Abstract
Purpose:
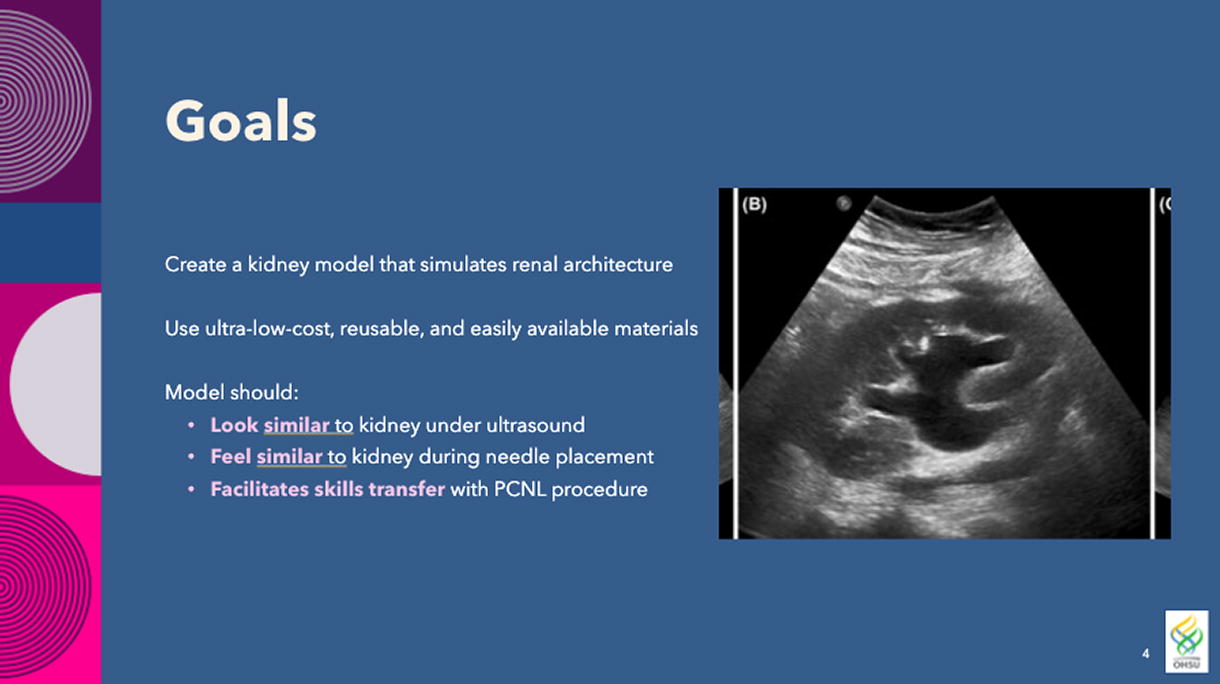
Utilizing ultrasound (US) guidance for percutaneous nephrolithotomy (PCNL), a complex and potentially lifesaving procedure, increases urologist independence and reduces dependence on interventional radiology or fluoroscopy. We demonstrate a method for creating a do-it-yourself (DIY) kidney phantom using household products and items commonly found in hospitals as a method of on-demand, low-cost, US-guided PCNL training.
Methods:
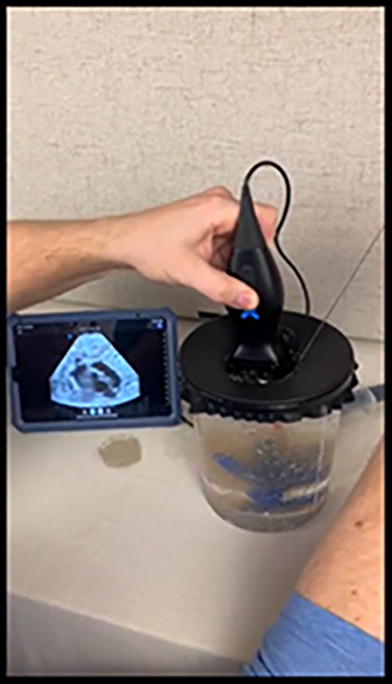
Phantoms were created to simulate kidneys and surrounding tissue in home kitchens near the course locations without specialized equipment. To create each model, a surgical glove was used to simulate renal calyces, gelatin and psyllium husk were used to simulate peripelvic fat and renal parenchyma, and an US gel-water slurry was used to simulate abdominal tissue. Correct needle placement was confirmed with efflux of water from the needle. During each course, participants were given one hour of instructional lectures, after which they used handheld portable point-of-care ultrasound to identify targets within a phantom and demonstrate proper needle maneuvering techniques to reach the target. Pre- and post-session surveys assessed their experience.
Results:
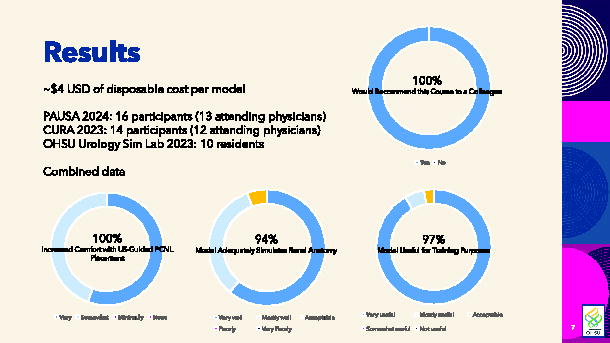
The estimated cost of each model was about $7 United States dollars per model. Each model was used by up to 15 participants before degrading. Of the 40 participants in the courses, 63% were attending physicians. A total of 53% of participants reported being “very” or “somewhat” comfortable with US-guided needle placement prior to the course. After the course, 100% of participants reported improved comfort in performing US-guided nephrostomy tube placement, 94% reported that the phantom adequately simulated renal anatomy, 97% reported that the phantom is useful for training purposes, and 100% would recommend the course to a colleague.
Conclusions:
Our DIY ultra-low-cost kidney phantom was a useful modality for training US needle guidance for PCNL procedures and improving comfort level with the procedure.
The authors have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Runtime of video: 7 min 42 sec.
Author Disclosure Statement:
This work was supported by the Urology Care Foundation Humanitarian Grant Award. Financial support for training courses was received from Dr. John Barry.
Get full access to this article
View all access options for this article.
