Abstract
The mechanical integrity of polymethyl methacrylate (PMMA) bone cement is crucial for the long-term fixation of orthopaedic implants, yet it is often compromised by porosity introduced during mixing. This study investigates the influence of mixing technique and vacuum level on the structural and mechanical properties of PMMA bone cement. Three clinically relevant mixing approaches, open bowl, vacuum bowl and vacuum cartridge were evaluated at vacuum levels ranging from 0 to 650 mm Hg. Cylindrical PMMA specimens were produced and their porosity assessed using high-resolution micro-computed tomography (µCT), with corresponding mechanical properties determined through compressive testing in accordance with ISO 5833:2002. µCT analysis revealed significant reductions in porosity at higher vacuum levels, particularly with the vacuum cartridge system. A strong and significant negative correlation was observed between compressive strength and porosity (R2 = 0.864), while specimen mass showed no predictive value for mechanical performance. Although vacuum mixing reduced porosity, no consistent changes in Young’s modulus were detected across the mixing groups. These findings emphasise the importance of porosity control in bone cement preparation and highlight the limitations of current ISO standards. The study advocates for improved testing protocols that more accurately reflect clinical conditions to enhance the predictive value of in vitro assessments of PMMA cement performance.
Keywords
Introduction
Polymethyl methacrylate (PMMA) bone cement is widely used in orthopaedic surgery due to its high compressive strength, ease of handling and long-term clinical reliability.1–3 In total hip arthroplasty, for instance, liquid monomer methyl methacrylate (MMA) is mixed with powdered PMMA, initiating a polymerisation reaction that forms a viscous slurry. During this handling phase, the PMMA mix is introduced into the prepared femoral canal prior to insertion of the femoral stem. As the mix rapidly hardens into a solid polymer, it securely anchors the implant in place. These mixing and deposition stages are typically performed using disposable medical devices, which are designed to control cement processing conditions and optimise mechanical performance and delivery efficacy.
Despite ongoing advancements in joint replacement implants, the mechanical properties and effectiveness of the anchoring PMMA cement are often compromised by defects within the mix.3–12 Internal voids, or pores, reduce cement performance and reliability over time. Throughout the lifecycle of an implant, it is subjected to compressive and cyclic stresses, which contribute to progressive mechanical degradation of the PMMA cement.5,9,10,13
Multiple studies have demonstrated that pores within PMMA serve as preferred sites for fracture origin,5,10–12,14–16 with the majority of fractures originating from these voids.14,17,18 This increased potential for fractures is particularly concerning as it increases the risk of implant aseptic loosening, the leading cause of revision surgeries,19,20 accounting for ∼35% of all cases. 21 Fractures occurring in close proximity to the implant-cement interface weaken adhesion, eventually compromising the mechanical fixation between them.22,23 When this occurs, the implant becomes unsafe and revision surgery is required.22,24,25 Consequently, there is a consensus that reducing porosity in bone cement will result in longer-lasting and more durable joint replacements.3,9,12,26 However, achieving this in practice depends strongly on how cement is mixed and handled clinically.
Cement porosity arises from the presence of small voids in the solidified polymer, which are categorised based on their size: macropores (≥1 mm) and micropores (0.1–1 mm). 4 They typically form during the mixing stage, where different processes and techniques influence the resultant porosity of the solidified cement. During the incorporation of the PMMA powder with liquid monomer, air often becomes trapped within the mixture, creating pores.4,8,14,27,28 These pores act as local stress concentrators that promote crack initiation and growth under repeated physiological loading.5,12,27 If the mixing is performed under uncontrolled conditions, especially without a vacuum, larger amounts of air are likely to be entrapped into the cement. 4 Furthermore, inconsistent and inadequate mixing can lead to uneven distribution and incomplete polymerisation between the polymer and liquid monomer, resulting in greater pore formation.12,28–30 Accordingly, in addition to bulk mechanical properties, pore distribution particularly near the implant interface, is critical for prosthesis longevity. This highlights the need to better characterise how clinically relevant mixing conditions influence internal pore structure.
To address the issue of porosity in PMMA bone cement, various mixing methodologies have been developed. Techniques that combine vacuums with a mechanical rotating axis have proven particularly effective.3,4,7–10,29,31,32 Research indicates that using a vacuum can reduce overall porosity to less than 5%, 4 compared to porosity levels of 5%–10% typically seen with open bowl mixing in uncontrolled settings.4,12 Modern mixing devices have advanced to feature integrated mixing and delivery systems, designed to prevent the cement from being exposed to atmospheric conditions during and in between the mixing and injection stages. These devices are primarily categorised into two types: bowl mixing systems and cartridge (syringe) mixing systems.
Initially, both approaches operate similarly. The PMMA cement components are added, the device is closed and a vacuum is then applied. The vacuum cartridge system uses a masher-style mixer, while the vacuum bowl uses a rotating paddle. Following mixing, the vacuum cartridge device is configured according to manufacturer instructions for delivery, typically involving the removal of the mixing handle, attachment to a delivery gun, and the addition of a delivery nozzle. In contrast, with the vacuum bowl system, the cement is transferred from the bowl to a delivery device using a spatula. Given these large variations in preparation techniques, it is likely the resulting cements will exhibit distinct structural and mechanical characteristics. However, direct comparisons of these systems using quantitative 3D porosity assessment are limited.
ISO 5833:2002 standardises the preparation and the mechanical testing of acrylic bone cements, providing guidelines on the mixing, moulding and evaluating compressive and flexural properties. Adherence to ISO 5833:2002 is crucial for standardising research in this field, allowing for credible and comparable assessments of bone cement mechanical performance and iterative improvements.
While traditional methods such as radiography and SEM have been used to estimate porosity,3,6–9,12,33 they provide only limited two-dimensional information and are insufficient for thoroughly assessing the 3D morphology and volumetric porosity. The two-dimensional images produced from these methods overlook the irregular 3D structure of pores, leading to inaccurate porosity volume measurements. Additionally, cross-sectional analysis assumes homogeneity across the entire sample, but studies have demonstrated that the distribution of porosity is affected by mixing techniques and varying distribution significantly affects specimen strength.5,6,34 Therefore, this assumption of homogeneity undermines the validity of conclusions about the overall impact of pores.
Among the few studies that have employed 3D scanning techniques for porosity analysis, Cox et al. 35 investigated the use of micro-computed tomography (micro-CT) compared with traditional methods. Their work demonstrated CT scanning as a superior approach for measuring porosity, particularly when non-destructively analysing the interior of specimens, as it better identifies bulk porosity. Moreover, 3D scanning allows for detailed modelling of internal pores, providing precise evaluations of pore size and distribution, which is especially valuable for analysing non-homogeneous specimens. Despite its advantages, few studies have used micro-CT to systematically compare different mixing methods in combination with standardised mechanical tests. As a result, the relationship between mixing technique, 3D pore architecture, and mechanical performance remains insufficiently resolved.
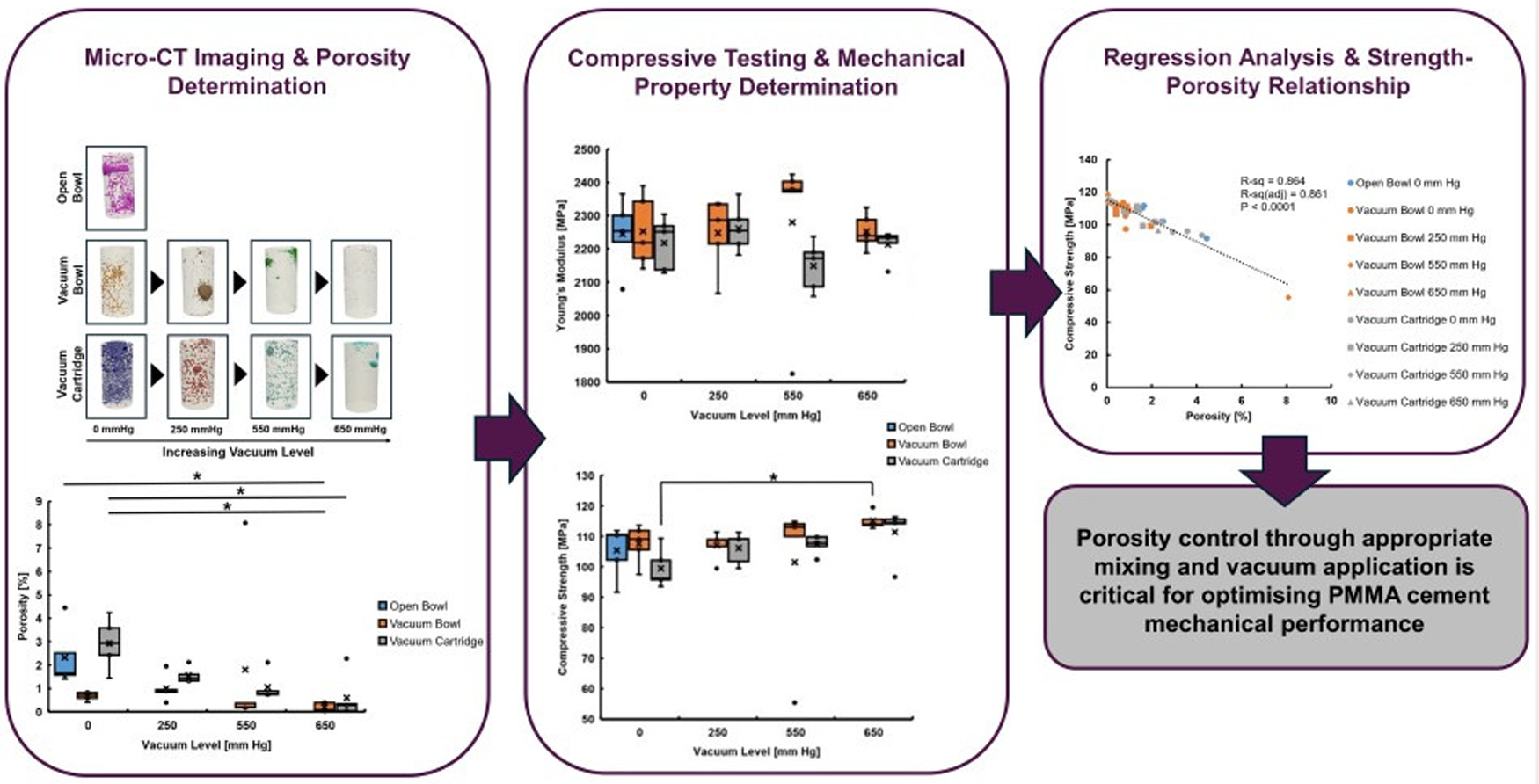
The objective of his study was to investigate how different mixing techniques and vacuum levels affect the internal porosity and mechanical properties of PMMA bone cement. By combining micro-CT imaging with standardised ISO 5833:2002 mechanical testing, this work provides a comprehensive assessment of the relationship between mixing conditions, pore structure and compressive performance. This approach addresses a key gap in the literature by linking 3D porosity characterisation with clinically relevant cement preparation methods.
Methodology
Cement mixing and test specimen production
Batches of PMMA bone cement were prepared by mixing individual 40 g packs of PALACOS® MV (Heraeus Medical, Wehrheim, Germany). The mixing methods and vacuum levels evaluated in this study are summarised in Table 1. Open bowl (Open Bowl and Spatula, Summit Medical Ltd, Produce Code: B710), vacuum bowl (HIVAC™ BOWL, Summit Medical Ltd, Product Code: B713) and vacuum cartridge (HIVAC™ 7, Summit Medical Ltd, UK. Product Code: C701) devices were investigated. The specified range of vacuum levels (0–650 mm Hg) was chosen to reflect the recommended production levels for these devices. An inline manometer was used to monitor and maintain the target vacuum levels (Digitron 2022P 0–2 bar Manometer).
The mixing methods and vacuum levels tested in this study.

For delivery, cement from both bowl devices was transferred to a cartridge syringe (Summit Medical Ltd, UK. Product Code: C701)) fitted with a 6.35 mm nozzle (Summit Medical Ltd, UK, Product Code: 414705) and a ratchet delivery gun (Summit Medical Ltd, UK, Product Code: H759). The vacuum cartridge device allowed for direct attachment of the nozzle and ratchet gun.
Cement produced by each mixing method was dispensed into 5 Ø6mm × 12 mm cavities within moulds, following ISO 5833:2002 specifications. The moulds were manufactured from polyoxymethylene acetal (Delrin®), which provides high dimensional stability and allows precise machining of the specified geometry, as no material specification was given in the standard. Ambient room temperature during cement curing was monitored using a thermometer (Hanna Instruments Woonsocket RI thermometer, Bedfordshire, UK) and maintained between 19°C and 23°C, consistent with typical operating theatre conditions and cement components were preconditioned to this temperature range for at least 4 h prior to use. The samples were allowed to cure for 24 h prior to removal from the mould. This process produced 5 Ø6mm × 12 mm PMMA samples per mixing test group.
Structural properties
Mass measurements
The mass of each PMMA specimen was measured using an electronic balance (Mettler XP205, METTLER TOLEDO, Switzerland). Prior to weighing, samples were acclimatised in open containers at laboratory conditions for 48 h. The lab conditions were maintained at a humidity of 52.5% (±1%) and a temperature of 21.2°C (±1 °C) during both the acclimatisation period and the weighing process.
Each specimen was weighed five times to calculate its mean mass. The mean masses of samples within each test group were then used to determine the final mean mass for each group.
Porosity measurements
All PMMA samples were scanned using a micro-CT scanner (HR-pQCT, XtremeCT, Scanco Medical AG, Switzerland) at 82 μm isotropic voxel size (900 μA, 60 kVp, 300 ms exposure). Scans were analysed using Simpleware ScanIP (2022, Synopsis, USA).
For sample porosity analysis in Simpleware ScanIP, a similar methodology to that established by Cox et al. 35 was used. Sample segmentation was performed using a consistent greyscale threshold across all scans. A region of interest (ROI) was defined for each sample based on the known dimensions of the cylindrical specimens. Voxels within the ROI with greyscale values above the threshold were classified as cement, while those below the threshold were identified as pores. Pore and cement volumes were quantified from voxel counts and known scan resolution. The three-dimensional distribution of pores was visualised using Simpleware ScanIP, with representative examples from each test group shown in Figure 1. Porosity percentage was calculated as the ratio of pore volume to total sample volume.
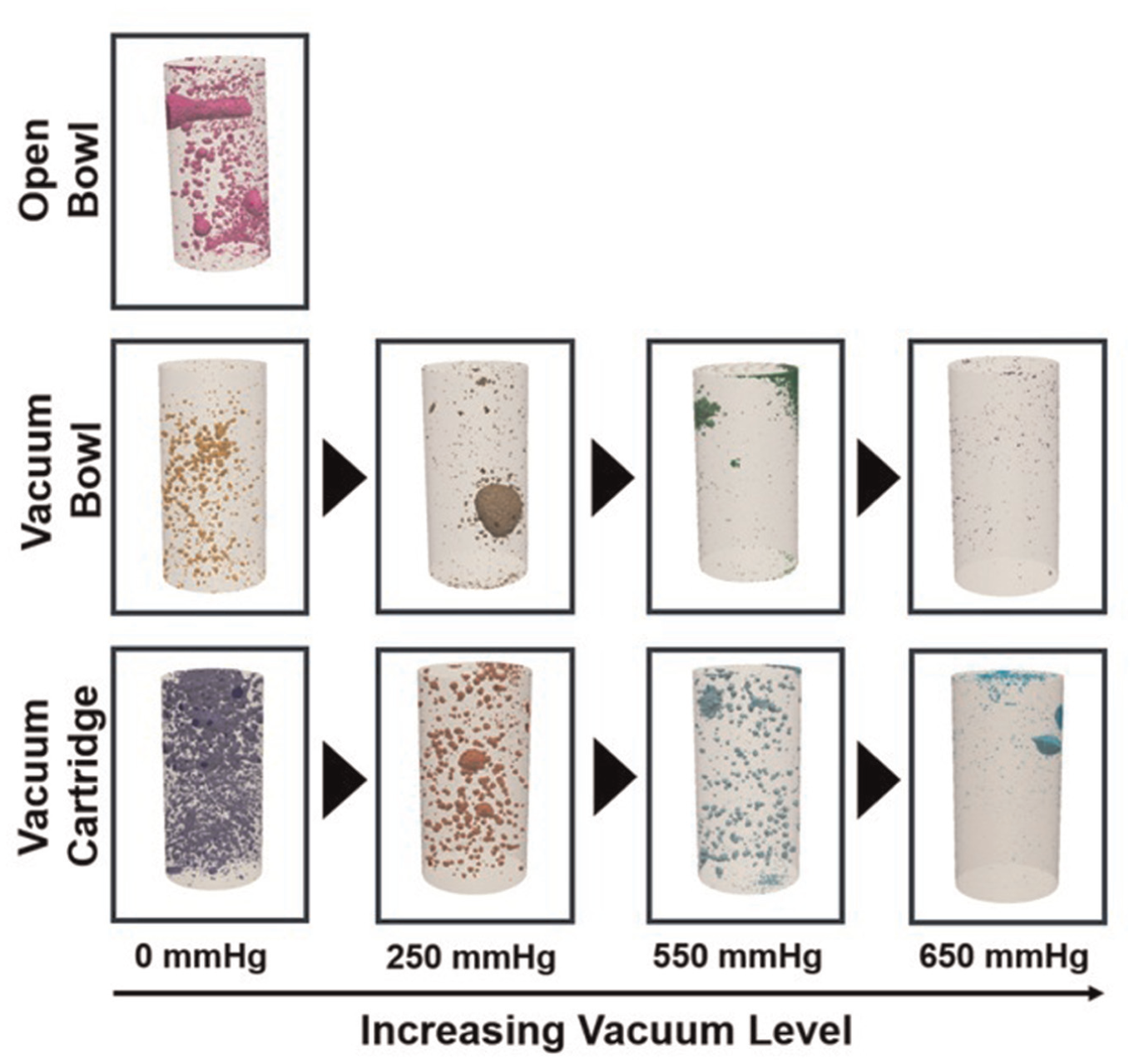
3D outputs from Simpleware ScanIP showing pore definition and distribution for a representative bone cement sample from each test group.
Mechanical properties
Compressive testing of the PMMA specimens was conducted according to ISO 5833:2002 guidance. Tests were performed using a materials testing machine (Instron 3366 fitted with a 10 kN load cell, Buckinghamshire, UK). Specimens were subjected to compression at a displacement rate of 20 mm/s until fracture occurred.
According to ISO 5833:2002, the compressive strength is calculated using either the load required to cause fracture, the 2% offset load or the upper yield-point load, whichever is observed first. In all cases, the 2% offset load occurred first and was therefore used.
The loading data was processed using MATLAB (v2023a, MathWorks), converting force-displacement data into stress-strain data, using the known sample cross-sectional area. A bespoke code was used to determine the 2% offset load values for compressive strength and to calculate Young’s modulus, with a model fit of R2 > 0.99 in all instances.
Statistical analysis
IBM SPSS Statistics 26 was used to perform between-group statistical analyses. Data normality was assessed using the Shapiro–Wilk test. Where normality assumptions were violated, non-parametric tests were applied. The Kruskal–Wallis test was used to compare multiple groups, with post-hoc pairwise comparisons performed using the Mann–Whitney U test with the Bonferroni correction for multiple tests. A p-value of <0.05 was considered to be statistically significant.
Single and multiple linear regression analyses were performed to examine correlations between the physical and mechanical properties of PMMA specimen. Again, a p-value of <0.05 was considered to be significant.
Results
Structural properties
Significant differences were found to occur for specimen mass between the following mixing groups: Vacuum Bowl 0 mm Hg versus Vacuum Cartridge 0 mm Hg, Vacuum Bowl 0 mm Hg versus Vacuum Cartridge 250 mm Hg, Vacuum Cartridge 0 mm Hg versus Vacuum Bowl 650 mm Hg and Vacuum Cartridge 250 mm Hg versus Vacuum Bowl 650 mm Hg (Figure 2(a)). Outliers were observed in five of the nine groups investigated (Open Bowl 0 mm Hg, Vacuum Bowl 0 mm Hg, Vacuum Cartridge 250 mm Hg, Vacuum Bowl 550 mm Hg and Vacuum Cartridge 550 mm Hg).
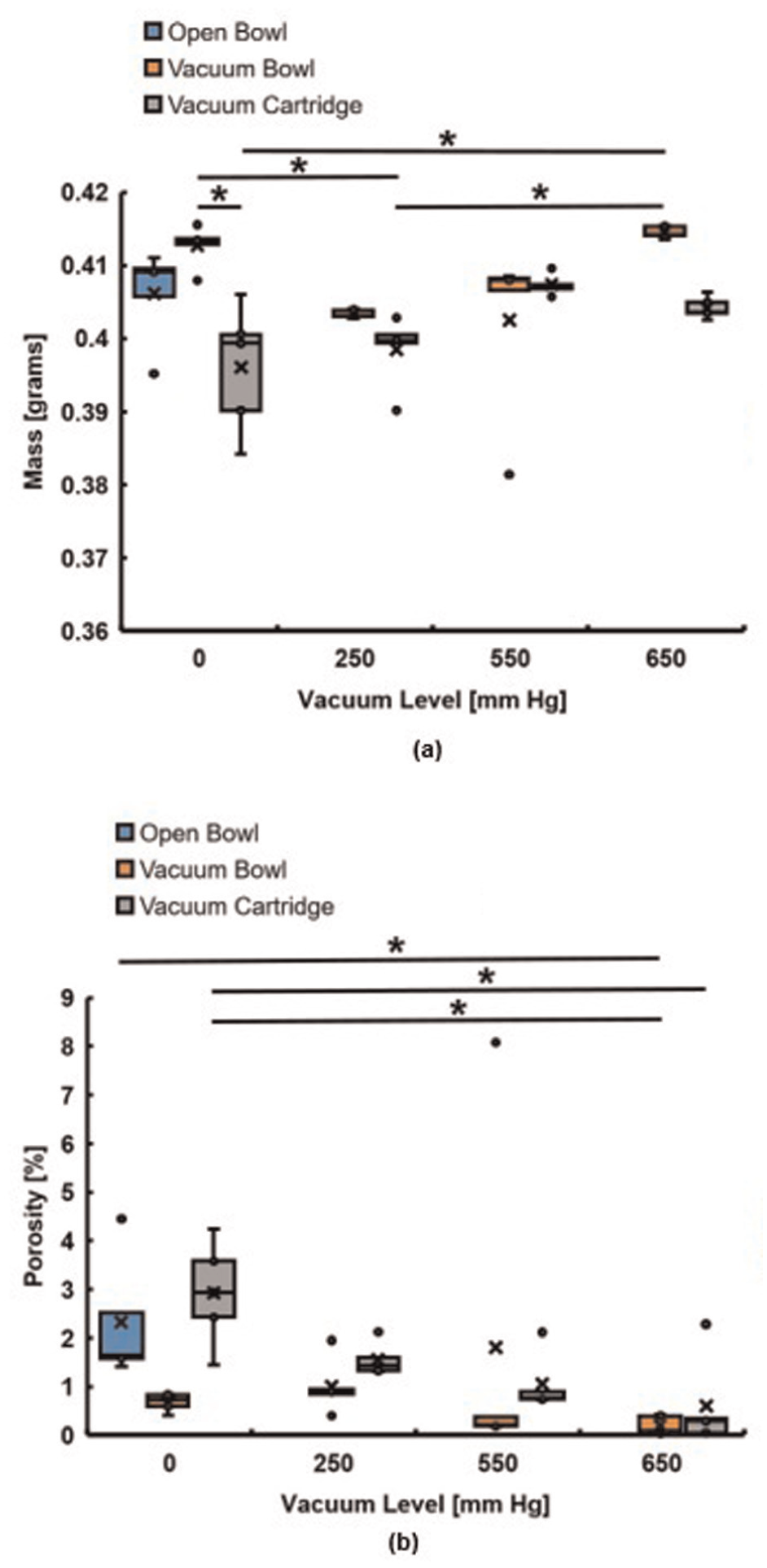
Box and whisker plots of the structural properties of PMMA cement specimens produced using the indicated mixing methods and vacuum levels (n = 5 for each group): (a) mass and (b) porosity measurements. Mean and outlier values are denoted by x- and dot symbols respectively. *Indicates significant difference (p < 0.05, Kruskal-Wallace test followed by Mann-Whitney U post-hoc analysis).
Significant differences were found to occur for specimen porosity between the following mixing groups: Open Bowl 0 mm Hg versus Vacuum Bowl 650 mm Hg, Vacuum Bowl 0 mm Hg versus Vacuum Cartridge 650 mm Hg and Vacuum Bowl 0 mm Hg versus Vacuum Bowl 650 mm Hg (Figure 2(b)). Outliers were again present, this time in six of the nine groups (Open Bowl 0 mm Hg, Vacuum Bowl 250 mm Hg, Vacuum Cartridge 250 mm Hg, Vacuum Bowl 550 mm Hg, Vacuum Cartridge 550 mm Hg and Vacuum Cartridge 650 mm Hg). The greatest outlier was a porosity of 8.2% in the Vacuum Bowl 550 mm Hg group.
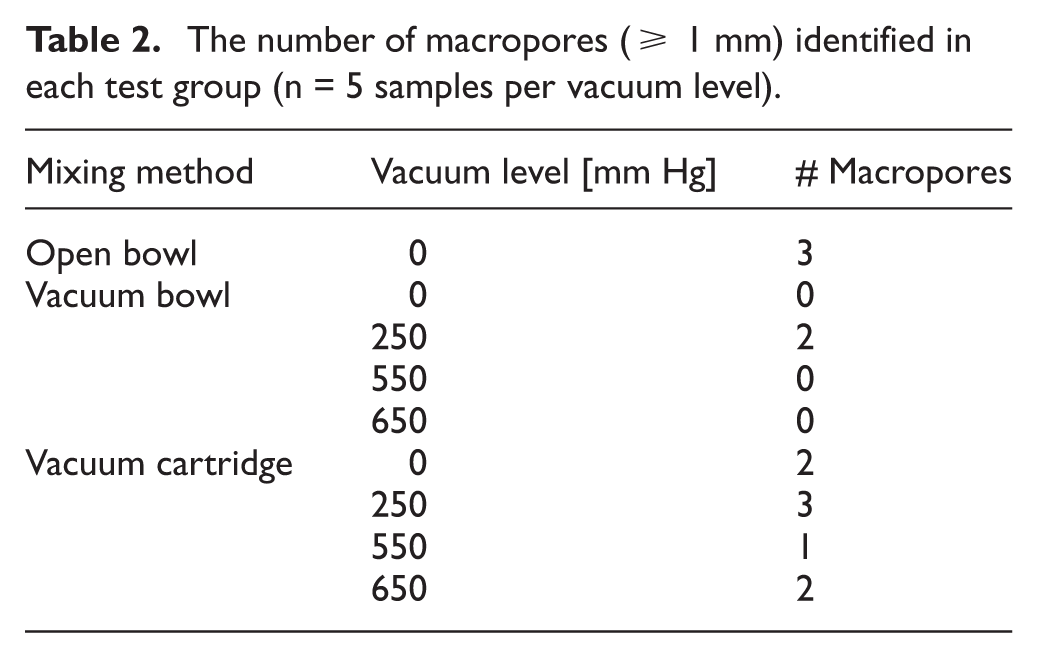
The number of macropores (≥1 mm) identified per group are shown in Table 2. Fewer macropores were observed in the open-bowl mixing group (2 in 20 samples) compared to the vacuum cartridge group (8 in 20 samples).
The number of macropores (≥ 1 mm) identified in each test group (n = 5 samples per vacuum level).
Mechanical properties
For Young’s modulus, no significant differences were detected between any of the mixing groups (Figure 3(a)). Outliers were present in the Open Bowl 0 mm Hg, Vacuum Bowl 550 mm Hg and Vacuum Cartridge 650 mm Hg groups.
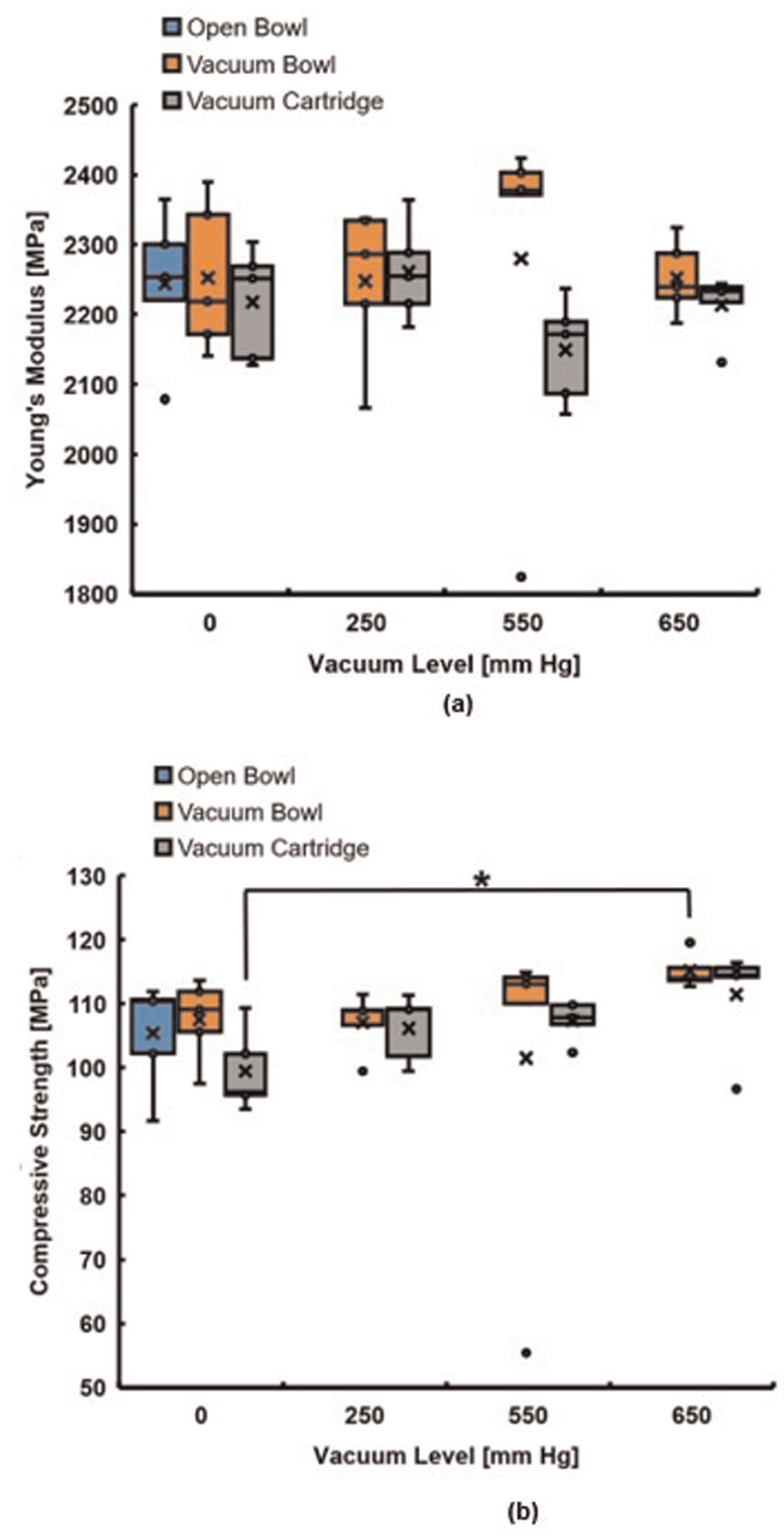
Box and whisker plots of the mechanical properties of PMMA cement specimens produced using the indicated mixing methods and vacuum levels (n = 5 for each group): (a) Young’s modulus and (b) compressive strength measurements. Mean values and outliers are denoted by x- and dot symbols respectively. *Indicates significant difference (p < 0.05, Kruskal-Wallace test followed by Mann-Whitney U post-hoc analysis).
For compressive strength, a significant difference was identified between the Vacuum Cartridge 0 mm Hg and Vacuum Bowl 650 mm Hg groups, but no differences were found among the remaining groups. Outliers were observed in five groups (Vacuum Bowl 250 mm Hg, Vacuum Bowl 550 mm Hg, Vacuum Cartridge 550 mm Hg, Vacuum Bowl 650 mm Hg and Vacuum Cartridge 650 mm Hg).
Regression analysis
Using simple regression analysis, the only strong and significant correlation (R2 = 0.864, p < 0.05) was between compressive strength and porosity (Figure 4). All other correlations examined (Young’s modulus vs porosity, compressive strength vs mass, and Young’s modulus vs mass) were also significant (p < 0.05) but weak (R2 < 0.5).
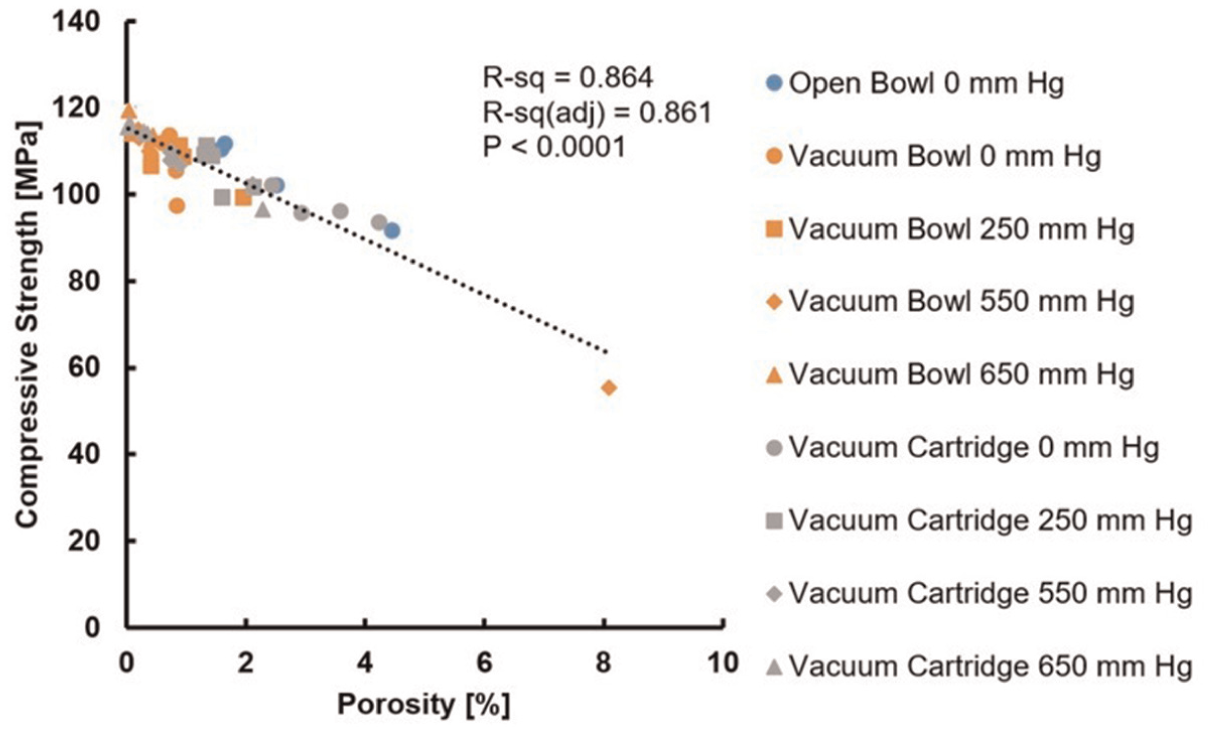
Plot of compressive strength versus porosity for all the specimens investigated in all test groups. A regression analysis demonstrated a strong and significant correlation.
When both porosity and mass were used as predictors in a multiple regression model, porosity was a significant predictor of Young’s modulus and compressive strength (p < 0.05 in both cases), whereas mass was not (p > 0.05 in both cases).
Discussion
Polymethyl methacrylate bone cement is commonly used as an interface substrate to fixate orthopaedic implants such as joint replacements to host bone. However, the cement can be susceptible to mechanical degradation, particularly fracture, due to void formation during the mixing process. These defects can compromise long-term fixation and contribute to aseptic loosening and failure of implants.36,37 This study aimed to determine the effects of different mixing methods and vacuum levels on the structural and mechanical properties of PMMA bone cement.
Forty-four out of the 45 PMMA specimens produced using the open bowl, vacuum bowl and vacuum cartridge mixing approaches had porosities of <5%. The remaining specimen produced in the Vacuum Bowl 550 mm Hg group had a porosity of ∼8%. It has been suggested that mixing without a vacuum can lead to porosities as high as 10%. 4 The lower values observed in this study indicate that our open bowl method was either performed particularly carefully or benefitted from the standardised delivery approach, which minimised additional air entrapment.
Vacuum bowl mixing was found to produce PMMA specimens of significantly higher mass than the vacuum cartridge approach when no vacuum was applied. However, this effect was not consistent across other vacuum levels, suggesting no independent effect of mixing method or vacuum alone on specimen mass (Figure 2(a)). Although higher vacuum levels would be expected to increase mass by removing air, no statistically significant intra-device differences were observed.
The porosity analysis presented in Figure 2(b) indicates that while maximum vacuum levels resulted in significantly lower porosity compared to atmospheric mixing, the reduction did not follow a consistent linear pattern across all intermediate levels. A significant difference was found between 0 and 650 mm Hg in the Vacuum Cartridge groups. However, notable variance and outliers in several groups likely reduced the ability to detect consistent statistical differences at the intermediate stages (Figure 2(a) and (b)). These results suggest that high vacuum levels are required to effectively reduce porosity, but the relationship is nonlinear. As demonstrated in the literature,7,10 the reduction in porosity is not solely dependent on vacuum pressure but is mediated by device-specific factors, including paddle geometry and the rheological behaviour of the cement during mixing.
Mechanical testing revealed few significant differences between mixing methods and vacuum levels. Young’s modulus showed no group differences (Figure 3(a)), while compressive strength differed only between Vacuum Cartridge 0 mm Hg and Vacuum Bowl 650 mm Hg (Figure 3(b)). Although there was a trend towards higher compressive strength with increasing vacuum, particularly in the cartridge system, statistical evidence was limited. This may be explained by the relatively small sample size (n = 5) and intrinsic variability in PMMA preparation and curing. Nevertheless, all specimens exceeded the ISO 5833:2002 minimum compressive strength threshold of 70 MPa, confirming clinical relevance.
Regression analysis showed that specimen mass was not a significant predictor of mechanical properties. In contrast, porosity quantified via µCT strongly correlated with compressive strength (R2 = 0.864), even with the presence of outliers (Figure 4). This suggests that internal void fraction, rather than bulk material quantity, is the dominant factor controlling strength. Young’s modulus did not show a similar correlation with porosity. We hypothesise that the modulus remained consistent because it is derived from the material’s elastic region and therefore is less sensitive to localised defects than ultimate strength. As described in the literature,27,28 pores act as stress concentrators that facilitate crack nucleation, this predominantly determines the point of failure (from compressive stress) rather than the material’s initial elastic behaviour (from its Young’s Modulus).
Prior investigations have used radiography,6,8 electron microscopy3,9,12 or densitometry 32 to determine the porosity of PMMA bone cement. To improve accuracy and obtain three-dimensional data, this study employed µCT scanning and then compared CT-derived porosity to measurements obtained via specimen mass measurements. No correlation was observed between CT-measured porosity and the weight-based method. This discrepancy largely arises because the CT analysis employed a precise cylindrical region of interest similar to the approach of Cox et al., 35 to exclude rough edges, minor surface deviations and standardise each sample’s shape. By contrast, the weight-based technique included all extraneous material or “flash” at the sample ends, effectively inflating the measured mass without reflecting internal void volume. Consequently, regression analysis revealed that CT-determined porosity was a significant predictor of compressive strength (Figure 4), whereas mass showed no correlation with any property. This finding aligns with previous studies demonstrating that internal pore architecture, quantified via imaging techniques such as µCT, has greater predictive value for mechanical performance than bulk mass or density measurements.7,9,28,35
Macropores are recognised initiation sites for cracks in PMMA.11,14–16 The µCT models used in this study enabled quantification of macro- and micropores. When comparing vacuum assisted methods, mixing with the vacuum bowl produced 75% fewer macropores than the vacuum cartridge (Table 2). This observation aligns with prior studies that have shown mixing technique and device design can significantly affect pore formation.7,10,11,31 However, no consistent effect of vacuum level on macropore frequency was observed across all mixing systems. This contrasts with previous reports suggesting that increasing vacuum levels generally reduce microporosity.4,8,10 The discrepancy may be attributed to differences in device mechanics, cement handling after mixing or variability in pore clustering, underlining the need for further study on the complex interplay between mixing parameters and pore architecture.
While pore quantity in PMMA offers useful information, pore distribution and location may play an even more critical role in crack initiation. Studies by Murphy and Prendergast 17 and Jeffers et al. 18 suggest that two or more pores forming in close proximity to one another are more likely to promote crack initiation. Similarly, Cristofolini et al. 14 highlights that surface adjacent pores in PMMA are particularly prone to initiating cracks. These findings highlight the influence of pore distribution on mechanical and fatigue properties. Future investigations should therefore map pore location and clustering to better predict crack initiation and fatigue performance.
ISO 5833:2022 imposes several limitations that affect the translational relevance of findings from in vitro studies. Firstly, the standard requires only five samples per preparation method. In the present study, this restriction severely limited statistical power and the ability to account for inherent material variability. This limitation was observed in our results, where outliers appeared in five of the nine mixing groups (most notably in the Vacuum Bowl 550 mm Hg group). These outliers skewed mean values and likely precluded the detection of statistical significance across the intermediate vacuum levels, demonstrating that the ISO-mandated sample size is insufficient for robust characterisation. Furthermore, the standard restricts samples to cylindrical specimens of 6 mm diameter and 12 mm height. This standardised geometry prevents investigation of how varying sample sizes and aspect ratios influence heat generation, curing kinetics, and pore distribution, factors known to affect the mechanical and thermal behaviour of PMMA.29,30,38 Furthermore, the cement volumes used in these specimens (∼1300 mm3) are significantly smaller than those in clinical applications, where femoral canal cement mantles can exceed 35,000 mm3. 38 This scale difference affects thermal gradients, polymerisation shrinkage and stress distribution, reducing the relevance of uniaxial compression tests on small specimens to predict the in vivo performance of cement mantles in joint replacements. Additionally, the choice of mould material is not specified by ISO 5833:2022, which may introduce uncontrolled variation. While this study used Delrin® (polyoxymethylene), alternative materials such as metal or silicone possess markedly different thermal conductivities and may accelerate or dampen heat transfer during polymerisation, thus affecting porosity and curing dynamics. 30
Alternative experimental approaches could more directly evaluate the functional role of porosity in implant fixation. For instance, this study did not address the mechanical bonding interface between PMMA and prosthetic components, a critical factor in the initiation of aseptic loosening. Geiger et al. 39 investigated this interface using push-out testing of metallic pins embedded in cement, providing insights into interfacial shear strength and debonding mechanisms. Incorporating a similar testing approach could help assess how pore architecture affects load transfer and failure at the implant-cement interface. Other future studies could build on this work by evaluating PMMA performance in more anatomically and mechanically realistic models, such as cemented femoral stems in composite Sawbones® surrogate femurs. 40 Such approaches may offer valuable insight into implant-cement and cement-bone interactions, and serve as validation platforms for computational models of cement behaviour under clinical conditions.
In conclusion, within the constraints of the sample size (n = 5) mandated by ISO 5833:2002, the study demonstrated a significant and strong correlation between the porosity and compressive strength of PMMA bone cement produced using three different mixing methods. Vacuum bowl mixing under high levels of vacuum (650 mm Hg) produced cement with significantly lower porosity than open bowl mixing under atmospheric conditions. Similarly, in the vacuum cartridge system, high vacuum mixing reduced porosity relative to mixing without vacuum.
These findings also highlight key limitations in the current ISO 5833:2002 standard, including insufficient sample size, overly restrictive geometry and a lack of clinically representative testing protocols. Addressing these limitations through expanded standards and more physiologically relevant test methods would improve the predictive value of in vitro PMMA assessments to better inform the pre-clinical evaluation of orthopaedic bone cements.
Footnotes
Acknowledgements
The authors would like to thank the Institute of Medical and Biological Engineering for hosting the summer intern student who performed the majority of this work.
Ethical considerations
This article does not contain any studies with human or animal participants.
Consent to participate
There are no human participants in this article and informed consent is not required.
Author contributions
Harry Barratt: Data curation, Formal analysis, Investigation, Methodology, Project administration, Visualisation, Writing – original draft, Writing – review and editing. Harry Templeman: Conceptualisation, Methodology, Resources, Supervision, Writing – review and editing. Karthik Nair: Conceptualisation, Methodology, Resources, Supervision. Gavin Day: Conceptualisation, Methodology, Resources, Supervision, Writing – review and editing, Project administration. Anthony Herbert: Conceptualisation, Methodology, Resources, Supervision, Writing – review and editing, Project administration, Funding acquisition.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the School of Mechanical Engineering through the Faculty of Engineering and Physical Science Summer Internship Scheme at the University of Leeds.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
