Abstract
Introduction:
There is a scarcity of literature documenting how women facing maternal morbidity issues deal with challenges to breastfeeding. This case study documents challenges faced by two women, one who underwent major abdominal surgery immediately after a Caesarean section at 32 weeks, and the other who had a primary and secondary postpartum hemorrhage with repeated hospital admissions.
Main Issue:
In the first case, the key issues for lactation were the mother–infant separation and difficulty in initiation and sustaining breastfeeding due to abdominal surgery after her Caesarean section. Early and frequent removal of milk are critical for establishing and sustaining supply and were challenging for the mother in the intensive care unit for 3 weeks. The second case involved a mother experiencing severe postpartum hemorrhage. Having lost over 3 L of blood, this mother faced a significant risk of a reduction in prolactin and activation of her milk supply. Her subsequent weakness and dyspnoea due to anaemia meant breastfeeding required extraordinary effort.
Management:
Establishing lactation under these circumstances was challenging. Both mothers needed guidance and encouragement to build up and maintain their supply and the practical support of family to care for the infant. In Case Study 1, donor milk was used and alternated with artificial breastmilk substitutes until the mother re-established her supply after discharge. In Case Study 2, the mother required help to express, position, and hold the baby while she breastfed.
Conclusion:
Despite overwhelming medical and physiological odds, it is possible to establish exclusive breastfeeding with consistent personalized health-system support/training and relentless determination.
Keywords
Introduction
It has been reported that few women meet their breastfeeding goals, let alone the gold standard for infant feeding according to the World Health Organization (WHO), which is exclusive breastfeeding for the first 6 months of life and continued breastfeeding for up to 2 years or beyond (WHO & United Nations Children’s Fund [UNICEF], 2003).
Reasons for this are multifactorial and include difficulties and lack of confidence in establishing lactation, fears of insufficient milk production, lack of self-efficacy, and medical and surgical complications, including prematurity and medication taken by the mother (Odom et al., 2013). There is a scarcity of literature documenting how women facing maternal morbidity overcome these additional challenges.
Preterm infants are particularly vulnerable, and supporting these mothers to provide their infants with tailor-made mother’s own milk is therefore essential. Equally important is the support required by mothers who face medical complications post-delivery. Multiple factors can interfere with secretory activation and establishing a milk supply. These include the stress of dealing with a preterm infant, their inability to latch to the breast, the stress of maternal morbidity, and separation of the dyad. Successful Lactogenesis II is dependent on the early initiation of human milk feeding or expressing (Fok et al., 2019; Rostom et al., 2022). Meier et al. (2017), in her review on promoting human milk feeding within a neonatal intensive care unit (NICU), reiterates how important it is to prioritize the support in the early lactation period, so mothers build up sufficient volume to meet their breastfeeding goals. Using donor human milk (DHM) does not provide the same immunological, nutritional and protective benefits of mother’s own milk (Meier, 2022).
Methodology
This paper was compiled using two case studies to provide a descriptive and observational method to present these unique circumstances, and the lactation interventions and interactions which occurred within the social environment (Tomlin & Borgetto, 2011). A case study methodology was chosen as it enabled an in-depth investigation of two complex cases to explore the nature, real-life context, and physical settings in an attempt to gain an understanding of events and their inter- relationships (Feagin et al., 1991; Stake, 1995; Yin 1989, 1994, 2009). The case studies could provide insight and understanding in similar settings (Alpi & Evans, 2019). As these cases were complex, they provided an opportunity for an holistic approach to multiple issues which needed specific physiological knowledge and psych-social considerations and support from trained healthcare professionals.
Data were gathered using observation, interviewing key informants and extended family members, and creating a data base and the chain of evidence (Stake, 1995; Yin, 1993). Analysis included examining the data in light of the literature, and inspecting the data and the patterns that emerged (Dul & Hak, 2008; Huberman & Miles, 1994). Validity was ensured by long-term observation, member checks, and two lactation peers examining the data and making the investigator’s position clear (Merriam, 1998).
Two case studies were chosen as the subjects approached the researcher for help and were supported by her; both were incapacitated by the medical challenges they faced. The researcher is an International Board-Certified Lactation Consultant (IBCLC) from Africa and worked there for many years. She is currently residing in Europe, so is equally familiar with both lactation contexts and the challenges these women faced in their particular settings. The woman in Africa in Case Study 1, delivered in a private 469 bed hospital with a Neonatal Intensive Care Unit and, although not designated Baby Friendly, did have external private Lactation Consultants available to help women who needed support. They also operated a network of Human Milk Banks. The woman in Case Study 2, delivered in a National Health hospital in Europe which is Baby Friendly and, in 2021, the maternity unit had 5,536 deliveries. The inclusion criteria were that both mothers approached the researcher for help, and faced medical challenges which made it unlikely that they would successfully establish and sustain breastfeeding. Exclusion criteria were the women not facing medical challenges and not approaching the researcher for support.
Key Messages
Establishing lactation in the context of maternal morbidity is challenging.
Access to lactation and family support improves outcomes.
Despite overwhelming odds, it is possible to establish exclusive breastfeeding with consistent support, training and resilience.
Theoretical Model
Wilson et al. (2012) in their article “Overcoming Breastfeeding Challenges: A Qualitative Inquiry” generated a model for overcoming breastfeeding challenges from the data they collected, and this was used to guide the analysis and discussion in this paper. The generated theory included anticipatory guidance; breastfeeding closely interconnected the maternal role; and resilience.
Anticipatory guidance is a concept that helps pregnant women prepare for challenges they may face when breastfeeding, by providing knowledge and guidance ahead of time and so empowering them with the intention to reduce the risk of complications.
Mercer (2004) defines maternal role as a process by which a mother becomes competent, incorporating her activities as a mother into her new identity. This includes her competence as a mother and her capacity to nurture and care for her infant. Shrestha et al. (2019) describes two components to a maternal role: the first is childcare activities, and the second is cognitive-affective, which includes attitudes of caring and tenderness.
Resilience has been defined as the process of successfully adapting to change and persevering in challenging life circumstances and pressures, and developing new coping skills, and often is found together with self-efficacy and self-confidence.
The theory depicts how the desire and anticipation to successfully breastfeed encourages the experience and reflects the natural inborn resilience to overcome the breastfeeding challenges.
There is very little understanding and research on what enables women “faced with medical complications” to successfully overcome challenges and breastfeed. Examining these two case studies may help identify ways to motivate and provide the necessary support to enable more women to succeed and reach their breastfeeding goals.
Ethics
The participants in these cases gave written consent for the stories to be published and both have reviewed the manuscript and approved it for publication. An exemption from institutional ethics approval has been provided by the Biomedical Research Ethics Committee of University of KwaZulu Natal, South Africa (EXM 004/2024).
History and Observational Assessment
These case studies describe two mothers who faced serious surgical and medical complications. Both mothers identified as female and are referred to as her/she.
Case Study 1
A Grav 3 Para 2 mother who successfully breastfed two previous children, both for 2 years each. She is a birth doula and breastfeeding advocate. She had a spontaneous rupture of membranes at 32 weeks with a placenta previa, so underwent an emergency Caesarean section. The infant was admitted to the NICU and was ventilated for a day until her condition stabilized.
On Day of Life 1 (DOL) the mother reported severe abdominal pain and distention and was diagnosed with a suspected ileus. DOL 2 she was taken to theatre to attempt to reduce abdominal distention. DOL 3, the mother was taken back to theatre for a hemicolectomy, and the removal of the caecum and part of the ileum due to a caecal bascule. She was admitted to the intensive care unit and then isolated on DOL 19 due to klebsiella infection in her wound.
The key issues for lactation were the mother–infant separation which caused stress to the dyad and is associated with difficulty in initiating and sustaining breastfeeding.
Frequent and effective pumping is demanding in an intensive care environment and more so for an acutely ill mother. This mother chose to only hand express. The infant was not able to breastfeed directly until after the mother was discharged, almost 3 weeks post-delivery. Due to maternal medication, the mother had to continue to “pump and dump” until the infant was 6 weeks old. The infant had been both tube and bottle fed and had to readjust and learn to suckle at the breast, which was challenging as she was born at 32 weeks.
Case Study 2
This woman was a Gravida 1 gestational diabetic, with a presenting breech. She had a trial for a normal vaginal delivery at 39 weeks which lasted 24 hours but ended up as an emergency Caesarean section. At the mother’s insistence, skin-to-skin was practiced in theatre where she also attempted to latch the infant. She had a primary postpartum hemorrhage (PPH) of 800 ml at delivery.
Mother and infant were discharged on DOL 2, but the mother was readmitted on DOL 7 for a further PPH, and then again on DOL 10 for a further bleed. She lost over 3 L of blood, and had a manual removal of clots and dilatation and curettage. This resulted in the separation of mother and infant. Breastfeeding had been going well until then. Twelve hours after arriving home, her infant was admitted to hospital with an unknown virus which was later diagnosed as corona virus. The mother was too weak to go with her infant, so the father accompanied him to hospital.
Furthermore, her subsequent weakness and dyspnea due to anemia meant breastfeeding required effort and help to position and hold the baby while she fed. During periods of mother–infant separation she needed assistance to express and sterilize bottles and pump. She also required someone to hold the pump in position, as she was too weak to do this. The corona virus infection further compromised the health of both the mother and her infant, introducing yet another factor which could have compromised breastfeeding.
In both instances, these mothers faced medical problems which made it extremely unlikely that they would be able to initiate lactation and establish an adequate milk supply for their infants.
Management
Case Study 1
This was a challenging time for the mother, and her nuclear and extended family. The mother was acutely ill, and spent almost 3 weeks in the ICU, and further time in a high care unit. Her infant received expressed colostrum for 2 days before surgery, after which she was fed with donor human milk (DHM). During her time in ICU, despite being critically ill, the mother managed to maintain frequent hand expressing. She received very little support for breastfeeding during her hospital stay. The hospital, although not designated as Baby Friendly, does train all staff to support breastfeeding. When she requested DHM for her infant, the private consultant expressed surprise and said he had never heard of it. The analgesics she was taking were incompatible with breastfeeding, so she had to discard her milk. While in the ICU, her infant was tube and then bottle fed with DHM. The HCP in the hospital motivated for her infant to receive DHM beyond the normal period of 2 weeks, which is the customary time to provide DHM, due to scarcity of supply. Figure 1 provides a summary timeline of events.
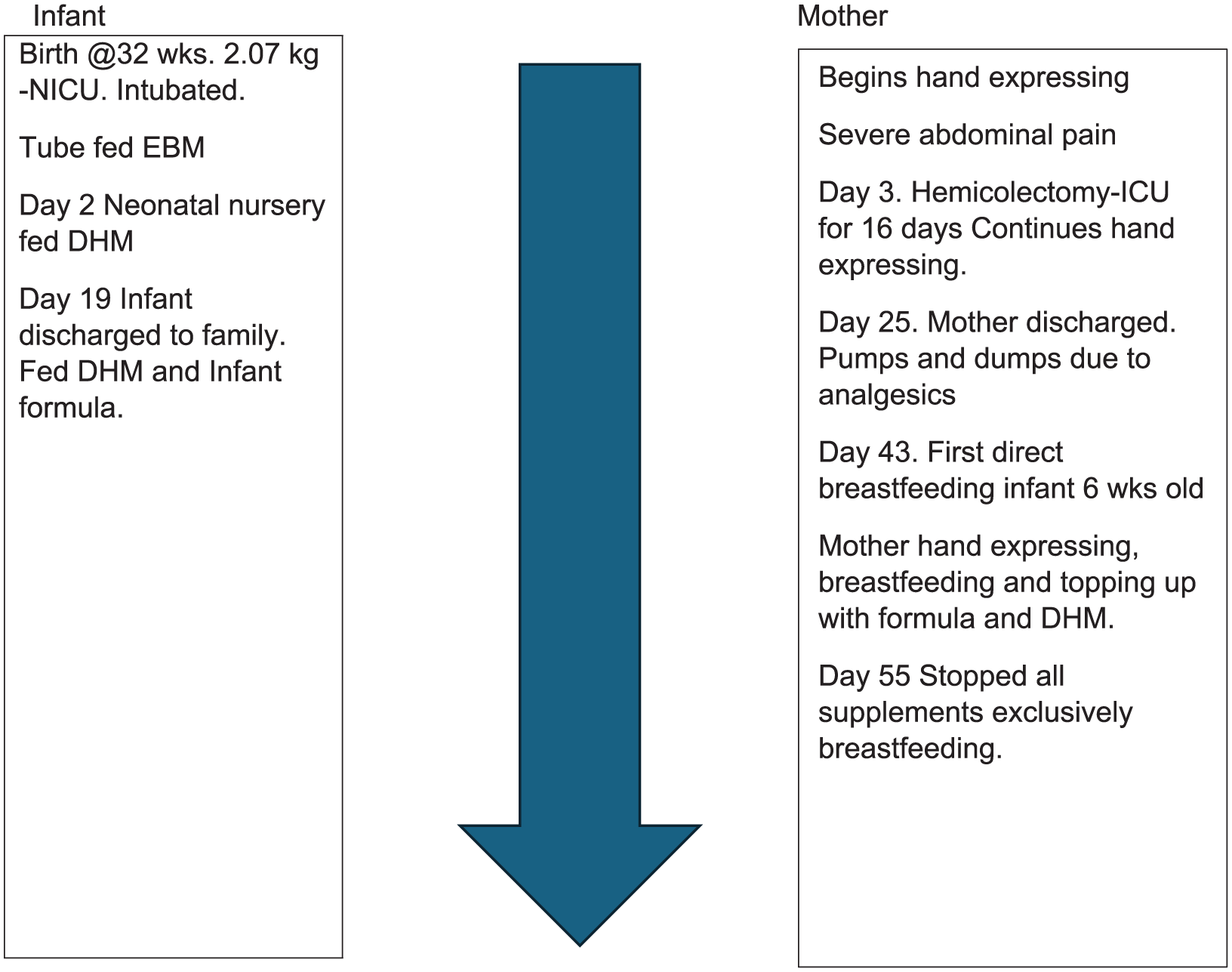
Case Study 1: The mother had a hemi-colectomy following a Caesarean section.
Establishing lactation under these circumstances, when the mother was extremely ill and separated from her infant and traumatized, was challenging. Recovering from three major abdominal operations in under a week, while attempting to initiate and sustain lactation, seemed an almost impossible task. The mother was weak post-operatively, in severe pain, and on a restricted diet. She was in frequent telephonic contact with another doula and an International Board-Certified Lactation Consultant (IBCLC), who provided consistent guidance and encouragement about exclusive pumping and sustaining a milk supply. The infant was discharged on DOL 16 into the care of the husband, grandmother, and sister. The hospital organized for an extra supply of DHM to accompany the infant on discharge, while the mother remained in hospital to recover. However, as supplies ran low, DHM was alternated with artificial breastmilk substitutes. Once the mother was discharged on DOL 25, she was still unable to breastfeed due to opioid analgesics and so was pumping and dumping. Only when the infant was 6 weeks old was the mother able to start direct breastfeeding. As she had not yet established a full supply, keeping the baby interested enough to continue suckling was a further challenge. She alternated breastfeeding with bottle feeding using artificial breastmilk substitutes as the supply of DHM was now depleted. In addition, she was power pumping regularly to further stimulate her supply and practicing skin-to-skin by spending most the day in bed with her infant. She was breastfeeding every 2 hours, day and night. The infant’s birth weight was 2.07 kg and at 55 days she weighed 3 kg. The mother maintained this routine for a further 30 days until she reported hearing swallowing at the breast at which time she stopped the artificial substitute supplementation. This mother was suffering from stress and depression following her life-threatening ordeal and was subsequently diagnosed with post-traumatic stress.
Case Study 2
This first-time mother had no previous breastfeeding experience and was new to the country where she delivered, so did not have an extensive support network. Prior to delivery, an IBCLC had suggested a resource on breastfeeding for her to read. On Day 2, the mother and infant were discharged home. An IBCLC did a home visit and provided guidance around latch and reassurance about breastfeeding. The infant was latching well and transferring milk. Mother was weak after surgery and the primary PPH. Figure 2 provides a summary timeline of events.
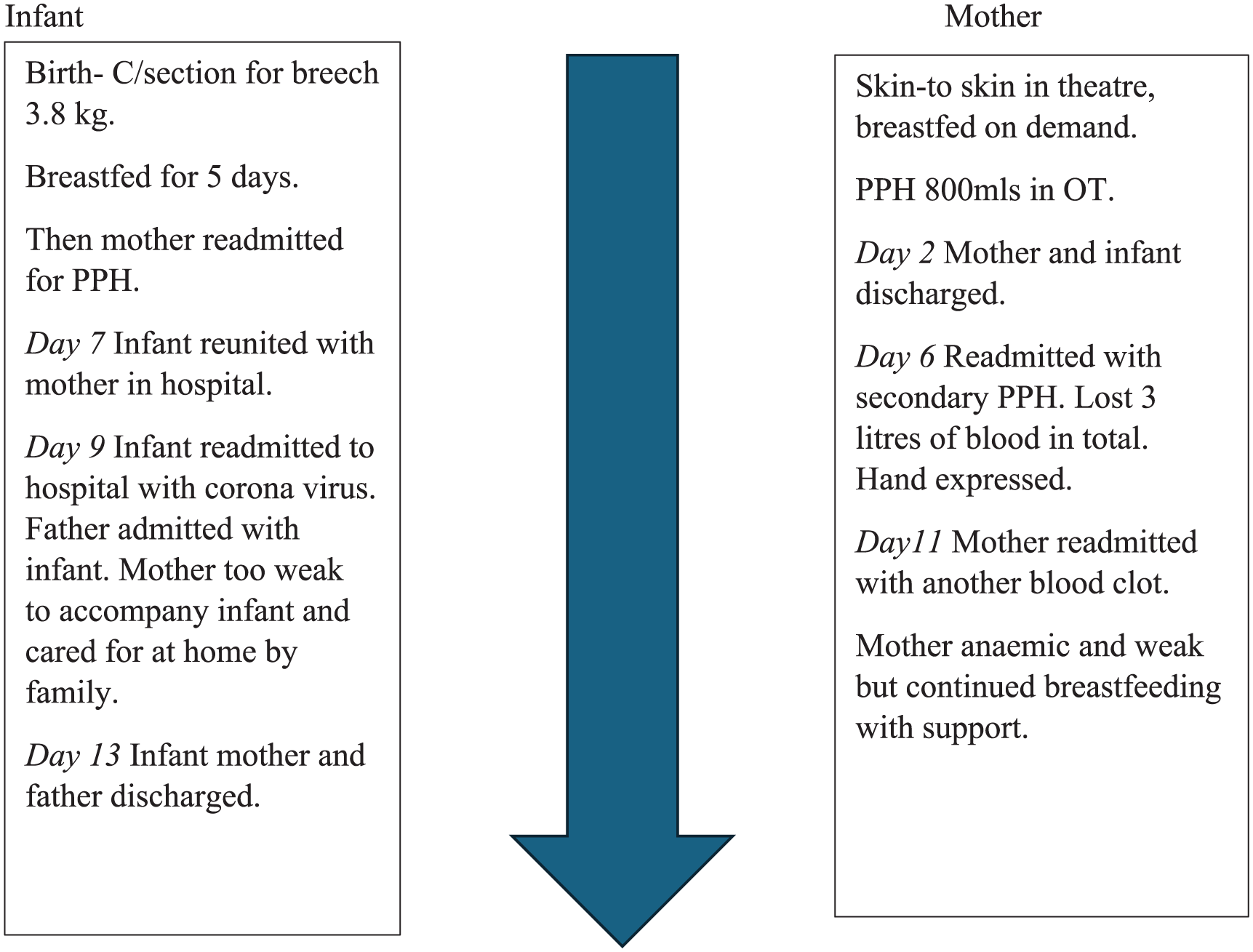
Case Study 2: The mother with a postpartum hemorrhage.
On DOL 6 the mother was readmitted to hospital with a secondary PPH. During this first readmission for a secondary PPH she had to wait 12 hours to go to theatre, and the infant stayed at home with friends while her partner accompanied her to hospital. She expressed manually during this time with the help of staff in the unit, as she was apprehensive to use the breast pump and dislodge the uterine clots before she went to theatre. A manual removal of clots and dilatation and curettage was performed. One unit of blood was administered. The infant then joined the mother in hospital for 2 days and she was able to breastfeed him directly. The life-threatening primary and secondary postpartum hemorrhage left her exceptionally weak and breathless.
On DOL 9, both she and the infant were discharged. The day she arrived home, an ambulance was called to take the infant to hospital with an unknown virus, which was later diagnosed as corona virus. The mother was too weak to accompany him, so the father was admitted with him, and the extended family were called to help care for the mother. She required assistance with the simplest tasks, walking, bathing, and expressing. She was unable to hold the breast pump in place.
She pumped 3 hourly and friends took the expressed breastmilk to hospital. Family members washed and sterilized bottles and the breast pump and cared for her. After being separated from her infant for 24 hours, the mother was readmitted with another uterine clot and further bleeding. Her husband was then diagnosed with coronavirus. Shortly afterwards the mother, too, was diagnosed with coronavirus.
Severe maternal morbidity of both mothers presented major obstacles to the establishment of an adequate supply of breastmilk and reduced the chances of successful breastfeeding.
Outcomes
Case Study 1
After significant effort and support, at just over 2 months this mother was exclusively breastfeeding, despite that fact that she was still recovering from her surgery and suffering from post-traumatic stress. Her main symptoms were profound depression and anxiety. She was seen by psychologists and a psychiatrist and prescribed medication. The infant weighed 3.4 kg. The triple feeding program (breastfeeding, topping up with artificial substitutes, and expressing) is demanding even for mothers who are healthy, so to maintain the regime meant commitment and hard work but ultimately it was a belief that human milk would provide optimal health for her infant that kept her going. A quote from her:
After successfully breastfeeding my other two daughters, I knew the bonding experience that I would miss if I could not breastfeed my baby. What really drove me was: I am a doula—I cannot fail! I have helped many moms to successfully breastfeed their babies, I have to get it right. It was so hard; in my mind I wanted to give up many times. Looking back now, I am so thankful that I persevered, enjoying a wonderful bonding experience for nearly 2 years with my baby.
Case Study 2
Once all the family were home, the infant began cluster feeding, at times for 7 hours at a time, which was exhausting for the already weakened and anemic mother. This was possibly a reaction to the stress of hospitalization and his separation from her. It provided ample breast stimulation, and her milk production was soon more than sufficient for his needs.
The fact that this mother was able to maintain her supply and exclusively breastfeed despite her significant postpartum hemorrhage, anemia, and coronavirus infection is testament to her steely determination and the support of her close family, health care professionals, and friends. The mother took many months to regain her health and be able to care for herself and her infant.
A quote from her:
I purposely sought advice from one lactation specialist and didn’t ask or take advice from other health professionals because I wanted the consistent voice of one expert. I remained calm throughout the process. The first thing I said to my baby was “This is my first day on the job as your mum and I’m learning too, so we can learn together.” . . . The IBCLC recommended a breastfeeding book which really helped me understand the fundamentals of breastfeeding. Breastfeeding was extremely challenging throughout the early trial; however, I understood and believed in the long-term benefits of breastfeeding, therefore I was tenacious and did not want to give up or accept defeat, for my baby’s sake. My story is a testament of faith and encouragement to all mums. I truly believe that if you put your mind to something and don’t give up, you will be able to conquer any challenges thrown at you, and this story can prove that to you. Table 1 provides an overview of the similarities and differences between these two case studies.
Similarities and Differences in Case Studies.
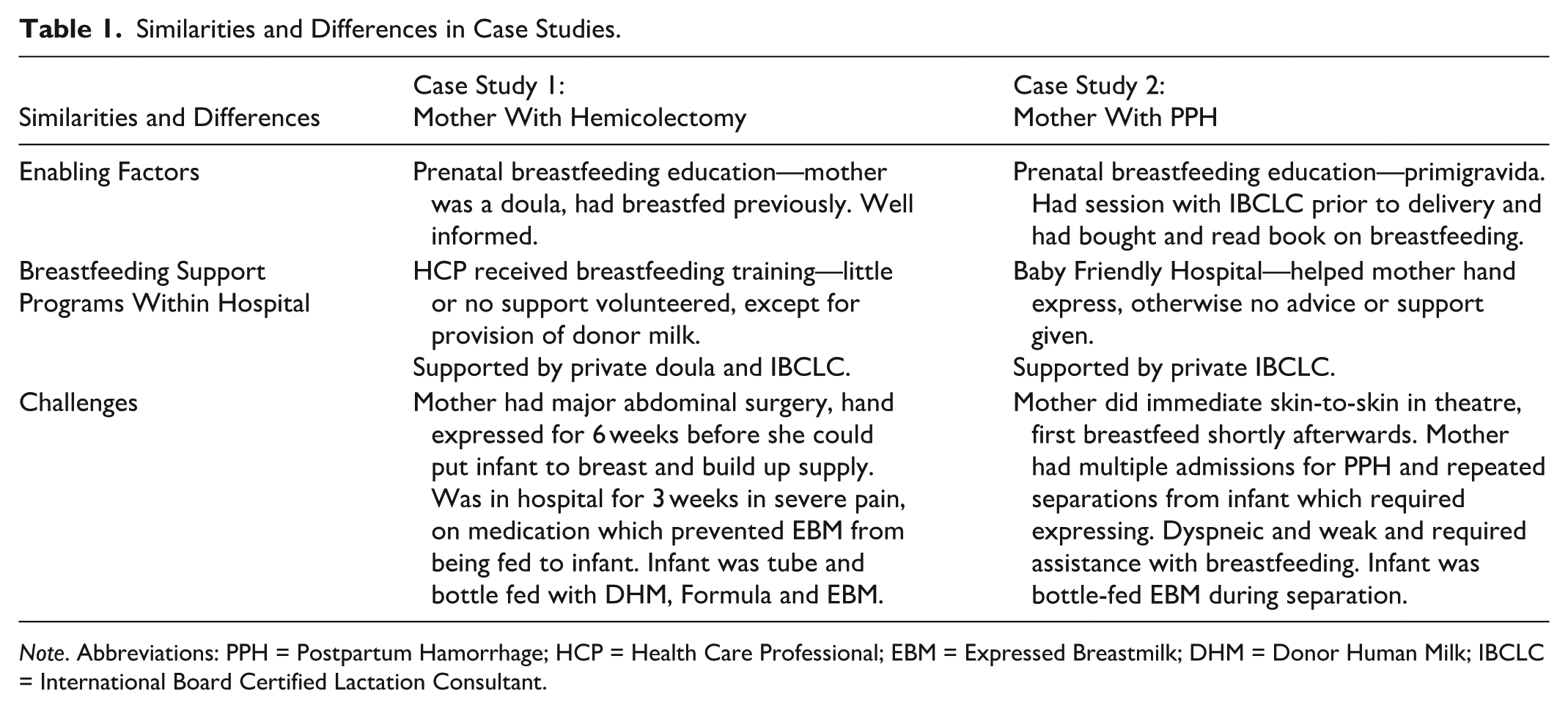

Note. Abbreviations: PPH = Postpartum Hamorrhage; HCP = Health Care Professional; EBM = Expressed Breastmilk; DHM = Donor Human Milk; IBCLC = International Board Certified Lactation Consultant.
Discussion
These case studies were examined to gain an understanding of what enabled these women with medical complications to successfully breastfeed.
Being well informed about breastfeeding prior to delivery meant these women had a positive approach to breastfeeding; they were single minded and determined to succeed. This correlates to the anticipatory guidance in the theoretical model where women drew upon guidance and resources they had obtained prior to delivery, and this is confirmed by multiple studies finding high breastfeeding rates in women who received prenatal education (Kehinde et al., 2023). Breastfeeding success was despite the maternal and infant separation and medical interventions, which are often associated with early weaning and a decrease in exclusive breastfeeding (Feldman-Winter et al., 2016; Neovita Study Group, 2016; Vetulani, 2013). Similarly, women with PPH are less likely to be breastfeeding on discharge due to reduced blood flow to the pituitary gland and a decrease in the production of prolactin. (Flood et al., 2023). Early intervention and support for these mothers helped overcome possible insufficient supply issues.
Both these mothers were at times anxious about their condition and their ability to sustain or build up an adequate supply, and they both needed reassurance and encouragement from lactation professionals. What was important was that there was a consistent voice advising them. Too often, health care professionals lack the necessary skills and knowledge to provide evidence-based breastfeeding support (Mulcahy et al., 2022.) Essential support helps counteract stress, provides reassurance, and addresses concerns about milk yield and pumping (Li et al., 2024; Rieth et al., 2018; Watson et al., 2013). The hospital where the mother in Case Study 2 delivered was Baby Friendly, and the other was not, yet it made little difference in the breastfeeding support they received, despite the fact that being Baby Friendly should play a crucial role in supporting lactation (Pérez-Escamilla et al., 2016).
Throughout the initial weeks negotiating their challenges, the maternal role of both women was influenced by their desire to nurture their infants and the interaction with their family and support networks. Their expectations and that of their supporters of succeeding to breastfeed, helped influence their ability to overcome their challenges (Rafii et al., 2020; Wilson et al., 2012). The hormones of lactation—oxytocin and prolactin—also play an important role in maternal attachment and bonding and help cultivate self-confidence (Modak et al., 2023).
The third theme found in these case studies, and identified in the theory, was that of resilience. Both mothers were well-informed and had clear goals about breastfeeding. A strong intention to breastfeed has been associated with successful breastfeeding practices postnatally (Naja et al., 2022). These mothers managed to take the necessary steps to ensure breastfeeding succeeded. Direct breastfeeding was not possible for 6 weeks in Case Study 1, and innovative ways had to be found both to maintain her supply and to feed the infant. In Case Study 2, the mother had multiple separations from her infant and required help to express and feed her infant. The literature confirms that while separated from their infants, mothers had substantial needs for education, emotional and practical support, and assistance from knowledgeable IBCLCs and families (Alves et al., 2016). The combination of knowledge and the necessary emotional support gave them the necessary resilience to adapt to the challenges they faced—and to succeed. Chetwynd (2024) discusses the vulnerability of breastfeeding and the need to use resilience to meet challenges in our circumstances, environments, and our lived experiences. This can mean adapting what we consider standard ways of breastfeeding to accommodate extraordinary circumstances faced by mothers and find creative ways to continue to provide breastmilk to infants.
The main lessons learnt in these case studies are that, despite overwhelming medical and physiological and psychological odds, it is possible to sustain lactation and establish exclusive breastfeeding. Fundamental to the successes of these two mothers were being well-informed prior to delivery, consistent professional lactation support, being highly motivated to breastfeed, having supportive partners and extended family who encouraged and provided practical support, and being resilient to overcome the challenges they faced.
No one escapes pain, fear, and suffering. Yet from pain can come wisdom, from fear can come courage, from suffering can come strength—if we have the virtue of resilience. (Grietans, 2015, p. 3)
Limitations
The findings in this case study may not be applicable to other settings. The researchers were aware of their biases and made every effort to ensure they did not influence the research, yet it remains a possibility.
Future Research
Identifying the characteristics of mothers at risk of early weaning should add important information for developing appropriate supportive policies and procedures. Research investigating the most effective ways of ensuring that health care professionals provide much needed evidence- based lactation care and support, especially for mothers with significant morbidity, is vital. The Lancet Breastfeeding Series 2023 highlights the importance of creating multilevel and multicomponent approaches to provide the enabling environment women need (Pérez-Escamilla et al., 2023).
Footnotes
Acknowledgements
The authors would like to thank the participants for their bravery, determination and their consent to share their stories. Thank you to Shannon Kenny for her language editing and to Pamela Morrison for her feedback and input.
Author Contributions
Funding
The author received no financial support for the research and/or authorship of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: PR is an IBCLC who knew and helped the two participants with lactation advice. AC has no conflict of interest to declare.
