Abstract
We document the lived experience of Shiv, a care home recruitment manager, during the period of mandated employee vaccination in the COVID-19 pandemic. Care homes in the United Kingdom, as in many parts of the world, became a brutal front line in the battle to mitigate the pandemic’s worst effects. Residents and staff were among the most vulnerable to infection, a risk heightened by failure to test incoming residents and employees. In response to rising mortality in care homes, the UK government made vaccination a condition of employment from 11 November 2021. Through Shiv’s reflective narrative, we examine the ethical tensions and practical challenges of enforcing mandatory vaccination in care homes – and the confusion and consequences that followed its abrupt withdrawal.
Keywords
Introduction
Securing a skilled and motivated workforce has long been a challenge in the social care sector. Low wages, coupled with persistent labour and skills shortages exacerbate the inherent tensions of a market-driven approach to provision (Aronson and Neysmith, 2006; Needham et al., 2023). Maintaining adequate staffing levels is essential for supporting residents’ health and well-being yet remains a persistent challenge even under normal operational conditions. While some evidence suggests that average vacancies and turnover decreased during the pandemic (Skills for Care, 2021), the crisis also introduced significant additional staffing pressures. These included increased staff absences due to infection and illness, reduced labour supply and the need to manage the risk of viral transmission. Compounding these issues, care homes were generally unprepared for the pandemic, having inadequate levels of personal protective equipment (PPE) and robust policies to prevent transmission between residents, staff and visitors (Brainard et al., 2021).
This account explores how the introduction – and subsequent reversal – of mandatory employee vaccination as part of the UK government’s pandemic response, created new and complex challenges for the social care sector. Rooted in public health ethics, the policy reflected a utilitarian logic and ethical balancing act aimed at protecting vulnerable populations by prioritising collective welfare over individual autonomy (Savulescu et al., 2020). Informed by evidence that vaccination may significantly curb transmission (Gordon et al., 2022), this approach echoed wider debates about state intervention (D’Errico et al., 2021). However, beyond its ethical rationale, the policy’s sudden shifts intensified existing workforce pressures (Johnson and Bagatell, 2020), as some workers refused vaccination and faced dismissal or chose to resign. Responses that highlight the tensions between public health measures and personal choice.
Shiv’s experience reveals the friction between everyday moral reasoning (Sayer, 2000, 2007) and top-down vaccination policies enforced through the employment relationship. Balancing often contradictory perspectives from staff and residents added further complexity. Care homes occupy a unique ethical space, with heightened obligations to protect both vulnerable residents but also the well-being of staff – dual responsibilities that intensified the moral conflict surrounding mandatory vaccination.
At face value, the mandate was a legal requirement designed to protect residents at heightened risk. Yet its enforcement exposed deeper tensions. While the law provided clear obligations, requiring employers to bar unvaccinated staff from entering care homes, many were caught between their duty to comply with the regulations and their loyalty to experienced staff who had risked their health earlier in the pandemic. This conflict was especially acute because the policy disrupted longstanding employment relationships, forcing managers to choose between regulatory compliance and retaining valued employees at a time when acute staff shortages were already undermining care outcomes.
The subsequent reversal of the mandate (March 2022) – informed by public consultation, the emergence of the less severe Omicron variant and increasing population immunity – created further complexity. Without legal compulsion, care homes faced a new ethical question: whether maintaining vaccination requirements constituted responsible stewardship or undue infringement on autonomy. What had begun as a public health measure thus became a deeply personal moral dilemma for managers, requiring them to weigh risks, rights and institutional responsibilities, without clear precedents.
The UK social care context and COVID-19 challenges
Prior to the pandemic, residential and nursing care homes in the UK served approximately 400,000 residents who required support both day and night due to complex medical conditions that make independent living challenging (Age UK, 2019). Care homes provide accommodation for individuals whose homes cannot be adapted to meet their needs, who lack sufficient family support, or for whom independent living or in-home care services are not feasible. Demand for care homes has grown significantly, driven primarily by the UK’s ageing population (Mogaji, 2019; Needham et al., 2023). In response, the UK, like many countries, has increasingly relied on private (often for-profit) providers to deliver care services, resulting in a quasi-marketised approach (see also Baron and West, 2017).
Despite growing demand, profitability for the sector’s predominantly private providers (83%) has sharply declined in recent years (Dalley, 2022). Since 2017, the government welfare austerity policies have resulted in real-terms funding cuts to local authorities. In response, many have reduced their contributions to social care, leaving care home funding up to 10% below the actual cost of provision in many cases (Baines et al., 2022; CMA, 2017). As a result, many homes operate under severe financial strain. With staffing costs accounting for around 60% of overall expenses (Care Quality Commission [CQC], 2023), providers often make difficult budgetary decisions – cutting operational and staffing expenditures or deferring essential investments. Low pay, limited career development opportunities and poor working conditions are endemic to the sector, issues exacerbated by the lack of a sustainable funding model (Read and Fenge, 2019).
These financial pressures intersect with longstanding structural challenges in care home employment relations. On the eve of the pandemic, Skills for Care (2019) reported an average staff turnover rate of 30.8%. Although most leavers remained within the sector, workforce instability persisted, with vacancy rates of around 8%, compounded by a 20% decline in registered nurses since 2012 – significantly eroding the sector’s clinical capacity. Compounding these issues, nearly a quarter of staff worked on zero-hour contracts, while stagnant wages offered little incentive for younger workers to join the sector.
The sector’s structural weaknesses – chronic skills shortages, high turnover and heavy reliance on agency workers – created a fragile employment ecosystem long before COVID-19 emerged (Baines et al., 2022; Hebson et al., 2015). While agency staff provided temporary flexibility, their lack of familiarity with residents’ needs and institutional routines increased risks of clinical errors and undermined team cohesion (Banerjee et al., 2015; Porter et al., 2022). Precarious working conditions, including fragmented schedules and limited career progression pathways, further exacerbated retention challenges (Read and Fenge, 2019). These pre-existing vulnerabilities became critical pressure points when the pandemic struck, as acute staffing shortages forced care homes into even greater dependence on agency labour while simultaneously battling to maintain infection control (Skills for Care, 2021). This fragility framed much of the feedback during the consultation on mandatory vaccination, where concerns were raised about exacerbating staffing shortages and disproportionately affecting protected groups, including pregnant women and some ethnic minority communities (Department of Health and Social Care [DHSC], 2021c).
The COVID-19 pandemic brought care homes into the public eye in an unprecedented way. Historically, care homes have operated as a largely hidden service, familiar to those with direct experience as employees, residents or family members, yet often obscured from public view and wider consciousness. Residents of both residential and nursing homes receive care from visiting primary care specialists and community-based nurses (Gordon et al., 2022), making them significant consumers of National Health Service (NHS) services. Additionally, care homes are among the most substantial recipients of discharged NHS patients. COVID-19 graphically illustrated the porosity of the boundary between the NHS and care homes. To free up critical care capacity, NHS trusts postponed non-urgent operations and discharged hospital in-patients who were medically fit to leave (Guthrie et al., 2022). During the early phase of the pandemic, rapid testing was not widely available, and testing for patients discharged from the NHS into care homes was mandated only from 15 April 2020. As a result, throughout much of the first wave of the pandemic, patients were discharged into care homes without a negative test result – an approach subsequently deemed unlawful.
Between 9 March and 19 July 2020, there were 6811 recorded COVID-19 outbreaks in care homes across England, with 77% occurring before May. This early surge coincided with a sharp rise in COVID-related deaths, peaking at 3525 in the week ending 24 April 2020 (Office for National Statistics, 2022) (Figure 1). By contrast, in the two to three months following the introduction of mandatory vaccination for care home workers on 11 November 2021, weekly deaths among residents ranged from 62 to 337 – far lower than the first-wave peak. Notwithstanding the different contexts of these two periods, including prior immunity, improved treatments and changes in viral variants, there is little or no evidence to suggest that mandatory vaccination directly reduced mortality.
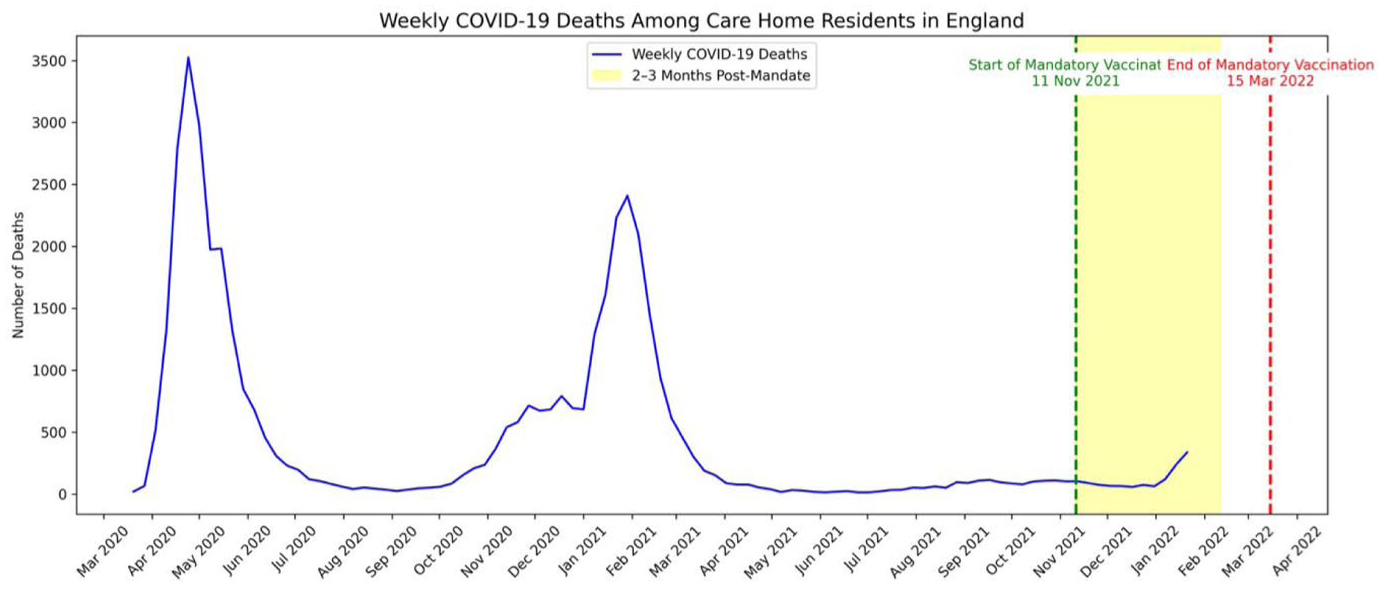
Weekly COVID-19 deaths among care home residents in England between March 2020 and April 2022.
The impact of the pandemic was unevenly distributed, with fewer than 30% of care homes accounting for almost all COVID-related deaths (Morciano et al., 2021). By May 2022, a consensus emerged that, while hospital discharges contributed to some outbreaks, staff and visitor movement were more likely the dominant routes introducing infection into care homes (Guthrie et al., 2022). Recognising these challenges, the government provided additional funding to enhance infection control (DHSC, 2021a), support the rapid testing of visitors and care home staff (DHSC, 2021b), maintain safe staffing levels and discourage staff movement between care homes and other care settings (DHSC, 2021d).
Given the vulnerability of care home residents and the close-contact nature of care, mandating vaccination as a condition of employment was designed to achieve two core objectives: reduce transmission risk between staff and residents and minimise staff absence due to illness. From an ethical perspective, the mandate aligned with healthcare’s duty of care to minimise harm, while also supporting workforce sustainability during operational crises (Savulescu et al., 2020). However, the UK was comparatively slow to act, ranking 15th out of 22 high-income countries in introducing an occupational vaccination mandate, which was implemented only in November 2021 and subsequently revoked in March 2022 (Cameron-Blake et al., 2023; DHSC, 2022). Modelling indicates that staff vaccination could have prevented around 30% of care home infections and halved COVID-related deaths (Gordon et al., 2022: 2).
Although mandatory vaccination offered clear potential benefits for residents, it also provided protection for care home employees, who were generally at an elevated risk of infection (Brainard et al., 2021). However, concerns were raised within the sector that mandatory vaccination would exacerbate staffing challenges, in an already highly strained labour market (Limb, 2021). These concerns focused on fears that an inability to maintain safe staffing levels could lead to reduced care quality and home closures, leading to a reduction in available beds. Subsequent analyses revealed that mandatory vaccination led to a 3–4% reduction in staffing levels, with, as previously noted, little evidence of reduced mortality among residents (Girma and Paton, 2024). Thus, the estimated 20,000 care home workers who either left their jobs or were dismissed (Everycare, 2022), significantly reduced the overall care home workforce, which has yet to fully recover. This operational context sets the stage for the following discussion, which explores the impact of these staff losses and the enduring legacy of the policy, even after the reversal of mandatory vaccination.
Care home recruitment and mandatory vaccination: Shiv’s reflections
Team Care Group (pseudonym) has been providing care for older adults for over 30 years, specialising in high-quality care homes located in the North of England. Operating 10 care homes, the organisation is committed to person-centred care, emphasising family involvement and striving to be both a provider and employer of choice. Their facilities offer residential, dementia and nursing care, as well as short-term respite care packages. In response to recruitment challenges, Team Care Group has prioritised employee recognition and placed an increased emphasis on career development to attract and retain staff.
Shiv (pseudonym) began their account by talking about their entry to the role: I started in October 2021, in a position created to address some of the recruitment challenges faced by the Team Care Group. Historically, staff recruitment has been done independently by each home, but the group saw an opportunity to centralise these processes. My team handles initial job advertisements, candidate attraction and screening interviews, and ensures regulatory compliance with criminal record checks, reference checks and other legal requirements. Recruitment is vital for the success of our care homes, impacting both business performance and the quality of care provided. I’ve worked in recruitment most of my life, but recruitment in social care is by far the most challenging. Nationally there is a shortage of carers, yet the number of residents increases monthly. Retention is a big issue for us, and we put a lot of thought into recognition and showing that we value our staff. This also helps to attract staff, and generally our market position as a high-quality care provider that offers advantages too.
A significant part of my role is attracting people from other sectors into social care, which often involves challenging perceptions about care work. It’ll always be a challenge to recruit, as negative perceptions persist. However, unlike some other care settings, our carers have the opportunity to build genuine, lasting relationships with those they support – something often missing in NHS roles. That said, there is no disguising the fact the work we do is hard. We often work 12-hour shifts – you’re up and down, it can be physically demanding but also rewarding, it can also be very emotionally draining. Sometimes residents aren’t thankful so, you know, you’re working hard for somebody who doesn’t appear to appreciate it. Residents can have quite complex care needs. In our dementia communities, for example, many residents can be non-verbal, which, if you haven’t experienced something like that before, can be quite a challenge.
We face significant recruitment challenges across most roles in our homes, but I spend most of my time focused on hiring healthcare assistants (HAs) and nursing staff. Recruiting for HAs is particularly demanding, largely due to the high number required to ensure smooth operations within each home. HAs provide essential, individualised personal care, supporting residents with their daily routines and care plans. Ideally, they would have prior experience in care work and be capable of safely moving and handling patients with sensitivity and care. Currently (July 2022), for instance, I need to recruit enough HA to cover approximately 300 care hours in one of our homes.
In contrast, although nurses play a critical role, we only have about 40 to 50 nursing hours to cover, which could be managed by one or two qualified staff members. Nurses are required to be qualified, registered professionals who take the lead on clinical and medical care for residents. Beyond their clinical duties, they also fulfil an essential leadership role providing guidance and coaching for the rest of the team. While we often rely on agency or bank staff to fill nursing vacancies, it’s not feasible to do the same for HAs, due to the volume of hours required.
Care homes can fail in two main ways: clinically and financially. Clinically, a failure often occurs when reliance on agency staff prevents the formation of meaningful relationships between staff and residents, as well as among staff themselves. This lack of continuity and familiarity can lead to mistakes, and impact care quality. Financial failure happens when the cost of using agency staff, among other things, makes the home financially unviable. Recruitment plays a pivotal role in avoiding both scenarios by ensuring a stable, secure staff base that not only reduces costs but also improves the quality of care. Our business operates on a small profit margin, it is not government-run, making efficient recruitment strategies even more critical.
We began requiring mandatory vaccination in our job adverts as soon as we knew it was to become law. From October (2021), I was having to ask candidates at interview if they’d had the vaccination. If they hadn’t, I couldn’t continue with their application. There were cases where I had to terminate interviews as there was no point in proceeding since you’ve got to have a minimum of six weeks between your first dose and second dose. If, at interview, applicants have not had their first dose, there is no point speculating what position the home will be in six weeks later when they would potentially be able to work. I just clearly and honestly explain to candidates: ‘I’m more than happy, if you do decide to have your vaccination, for you to come back to me and then we can proceed with your application’. People respond differently. A young applicant told me that she’d had her first vaccine but suffered a bad reaction to it. She didn’t want to have the second because she’d reacted badly. In such cases, a GP can provide evidence of a medical exemption. Very few new applicants have questioned the vaccine requirement.
Within the homes, for current employees, I think it has been a very different experience. Some employees have had to leave because they refused vaccination. The exit interviews in these cases have been quite upsetting and difficult. Some colleagues have held strong ‘anti-vax’ beliefs and felt very let down when they have had to leave. I think the strong feelings around this issue stem largely from what staff experienced before vaccinations were required. No one was prepared for the situation, and although we were able to secure some PPE for our staff – many even provided their own – there was significant anxiety among our staff, not so much for themselves, but for the risk they could pose to their families or to our residents. It wasn’t uncommon for employees to change out of their uniforms as soon as they arrived home and to wash them at high temperatures. Some, who have vulnerable family members, effectively isolated themselves and made countless other personal sacrifices. Dismissing them, after all that they have endured, was incredibly tough. Although most of the staff understand it’s a government-led policy, I don’t underestimate the strength of feelings involved. Staff know we’re not individually stating what our beliefs [about the vaccination] are, and that we’re not making people do stuff [have the vaccination] they don’t want to do, but it does feel like a betrayal. I’ve heard comments like ‘we’ve used them’, and they are really upset about having to leave. You also have those who don’t really want the vaccine but have had it just to keep their job.
In terms of recruitment, if applicants say, ‘Yes, I’ve had my first dose’, or ‘I’m having my first dose on x date’, then if they haven’t yet had it, I suggest we keep in touch and see how things go. If they say something like, ‘I’m booked in to have my second jab on x date’, then I’d be happy to proceed with the interview, and tell them that we can do the interview, we can do the onboarding, but they won’t be able to start until they’ve provided evidence of vaccination. Even though it is clearly stated in the advert, and a matter of very public debate, we still have applicants who think they’ll be able to start with us without the vaccination.
When asking candidates about their vaccination status, I try hard to not let people think that I’m judging them. My personal belief, outside of work, is that people employed in a care home should be vaccinated, but I also believe that vaccination is a personal choice. I’ve learnt that people have many different reasons for refusal, and it’s none of my business why they may not want a vaccination. Therefore, I’m conscious that I want to be impartial with people at interview. My personal feelings don’t really come into it as it’s not the case that what I say, or what I think, about vaccination changes whether or not they’re going to get the job. They need to provide evidence. I’ve never said anything like ‘you really should take this because the residents are at risk if you don’t’.
Vaccination U-turns and moral ambiguity
The U-turn on vaccination has placed us in a predicament regarding staff members who voluntarily left or were dismissed. Should we reach out to these individuals and ask them to return when we’re so desperate for staff?
Previously, our concerns centred on the legality of requiring new hires to be vaccinated and the firm’s risk of potential litigation. At that stage, it was primarily a matter of law or regulation – something beyond our control. Now, no one is telling us what to do. With vaccination no longer mandated, we’re left to make our own judgement: should we still require it, knowing that unvaccinated staff could pose a risk to residents? And if we no longer require it, should we consider reaching out to staff who left because of the mandate? If we reemploy those we dismissed, how would it affect those who chose to be vaccinated – perhaps reluctantly – just to keep their jobs? How would they feel about colleagues returning who refused the vaccine on principle? It has become more of a moral dilemma than ever before. There are strong emotions, particularly among home managers, who feel that inviting back those who left could cause real resentment among those who stayed. One manager put it bluntly: ‘If you invite people to return who left because they refused the vaccine, there would be very, very strong feeling in the home from people who stayed’. It’s a deeply emotional and difficult issue.
Losing a job is difficult at any time, but during COVID, with all its uncertainty, it was especially challenging. I experienced this myself – losing a job during the pandemic was frightening. It wasn’t just about the immediate worry of paying the mortgage and covering basic expenses, it was happening amid a global crisis, adding a whole new layer of uncertainty. But losing a job due to vaccine status? That’s different. Who’s to say what the personal circumstances of those people are? Some of the staff we had to let go were sole breadwinners for their families. Others felt they had no real choice but to get the jab – and that decision carries lasting consequences. Once it’s in your body, you can’t undo it. I can see why those people might feel aggrieved if we now bring back staff who refused vaccination. They might think: ‘If I’d just held firm, I’d still have my job’. There’s also the sense that care workers were pressured into vaccination. Some of those who left – or were dismissed – might not want to return out of principle. They could feel they were treated unfairly or that we, as an employer, lacked empathy. While some may understand that we had no choice, I imagine others will feel bitter and may not want to re-enter the industry at all.
I also think about what happened to the people who left us, and whether they’re in a better place now. Many have left the care sector – especially those who worked through the hardest phases of the pandemic, when the job was incredibly demanding. I believe we’ve lost a significant number to other industries, like hospitality. Some may have moved on and thought, ‘Actually, this is better’, while others might still feel valued by us and be open to returning. Either way, I know there will be strong feelings on both sides.
Within the industry, most providers are still weighing up whether to approach people who either left or were dismissed. The next stage will be to try and have a conversation with the home managers to get their thoughts. They will be thinking a lot about people in the home who did have the vaccine. I think they’ve got to play it on an individual basis. So, I don’t think we will strategise to target people specifically, I think we’ll just continue with our recruitment campaign as normal, but the pressure to fill roles drives everything and I am not sure the sector will ever fully recover.
Footnotes
Acknowledgements
The authors are grateful to all reviewers and the Editor, Professor Gabriella Alberti, for the constructive and helpful reviews of the manuscript. We are immensely grateful to Shiv Varma for sharing their experiences so candidly.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research received a Newcastle University Business School small project grant.
Ethics statement
The project ‘The impact of mandatory vaccination on the recruitment and retention of adult Social Care workers’ received full ethics approval from Newcastle University (Ref.: 26901/2022).
