Abstract
Highlights
• Among Brazilian older adults, dynapenic abdominal obesity was associated with the occurrence of a single fall. • Those with abdominal obesity, dynapenia, and dynapenic abdominal obesity had a higher chance of recurrent falls.
Introduction
Falls are multifactorial in nature and have negative repercussions on individuals’ health and well-being of individuals, resulting in long-term care needs with a significant impact on health system costs (Khow & Visvanathan, 2017). Approximately 28–35% of people aged 65 and over fall each year, increasing to 32–42% for those over 70, with half of them falling more than once (World Health Organization, 2020).
A meta-analysis showed that obese older adults are more likely to fall compared to those without obesity, and the mechanisms that can explain this association are still not well understood (Neri et al., 2020). However, there is evidence of mediation with chronic health conditions, sedentary behavior, medication use, functional limitation, and disability (Himes & Reynolds, 2012; Mitchell et al., 2015) leading to reduced postural control, reactive movement strategies, verticality, and compromised gait (Horak, 2006). Epidemiological research also showed that dynapenia, an age-associated of muscle strength, contributes to the increased likelihood of falls in older adults (Balogun et al., 2017; Mitchell et al., 2014; Moreland et al., 2004).
Further, obesity, particularly abdominally, can exacerbate dynapenia through inflammatory and endocrine mechanisms (Delmonico et al., 2009) which promote damage to skeletal muscle (Scott et al., 2014) and impairment of motor neuron repair (Senechal et al., 2012). Thus, the coexistence of global obesity and dynapenia called dynapenic obesity has been linked to increased falls risk in some (Himes & Reynolds, 2012; Mitchell et al., 2015), but not all (Neri et al., 2020) studies. Meanwhile, dynapenic abdominal obesity (Senechal et al., 2012), the most clinically relevant phenotype due to the well-established adverse effects of central obesity (Delmonico et al., 2009; Scott et al., 2014; Senechal et al., 2012), still has incipient studies regarding its impact on falls (Balogun et al., 2017; Gadelha et al., 2020; Máximo et al., 2018), especially in older adults who fall recurrently (Máximo et al., 2018).
Waist circumference has been considered as an important clinical criterion for identifying abdominal obesity, and abdominal obesity has been highlighted excessive intra-abdominal fat accumulation has a good prognostic to predict falls (Alexandre et al., 2018; Bouchard & Janssen, 2010; Gadelha et al., 2016; Máximo et al., 2018; Neri et al., 2017; Pereira et al., 2019). However, research that evaluates the coexistence of these two conditions, called dynapenic abdominal obesity (Senechal et al., 2012) and its impact on falls is still incipient (Balogun et al., 2017; Gadelha et al., 2020; Máximo et al., 2018), especially in older adults who fall recurrently (Máximo et al., 2018). The synergistic risk of both dynapenia and abdominal obesity on fall occurrence requires further consideration. The coexistence of dynapenia and abdominal obesity has been recently introduced as dynapenic abdominal obesity (Alexandre et al., 2018; Máximo et al., 2018; Pereira et al., 2019), which was associated with dynamic balance, falls, and fear of falling (Máximo et al., 2018; Pereira et al., 2019). Population-based investigations can help identify profiles and in improve the understanding of the association between abdominal obesity and dynapenia, in single and recurrent falls and contribute to the design of fall prevention programs. This is a cross-sectional study that aimed to verify the association between dynapenic abdominal obesity and the occurrence of single and recurrent falls in a representative sample of Brazilian adults aged 50 years and over.
Methods
Study Population
This study used baseline data from the Brazilian Longitudinal Study of Aging (ELSI-Brazil), collected in the years 2015 and 2016. ELSI-Brazil is a nationwide and home-based survey that investigates the living and health conditions of the non-institutionalized population aged 50 and over. The study was approved by the Research Ethics Committee of the Oswaldo Cruz Fundation, Minas Gerais (CAAE 34649814.3.0000.5091). All participants signed a free and informed consent form at the time of the interview to participate in the study. More details can be obtained on the research homepage (http://elsi.cpqrr.fiocruz.br/) and in a previous publication (Lima-Costa et al., 2018).
The ELSI-Brazil sample plan was based on strata. For smaller municipalities, the selection was made by the municipality, census tract, and household, while for larger municipalities, the selection was made by the census tract and household. The sample size was estimated at 10,000 individuals (9412 participated) living in 70 municipalities, in the five geographic regions of the country. Data were collected using a questionnaire applied during a face-to-face interview and a physical examination, both performed at the participants' homes. For this study, those who had complete data were selected, which resulted in a final sample of 8374 older adults (89.0% of the study participants).
Variables and Collection Procedures
We considered falls in the 12 months preceding the interview based on the information obtained from the interviewee’s (93.5%, n = 7810 for unweighted data) or proxy (6.5%, n = 564 for unweighted data) informant’s report. The outcome variable was categorized as: did not fall, single, and recurrent falls (two or more falls in the evaluated period).
Abdominal obesity was identified using waist circumference (WC), according to cutoff points commonly used in the literature (Lean et al., 1995). Thus, WC values ≥88 cm for women and ≥102 cm for men were considered indicative of abdominal obesity. WC was measured at the midpoint between the last rib and the iliac crest using a flexible and inelastic measuring tape, after a normal expiration, with the subject standing up (World Health Organization, 2008).
The presence of dynapenia was assessed using handgrip muscle strength, measured using a handheld hydraulic dynamometer (Saehan Corporation, 973, Yangdeok-Dong, Masan 630–978, Korea). Three maximum handgrip maneuvers were performed with the dominant hand, with verbal stimulation, always with a one-minute rest interval between each assessment, the highest value obtained was considered in the analysis. The test was performed with the participant seated, with the elbow flexed at 90°, the forearm in a neutral position, and the thumb pointing to the ceiling. Men with handgrip strength <26 kg and women <16 kg, according to cutoff points suggested by the Foundation for the National Institutes of Health Sarcopenia Project (Alley et al., 2014), were considered dynapenic.
We categorized the study population as follows: (1) without abdominal obesity and dynapenia; (2) abdominal obesity alone; (3) dynapenia alone; and (4) dynapenic abdominal obesity.
The covariables included in our analysis were selected based on biological and clinical plausibility as risk factors for abdominal obesity, dynapenia, and the occurrence of falls, especially in the population of older adults (Alexandre et al., 2019; Borges et al., 2020; Máximo et al., 2018).
The sociodemographic variables considered were age in years (continuous), sex (female and male), and education (<4 years, 4–7 years, and 8 or more).
Regarding health behaviors, information was obtained on smoking (non-smoker, ex-smoker, and current smoker), alcohol consumption (non-consumption, low-risk consumption, and at-risk consumption), and level of weekly physical activity (not recommended and recommended). Smoking was assessed based on self-reported use of any tobacco product (industrial cigarettes, cigars, straw cigarettes, etc.), regardless of the amount consumed. Alcohol consumption was considered low risk when the intake was 1–7 doses/week for women and 1 to 14 doses/week for men, and as at-risk consumption when the intake of >7 doses/week for women and >14 doses/week for men. In addition, the consumption on a single occasion in the last 30 days of ≥4 doses/day for women and ≥5 doses/day for men was also classified as at-risk alcohol consumption (NIAA, 2010). Physical activity was assessed using the reduced version of the International Physical Activity Questionnaire (IPAQ) validated in the Brazilian population (Matsudo et al., 2001). The information from the IPAQ was converted into total physical activity time performed in the week before the interview. Those participants who practised any mild physical activity (such as walking) or less than 150 minutes of moderate or 75 minutes of vigorous physical activities per week were defined as having an insufficient level of physical activity (World Health Organization, 2010). Those participants who practised 150 minutes or more per week of moderate and/or vigorous activities were defined as having a sufficient level of physical activity, as recommended by the World Health Organization (2010).
The body mass index (BMI) was calculated from the direct measurements of weight and height, using the formula weight(kg)/height(m)2. Height was measured using a portable vertical stadiometer (Nutri-Vida brand) and weight using a calibrated portable electronic scale (SECA brand), with the individual wearing light clothing and without shoes according to techniques recommended by the literature (Brasil, 2015). Both measurements were taken twice in a row by the interviewer, and the mean was considered as the final result.
Multimorbidity was defined as the presence of two or more chronic diseases (World Health Organization, 2016). The conditions included were cataracts, glaucoma, diabetic retinopathy, macular degeneration, hypertension, diabetes, high cholesterol, heart problems (infarction, angina, and heart failure), stroke, asthma, lung diseases (emphysema, chronic bronchitis or chronic obstructive pulmonary disease), arthritis or rheumatism, osteoporosis, spinal disorder, cancer, chronic renal failure, depression, Parkinson’s, and Alzheimer’s disease (Nunes et al., 2018). The presence or absence of these diseases was assessed by answering the following question: “Has any doctor ever said that you have…,” except for cataracts, glaucoma, diabetic retinopathy, and macular degeneration, which were evaluated by an ophthalmologist.
Disability included limitation in basic activities of daily living (BADL) (no/yes), according to the model previous (Alexandre et al., 2018) assessed based on the self-reported performance of the following activities: using the bathroom, showering, dressing, eating, going through a room, or walking from room to room on the same floor and lie down or get out of bed. All activities evaluated had four response options: 1) has no difficulty; 2) has little difficulty; 3) has great difficulty; 4) is unable to do it. Individuals who reported any difficulty (little, great or unable) to perform one or more of the six activities evaluated were considered to have limitations in BADL.
Statistical Analysis
The variables analyzed in the present study were compared between the categories of the outcome variable, using Pearson’s Chi-square test with Rao–Scott correction (categorical variables) and linear regression T-test (continuous variables).
Multinomial logistic regression analysis was used to assess the association of dynapenic abdominal obesity with the occurrence of falls, obtaining the odds ratio (OR) estimates and respective 95% confidence intervals. The reference category for the outcome was the group of older adults who did not fall (OR = 1.00) and the reference category for the explanatory variable was those who did not have abdominal obesity or dynapenia (OR = 1.00). For this, the following models were built:
Unadjusted Model
Model 1: adjusted for age, sex, education, smoking, alcohol consumption, level of weekly physical activity, and BMI.
Model 2: adjusted for the same variables as model 1, plus multimorbidity, and disability.
Two sensitivity analyses were also performed. First, as in previous studies (Gadelha et al., 2020; Scott et al., 2014), we performed additional analyzes, in which sex-specific handgrip strength tertiles were calculated. Individuals in the first tertile of muscular strength (<18 kg and <30 kg, respectively, for women and men) were considered to be dynapenic, while those in the second and third tertiles were considered to be non-dynapenic. Sex-specific WC tertiles were also calculated, as the cutoff points commonly used in epidemiological studies are not specific for older adults (Lean et al., 1995). Those in the third tertile (WC>97 cm and >100 cm, for women and men, respectively) were classified as having abdominal obesity, while those in the first and second tertiles were classified as having no abdominal obesity.
Second, we evaluated whether the exclusion of older adults classified as underweight (BMI <18.5 kg/m2) would alter the results obtained for the total study population. This analysis was performed since some authors (Máximo et al., 2018) reported that low weight is an important risk factor for dynapenia and falls, which could skew the results.
All estimates were obtained using the svy procedure in Stata® software version 13.0 (StataCorp LLC, College Station, TX), considering the individuals' weights and the complex sample design.
Results
Of all the older adults evaluated, 38.8% (95% CI: 37.3–40.4) presented only abdominal obesity, 10.4% (95% CI: 9.1–11.8) only dynapenia and dynapenic abdominal obesity was present in 8.1% (95% CI: 7.1–9.1) of the participants. The prevalence of a single fall among older Brazilian adults was 10.4% (95% CI: 9.7–11.2) and of recurrent falls was 10.8% (95% CI: 9.9–11.9).
Participant’s Distribution of Characteristics According to the Occurrence of Falls. Brazilian Longitudinal Study of Aging (2015–2016).
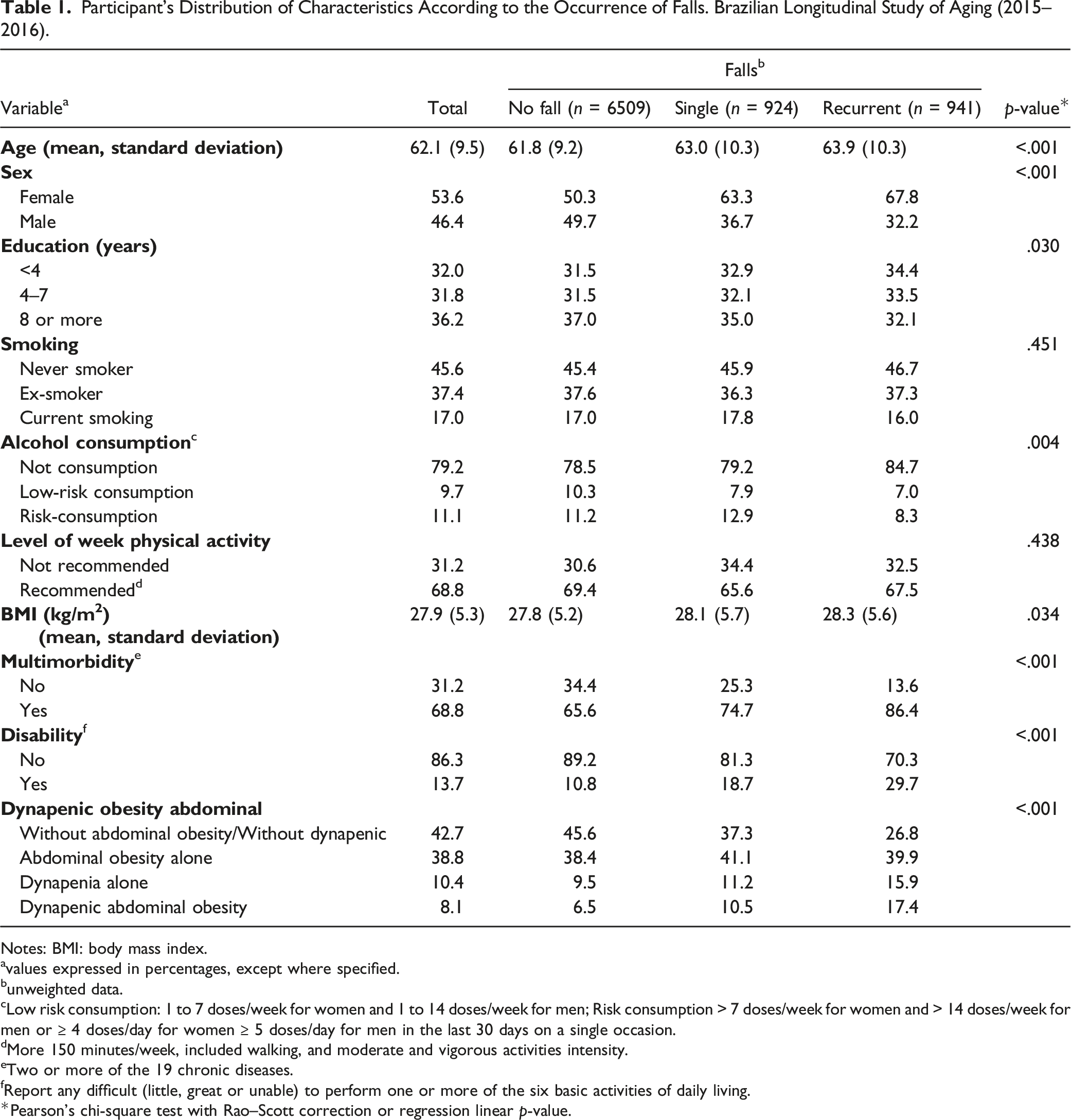
Notes: BMI: body mass index.
avalues expressed in percentages, except where specified.
bunweighted data.
cLow risk consumption: 1 to 7 doses/week for women and 1 to 14 doses/week for men; Risk consumption > 7 doses/week for women and > 14 doses/week for men or ≥ 4 doses/day for women ≥ 5 doses/day for men in the last 30 days on a single occasion.
dMore 150 minutes/week, included walking, and moderate and vigorous activities intensity.
eTwo or more of the 19 chronic diseases.
fReport any difficult (little, great or unable) to perform one or more of the six basic activities of daily living.
*Pearson’s chi-square test with Rao–Scott correction or regression linear p-value.
Association Between dynapenic Abdominal Obesity and Falls Among Older Adults. Brazilian Longitudinal Study of Aging (2015–2016).

Notes: Reference category: non-faller;
OR (95%CI): odds ratio (95% confidence interval).
Dynapenia: handgrip strength <18 kg for women and <26 kg for men;
Abdominal obese: waist circumference >100 cm for men and >97 cm for women.
Adjustment: Unadjusted model: no adjustment. Model 1: adjusted for age, sex, education, smoking, alcohol consumption, level of weekly physical activity, and BMI. Model 2: adjusted for the variable of the previous model, in addition to multimorbidity and disability.
Additional Analyses
In the additional analyses that used tertiles to define the status of abdominal obesity and dynapenia, we found different results. Those classified as having dynapenia alone were likely to have a single fall (OR: 1.27; 95% CI 1.01–1.59), while those classified as having abdominal adiposity alone (OR: 1.30; 95% CI: .97–1.74) did not show a statistical association with recurrent falls.
Participant’s Distribution of Characteristics According to the Missing or Include in the Final Analyses. Brazilian Longitudinal Study of Aging (2015–2016).
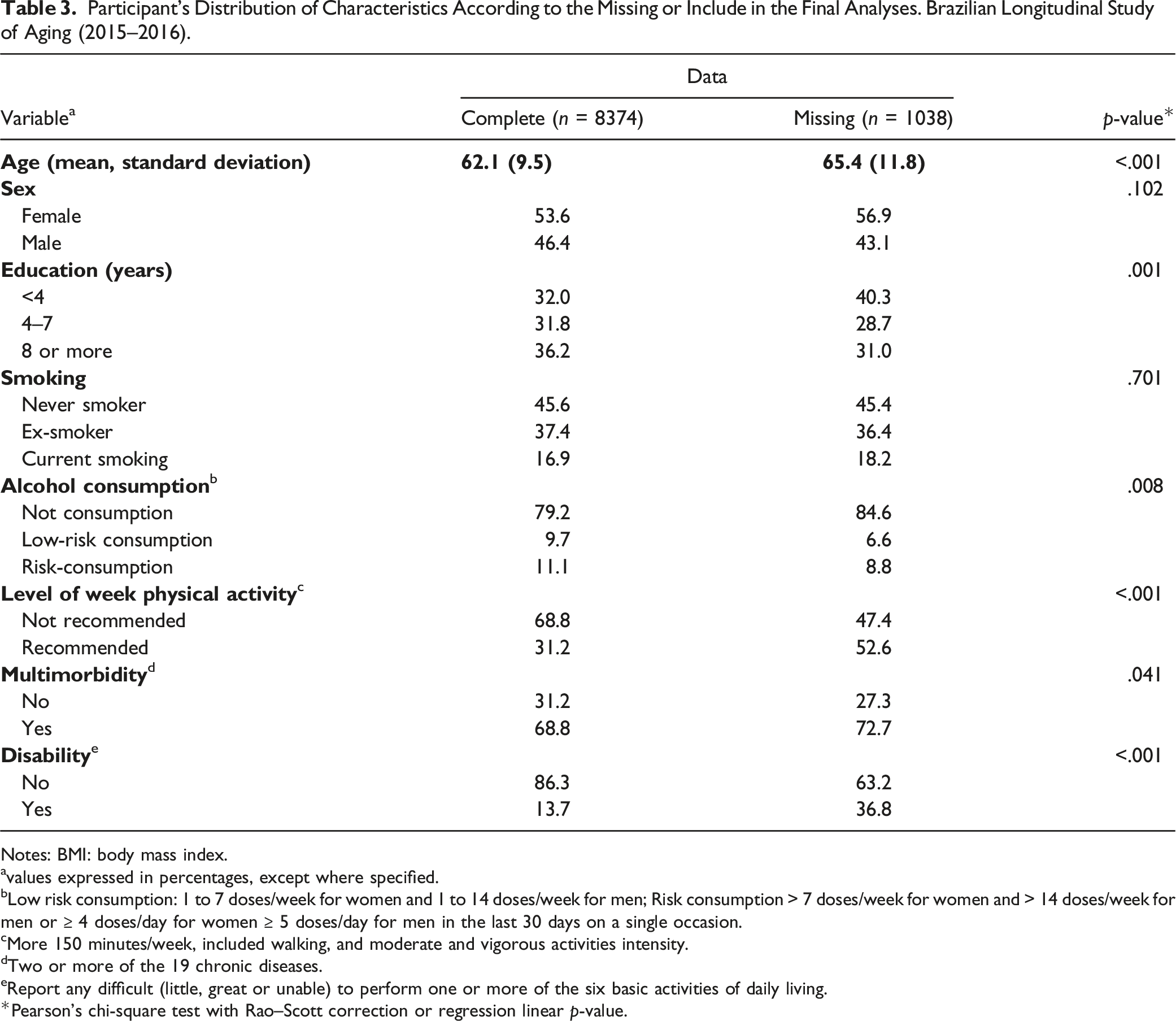
Notes: BMI: body mass index.
avalues expressed in percentages, except where specified.
bLow risk consumption: 1 to 7 doses/week for women and 1 to 14 doses/week for men; Risk consumption > 7 doses/week for women and > 14 doses/week for men or ≥ 4 doses/day for women ≥ 5 doses/day for men in the last 30 days on a single occasion.
cMore 150 minutes/week, included walking, and moderate and vigorous activities intensity.
dTwo or more of the 19 chronic diseases.
eReport any difficult (little, great or unable) to perform one or more of the six basic activities of daily living.
*Pearson’s chi-square test with Rao–Scott correction or regression linear p-value.
Participant’s Distribution of Characteristics According to the Occurrence of Falls. Brazilian Longitudinal Study of Aging (2015–2016).
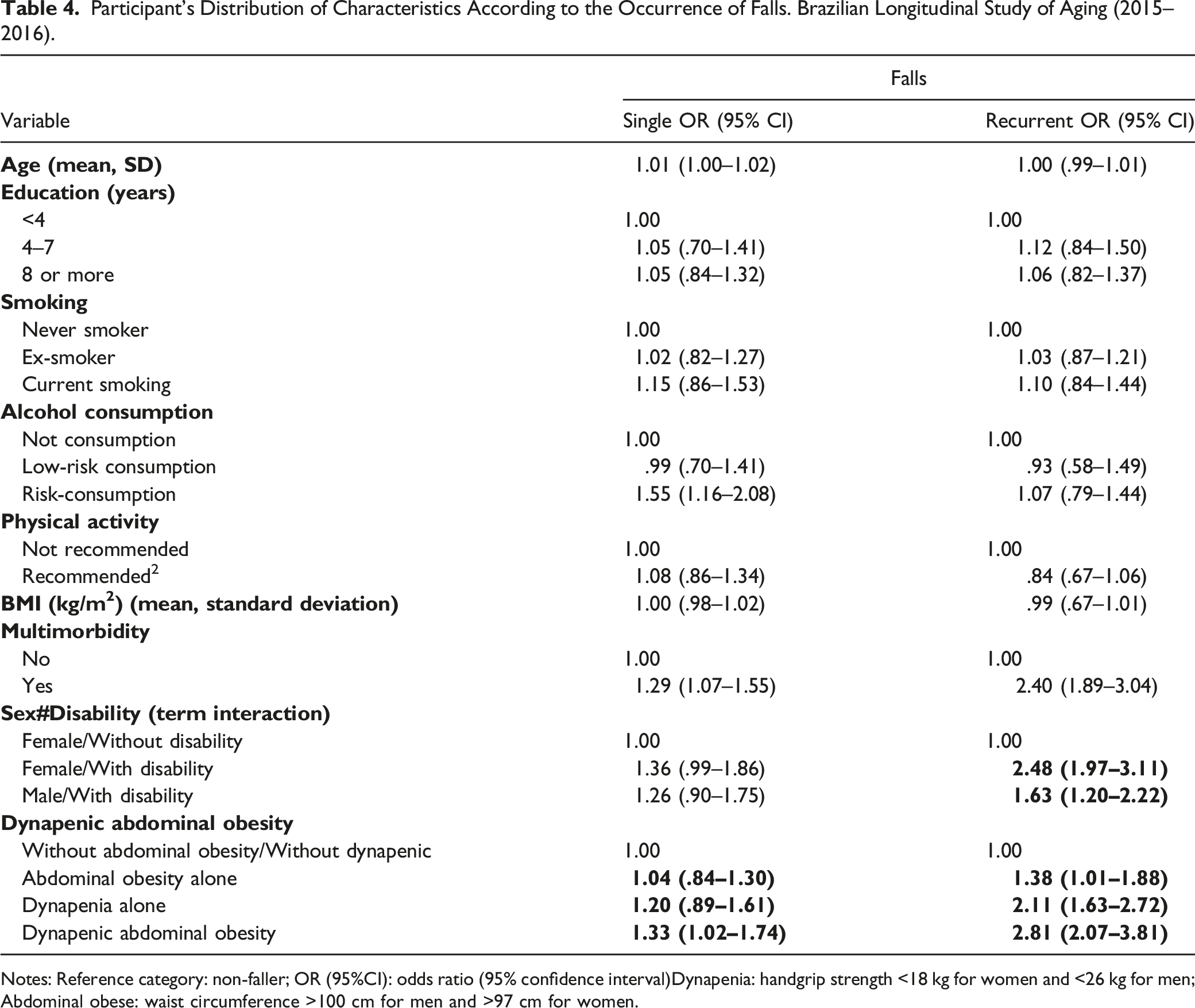
Notes: Reference category: non-faller; OR (95%CI): odds ratio (95% confidence interval)Dynapenia: handgrip strength <18 kg for women and <26 kg for men; Abdominal obese: waist circumference >100 cm for men and >97 cm for women.
Discussion
The results obtained in the present study showed that about 20% participants aged 50 years and over experienced a single fall or recurrent falls in the 12 months preceding the interview. There was an association between dynapenic abdominal obesity with a report of a single fall and between abdominal obesity, dynapenia, and dynapenic abdominal obesity with recurrent falls. Older adults with dynapenic abdominal obesity had nearly three times the chance of report of falling recurrently, even after adjustment for covariates.
The analysis of the body composition profile showed an increase in the likelihood of report of falls according to the existence of abdominal obesity and dynapenia, reinforcing the relationship between dynapenic abdominal obesity and falls, a hypothesis that guided the conduction of this investigation. Noteworthy, in the present study, we included recurrent fallers, that is a group less investigated in previous studies. Most studies analyze the occurrence of falls, but it is crucial to better understand recurrent fallers since they might have different intrinsic and extrinsic characteristics and multiple causes (Deandrea et al., 2010). Thus, this combination of anthropometric markers can reveal the result of different pathogenic processes and complement the interpretation of the associations found.
We observed a greater chance of a single fall in the group with dynapenic abdominal obesity, which is in line with previous studies conducted in older adult populations (Gadelha et al., 2020; Máximo et al., 2018; Scott et al., 2014). For example, a cross-sectional study carried out with 1046 individuals aged 60 years or more concluded that dynapenic abdominal obesity, assessed similarly to ELSI-Brazil, was more strongly associated with the report of a single fall than only abdominal obesity or dynapenia and that this association was independent of BMI (Máximo et al., 2018).
Another study that followed 674 older adults for 5 years found that dynapenic abdominal obesity was predictive of an increased risk score for future falls in both men and women (Scott et al., 2014). In this study, dynapenic abdominal obesity was defined based on the highest tertile of abdominal obesity and the lowest tertile of quadriceps muscle strength, both assessed based on dual-energy X-ray absorptiometry. Similarly, a study conducted with 201 older women who were followed for 18 months showed that those with dynapenic abdominal obesity had a greater risk of a single fall than those without this condition (Gadelha et al., 2020). However, these two studies did not adjust their analyses by measures of body fat distribution, such as BMI. Such an adjustment is necessary since we seek to evaluate the effect of abdominal obesity on the occurrence of falls that is not attributed to general obesity.
Despite differences in how abdominal obesity and dynapenia were assessed, as well as in the analyses conducted and adjustment variables considered, the results of ELSI-Brazil are consistent with previous findings (Balogun et al., 2017; Benjumea et al., 2018; Gadelha et al, 2020; Landi et al., 2012; Máximo et al., 2018; Schaap et al., 2018; Scott et al., 2014) showing that the coexistence of abdominal adiposity and low muscle strength has implications for a greater chance of report of a single fall in older adults.
Regarding recurrent falls, our results showed that, although having only dynapenia or abdominal obesity could contribute to this event, older adults with dynapenic abdominal obesity were more likely to have suffered two or more falls in the year before the interview, when compared to those without these conditions or with only abdominal obesity. To our knowledge, only one study to date has assessed this association. In this study with community older adults in the Health, Well-Being, and Aging Study (SABE), however, the authors found different results from those presented by ELSI-Brazil, where only those with dynapenia had a greater chance of recurrent falls (Máximo et al., 2018).
Possible explanations for the findings of the present study may be related to changes in postural control due to postural misalignment and a consequent change in the center of gravity of the body generated by the increase in abdominal volume and the presence of dynapenia as a reflection of the severity of sarcopenia. Increased WC can lead to poor postural alignment, requiring greater efficiency in motor balance strategies to maintain verticality and avoid falls (Corbeil et al., 2001). In this sense, a more anterior positioning resulting from abdominal obesity requires a significant increase in torque at the ankle to return the body to equilibrium in a stance position and considerably increasing the risk of falls (Corbeil et al., 2001). Dynapenia, in turn, reveals the muscular inability to respond to the necessary postural corrections imposed on the imbalance of abdominal obesity (Moreland et al., 2004).
It must be considered that the muscle deficit resulting from neuromuscular physiological abnormalities can be aggravated by obesity, especially with fatty infiltrates, and the combination of these conditions can contribute to greater postural instability by requiring additional strength to keep the center of mass aligned (Carvalho et al., 2019; Clark and Manini, 2008; Schrager et al., 2006). Thus, the failure of this system in the presence of dynapenic abdominal obesity puts the postural control mechanisms at a disadvantage (Horak, 2006). Unlike sarcopenic obesity, which may also be associated with falls (Landi et al., 2012; Schaap et al., 2018), dynapenic obesity may be an indicator that better discriminates older adults who fall, since dynapenia has been considered a measure of worsening of sarcopenia (35Benjumea et al., 2018).
The disadvantage imposed on postural control forms a truly vicious cycle that may partly explain the recurrence of falls. Previous evidence has shown that a fall (sporadic) can trigger fear or anxiety, limit mobility, be associated with chronic diseases, physical inactivity, obesity, and sarcopenia, and, consequently, be a risk for another fall (Pinheiro et al., 2010). The cycle of falls, therefore, explains the part of the recurrence of events by including functional decline as an important determinant of falls.
Single fall was reported only by individuals who had dynapenic abdominal obesity, which can be considered to have a more severe condition. Probably, then, because it was easier to trigger a vicious cycle, any condition, abdominal obesity alone, dynapenia alone, or dynapenic abdominal obesity, triggered a recurrent fall. However, a larger effect size has been demonstrated for dynapenic abdominal obesity, which confers a greater chance of recurrent falls than abdominal obesity or dynapenia alone.
Regarding the sensitivity analyses conducted, we found that, although previous studies have pointed out that the inclusion of individuals with low weight in the analyses may skew the results (Máximo et al., 2018), we found that the exclusion of these individuals from the analyses did not alter the findings (data not shown). Thus, to preserve the statistical power in the analyses, the sample was considered in its entirety. Also, the finding shows that the results of the association between dynapenic abdominal obesity and falls may differ in terms of the cut-off points used to define both abdominal adiposity and dynapenia, which demonstrates the need to standardize the definitions of these conditions for better comparability of the findings for different populations.
In the analyses that used tertiles to define abdominal obesity and dynapenia, we found that the results changed for single falls for those classified as having only dynapenia, who presented a greater chance of the outcome (data not shown) and for recurrent falls for those classified as having only abdominal adiposity, who did not present statistical association with the outcome. This finding shows that the results of the association between dynapenic abdominal obesity and falls may differ in terms of the cut-off points used to define both abdominal adiposity and dynapenia, which demonstrates the need to standardize the definitions of these conditions for better comparability of the findings for different populations.
Among the limitations of the present study, its cross-sectional nature stands out, which does not allow the establishment of a temporal relationship between the variables, given some of these associations may result from reverse causality. In addition, the difficulty that older adults may have in remembering the outcome of the last year is possible information bias. Further, the older adults not included in this analytical sample due to loss of information were older, had less education, were more physically active, did not drink consumption, and had more multimorbidity and disability might be understood as potential selection bias. On the other hand, this study has some important strengths. First, use easy and standardized tools to detect abdominal obesity and dynapenia in clinical practice settings. Second, was carried out based on data from a population-based study, collected by trained interviewers. Finally, consider several confounding factors in the statistical analyses. Thus, the study contributes to the existing literature by showing evidence that new composite anthropometric indicators are associated with both single and recurrent falls.
Conclusions
Our results suggest that evaluating combined measures of abdominal obesity and muscle strength may be useful to identify older adults who have a greater chance of both single and recurrent falls. These individuals can be easily identified using non-invasive, low-cost, and easily performed measures in clinical practice as well as in population-based surveys, based on the measurement of WC and handgrip strength.
In addition, given the growing population of older Brazilian adults, interventions aimed at reducing the prevalence of abdominal obesity and improving muscle strength may be able to reduce the incidence of future falls and mitigate the burden associated with falls.
Footnotes
Acknowledgements
Author’s Contribution
Design, analysis, data interpretation and final article writing: JSCA. Planning, design, critical review and final article writing: MANS. Data interpretation, critical review and article writing: TSA, ROM, MRP. All authors have approved the final version of the manuscript and assume public responsibility for its content.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The ELSI-Brazil baseline study was supported by the Brazilian Ministry of Health (DECIT/SCTIE – Department of Science and Technology from the Secretariat of Science, Technology and Strategic Inputs (Grant 404965/2012-1); COSAPI/DAPES/SAS – Healthcare Coordination of Older Adults, Department of Strategic and Programmatic Actions from the Secretariat of Health Care) (Grants 20836, 22566, and 23700); and the Brazilian Ministry of Science, Technology, Innovation and Communication.
Ethical Approval
This current project received ethics approval at two levels. Consent to participate was obtained for all participants under the ELSI-BRASIL ethics process approved by the Research Ethics Committee of the Fundação Oswaldo Cruz.
Informed Consent
Written informed consent was obtained from all ELSI-Brasil participants prior to enrollment.
