Abstract
Background
In recent years, gestational and congenital syphilis have re-emerged as significant public health concerns in Hungary. Although national surveillance data are available for syphilis, they do not include gestational cases, and recent studies describing the epidemiological and clinical characteristics of gestational and congenital syphilis remain limited. The aim of the study was to analyze 10 years of data to evaluate the clinical characteristics and outcomes of gestational and congenital syphilis and to identify gaps in prenatal screening and care.
Methods
We conducted a cross-sectional, single-center study at the National STD Centre in Budapest, analyzing data from pregnant women diagnosed with syphilis and their newborns between 2015 and 2025. Maternal epidemiological and clinical data were collected, and neonatal clinical and laboratory data were evaluated where available.
Results
A total of 180 pregnant women with 185 pregnancies were included. Diagnosis was made in the second or third trimester in 139 cases, and 110 cases were classified as early latent syphilis. 173 women were asymptomatic at the time of diagnosis. Penicillin was administered in 176 out of 185 (95%) cases, and an adequate serological response, defined as a ≥4-fold decline in RPR titer, was observed in 176/185 (95%). Neonatal data were available for 106 newborns. 10 (9%, 95% CI: 5–17%) neonates met the diagnostic criteria for congenital syphilis, including nine probable and one confirmed case. Clinical manifestations ranged from asymptomatic infection to severe multisystem involvement. All neonates with congenital syphilis (n = 10), as well as those whose mothers had not received adequate treatment (n = 10), in total 20/106 neonates (19%; 95% CI: 12–27%) were treated with penicillin.
Conclusion
Gestational and congenital syphilis remain significant public health concerns in Hungary. The high proportion of late diagnoses highlights the need for repeated antenatal screening and interdisciplinary collaboration to prevent congenital infection.
Introduction
Syphilis incidence has been increasing in Europe, including Hungary 1 . Consequently, gestational (GS) and congenital syphilis (CS) have re-emerged as public health concerns. This is particularly important as untreated maternal syphilis can lead to severe adverse outcomes, including miscarriage, stillbirth, and multisystem neonatal disease 2 . Despite the availability of national surveillance data 3 , recent studies detailing clinical characteristics and outcomes of GS and CS in Hungary are limited4,5. Therefore, we aimed to analyze 10 years of data from the National STD Centre in Budapest, focusing on epidemiological trends, clinical presentation, and outcomes of GS and CS. Our goal was also to contribute to bridging the gap between surveillance and clinical practice by identifying screening limitations and clinical characteristics to inform prenatal care and prevent vertical transmission.
Methods
This cross-sectional, single-center study was conducted at the National STD Centre of the Department of Dermatology, Venereology and Dermatooncology, Faculty of Medicine, Semmelweis University, Budapest, Hungary. We included 180 pregnant women diagnosed with syphilis and 106 of their newborns from 1st April 2015 to 31st March 2025.
Maternal data included age, trimester at diagnosis, disease stage, clinical manifestations, serological results (which, in addition to specific screening tests (Treponema pallidum particle agglutination/Treponema pallidum hemagglutination assay (TPPA/TPHA), and Treponema pallidum enzyme-linked immunosorbent assay (TP ELISA), also included rapid plasma reagin (RPR) titers at diagnosis and during follow-up), comorbidities, coinfections, and treatment. At out clinic, partner notification and management are routinely undertaken for all patients diagnosed with syphilis according to the local guidelines. However, partners were outside the scope of the present study, and no statistical analysis of partner-related data was performed.
Available neonatal data comprised birth outcomes, clinical findings, laboratory results, and administered therapy. Newborns were classified as confirmed and probable CS according to the Hungarian national guideline 6 .
Descriptive statistics were used for data analysis. Medians, interquartile ranges, counts, percentages, and 95% confidence intervals (CI) (with Clopper–Pearson method) were calculated. Statistical analyses were performed by using Microsoft Excel and GraphPad Prism 10.0.
Results
Gestational syphilis
Maternal characteristics of pregnant women diagnosed with syphilis (N = 180).
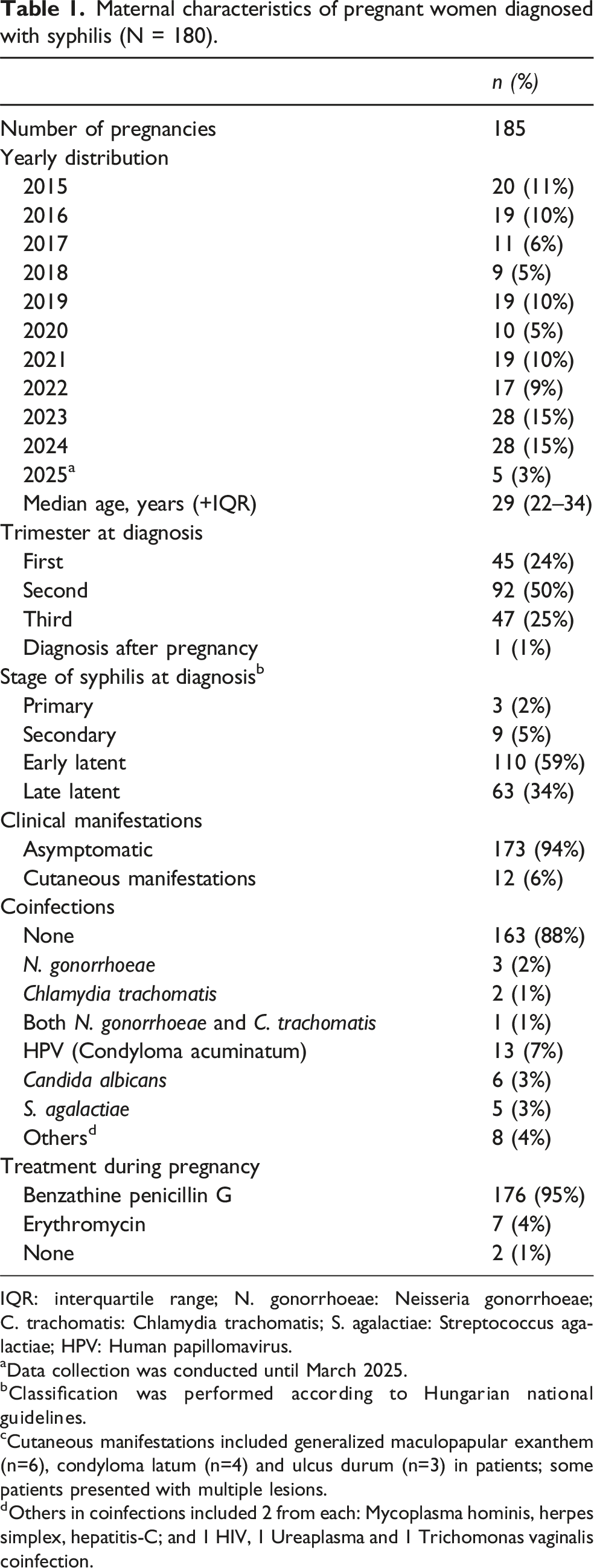
IQR: interquartile range; N. gonorrhoeae: Neisseria gonorrhoeae; C. trachomatis: Chlamydia trachomatis; S. agalactiae: Streptococcus agalactiae; HPV: Human papillomavirus.
aData collection was conducted until March 2025.
bClassification was performed according to Hungarian national guidelines.
cCutaneous manifestations included generalized maculopapular exanthem (n=6), condyloma latum (n=4) and ulcus durum (n=3) in patients; some patients presented with multiple lesions.
dOthers in coinfections included 2 from each: Mycoplasma hominis, herpes simplex, hepatitis-C; and 1 HIV, 1 Ureaplasma and 1 Trichomonas vaginalis coinfection.
Diagnoses were confirmed primarily in the second (n = 92) and third (n = 47) trimesters. Latent stage disease was most common, accounting for 173 out of 185 cases (94%), including early latent (n = 110) and late latent (n = 63) syphilis, whereas secondary (n = 9) and primary (n = 3) stages were less common.
In total, 173 (94%) patients were asymptomatic. Among those with cutaneous manifestations (n = 12; 6%), generalized maculopapular exanthema was most common (n = 6; 3%).
At diagnosis, three patients tested positive for Neisseria gonorrhoeae, two for Chlamydia trachomatis, and one for both. Additional infections included condyloma acuminatum, candidiasis, and Streptococcus agalactiae colonization. All patients were routinely screened for HIV; only one tested positive, but in her case, it was not a recent infection, as she was already receiving antiretroviral therapy.
95% of the patients (n = 176) received intramuscular 2.4-million-unit benzathine penicillin according to the national guideline, preceded by steroid premedication (2 × 24 mg methylprednisolone per os) 6 . Seven patients received oral erythromycin and postpartum doxycycline therapy due to penicillin allergy. Two patients did not appear for treatment. Coinfections were managed according to relevant guidelines.
Congenital syphilis
Neonatal data were available for 106 out of 185 pregnancies (57%). Information regarding the remaining newborns could not be retrieved as deliveries occurred outside the institution, and follow-up data were not provided by the mothers.
Three pregnancies ended in miscarriage, one of which was confirmed as intrauterine syphilis by histology. Two were terminated at parental request, and one resulted in intrauterine fetal death at 30 weeks’ gestation; in this case, no further information could be obtained. In one instance, premature rupture of membranes occurred at 32 weeks’ gestation; histopathological examination confirmed syphilitic placentitis and intrauterine infection.
Clinical and laboratory characteristics of neonates meeting diagnostic criteria for congenital syphilis.
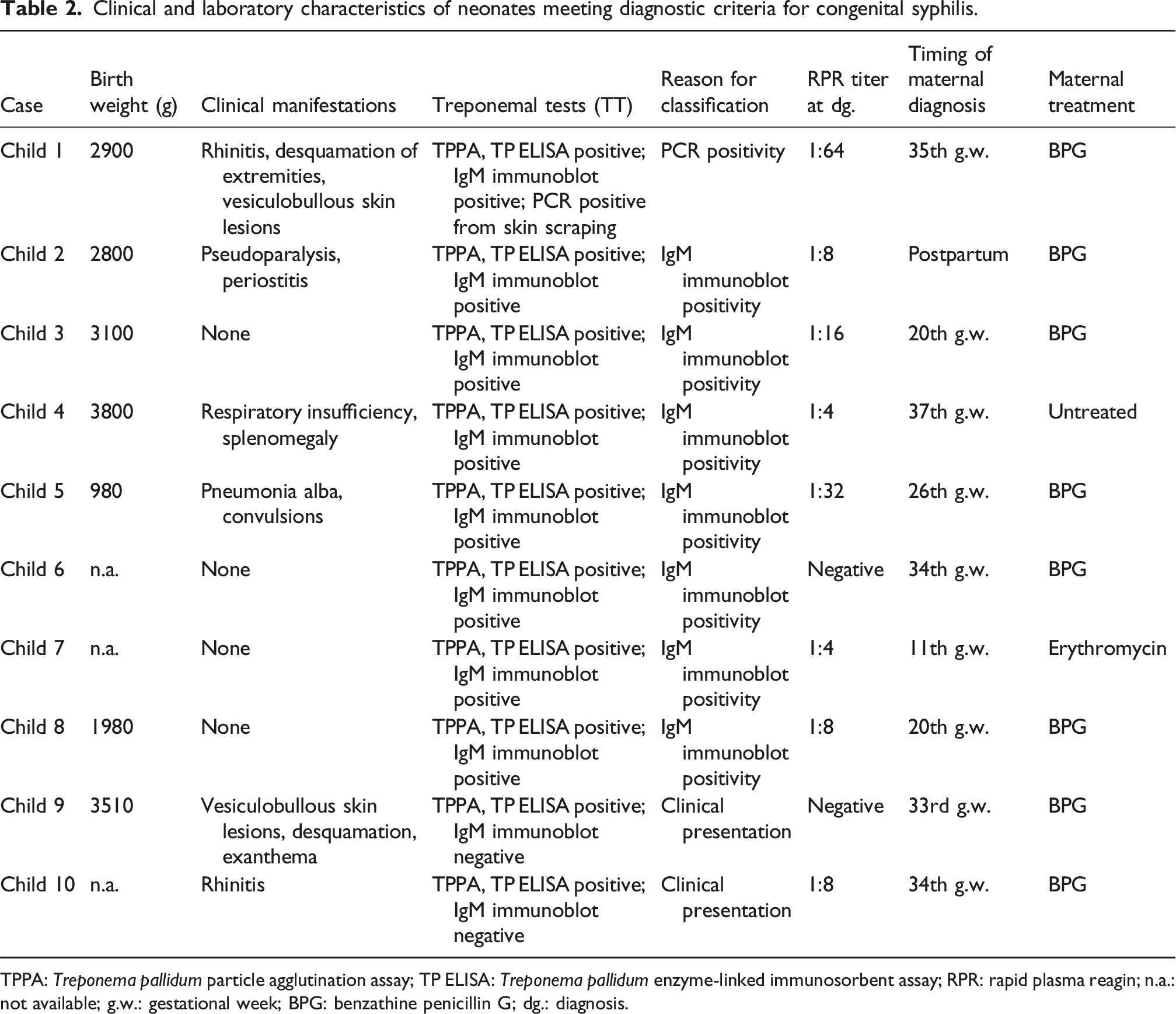
TPPA: Treponema pallidum particle agglutination assay; TP ELISA: Treponema pallidum enzyme-linked immunosorbent assay; RPR: rapid plasma reagin; n.a.: not available; g.w.: gestational week; BPG: benzathine penicillin G; dg.: diagnosis.
At the 3-month follow-up, all newborns showed an appropriate decline in RPR titers.
Among CS cases, four newborns were asymptomatic. Symptomatic neonates presented with a range of clinical features, including cutaneous manifestations (erythema with desquamation and blistering, pustular lesions on the extremities and trunk), rhinitis, osteochondritis, pseudoparalysis of Parrot and respiratory failure (Table 2).
According to clinical guidelines, all neonates with confirmed or probable CS (n = 10), as well as those whose mothers were treated with a non-penicillin regimen or within 30 days prior to delivery (n = 10), were treated with intravenous crystalline penicillin G6,7. In total, 20/106 neonates (19%; 95% CI: 12–27%) received treatment.
Discussion
In this study, we evaluated the epidemiological trends, clinical characteristics, and outcomes of gestational and congenital syphilis over a 10-year period at a national referral center. We observed higher numbers of GS diagnoses after 2020, with the highest case counts recorded in 2023 and 2024. The marked decrease in diagnoses observed in 2020 is most likely attributable to reduced healthcare utilization and diagnostic testing during the COVID-19 pandemic. In contrast, we did not observe a continuously increasing trend in CS cases comparable to national and international trends, which may be explained by relatively small case numbers and limited access to neonatal documentation.
Despite the mandatory first-trimester syphilis screening in Hungary, most cases in our cohort (n = 139) were diagnosed in the second and third trimesters. This finding underscores the limitations of single time-point screening and highlights the importance of repeated testing during pregnancy. As 173 of the maternal cases were asymptomatic, diagnosis relied primarily on serological screening, emphasizing its critical role in preventing adverse maternal and neonatal outcomes.
Appropriate treatment was associated with improvement in both clinical symptoms and serological parameters. This may provide an explanation for the proportionally lower cases of newborns diagnosed with congenital syphilis compared to mothers diagnosed with syphilis.
The possible outcomes of intrauterine exposure to syphilis are well described 8 . In our study, severe outcomes were also observed, including miscarriage, stillbirth, prematurity, low birth weight, and severe symptomatic neonatal diseases. Among 106 newborns with available data, 10 fulfilled the diagnostic criteria for CS. Of these, nine were classified as probable and one as confirmed cases; additionally, in one case, histopathology of the placenta revealed syphilitic placentitis, although additional information could not be obtained about the newborn. The low number of confirmed cases may be due to the limited availability of diagnostic tests, since direct detection of the bacteria is rarely conducted. Furthermore, we were not able to gather more information about a large number of children due to compliance limitations such as missed follow-up examinations, or failure to provide newborns’ blood for tests.
In our study, none of the neonatal cases showed a fourfold higher RPR titer compared with the mother. Although IgM positivity confirmed infection, a negative IgM result did not exclude CS, and clinical context remained essential.
Limitations
Given the cross-sectional observational design of our study, the analysis was necessarily based on previously recorded clinical documentation. A further important limitation is that adequate information on neonatal outcomes was available for only 106 of the 185 pregnancies, which may have resulted in an underestimation of the true number of congenital infections.
Conclusion
In conclusion, GS and CS remain significant public health concerns in Hungary and require interventions. The large number of diagnoses made in the second or third trimester indicate that a single first-trimester screening is insufficient in the current epidemiological trends, and repeated screening during pregnancy as well as at the time of birth if no tests were performed before should be mandatory. Our findings highlight the need for interdisciplinary collaboration, with antenatal screening primarily conducted in obstetric care and sustained clinical vigilance for CS within pediatric practice. Our study also highlights significant structural barriers, including late presentation to prenatal care and high rates of loss to follow-up, which frequently delayed diagnosis and prevented the collection of neonatal data. To address these challenges in vulnerable populations, diagnostic services could leave hospital settings through point-of-care testing in community settings. This approach reaches isolated groups with limited transportation or access to prenatal care. Furthermore, enhancing health literacy through education and public health campaigns can support early doctor visits and reduce the stigma associated with syphilis screening. Overall, this study provides insight into domestic epidemiological patterns and the specific clinical characteristics of syphilis in pregnancy.
Supplemental material
Supplemental material - Epidemiological and clinical characteristics of gestational and congenital syphilis in Hungary: A cross-sectional, single-center case analysis
Supplemental material for Epidemiological and clinical characteristics of gestational and congenital syphilis in Hungary: A cross-sectional, single-center case analysis by Ugur Cakir, Gábor Karácsony, Eszter Ostorházi, Péter Holló, Béla Tóth in International Journal of STD & AIDS
Footnotes
Ethical considerations
The study was conducted in accordance with institutional and national ethical standards, approved by Semmelweis University Regional, Institutional Scientific and Research Ethics Committee (SE RKEB, decree no: 8/2026)
Consent to participate
The authors declare that this study does not contain any personal information that could lead to the identification of the patients.
Funding
The authors disclosed receipt of no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data are available upon reasonable request from the corresponding author.
Supplemental material
Supplemental material is available online.
