Abstract
In the United States, African American (AA) women suffer from higher rates of obesity as compared with Caucasians or Asians. Unfortunately, most weight management interventions have been unsuccessful in maintaining weight loss. Prior research has revealed that AA women face unique barriers in managing obesity; therefore, more research is warranted to address this problem. Leininger’s theory is used to understand obesity through a cultural lens. The constructs of the sunrise model are defined as a means to intervene when providing nursing care through cultural preservation, accommodation, and repatterning. We conclude that culture care theory offers a theoretical framework to assist nurses in providing culturally sensitive care to Black women with obesity. Nurses caring for this population can utilize this theory to tailor interventions specific to the cultural needs of women to improve outcomes in the management of obesity. In this article, we use AA and Black interchangeably to represent Americans whose ancestors originate from Africa.
Obesity is a growing epidemic in the United States and is the second leading cause of preventable deaths after smoking (Goldman, 2020). Obesity is best defined as a disease process of excess body fat accumulation associated with genetic and environmental causes and multiple pathological consequences (Endalifer & Diress, 2020). People who are obese have an increased risk of developing a variety of ailments, such as hypertension, type 2 diabetes, osteoarthritis, hyperlipidemia, cardiovascular disease, and certain cancers. The estimated medical cost of caring for patients with obesity in the United States is about $147 billion annually (Goldman, 2020). A systematic review by Endalifer and Diress (2020) concluded that genetics and sociodemographic and behavioral factors are associated with obesity (Figure 1).
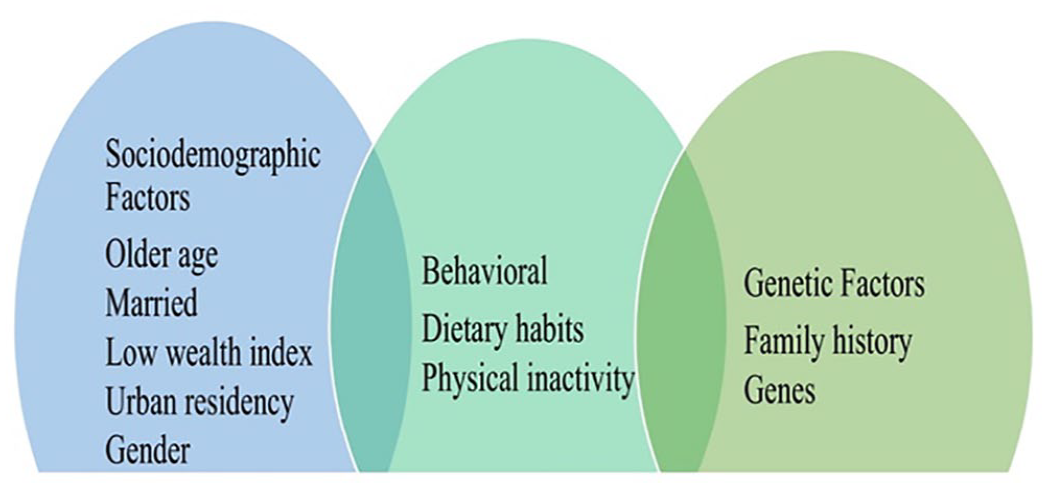
Factors Associated With Obesity.
African American (AA) women are disproportionately affected with the highest rates of obesity as compared with any other group in the United States, and about 80% are either overweight or obese (US Department of Health and Human Services, 2020). Nurses provide direct care to patients with obesity and witness the devastating effects of this disease. Educating nurses on interventions that are culturally sensitive empowers them to motivate obese patients to engage in healthier habits. When compared with Caucasian women, AA women have higher rates of diabetes (12.2% vs. 3.3%), hypertension (54.4% vs. 38.9%), and cardiovascular disease (Banerjee et al., 2018). Various approaches have been targeted to control and prevent weight gain, but many have failed. Some of these methods include dieting, exercise, weight loss surgery, and diet pills.
These approaches may have been unsuccessful due to such things as a lack of time, motivation, monetary constraints, personal attitudes, and family problems (Greaves et al., 2017). Furthermore, some studies have revealed that in weight loss intervention programs, AA women lose less weight than Caucasian women (Banerjee et al., 2018). Research by McClelland and colleagues (2015) suggests that the success of health promotion interventions depends on the group’s cultural views on health and wellness. They revealed that obesity or being overweight is acceptable and bears no shame in the Black culture. Since obesity is permissible in the Black community, it could explain why health promotion interventions geared toward the general population do not work in the community. We aim to understand obesity through a cultural lens to provide culturally competent nursing care and improve health outcomes.
Literature Review
A biopsychosocial approach is ideal for understanding obesity from a cultural perspective because it recognizes genetics and culture, environment, and socioeconomic status as reasons for the development of obesity and weight-related health behaviors (Sutton et al., 2016). Research has revealed that AAs face unique barriers when it comes to obesity.
Most older AA women generally cite social, environmental, and personal factors as reasons for not engaging in physical activity (Gothe & Kendall, 2016). Conversely, Black women report a lack of safety, weather conditions, poor neighborhood conditions, self-consciousness, hair maintenance, and not being highly conscious of their weight and body size (Gothe & Kendall, 2016; Pekmezi et al., 2013). These differences suggest that Black women have unique circumstances that prevent them from engaging in physical activity. Additionally, Pekmezi and colleagues (2013) suggested that AA women had positive overtones with weight gain at different points of their lives. These researchers found a common trend in which large body size is acceptable since some women in the community seek to gain more weight even when they are considered overweight by health professionals.
In 2014, Awad and colleagues suggested that when asked about body image, Black female students strived to live up to the cultural standard of “thick and curvy.” Some women revealed that they engaged in practices such as squatting or eating certain foods to gain a curvy figure while avoiding vigorous activities to lose weight. Barrington and colleagues (2020) found an inverse correlation between obesity and education, occupation, and family income—that is, as income increases, the rate of obesity reduces and vice versa.
Due to negative historical experiences, AAs are less likely to trust the healthcare system as compared with other racial groups. Mistrust interferes with healthcare interventions and inhibits inclusive nursing care (Muvuka et al., 2020). The major themes identified in the literature review were mistrust of healthcare providers, positive body image, lack of time, hair maintenance, and environmental safety concerns.
Theoretical Framework
Leininger (1988) developed the transcultural nursing theory or culture care theory, which seeks to understand different cultures’ health-illness caring practices, values, and beliefs to provide meaningful and productive nursing care within persons’ cultural contexts. Leininger developed the theory from an anthropological perspective and asserted that people are born, live, and die within a cultural context but depend on human care for survival. As humans, nurses are charged with caring for patients from different backgrounds. Therefore, the goal of the theory is to empower nurses to provide culturally competent care. Leininger also asserted that cultural care preservation, accommodation, and repatterning provide culturally congruent care.
Culture care preservation includes activities that help cultures maintain beneficial health practices (Leininger, 1988). For example, by respecting the patients’ culture, nurses may accommodate their religious rituals. Preserving culture may enable a patient to accept nursing interventions, thus improving health outcomes. Culture accommodation includes activities that help cultures compromise with others for culturally safe and effective care. For example, involving the patient’s family and social support network may instill trust in the healthcare system. Repatterning consists of modifying cultural values to create room for healthcare patterns that are beneficial for the health of a patient. A nurse should strive to understand the cultural backdrop of the patient and the perception of modern medicine. With this in mind, the nurse can discuss with the patient how to adjust cultural values to fit within the framework of contemporary healthcare delivery and ensure optimal health.
The tenets of the culture care theory are supported by 13 assumptive premises: technology, religion and philosophy, kinship, society, cultural values, beliefs and lifeways, politics, law, economy, education, and language. It also includes the Sunrise Enabler, a conceptual picture that depicts how the components of the theory influence the care and health status of individuals, families, and sociocultural groups (Leininger, 1988). The Sunrise Enabler can guide nurses in understanding AA women’s worldview, religious orientation, kinship, folk and professional care practices, ethnohistory, and other factors that may affect the healthcare that they receive. See figure 2, which depicts the sunrise model.
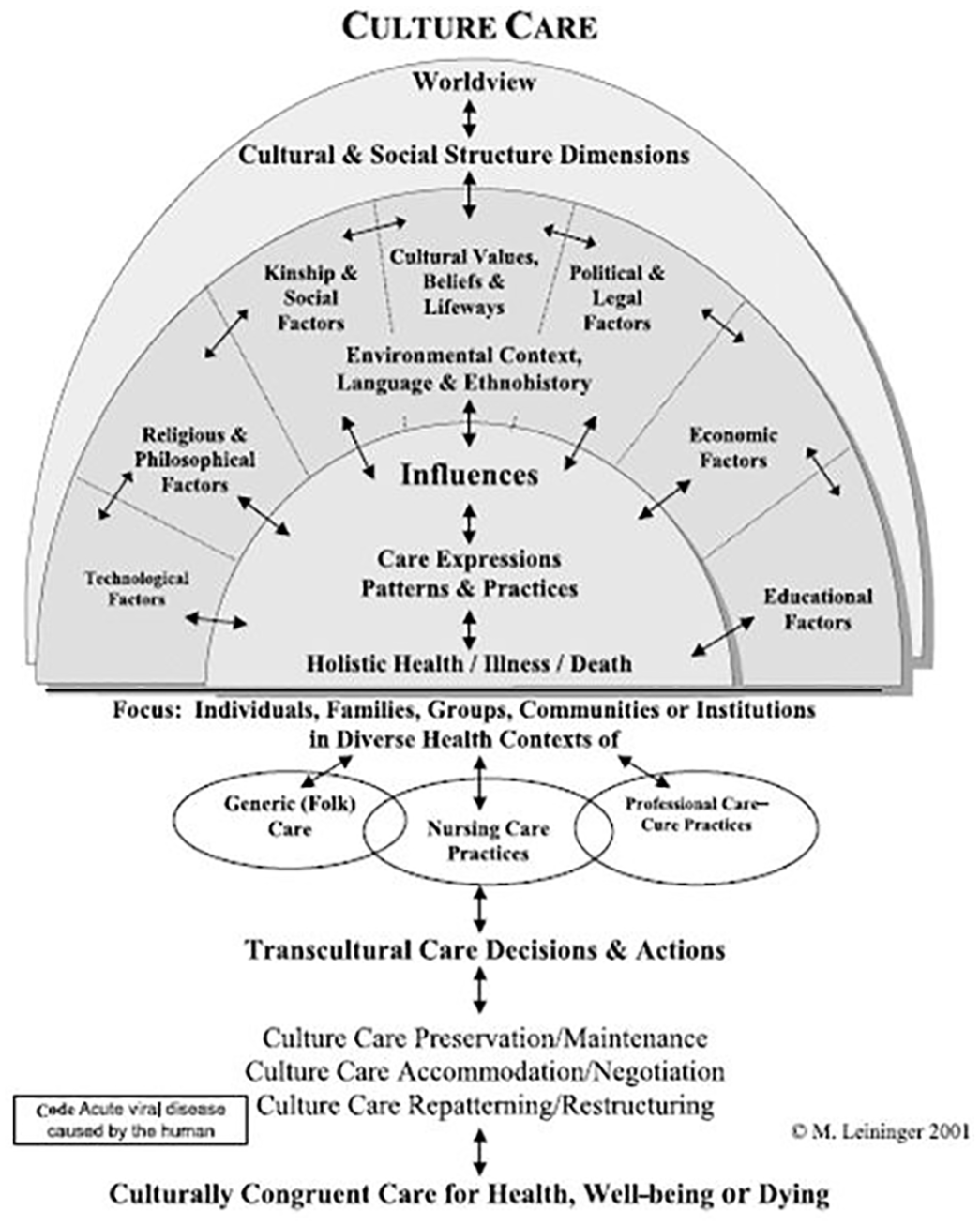
Leininger’s Culturally Congruent Care for Health, Well-Being, or Dying.
Implementing the Culture Care Theory
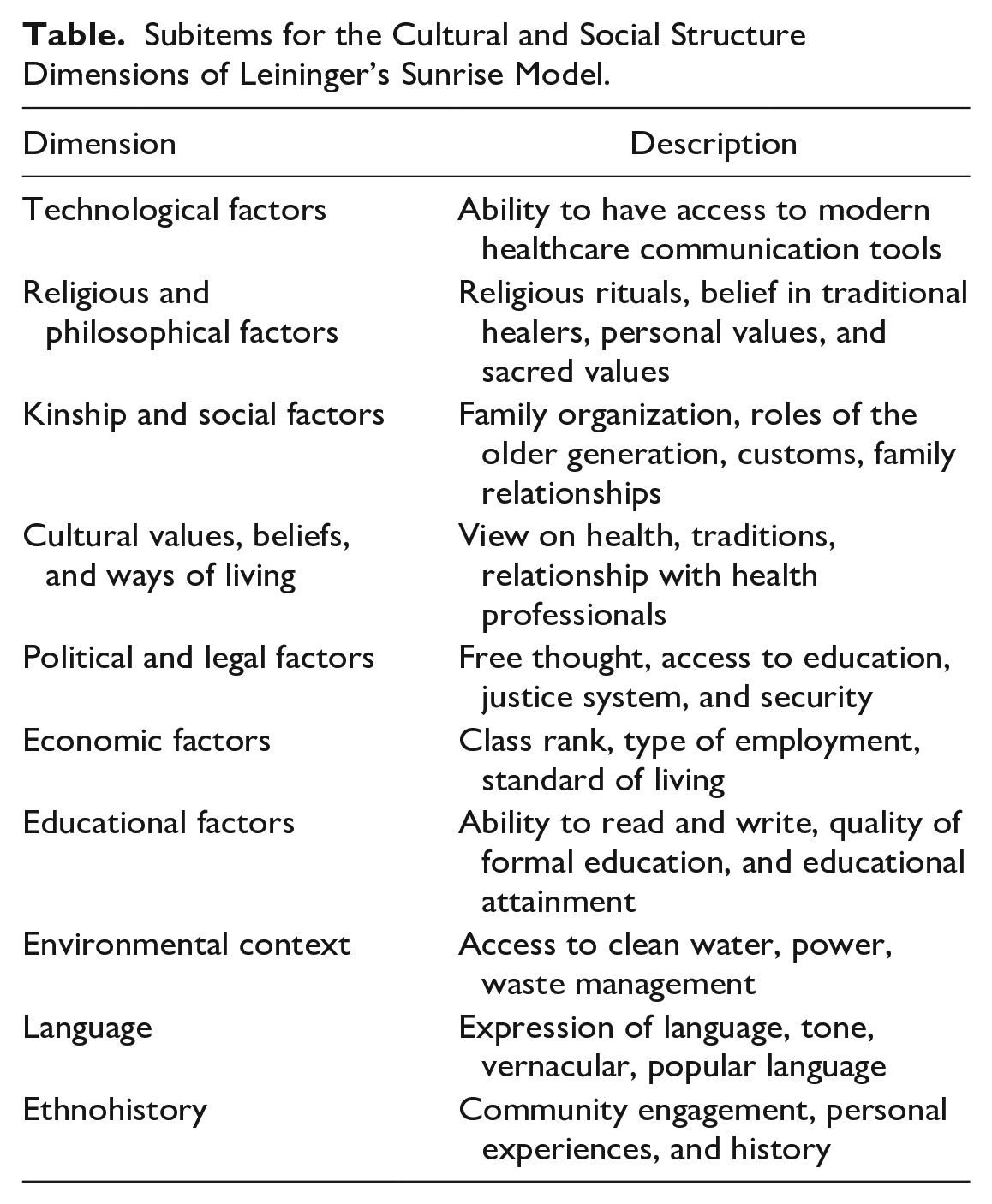
The nurse may utilize Leininger’s theory in the nursing care of AA women with obesity in an effort to understand and provide culturally competent care. Incorporating the 13 components of the theory during nursing care enables the nurse to arrive at a comprehensive, holistic, and accurate assessment to understand cultural care (Leininger, 1988). When interacting with the patient, the nurse may first conduct interviews to understand the patient’s health needs. Thereafter, the nurse develops a nursing diagnosis and critically analyzes collaborative problems using cultural care preservation and maintenance, culture care accommodation, and cultural repatterning and restructuring (Leininger, 1988). Finally, the nurse may select several concepts from Leininger’s theory to understand the needs of a patient during nursing care (Table).
Subitems for the Cultural and Social Structure Dimensions of Leininger’s Sunrise Model.
Technological Factors
Research showed that modern technology can modify negative behavior and encourage healthier habits. Integrating a mobile health application in treating patients with hypertension and type 2 diabetes effected positive health outcomes (Doocy et al., 2017). Additionally, Plotnikoff and colleagues (2017) used the eCoFit application to assess its effect among adults diagnosed with type 2 diabetes. The research results revealed a significant increase in physical activity, lower body muscularity fitness, and health outcomes. James and colleagues (2016) postulated that culturally sensitive e-health via smartphones might benefit AA women with chronic illness, as it may help in disease management. Specifically, most women in the study were willing to opt in to receive messages from healthcare providers on their smartphones.
Cultural Values, Beliefs, and Ways of Living
AAs are less likely to trust healthcare providers than other racial groups. This is due to health researchers’ long history of maltreatment and unjust practices (Muvuka et al., 2020). Three historical atrocities—Lacks, Tuskegee, and Sims—explain the background of this distrust (Lockhart, 2020). Consequently, distrust in the healthcare system is deeply embedded in the Black community, making it harder for women to seek medical attention or the advice of a health professional. In light of the COVID-19 pandemic, a survey by the Langer Research Associates (2020) disclosed that only 14% of Black respondents trusted the safety of the COVID-19 vaccine. Therefore, the nurse caring for AA women with obesity should be sensitive to this history and establish trust before engaging in nursing care. Lack of trust in the healthcare system can lead to poor health outcomes in this population.
Religious and Philosophical Factors
Multiple research studies have shown the role of religion in the Black community. About 83% believe in God, and Black women are more likely to use religion as a coping strategy as compared with men (Harris et al., 2019). Church-based intervention groups have been successful among AA communities. In a church-based weight loss study by Newton and colleagues (2018) with a sample of 97 participants, the weight loss difference between the intervention and control groups was significant (
Kinship and Social Factors
Intergenerational family support has been the mainstay of healthcare in AA culture (Stanford Medicine, 2019). Most AA families have solid intergenerational relationships and care for one another. The social support and family bonds in Black families are strong, and the culture encourages reciprocal care giving of relatives. The nurse should therefore discuss the intergenerational and generational responsibilities within the family during nursing care.
Educational and Economic Factors
A systematic review by Same and colleagues (2018) revealed that Black students have inadequate access to top-level math and science courses, are more likely to receive school suspensions, and have inexperienced teachers as compared with White students. This leads to decreased educational opportunities and achievement among Black students. Moreover, systematic factors, such as discriminatory policies and practices, have reduced AAs’ access to the resources and skills needed to understand health information (Muvuka et al., 2020). Additionally, poor housing conditions and lack of proximity to fresh-food supermarkets or farmers’ markets in Black communities contribute to poor health (Kim et al., 2021). Therefore, nurse can work with the multidisciplinary team to find resources in the community to assist the patients.
Discussion
Leininger’s (1988) theoretical model can be used to not only provide care but inform culturally competent care in various settings. Obesity is a multipronged and complicated disease that involves socioeconomic, community, individual, and cultural factors. Research has consistently found that Black women have high rates of obesity in the United States as compared with Caucasian, Asian, and Hispanic women (US Department of Health and Human Services, 2020). Obesity leads to high rates of metabolic disorders, hypertension, and diabetes among Black women versus their White counterparts. To understand and provide care in a manner that uses the model to inform such care in Black women, a cultural perspective is needed. Leininger’s theory offers a conceptual framework that can be utilized in the care of obese women by understanding the constructs with a backdrop of Black culture. In addition, the Sunrise Enabler, which is a visual representation of Leininger’s theory, can act as a guide during the nursing process as the nurse intervenes to provide care. Culturally sensitive research can offer insight on how to approach obesity in the Black community. Additionally, nurses cannot ignore the unique socioeconomic and racial disparities encountered by this population.
Conclusion
Obesity affects AA women disproportionately despite interventions and research to address the issue. Culturally sensitive research is needed to develop interventions that are influential in promoting behavioral change to mitigate obesity. The Leininger theoretical framework offers an appropriate model for integrating the constructs to understand and accommodate culture. The theory can be used to understand and provide culturally sensitive nursing care to Black women with obesity.
