Abstract
Background:
Patients undergoing holmium laser enucleation of the prostate (HoLEP) are increasingly elderly, comorbid, and likely to present with asymptomatic bacteriuria. Postoperative infections are common in this growing subset, and optimal perioperative prophylactic antibiotic duration is understudied. Therefore, we aim to analyze the association between the postoperative antibiotics duration and the postoperative infection rates in patients undergoing HoLEP at increased risk for infection.
Methods:
This retrospective single-center cohort study was performed with patients undergoing HoLEP between 2018 and 2023. We included patients with risk factors for infection, including positive preoperative urine culture, catheter dependency, immunosuppression, history of urosepsis, history of pyelonephritis, or history of recurrent urinary tract infections (UTIs). Patients were categorized according to antibiotic duration in the postoperative setting as either short-term (≤3 days) or long-term (>3 days) groups. The primary outcome was the 30-day infection rate, defined as treatment provided for a clinically diagnosed UTI. Propensity score was applied for adjusted analysis.
Results:
We identified 204 high-risk patients, of which 76 were in the long-term group. The short-term group had an infection rate of 18.8% (N = 24), while the long-term group had a rate of 6.6% (N = 5) (p = 0.016). The positive urine culture rate was 11.7% (N = 15) in the short-term group and 3.9% (N = 3) in the long-term group (p = 0.074). After adjusting for factors associated with postoperative infection, the long-term group had a 12.1% lower chance of infectious complication than the short-term group (95% confidence interval [CI]: 3.4–20.9, p = 0.006). The long-term group had a 7.8% lower chance of positive urine culture than the short-term group (95% CI: 0.7–14.9, p = 0.032).
Conclusion:
This study demonstrated that postoperative antibiotic duration affects infectious complications rates in patients undergoing HoLEP with a higher risk of infection. When prescribing antibiotic prophylaxis, longer durations of postoperative antibiotics should be considered.
Keywords
Introduction
Holmium laser enucleation of the prostate (HoLEP) is a size-independent surgical treatment for benign prostatic hyperplasia (BPH) that has been increasingly adopted over the last decade. 1 Although transurethral resection of the prostate (TURP) remains the gold standard, HoLEP has demonstrated comparable efficacy with better safety outcomes, including short catheterization time and lower blood transfusion rate.2,3
When considering postoperative infectious complications, Ahyia et al. conducted a meta-analysis and reported an average rate of 0.9% in HoLEP studies, compared with 4.1% in TURP cohorts. 4 The infectious complication risk can be higher in patients with preoperative risk factors such as indwelling catheters and asymptomatic bacteriuria. This complication not only affects the patient’s quality of life but also places a burden on the health care system, underscoring the need for appropriate perioperative management strategies to decrease postoperative infection rates.5,6
Recent studies have attempted to define optimal perioperative management of infectious complications in HoLEP cases. Following this approach, the American Urological Association (AUA) recommends a single dose of preoperative antibiotic prophylaxis for all uncomplicated surgical cases of BPH. Nonetheless, both studies and guidelines have largely excluded patients more prone to infection, highlighting a significant literature gap.6–8
To address this gap, previous literature demonstrated that more than 3 days of preoperative antibiotic prophylaxis reduced postoperative infectious rates in high-risk patients undergoing HoLEP. 9 However, postoperative antibiotics, commonly prescribed in daily clinical practice, were not assessed as an independent variable. Therefore, we aimed to analyze the association between postoperative antibiotic duration and infection rates in patients undergoing HoLEP with an increased infection risk, with the hypothesis that longer duration of postoperative antibiotics will be associated with decreased infection risk.
Materials and Methods
Design and population
We conducted a retrospective cohort study at a single academic institution between 2018 and 2023. The inclusion criterion was patients with BPH at high risk for infectious complications undergoing HoLEP. High-risk patients were defined as those with asymptomatic bacteriuria, catheter dependency, immunosuppression, history of pyelonephritis or urosepsis, or history of recurrent urinary tract infection (UTI). Asymptomatic bacteriuria was defined as a single positive preoperative urinary culture, isolating at least one bacterium with a minimum of 100,000 colony forming units (CFUs) per mL of urine. 10 Additionally, immunosuppression was a broad term to comprise several conditions with immunosuppressive potential, such as solid cancer within the last 5 years, active hematologic malignancy, neutropenia, solid-organ transplant, long-term use of steroids or other immunosuppressive drugs, human immunodeficiency virus infection, or genetic immunodeficiency. 11 Furthermore, two UTI episodes within 6 months or three within 1 year were the criterion for recurrent UTI. 12 History of prostatitis was not part of our inclusion criterion, as evidence regarding its association with postoperative infectious complications remains limited. Although chronic prostatitis may increase postoperative infection risk due to its clinical overlap with recurrent UTIs, 13 we believe that such patients would already be captured within our defined cohort.
The decision of the inclusion criterion was based on current literature and clinical expertise.5,6 We also performed an ad hoc analysis of our entire HoLEP cohort to confirm the impact of each selected factor on the postoperative infectious complications. For that, we included all patients with BPH who underwent HoLEP and had follow-up for at least 1 month after the procedure (N = 449). The simplified multiple logistic regression model demonstrated that most of the inclusion factors had statistically significant or marginally significant associations with postoperative infections (see Supplementary Appendix S1).
We excluded the following: patients receiving antimicrobials for reasons other than procedure prophylaxis, patients undergoing concurrent procedures besides cystolitholapaxy, patients with no follow-up data, patients with UTI symptoms at the preoperative setting, and patients with neurogenic bladder.
Preoperative urine culture management was performed as the follows: patients would complete it within 1 month of the procedure, unless a more recent result—within 1 month of the preoperative appointment—was already available. In cases where the patient had recently completed an antibiotic course, an additional urine culture was ordered to confirm clearance before surgery. Regarding antibiotic prophylaxis management at our institution, all patients received intraoperative antibiotics per AUA guidelines. Additional preoperative or postoperative antimicrobials were prescribed per surgeon’s discretion, based on the case assessment of infectious risk factors.
Data from the electronic healthcare record were abstracted and maintained using the electronic database REDCap®. The collected variables were related to demographic characteristics, past medical history, preoperative risk factors for infection, and perioperative variables, including the American Society of Anesthesiologists (ASA) score, antimicrobial prophylaxis duration, type of pathogen detected, recent UTI treatment, prostate weight, presence of median lobe, surgery duration, concurrent cystolitholapaxy, intraoperative complications, intraoperative antibiotic type, postoperative antibiotic type, postoperative antibiotic route, need for transfusion, same-day discharge, and Foley catheter removal on first postoperative day. Postoperative safety outcomes were abstracted in conjunction with an integrated system that captures data from other institutions in the community, allowing us to record infectious complications treated at an outside facility.
The groups were categorized according to antibiotic duration in the postoperative setting, combining discharge and inpatient antibiotics. Patients who received less than or equal to 3 days of antimicrobials were categorized as the short-term group, whereas those who received more than 3 days were categorized as the long-term group. The decision to use a 3-day cutoff was based on a similar study by Pramod et al. 9
Outcomes
The primary outcome was postoperative infectious complication rate, defined as treatment provided for a clinically diagnosed UTI within 30 days of the procedure. To capture that, we searched for antibiotic prescriptions associated with UTI diagnosis within 30 days of the procedure in the electronic health care database. The secondary outcome was the positive urine culture rate within 30 days of the procedure. A positive urine culture was defined as a culture identifying at least one bacterial strain with a minimum of 10,000 CFUs per mL of urine. 9
Statistical analysis
Descriptive analysis was conducted using percentages for categorical variables and median with interquartile ranges (IQR) for continuous ones. We applied the Pearson chi-square or Fisher exact tests for the primary and secondary outcomes. Regarding the adjusted analysis, the propensity score with inverted weights was used to calculate the independent variable’s average treatment effect (ATE). To achieve group balancing, we only applied variables clinically known to be associated with both the exposure factor (long-term use of antibiotics) and the outcome (postoperative infectious rates), or solely the outcome, as described in the literature.14,15 Therefore, the covariates used for the model were diabetes, chronic kidney disease, asymptomatic bacteriuria, catheter dependency, immunosuppression, history of pyelonephritis or urosepsis, history of recurrent UTI, duration of preoperative antibiotic prophylaxis, same-day discharge, and postoperative Foley catheter removal time. To assess the relative contribution of each inclusion criterion as well as the postoperative antibiotic duration to the primary outcome, we conducted a penalized multiple logistic regression analysis. Statistical tests were performed using Stata/MP 18®.
For the subanalysis, we performed unadjusted associations limited to the patients who received any postoperative antibiotics, aiming to assess the impact of antibiotic duration, route, and type with postoperative infectious complications. Although it would be valuable to compare antibiotic prescribing patterns between our high-infection-risk cohort and the non-high-risk counterparts, our database did not contain sufficiently detailed antibiotic-related data for the latter group.
The study protocol was approved by the Institutional Review Board of the University of California San Francisco under the number 24-43006 and adhered to the principles of the Declaration of Helsinki.
Results
In our cohort of 471 patients, we identified 204 (43.3%) high-risk individuals, of which 37.3% (N = 76) were in the long-term group. Among the patients in the short-term group, 74.2% (N = 95) did not receive any antibiotics. The median duration of antibiotic use was 0 [0–1] days in the short-term group and 8.5 [7–14] days in the long-term group. The main risk factor was catheter dependency (80.4%), followed by asymptomatic bacteriuria (34.3%) and recurrent UTI (23%). A visualization of the risk factor distribution across the cohort is seen in Figure 1. The median age was 77 [66–72], with 70.1% composed of white individuals. The prevalence of hypertension was 76.3% in the long-term group, compared with 53.1% in the short-term group (p < 0.001). There were no other significant differences between baseline characteristics across the groups (Table 1).
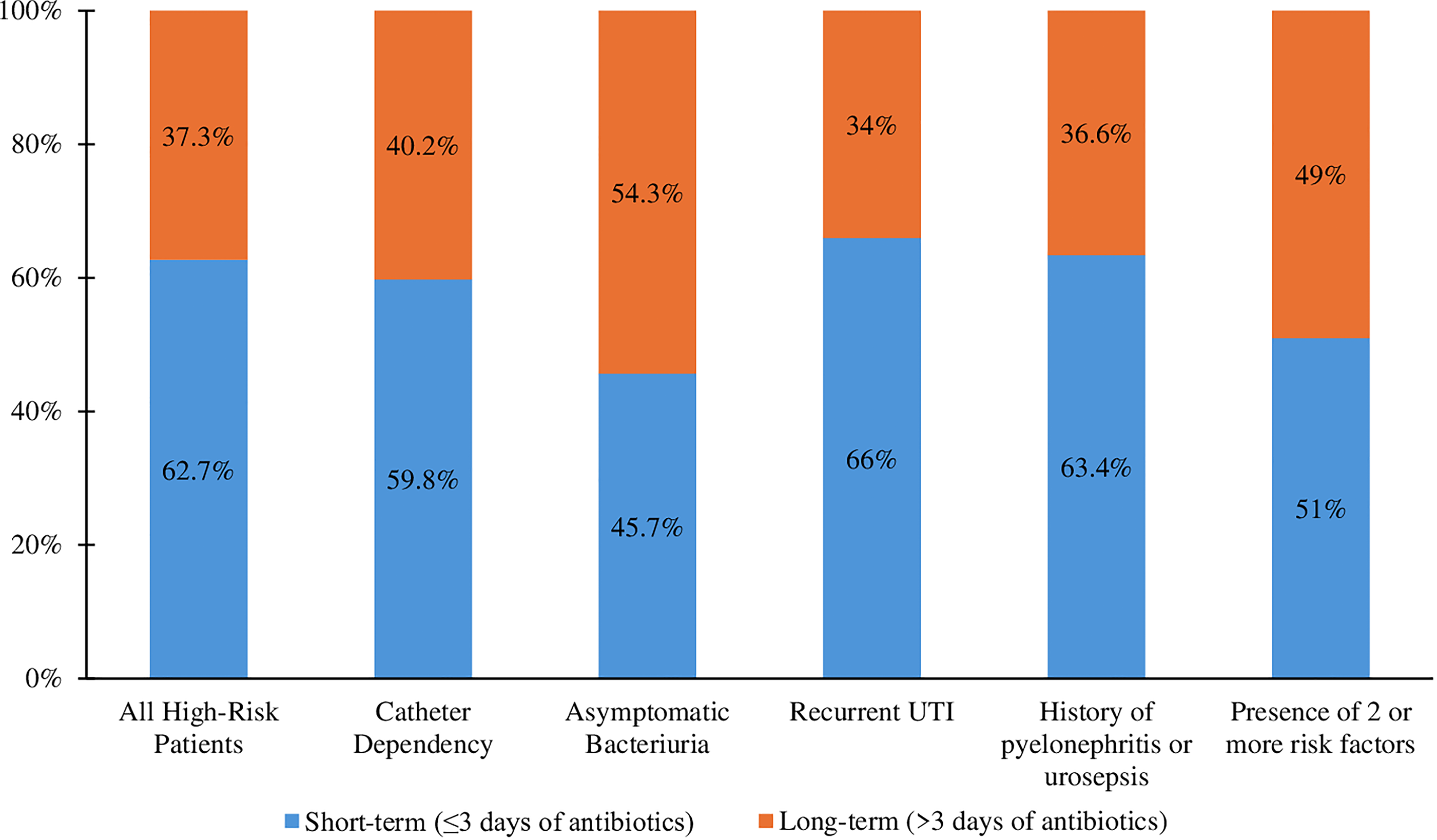
Distribution of risk factors according to prophylactic antibiotic duration. UTI = urinary tract infection.
Baseline Characteristics
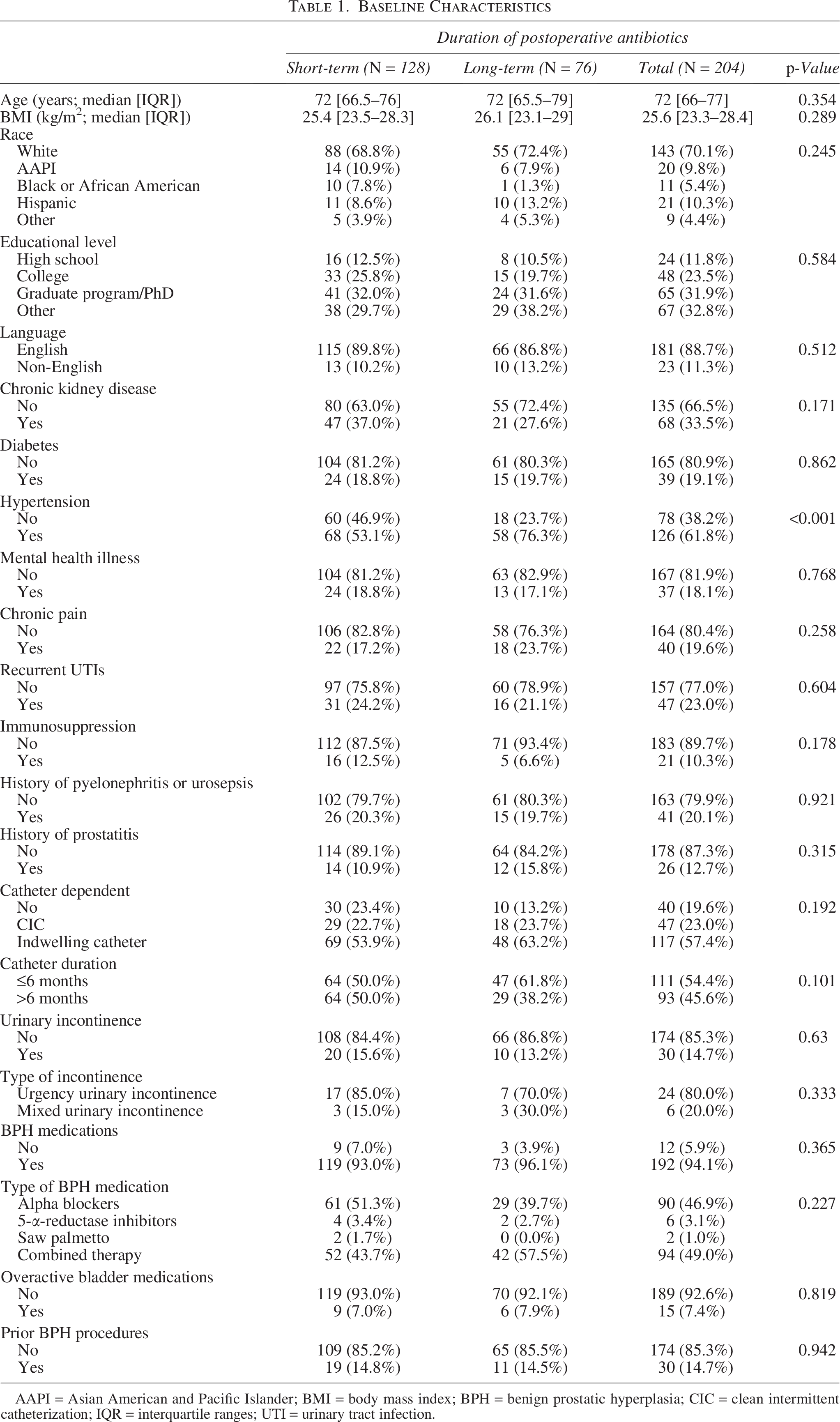
AAPI = Asian American and Pacific Islander; BMI = body mass index; BPH = benign prostatic hyperplasia; CIC = clean intermittent catheterization; IQR = interquartile ranges; UTI = urinary tract infection.
The presence of asymptomatic bacteriuria was higher in the long-term group when compared with the short-term group (50% vs 25%, p < 0.001; Table 2). There were also more patients with multiple infectious risk factors in the long-term group than in the short-term group (49% vs 39.8%, p < 0.001; Table 2). In addition, fewer patients received a longer prophylactic scheme from 2022 to 2023 compared with 2017 to 2021 (34.2% vs 49.2%, p = 0.037; Table 2). In the long-term group, 46.1% had an ASA score of 3, whereas 31.2% had the same score in the short-term group (p = 0.034; Table 2). Additionally, a smaller proportion of the long-term group had same-day discharge (22.4% vs 35.9%, p = 0.043; Table 2) and Foley catheter removal on the first postoperative day (34.2% vs 51.6%, p = 0.016; Table 2) compared with the short-term group.
Perioperative Variables
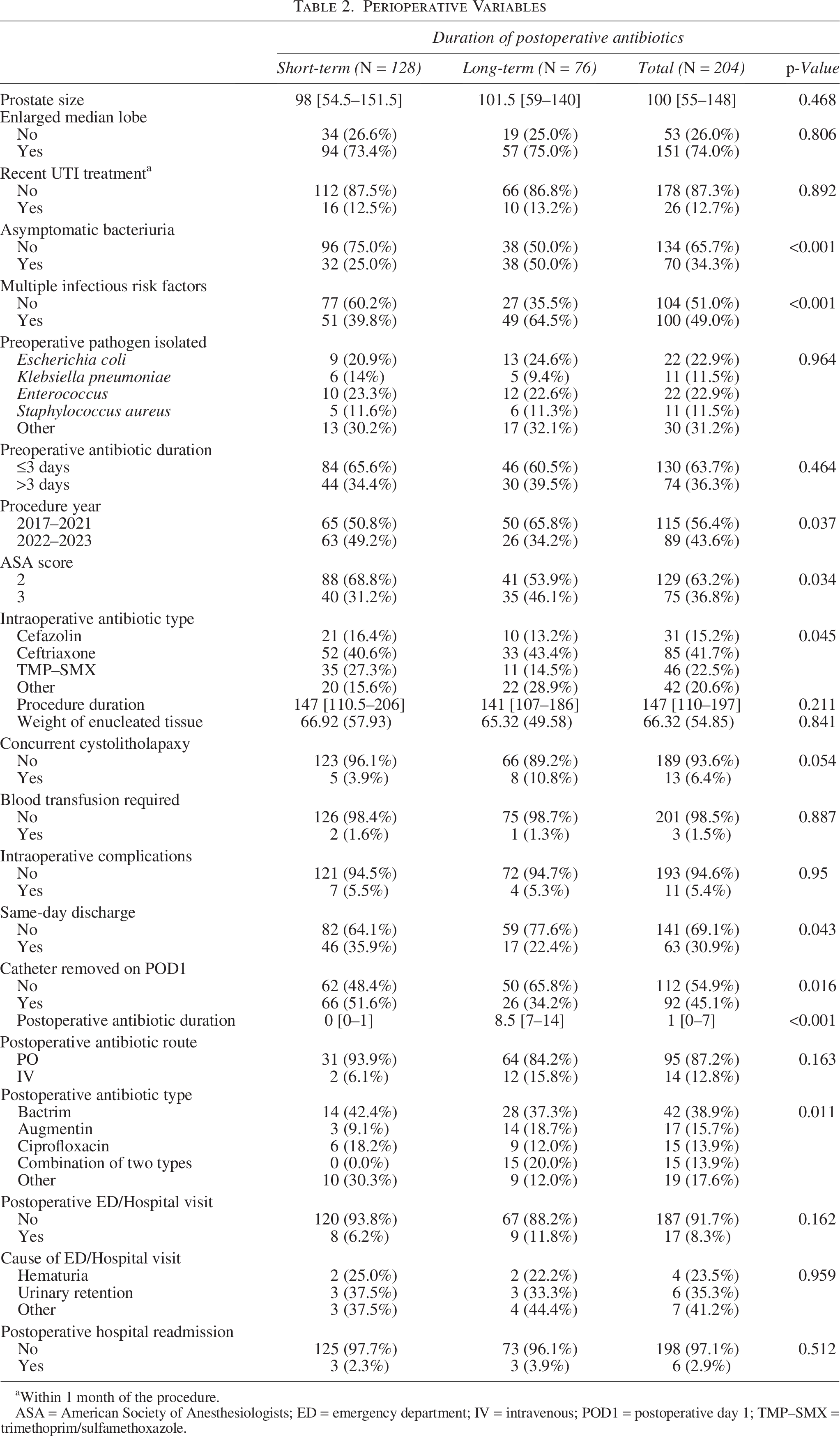
Within 1 month of the procedure.
ASA = American Society of Anesthesiologists; ED = emergency department; IV = intravenous; POD1 = postoperative day 1; TMP–SMX = trimethoprim/sulfamethoxazole.
Our cohort had 29 (14.2%) postoperative infectious complications. Compared with the overall cohort, the subset of patients classified as high infectious risk experienced a significantly higher rate of postoperative infectious complications than the non-high-risk group (14.2% vs 1.9%, p < 0.001). The long-term group yielded a postoperative infectious complication rate of 6.6% (N = 5), whereas the short-term group had a rate of 18.8% (N = 24) (p = 0.016; Fig. 2). Regarding the secondary outcome, 18 (8.8%) had a positive urine culture. The prevalence of postoperative positive urine culture was 3.9% (N = 3) in the long-term group, compared with 11.7% (N = 15) in the short-term group (p = 0.074; Fig. 2). The three patients (1.5%) who developed urosepsis were in the short-term group. In addition, Enterococcus sp. was the most isolated pathogen (27.8%), followed by Klebsiella pneumoniae (22.2%) and Escherichia coli (16.7%). None of the postoperative pathogens identified matched their corresponding preoperative organisms. Among patients with a postoperative infectious complication, 90.9% of those who received postoperative antibiotics were prescribed the same antibiotic type preoperatively (see Supplementary Appendix S2).
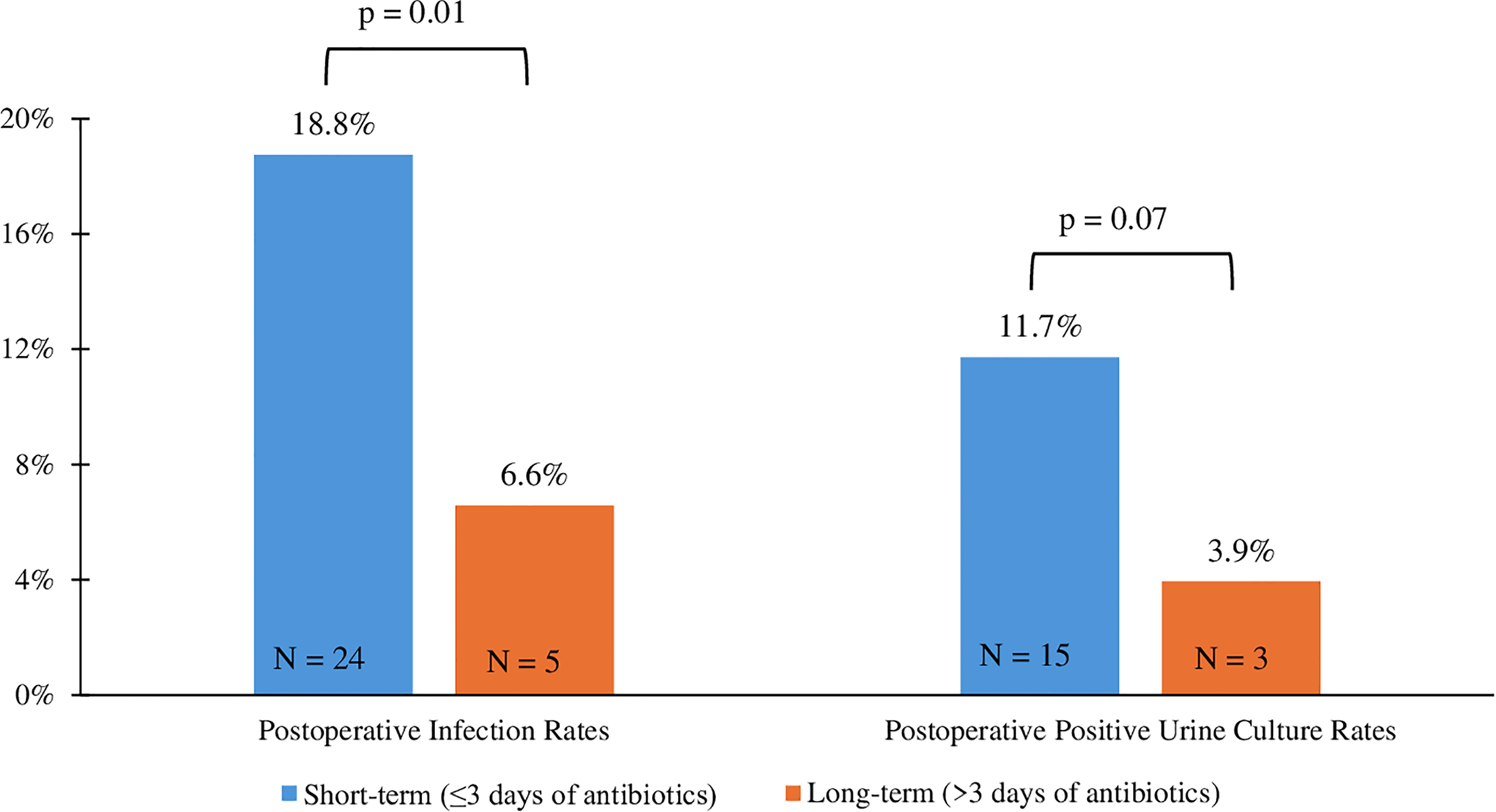
Comparison of the 30-day postoperative infectious complication rates and the confirmed UTI rates between the long-term (>3 days) and the short-term (≤3 days) groups.
On the adjusted analysis, the long-term cohort had a 12.1% lower chance of postoperative infectious complication than the short-term cohort (95% confidence interval [CI]: 3.4–20.9, p = 0.006; Table 3). For the secondary outcome, the long-term cohort had a 7.8% lower chance of positive postoperative urine culture than the short-term cohort (95% CI: 0.7–14.9, p = 0.032; Table 3).
Average Treatment Effect Calculation of the Antibiotic Duration on the Postoperative Infectious Complication Rates and Positive Urine Culture Rates Through a Propensity Score Model
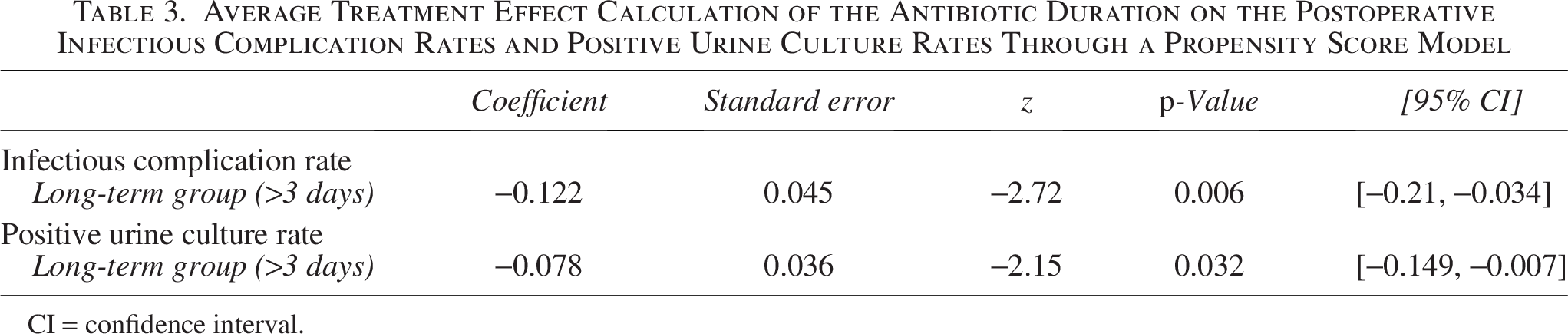
CI = confidence interval.
The multiple logistic regression analysis, which accounted for all inclusion criteria as well as the duration of postoperative antibiotics, demonstrated that patients in the long-term group were 67% less likely to have a postoperative infectious complication (OR = 0.33; 95% CI: 0.12–0.90; p = 0.03; see Supplementary Appendix S3). None of the individual inclusion criterion was significantly associated with the primary outcome.
In the subanalysis, there was a trend toward lower postoperative infection rates among those who received longer antibiotic courses (7 [3–10] vs 2 [1–7.5] days; p = 0.065). None of the patients who received intravenous antibiotics developed an infectious complication, although this difference was not statistically significant compared to those who received oral antibiotics (0% vs 12.6%; p = 0.159). Among patients who did not develop postoperative infectious complications, the most commonly prescribed antibiotics were Bactrim (37.5%), followed by a combination of two antibiotic types (15.6%), Augmentin (14.6%) and Ciprofloxacin (14.6%). Antibiotic type was not associated with the primary outcome (p = 0.502).
Discussion
Along with the direct correlation between BPH prevalence and age, there is also an association between age and symptomatic BPH. As a result, a growing number of elderly men are expected to seek treatment for this condition in the coming years. One of the challenges associated with this trend is that this population usually presents with a higher comorbidity burden and higher perioperative risk of complications.16,17 Among them, postoperative infection is a common adverse event whose rates can be even higher in this subset of patients. 4 This underscores the need for more comprehensive perioperative infection management guidelines in patients undergoing HoLEP. Our retrospective study conducted at a large academic institution found that longer postoperative antibiotic regimens are linked to a reduced rate of postoperative infectious complications in patients undergoing HoLEP with high risk for infection. Future prospective clinical trials should aim to determine the optimal antibiotic management for patients undergoing HoLEP. Subsequent studies should also expand this evaluation to other bladder outlet procedures, enabling meaningful comparisons of antibiotic durations while accounting for different endourologic interventions, such as TURP.
The absence of guidelines for patients with a higher infectious risk who wish to undergo HoLEP places the responsibility for decision making largely on the clinician’s expertise.8,18 Consequently, this leads to significant heterogeneity in infection prophylaxis practices. A Japanese survey of 59 national institutions assessed the perioperative infection management of HoLEP procedures and found divergence in the antibiotic dose, type, duration, and route of administration. Nonetheless, slightly above 60% of the institutions used intravenous cephalosporins within 1–3 days of the procedure. 19 Thus, the high heterogeneity in perioperative infectious management may lead to antibiotic misuse and overuse, which could be minimized with standardized guidelines.
The dependence on the clinician’s judgment in determining antibiotic duration may also have influenced some of our findings. Factors such as higher ASA scores, asymptomatic bacteriuria, and delayed catheter removal were more commonly observed among patients who received longer courses of antibiotics. Although asymptomatic bacteriuria has been more consistently linked to postoperative infectious risk in the literature, other factors remain less clearly defined and warrant further investigation to determine their true predictive value in infectious complications and justify prolonged antibiotic use.
We reported an overall postoperative infectious complication rate of 14%, above the 3.9% rate observed in a similar study. 9 This might be explained by the distinct criterion applied for the primary outcome. In our study, a positive urine culture was not required for the primary outcome, which could increase the risk of false positives. Irritative voiding symptoms secondary to BPH/instrumentation can be challenging to differentiate from a true UTI. However, this better reflects a real-world practice, where patients are often treated for a presumed UTI without having laboratory confirmation. To overcome this limitation, our secondary outcome was defined as a positive urine culture, whose incidence of 8.8% is closer to the previous report.
Although many articles address the best management of preoperative antibiotics in HoLEP procedures, there is scant evidence of associations between postoperative antibiotic duration and infectious complications.6,7,9 Our adjusted analysis demonstrated that longer antimicrobial prophylaxis schemes decrease the probability of postoperative infectious complications by 12.1% and the probability of a positive urine culture by 7.8%. This finding raises the question of whether the timing of antibiotic prophylaxis affects postoperative UTI rates in high-risk patients.
Pramod and colleagues showed that extended preoperative antibiotic prophylaxis in patients undergoing HoLEP at high risk of infection reduced the likelihood of postoperative complications by 76%. 9 Their sample of 407 patients and their adjusted analysis for other cofactors, such as intraoperative and postoperative antibiotics, further support their findings. However, Bheenick et al. conducted a retrospective review to assess if asymptomatic bacteriuria affected postoperative infectious complication rates in patients undergoing HoLEP who were not routinely prescribed preoperative antibiotics. In this study, all patients received intraoperative intravenous antimicrobials, with the addition of postoperative antibiotics at the surgeon’s discretion. They concluded that asymptomatic bacteriuria was not a predictive factor for UTIs nor urosepsis. 20 Even though the use of postoperative antibiotics was quoted as “low” between the groups, it may have prevented an infection in the patients considered to be at an elevated risk.
Discrepancies in the literature regarding optimal perioperative antibiotic timing may arise from factors like premature antibiotic discontinuation or patient preference, which increases the risk of bacterial recolonization. 20 Provider bias in diagnosing postoperative infections may also be influenced by the timing of prophylactic antibiotics. Patients who received antibiotics post-procedure may be less likely to be diagnosed with a UTI, potentially reducing lab testing and treatment. Additionally, differences in institutional guidelines and their adherence may affect infection rates. Therefore, prospective randomized clinical trials are needed to establish best practices for infection prevention, with careful consideration of antibiotic timing.
Our study has limitations. The retrospective design may introduce confounders and selection bias, despite efforts to balance variables using propensity scores. Importantly, the definition of “high-risk” patients for infectious complications following HoLEP is not well established in the literature. Future studies with larger, multi-institutional datasets are needed to better understand the impact of each infectious risk factor in this population. The low event rate limits the power of our analyses. Additionally, our sample is predominantly white men treated at a tertiary care center, which may affect the generalizability of the results. Finally, we could not account for patient adherence to antibiotic regimens or variations in antibiotic type, route, and dosing, which may impact infectious complications. Nonetheless, our subanalysis did not demonstrate any significant associations between antibiotic route or type and postoperative infectious complications.
Conclusion
When prescribing antimicrobials for high-risk patients undergoing HoLEP, longer durations of postoperative antibiotics should be considered. Future prospective trials should be done to standardize perioperative antibiotic management in this patient subset. In addition, the timing of antibiotic prophylaxis should be investigated to assess any differences between the preoperative and postoperative settings.
Authors’ Contributions
F.C.M.: Conceptualization (supporting), data curation (lead), formal analysis (lead), investigation (lead), methodology (lead), project administration (lead), visualization (lead), and writing—original draft (lead). P.S. and M.M.: Conceptualization (supporting), data curation (supporting), investigation (supporting), and writing—review and editing (equal). M.C.V.: Conceptualization (supporting), data curation (supporting), investigation (supporting), validation (equal), and writing—review and editing (equal). U.M., K.T., J.T.F., J.E.B., H.Y., and W.S.: Conceptualization (supporting), validation (equal), and writing—review and editing (equal). T.C.: Conceptualization (lead), resources (lead), supervision (lead), validation (lead), and writing—review and editing (equal).
Footnotes
Author Disclosure Statement
The authors declare that they have no conflicts of interest to disclose.
Funding Information
The authors received no specific funding for this article.
Supplemental Material
Supplemental Material
Supplemental Material
Abbreviations
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
