Abstract
Background
Dementia affects 55 million people worldwide and low muscle mass may be associated with cognitive decline. Mid-arm muscle circumference (MAMC) correlates with dual-energy Xray absorptiometry and bioelectrical impedance analyses, yet are not routinely available. Therefore, we examined the association between MAMC and cognitive performance in older adults.
Methods
We included community-dwelling adults ≥55 years from the China Health and Nutrition Survey. Cognitive function was estimated based on a subset of the modified Telephone Interview for Cognitive Status (0-27, low-high) during years (1991, 1993, 1997, 2000, 2004, 2006, 2009, 2011, 2015, 2018). A multivariable linear mixed-effects model was used to test whether MAMC was associated with rate of cognitive decline across age groups and cognitive function overall.
Results
Of 3702 adults (53% female, 63.2 ± 7.3 years), mean MAMC was 21.4 cm ± 3.0 and baseline cognitive score was 13.6 points
Conclusion
Higher MAMC at any age was associated with better cognitive performance in older adults. Understanding the relationship between muscle mass and cognition may identify at-risk subgroups needing targeted interventions to preserve cognition.
Introduction
Dementia affects 55 million people worldwide with an incidence of 10 million new cases each year. 1 Contributing factors to the development of dementia are difficult to isolate due to the heterogeneity of the disease. However, identifying contributors are important, as dementia significantly increases an individual’s risk of morbidity and mortality. 2 Emerging evidence suggests that anthropometric and body composition characteristics, such as higher waist circumference, fat mass, body mass index (BMI), and low muscle mass, may be associated with cognitive impairment and decline.3-8 Total fat and visceral adipose fat, may be associated with worse cognitive performance in both men and women.7-10 Additionally, sarcopenia, the loss of muscle mass, strength, and function, may also be associated with cognitive decline.3,4 In fact, loss of muscle mass may be more of a sensitive marker for cognitive decline than higher levels of adiposity, while poor muscle strength or function may be more closely associated with cognitive decline than muscle mass itself.4,11-14
While anthropometric measures such as BMI and waist circumference may be conveniently measured in clinical practice, they cannot distinguish between muscle and adipose tissue. Their diagnostic accuracy contrasts with highly sensitive measures of body composition measured by computed tomography or magnetic resonance imaging.7,15,16 Certain clinical practices have the capabilities of using dual energy X-ray (DEXA) absorptiometry or bioelectrical impedance (BIA); however, each have their own limitations making it challenging to balance sensitivity and specificity vs the practicality of integrating their assessments in clinical workflows. Mid-arm muscle circumference (MAMC) is a simple, easily attainable bedside measure that has been found to correlate strongly with BIA and DEXA measures of muscle mass.17,18 While MAMC has known limitations, including the absence of sex-specific global cut offs, it may be a cost-effective, non-invasive marker of sarcopenia. Few studies have examined the potential association between MAMC and cognitive performance in older adults. The purpose of this study was to examine the association between MAMC and cognitive performance in older adults. If successful, our findings could identify potential areas for assessment of sarcopenic in clinical practice and identify subgroups who are high risk for targeted interventions.
Methods
Study Participants
For this analysis, we used data from the China Health and Nutrition Survey (CHNS). CHNS is an ongoing household-based cohort study that includes participants across 12 provinces and 3 mega-cities and across eleven rounds of surveys from 1989 to 2018. A full explanation of the cohort designs is described in Socioeconomic gradients in the Westernization of diet in China over 20 years by Green et al. 19 Each CHNS participant provided a written informed consent, and the study was approved by institutional review board from National Institute for Nutrition and Food Safety, Chinese Center for Disease Control Prevention, and the University of North Carolina at Chapel Hill. Further information on survey procedures and the rationale of the CHNS can be found elsewhere. 20
Our analytical sample consisted of data collected at 6 rounds of the survey (1997, 2000, 2004, 2006, and 2015) where questions regarding cognitive function were asked. MAMC was measured in all survey years (1991, 1993, 1997, 2000, 2004, 2006, 2009, 2011, 2015, and 2018). However, to ensure comparability between the time of MAMC assessment and cognitive function measures, we restricted our analysis to only the years where cognitive function data was collected. Since mega-cities were added to the sample starting in 2011, and there are noticeable differences between mega-cities and provinces, we only included individuals from the 9 provinces in the sample in 1997 to maintain consistency across time. Cognitive function was assessed in individuals 55 years of age or older, and therefore our eligible sample included 8330 individuals. We excluded 4564 individuals with only 1 cognitive measure to ensure we could examine the association between MAMC and cognitive decline with cognitive assessment data fully completed. We also excluded 41 individuals missing either MAMC or triceps skinfold measurement, and 23 individuals missing covariate data for a final analysis sample of 3702 individuals with an average number of 2.6 visits per individual. Individuals excluded from our eligible sample were older (
Mid-arm Muscle Circumference (MAMC)
Triceps skinfold measurement (TSF) and mid-arm arm muscle circumference (MAMC) were collected by trained health care professionals according to standardized protocols. MAMC was measured at the halfway point between the olecranon process of the ulna and the acromion process of the scapula. TSF was measured by skinfold calipers using a similar approach to Chen et al: to “the nearest .5 mm at the triceps on the right arms (between the tip of the olecranon process of the ulna and the acromion process of the scapula).” 21 For both TSF and MAMC, 3 measurements were collected on each subject with the average calculated and used in all analyses.
Our primary exposure of interest was MAMC which was derived based on validated equations from TSF and MAMC.
22
Arm muscle area (AMA, men) = (MAMC − π × TSF)2/4π − 10 cm2 Arm muscle area (AMA, women) = (MAMC − π × TSF)2/4π − 6.5 cm2 Mid-arm area (MAA) = Arm fat area (AFA) = MAA − AMA
We additionally examined whether the association was consistent for other metrics including TSF as well as 3 other measures derived from a combination of TSF and MAMC based on validated equations including mid-arm area (MAA), arm muscle area (AMA), and arm fat area (AFA).
Cognitive Function
Cognitive function was assessed in person via interview using a modified version of the Telephone Interview for Cognitive Status. 23 This is a standardized, validated cognitive screening, and each survey collector was trained in properly administering this survey per a standardized administration protocol. More specifically, this included immediate and delayed recall of a list of 10 words, counting backwards from 20 to zero, serial 7 subtraction, and orientation. From these components, a global cognitive score was calculated. For this score, 1 point per word was assigned for each correct word for the immediate and delayed recall, for a total of 20 points maximum. If the participant successfully counted backwards on the first attempt, they were assigned 2 points, and 1 point was assigned if the participant was unsuccessful at the first attempt but successful on the second attempt. One point for each answer, for a maximum of 5 points, were assigned based on successful subtraction of serial sevens. Scores therefore could range from zero to 27, with higher score assigned to those with better performance on the cognitive function assessment. Verbal memory scores were calculated based on 1 component of the global cognitive function score, the immediate and delayed word recall, for a total of 20 points. Cognitive decline was considered to be any decrease in score in any age bracket over the study period.
Covariates
Information about age, sex, highest education level achieved, and marital status were collected from survey questionnaires. Age was categorized into 5-year age groups, 55-60, 60-65, 65-70, 70-75, and 75 years or above. Education level was categorized into 3 categories: no formal education completed, primary school completed, or additional post-primary school completed. Marital status was classified as married or not. Based on a series of questions about formal and informal occupational employment, employment status was derived and classified as “not currently working” or “currently working,” in either formal or informal employment. 24 Household income was determined from asset and economic activity and individual and household questionnaires from time-use. These values were inflated to 2018 yuan currency for comparability. Income was categorized into year-specific tertiles, to better capture relative income. Northern, Central of Southern China was the categorized region. A multicomponent and validated continuous index, derived from 12 components to capture the complexity of urbanization, was used to calculate urbanization at the community level each year. Indices included population density, economic activity, traditional markets, modern markets, transportation infrastructure, sanitation, communications, housing, education, diversity, health infrastructure, and social services. 25 As China has undergone rapid urbanization between 1997 and 2015, to account for potential cohort effects, we defined a birth cohort variable: born before 1930, between 1930-1940, between 1940-1950, between 1950-1960, or after 1960. 26
Lifestyle behaviors included smoking status and leisure activity. Smoking status was categorized as “never a smoker,” “former smoker,” or “current smoker.” The average hours per week of leisure activity was collected from a detailed time-use questionnaire. 27 Due to the small number of individuals (11.2%) participating in any leisure activity, this was categorized as “participating in none” or “some leisure activity.” A standard protocol was used to measure height based on Lynch et al’s protocol. Height was measured, “without shoes, to the nearest .1 cm using a portable stadiometer” and weight, “without shoes and in light clothing, to the nearest .1 kg on a calibrated floor scale to generate BMI (kg/m2).” 24 BMI was calculated by dividing the participant’s weight in kilograms by height in meters squared, and was categorized into underweight (<18.5 kg/m2, normal weight (18.5-23 kg/m2), overweight (23-27.5 kg/m2) or obesity (≥27.5 kg/m2) based on WHO cut points for Asian populations. 28 A participant was defined as having had a history of a stroke or myocardial infarction, diabetes, or hypertension based on self-report of a doctor’s diagnosis.
Statistical Methods
Descriptive statistics were calculated for the baseline visit, overall and by age group and sex at baseline. Tests for differences in means or percentages across age groups at baseline were estimated using ANOVA or Chi-squared test for continuous and categorical variables respectively. Linear mixed effects models were used for all other analyses to account for correlation due to data collected across multiple years for each individual and correlation within individuals living in the same community. We include both a random intercept and a random slope at the individual and community level. Given there are known age-related declines in cognitive function, age was used as the timescale given the primary question of interest was to determine whether age-related declines in cognitive function varied by MAMC. Using these models, we first examined whether cognitive decline was associated with MAMC, specifically using an interaction term between age group (55-60, 60-65, 65-70, 70-75, and 75 years or above) and MAMC. To aid in interpretation and visually evaluate whether there was any interaction, adjusted estimates of cognitive function were estimated from the model with the interaction term at the mean MAMC for our sample and at a MAMC value 1 standard deviation above the mean. Additionally, we estimated the rate of decline between each age group for these same 2 different MAMC profiles. If there was no significant association with cognitive decline, as defined by an interaction term with a
Results
Descriptive Statistics for Baseline Visit by Age Group.
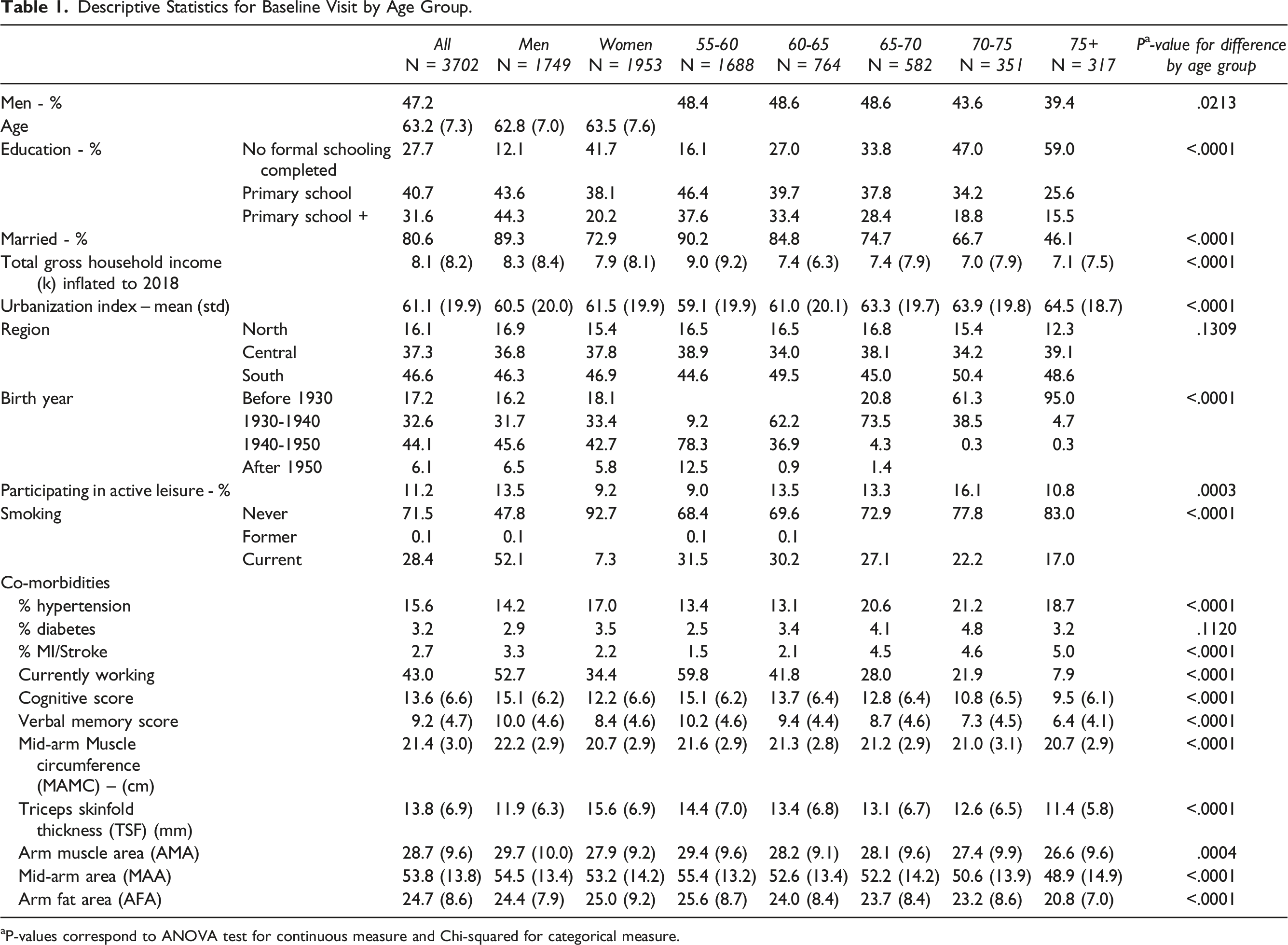
aP-values correspond to ANOVA test for continuous measure and Chi-squared for categorical measure.
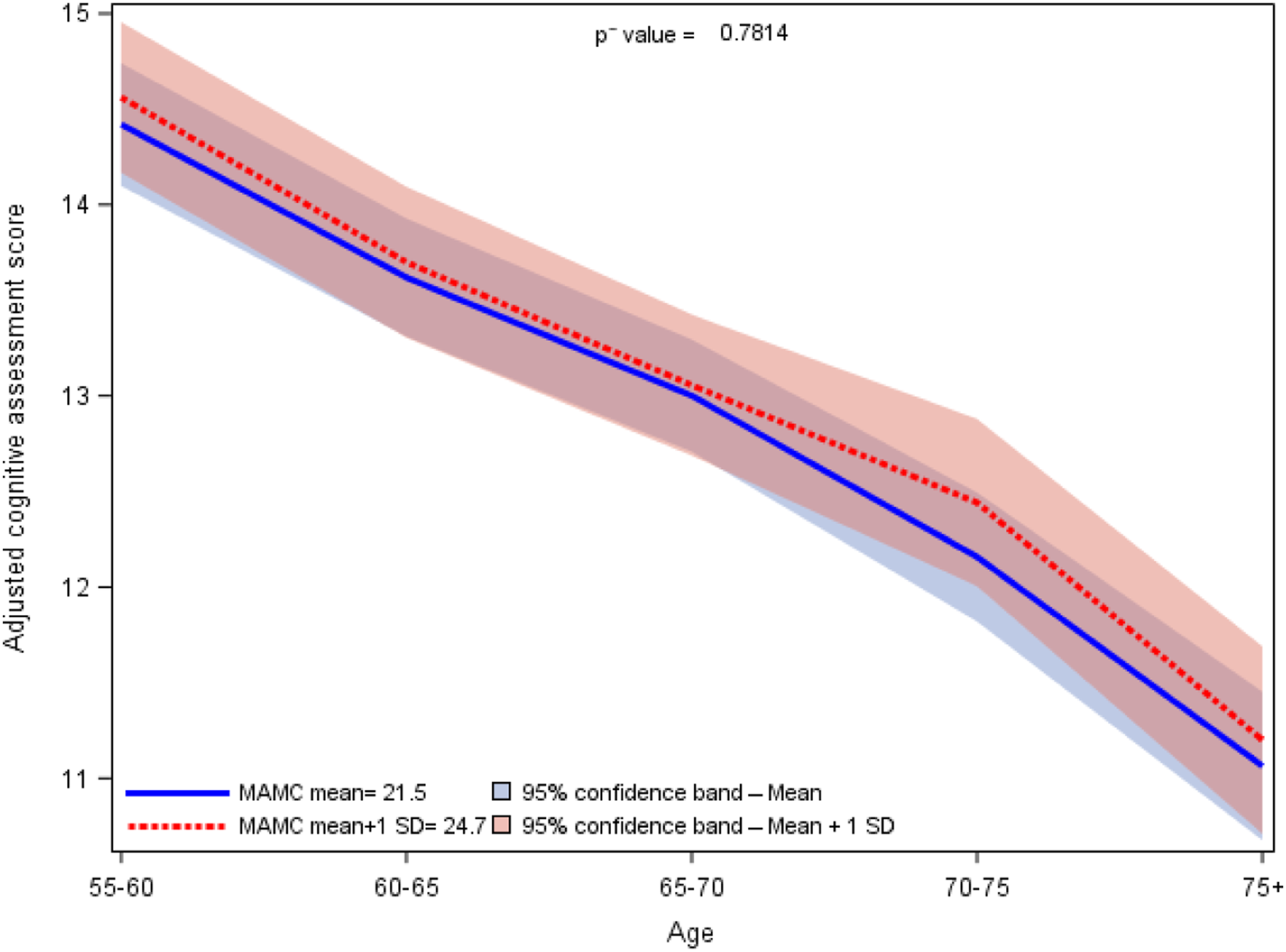
Adjusted Global Cognitive Function Scores Estimated From Minimally Adjusted Model* and Mid-arm Muscle Circumference (MAMC). *Adjusted cognitive assessment scores are predicted from a model controlling for sex, education, marital status, income, urbanization index, birth cohort, region, working status, and include MAMC, age group and an interaction term between age group and MAMC. ∼
Given we found no evidence of differences in the age-related decline by cognitive function (Figure 2), all subsequent model results are based on the models without an interaction term, which assumes similar associations between MAMC and cognitive function across all ages. Figure 2 specifically shows no difference between high and low MAMC for cognitive decline across age groups. Higher MAMC was associated with higher cognitive function across all ages (Table 2). In minimally adjusted models, each 1 standard deviation increase in MAMC was associated with a .13 ( Adjusted estimates of rates of decline across age groups in Global Cognitive Score associated with mean MAMC and 1 standard deviation higher than mean MAMC from minimal adjusted model. Adjusted Estimates of Change in Global Cognitive and Verbal Memory Score Associated With a 1 Standard Deviation Change in MAMC Measures. *Minimally adjusted model included adjustment for sex, education, marital status, income, urbanization index, birth cohort, region, and working status and include MAMC and age group. ***Fully adjusted model included all covariates from the minimally adjusted model as well as adjustment for lifestyle behaviors including leisure activity and smoking status, weight category, and self-reported diagnosis of hypertension, diabetes and myocardial infarction or stroke and include MAMC and age group.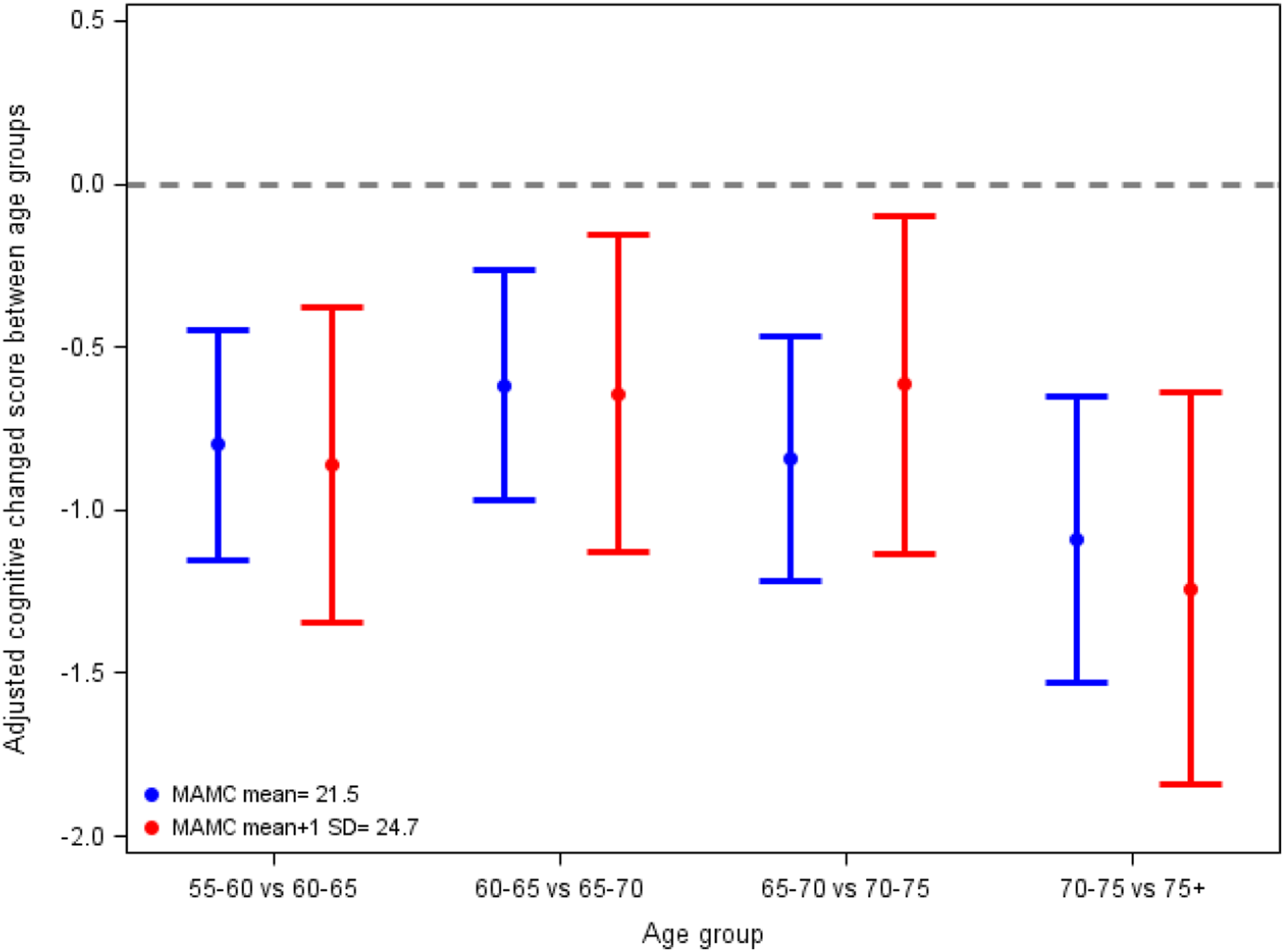
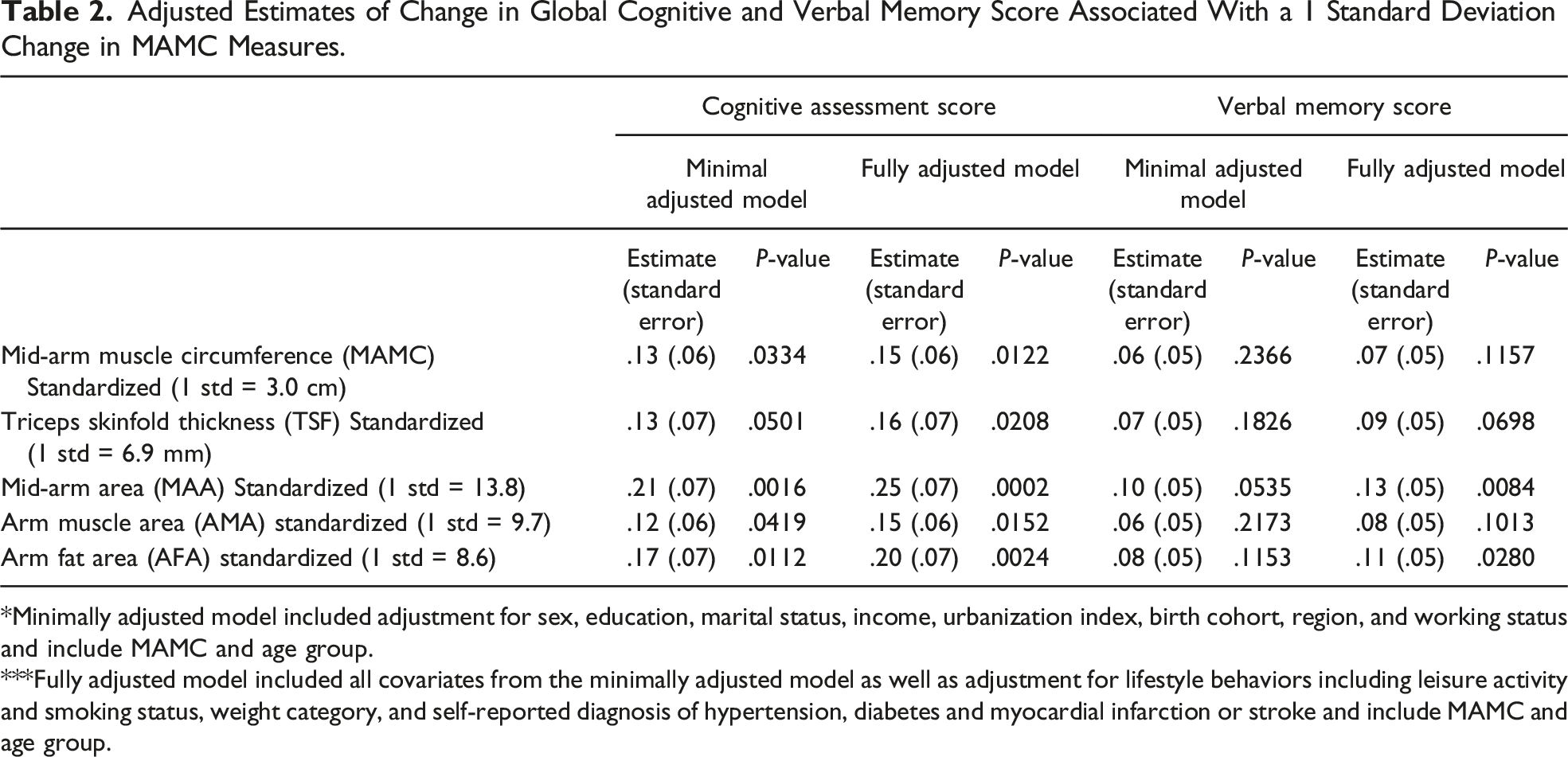
We also found consistently significant positive association between global cognitive function and other measures for both minimally (TSF (.13 (SE .07),
There were also consistently positive associations, although not always statistically significant, between TSF, MAA, AMA and AFA and verbal memory scores in both minimally and fully adjusted models (Table 2). For MAA and AFA we found a significant positive association with verbal memory score in fully adjusted models; with a 1 standard deviation higher MAA and AFA associated with a .13 (.05 SE) (
As with the overall models, in sex-stratified models we found no evidence that MAMC was associated with decline in global cognitive function (Supplemental Figure 3(a):
Adjusted Estimates of Change in Global Cognitive and Verbal Memory Score Associated With a 1 Standard Deviation Change in MAMC Measures Stratified by Sex.
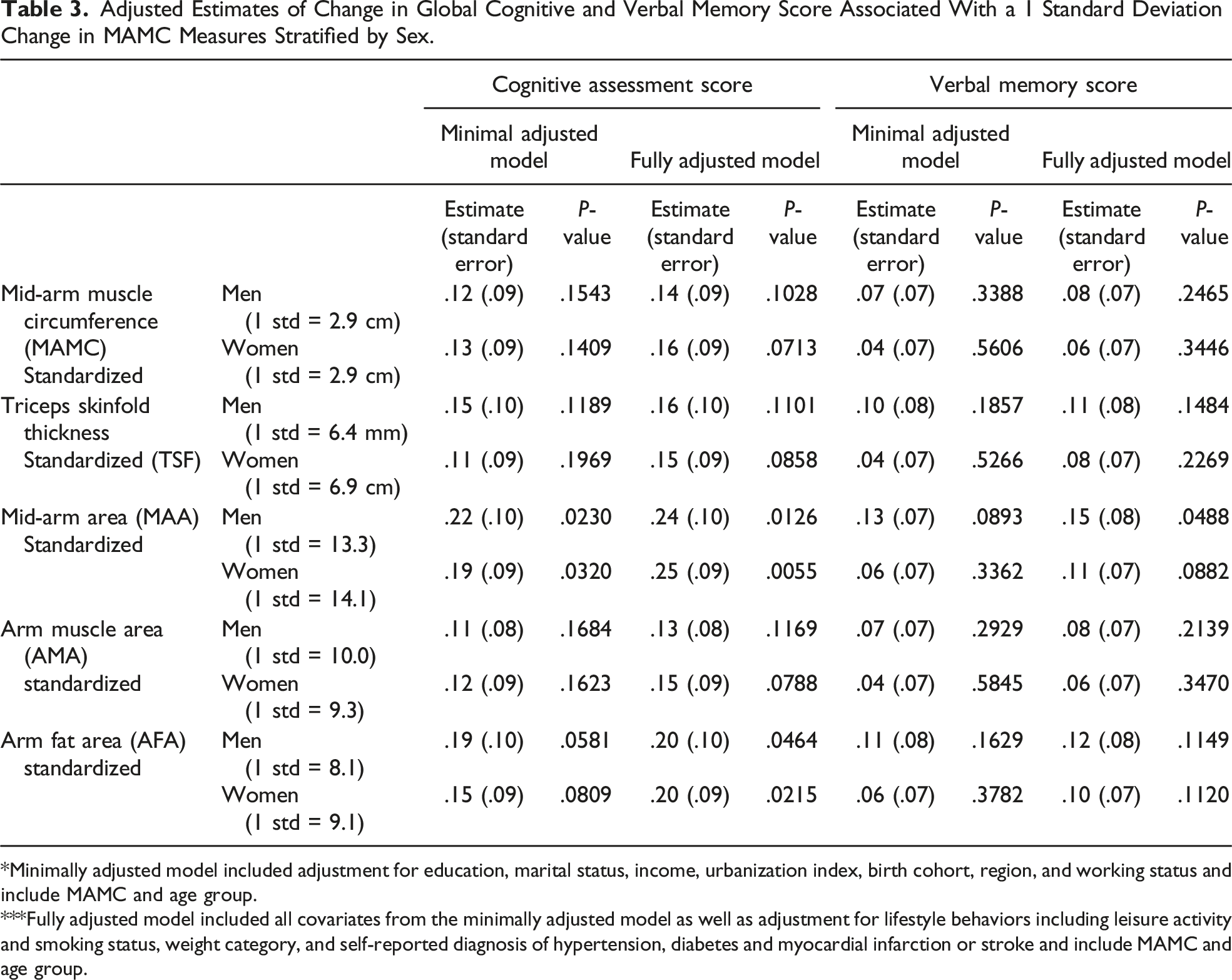
*Minimally adjusted model included adjustment for education, marital status, income, urbanization index, birth cohort, region, and working status and include MAMC and age group.
***Fully adjusted model included all covariates from the minimally adjusted model as well as adjustment for lifestyle behaviors including leisure activity and smoking status, weight category, and self-reported diagnosis of hypertension, diabetes and myocardial infarction or stroke and include MAMC and age group.
Discussion
While MAMC was not associated with rate of cognitive decline across age groups, our findings suggest that higher MAMC is associated with better cognitive performance. Although not reaching statistical significance, we found positive associations between multiple arm muscle mass measurements and cognitive performance. Identifying the association between muscle mass indices with cognition in older adults may shed light on subgroups of the population who might best be targeted for interventions to mitigate the natural decline in muscle mass and preserve cognitive function.
While we observed an association between MAMC and better cognitive performance, there may have been environmental variables impacting the observed trajectories. For example, cultural changes were taking place in China during the study period, which may have impacted the observed trends. There was a notable increase in the rates of smoking and a decline in the proportion of population with formal schooling over the study time period, which may have negatively impacted and cognitive performance and confounded the relationship between body composition and cognition.30,31 These environmental factors may confound the association between MAMC and cognitive function, as smoking and lower education levels are associated with cognitive decline. 32 However, higher MAMC was associated with better global cognitive function even when controlling for environmental variables, with no differences between sex (Table 1), suggesting these associations may be independent of behavioral factors. The lack of statistically significant association between mid-arm anthropometrics and verbal memory score may suggest that, for this population, the attention aspect of cognition (e.g., ability to complete serial sevens) may be more related to MAMC than memory (e.g., delayed word recall).
Our data suggests that MAMC may be a less expensive and more accessible tool than BIA and DEXA to accurately quantify muscle mass as a predictor for future cognitive performance.7,9,10,15,17,18 MAMC may overestimate muscle content for individuals with sarcopenic obesity as MAMC does not consider intramuscular fat. MAA, AMA, and AFA present the same limitation. In the Bunkyo Health Study, Japanese older adults with sarcopenic obesity had an increased risk of both mild cognitive impairment and dementia. 33 Because individuals with sarcopenic obesity have increased intramuscular fat that may confound MAMC and cognition associations, accurately quantifying muscle mass vs fat content using gold standard imaging (e.g., MRI) may be necessary to understand the most accurate relationship between anthropometrics with cognition.
To our knowledge, this is one of the few studies examining the association of MAMC with cognition in a period of rapid urbanization. Sarcopenia is impacted by environmental factors such as nutrition, lifestyle, education, and urbanization, all of which were changing in China during the study period, limiting generalizability to other settings. An additional strength of this study is our analysis of a large heterogeneous data set. The applicability of these results is limited by the retrospective nature of the study and the heterogeneity of sarcopenia, which limits the causative relationships between variables. Additionally, participants who were excluded from the study differed from included participants in terms of demographics and anthropometrics (Supplemental Table 2).
Conclusion
We observed a positive association between MAMC and cognitive performance in older adults. Better understanding the relationship between anthropometric measures and cognition may help identify individuals at highest risk for cognitive decline. Understanding the relationship between muscle mass and cognition may identify at-risk subgroups for targeting individual for interventions to preserve cognition. Future studies need to examine the MAMC and cognition relationship over time and across different populations for generalizability.
Supplemental Material
Association Between Mid-arm Muscle Circumference and Cognitive Function: A Longitudinal Study of Chinese Adults
Supplemental Material for Association Between Midarm Muscle Circumference and Cognitive Function: A Longitudinal Study of Chinese Adults by Hillary B. Spangler, David H. Lynch, Annie Green Howard, Hsiao-Chuan Tien, Shufa Du, Bing Zhang, Huijun Wang, Penny Gordon Larsen, and John A. Batsis in Journal of Geriatric Psychiatry and Neurology
Footnotes
Acknowledgments
We thank the National Institute for Nutrition and Health, China Center for Disease Control and Prevention, Beijing Municipal Center for Disease Control and Prevention, and the Chinese National Human Genome Center at Shanghai. We are also grateful for infrastructure provided by the Carolina Center for Population Aging and Health.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research uses data from China Health and Nutrition Survey (CHNS). We are grateful to research grant funding from the National Institute for Health (NIH), the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) for R01HD30880, the National Institute on Aging (NIA) for R01AG065357, the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) for R01DK104371 and P30DK056350 and the National Institute of Heart, Lung and Blood for R01HL108427, the NIH Fogarty grant D43 TW009077 since 1989, the Carolina Population Center for Carolina Population Center for P2CHD050924 and P30AG066615 since 1989, the China-Japan Friendship Hospital, Ministry of Health for support for CHNS 2009, Chinese National Human Genome Center at Shanghai since 2009, and Beijing Municipal Center for Disease Prevention and Control since 2011.
Supplemental Material
Supplemental material for this article is available online.
Appendix
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
