathinones activate central serotonergic and dopaminergic systems. Patients who ingest toxic coffee packets usually present with sympathomimetic symptoms, which are similar to those produced by methamphetamine and MDMA toxicity.24,33 Interestingly, hyperthermia was relatively uncommon in our series; three patients (5%) had a BT > 38°C, and only one patient had significant hyperthermia with a BT > 39°C. In a series involving 81 patients with laboratory-confirmed cathinone use in southern Germany, hyperthermia (>38.5°C) was noted only in 4% of patients. 29 Some other reports have shown similar findings.10,22 In an animal study, brain and body hyperthermic effects of methylone and MDPV in rats were modest in magnitude (<2°C) even at relatively high drug doses that exceeded the range of “typical” human recreational consumption. 34 A larger clinical study should be conducted to confirm this observation.
Significant hyponatremia occurred in one of our patients (case no. 3 in Table 2). This 19-year-old male ingested a few toxic coffee packets and several liters of water and developed polyuria and hypo osmolar hyponatremia with a serum sodium level of 120 meq/L. He responded well to normal saline infusion and was discharged on the following day. 4-Chloromethcathinone was the only psychoactive drug detected in a further confirmation test (Table 2). Hyponatremia is a rare presentation in synthetic cathinone poisoning.35,36 It may be caused by excessive sweating with electrolyte loss and increased free water consumption during cathinone use (presumably the main reason for hyponatremia in our case). Additionally, some synthetic cathinones possess an MDMA-like effect, which can result in hyponatremia by inducing secretion of antidiuretic hormone mediated via serotonin. 35
Peripheral visual field defects occurred in three of our patients following ingestion of toxic coffee packets. These patients received serial examinations, including brain imaging and ophthalmoscopy, and no abnormal findings were revealed except subtle macular edema in one patient. Their visual symptoms all subsided within a few days. Confirmation tests were available in two patients, which showed they had been exposed to cathinone mixtures and ketamine. In a large series of 236 patients exposed to bath salts and legal highs, blurred vision was found in seven patients (3%). 22 In a Scottish survey involving 205 students who used mephedrone, 21% reported the adverse effect of blurred vision. 3 However, there was no further description in either study. Decreased visual acuity or transient loss of vision and retinal hemorrhage have been reported in amphetamine and cocaine abuse.37,38 Most of these ocular effects are thought to be due to the sympathomimetic effects of vasoconstriction or vasospasm. 37 It is reasonable to assume that synthetic cathinones may have a similar effect although the exact mechanism has not been well studied.
In response to the rapid emergence of NPS with molecular structures that were not covered by legislation, several countries have created new mechanisms of control, with accelerated ways to restrict the free sale and distribution of these substances. 2 The prevalence of an illicit substance usually decreases once it has been well scheduled. 39 In Taiwan, TFDA and the Ministry of Justice have controlled the majority of commonly abused synthetic cathinones since the early 2010s. However, the prevalence of synthetic cathinones continued to rise after scheduling. 14 There are a few possible explanations. First, most of the popular synthetic cathinones are classified as Category III substances in Taiwan. Although the production, transportation, or distribution of these substances is criminal, possession of small amounts or use of them is not a criminal offense. 26 Second, legislative mechanisms tend to be rigid in Taiwan. A drug should be proved to possess addictive potential, abuse liability, and social harm liability before it can be controlled. 14 However, it is usually difficult to prove promptly whether a new psychoactive drug is addictive and, in turn, difficult to collect data on its abuse and social harm liability. A study showed that compared to the neighboring countries China, Japan, and South Korea, Taiwan controlled the fewest NPS. 40 Third, synthetic cathinone use is seldom identified and reported in healthcare facilities because of the unavailability of adequate laboratory capacity and unawareness of synthetic cathinone poisoning patterns. 15 Reporting by healthcare facilities could provide important toxic surveillance information in NPS abuse; however, this has not been successful in Taiwan. Moreover, the public does not have sufficient knowledge of toxic coffee packets and synthetic cathinone toxicity. To mitigate the harmful influence of toxic coffee packets, education for both the public and healthcare providers should be emphasized, and laboratory capacity should be enhanced.
This study has several limitations. First, this is a retrospective study including a small number of ED patients. The rate of each presentation and mortality may not be precisely evaluated. Second, confirmation tests were not available in most of our cases, and a unified testing method could not be achieved because this was a retrospective study covering a time span of 5 years. Moreover, a newly introduced NPS would not be correctly identified because the testing was focused on the known illicit drugs or NPS in Taiwan. Third, the inclusion basically relied on exposure history, which may not be correct in some cases. However, based on the high positive rate of illicit drug detection in patients’ urine samples in some of our cases, we consider that most of the inclusions were reliable.
Conclusions
ED patients who report ingesting “toxic coffee packets” are very likely to have been exposed to synthetic cathinones and present with sympathomimetic symptoms. Exposure to multiple psychoactive substances is common following ingestion. Although most patients recovered rapidly after supportive treatment, severe complications such as rhabdomyolysis, AKI, and life-threatening cardiac arrhythmia can occur. A GCS score ≤ 13 and the presence of seizure are associated with the need for ICU care. To provide appropriate diagnosis and management, physicians should be aware of this new pattern of synthetic cathinone poisoning.
Footnotes
Acknowledgments
The authors would like to thank the following reference laboratory units for conducting the confirmation tests: (1) Clinical Toxicology & Occupational Medicine Division, Internal Medicine Department in Taipei Veteran General Hospital and (2) Forensic & Clinical Toxicology Center in College of Medicine, National Taiwan University Hospital.
Authors’ contribution
H-H Chou and C-H Hsieh are both the first authors. The first two authors contributed equally to this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Chang-Gung Memorial Hospital Research Grants (CMRPG3H0921 and CMRPG3H0922).
