Abstract
Background
Sexually transmitted and blood-borne infections (STBBIs) disproportionately affect key populations in Canada. For example, recent estimates suggested that the proportion of people living with hepatitis C is the highest among people who use injection drugs and that gay, bisexual and other men who have sex with men represent a high proportion of new cases of infectious syphilis. Understanding what STBBIs test users and potential testers perceive as important aspects of testing will help inform testing initiatives. We aimed to determine aspects of STBBI testing that are important to a diverse range of key populations in Canada.
Methods
We conducted qualitative interviews and focus groups with people from key populations (gay, bisexual, and other men who have sex with men; African, Caribbean, or Black individuals; Indigenous individuals; sex workers; people who use substances and injection drugs) and people who do not identify as a key population member. We conducted a thematic analysis.
Results
Two major themes emerged: stigma and inequality, and journey into and through the healthcare system. Within the first theme, participants had diverse perspectives on how aspects of their identity interacted with willingness to seek testing. Within the second theme, participants discussed aspects of testing. Test costs, wait times, and testing accuracy were all viewed as important, but differing perspectives emerged about privacy of testing and receiving results, testing location, and who administers the test.
Conclusions
Participants’ perspectives on STBBI testing and willingness to test were informed by their experiences and aspects of their identity.
Introduction
Sexually transmitted and blood-borne infections (STBBIs) have a substantial impact on individuals’ health and well-being. 1 Maximizing testing enables early diagnosis and treatment and reduces transmission. 1 Investigating ways to optimize STBBI testing options is an important step toward expanding access to care for people at risk for STBBIs. Equity-deserving groups are disproportionately affected by STBBIs in Canada, including gay, bisexual, and other men who have sex with men, transgender people, people with experience in a prison environment, Indigenous individuals, people who use substances and injection drugs, sex workers, and people who are from countries where HIV and hepatitis B and C are endemic. 2 These populations experience discrimination and stigma, which can decrease access to testing. These populations are also disproportionately affected by STBBIs in Canada. For example, about 0.56% of the general population were living with chronic hepatitis C in 2021. 3 By contrast, the proportions varied by populations: 0.9% among gay, bisexual and other men who have sex with men, 3.2% among people incarcerated in federal prisons, 3.3% among Indigenous individuals, and 36.9% among people who use injection drugs. Another example is infectious syphilis: of all cases reported in Canada in 2022, males accounted for 65% of cases, of which gay, bisexual and other men who have sex with men accounted for 41% (27% of all cases).4,5 It is important to understand how people value different aspects of STBBI testing and determine any variations in preferences among different groups, which can improve uptake of testing, and better inform future testing policies.
Few studies in Canada explore people’s preferences for STBBI testing options,6–11 and most limit their focus to certain subpopulations or types of STBBIs. Studies focusing on HIV testing identified barriers to testing that include fears of a potential positive test result, perceived low risk for exposure to HIV, stigma, and insufficient knowledge. 8 Population-specific barriers include accessibility for those living in rural communities, stigma about behaviours for sex workers and people who use substances and injection drugs, and a lack of multilingual support for those whose first language is not English. 8 Studies of people who identify as gay, bisexual, and other men who have sex with men identified enablers such as more inclusive testing locations, extended hours, reduced waiting and testing time, multiple and convenient testing options, and non-judgemental and non-stigmatizing provider relationships.12,13
In this study, we determined aspects of STBBI testing in general that are important to a diverse range of key populations.
Methods
Study design and population
We conducted a qualitative study among people from five key populations (gay, bisexual, and other men who have sex with men; members of the African, Caribbean, or Black communities; sex workers; people who use substances and injection drugs; and/or Indigenous individuals) as well as individuals who did not identify as a key population member. Participants were eligible if they were 19 years or older, were able to read and speak English, and resided in Canada.
Participant recruitment
We recruited participants using purposive and snowball sampling methods to ensure there was adequate participation from each of the key populations, and there were participants from across Canada and in both urban and rural locations. Recruitment occurred via advertisements on Facebook, Twitter (now known as X), REACH BC (a provincial research network), and word of mouth. The eligibility of interested individuals was assessed via a participant characteristics questionnaire. A consent form was completed by eligible individuals. Recruitment occurred between August 2021 and October 2022. Rather than determining a sample size for the study a priori, which is inconsistent with qualitative research principles, we collected data until we reached theoretical saturation.
Data collection
We conducted focus groups and interviews, depending on participants’ preferences, via videoconferencing, using a semi-structured guide. Information on demographics such as gender identity, age, and whether they identified with any key population(s) was collected before focus groups and interviews were conducted. Two authors (MES, CEO) conducted the interviews and focus groups, which were recorded and transcribed verbatim by a professional transcription company under a non-disclosure agreement. One author (CEO) reviewed all of the transcripts for accuracy. Participants were provided with a $50 gift card.
Data analysis
We conducted a thematic analysis to find patterns and themes within the data. 14 Three researchers (MES, CEO, MB) read, coded, and analyzed the transcribed interviews. All three researchers have experience in health services research as well as diverse research interests such as health equity, program evaluation, and care delivery. CEO is also a trained medical doctor. One researcher (MB) conducted line-by-line coding in NVivo 12 and the team met frequently to discuss arising patterns and points of interest. The team created a codebook with preliminary codes and potential categories. MB, AE, and MES analyzed the data by moving related codes together into categories, which informed future themes. After iteratively analyzing the data, the team developed the final themes. Analyses were constructivist as we explored our participants’ experiences with testing and looked for connections across categories. 15 Constructivism assumes that the researchers were not simple observers of the data. Instead, the researchers and their interactions with the participants co-produced the data. This means that throughout the analysis, the researchers immersed themselves in the participants’ narratives and perspectives and kept them in the foreground as they developed the codes, categories, and themes. 15 A selection of quotes from interviews and focus groups are included in the Results section. All participants were assigned a randomized letter as a pseudonym initial to protect their anonymity.
Ethics approval
Approval was granted by the University of British Columbia-Providence Health Care Research Ethics Board (REB Number H20-03266).
Results
Participant demographics (n = 31).
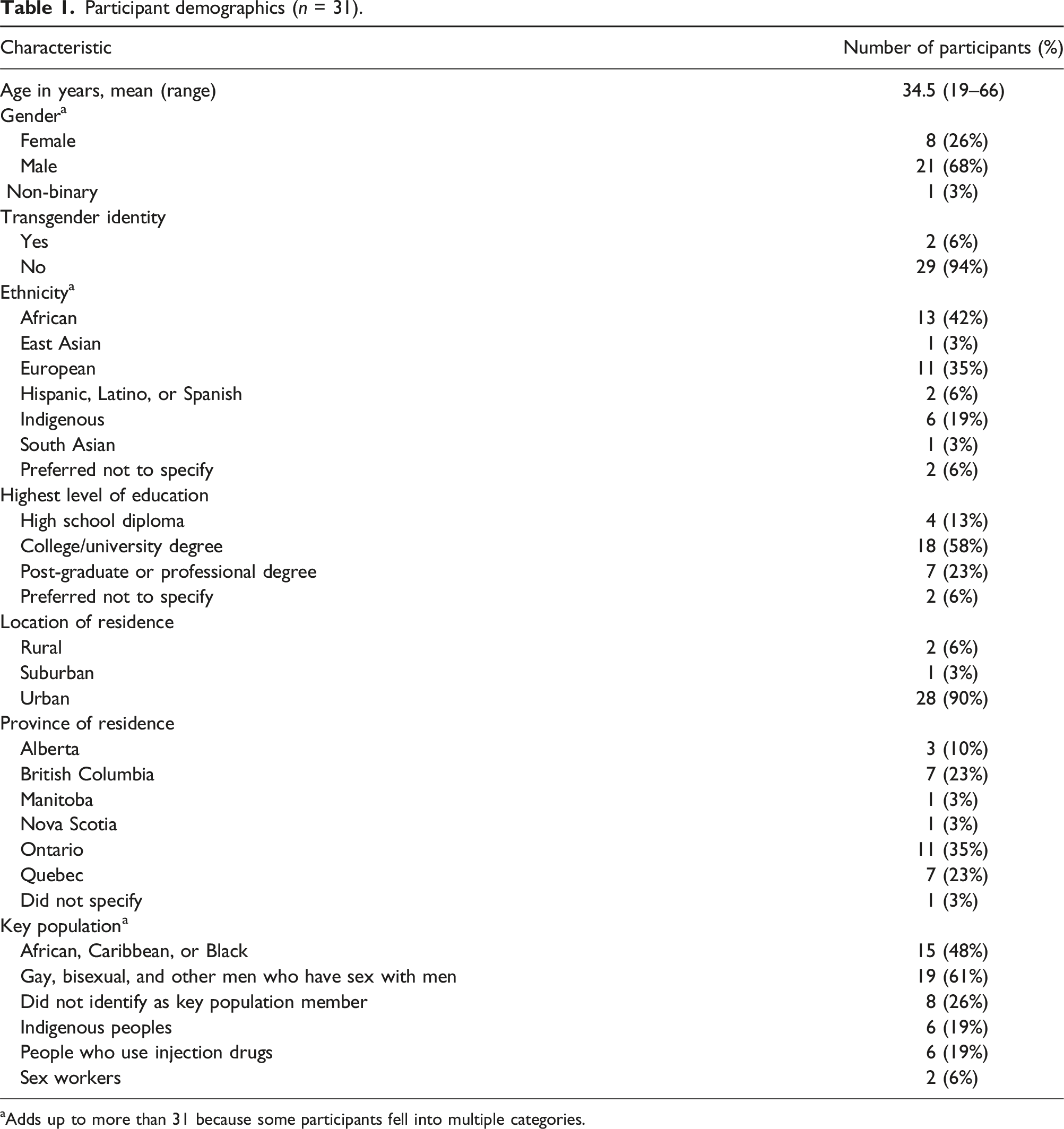
aAdds up to more than 31 because some participants fell into multiple categories.
Illustrative quotes relating to themes and subthemes.

Note. All participants were assigned a randomized letter as a pseudonym initial to protect their anonymity. Abbreviations: ACB = African, Caribbean or Black; GBMSM = gay, bisexual or other men who have sex with men; PWUID = people who use injection drugs; SW = sex worker.
Stigma and inequality
Overview of experiences
For many participants, discussions about the barriers and willingness to seek STBBI testing were intertwined with discussions about stigma against various aspects of identity.
A common point of discussion for both participants who identified as gay, bisexual, and other men who have sex with men and participants who identified as African, Caribbean, or Black or Indigenous was the availability of testing services that were appropriate for those belonging to equity-deserving groups. This manifested as expressing aversion towards medical clinics that lack staff who are trained to use affirming language (Table 2 Quote A). Others were concerned that immigrants for whom English is not their first language would have greater difficulties accessing testing. Some participants who identified as gay, bisexual, and other men who have sex with men also discussed how living in rural communities may exacerbate barriers that some groups face, whether because of limited safe testing options nearby, financial burden with travel, or with gossip when a person is recognized by community members during a testing visit (Quote B). The possibility of being noticed or stared at or watched whilst accessing healthcare was also a concern for participants who identified as African, Caribbean, or Black (Quote C). Some African, Caribbean, or Black participants also felt historically underserved by projects in the community that aimed to improve testing uptake.
Participants who used injection drugs discussed how drug use intersected with precarious housing and sex work. In particular, they felt individuals who are experiencing precarious or inadequate housing or who are living with substance use disorder may not be able to book and make appointment times or physically travel to clinics due to their concentration in limited urban areas, or may be further stigmatized even if they do access these services (Quote D).
Perceptions on the possibility of a positive test result
We also found that perceptions about the possibility of a positive test result also varied across our participants. Participants who identified as gay, bisexual, and other men who have sex with men or participants who did not identify as a member of a key population discussed the importance of knowing the results and that the fear of a positive test was not a barrier or that it was a barrier that can be overcome (Quote E). Rather, not knowing was an expressed fear for some but not all participants. Among participants who identified as African, Caribbean, or Black or Indigenous, there was notable fear over receiving a positive result and this translated to fear about testing. Participants who identified as gay, bisexual, and other men who have sex with men and African, Caribbean, or Black or Indigenous also shared the fears expressed by participants who were African, Caribbean, or Black or Indigenous (Quote F), but one participant noted the importance of knowing and being brave.
Stigma as a barrier
Participants went on to discuss stigma related to STBBI status and testing, and how the stigma acts as a barrier for testing. Some participants traced the stigma to socio-cultural biases about STBBIs. There were discussions about the lack of normalization as well as negative cultural attitudes around engaging in sexual activities or being tested (Quote G). The potential for feelings of shame or embarrassment relating to testing, and the potential for victimization due to a positive result that stems from stigmas towards STBBIs, were perceived barriers to getting tested. One participant who identified as African, Caribbean, or Black elaborated that it is not just public stigma from others, but also self-stigma that needs to be overcome when seeking testing (Quote H). While the need for education to address stigma was brought up by different participants, this was viewed as particularly important for African, Caribbean, or Black or Indigenous individuals. For participants who identified as gay, bisexual, and other men who have sex with men, a strong sense of community and a stable social network was expressed as a protective factor and helped with testing uptake (Quote I). Some also discussed stigma arising from the healthcare system. Participants described interactions with healthcare providers that spanned both enacted stigma (e.g., receiving substandard care) and perceived stigma (e.g., feeling judged) against them based on their group membership.
In summary, we found that parts of participants’ identity and their past experiences framed their discussions about STBBI testing. This first theme establishes the context in which themes about the testing journey itself emerge.
Journey into and through the healthcare system
Participants shared their perspectives on different features of the testing process, and we have used these features to define the following subthemes. We encourage the reader to bear in mind the context set out in the first theme, and that participants approached the discussions differently.
Funding and costs
There were discussions around the need for funding to increase access to testing, such as providing more testing locations and longer hours at testing locations, and funding innovative programs to reach those who have limited access, which was seen by some as a way to combat stigma (Quote J). Overall, participants valued public funding of tests. This related to discussions around their costs: some participants expressed tests should be free for all while others were willing to pay out-of-pocket (Quote K). Of those willing, there was some acknowledgement that their willingness was because of having financial sufficiency through employment or support from their community (Quote L). It was also noted that even if tests are free, if treatment is not also free, some people may be deterred from testing at all. Some participants worried that if a test was provided for free it would not be as accurate or comprehensive as a test that one had to pay for.
Privacy and confidentiality (Quote M)
Privacy and confidentiality, both related to sample collection and receiving test results, were discussed from different perspectives. Participants who identified as gay, bisexual, and other men who have sex with men generally focused on maintaining privacy of testing and results between themselves and their healthcare providers. Some of these participants had positive relationships with their healthcare providers and welcomed testing in their offices, but there were concerns by others of information potentially spreading to family members in the context of family physician care [see Engagement with healthcare professionals]. Participants who engaged in other stigmatized behaviours, such as sex or drug use, raised concerns with being seen or recognized at testing locations (Quote N). Some of these participants also noted both the convenience and added privacy risk with using digital means to communicate test results (Quote O). Privacy was mentioned as a benefit of self testing, as one would avoid being seen at a location where STBBI tests are conducted. This was mentioned as especially important in small, rural communities where most people know each other.
Wait times
Participants discussed anxiety related both to waiting for a test and waiting for test results (Quote P). Long wait times and limited hours of operations (whether for drop-in or appointment) were barriers for those waiting to get a test. Waiting for test results also caused stress and anxiety and the wait times that were considered acceptable depended on whether they are waiting for routine tests or following a high-risk exposure. In the case of participants who engaged in sex work, concerns about wait times were also driven by the impact on their ability to work.
Accuracy
Participants felt it was important that tests were accurate and they generally expected test accuracy to be very high (Quote Q), although some believed self-tests had unacceptably low levels of accuracy (Quote R). Thus, while no one liked waiting for a test result, some participants revealed they would not trust the accuracy of test results that were received quickly. Some participants were willing to accept a slightly lower accuracy for tests for STBBIs that they considered less severe or for diseases without treatment.
Location (Quote S)
The way location affects STBBI testing decisions relates to both geographical location and appropriateness of the setting. The distance to the clinic and opening hours were noted as a barrier to testing, especially for those living in rural and remote communities who have to travel long distances to reach healthcare services. Participants noted self-testing could overcome this (Quote T). Different participants expressed different preferences for where they would like to have a test conducted. Some preferred a clinical setting, such as a sexual health clinic or a lab in the community, often due to the perception that a test would be more accurate when conducted in a professional setting (Quote U). Others expressed preference for an at-home test due to convenience and privacy (Quote V). Some indicated that they would prefer a location that caters to their cultural needs, such as clinics specifically for people who identify as queer.
Engagement with healthcare professionals
The type of healthcare professional participants prefer to engage with to obtain an STBBI test varied. Some participants preferred their family doctor because they felt their family doctor had knowledge of their health history and they have an established, trusting relationship with them. Going to a family doctor also meant they would already be connected to follow-up treatment if needed, which helped ease stress related to the uncertainty around what would happen if they received a positive test result (Quote W). Conversely, some participants feared their privacy and confidentiality would not be maintained, since their family doctor knows their family members (Quote X).
Methods of testing (Quote Y)
Participants also discussed preferences related to methods used for testing and which STBBIs are tested for, but these varied from person-to-person based on their personal situations (e.g., preferring a finger prick over a blood draw for people who are afraid of needles, being tested for specific STBBIs based on a known exposure to a particular infection).
Financial accessibility of healthcare services
Participants discussed the cost of subsequent healthcare services (including treatment) following a positive test. Participants noted that the cost of subsequent treatment and the lack of insurance coverage can discourage testing (Quote Z). Some participants perceived that the lack of a family doctor and difficulty becoming attached to primary care limits the available options for subsequent healthcare services, and this ultimately contributes to the financial barrier of accessing care following testing (Quote AA).
Discussion
The study participants discussed factors that influence decisions about STBBI testing that are related to aspects of their identity and life experiences (contextual factors) and aspects of the testing process (systemic factors). Test costs, accuracy, and testing wait time were all viewed similarly by our participants: having publicly funded and accurate tests that do not require long wait times to receive are important. However, there were some interactions between these three aspects such as a belief that test accuracy is a function of test cost and turnaround times for results. There was also a perception that self-testing and testing in the community would not be as accurate compared to testing in a professional healthcare setting, which is contrary to guidance by Health Canada that requires, e.g., HIV rapid diagnostic tests to have a minimum sensitivity and specificity of 99% or above. 16 Perceptions about testing location, which healthcare provider a test-seeker interacts with, and privacy concerns differed by equity-deserving group and context. Maintaining the confidentiality of test results between the provider and the test taker was most important for participants who identified as gay, bisexual and other men who have sex with men. By contrast, privacy concerns from participants who were engaged in sex work or who used injection drugs were related to the testing process itself: they were concerned with being identified or recognized in waiting rooms and at testing clinics. Those with privacy concerns were particularly interested in home testing options as a means to avoid being recognized. Preference for whom participants interacted with during testing depended on whether they had access to primary care and family contexts (e.g., whether family members were attached to the same primary care provider or not).
Our findings are similar to other Canadian studies that have explored factors influencing decisions about STBBI testing.7,8,12,13 Concerns with testing identified in the literature include: lack of privacy and confidentiality, stigma, geographic location, wait times, limited opening hours, lack of culturally sensitive services, cost, insufficient knowledge and lack of resources, low risk perception, and fear of a positive result.8,12 Enablers of testing uptake include: more accessible clinics (locations and hours), no wait times, privacy protection, non-stigmatizing and culturally sensitive testing locations.7,13 These existing studies were primarily focused on men, especially gay, bisexual, and other men who have sex with men, in major urban centres. Our study expanded these findings to include participants from across Canada and participants from diverse populations, highlighting how unique people’s experiences with STBBI testing are, and how these were informed in part by what STBBI status symbolizes to different groups of people.17–20 Our inclusion of diverse participants also enabled the analysis of intersections in identity and experience, particularly among people who use substances and injection drugs. For example, a systematic review of HIV testing facilitators and barriers in different key populations found stigmatization was a common barrier for sex workers but not for people who use substances and injection drugs. 8 Our study found similar stigmatization among sex workers but we also found people who use substances and injection drugs discussed stigma in the context of their experience with sex work and precarious housing. This form of intersectional stigma affirmed the challenges associated with meeting healthcare needs of diverse populations.8,21
A key strength of this study was our focus on including multiple key populations, which enabled us to uncover some of the interactions between personal contexts and different aspects of participants’ identity. Another strength was the strategies used to enhance qualitative research rigour, including purposive sampling strategies to include a diverse range of key populations and maintaining detailed documentation of our analysis process and meeting regularly as a research team. A limitation of our study was that, although we reached a broad range of different key populations, there were only a very small number of participants from some of these populations. Recognizing there is variability within each group, we may not have captured the breadth of experiences and perspectives within each key population. Second, virtual interviews and focus groups exclude those without Internet access. While Indigenous individuals were included in the study, Indigenous communities were not engaged and the study did not use an Indigenous worldview or methodologies. 22 Future Indigenous-specific research should explore this topic.
Conclusion
Many aspects of STBBI testing services are important to people and people weigh multiple factors when choosing to seek, or not seek, STBBI testing. Privacy and confidentiality were particularly important due to the stigma associated with STBBIs. Willingness to seek STBBI testing was also tightly bound to stigmas associated with different aspects of identity. Home-based self-testing may be a preferable option for people who may be concerned about the privacy and confidentiality of visiting clinics at which they may be recognized. However, there were misconceptions that self-testing is not accurate and that free testing, particularly options run by public health programs, is not accurate. Education campaigns to dispel these beliefs may facilitate testing uptake.
Footnotes
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Wei Zhang is leading a project on an entirely different topic which is funded by a grant-in-aid from Pfizer Canada. The University of British Columbia is the grant recipient.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Canadian Institutes of Health Research Team Grant: HIV/AIDS Biomedical and Clinical Research – Prevention – Large.
Ethical statement
Data Availability Statement
Due to the sensitive nature of the research, supporting data is not available.
