Abstract
Introduction
Population aging has emerged as a global phenomenon due to rising life expectancy and decreasing fertility rates. 1 While this demographic shift began in high-income countries, low-and-middle-income countries (LMICs) are now experiencing the fastest rates of aging. By 2050, nearly 8 in 10 older adults aged 60 or above will reside in LMICs. 2 Nepal, a LMIC in the Southeast Asia region, is undergoing similar demographic transition. The population of older adults in Nepal has increased from 8.13% to 10.21% from 2011 to 2021. 3 Notably, the annual average growth of the older adult population far exceeds the average growth rate of the total population growth rate (3.29% vs 0.92%), 3 indicating the accelerated pace of aging in Nepal.
Older adults are particularly vulnerable to developing mental health conditions due to a myriad of risk factors, including deterioration of physical health, chronic conditions, cognitive impairment, social isolation, and loneliness.4-6 Depression and anxiety are highly prevalent in older adults. Depression is typically characterized by persistent low mood, loss of interest and lack of energy, 7 while anxiety involves excessive and persistent worry, heightened fear and may include panic attacks that disrupts daily functioning. 8 In addition to these clinically recognized conditions, insomnia (difficulty initiating or maintaining sleep) and loneliness (absence of close emotional attachment or engaging social network) are common in older adults.9,10 These mental health conditions are associated with a reduced quality of life, 11 and a greater risk of morbidity and mortality, 12 resulting in greater healthcare needs. Despite this, mental health conditions among older adults often go unrecognized and untreated, particularly in LMICs.
Nepal’s mental health system is underdeveloped, with significant systemic challenges (such as fragmented governance, critical shortages of mental health providers, limited funding, and weak health information structure). 13 According to the Nepal Health Facility Survey 2021, only one in four health facilities offered mental health services and less than half of health facilities had any essential medicines to treat mental illnesses such as depression, anxiety, insomnia and bipolar disorders. 14 The country has just 1.5 beds for mental health disorders per 100, 000 population. 13 In addition to these systemic barriers, poverty and stigma further hinder mental health service utilization. 13 Given these broader structural gaps in the national mental health system, geriatric mental health has received little policy attention and remains largely overlooked. Government programs have primarily focused on providing a minimal social security allowances to the older adults, 15 rather than offering comprehensive health care that includes mental health services. Although the National Health Insurance Program covers the insurance premiums for individuals aged 70 and above, the program is limited in both population coverage and the scope of services it provides. 16 Mental health services are minimally represented in the benefit package, 13 and the annual coverage cap of NPR 100,000 (approximately USD 730 as of June 2025) is insufficient to meet the complex and recurring care needs of older adults with mental health conditions. 16
Empirical evidence on mental health among older adults in Nepal is limited and shows substantial heterogeneity across studies and settings. A recent meta-analysis showed that the prevalence of depression among older adults in Nepal is 52%, with a wide range of heterogeneity across geographic regions, old age homes, and community centers. 17 For example, it found that depression among older adults in eastern, western, and central Nepal was 46%, 49%, and 55% respectively. The pooled prevalence among residents of old age homes was 58% and that of community centers was 49%. 17 Another systematic review revealed that depressive disorders in older adults ranged from 4.4% at the community level to 53.2% at hospitals. 18 Similarly, evidence on anxiety among older adults, though limited, shows considerable variability, with studies reporting prevalence ranging from 8.8% to 60.3%.19,20 Such heterogeneity within and across different settings may reflect several factors, such as regional differences in mental health service availability and detection, 21 social isolation among residents of old-age homes, and variation in screening tools used to assess depression. 17
Although these findings highlight a substantial burden, most studies were primarily conducted in central Nepal and in urban areas, thereby failing to capture the rural burden. Two studies conducted in rural municipalities of central Nepal reported a depression prevalence of 28.9% 22 and 31.1%, 23 while we could not find any comparable studies from the far-western or mid-western areas. Evidence from other South Asian Countries suggests that the mental health burden among older adults may be even higher in rural areas.24-26 For example, a study in India reported the prevalence of depression in rural and urban areas were 38% and 28% respectively. 25 Comparable patterns were observed for anxiety, although evidence remains limited. A study conducted in two districts of Province 5 reported a prevalence of 18.1% among older adults 20 whereas a community-based study in Kathmandu showed 27.4%. 27 and a facility-based study in geriatric centers reported 8.8%. 28
Despite these findings, most existing studies have focused on depression and anxiety, with limited data on loneliness, insomnia, and well-being. For instance, a study with a small community sample in Kathmandu reported a prevalence of loneliness of roughly 55% among older adults, 29 while two studies with small community samples in Banepa and Makawanpur, Nepal reported insomnia prevalence ranging between 46% and 71%.30,31 This regionally concentrated and condition-specific evidence highlights the need for comprehensive research on mental health of older adults, particularly in understudied mid-western and far-western areas of Nepal.
Our study aimed to bridge this knowledge gap by estimating the prevalence of several mental health conditions— (anxiety, depression, insomnia and loneliness)— in the older adult population of Dang district in Nepal and exploring the socio-demographic factors associated with these conditions. In addition, we included mental well-being as an outcome because it captures both negative psychological states (such as depression and anxiety) and positive dimensions (such as satisfaction and happiness), offering a more holistic view of mental health. By identifying the burden and determinants, our findings can help prioritize target groups for mental health screening within older adults, guide the development of community-based interventions, and support policy efforts to integrate geriatric mental health into Nepal’s broader health system.
Methods
Study Design and Setting
We conducted a cross-sectional study to estimate the prevalence and correlates of common mental health conditions among the older adults in western Nepal. The study was conducted in Ghorahi Sub-Metropolitan, located in Dang district of Lumbini province, Nepal. Data were collected between August 2023 and January 2024.
Sample Population
The target population included individuals aged 60 or above in the selected wards. Five wards (3, 4, 5, 6, 7) were purposively selected based on the involvement of ongoing community mental health programs led by the Health Foundation Nepal (HFN). These wards were chosen to leverage HFN’s existing health infrastructure and community trust to ensure efficient implementation and cost-effectiveness. HFN is a non-profit organization, established in 2013, that primarily works on promoting access to mental health care services and providing low-cost interventions for non-communicable diseases among underserved communities in Nepal.
Sample Size, and Sampling Method
A purposive sampling method was used to ensure representation, with efforts made to include at least 20% of the older adult population from each ward. Of the estimated 3746 individuals aged 60 or above across the selected wards, we collected data from 814 participants.
Inclusion and Exclusion Criteria
Older adults (aged 60 or above) in the selected wards were included in the study. Our exclusion criteria included individuals with psychotic or other serious mental illnesses that impaired their ability to provide consent, as well as individuals who were unable or unwilling to provide informed consent for other reasons. We didn’t use specific tools to identify people with other severe mental illnesses. The study team was trained to identify people with aggression, agitation, active hallucinations, or delusions. Everyone in our study met the inclusion criteria.
Data Collection
Structured face-to-face interviews were conducted by a trained field team from HFN, consisting of ten community mental health workers and two psychosocial counsellors with experience in community-based mental health programs. HFN has implemented community-based mental health programs since 2013, and its team has received several structured mental health training packages endorsed by the Ministry of Health and Population of Nepal, which adds institutional credibility and field experience in data collection process. Before data collection, the study team participated in three days intensive training led by a multidisciplinary team that included psychologists, public health professionals, the principal investigator (PI) and a senior public health nurse (project coordinator). The training covered study protocols, ethical conduct and standardized administration of mental-health assessment tools. Data were collected using the KoBo Toolbox application (https://www.kobotoolbox.org/), a secure, freely available data collection platform, on encrypted tablet devices to ensure data accuracy, efficiency, and confidentiality. Throughout the data collection period, the community mental health workers received continuous supervision and guidance from the psychosocial counselors, project coordinators and PI to maintain data quality and adherence to the research protocols. Interviews were held in participants’ homes to ensure accessibility and comfort. Ethical approval was obtained from the Nepal Health Research Council (NHRC) institutional review board (Protocol Registration: 385/2023). Written informed consent was obtained from all participants before data were collected. Individuals identified with mental health problems were provided with psychological counseling and follow-up support as part of HFN’s ongoing community health initiatives.
The study used validated instruments including the WHO-5 Well-being index, GAD-7, UCLA loneliness scale (3 item) and the Insomnia Severity Index (ISI-7) (Detail mentioned in next section). All instruments were translated into Nepali language using a standard forward-backward translation process conducted by two independent bilinguals medical professionals. The translated versions were reviewed by a linguistic expert for semantic and conceptual accuracy. We pilot tested the questionnaire among 20 older adults in Dang District to ensure cultural relevance and comprehension. Feedback from pilot testing was incorporated before final data collection. Interviews were administered in Nepali language.
Variables and Data Collection Tools
Dependent Variables
We assessed five dependent variables: well-being, insomnia, loneliness, GAD, and depression. The detail on each instrument is discussed below.
Well-Being Index
For well-being, we used the WHO-5 Well-being Index. 32 This questionnaire consists of five straight-forward and non-invasive statements; each statement has six possibly non-overlapping answers: “all of the time (5), most of the time (4), more than half of the time(3), less than half of the time(2), some of the time(1), at no time (0)”. The number in parenthesis of each option denotes a raw score associated with that option. According to the WHO-5 Well-being Index guideline, the sum of the raw score was multiplied by 25, resulting in a final score that ranged from 0 to 100. Based on the recommendation from previous studies, 32 we classified well-being into two categories: low well-being (final score of <50), and high well-being (final score of ≥50). A panel of experts in the field of health-related quality of life (HQoL) ranked WHO-5 Well-being Index at the top among 20 other scales to measure HQoL. With a content validity score of 0.80, 100% items were judged as important. 33 Several studies showed that the index has high sensitivity and specificity for diagnostic accuracy, including more than 90% sensitivity and 80% specificity for geriatric depression. 32 Having demonstrated adequate validity globally, this tool has been validated and applied in the Nepali context in a few studies.34,35 The details of the questionnaire are presented in Supplemental Material I.
Insomnia Severity Index
For insomnia, we used the Insomnia Severity Index (ISI), a brief instrument that assesses insomnia through the patient’s perception. This instrument has been validated in diverse settings, 36 including primary care and community settings. 37 The questionnaire consists of 7 items, with each question rated on a five-point Likert scale, with scores ranging from 0 to 4. The total score ranges from 0 to 28, with a higher score denoting more severe insomnia. Based on the ISI scoring system, 38 we classified insomnia into four categories: “1) No Clinical Significant Insomnia (0-7); 2) Subthreshold Insomnia (8-14); 3) Clinical Insomnia (Moderate Intensity) (15-21); and 4) Clinical Insomnia (Severe Intensity) (22-28).” We dichotomized insomnia into clinical and non-clinical insomnia based on a cut-off score of >14, as recommended by the developers of the ISI. A recent meta-analysis showed that ISI has high internal consistency, with most studies reporting Cronbach’s alphas of ≥0.7. 39 While formal validation studies of Nepali context are limited, the ISI has been used in prior research in Nepali population,40-42 supporting its feasibility and face validity in the local context. The details about the questionnaire and scoring system are presented in Supplemental Material II.
UCLA Loneliness Scale
To measure loneliness, we used the three-item UCLA Loneliness Scale. Each question has three options, ranging from “hardly ever,” “some of the time,” and “often,” with a score of 1, 2, or 3, respectively. The total score ranges from 3 to 9. This brief questionnaire has good internal consistency and reliability, with the Cronbach’s alpha coefficient ranging 0.89 to 9.94, and strong correlation with other measures of loneliness. 43 Based on the scoring system, two categories were created: Not Lonely (3-5) and Lonely (6-9). This three-item UCLA loneliness scale has been widely used in older adults internationally,44-47 and in Nepal, it has been employed in at least two studies among older adults.48,49 More importantly, a recent study has also demonstrated that UCLA-3 has high validity and reliability in the Nepali context, 50 supporting its use in this population. The details of the questionnaire and its scoring system are presented in Supplemental Material III.
General Anxiety Disorder (GAD) Questionnaire
To assess anxiety, we used a seven-item GAD questionnaire 51 ; each item has four options, ranging from “not at all,” “several days,” “more than half the days,” and “nearly every day,” with an assigned score of 0, 1, 2, and 3, respectively. The total score ranges from 0 to 21. Earlier studies have shown that this questionnaire has high reliability and validity, with Cronbach’s alpha of more than 0.85, and high correlation with PHQ.52,53 According to the scoring system, we classified GAD into four categories: Minimal (0-4); Mild (5-9); Moderate (10-14); and Severe (15-21). We binarized GAD into two categories: No or minimal anxiety, and anxiety. The latter consisted of mild, moderate, and severe anxiety. Several studies conducted in Nepal have used the seven-item GAD questionnaire.54-57 Notably, the 2022 Nepal Demographic Health Survey adopted GAD-7 for the first time, 58 further reinforcing its acceptance and applicability in the Nepali context. The details of the questionnaire and its scoring system are presented in Supplemental Material IV.
Patient Health Questionnaire (PHQ-2 & PHQ-9)
We used the PHQ-2 to screen for depression. 59 This questionnaire presents “Yes/No” questions: “Have you often been bothered by feeling down, depressed, or hopeless? And have you often been bothered by little interest or pleasure in doing things?” If a respondent, answered “Yes” to either question, he or she was considered as screening positive, and he or she was then assessed for depression using the PHQ-9. 60 Based on the scoring guideline, 59 we classified respondents into two categories: Positive for depression screening or Negative for depression screening. The details of the questionnaire and its scoring system are presented in Supplemental Material V. The approach of pre-screening with the PHQ-2 followed by the full administration of PHQ-9 has demonstrated acceptable accuracy for depression screening.61,62 The PHQ has been validated in Nepali context and several studies have used it.63-66 Furthermore, similar to the GAD-7, PHQ-9 was included for the first time in the 2022 Nepal Demographic Health Survey, 58 reinforcing its relevance and applicability in Nepal.
Independent Variables
Based on prior studies17,18 and our understanding of the local context, we had a priori hypotheses regarding certain sociodemographic characteristics that would be associated with our dependent variables. Those variables were age, gender, marital status, educational status, current family size, current employment status, type of caregiver, presence of chronic diseases (self-reported history of one or more of the following conditions: hypertension, chronic heart disease, diabetes, chronic kidney disease, chronic obstructive pulmonary diseases, thyroid disorders or any other long term illnesses lasting more than one year and requiring medical attention), family history of mental illness, history of chewing tobacco, history of smoking, and alcohol intake habit. We used broader ethnic categories of Brahmin/Chhetri (in general upper social class), Janajati (middle social class including indigenous groups) and Dalit (lower social class including the previously defined untouchable group).67,68 The details on independent variables are presented in Supplemental Material VI.
Data Analyses
First, we conducted a descriptive analysis of the sample and presented categorical variables in frequencies and percentages, and continuous variable (age) in median and interquartile range. Then, we conducted multiple logistic regression analyses, where each mental health outcome (well-being, insomnia, loneliness, anxiety, and depression) was modeled separately using the same set of independent variables. 69 All five outcomes were binary, and each model included the full set of covariates. Prior to fitting the regression models, we assessed multicollinearity among independent variables using a two-step approach. First, we examined pairwise correlation between variables and found a high correlation between “habit of alcohol intake” and “history of alcohol intake in the past year” (correlation coefficient: 0.75). We retained “habit of alcohol intake” in the model as it better reflected long-term behavioral patterns. Second, we computed Variance Inflation Factor (VIF) using the collin command in Stata. All included variables had VIF values below 1.5, well under the commonly accepted threshold of 5 to 10,70,71 indicating no significant multicollinearity. We assessed the normality of age, the only continuous variable, using the Shapiro-Wilk test and found that age of participants was not normally distributed. Because participants were nested within five wards and individuals within the same ward share unobserved contextual factors (such as exposure to similar community programs and health service access), we clustered standard errors at the ward level to adjust for intra-ward correlation, thereby producing robust standard errors. We presented the results as an odds ratio (OR) with 95% confidence intervals (CIs) and P-values. A P-value of less than 0.05 was considered significant. For all analyses, we used Stata, Version 18. 72
Results
Characteristics of Participants
Summary Statistics: Sociodemographic Characteristics of Respondents.
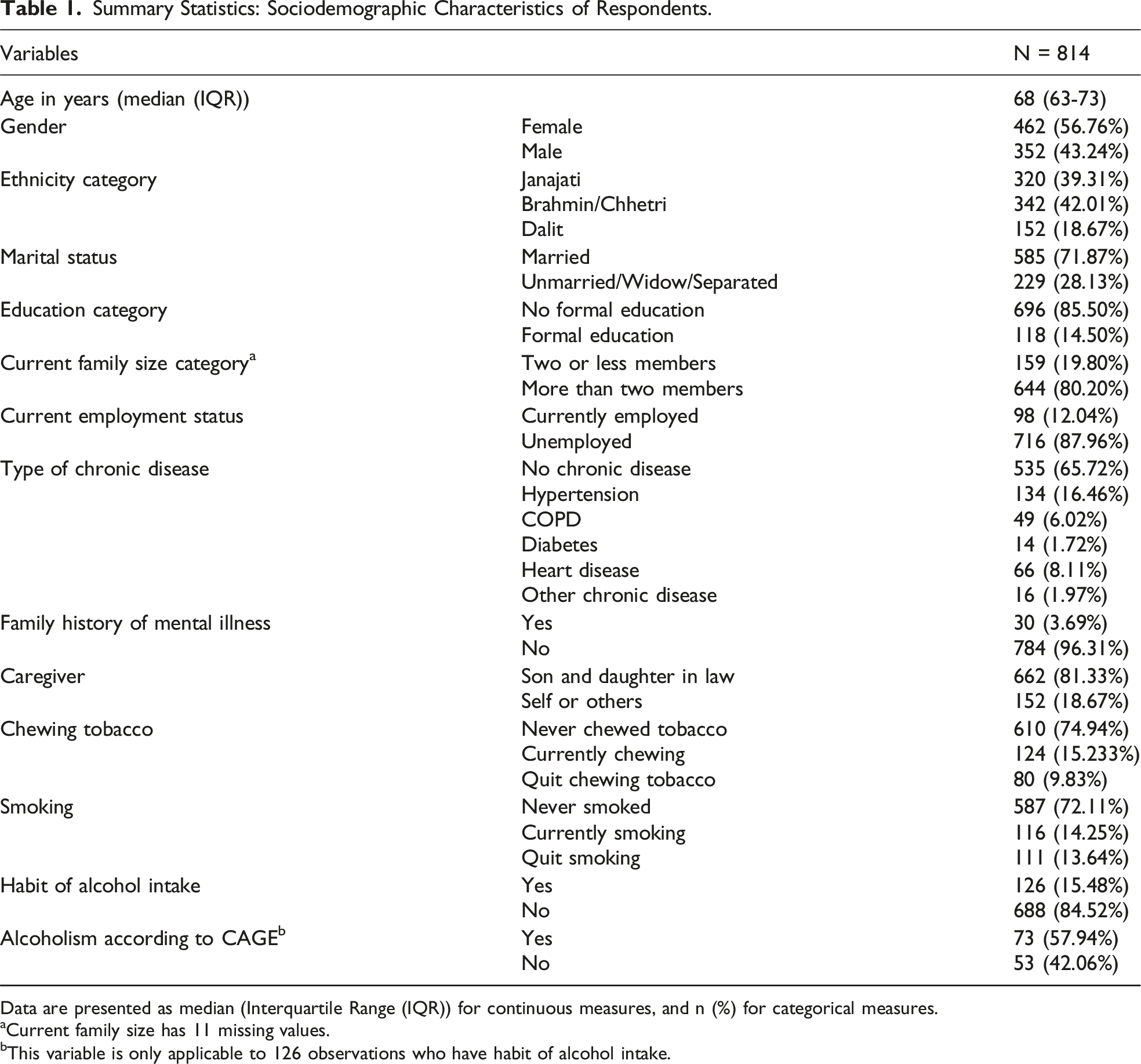
Data are presented as median (Interquartile Range (IQR)) for continuous measures, and n (%) for categorical measures.
aCurrent family size has 11 missing values.
bThis variable is only applicable to 126 observations who have habit of alcohol intake.
Prevalence of Well-Being and Mental Health Conditions
Prevalence of Mental Health Conditions.
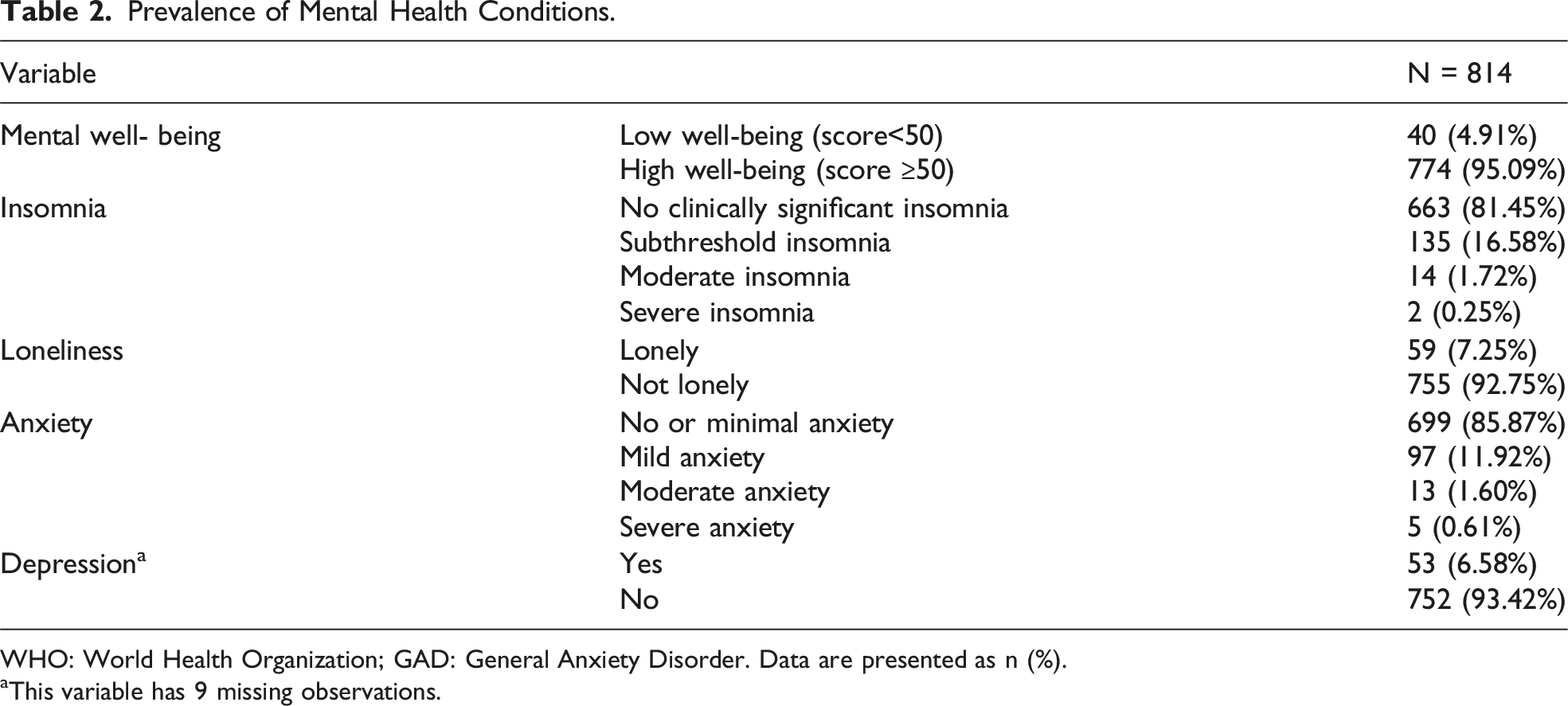
WHO: World Health Organization; GAD: General Anxiety Disorder. Data are presented as n (%).
aThis variable has 9 missing observations.
Regression Findings
Factors Associated With Anxiety, Well-being, Loneliness, Depression, and Insomnia Using Logistic Regressions.
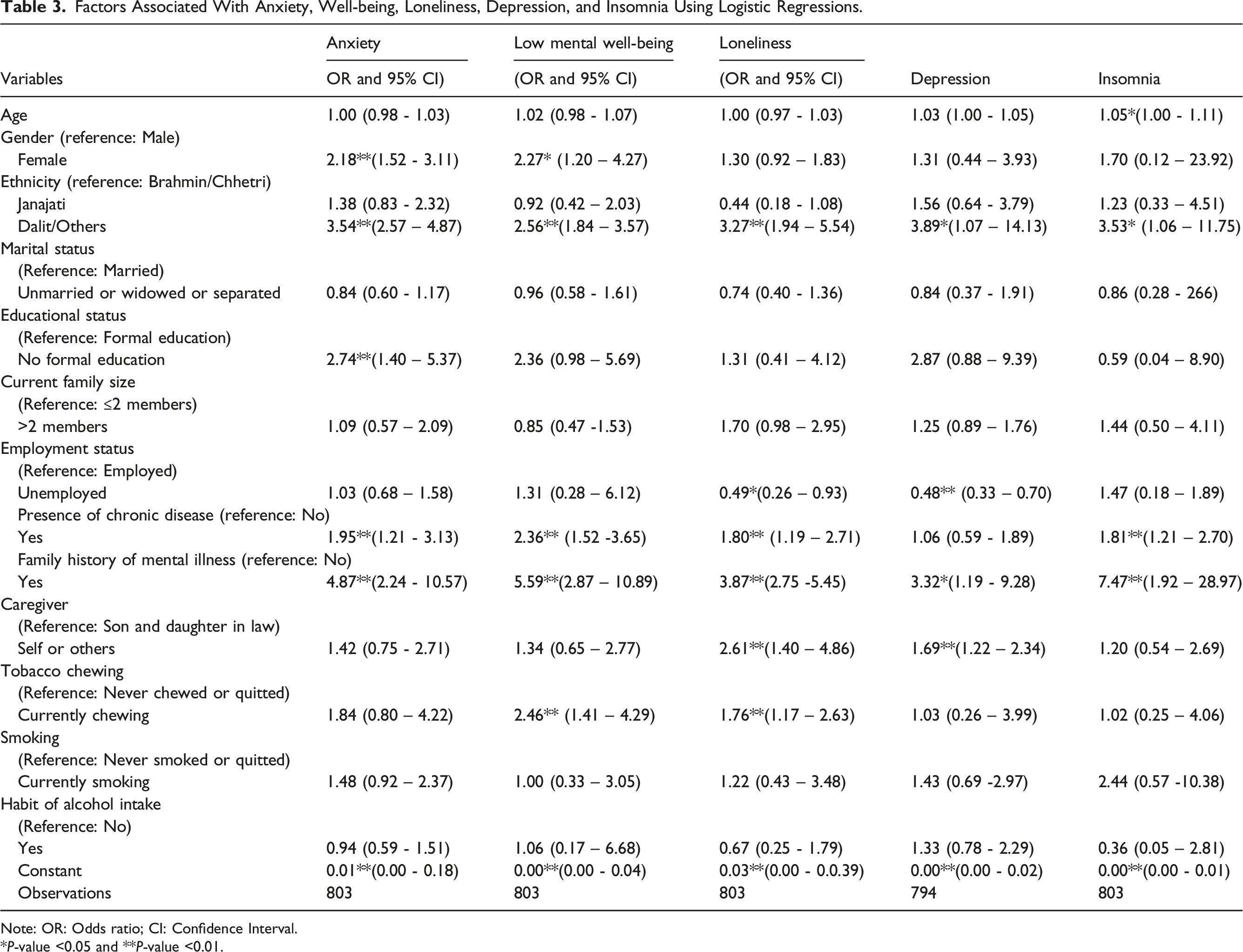
Note: OR: Odds ratio; CI: Confidence Interval.
*P-value <0.05 and **P-value <0.01.
Older adults from the Dalit ethnic group had 2.6 times higher odds of reporting low well-being compared to those from the Brahmin/Chettri group (OR: 2.56; 95% CI:1.84 – 3.57). Similarly, those with a chronic disease (OR: 2.36; 95% CI: 1.52 – 3.65), those who currently chew tobacco (OR: 2.46; 95% CI: 1.41-4.29), and those with a family history of mental illness (OR: 5.59; 95% CI: 2.87 – 10.89) had significantly higher odds of low well-being compared to their respective counterparts.
Compared to older men, the odds of reporting anxiety were 2.2 times higher (OR: 2.18; 95% CI: 1.27 - 3.73) among older women. Dalit older adults had 3.5 times higher odds of reporting anxiety than those from the Brahmin/Chettri ethnic group (OR: 3.54; 95% CI: 2.57 – 4.87). Additionally, older adults with no formal education (OR: 2.74; 95% CI: 1.40 – 5.37), chronic disease (OR: 1.95; 95% CI: 1.21 - 3.13), and a family history of a mental illness (OR: 4.87; 95% CI: 2.24 – 10.57) had significantly higher odds of anxiety compared to their respective counterparts.
Similar patterns were observed for loneliness and depression. The odds of reporting loneliness among older adults from the Dalit ethnic group were 3.3 times higher compared to those from the Brahmin/Chhetri group (OR: 3.27; 95% CI: 1.94 – 5.54). Similarly, older adults with a family history of mental illness (OR: 3.87; 95% CI: 2.75 – 5.45), those with a history of chronic disease (OR: 1.80; 95% CI: 1.19-2.71), and those who currently chew tobacco (OR: 1.76; 95% CI: 1.17-2.63) had significantly higher odds of reporting loneliness compared to their counterparts. Unlike the patterns observed for low well-being, and anxiety, the older adults who reported self-care had significantly higher odds of reporting loneliness compared to those whose primary caregiver were their son and daughter-in-law (OR: 2.61; 95% CI: 1.40 – 4.86). Regarding depression, older adults from the Dalit community (OR: 3.89; 95% CI: 1.07 – 14.13) and those with a family history of mental illness (OR: 3.32; 95% CI: 1.19 - 9.28), and those who reported self-care (OR: 1.69; 95% CI: 1.22 – 2.34) had significantly higher odds of experiencing depression compared to their respective counterparts. Similar to other mental conditions, the odds of reporting insomnia among older adults with a family history of chronic disease (OR: 1.81; 95% CI: 1.21 – 2.70), those with a family history of mental illness (OR: 7.47; 95% CI: 1.92 – 28.97) were significantly higher compared to their respective counterparts.
Discussion
Our study found that only a minority of the older adults in Dang district of Nepal reported having low well-being. However, loneliness, anxiety, and depression were more prevalent. Most of our study population reported good sleep health with a minority of them reporting moderate or severe insomnia. Further, we found that mental health conditions among older adults are associated with multiple factors (eg, gender, ethnicity, educational status, presence of chronic illnesses to the family history of mental illness).
The prevalence of mental health conditions among older adults in our study was comparatively lower than that reported in previous studies. For example, a meta-analysis showed that the pooled prevalence of depression among older adults in Nepal was 52%, 17 with most studies having prevalence more than 50%,73-76 and only two studies showing a prevalence of less than 20%.20,77 Similarly, a systematic review showed that the prevalence of anxiety among older adults ranged from 21.7% to 32.3%. 16 Chalise and colleagues even reported an incidence rate of 68.7% of loneliness among the older adults in Kathmandu. 48 In contrast, our findings showed lower prevalence rates for depression, anxiety, loneliness, and insomnia. Several factors may explain this discrepancy. First, our study was conducted in rural community settings rather than hospitals or old age homes. The higher rate of mental health conditions in hospital can be due to sample selection bias, as patients in care settings are more likely to have coexisting physical or psychological conditions. Higher rate in old-age homes may be due to feeling of powerlessness, lower self-esteem or limited social interaction in institutional settings. 78 Second, older adults in rural areas often live in multi-generational households, which can provide stronger social support and reduce loneliness. Finally, and more importantly, differences in sensitivities of the assessment instruments may have contributed to variation in prevalence. For example, our estimate of insomnia (2%) was substantially lower than the 46.2% reported by Bajracharya et al. (2022) among older adults. 31 One factor of such a stark difference in prevalence may be due to the use of different tools to measure insomnia. They used Pittsburgh Insomnia Rating Scale, which is a longer and more sensitive instrument, capturing a broad range of sleep-related disturbances, whereas our study used ISI, which identifies only clinically significant insomnia. Such variations highlight the importance of considering methodological and contextual factors when interpreting prevalence rates across studies.
Our study identified important contextual findings: individuals from Dalit community were significantly more likely to experience low well-being, anxiety, loneliness, and depression. Although our study was unable to accurately discern the reasons behind it, historical and systematic inequities may play a crucial role. Dalit community in Nepal is historically marginalized, considered a lower caste and faced barriers such as limited access to education, healthcare, and economic opportunities.67,68,79 Our finding is consistent with social stratification theory, which argues that subjective well-being tends to be highest among those who have greater access to resources and opportunities. 80 In addition, these results can be better understood through the lens of the cumulative advantage/disadvantage theory,81,82 which posits that advantages or disadvantages tend to amplify over time, leading to increasing divergence in outcomes for advantaged and disadvantaged groups. Studies have shown that Dalits are disproportionately affected by poverty, have lower literacy rates, and more likely to face barriers in medical care due to caste-based discrimination and economic hardship.67,68,79 These persistent inequities can lead to chronic stress, social isolation and reduced resilience,83,84 which are the known risk factors for mental health illnesses. 6
Another notable finding from our study is that mental health conditions among older adults with a family history of mental illnesses, are significantly more prevalent. This may be due to a combination of genetic and environmental influences. Genetically, certain inherited traits can increase the susceptibility of mental health conditions like depression and anxiety. 6 Environmentally, living with or caring for family members with mental illness in Nepali context, where mental health is often stigmatized, 85 may lead to higher stress levels, reduced social networks, and the gradual development of less effective coping mechanisms over time.
In addition, our study revealed that older adults who took care of themselves or had caregivers other than son and daughter-in-law were more likely to experience loneliness. In Nepal’s traditional social structure, sons and daughter-in-law are considered the primary caregivers for older adults. When this traditional caregiving arrangement is absent, the older adults may face reduced family interaction, companionship, and a diminished sense of traditional care, leading to a higher likelihood of loneliness. Moreover, given that there is a high out-migration of the young population from the country for employment and other opportunities, an increasing number of older adults are left without traditional care. It is likely that this demographic trend could be contributing to an increase in loneliness among Nepal’s older adult population.
Further, we found that the presence of chronic diseases among the older adults increases the likelihood of anxiety and well-being. Chronic diseases evidently increase physical discomfort, lifestyle disturbance, and increase medical and financial strain.86,87 Other than the above-mentioned predictors, older women in western Nepal had a higher risk of anxiety compared to male counterparts, which is consistent with the previous studies conducted in Nepal20,88 and internationally. 89 This gender difference was not observed for depression, insomnia and low well-being. Several factors may explain this pattern. First, older women in rural Nepal may face greater financial uncertainty in later life due to limited financial independence and reliance on family support throughout the life. 90 They may also experience the cumulative effects of life-long gender based discrimination, including restricted decision making power and unequal access to education and health care, 91 which may further heighten psychological stress. Moreover, evidence suggests that women are generally more likely to recognize and report anxiety symptoms,92-94 whereas distress related to depression may be less openly discussed due to stigma associated with depression. 95
Our findings have several policy implications. First, given that more than one in ten people in Nepal are older adults and a significant proportion of them experience a wide range of mental health conditions that can be detected and managed at the community level, the government and the concerned stakeholders should prioritize community-level geriatric mental health interventions. The Nepal government adopted National Mental Health Care Program (NMHCP) in 2022 which emphasizes on practical, equitable and need based mental health care, by delivering basic package of mental health services at PHC level. Given that older adults are more vulnerable to mental health illnesses, and their mental health care needs are different than others, the package can be tailored to the specific needs of older adults. Second, our study showed that certain populations, such as those in the marginalized Dalit community and individuals with a family history of mental illnesses, are disproportionately likely to suffer. One of the guiding principles of NMHCP is equity, therefore, older adults from these vulnerable groups need targeted community-based mental health programs. Such programs could include targeted outreach efforts, counseling services, and culturally sensitive interventions–such as community-based programs that acknowledge caste-related stigma, strengthen family and social support systems and integrate local language–to address the mental health needs of older adults, particularly among Dalit communities. Third, this research is a part of the community mental health program for older adults conducted by the HFN in specific wards of a district. However, to reach a wider population, there is a need to integrate such programs within the country’s primary health care system. Fourth, considering the link between chronic diseases and mental health disorders in older adults, there is a need to integrate mental health screening and support into the management of non-communicable diseases. Nepal adopted the prevention of non-communicable disease (PEN) package, developed by the World Health Organization, in 2016. 47 It includes early detection and management of the most common non-communicable diseases, such as coronary artery diseases, diabetes, chronic obstructive pulmonary diseases, and cancer at local-level health facilities. Exploring the feasibility and efficiency of integrating mental health screening of older adults into this package and other existing community-level interventions may serve as a cost-effective approach to address growing concerns among the older adults.
Strengths and Limitations
Our study is likely the first to simultaneously estimate the prevalence of comprehensive mental health conditions—anxiety, well-being, loneliness, insomnia, and depression—among the older adult population in rural Nepal. This provides valuable insights into the wide spectrum of geriatric mental health conditions in the country. Further, our study explored socio-demographic characteristics associated with geriatric mental health conditions, offering evidence for the policymakers to design contextual interventions. Despite these strengths, our study has several limitations. First, since the study was conducted in a single Western district, our findings may not be representative of other districts, provinces, or the nation as a whole. Therefore, there is a need to conduct district, province, and national-level studies to accurately estimate the burden of geriatric mental health conditions. Second, our study was a part of the community-based intervention to strengthen mental health and general well-being among the older adults, which might have introduced reporting bias. Because data were collected from the wards where HFN operates community mental health programs, the prevalence of mental health conditions observed in this study may be slightly lower than in the areas without such programs. Nevertheless, the setting provided an ethically appropriate and logistically feasible context for studying mental health among older adults in rural Nepal. Third, we included a wide range of tools to assess mental health conditions among the older adults. While this approach allowed us to capture geriatric mental health conditions comprehensively, it may have been burdensome for the participants. Although our community mental health workers were trained to reduce reporting bias and collect quality data, we cannot eliminate this concern completely. Fourth, while we widely used previously adapted tools in the Nepali context, we did not perform validity and reliability tests for these tools. Therefore, there may be unmeasured variation in how these tools perform among older adults in rural Nepal. Fifth, although we identified factors associated with several geriatric mental health conditions, these associations do not imply causation due to the cross-sectional nature of the study and related methodological limitations. Nevertheless, our study provides a comprehensive picture of geriatric mental health conditions in western Nepal, shedding light on the disproportionate burden among marginalized and vulnerable populations.
Conclusion
Our study offers important insights into the prevalence and determinants of a wide range of geriatric mental health disorders in a district in western Nepal. Notably, our study revealed a disproportionate burden of geriatric mental health disorders among individuals from Dalit community and those with a family history of mental illnesses, potentially highlighting long-standing social and economic inequalities. In addition to these findings, a higher likelihood of mental health problems among older adults with chronic diseases and those who lack traditional care arrangements highlight the need for targeted interventions. Future research should aim to expand our approach in a large-scale population to build robust evidence that can guide policymakers for regional or national interventions.
Supplemental Material
Supplemental material - Aging, Mental Health and Ethnic Disparities: Understanding Geriatric Mental Health in Western Nepal
Supplemental material for Aging, Mental Health and Ethnic Disparities: Understanding Geriatric Mental Health in Western Nepal by Mukesh Adhikari, MPH, Prayas Gautam, MPH, Sushrusha Arjyal, MD, Binita Adhikari, MSPH, Pratigya Gyawali, MBBS, Sanjay Yadav, MD, Theodore A. Stern, MD, Shreedar Paudel, MD in Journal of Geriatric Psychiatry and Neurology
Footnotes
Acknowledgements
We would like to thank the older adults who participated in our research project; we appreciate their time and efforts. We are thankful to the staff of Health Foundation Nepal who helped in data collection and program implementation at community level.
Author Contributions
All authors contributed voluntarily to designing, conducting, and publishing this article.
Declaration of Conflicting Interests
The authors declared no potential conflict of interests with respect to research design, conduction, authorship and publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research project was conducted under the community mental health program for older adults by Health Foundation Nepal (HFN), a non-profit organization registered in the US and Nepal. During the study period, Prayas Gautam was a program officer and reimbursed by the HFN.
Ethical Consideration
The Nepal Health Research Council Ethical Review Board approved this research (Protocol Registration # 385/2023).
Supplemental Material
Supplemental material is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
