Abstract
Candida lusitaniae is a vaginal commensal. Cases of vaginitis, vulvovaginitis and recurrent vulvovaginitis caused by this yeast are very rare. In the oral cavity, C. lusitaniae causes stomatitis in immunocompromised patients. We describe a case of stomatitis and angular cheilitis caused by C. lusitaniae in a female patient with type 2 diabetes. The infection was most likely transmitted following genital-oral intercourse with the patient’s girlfriend, who was affected by C. lusitaniae vulvovaginitis.
Introduction
Candida lusitaniae is a vaginal commensal.1,2 Cases of vaginitis (V), vulvovaginitis (VV) and recurrent vulvovaginitis (RVV) caused by this yeast are very rare.3–16 In the oral cavity, C. lusitaniae causes stomatitis in patients with dentures, diabetes, HIV-positivity, neoplasms, and in patients receiving chemotherapy, radiotherapy and broad-spectrum antibiotic therapy.17–23 We describe a case of stomatitis and angular cheilitis caused by C. lusitaniae in a female patient with type 2 diabetes. The infection was most likely transmitted following repeated genital-oral intercourse with the patient’s girlfriend, who was affected by C. lusitaniae VV.
Case
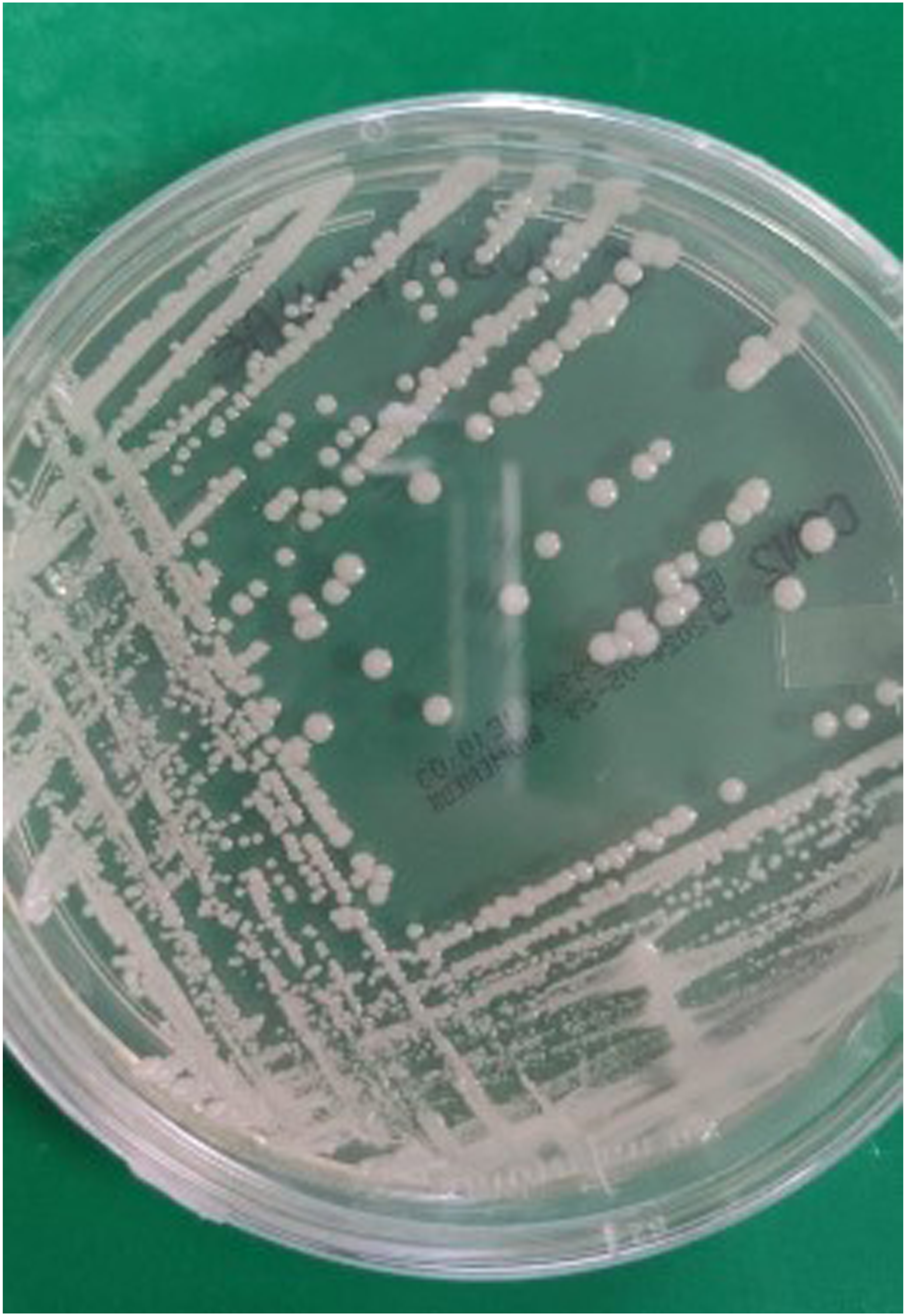
A 37-year-old female was admitted with a clinical diagnosis of angular cheilitis. The patient stated that she had type 2 diabetes mellitus since the age of 32, for which she was on therapy with metformin (1 g/day). The patient also said that her cheilitis appeared approximately 1 month earlier and that it was unsuccessfully treated, at other dermatological centres, with topical betamethasone valerate, fusidic acid and gentamicin. The patient also stated that her girlfriend was affected by vulvovaginal candidiasis caused by C. lusitaniae and that they had 2-3 episodes of genital-oral intercourse weekly. Dermatological examination revealed, at both commissures, an irregular erythematous area with small crusts and scales (Figure 1). The oral cavity was mildly erythematous. The patient complained of burning sensation in the oral cavity and mild pruritus at the commissures. Laboratory tests showed increase in glucose levels (136 mg/dl) and glycated haemoglobin (7.4%). All other tests were within normal ranges. Bacteriological examinations were negative. Mycological cultures on CAN 2 BioMérieux, obtained from commissures, tongue and cheeks, were positive for C. lusitaniae (Figure 2). The patient declined an oral antimycotic therapy. She was therefore treated with miconazole oral gel (3 rinses/day for 3 weeks). Complete remission was observed 1 month later. Follow up (at 5 months) was negative. Angular cheilitis caused by C. lusitaniae. Culture of C. lusitaniae on can 2 BioMé.rieux.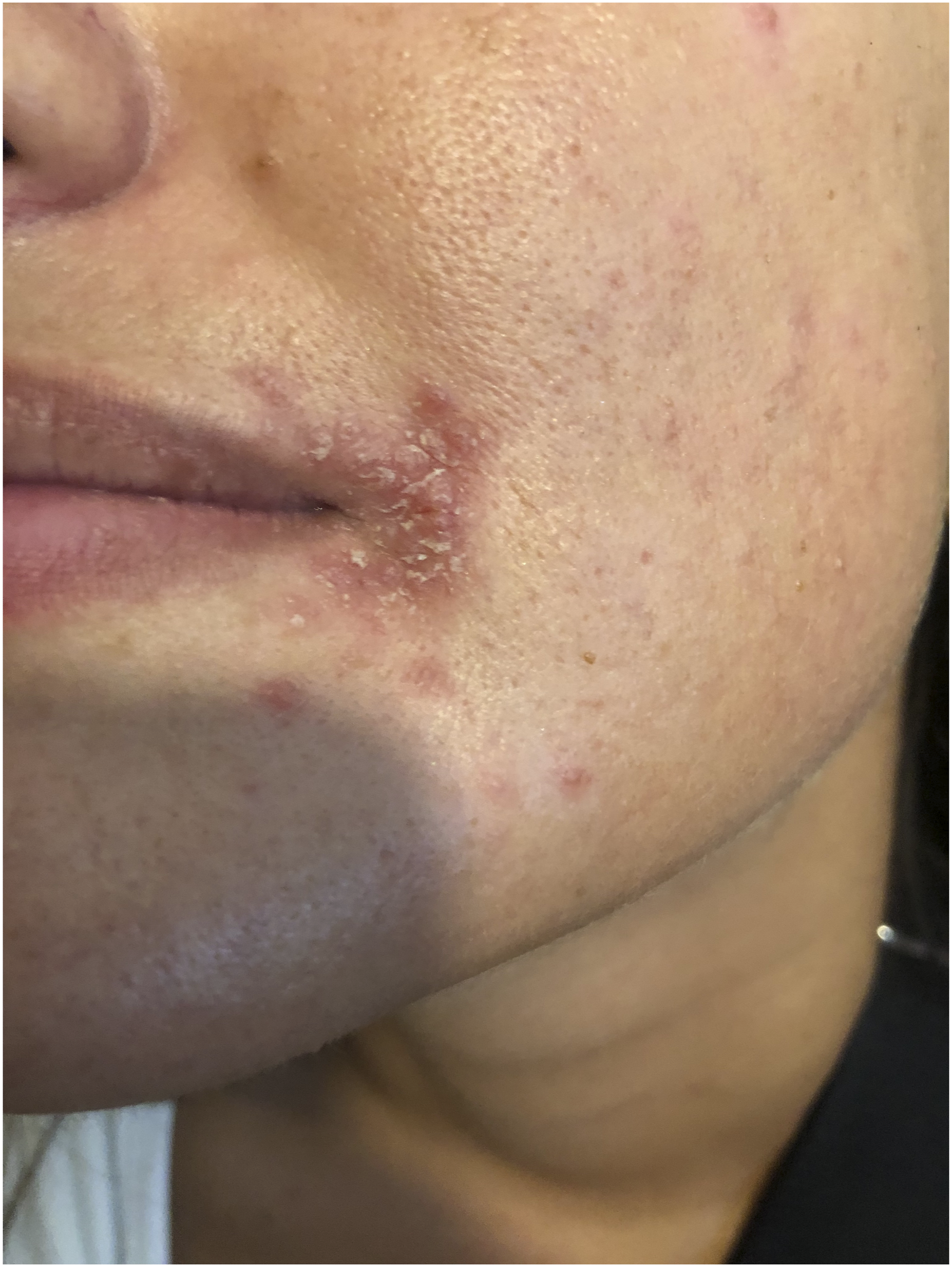
Discussion
C. lusitaniae is a vaginal commensal.1,2 To our knowledge, the first case of C. lusitaniae V was reported in 2000. 3 Cases of V, VV and RVV caused by C. lusitaniae are very rare.4–14 In the study by Richter et al., 6 C. lusitaniae was isolated in one out of 593 vulvovaginal isolates. This yeast was isolated in 1% of Jamaican women with VV 7 ; in 1/272 isolates (0.37%) of Tanzanian pregnant women with V 8 ; in 0.2% of Chinese patients with VV 10 ; in 0.48% of Ugandan pregnant women with VV 11 ; in 0.39% of Vietnamese patients with V 13 and in 1.9% of Iranian women with VV and RVV. 14 Only in another Iranian study, C. lusitaniae was isolated in 18.95% of patients with VV or RVV, resulting as the second most common cause of VV. 15 Finally, in a recent study carried out in Colombia, the yeast was isolated in 7.5% of RVV candidiasis. 16 In the oral cavity, C. lusitaniae is not considered as a commensal. This yeast causes stomatitis17–23 in patients with poor oral hygiene, 22 xerostomia, 22 partial or total dentures,18,19 diabetes,19,23 HIV-positivity, 21 neoplasms,19,20,22 and in patients receiving chemotherapy, 19 radiotherapy 19 and broad-spectrum antibiotic therapy. 19 In children and adolescents with neoplasms, the most frequent location of C. lusitaniae candidiasis was the tongue (in 72.7% of patients); the pseudomembranous variety was the most frequent clinical presentation (in 78.7% of patients). 20 40 per cent of HIV-positive patients had angular cheilitis as the most frequent clinical variety. 21 C. lusitaniae can also be responsible for esophageal involvement.2,17 Literature data about the therapy of C. lusitaniae infections are conflicting. This yeast is susceptible to terconazole, 3 miconazole 17 and anidulafungin, 22 sometimes resistant to caspofungin 15 and fluconazole15,22 and always resistant to itraconazole (100% of resistance in the study by Mukasa et al.) 11 and amphotericin B.24,25 As previously mentioned, our patient was successfully treated with miconazole oral gel, while her girlfriend’s VV was treated by her gynecologist with fluconazole (150 mg). In summary, we have described a case of stomatitis and angular cheilitis caused by C. lusitaniae in a female with type 2 diabetes mellitus. It is very likely that this infection was transmitted by genital-oral intercourse. To our knowledge, this event was never reported in the international literature.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
