Abstract
Although ingestion of methyl ethyl ketone peroxide (MEKP) is rare, it carries a high risk of morbidity and mortality. This paper reports the first such case from Turkey in which a 70-year-old man unintentionally ingested MEKP in his kitchen. The patient was brought into the emergency department (ED) within 1 hour of ingestion, with the symptoms of sore throat, shortness of breath, nausea and vomiting. Visual examination of the oropharynx revealed minor burns and uvular edema. A laryngoscope examination performed in the ED showed superficial mucosal injury with edema of the oropharynx, uvula, posterior pharynx, epiglottis, arytenoids and vocal cords. Lateral cervical radiography revealed a narrowing of airway due to a thickened epiglottis. After the diagnostic evaluation was completed, the patient was admitted to the gastroenterology intensive care unit for monitoring of adverse reactions. During follow-up, the patient made an uneventful recovery. Ingestion of MEKP generally results from accidental ingestion from a container. Therefore, these containers should be kept in safe places. In addition, the priority following the ingestion of MEKP should be given to maintain open and adequate airway in the ED.
Introduction
Methyl ethyl ketone peroxide (MEKP) is organic peroxide. It is a colorless, odorless liquid and very reactive oxidizing agent. MEKP is used as a hardener and curing agent for plastics such as unsaturated polyester and fiberglass resins. There is little information about what happens to MEKP once it is absorbed in the human body. However, MEKP has several physico-chemical properties that could contribute to its toxic action. The MEKP monomer is likely to split into hydrogen peroxide (H2O2) and methyl ethyl ketone. 1 In biological systems, the heme group has been identified as a strong accelerator of this radical formation process. 2 In rats, LD 50 for MEKP has been found to be 484 mg/kg and LC 50 was found to be 170 ppm/4 h. 3
The presence of free radicals induces lipid peroxidation of target organs, particularly of respiratory tract, digestive tract and liver. 4 The respiratory and digestive tracts in MEKP intoxication are directly exposed to the agent after ingestion. MEKP may induce fibrosis and stenosis in proximal digestive tract following the acute phase. The liver is also exposed to MEKP but only after systemic absorption possibly inducing acute liver failure, which is the major cause of death in this intoxication. In humans exposure to MEKP may cause metabolic acidosis, local burns of skin and mucosa on contact, and neurological lesions such as inflammation and ischemia of the optic nerve. 5
There is no effective and specific treatment for MEKP intoxication, neither on the basis of accumulated experience in human intoxications nor on the basis of experimental studies. 2
However, the ingestion of MEKP has a high morbidity and mortality rate as reported in the literature.2,6 In this article, we present a study of the first reported case of MEKP poisoning in Turkey, in which a 70-year-old man unintentionally ingested MEKP.
Case report
A 70-year-old man unintentionally ingested an estimated 10 ml of solution in his kitchen. The liquid, brought from home by his son, was unknown but then identified as a 50% solution of MEKP in dimethyl phthalate (Akperox-A 60; Akpa Chemicals, Istanbul, Turkey). The patient was brought to the emergency room within 1 hour of ingestion, with the symptoms of sore throat, shortness of breath, nausea and vomiting. His previous medical history included hypertension and diabetes mellitus.
On physical examination, the patient was somewhat anxious, not stridor with a blood pressure of 145/90 mm Hg, a pulse rate of 126 beats/min, a peripheral oxygen saturation of 93% and a core temperature of 36.8°C. Examination of the oropharynx revealed burns and uvular edema. No significant abnormal findings were found on the patient’s chest and abdominal examination. The rest of the physical examination was unremarkable. The rigid endoscopic examination at 15 minutes after arrival to the emergency department (ED) showed superficial mucosal injury with edema of the posterior hypopharynx, epiglottis, arytenoids and vocal cords (Figure 1). An esophagogastroduodenoscopy performed 2 hours after admission revealed that the whole esophagus was coated with a white slough, there was considerable inflammation and also divertucular lesions of the distal esophagus, however, the stomach and the duodenum were not affected. The ultrasound of the abdomen, chest radiogram and electrocardiogram on the day of admission were all normal. Lateral cervical radiography showed narrowing of the airway due to thickened epiglottis (Figure 2).

The rigid endoscopic examination shows superficial mucosal injury with edema of the posterior hypopharynx, epiglottis, arytenoids and vocal cords.
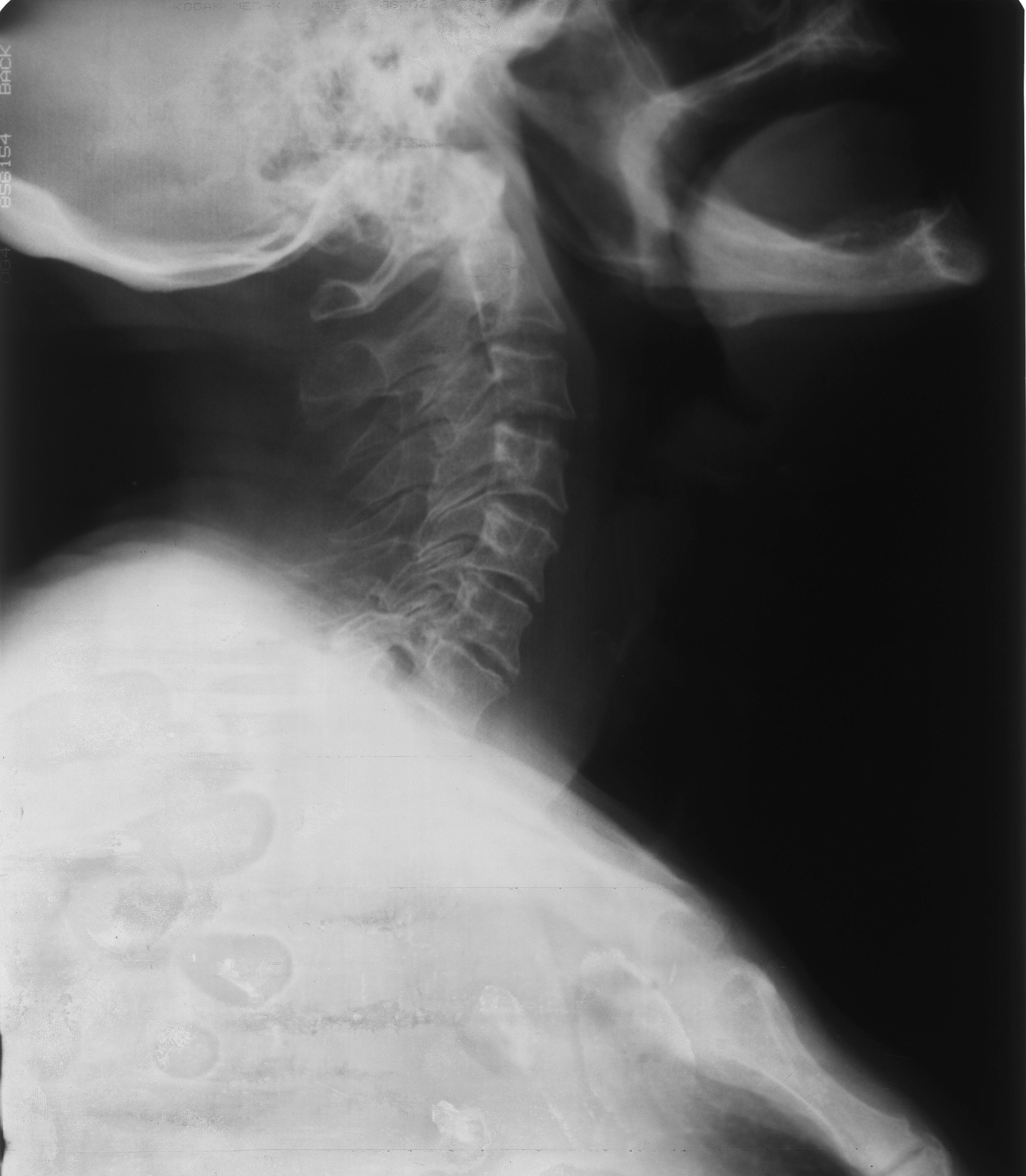
The lateral cervical radiography shows narrowing of the airway due to a thickened epiglottis.
On day 1, laboratory evaluation revealed a slight leukocytosis (14,500 K/μL), hyperglycemia (346 mg/dl) but no elevations of the liver enzymes. Arterial blood gas values at this time showed a mild hypoxemia, but no metabolic or respiratory acidosis. Other laboratory findings were all within normal limits. Liver function also remained normal during the admission period.
After the diagnostic evaluation, the patient was admitted to the gastroenterology intensive care unit for monitoring of vital signs. His glucose levels were checked four times a day and he was given insulin for his existing diabetes when needed. He was also given ampicillin/sulbactam, prednisolone, clinomel solution, ringer lactate, 5% dextrose and pantoprazole intravenously. Normal oral feeding was stopped from day 1 to day 7 of his hospital stay. N-acetylcysteine was not administered as antidotal therapy. Our patient, who failed to develop metabolic acidosis with an elevated anion gap and osmolal gap, did not need hemodialysis. Propionic acid and formic acid were not measurable at any time. Initially, there was ketonuria which subsided within 1 day. At no time was there any hemodynamic or respiratory instability, neither were there any abnormal results from the liver function tests.
On second day of admission, the patient was transferred to the department of gastroenterology from where he was discharged in good health on day 8. The patient refused the second endoscopy examination. The patient was discharged for out-patient follow-up with instructions that he could resume normal oral feeding after 3 months.
Discussion
In the literature, studies have postulated that the mechanism of toxicity of MEKP is a free radical formation that leads to lipid peroxidation and results in corrosive damage to the respiratory and gastrointestinal mucosa and also liver damage. Lipid peroxidation is a free radical-initiated chain oxidation of unsaturated lipids. Subcellular membranes are rich in unsaturated fatty acids and therefore they are the target for lipid peroxidation that results in cellular dysfunction and death.
The toxic dose of MEKP has not been established, but ingestion of any amount should be regarded as potentially serious. In cases in which the dose was known, toxicity occurred after ingestion of 50–100 ml in adults. 7 In our case, the patient unintentionally ingested an estimated 10 ml of the solution.
Dimethyl phthalate is commonly used as an insect repellent. It is often added to solutions of MEKP as a plasticizer to reduce the risk of explosion. 8 It is considered to have relatively low toxicity and is an irritant rather than corrosive. 7 A dose of 5 g of di-2-ethylhexyl phthalate caused no adverse effects, and 10 g can result in mild diarrhea. Nausea, dizziness and mild renal damage have been reported after ingestion of 10 g of dibutyl phthalate. 4 Dimethyl phthalate may have contributed to nausea and vomiting as observed in our patient.
The studies have shown that the clinical spectrum of this intoxication in the acute phase can be subdivided into four categories. 2 First, there are the airway and the gastrointestinal signs. In the acute phase, an airway edema may be the cause of death. Therefore, for our patient, laryngoscopy was performed 15 minutes after admission. There were superficial mucosal injury noted with edema of the oropharynx, uvula, posterior pharynx, epiglottis, arytenoids and vocal cords. Since the patient responded to medical treatment, cricothyroidotomy or tracheostomy was not needed. Due to inflammation and ulceration of exposed parts of the gastrointestinal tract, the gastrointestinal symptoms can range from vomiting and acid burns to hemorrhage and perforation. In our case, esophageal burns were superficial but the entire esophagus was coated with a white slough with considerable inflammation.
Second, there is free radical-mediated liver damage, which is the main cause of mortality after the acute phase. Typically a patient who ingests MEKP develops liver function abnormalities within a few hours, progressing to acute liver failure due to generalized liver necrosis within the next 2 to 3 days leading to death within 4 days. 7 Bates et al. reported that the case fatality rate of this intoxication due to acute liver failure is estimated to be (6/23). The case fatality rate could be an overestimation because of publication bias. Thirdly, there are complications due to the decomposition of MEKP that results in the generation of organic acids. 1 Apart from metabolic acidosis, formic acid can induce a variety of neurological complications of which optic nerve toxicity is the most prevalent. 5 Finally, there are secondary acute complications such as acute renal failure due to rhabdomyolysis, ventilator-associated pneumonia, adult respiratory distress syndrome and myocarditis. 2
Although ingestion of MEKP is rare, it carries a high degree of morbidity and mortality.2,6 To date, more than 20 cases of MEKP ingestion have been reported in the literature. 2 To our knowledge, this case is the first report from Turkey. The clinical effects from ingestion of MEKP have been reported to include vomiting, hematemesis, oral and esophageal burns, gastritis, airway obstruction, stridor and dyspnea. 2 Metabolic acidosis, leukocytosis, respiratory distress, adult respiratory distress syndrome, aspiration pneumonitis, hypotension, hematuria, acute renal failure and liver damage may also be observed in severe cases. In addition myocarditis with tachycardia, inverted T waves, congestive heart failure and gallop rhythm and myocardial infarction have been reported. 9 We did not observe any obvious cardiac and hepatic toxicity in this case. Early gastrointestinal hemorrhage and perforation, in addition to delayed esophageal stricture, may occur. Our case confirms the mild corrosive damage to the esophagus occurring particularly at the sites of softened contact. There was no evidence of systemic absorption which suggests that our patient only drank a small quantity of liquid, but this resulted in significant local damage.
Gastric lavage and emesis are contraindicated after ingestion of a corrosive substance because of the risk of trauma or further injury to the upper gastrointestinal tract on re-exposure. 10 The patient in our case had already vomited twice before admission to ED. Administration of fluids orally should be avoided after ingestion of MEKP because of the possibility that perforation of the gastrointestinal tract may have occurred. Therefore, it is controversial to administer milk in treatment of MEKP ingestion. In the acute phase, all patients should be immediately evaluated for airway obstruction. The early and repeated endoscopic evaluation of the upper respiratory and gastrointestinal tract is also important. The ECG, arterial blood gases, respiratory, renal and liver functions should be monitored. Once past the acute phase, patients will require ongoing follow-up because of the risk of late scarring and stricture formation.
Vitamin E and acetylcysteine have been suggested as possible therapies for MEKP toxicity however, there are no clinical data to support their usage. 1 Compared with controls, stricture formation was less frequent and less severe in animals that were treated with either acetylcysteine or prednisolone. Acetylcysteine and prednisolone demonstrated similar efficacy in reducing the development of strictures in this animal model. 11 The administration of prednisolone is important in both early and late phases of MEKP ingestion. The use of prednisolone should be considered in MEKP intoxication in order to resolve airway edema.
Conclusion
Although ingestion of MEKP is rare, most cases reported in the literature involve accidental ingestion from a drink container that originally contained rum, vodka, orange juice, beer or orangeade.9,12 Therefore, the use of these containers for the storage of toxic/poisonous chemicals should be avoided. All containers for dangerous liquids should be clearly marked. In addition, the priority following the ingestion of MEKP should be given to maintain open and adequate airway in the ED.
Footnotes
The authors declared no conflicts of interest.
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
