Abstract
Suicide rates have increased among Black youth. Caring contacts can decrease adult suicide reattempts and rehospitalizations and may be both acceptable and scalable among adolescents. We assessed the experiences of Black adolescents visiting an emergency department (ED) for suicidal thoughts and/or behaviors and their perceptions about a caring contacts intervention. We used a qualitative thematic analytic approach to generate key findings from 10 in-depth interviews with patients and/or their parents after ED discharge. Black adolescents experienced lacking ED-based therapeutic interventions, family-inclusive services, and orientation to future steps. Participants perceived caring contacts as an acceptable, developmentally and culturally appropriate postdischarge intervention.
Adolescent suicide has experienced a steady rise in the last 2 decades. In 2023, suicide was the second leading cause of death in youth aged 10 to 34 years (Centers for Disease Control and Prevention [CDC], 2023; Ivey-Stephenson et al., 2020). Among Black youth between 5 and 18 years of age, suicide moved from ranking as the fifth in 2008 to the third leading cause of death in 2018, increasing at a higher rate than in other racial or ethnic groups. According to student self-report survey data, Black high schoolers are considering suicide, making a suicide plan, or attempting suicide at higher rates than a decade ago (Centers for Disease Control and Prevention, 2024). Additionally, suicide rates in Black youth younger than 13 years were double those of White peers. These facts call for culturally informed and developmentally tailored prevention efforts (Bridge et al., 2015, 2018).
Other studies have found higher rates of discharge home from the emergency department (ED), lower inpatient admission rates, and less recent suicidal ideation (even when they had similar rates of lifetime suicidal attempts) among Black youth ages 8 to 12 compared with other racial groups, highlighting the importance of improving interventions delivered in the ED (Vidal et al., 2023). Older adolescent Black males with a disruptive behavior are more likely to present with a chief complaint not related to suicide but screen positive on the Ask Suicide-Screening Questions (ASQ) (Horowitz et al., 2012). These findings suggest potential racial differences in the presentation of suicidal behaviors (Cwik et al., 2021). Additionally, Black youth present higher need than actual use of mental health services, and their barriers to access are understudied (Planey et al., 2019).
Between 2011 and 2020, emergency services utilization for mental health reasons in youth doubled overall, and there was a 5-fold increase in suicide-related ED visits (Bommersbach et al., 2023). Yet, EDs are often underequipped to handle these mental health emergencies. In a study of mostly Black pediatric patients presenting for a mental health emergency and at risk for suicide who boarded in an ED for more than 24 hours between 2015 and 2018, only half were evaluated by a psychiatrist and received treatment recommendations, and close to one out of five of those patients for whom hospitalization was recommended were ultimately discharged home. Additionally, one fourth had a subsequent ED encounter for mental health concerns (O’Donnell et al., 2020). Given that at-risk children are all eventually discharged home and do not reach specialty psychiatry units, ED-based behavioral interventions and chain-of-care approaches that effectively bridge ED and inpatient units with community-based mental health care are needed.
There is a heightened risk of suicide attempts during the first month of treatment initiation among individuals at high suicide risk (Brent et al., 2009), suggesting a need for time-sensitive and front-loaded interventions. One potentially effective method for reducing suicide attempts after hospital discharge following a suicide emergency is a caring contacts intervention. Caring contacts are nondemand messages of hope and resilience delivered after discharge that have been shown to reduce subsequent suicidal behavior. A systematic review and meta-analysis of caring contacts for suicide prevention yielded 13 articles (Skopp et al., 2023). Although most studies reported on quality improvement projects, promising data show acceptability of caring contacts in adolescents (Thomas et al., 2024). The caring contacts intervention is a relatively easy-to-deliver clinical intervention with potential to prevent suicide, but research on this intervention in adolescents is limited, and its applicability in minority populations is poorly understood.
The objectives of this study were to better understand the perceptions of mental health services among Black adolescents with a visit to the ED for suicide-related thoughts or behaviors along with their parents’ experiences, regardless of subsequent disposition to psychiatric inpatient care or to home, and to explore the acceptability and feasibility of a text-based caring contacts intervention to inform its cultural adaptation.
Methods
We conducted an exploratory study with qualitative data consisting of in-depth interviews. Participants were patients recruited from the pediatric ED and the psychiatric inpatient unit of an urban tertiary hospital in the U.S. Mid-Atlantic region. All patients are administered the ASQ (Horowitz et al., 2012), a well-validated suicide screener, by nursing staff. Electronic medical records of 12- to 17-year-olds seen in the ED were reviewed by the research team. Eligible patients and their parent/guardian were approached and given information about the study. If inclusion criteria were met and the patient and parent agreed to participate, they were contacted after discharge to obtain informed consent and schedule an interview.
Inclusion criteria were (a) a patient aged 12 to 17 years or the parent of a patient; (b) Black or African-American race; (c) ability to read and write independently; (d) admitted to the ED with a plan for discharge to the psychiatric inpatient unit or home; (e) having completed an ASQ screen and scored positive on questions 1, 2, 3, and/or 5 and/or having a presenting concern of suicidal ideation/attempt; (f) giving assent and having a parent/guardian who gave consent to participate in the study; and (g) having access to a smart phone. Exclusion criteria included disorders with functional impairment that could interfere with the review process, such as (a) being acutely suicidal or homicidal with imminent plan to hurt oneself or others; (b) presenting psychotic symptoms; and (c) having a neurodevelopmental disorder limiting communication and ability to participate in the interview assessment. Parents/guardians of study-eligible adolescents who gave consent for participation were eligible for inclusion. Each participant received a gift of $50 for participating in an in-depth interview. The Johns Hopkins University School of Medicine IRB approved the study.
An interview guide developed by the study team contained questions about the patients’ visit to the ED for a mental health crisis (supplemental material). The first set of questions asked about the ED experience, including what the patients thought would have been helpful, the obstacles they had experienced in the past when trying to obtain mental health help, their experience after discharge from the hospital, and the overall hospital experience based on their cultural background. Participants were then shown an example of the caring contacts intervention currently in use in another pediatric hospital system and were told that the intervention would be delivered following discharge through a series of text messages that they would receive at regular intervals. They were asked their thoughts about the intervention, including its perceived value format (text vs. phone call, letter, postcard, videos, email, or social media-based messages), content (images, and text), and duration. They were also asked about other interventions that would be helpful at discharge and ways to engage them after their discharge home.
A total of 10 interviews were conducted with the patient alone, the patient’s parent alone, or both the patient and the patient’s parent together. Participants included 8 patients discharged from the ED and 9 parents who agreed to be contacted for an online (zoom-based) interview. Participants were interviewed between April 2023 and November 2024. Patients’ age ranged from 14 to 18, with a mean age of 16.2 years. There were 9 females and 1 male (Table 1). Interviews were conducted by a research assistant, an undergraduate student, and a pediatric psychiatrist using the interview guide and were audiorecorded and transcribed.
Interview number, patient’s sex at birth, and interviewee’s identifiers.
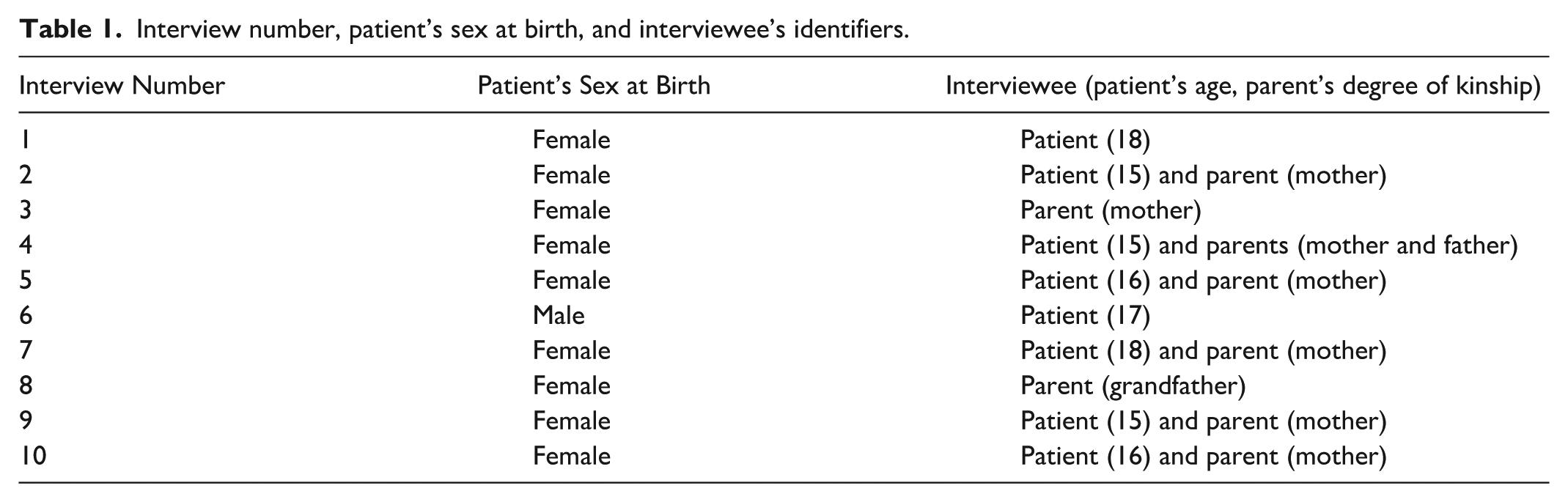

The interviews with patients and parents explored perceived barriers to traditional outpatient services and the appropriateness of the caring contacts intervention for Black youth. Interviews ranged from 45 to 210 minutes in duration. Study team members coded the interviews separately and met on seven occasions between May 17, 2024, and March 6, 2025, to discuss the codes and overarching themes. We followed a qualitative inductive thematic analysis of the transcribed study interviews (Naeem et al., 2023). Team members selected key statements and quotes separately, and these were grouped into codes after discussion and agreement during team meetings. The codes were grouped into themes as described below. Interviews were conducted until information saturation was achieved. Information saturation was decided by the coders by consensus when no new information was gained from the interviews. We propose a conceptual model of experiences across the continuum of care for Black youth presenting to the ED with suicide emergencies.
Results
Study participants’ characteristics are displayed in Table 1. Selected quotes reflecting each of the general themes and subthemes are displayed in Table 2 (preadmission, emergency department experience, inpatient experiences, postdischarge), Table 3 (caring contacts), and Table 4 (general experiences across services). Themes and codes are explained below. Figure 1 shows the themes and the role of caring contacts in the continuity of care.
Preadmission, Emergency Department, Inpatient Unit, and Postdischarge Perceptions.

Caring Contacts.

General Experiences Across Services.

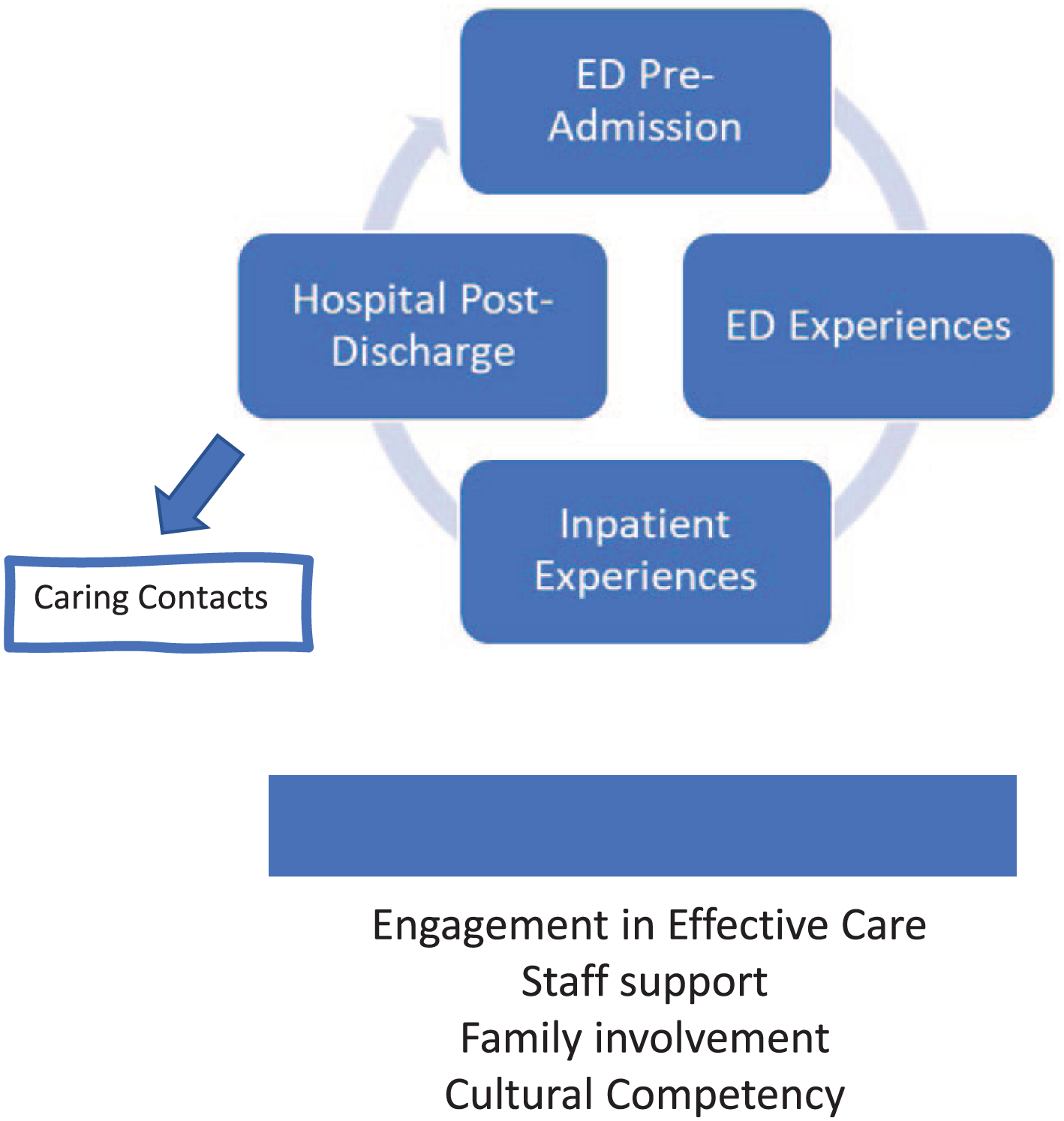
Caring contacts interventions in the continuum of care. ED, emergency department.
Preadmission
The ED was sometimes the first point of contact with mental health services after a suicide-related emergency, but some participants reported contact with professional mental health services and informal support prior to arriving to the ED. This support was often provided at school. Barriers to accessing care included dissatisfaction with the type of care delivered and the relationship with the healthcare provider.
Formal and Informal Support Prior to the ED Admission
Participants received both formal and informal support prior to admission.
Role of Schools in Preadmission
Schools had a role in mental health prior to admission. They could be a source of stress but also a source of referral to services, specifically to the ED. Participants explained disclosing suicidal ideation to school staff who would then refer them to the ED for an evaluation.
Barriers to Mental Health Care Prior to ED Admission
Barriers to receiving mental health care prior to ED admission included parents’ responsibilities with other siblings and the need to navigate outpatient services. Even when outpatient services were available, access challenges could be present, such as fragmented or ineffective services, changes in provider, and failure to address problematic behaviors (e.g., disruptive behaviors). Oftentimes, the provider-patient relationship was inadequate or the patient felt uncomfortable or perceived the provider to be biased. Other barriers related to the provider included poor or insufficient engagement and need for more flexibility. Participants expressed needing to “feel heard and respected,” to balance autonomy with harm-risk reduction in therapy in order to build trust, and to have more choices (e.g., patient directing content in therapy sessions, combining apps and in-person interaction). One personal barrier mentioned was “downplaying struggles, and thinking others had it harder,” which made the person think, “Do I really need a therapist or am I just being sensitive and emotional?”
Emergency Department Experience
Mechanisms of Referral and ED as First Mental Health Contact
The ED could be the first patient’s contact with mental health services. At times, the patient had not sought mental health support due to not knowing how to communicate feelings to adults. In addition to voluntarily requesting to be evaluated or calling the suicide hotline, referral to the ED could be initiated by the school or by an emergency petition. The participants interviewed had had positive experiences with police before being sent to the ED during emergency petitions and noted that police and the ED staff worked well together: “Everybody [was] doing their due diligence.” Calling an ambulance was seen as the only option when the patient was having a “meltdown.”
ED Expectations and Experiences
Participants perceived the ED to be a “bedspace,” or a place to wait for inpatient admission, and wished for more activities to be available so that it was not just “a passing time” place. They felt they had to wait for too long to be seen. For those visiting the ED for the first time, some experiences were fear-provoking. Participants expressed uncertainty about what to expect and wanted to be warned about the inpatient experience to help transition services. Participants suggested clinicians should approach them by providing comfort first and then asking questions; otherwise, the evaluation felt “like an interrogation.” Some participants personally experienced feeling “numb” and “out of it” during their ED stay (e.g., one participant remembered their experience as “a big blur” in the context of an overdose-related seizure). The intake process was perceived as efficient and nonjudgmental. The provision of transportation to families who otherwise could not have visited the patient was appreciated. Some parents expressed that the setting was patient-centered but not family-inclusive. They understood that the ED’s goal was to keep patients safe but did not feel enough emotional support was provided. Conversely, other parents felt supported by staff and that they received the “best care” possible given the circumstances.
Therapeutic Interventions in the ED
Overall, there was a perception of a need for therapeutic mental health interventions in the ED. The ED was seen as a place “to get away” where patients were “doing nothing, but eating, watching TV, and sleeping” [Interview 1]. During their stay in the ED, participants used a mobile app with breathing exercises that was perceived as helpful. Some participants proposed using well-designed applications that could potentially be less triggering than a staff member who had not been well-trained, stating that “you never know who you are dealing with” as “nurses are always switching.” Brief visits for less serious issues were seen as a good alternative to prolonged ED stays.
Staff Support in the ED
Having someone to talk to other than nurses or doctors, without that person needing to have too much professional training, was seen as an option to improve communication with the patient. Parents also expressed a need for support, either with chaplains or other professionals, given the stress of dealing with a child with a mental health emergency.
Physical Environment in the ED
The ED was perceived as physically comforting. Nursing staff would provide comfort by bringing chairs for the parents to sit on. However, the psychiatric space was seen as “sterile,” not colorful, and “plain” (“white blanket and a bad pillow”). Participants appreciated the TV and other entertainment provided in the ED. Having a sitter (or a one-to-one support staff) and security could be perceived as supportive and gave a sense of safety. For others, the presence of a security guard was “scary.”
Inpatient Experiences
Patient Personal Experiences Participants perceived their inpatient unit stay as “taking a break from outside.”
The experience varied from the one in the ED. Although there were therapeutic groups, some participants expressed being “triggered” in groups. They perceived having little interaction with the outside world, and this perception was true even for one patient who had had daily interactions with friends and family while admitted.
Therapeutic Interventions in the Inpatient Unit
The psychiatric inpatient hospitalization in this particular hospital was seen as useful. However, some patients had felt neglected in other inpatient units (i.e., parents not being contacted right away after an episode of self-harm, or staff not tending the patient’s wounds quickly enough, expressed as “eventually they tended to my wounds”). The therapeutic groups (which in this unit included psychoeducation, dialectical behavioral therapy, and occupational therapy groups) were perceived as “repetitive.” Groups about coping skills were not always seen as helpful, and a participant expressed that “coping skills are overrated.” Others saw suicidal thoughts as temporary, or negative thoughts that “just pop up, and they’ll go away quickly as soon as I calm down,” and appreciated the role of coping skills in overcoming moments of distress that triggered suicidal thoughts. Another issue related to the inpatient stay had to do with handling controversial topics. A patient expressed feeling that it was important to shut down talks about religion that made her feel uncomfortable. However, others brought up a desire to discuss more in-depth topics and share more personal stories, using warnings to avoid triggering others, or focusing on certain symptoms of depression (e.g., hygiene habits, healthy relationships, self-care and “self-love,” mental health conditions, and/or how to communicate with family members). Patients also had a desire for more groups that were directed by the children. For some, the hospital stay was validating and helped them understand the need to accept help for mental health issues. Learning to communicate with parents and hearing the stories of other people were helpful. Medication changes were not always seen as helpful as “venting or talking” to supportive staff and peers in groups.
Preparation and Communication With Out-of-Hospital Support
There was an understanding of the need to prepare for discharge. Transitioning from the inpatient unit back to school after hospitalization could be difficult after being absent for some time. Participants found it difficult to explain the hospital stay to family and friends, and some perceived that “once you are released, there’s not that much more the hospital can do for you.” A common theme was the hospital’s staff communication with the family. Parents wished for more communication about the postdischarge treatment plan throughout the admission and not just at discharge. At the same time, others perceived the hospital team to have communicated well with family and other providers. Family visits and phone communication with family outside of the hospital facilitated by staff made some patients feel more supported. Some patients expressed a desire to have social media access and more phone time during their hospital stay.
Postdischarge
Referrals and Follow-up
Although postdischarge outpatient appointments and resources were consistently provided for the patients, there could be gaps in treatment due to difficulties accessing those programs, the caregiver not receiving the discharge paperwork, the patient running out of medications before seeing the outpatient provider, or having inappropriate or inconsistent therapy after discharge. Telehealth visits, quarterly follow-up visits, house visits, and phone calls were seen as options to stay connected with the hospital after discharge and cover gaps in the continuum of care. Intensive outpatient postdischarge treatment and group therapy-based programs were considered advantageous. Some parents expressed a desire for referrals and information about pediatric mental health for themselves and other family members, like the patient’s siblings (e.g., support for parental trauma, a phone number to call, and guidance on how to act or talk with a child with a mental health disorder). Being able to look up the next appointment in the system when services were within the same system made transitions smoother. Having flexibility in the frequency of visits depending on the patient’s need was suggested as a solution. Some perceived follow-up to be appropriate.
Postdischarge Personal Support
Informal supports such as grandparents picking up after discharge or attending church were described by a participant as “chicken noodle soup for the soul.” Suggestions were made to support families of children with mental health crises (e.g., a support group for families, orientation for parents who may disagree on how to support the patient, or a social media or online support group for parents). Hotlines were perceived as helpful “because they can be anonymous and are free.”
Barriers to Access Postadmission and Readmission
Even when given resources, participants sometimes perceived the paperwork and information to not be straightforward. Additionally, school and work schedules could get in the way of attending scheduled outpatient visits. For those with repeated readmissions, there was a gained understanding of the processes of admission.
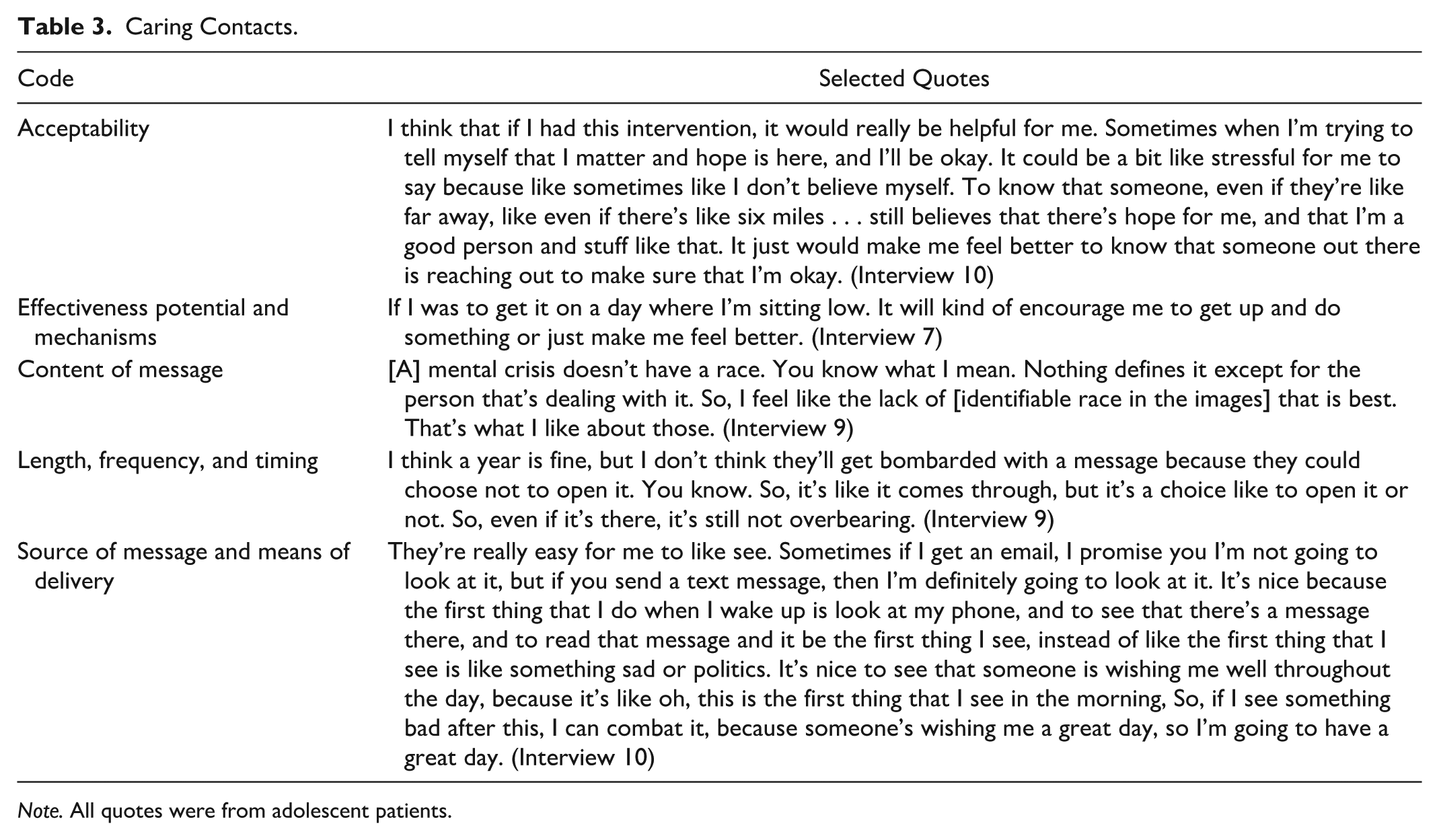
Caring Contacts
Acceptability and Effectiveness of Caring Contacts
Participants unanimously perceived caring contacts text messages to have the potential to be helpful. Participants felt that these messages were a “generous” gesture that could be helpful “when you are having a bad day.” The messages gave the impression that the system was organized. Patients believed the messages could be helpful for parents as well.
Effectiveness Potential and Mechanisms
The messages could be helpful by making patients and family feel like “someone cares” and was thinking of them that day, and as a reminder of the hospital stay and the need to care for one’s mental health. The messages were also a way to stay connected to people in the inpatient unit. The messages would give patients motivation to keep working and taking small steps. The messages provided patients an opportunity to discuss the content of the text message with the parents. Finding motivational images online was different than receiving a message from the hospital because there was a personal connection involved, even when the messages were one-way. Text messages were not perceived as intrusive because patients did not have to open or read a message and could opt out.
Content of Message
The content shown was perceived as age-appropriate. Some suggested that content and image preferences may vary by individual and gender (“sportier”). The messages were perceived as racially inclusive. One person thought more local sites were more relatable (e.g., city landmarks), but overall, a variety of content was preferred. Participants emphasized the importance of providing the suicide prevention phone line number and highlighting that the text messages were not monitored so people did not feel unsupported if there was no response. The images accompanying messages were perceived to be powerful because they evoked pleasant situations. However, a variety of opinions were expressed regarding the images. Some participants thought that earthy images (i.e., butterflies, water, animals) were calming. Images with cartoons and hand-drawings were well-liked, including those with emojis. Images of celebrities were not preferred by most participants. Some mentioned preferring images that did not involve reading. Others mentioned the potential of having personalized images that included the interests or preferences of the specific patient or images that varied by age (i.e., more colorful images and more drawings for younger adolescents and more real-life images for older adolescents). Images that were racially ambiguous were seen as positive because “mental health crisis doesn’t have a race.” Opinions varied regarding the text content of messages. Content that was informational and encouraging was welcomed. Some parents wished to have more text (“longer phrases”), whereas patients generally preferred shorter quotes. Patients also emphasized the need to have a nonemergency contact number in addition to the crisis number because calling the suicide line “may be intimidating.”
Length, Frequency, and Timing
The preferences on the timeframe of message, or how frequently or for how long the messages should be sent, varied among participants. There was a preference for frontloading of the messages. Half a year or a year of duration was considered acceptable. Overall, length was not viewed as a concern as long as one could opt out. Some preferred longer periods, as “it takes time to heal.” Preferences regarding the timing of the text message delivery also varied. Some preferred to receive text messages after school as they did not check messages in the morning, whereas some parents thought it was best for patients to receive messages in the morning upon awakening, so the patient would see the text message before the news and “before bad things happen.”
Source of Message and Means of Delivery
As a means of message delivery, participants preferred text-based caring contacts over social media. They believed that social media was good for awareness and outreach but was “less personal.” Text messages could also be kept and reread at a later time, whereas social media sites such as Snapchat did not allow that. Additionally, not everyone uses the same social media sites, which would make it harder to reach all patients seen at the hospital compared with using personalized text messages sent to a patient’s phone number. Phone calls were perceived as intrusive. One patient preferred postcards, which could be physically held and kept. The source of message also mattered. The fact that the messages were coming from the hospital made them seem more important (“hospitals save lives, they matter”). Some participants mentioned that it did not matter who sent the message, “as long as it is not a robot,” and admitted that a staff member sending them would be better and that it “would be nice for the people who treated you to see how you’re doing” (Interview 1). Peers sending messages could be supportive and use humor but could also “bring them [the patients] down” and were perceived as less motivational.
General Experiences
Staff Support in the Hospital
Talking to nurses, social workers, occupational therapists, and other staff was helpful. At times, participants perceived nursing staff to be more engaged and occupied with other staff members and health-related tasks (e.g., taking vital signs) than with the patients themselves. Participants emphasized the need for informal support within hospital. This support could be provided by a nonparental, trusted adult figure. Having a comfort object during their stay was also appreciated. Some patients wished for staff expectations to be dependent on the patient’s maturity and functioning level (i.e., approaching those with disruptive behaviors differently than those with internalizing disorders). Although aware of the challenges, patients also saw potential in balancing structured and unstructured time to be able to socialize with peers. Some parents expressed a need for someone to check on them in addition to checking on their child. One parent expressed that “nobody asked us how we were doing, you know, and I think that is important because I wasn’t doing too well” [Interview 4].
Family Perceptions of Mental Health System
Gaining experience with the system was valuable to families as they became more aware of how to navigate health care institutions and programs. A family mentioned that they expected the system to be “ready for you, as opposed to the other way,” but with experience, they had learned to advocate for their own family instead of focusing on the system’s failures. Parents’ perceptions of their children’s mental health status and hospital experiences varied. Some parents saw the ED visit as unnecessary. Some thought the patient was asking for attention or that the symptoms were related to “bad” behavior, whereas others thought the child was minimizing symptoms or traumatic experiences (e.g., sibling dying). For some parents, it was traumatic to have a child with a mental health crisis and not know what to do during a suicide emergency. Parents’ reactions to the child’s mental health crisis included surprise, grief, anxiety, and even fear when medical complications arose (e.g., during an overdose-related seizure). One parent recalled the experience of the patient’s hospitalization, saying, “I called the crisis unit because she was threatening to kill herself. . . . I didn’t have knowledge of what to do . . . [there is a need to be] more aware of what is out there in order [to] help teens that are going through things” [Interview 9, Parent].
Need for Family-Inclusive Services
Perceptions about family inclusion in care varied by service and personal experience. There was a need for age-appropriate services and different degrees of family involvement as the child matured. Although understanding that during adolescence there was an emphasis on autonomy and confidentiality, parents desired continued involvement in treatment, and this desire varied by family unit and cultural background. Even with adolescents, the separation from the child and the parent during the admission was challenging.
Barriers to Engagement in Effective Care
Participants often mentioned experiencing gaps in continuity of services. They believed text messages and other technologies could help maintain a connection with the therapist between sessions and before admission to, or after discharge from, the hospital. Some mentioned preferring to continue treatment with the hospital team as opposed to being referred to “random people.” They also saw a need to stay connected when changing schools or when not attending school while they were hospitalized (for school-based providers). Admissions to different hospitals and across states made the process of getting care difficult and stressful. This lack of continuity contributed to readmissions. Another issue related to lack of continuity was the repetitive questioning between and within levels of care (from the ED to inpatient stay and to day hospital). Notwithstanding, transitions were easier within the same system of care, and continuity of care was more disrupted when discharging back to outpatient treatment.
Cultural Competency and Discrimination
Overall, participants experienced services as culturally competent. They did not feel discriminated against because of their ethnic or cultural background. However, as mentioned earlier, families of cultures that were more collectivistic (e.g., Central American background) expected more family involvement in decision making for their child’s treatment (Heu et al., 2019). This gap could be surmounted by asking families about their thoughts and knowledge about mental health, which effective therapists were already doing. Especially challenging were differences in acculturation between first- and second-generation immigrants. Some participants perceived that therapists of the same gender and racial background as the patient understood the patient better because they were thought to have had similar experiences (e.g., others can have “sympathy but not empathy”). There was a perception of retribution and discrimination experienced by some participants. A parent had felt fearful of being blamed for her child’s mental health crisis. A patient perceived staff as afraid of her, showing an offensive tone of voice, quickly sending her back to the room when she was stepping out, and being defensive. There was also a general distrust with the health system among some participants. For example, one parent did not want to sign forms to allow emergency treatment on admission even when she reported the overall experience to have been positive.
Discussion
This qualitative study of experiences of Black adolescents presenting to the ED with a suicide-related emergency identified barriers to accessing care before the ED visit and recognized a need for better youth and family orientation to mental health care, greater availability of brief therapeutic interventions and treatment planning in the ED, and more family-inclusive services. Even when outpatient services had been secured, there were gaps after discharge, especially when additional barriers such as referrals outside of the health system or state occurred. Text-based caring contacts were well-accepted and considered culturally appropriate, with varying opinions but overall acceptance of the images, text, informational content, and the frequency and timing of delivery. Parents expressed a wish to be included in the delivery of text messages. Overall observations across services suggested a need for formal and informal support as well as a better understanding of systems of care and barriers to engagement in effective care. Although there was a general sense that services were culturally sensitive and inclusive, some patients and parents did not feel understood by mental health providers, perhaps due to different cultural backgrounds and perceived provider bias, and some parents were concerned they would be judged for their child’s mental health problems. Finally, schools were a common source of referral to the hospital during suicide emergencies. This role of schools suggests a need to equip them with tools to better identify and mitigate risk through programming and staff training in order to reduce potentially traumatic ED visits (American Academy of Pediatrics, 2025).
A prior qualitative study conducted with a sample of largely White parent-child dyads of children hospitalized for suicide-related risk in 2019-2020 in North Carolina revealed commonalities with our sample (Salem et al., 2025). That study also noted a sense of disorientation, the feeling that confinement in the ED was “jail-like,” and a sense of connection with staff and peers during inpatient hospitalization and disconnection from the outside world. Participants in both studies experienced the inpatient hospitalization as removing them from stressors but expressed concerns about its usefulness. Parents in both studies also expressed concerns about being separated from their children and worries about being blamed for the child’s presentation. The study recommended the implementation of trauma-informed approaches that empower patients, offer choice and collaboration in treatment planning, and ensure physical and emotional safety in staff-patient interactions. Greater integration of the family into treatment was recommended, along with consideration of the stress they face. Emphasis was placed on psychoeducation, provision of referrals, and accommodations for barriers such as transportation, as well as a postdischarge process for patients and caregivers that includes opportunities to coordinate care and facilitate engagement in treatment. Some programs such as SAFETY-A and youth crisis stabilization units for youth who attempt suicide already implement family-centered models of care that ensure continuity of care and focus on comprehensive safety planning (Kodish et al., 2023). Our findings and those of Salem and colleagues (2005) suggest that Black and White contemporary adolescents present overlapping experiences with mental healthcare during suicide emergencies.
Our findings suggest that some of the interventions applied on inpatient psychiatric units might be productively added to services in the ED, particularly during longer hospital stays and given the current environment of increased demand for ED-based mental health services. Many patients delayed engaging in care due to an inability to communicate distress to adult figures or difficulties finding appropriate services, highlighting the need for accessible universal and community-based interventions that are easy to adopt and acceptable to all families. Additionally, participants expressed a desire for informal support that was validating. This is a challenge as many crisis-oriented circumstances call for active problem-solving to mitigate risk, whereas children may be looking only for validation and support. However, this research points to existing possibilities for nursing and allied mental healthcare personnel to extend their hospital-based suicide prevention role beyond the hospital by using caring contacts.
Regarding postdischarge text messages, study participants were shown a caring contacts intervention designed, piloted, and implemented by a large Midwestern pediatric hospital. The feasibility and acceptability of this intervention have been tested through a postintervention survey, showing that the majority of patients approached enrolled and completed the program (Thomas et al., 2024). Over 80% of the survey responders felt supported and more hopeful, thought their peers would be helped by the text messages, and would like to continue receiving them. Close to one out of five of these patients were Black, and although they were approached at significantly lower rates, they had similar rates of survey completion as other ethnicities. The perceptions of the patients in our study support the acceptability of this intervention among Black adolescents across states, and the findings from both studies suggest that caring contacts could be more regularly used with U.S. Black adolescent patients.
Participants were satisfied with the caring contacts images and preferred a diverse representation of interests, races, and genders. The potential for personalization of images both in terms of racial and gender identity, as well as personal interests, has exploded with the widespread use of artificial intelligence (AI). Some teams are currently training AI to tailor caring contacts using information from the patients’ electronic health records (Steinberg et al., 2025). This ability to personalize an accepted and effective intervention after discharge could contribute to youth suicide prevention efforts. However, teams should exercise caution given that current AI models may not be ready to craft specific images and messages with appropriate tone and imagery without clinical and research expert supervision. Additionally, it is imperative to ensure that messaging is consistent with suicide prevention communication best practices.
This study had several limitations. It was conducted in a single site. Experiences in other EDs and inpatient units may differ. The study did not include younger children. Youth with disruptive behaviors and more outward aggression may be more vulnerable to bias and negativity. There was only one male participant, limiting any conclusions made about males. This qualitative study examined patients’ perceptions, which may have been biased due to stress, depression, or temperament. Finally, although there is some evidence from pilot studies, quality improvement data, and qualitative research, more powerful research designs such as randomized controlled trials are needed to establish caring contacts as a useful intervention in preventing suicide among adolescents from racial minorities following hospital discharge after a suicide emergency.
In conclusion, Black adolescents attending a hospital due to a suicide emergency generally experienced barriers to maintaining continuity of care and found a caring contacts intervention designed with neutral and diverse images to be acceptable and potentially useful. More research is needed to prove this intervention’s effectiveness in reducing suicide risk among adolescents.
Supplemental Material
sj-docx-1-nsq-10.1177_08943184261425397 – Supplemental material for Experiences of Black Adolescents With Suicide Emergencies: A Qualitative Study Focusing on Continuity of Care and Acceptability of Text-Based Caring Contacts
Supplemental material, sj-docx-1-nsq-10.1177_08943184261425397 for Experiences of Black Adolescents With Suicide Emergencies: A Qualitative Study Focusing on Continuity of Care and Acceptability of Text-Based Caring Contacts by Carol Vidal, Jotrina Vamboi, Leticia Manning Ryan, John Ackerman and John V. Campo in Nursing Science Quarterly
Footnotes
Acknowledgements
The authors thank Elena Camacho, LSW, and Fatimah Masood, LSW, MPH, for the design and sharing of the caring contacts, and Elizabeth Reynolds, PhD, and Mimi O’Hara, MS OTR/L, for identifying and connecting the research team to potential participants in the inpatient unit.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the authorship and/or publication of this review.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. Vidal receives research funding from the NIDA/AACAP Physician Scientist Training Physician Scientist Program in Substance Use Career Development Award (K12DA000357) and program implementation funding from the Maryland State Community Health Resources Commission. This study was funded by a Johns Hopkins University Pediatrics Innovation Grant.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
