Abstract
Introduction: The COVID-19 pandemic and social distancing measures forced sexual health services to engage with patients remotely. We aimed to understand perceived barriers and facilitators to the provision of digital sexual health services during the first months of the pandemic. Methods: An online survey and qualitative interviews with UK sexual healthcare professionals recruited online and via snowball sampling were conducted in May–July 2020. Results: Amongst 177 respondents (72% female, 86% White, mean age = 46, SD = 9), most utilised telephone and email as their main communication channels; however, their perceived effectiveness varied (94% and 66%, respectively). Most agreed that staff needed additional training (89%), the available technology was not adequate (66%) and health professionals were hesitant to provide online consultations (46%). They had positive attitudes towards digitalisation, improving service quality and cost-effectiveness but were concerned about exacerbating health inequalities. Discussion: The study identifies a need for clear guidelines and training around the use of digital tools as well as a demand for investment in hardware and software required for the provision of remote services. Future research needs to explore the acceptability, safety and effectiveness of various digital tools to narrow health inequalities in sexual health service users.
Keywords
Introduction
Between March and May 2020, a UK nationwide lockdown was put into place to reduce excess hospitalisation of patients due to COVID-19, while most outpatient and primary care services restricted face-to-face access, recording a significant decline in attendance and overall healthcare utilisation.1–2 Patients were advised to use alternative remote channels of communication, in particular telephone or video consultations with a range of tools such as emails, text message applications, digital leaflets and web chats. 3 Such a rapid adaptation of digital technologies during the first lockdown had a significant influence on the delivery of services and community-based programmes, often lacking a regulatory framework. 4 Healthcare professionals had to respond to the rapid provision of innovation to ensure service continuity. However, these were proceeded without contextual guidelines, best clinic practice examples, audits and ongoing evaluations to ensure equitable access and quality of care.
The utilisation of sexual and reproductive health services (SRHS) was also substantially reduced, as demonstrated by an 80% decrease in PEP prescription in a London clinic, 5 a 78% decrease in Madrid, 6 and 66% in Melbourne. 7 This reduction could be associated with a general decrease in sexual activity during this period 8 but also a possibility of constrained access for asymptomatic cases. 9 Public Health England reported an overall 13% reduction in consultations, with a 20% increase in digital consultations during the first lockdown accelerating the provision of digital sexual health services (DSHS). 10 Sexual healthcare professionals (SHPs) were required to utilise digital platforms for remote consultations with little evidence for their effectiveness, safety and acceptability to patients, with some advocating for sexual abstinence. 11 This led to concerns about exacerbating societal health inequalities due to limited access to technology, lower digital literacy and access to private and safe spaces for intimate conversations across patient groups.12–13 Equally, little is known about SHPs’ motivation and capabilities with conducting digital consultations. This study aimed to assess the attitudes of SHPs towards the rapid digitalisation of SRHS in the United Kingdom at the early stage of the COVID-19 pandemic. The objective was to identify the barriers and facilitators for the provision of DSHS to inform service development.
Methods
Design
This was a mixed-methods study incorporating an online cross-sectional survey with follow-up telephone interviews to understand the depth and range of views on the provision of DSHS during the first months of the COVID-19 pandemic. The study was approved by the University of Westminster Research Ethics Committee (ref: ETH1920-0979).
Participants and recruitment
We focussed on health professionals working in SRHS, that is, doctors, nurses and health advisors actively working in clinical practice in the United Kingdom. Between May and July 2020, an online study advert was distributed through Twitter and newsletters of professional organisations relevant to SRHS (i.e. the British Association for Sexual Health and HIV). Tailored invitation emails were also sent out individually to individual members and key sexual health specialists in the United Kingdom with a request to distribute the study advert within their professional networks. Recruitment utilised online snowball and convenience sampling approaches to gathering as many responses as possible. The response rate was not recorded due to the nature of snowball sampling. Participation was voluntary and no incentive was offered. Upon survey completion, participants could provide their contact details to arrange a follow-up interview. Opportunity sampling was obtained by contacting all interested in taking part.
Measurements and procedure
Upon clicking on the study advert, participants were directed to the online Qualtrics survey which consisted of eight questions and four scales. Participants were asked demographic questions (i.e. gender, age, ethnicity, country of professional practice and professional role) and whether their role was affected by the COVID-19 pandemic. Next, they were shown a list of digital and remote communication channels, such as telephone, email, social media, web chat or phone applications, and asked to indicate which they used in contact with patients. Following this, questions explored the perceived effectiveness of these communication channels, using 5 options ranging from ‘very ineffective’ to ‘very effective’. Afterwards, a nine-item scale explored SHPs’ experiences with providing DSHS, with 7-Likert response options ranging from ‘strongly disagree’ to ‘strongly agree’. These items assessed views on staff training, digital equipment and software, DSHS guidelines and access to IT support. An additional nine-item scale explored attitudes towards the rapid digitalisation of services due to COVID-19, assessing perceived quality, safety and confidentiality of DSHS, perceived level of skills and knowledge regarding digital technologies used in SRHS and the potential impact on health inequalities. The survey took approximately 12 min to complete.
The subsequent follow-up interviews used a topic guide to further explore barriers and facilitators to the provision of DSHS during the COVID-19 pandemic (March–June 2020). They aimed to investigate the lived experiences of SHPs, the impact on SRHS and the usage of technology within the context of COVID-19. The interviews were conducted by AL via telephone or Skype lasting approximately 30 min. All were audio-recorded and transcribed verbatim.
Data analysis
Descriptive analysis of qualitative data was undertaken using SPSS. Percentages and simple statistical tests (i.e. mean, median, range and standard deviation) were performed and results were presented graphically using column charts. The perceived effectiveness and ineffectiveness of each communication channel was considered alongside their actual usage. Furthermore, the percentages of SHPs agreeing and disagreeing with the attitudinal and experiential questions were considered.
The qualitative data were analysed thematically which involved familiarisation with the data in the written transcripts and the identification of patterns in participants’ responses, in line with the approach recommended by Braun and Clarke (2006). 14 Microsoft Excel software was used to organise data into themes and subthemes with corresponding quotes. The analysis formulating codes, themes and subthemes was conducted by AL and validated by TN in terms of consistency, coherence and applicability.
Results
Attitudinal survey
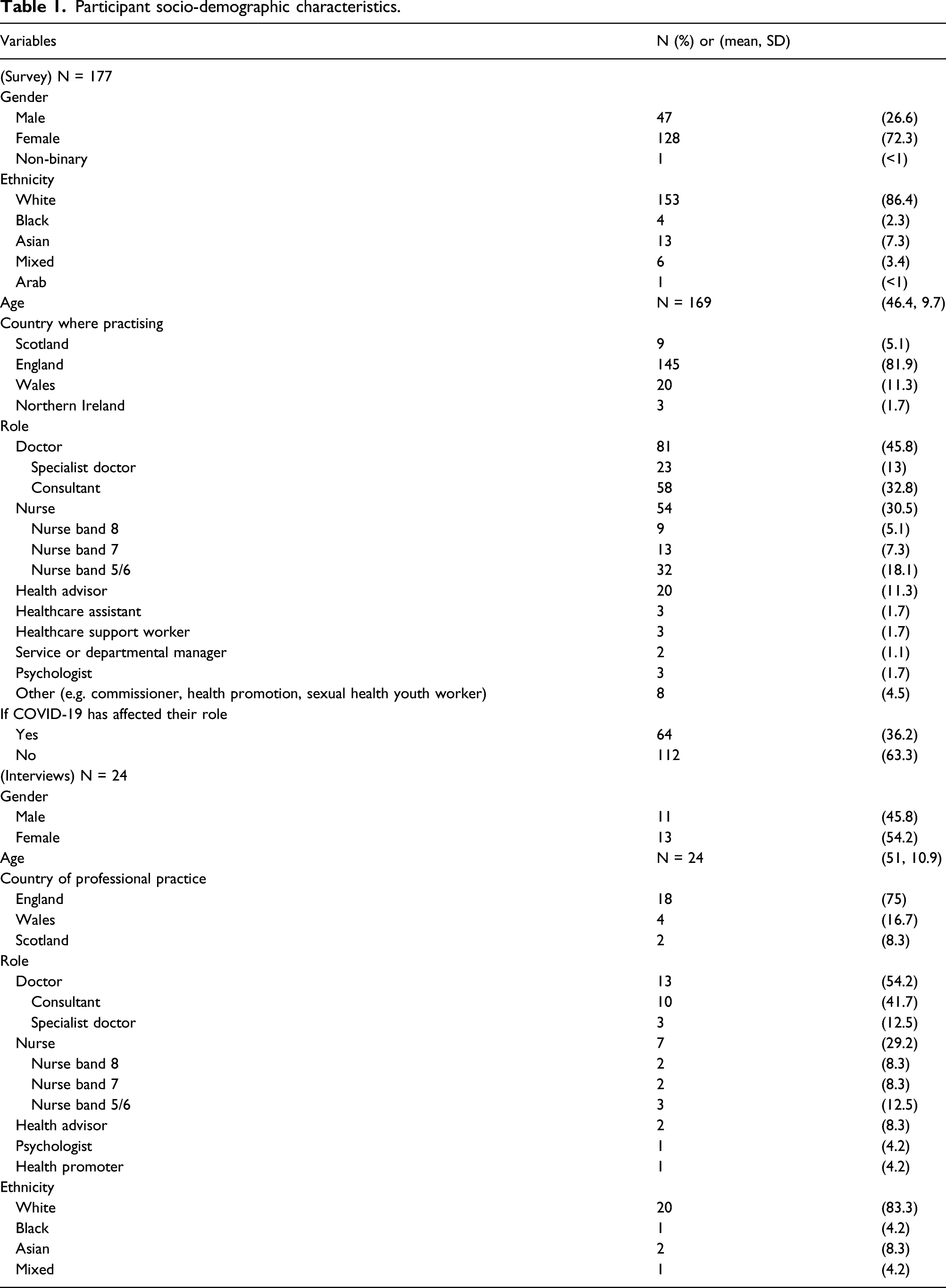
Participant socio-demographic characteristics.
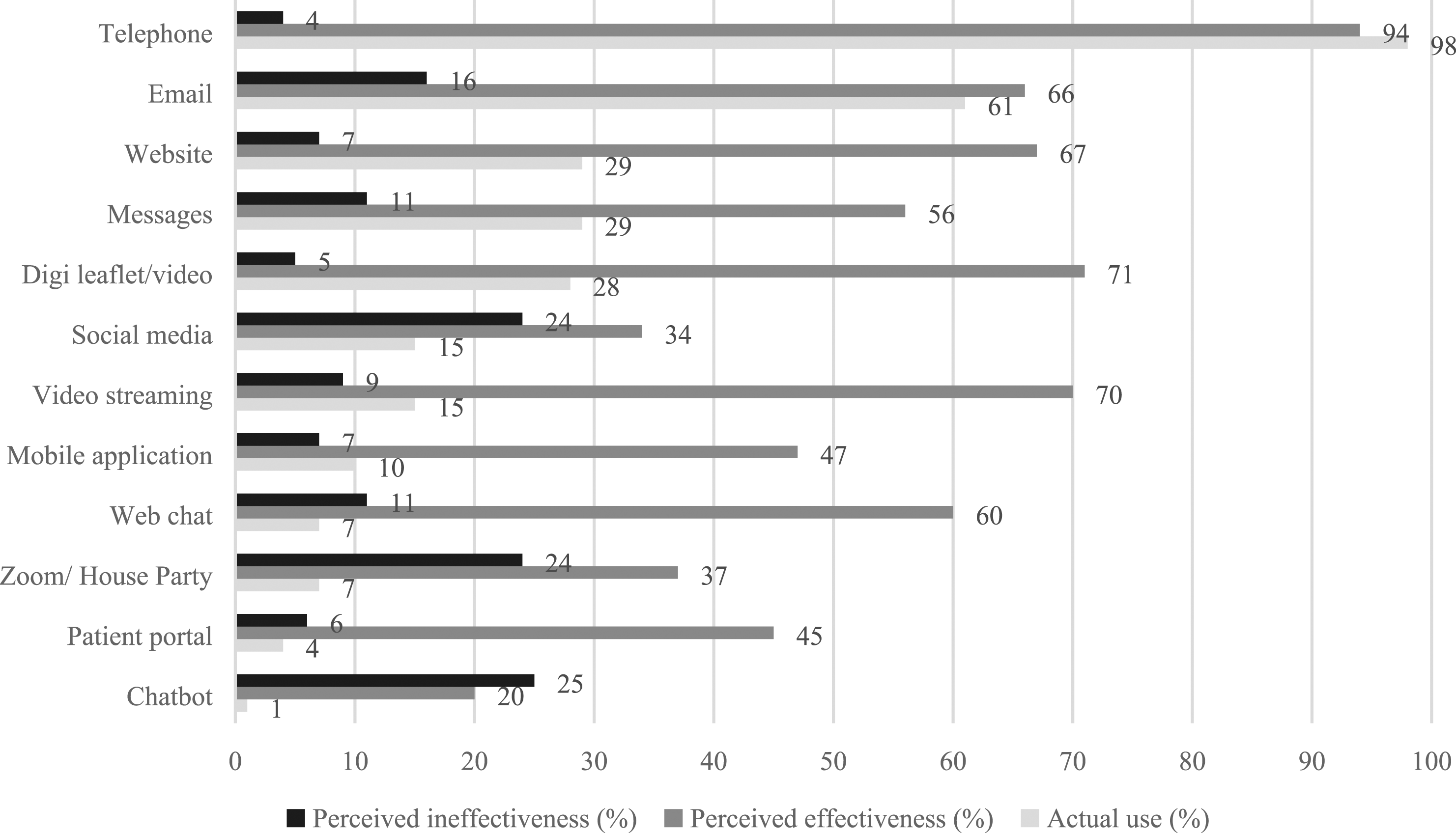
Sexual healthcare professional actual usage, perceived effectiveness and ineffectiveness of different digital communication channels.
As seen in Figure 2, most participants reported the need for staff training (89%) and clearer guidelines (47%) around the use of DSHS. Despite having access to IT support (67%), the majority agreed that their digital equipment was not optimised (62%), with inadequate technology (66%). Around half of SHPs thought that most doctors and nurses were hesitant to provide online consultations (46%), with about a fifth being concerned about patient access to digital services (19%). In general, SHPs had positive attitudes towards the provision of DSHS (69%), with the majority believing that they improved service quality (64%) and cost-effectiveness (70%), and that they were acceptable to service users (81%). However, only half thought DSHS were safe in terms of data security (55%), and a third reported they had the knowledge (29%) and skills (64%) needed to provide DSHS effectively. Just under half were concerned that DSHS may broaden health inequalities (43%). Experiences and attitudes of SHP regarding DSHS in the early stages of the pandemic. SHP: Sexual healthcare professionals; DSHS: digital sexual health services.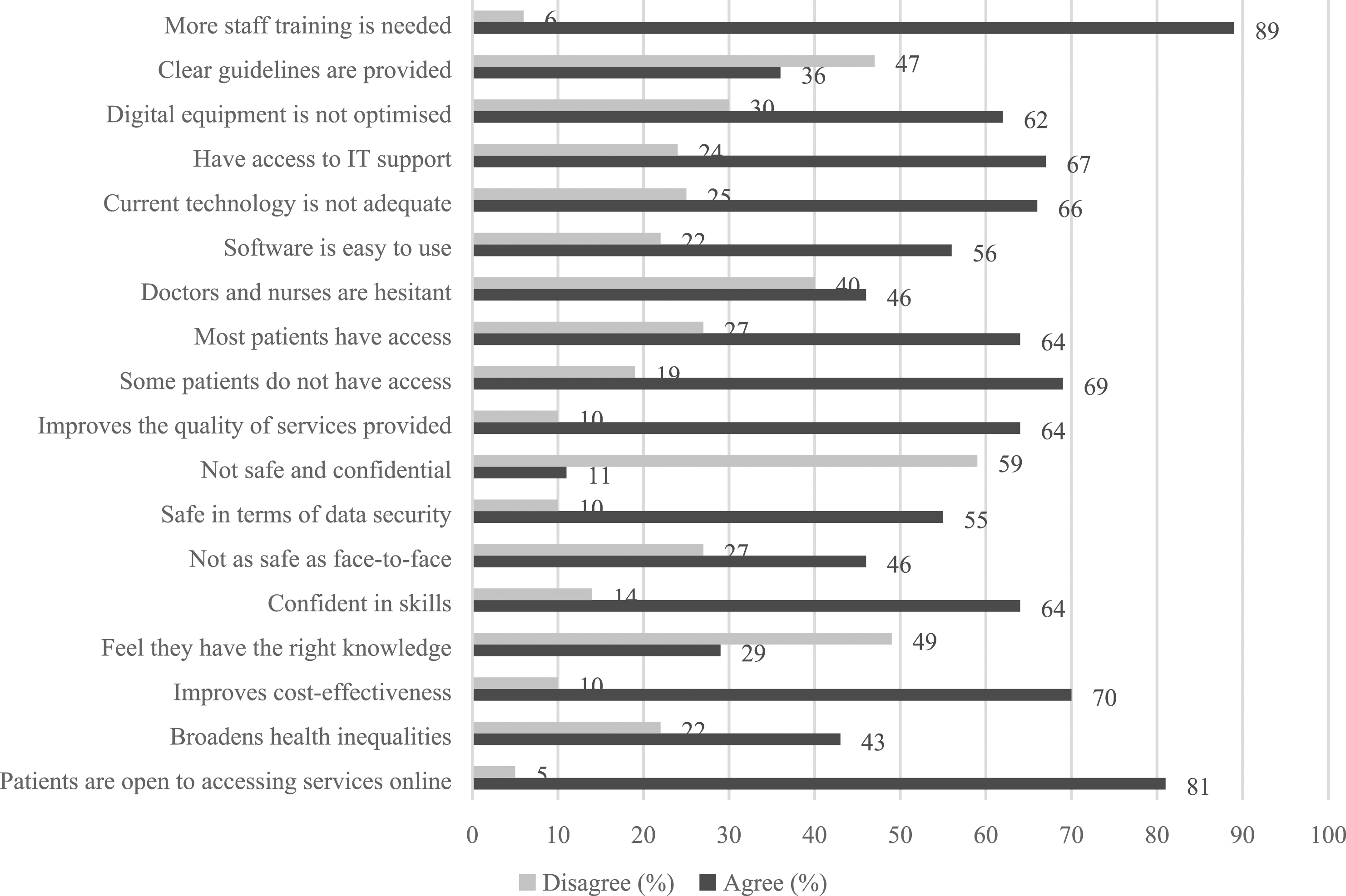
Qualitative interviews
Qualitative themes and exemplar quotes from interviews with SHPs.

HCP: healthcare professional; MSM: men who have sex with men.
COVID-19: Experiences and attitudes regarding service digitalisation
All interviewees reported that COVID-19 instigated almost instantaneous change within their services. They viewed COVID-19 as an opportunity to trial digital technologies that their clinics had been considering before the pandemic. Responses to changes were mostly positive and viewed as an advancement of the services. The pandemic enabled re-evaluation of the utility and usefulness of services that had been mostly offline. Most interviewees remarked that COVID-19 was a catalyst for permanent change. The desire for telemedicine and face-to-face clinics being utilised for varied patient needs was remarked upon because it was seen as a ‘streamlined’ and integrative method of sexual health care. Negative perceptions were viewed particularly concerning the experience of working during COVID-19, a time in which their services had been ‘decimated’ and cut back significantly. Some were concerned about the capacity of digital technologies when services return to pre-pandemic demand.
Barriers: Access, communication and security concerns
Most participants were concerned about patient access to services, disenfranchising certain service users and increasing health inequalities. This pertained notably to the vulnerable, marginalised and minority groups that may not be able to effectively engage with such services due to their inability to use technology, language barriers, lack of safe space for discussions or other insufficient resources. Some SHPs believed that health professionals were not adequately equipped to offer effective online consultations due to inadequate equipment, unstable network connectivity or outdated software. Financial and operational cuts for sexual health were seen as a major barrier to the implementation of DSHS. Sexual healthcare professionals reported communication barriers, such as a reduced ability to form a rapport with patients or to extract sufficiently detailed information such as their sexual health history, via telemedicine. Digital sexual health services were seen as restrictive in providing reassurance and emotional support which are vital for effective and compassionate health care. Participants were concerned about lower disclosure rates, alongside feelings of being less able to pick up visual cues regarding safeguarding and health issues. Sexual healthcare professionals were concerned about confidentiality and data security when using various communication channels, especially during remote working. This was emphasised when describing the handling of patient information and personal details. Sexual healthcare professionals were unsure about maintaining appropriate boundaries with DSHS.
Facilitators: SHP attitudes and maximising patient access and service quality
The digitalisation of the NHS service was seen as a positive advancement, with most SHPs perceiving DSHS as highly acceptable for their patients. They were seen as convenient and potentially reaching populations that experience barriers to physically accessing services. Many felt that patients should be able to access services from home or work, where service users may be more relaxed and open to discussing their health. Sexual healthcare professionals thought that the provision of DSHS before COVID-19 increased the efficiency of their services, through better demand management and online triage systems. Digital sexual health services were seen to facilitate more time with services users presenting with symptoms while providing more patient-centred care and sexual health education. The anonymity, or ‘disembodied voice’, present within a telephone consultation was seen as beneficial to patient disclosure, especially when discussing issues of higher perceived stigma. Sexual healthcare professionals felt that providing a panoply of services would likely suit a large range of patients, having a wider choice of consultation methods to suit different patient needs. Several interviewees also noted they felt a need for the NHS to engage with innovation and advancement to provide services that correspond to the generational and societal norms. Two of the interviewees noted that DSHS increased patients’ responsibility for their health, by providing methods of self-management and additional choices.
Discussion
To our knowledge, it is the first survey examining preparedness for and attitudes towards rapid digitalisation of SRHS in response to the COVID-19 pandemic. It demonstrates positive views on DSHS as well as concerns for safeguarding and increased health inequalities due to limited access to technologies in specific patient groups. Despite the availability of guidelines on the digital transformation of SRHS 15 in January 2020, a substantial proportion of the sample felt that the support for digitalisation was inadequate, expressing a need for additional training and equipment to provide remote services safely and effectively. Digital sexual health services were seen to increase patient access, improve service quality, aiding STI testing uptake, virtual diagnoses and managing demand or clinical workflow. Most SHPs were receptive to the digitalisation of SRHS; however, there was a strong emphasis on narrowing, rather than widening, health inequalities with the help of technology.
The participants identified important barriers for the successful provision of DSHS on both healthcare provider and recipient levels. The implementation of DSHS could be impeded by insufficient resources, notably outdated hardware, software and poor connectivity with patients. Thus, an investment is required to reduce barriers related to technological deficiency and disparity across SHS in various local authorities and simultaneously ensure the effectiveness and safety of DSHS. It is equally important to ensure that the ‘digitally disengaged’ can still access SHS via several other routes in order to ensure that the digital divide is not furthered, thus exacerbating health inequalities. Sexual healthcare professionals felt they had inadequate knowledge and skills regarding digital technologies, that the added digital layer mediates the efficacy of communication and disclosure, and that there is a lack of ethical consideration, each of which potentially impacts digital patient care. This is in line with previous research highlighting the potential harm of DSHS, considering the sensitive nature of sexual health consultations. 16 A systematic review of 12 studies on digital competencies amongst healthcare professionals showed that experiences of technology and attitudes towards innovation have an impact on individual motivation to provide online healthcare services. 17 As such, there is a need for ongoing training, digital education and organisational support to maximise these competencies. Similarly, a qualitative study of 18 healthcare experts in Germany showed that digitalisation of healthcare services was restricted by the absence of interoperability, hesitancy due to insufficient evidence on cost-effectiveness and safety as well as the lack of political will, legislation and financial regulations. 18 There is a possibility that the lack of familiarity with technology, perceived ease of use, computer self-efficacy and objective usability have influenced hesitancy towards some of the communication channels for sexual health advice.19,20 The perceived ineffectiveness of specific platforms for doctor–patient communications could be driven by the lack of familiarity; hence, training aimed at building skills and IT proficiency may alter these perceptions. Our present study identified financial cuts as an important obstacle for healthcare digitalisation. Thus, the transformation needs to be standardised and optimised by self-regulatory bodies overlooking the developmental process and providing incentives for digital solutions. More research is needed to examine the equity, acceptability, reach and cost-effectiveness of digital healthcare services to inform stakeholders about the value of innovation.
Although the mixed-methods design implemented in this study provides a more in-depth understanding of views on SHS digitalisation, several methodological issues exist. The views expressed in this study represent various perspectives on the use of telemedicine in the early stage of the COVID-19 pandemic, and these were likely evolving in line with the investment and training offered to sexual health staff. Due to opportunity sampling methods, an uneven distribution between socio-demographic categories within both datasets occurred. Our snowball sampling recruitment strategy may be associated with self-selection bias when health professionals with well-established views on telemedicine were more likely to participate. There were no participants from Northern Ireland, and there were fewer nurses than can be represented within the national workforce as a whole. Within both arms of the study, there was a skew towards consultants working in England and may not be representative of all perspectives within sexual health workers. There is no standardised questionnaire on attitudes towards digitalisation, and the Cronbach alpha coefficient relating to the survey was only at an acceptable level, indicating lower internal consistency of the measures. Therefore, the mean scores obtained from the Likert scales used to measure SHP attitudes and experiences may not be fully representative of the variables, limiting inferential statistics.
To conclude, the focus should be on a digitally enabled healthcare system, wherein a variety of communication methods are available to suit the patients’ needs, referring asymptomatic and non-complex patients to DSHS, and symptomatic, complex or vulnerable patients to in-clinic services. Digital technology allows for more patient-centred services with specific information being tailored to patients’ skills and characteristics. Thus, national guidelines on digital sexual health should be updated to reflect changes in technologies, user acceptability and various layers of barriers. Future research should explore the motivations and skills for DSHS in order to monitor any provider-level barriers to the provision. There is a need to understand whether there are discrepancies between specific professional roles or UK regions regarding remote services provision. This study offers insights into the baseline acceptability rates of various digital channels and platforms for online engagement with patients. Such a survey could be repeated in the future to assess the change in attitudes towards digital sexual health services and a potential reduction or increase of barriers.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Author contribution
All authors designed the study, contributed to the analyses and the interpretation of findings as well as the drafting of the manuscript and approved the final version of the manuscript. AL and TN collected and analysed the datasets.
Ethics approval
University of Westminster Research Ethics Committee (ref: ETH1920-0979).
