Abstract
Introduction
Like other European countries, such as the Netherlands, 1 there has been an increase in the number of HIV diagnoses through heterosexual transmission in recent years, as well as considerable increases in the numbers of diagnoses of other STIs, such as chlamydia and HPV, especially in young women as part of routine reproductive healthcare check-ups.2,3 Non-use of condoms is a key risk factor in STI/HIV transmission particularly in the context of partner change,4–6 and with new partners whose sexual history and STI testing practice is less likely to be known.
To date, research regarding factors associated with the non-use of condoms has mainly focused on men who have sex with men (MSM) as a population who are at particularly high risk of STI/HIV transmission, while the heterosexual population has gained increased attention in empirical research only in recent years. This research shows that single heterosexuals who are casually dating are more likely to use condoms than those in a committed relationship or with a steady sex-partner.4,6–11 While some other countries have population-based survey data to examine the context of non-use of condoms (e.g. 4,5,8,11,12), this has not been the case for Germany. The present study, to our knowledge, is the first to investigate factors associated with the non-use of condoms in the German population, focusing on heterosexually-active single people, in terms of the key sociodemographic characteristics, sexual behaviours and aspects related to the relational/situational features of the sexual encounter.
Materials and methods
Study and data collection
The “German Health and Sexuality Survey - GeSiD” is a cross-sectional study with a population representative sampling scheme conducted by the Institute for Sex Research, Sexual Medicine and Forensic Psychiatry at the University Medical Centre Hamburg-Eppendorf in collaboration with the social research institute KANTAR and funded by the Federal Centre for Health Education (BZgA). The study was approved by the ethics committee of the Hamburg Psychotherapy Association (“Hamburger Psychotherapeutenkammer”).
Based on a two-stage random sample design with names and addresses drawn from 200 “sample points” (usually coinciding with the residents’ registration offices) throughout the entire Federal Republic of Germany, in the time period 2018 to 2019. Altogether, 4,955 individuals (2,336 men and 2,619 women) aged between 18 and 75 years participated, which included oversampling those aged 18–35, accounting for 37.7% (n = 1,869) of the sample. The response rate, according to AAPOR criteria, 13 was 30.2% (AAPOR Response Rate 4).
The survey was conducted by means of computer-assisted personal interviews (CAPI) in the participant’s own home, and included an extensive self-completion section (computer-assisted self-interview, CASI). Before the start of the interview, respondents confirmed that they had been informed about the goals of the study, anonymisation and data protection, and the voluntary nature of participation by providing a written declaration of consent.
The questionnaire, which had previously been tested in a pilot study, 14 included over 260 questions on a range of topics including various sexuality-related topics, developed following extensive research of similar studies internationally, as well as the WHO Indicators of Sexual Health. 15 Women were interviewed by women and men by men. The mean duration of the interviews was 51 min (median = 48, range 19–208 min).
Population of interest
The present analyses focus on the subsample of heterosexually-active single people, defined as those who reported no current relationship, that they had been single for at least 1 year prior to interview, and who stated at least one sexual encounter with someone of the opposite sex during this time.
Primary outcome
Non-use of condoms at last sex
Participants were asked whether they had used any contraceptives at last sex and if so, which. The question had been adapted from earlier German studies 16 and offered multiple answer options. One of these options was condom use. Answers were dichotomised with regard to the non-use of condoms at last sex into “condoms used” and “non-use of condoms” (no contraception or other type of contraception).
Factors hypothesised to be associated with non-use of condoms
Sociodemographic characteristics
Categorised variables were included on the basis of the information provided by the respondents on: their age at the time of the interview (18–35 years; 36–75 years), level of education (“low”; “medium”; “high”; broadly corresponding to: no school-leaving qualification (yet) or lower secondary school; secondary school; university entrance qualification or academic degree) and migration background (“no”; “yes” [participant and/or parent born in another country]).
Sexual behaviour and sexual history
Type of sexual practices during the latest sex
Participants were asked in the CASI about the sexual practices they had performed at last sex (vaginal intercourse; oral sex; anal sex; other genital contact, e.g. manual contact). Multiple response options were categorized into “vaginal intercourse only”, “vaginal intercourse and oral sex” and “vaginal intercourse combined with oral sex and other genital contacts”. Other types and combinations of sexual practices were pooled into one category due to small numbers (n < 30).
Number of opposite-sex partners during the past year
Women were asked how many men they had had sex with, men were asked how many women they had had sex with during the past year. Free-text responses ranged from 1 to 40 and were categorized into “1”, “2” and “3+”.
Age at first heterosexual intercourse
Respondents were asked for their age at first sexual intercourse with an opposite-sex partner (“vaginal intercourse”; “oral sex”; “anal sex”; “other genital contact, e.g. manual contact”). Free-text responses ranged from 8 to 27 years (one person stated to have had other genital contact at the age of 8 years). Answers were categorized into “<16 years” and “16+ years” broadly corresponding to early and late sexual debut.
Non-use of condoms at first heterosexual intercourse
Analogous to the question about non-use of condoms at last sex (see above), a question asked about contraception use at first sexual intercourse with someone of the opposite-sex. Answers were categorized into “use of condoms” and “non-use of condoms“ (no contraception or other type of contraception).
Relational and factors relating to the circumstances of last sex
Type of relationship
Participants were asked how they perceived the relational context of their last sexual encounter (“What kind of relationship did you have with this person?”) and were offered three possible response options: “It was a one-night stand/non-recurring sex” [es war ein one-night-stand/einmaliger Sex]; “It was a longer relationship” [es war eine längere Affäre]; “It was the beginning of a loving relationship” [es war eine beginnende Liebesbeziehung]).
Initial meeting venue
Based on an item used in former studies, 17 participants were asked where they had met their last sex partner. Answer categories were dichotomized into “offline” (e.g. “going out in the evening”) and “online” (e.g. “via an online dating agency”).
Alcohol and/or drug use at last sex
Participants were asked “The last time you had sex, were you under the influence of alcohol or drugs?” Multiple answer options were categorized into “no” (“no, neither alcohol nor drugs”), “solely alcohol” (“yes, alcohol”) and, due to low case numbers (nunweighted = 31), a pooled category for “solely drugs or drugs combined with alcohol” (drug use options were: “cannabis”; “amyl nitrite (poppers)”; “a different substance”).
Talking about condom use before sex
With regards to their last sexual encounter, participants were asked “Did you discuss the use of condoms before having sex?” (“no”, “yes”) based on items previously used in German studies. 18 Participants who reported not remembering (n = 4) were excluded from analysis.
Statistics
The data were weighted on the basis of gender, age, education, nationality and region in accordance with the 2018 German census ahead of analyses. A detailed description of the methodology is provided by Matthiesen et al. 19 and with further regard to the operationalization of gender by Muschalik et al. 20
The statistical analysis was weighted using the “complex sampling” module in IBM SPSS Statistics, version 27. Descriptive frequencies are reported in conjunction with the 95% confidence interval (95%-CI). Variables hypothesised to be associated with the non-use of condoms were tested using binary logistic regression analysis. Crude odds ratios and odds ratios adjusted for gender and continuous age were reported including 95% CIs and, referring to AORs, overall p-values for associations.
Results
Sample description
Sample characteristics.
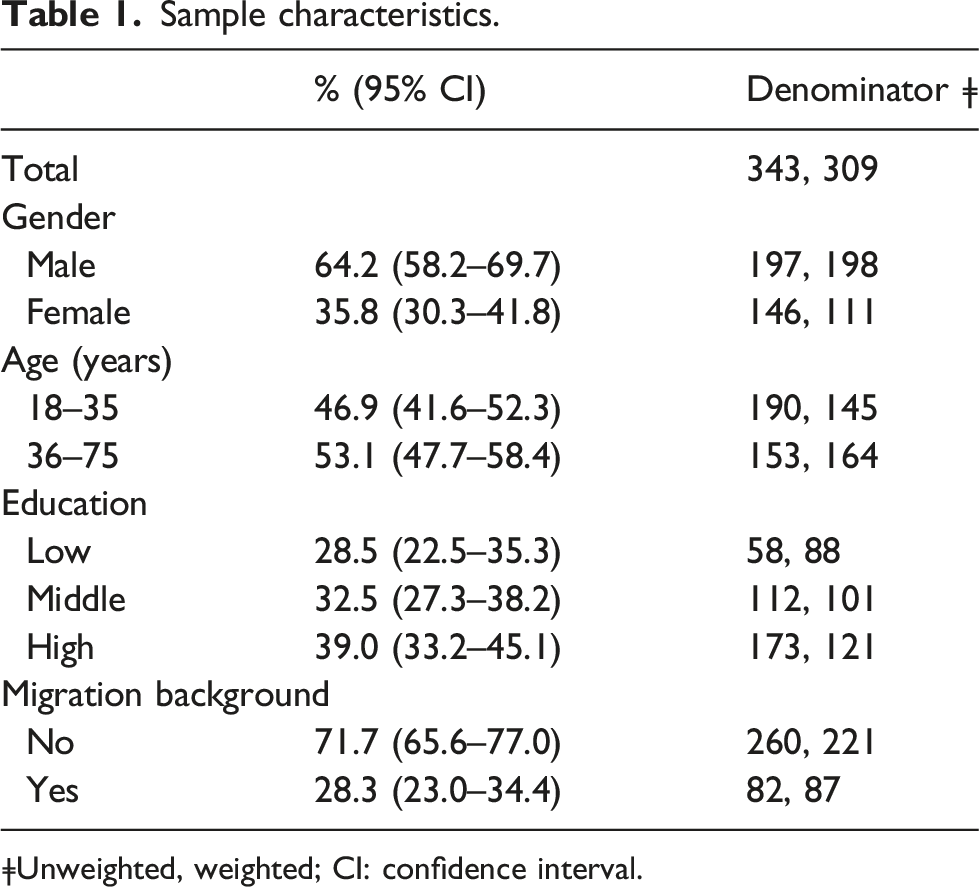
ǂUnweighted, weighted; CI: confidence interval.
Sociodemographic characteristics
Non-use of condoms at the last sex by participant characteristics.
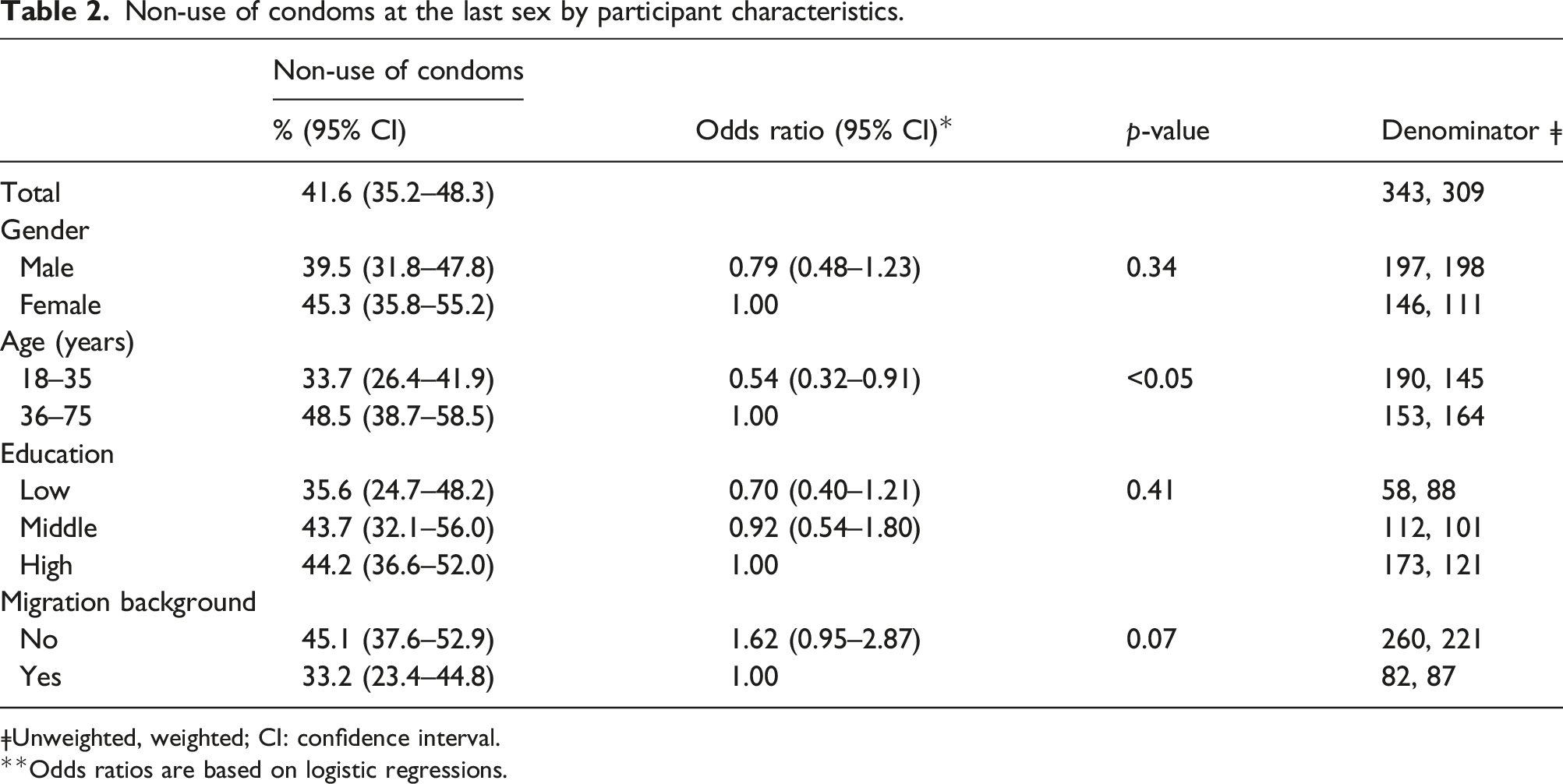
ǂUnweighted, weighted; CI: confidence interval.
**Odds ratios are based on logistic regressions.
Sexual behaviour and sexual history
Non-use of condoms at the last sex in singles by sexual behaviour and sexual history factors.
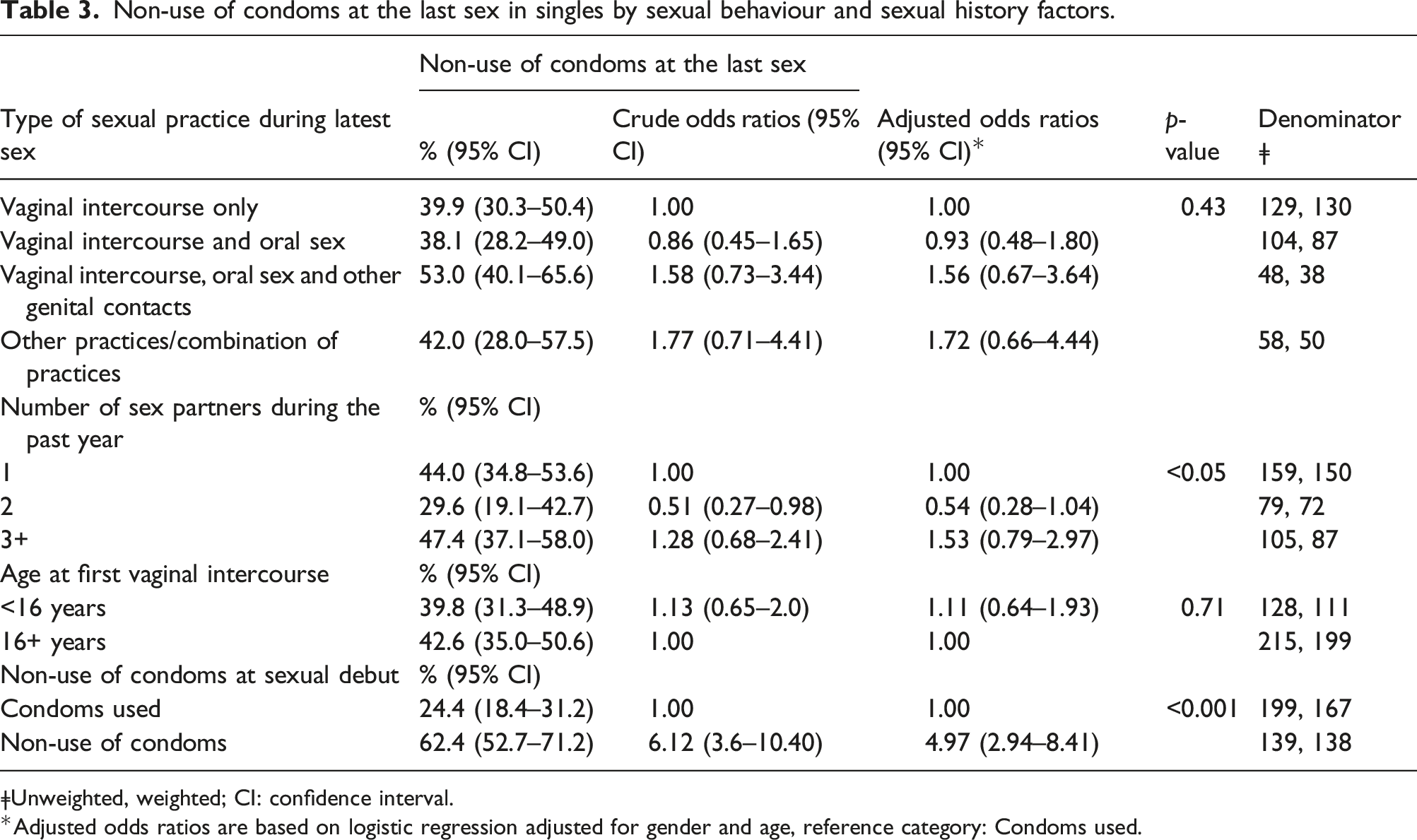
ǂUnweighted, weighted; CI: confidence interval.
*Adjusted odds ratios are based on logistic regression adjusted for gender and age, reference category: Condoms used.
Relational and factors relating to the circumstances of last sex
Non-use of condoms at last sex in singles by relational and factors relating to the circumstances of last sex.
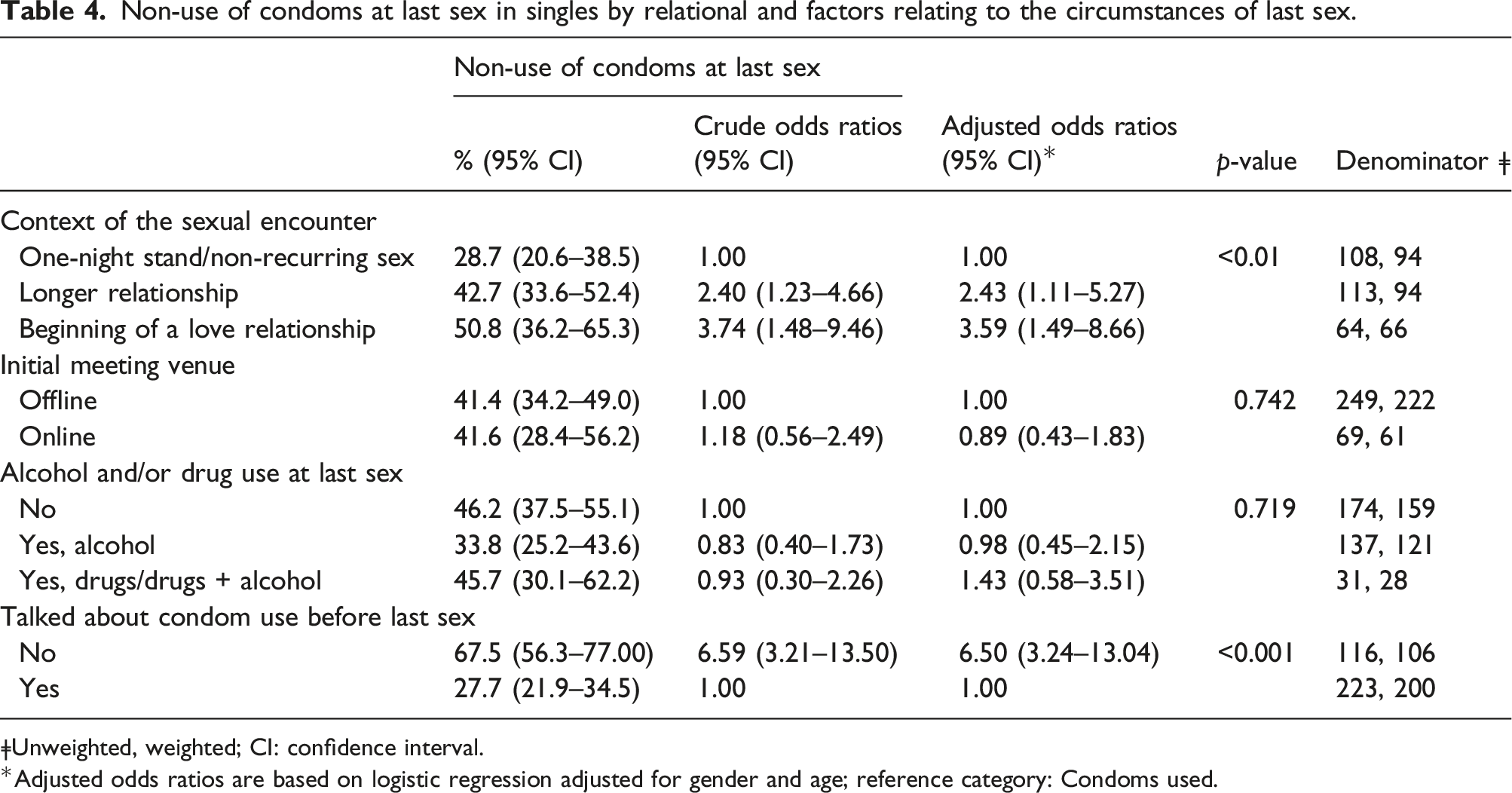
ǂUnweighted, weighted; CI: confidence interval.
*Adjusted odds ratios are based on logistic regression adjusted for gender and age; reference category: Condoms used.
Discussion
The present study analysed data from a survey designed to be broadly representative of the German population to investigate factors associated with reporting non-use of condoms at last sex among heterosexually-active single people in Germany. The prevalence of not using condoms in this population was estimated as over 40%. Although previous studies have used different measures of non-use of condoms, including over longer timeframes and for younger populations, our finding is consistent in that non-use of condoms remains common in Germany.10,18
Non-use of condoms was more prevalent in people in mid- and older life than in younger ages, a finding observed in numerous international studies on general condom-use, too.8,9,11,12,21 The relatively low importance of needing to prevent unintended pregnancies in middle-aged and older adults, 10 as well as less awareness and/or knowledge of STI risks relative to the younger generation, as indicated by another analysis within the GeSiD-study, 22 and reflecting how interventions including STI screening predominantly target younger people, 3 are possible explanations for greater sexual risk-taking in advanced ages at least according to this measure. In large studies from other countries, gender, 23 education11,24 as well as ethnicity in women8,11 were shown to be associated with condom-use. In contrast, in the present sample of specifically heterosexually-active singles’, condom-use at last sex was not found to be associated with gender, education and migration background. Whether these findings reflect the limited statistical power of the present analysis or turn out to be population-specific, should be investigated in future studies.
Non-use of condoms was more likely in the course of longer relationships (“längere Affäre”) or early loving relationships (“beginnende Liebesbeziehung”) than in one-night-stands (“one-night-stand/einmaliger Sex”), indicating that the duration of an acquaintance, as well as perceived closeness, familiarity and commitment may play a role in deciding whether to use condoms, in line with previous research.12,23,24 Not having talked about using condoms before sex was associated with the non-use of condoms. These two aspects may be related with each other considering findings from Peasant et al. 25 who showed that talking about condom use prior to sex seemed to be more difficult with growing familiarity in relationships.
Unlike findings from other studies,5,8,9 age at heterosexual debut did not seem to play a role, but not having used condoms at that time was associated with an increased likelihood for non-use of condoms at last sex. This appeared consistent with findings from other countries5,9 and supports the idea that routinely using condoms from the start of one’s sexual career may promote the adoption of safer sex practices at least in terms of condom use throughout adulthood.26,27
Findings from other countries which identified a large number of sexual partners4–6,28 as a risk factor for the non-use of condoms were replicated in our study. Interestingly, in our study the association between the number of sex partners and the likelihood for non-use of condoms appeared to be nonlinear: Having had two sex partners during the past year was associated with a lower likelihood for the non-use of condoms than having had only one or either three or more sex partners.
Whether participants had engaged in only one or several sexual practices did not affect the likelihood for non-use of condoms in the current study, which stands in contrast to findings by Hill et al., 29 who found that switching practices during a sexual encounter, for example between vaginal intercourse and oral stimulation, was critical for having condomless sex. However, it cannot be gathered from the questions asked about condoms in this study, whether a condom had been used continuously or removed during the sexual act. Further studies should look to ask more detailed questions about condom use in order to help identify and understand potentially risky situations.
Meeting the partner online or offline was not found to be associated with non-use of condoms, indicating that the likelihood for having condomless sex in Germany is not higher in online initiated contacts, in line with findings from Great Britain. 28 A closer look at online venue preferences and personal motivations (seeking casual sex or romantic relationships) might help gain further insights into different patterns of sexual risk taking.28,30 While sex-related alcohol consumption played a role in nearly 40% of the heterosexual singles’ sexual encounters in the present study, there was no association with the non-use of condoms, unlike other studies suggest.7,29
Limitations
Among those participants identified as being single for at least 1 year prior to interview, almost 40% reported sexual activity with someone of the opposite-sex during this timeframe. On the one hand, this means that the majority of singles live a “healthy” lifestyle in terms of STI risk simply by having no sex at all. On the other hand, the statistical power for the study’s examination of those heterosexually-active singles is limited. While we tried to increase the statistical power available, e.g. using only binary categories in our analyses, it is likely that we had limited ability to detect as statistically significant differences that may be of clinical or public health significance. Further analysis on larger samples is needed, enabling a greater granularity, for example by age, type of online meeting venue, and type of drug used. They should also to take account of specific health conditions, in particular having a current or recent STI-diagnosis which has been shown to be associated with condom use 11 but which could not be considered in the present study due to the small number reporting a STI diagnosis (7.4%, n = 24). Furthermore, with survey data like these it is not possible to determine chronology, i.e. whether the diagnosis was before or after last sex.
Findings are limited to the reports about condom-use during a single occasion, namely the last sex, allowing us to identify specific correlates and circumstances related to this particular event. It may be helpful for future studies to consider consistency of condom-use over a longer timeframe to shed further light on the mechanisms underlying risky behaviour. For example, with longer acquaintances, negotiations about condom use may only take place prior to the initial sexual encounter, such that they are not repeated in subsequent sexual encounters with the sex partner. Future studies need to highlight those factors that support ongoing discussion about condoms in relationships with growing familiarity.
Conclusions
Health promotion continues to be needed to promote the importance of condom-use in Germany, especially in the context of sex with a new partner from sexual debut and throughout the life course, regardless of relationship type, age, and relatedly, concerns around pregnancy risk. Improving skills for fear-free and natural communication around condom use and sexual interactions more broadly should be part of interventions promoted through public awareness campaigns and in individual counselling.
Footnotes
Acknowledgements
The authors would like to thank all the participants in this study.
Author contributions
SC conceived the paper, analysed and interpreted the data, wrote and edited the manuscript with further contributions from all authors who reviewed successive drafts, contributed to data interpretation and approved the final version. Statistical analysis was done by SC with support from CW. PB, AD and SM designed and managed the GeSiD study with support from UR (BZgA) and CM as a member of the study’s scientific board. SC, LP and CW contributed in data management. SC is the paper’s guarantor, accepts full responsibility for the work, had access to the data, and controlled the decision to publish.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The study was approved by the ethics committee of the Hamburg Psychotherapy Association (“Hamburger Psychotherapeutenkammer;” reference: 07/2018-PTK-HH).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by the Federal Center for Health Education (BZgA), grant numbers Z2/25.5.2.1/18; Z2/25.5.2.1/20.
