Abstract

Introduction
Sex- and gender-related differences in access to home dialysis, as well as disparities in kidney disease outcomes, have been consistently reported in numerous population-based and epidemiological studies. 1 Historically, the terms sex and gender have been used interchangeably in registries and large clinical trials, potentially obscuring important biological and sociocultural distinctions. In this editorial, sex refers to biological characteristics determined by genetics, chromosomes, gonadal anatomy, and sex hormones, whereas gender encompasses socially constructed identities, roles, behaviors, and societal expectations. 2
The mechanisms underlying sex-related differences in kidney disease outcomes have been investigated in multiple studies, particularly animal models, and have been linked to factors such as sex hormones and hemodynamic differences. Estrogen has demonstrated antifibrotic and anti-apoptotic effects in several organs, including the kidneys, heart, lungs, and liver, and these protective effects may also extend to the peritoneal membrane. 3 In addition, premenopausal women exhibit higher nitric oxide levels than men, which may contribute to more favorable hemodynamic effects on kidney function.1,4 Among patients receiving PD, anatomical differences between males and females may predispose sex-specific complications related to PD catheter placement, as well as differences in infection rates, which could further influence clinical outcomes. Moreover, as evident in this issue of PDI, issues related to future fertility, pregnancy planning, and pregnancy-related complications are an important part of care of females receiving PD.5–8
However, sex-based differences extend beyond biological mechanisms and encompass disparities in healthcare access, sociodemographic characteristics, cultural norms, attitudes toward illness, and the potential misinterpretation of study findings. In a survey of 51 nephrologists from 22 countries assessing sex disparities in kidney disease, females were more frequently identified as caregivers for partners receiving home dialysis or managing medications and were more likely to prioritize family health over their own. 9 Access to healthcare also differs by sex and varies across countries and cultural contexts. In some settings, females experience reduced access to healthcare services and fewer opportunities compared with males, whereas in countries such as Canada, females appear to access healthcare more frequently than males.9,10
Understanding variability in outcomes by sex and identifying the factors that contribute to these disparities are essential for improving PD-related outcomes, expanding access to home dialysis therapies, and enhancing the quality of care while addressing barriers faced across sexes. Although challenging, examining the association between sex and clinical outcomes—including survival, optimal dialysis, and PD discontinuation—while accounting for sociocultural, structural, and other confounding factors is essential and should be an integral component of any study aiming to elucidate these relationships.
When examining differences in PD clinical outcomes between males and females, it is essential to critically explore the underlying reasons for these differences rather than merely labeling observed associations without in-depth analysis. Recent studies have increasingly investigated the role of sex in peritoneal dialysis outcomes, including patient survival, transfer to hemodialysis, infection-related, and in-hospital outcomes.
Patient survival
Previous studies examining mortality among dialysis patients have yielded mixed results. Lim et al. 11 investigated incident dialysis patients in Australia and New Zealand between 1998 and 2018, including approximately 28% treated with PD, and evaluated both cause-specific and all-cause mortality among males and females. The study reported higher mortality among females during the first five years after dialysis initiation. This excess risk was primarily attributed to infections and dialysis withdrawal, whereas cardiovascular-related deaths were more common among males. In contrast, a recent analysis from the Peritoneal Dialysis Outcomes and Practice Patterns Study (PDOPPS) demonstrated that females, who comprised approximately 43% of the study population, had lower mortality, reduced rates of transfer to hemodialysis, and a lower risk of peritonitis compared with males. 12 Similarly, analyses from a study by Sabanayagam et al., including incident dialysis patients using data from the Australia and New Zealand Dialysis and Transplant Registry (ANZDATA), as well as studies from South Korea, suggested a trend toward lower mortality among female patients on PD compared with males.13,14
These findings should be interpreted with caution, given the influence of multiple confounding factors that may explain variability in outcomes. For example, in the study by Albakr et al. using the PDOPPS database, 39% of residual urine volume data were missing, which represents a significant limitation in light of the accumulating evidence supporting the role of residual renal function in survival and PD discontinuation. 15 Comorbidities such as diabetes and cardiovascular disease—which are more prevalent among males 16 —also had a substantial impact on survival and mortality in patients on PD, independent of sex, as demonstrated in the ANZDATA study by Sabanayagam et al. In addition, other factors, including serum albumin levels, malnutrition, and body mass index, were independently associated with mortality differences between males and females in Korean dialysis patients in the study by Jung et al. 14 Moreover, background sex-specific mortality differences in the general populations of the countries studied may contribute to observed disparities in dialysis survival and should be systematically examined and accounted for in future analyses. Collectively, these observations underscore the need for caution when interpreting sex-based differences in PD outcomes.
Transfer to hemodialysis (HD)
A major challenge for patients receiving PD is prolonging time on therapy while maintaining quality of life. Infection-related complications and insufficient dialysis remain among the leading causes of transfer to HD. 17 Pregnancy represents an additional consideration, as patients who are pregnant receiving PD often require transition to HD to achieve improved solute clearance and optimize fetal outcomes. 18 Recent studies from multiple countries, including Taiwan, New Zealand, the United States, and France, have consistently demonstrated lower rates of transfer to HD among females compared with males.12,19,20
This observed difference may not solely reflect biological sex effects but is likely influenced by non-biological factors as well. Males are more likely to rely on caregivers for PD, which may increase vulnerability to caregiver fatigue and burnout, potentially contributing to transfer to HD. 21 Conversely, females may be at higher risk for certain forms of PD discontinuation related to anatomical factors, including PD catheter dysfunction and gynecologic or urologic infections. Interestingly, despite these biological risks, the rate of transfer to HD among females has been low in many studies, suggesting that non-biological factors may play a significant role in observed sex differences.
Another non-biological determinant of transfer to HD is the reliance on Kt/V as a measure of dialysis adequacy. Because males generally have a larger volume of distribution, Kt/V may underestimate solute clearance in this group, potentially contributing to higher rates of perceived “inadequacy” and subsequent transfer to HD. 13 Although Canada and several other countries have moved away from using Kt/V as a strict treatment target, it remains widely used in many regions worldwide. Notably, recent International Society for Peritoneal Dialysis recommendations emphasize high-quality, goal-directed PD rather than a sole focus on solute clearance. 22
Further insight into non-biological contributors to transfer to HD comes from a recent study by Sabanayagam et al. using ANZDATA registry data. Among approximately 9700 incident patients who selected PD as their initial modality, male sex was associated with a higher hazard of PD discontinuation and transfer to HD compared with females. However, nearly 77% of the excess risk of PD discontinuation and 25% of the excess risk of transfer to HD were attributable to factors other than sex, particularly diabetes, cardiovascular disease, and smoking. 13 These findings highlight the importance of accounting for comorbidity burden when interpreting sex-related differences in PD outcomes.
Exit site infection and peritonitis
Infectious complications and their prevention remain a major focus in peritoneal dialysis, given their substantial impact on infection rates and overall PD outcomes. In a retrospective study by Hannah et al., published in this issue of PDI, sex differences in exit-site infections (ESIs) were examined over a 12-year period, with no significant differences observed between males and females. 23 Rates of ESI-associated peritonitis and catheter removal were also similar between sexes, and among ESIs that progressed to peritonitis, 49% of cultures yielded Gram-positive organisms.
In contrast, data from the PDOPPS cohort demonstrated lower rates of peritonitis among females compared with males, with a corresponding reduction in Gram-positive peritonitis. Similar findings have been reported in previous studies. 12 While these differences may partly reflect biological variation in innate and adaptive immune responses—including the influence of sex hormones on infection susceptibility 24 —the lower rates of Gram-positive peritonitis in females may also involve non-biological factors. One potential explanation is that females may achieve more consistent use of exit-site prophylactic antibiotics and maintain more meticulous hygiene practices, which could help reduce contamination and subsequent infection.
In-hospital outcomes
Thongprayoon et al. recently examined the association between sex and in-hospital outcomes among PD patients in a study published in this issue of PDI, including PD-related complications (such as peritonitis and mechanical issues), non-PD-related outcomes, mortality, and transfer to HD, in hospitalized patients between 2003 and 2018. Overall, no significant differences were observed between sexes. However, subgroup analyses showed that females younger than 60 years and those without heart failure or peripheral vascular disease had lower rates of transfer to HD and fewer PD-related complications. In contrast, females older than 60 years with heart failure had higher odds of PD complications. These findings may reflect non-biological factors, such as a more conservative management approach in younger females and lower baseline clinical severity in younger, healthier patients, which may not extend to older females with multiple comorbidities. 25
Is it just biology?
Despite the recent extensive efforts to elucidate the role of sex in dialysis outcomes, many aspects of this relationship remain incompletely understood. While certain differences may be attributed to genetic and hormonal variation between males and females—potentially influencing immune responses and reactions to therapeutic interventions—biological factors alone are unlikely to fully explain the observed disparities. A broader range of considerations must be incorporated to ensure findings that are both equitable and truly representative (Figure 1).
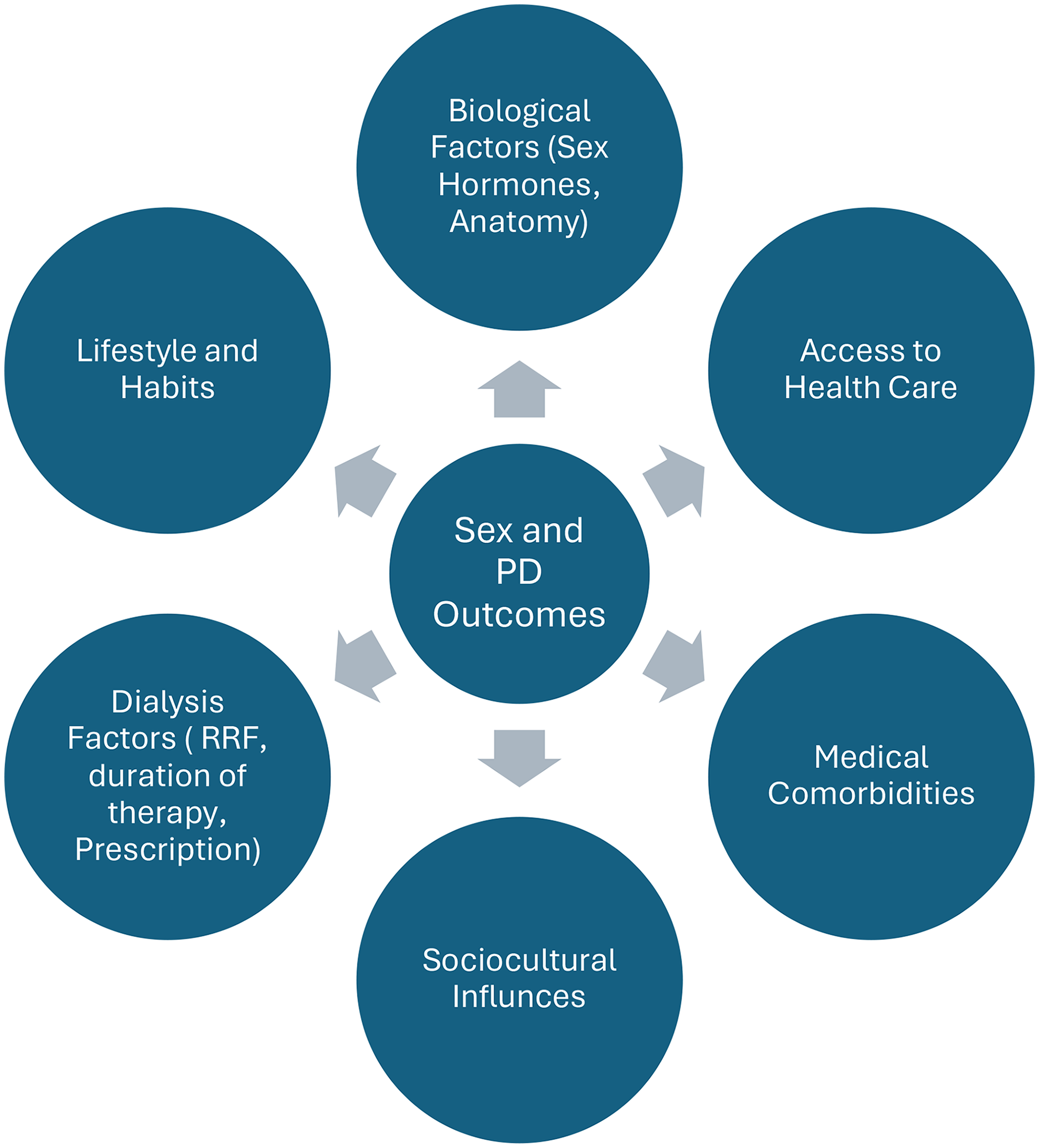
Potential mechanisms underlying sex differences in peritoneal dialysis outcomes. Sex-related differences in peritoneal dialysis outcomes are likely driven by a complex interaction of biological, medical, dialysis-related, and sociocultural factors, as well as disparities in access to health care. These domains may act independently or synergistically to influence patient survival, rate of transfer to hemodialysis, Peritonitis episodes and other PD-related outcomes. PD: Peritoneal dialysis, RRF: Residual renal function
Historically, sex disparities have been understudied and underappreciated, limiting our understanding of the relationship between sex and kidney disease outcomes, as well as the role of sex hormones in the pathogenesis of diseases leading to kidney failure. In the dialysis literature, the terms “sex” and “gender” have often been used interchangeably, a practice that may obscure true associations and reduce the generalizability of study findings.
In a meta-epidemiological analysis, Davids et al. evaluated how sex- and gender-related concepts were incorporated into randomized controlled trials (RCT) published in high-impact journals involving adults with kidney failure receiving dialysis. 26 Among 561 included RCTs, sex and gender representation were comparable to observational data from DOPPS; however, reporting of both sex and gender was infrequent, and most trials did not include either variable in analyses or outcome reporting. Similarly, in a meta-epidemiological study of phase II and III RCTs conducted in Canada between 2010 and 2019, none of the 118 trials reported both sex and gender variables. 27 Incorporating both sex and gender into clinical trial design and reporting is essential to better reflect real-world populations and improve the interpretability and applicability of research findings.
Moreover, before attributing kidney disease-related outcomes solely to biological sex, comparative studies should account for behavioral, social, and cultural factors that vary across regions and countries. In many societies, females are more likely to prioritize family caregiving over their own health and may avoid imposing perceived financial or emotional burdens, whereas males often have greater access to caregiving support. 9 Cultural norms related to decision-making, financial constraints, societal expectations, lifestyle, diet, and attitudes toward treatment may further influence outcomes, particularly among females. Although adjustment for these factors is challenging, it is essential for accurately interpreting sex-related differences in outcomes and underscores the importance of mixed-methods and qualitative research in elucidating the sociocultural influences on PD outcomes.
Conclusion and call to action
Moving beyond a purely biological framework toward a patient-centered approach that integrates social, cultural, and healthcare access factors—while clearly distinguishing between sex and gender and ensuring appropriate representation in clinical trials—may improve our understanding of sex-associated disparities in PD outcomes.
Future research should prioritize sex- and gender-equitable study design, recruitment, and access to care to better inform clinical practice. Clinical trials investigating sex differences in PD outcomes should incorporate not only key clinical variables—such as residual kidney function, dialysis adequacy, comorbidities, and laboratory parameters—but also comprehensive sociocultural and demographic factors to capture the full range of influences on patient outcomes.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
