Abstract
Valproic acid (2-propyl-pentanoic acid, VPA) is the most widely prescribed antiepileptic drug due to its ability to treat a broad spectrum of seizure types. VPA exhibits various side effects such as organ toxicity, teratogenicity, and visual disturbances. S-Methylmethioninesulfonium is a derivative of the amino acid methionine and it is widely referred to as vitamin U (Vit U). This study was aimed to investigate the effects of Vit U on lens damage parameters of rats exposed to VPA. Female Sprague Dawley rats were divided into four groups. Group I comprised control animals. Group II included control rats supplemented with Vit U (50 mg/kg/day) for 15 days. Group III was given only VPA (500 mg/kg/day) for 15 days. Group IV was given VPA + Vit U (in same dose and time). Vit U was given to rats by gavage and VPA was given intraperitoneally. On the 16th day of experiment, all the animals which were fasted overnight were killed. Lens was taken from animals, homogenized in 0.9% saline to make up to 10% (w/v) homogenate. The homogenates were used for protein, glutathione, lipid peroxidation levels, and antioxidant enzymes activities. Lens lipid peroxidation levels and aldose reductase and sorbitol dehydrogenase activities were increased in VPA group. On the other hand, glutathione levels, superoxide dismutase, glutathione peroxidase, glutathione reductase, glutathione-S-transferase, and paraoxonase activities were decreased in VPA groups. Treatment with Vit U reversed these effects. This study showed that Vit U exerted antioxidant properties and may prevent lens damage caused by VPA.
Keywords
Introduction
Antiepileptic drugs (AEDs) are used by millions of people worldwide for the treatment of epilepsy as well as in many other neurological and psychiatric conditions. AEDs can cause some adverse effects ranging from mild to acute and serious ones as well as metabolic alterations, including changes in serum lipids, hormones, and various vitamin levels. 1 Some drugs are responsible for the formation of reactive metabolites, such as arene oxides or atropaldehyde intermediates, in skin, liver, and other organs, causing hypersensitivity reactions or can enhance a commonly minor metabolic pathway increasing the formation of toxic metabolites. AEDs used for neurological disorders have also been associated with ocular complications. 2 –4
Valproic acid (2-propyl-pentanoic acid, VPA) is commonly used as an effective antiepileptic drug. VPA has some adverse effects such as hemotological, reproductive, gastrointestinal, and neurological systems and can produce hyperprolactinemia, hyperinsulinemia, alopecia, pancreatitis, or thrombocytopenia. 5 VPA, which is also a histone deacetylase inhibitor, demonstrated enhanced anticancer effects. 6
S-Methylmethionine sulfonium chloride is abundant in the tissues of flowering plants, especially in raw cabbage, and has been called vitamin U (Vit U). 7 Vit U is present in the largest quantity in species belonging to the Brassicacea family. 8 Vit U is reported to have antiulcer, anti-inflammatory, antidepressant, cytoprotective, antihyperlipidemic, wound-healing adipocyte differentiation, and hepatoprotective activities. 9
In this study, we aimed to investigate the effects of Vit U on VPA-induced lens damage in experimental animals for the first time.
Materials and methods
Animals and experimental design
The experiments were reviewed and approved by the Animal Care and Use Institute’s Committee of Istanbul University. In this study, 6–6.5-months-old female Sprague Dawley rats were used. All rats were clinically healthy. The rats were housed in metal cages at room temperature and fed with laboratory pellet chow and given water ad libitum. The animals were randomly divided into four groups. Group I: control animals (n = 8); group II: control animals given Vit U (n = 8; 50 mg/kg/day); group III: animals given only VPA (n = 12; 500 mg/kg/day); group IV: animals given VPA + Vit U (n = 11; in same dose and time). The animals were treated by Vit U 1 h prior to treatment with VPA every day. The Vit U was given to rats by gavage and VPA was given intraperitoneally. All these treatment doses were given for 15 days. The animals were then fasted overnight, and on day 16, all the animals were sacrificed under ether anesthesia.
Biochemical assays
Lens tissue samples were taken and frozen until needed for study. The tissues were homogenized in cold saline using a glass homogenizer to make 10% (w/v) homogenate. The homogenates were centrifuged, and the clear supernatant was used. The homogenates were used for protein, glutathione (GSH), lipid peroxidation (LPO) levels, and enzymes activities. The lens tissue GSH and LPO levels were determined according to the method followed by Beutler 10 and Ledwozyw et al., respectively. 11 Superoxide dismutase (SOD) activity was determined based on the method described by Mylorie et al., 12 glutathione peroxidase (GPx) by the Paglia and Valentine and modified by Wendel, 13 glutathione reductase (GR) activity by Beutler, 14 glutathione-S-transferase (GST) by Habig and Jacoby, 15 aldose reductase (AR) by Hayman and Kinoshita, 16 sorbitol dehyrogenase (SDH) by Bergmeyer et al., 17 and paraoxonase (PON) by Furlong et al. 18 . Protein levels were measured by the method of Lowry et al. using serum albumin as standard. 19
Statistical analysis
Biochemical results were evaluated using an unpaired t-test and analysis of variance using the NCSS statistical computer package (1984). The values were expressed as mean ± SD. The values of p < 0.05 were considered as significant.
Results
Lens GSH and LPO levels are shown in Table 1. Lens GSH level was significantly decreased in VPA group compared with the control group ( p < 0.005). Administration of Vit U significantly increased in the GSH level in VPA group ( p < 0.05). Lens LPO levels were significantly increased in VPA group compared with the control group ( p < 0.05). Vit U significantly decreased LPO level in VPA group ( p < 0.05; Table 1).
Effect of Vit U on GSH and LPO levels in the lens tissue of all the groups.a
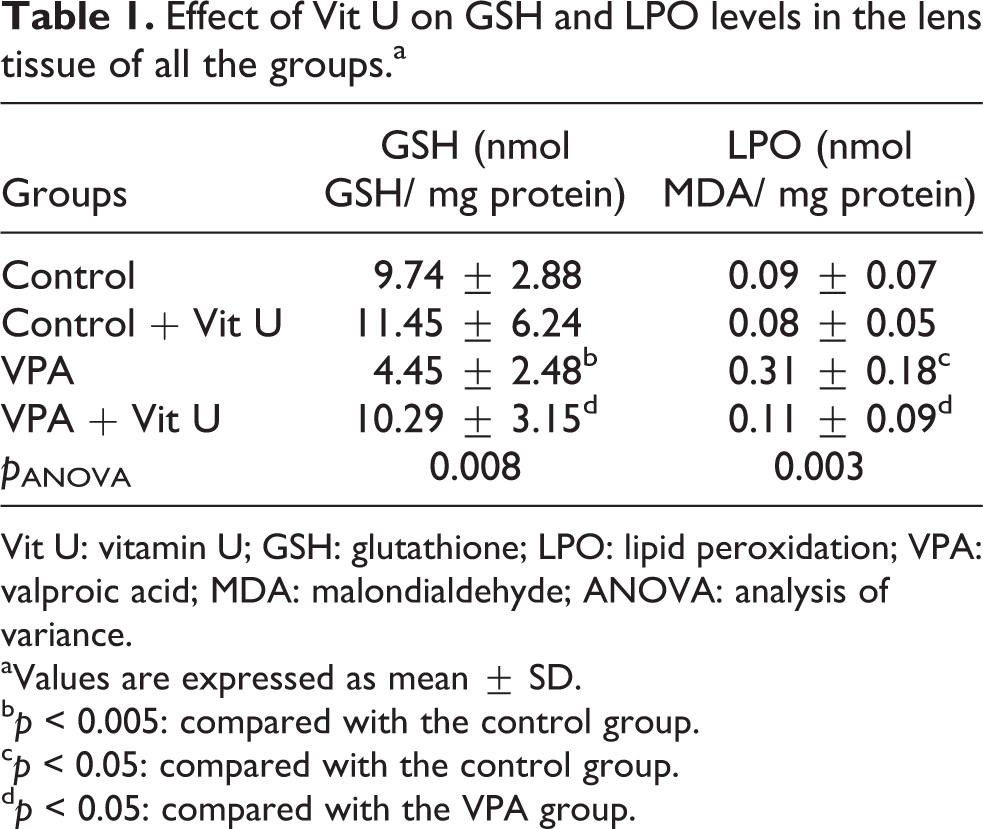
Vit U: vitamin U; GSH: glutathione; LPO: lipid peroxidation; VPA: valproic acid; MDA: malondialdehyde; ANOVA: analysis of variance.
aValues are expressed as mean ± SD.
b p < 0.005: compared with the control group.
c p < 0.05: compared with the control group.
d p < 0.05: compared with the VPA group.
SOD activity in the lens tissue was significantly decreased in VPA compared with the control group ( p < 0.05). However, in the Vit U-treated group significantly increased lens SOD activity ( p < 0.05; Table 2). GPx, GR, and GST activities are shown in Table 2. Lens GPx, GR, and GST activities were significantly decreased in VPA group compared with the control group ( p < 0.05, p < 0.005; Table 2). Administration of Vit U significantly increased GPx, GR, and GST activities in VPA group ( p < 0.05; Table 2).
Effect of Vit U on SOD, GPx, GR, and GST activities in the lens tissue of all the groups.a

Vit U: vitamin U; SOD: superoxide dismutase; GPx: glutathione peroxidase; GR: glutathione reductase; GST: glutathione-S-transferase; VPA: valproic acid; MDA: malondialdehyde; ANOVA: analysis of variance.
aValues are expressed as mean ± SD.
b p < 0.05: compared with the control group.
c p < 0.005: compared with the control group.
d p < 0.05: compared with the VPA group.
Lens AR and SDH activities were significantly increased in VPA group compared with the control group ( p < 0.005). Vit U significantly decreased AR and SDH activities in VPA groups compared with VPA group ( p < 0.05, p < 0.001). Lens PON activity was significantly decreased in the VPA group ( p < 0.05). Administration of Vit U was significantly increased the lens PON activity ( p < 0.005; Table 3).
Effect of Vit U on AR, SDH, and PON activities in the lens tissue of all the groups.a

Vit U: vitamin U; AR: aldose reductase; SDH: sorbitol dehydrogenase; PON: paraoxanase; VPA: valproic acid; MDA: malondialdehyde; ANOVA: analysis of variance.
aValues are expressed as mean ± SD.
b p < 0.005: compared with the control group.
c p < 0.05: compared with the control group.
d p < 0.005: compared with the VPA group.
Discussion
Epilepsia is a neurological disorder that may be associated with visual alterations. There are various antiepileptic drugs that have been used in the treatment of epilepsia. A number of antiepileptic drugs have recently been reported to result in various abnormalities of vision, particularly deficiencies in visual fields and color vision. 20,21 Some antiepileptic drugs change antioxidant enzyme activities in humans and experimental animals. 22 GSH redox cycle has a very important role among enzymatic or nonenzymatic cellular antioxidant mechanisms for protection against oxidative damage. GSH, which is highly concentrated in the lens and helps to reduce proteins, 23 contains a side chain of sulfhydryl –SH residue that enables it to protect cells against oxidants. The decrease in the GSH levels suggested that it might be due to exhaustion of GSH stores and increase in the oxidative stress. Reduction in the GSH amount may result in an increase of organic hydroperoxides. Cengiz et al., found that GSH levels were reduced in valproate groups. 22 In our study, lens GSH levels were decreased in VPA group indicating that VPA-induced tissue injury is associated with oxidative stress. Vit U increased GSH levels in the lens. In this study, Vit U significantly restored the levels of GSH in VPA-induced rats, a key antioxidant for protection against oxidative damage.
Free radical generation or oxidative stress develops where there is an imbalance between prooxidants and antioxidants ratio, leading to the generation of reactive oxygen species (ROS). 24 LPO has been hypothesized to be a major mechanism of cell damage by free radicals. VPA toxicity is associated with increased ROS formation, which in turn constitutes an important risk factor for tissue damage. 25 Several groups have investigated the mechanims of VPA toxicity in various cell lines and tissues using different schemes of administration as well as distinct animal species. 26 –28
In this study, elevation in lipid peroxides was observed due to the administration of VPA, which is attributed to the enhanced production of ROS. However, administration of Vit U prevented these changes. Several researchers recently demonstrated that Vit U decreased the level of LPO and inhibited blood lipid accumulation. 29 –31 This may be attributed to its free radical scavenging properties and antioxidative potential.
Endogenous antioxidant mechanisms exist to protect against the oxidative injury associated with normal metabolism. In the literature, there are numerous studies concerning the effect of AEDs on oxidant and antioxidant enzymes. 32,33 Similar to our study, some authors revealed that AEDs may lead to development of oxidative stress. 22,34 In our study, the results indicate that VPA-induced lens damage is associated with increased oxidative stress.
SOD is the most important defense mechanisms against toxic effects of oxygen metabolism. It catalyzes the conversion of superoxide radicals into hydrogen peroxide (H2O2) and water. This antioxidant enzyme can alleviate the toxic effects of ROS. 35 In our study, SOD activity is lowered by application of VPA. Vit U treatment increased SOD activity in the lens tissue. In the literature, SOD activity has been reported to be induced by VPA. 22 In another study, Yüksel et al. reported that SOD activity increased in erythrocytes of patients receving valproate over a 13-month period. 36 Sołowiej and Sobaniec observed that SOD activity was decreased in epileptic children receving VPA in comparison with relevant levels in nonepileptic patients. 37
GPx is an enzyme that plays an important role in removing excess free radicals and hydroxides and catalyzes the conversion of H2O2 into water in the presence of GSH. This may be critical in protecting cells against oxidants. There are conflicting reports about the effects of VPA on antioxidant enzymes. Sołowiej and Sobaniec and Yüksel et al. found lower levels of GPx in patients receiving VPA, 36,37 while Tunali 38 report the contrary. In our study, GPx activity was higher in VPA group compared with control group in lens tissue. Administration of Vit U decreased lens GPx activity in rats treated with VPA.
GR, one of the enzymes of the GSH redox cycle, has a critical role in maintaining a high cellular reduced GSH to oxidized GSH ratio. GR activity is also reported to be inhibited by valproate. 39 Graf et al. reported that in patients with a serious adverse experience related to VPA therapy, GR activity was elevated relative to values for the other groups. 40 In our study, GR activity was lower in VPA group compared with the control group in lens tissue. Administration of Vit U increased lens GR activity in rats treated with VPA.
GST is a metabolizing enzyme that plays a prominent role in the detoxification of oxidized metabolites and may serve as an antioxidant. GST catalyzes the conjugation of certain electrophiles, including oxidized products generated by ROS, with the reduced glutathione thiolate anion to form a nontoxic and excretable product. 41,42 Detoxification by GST provides protection against harmful endogenous ROS, and this enzyme is now believed to play a critical role in combating oxidative stress and cell toxicity. 41 In this study, GST enzyme activity decreased in the lenses of VPA-treated rats group compared with the control group. Administration of Vit U restored GST activity to normal level. An increase in lens GST activity indicates improvement in the lens injury.
AR is a monomeric-reduced, nicotinamide adenine dinucleotide phosphate (NADPH)-dependent enzyme and a member of aldoketo reductase superfamily. 43 This enzyme is key enzyme in the polyol pathway. The activation of this pathway could lead to the depletion of NADPH, thereby perturbing the cellular redox poise, leading to the formation of oxidative stress. In this study, VPA-treated rats showed a significant increase in the activities of AR compared with control rats. However, administration of Vit U significantly decreased lens AR activity in rats treated with VPA. The decrease in those increasing AR activity shows that Vit U prevented damage in the lens tissue.
SDH catalyzes the conversion of sorbitol to fructose in the presence of NAD. SDH is a specific indicator of cellular injury in rodents and humans. 44 In our study, SDH activity increased by application of VPA in lens. However, Vit U treatment significantly decreased SDH activity and prevented the lens damage.
PON is a calcium-dependent esterase that hydrolyzes a wide range of substrates, particularly oxidized lipids 45 and reduces oxidative stress. PON 1 activity is a marker of oxidative stress. Increased oxidative stress has been shown to reduce PON 1 synthesis in vivo and in vitro. 46 This study shows the changes in lens PON activity following administration of VPA. The decrease in PON activity is directly related to the degree of lens damage. SH groups are present in the activities of PON 1. 47 Sulfhydryl compounds prevented the inhibition of PON 1 activity caused by cigarette smoking. 48 In our study, administration of Vit U significantly increased lens PON 1 activity in rats treated with VPA. Lens PON activity were reduced indicating that VPA-induced tissue injury is associated with oxidative stress.
Elevated and decreased lens enzyme activity might be considered as VPA toxicity. In previous studies, antioxidative vitamins, such as A, C, E, and coenzyme Q have been shown to protect the body against diseases characterized by the disruptive activity of free radicals. 49,50 In our study, Vit U has been shown to protect against VPA-induced lens damage. These results demonstrated that Vit U is a potentially benefical agent to reduce the lens damage in VPA toxicity probably by decreasing oxidative stress.
Antioxidants lower indices of oxidative stress and increase antioxidantive enzyme activity and the level of nonenzymatic antioxidants. 50 It was stated that the compounds that have sulfhydryl group in their composition have the ability to catch free radicals that occured in some of the tissues. 51,52
Our results indicate that VPA-induced lens damage is associated with increased oxidative stress. The results of this study show that Vit U effectively ameliorated VPA-induced oxidative stress. The protective effect of Vit U may be due to its sulfhydryl group. Vit U may be used clinically for VPA-induced lens damage during epilepsy disease.
Footnotes
Conflict of interest
The authors declared no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
