Abstract
Background:
Improving breastfeeding practices is a worldwide priority. Pharmacists have the opportunity to actively promote breastfeeding and educate parents as well as the general public about its benefits.
Research Aims:
The aims of this study are to investigate Jordanian pharmacists’ present breastfeeding support practices and perceptions regarding their need for education and training in breastfeeding support.
Methods:
To examine sociodemographic characteristics of community pharmacists in Jordan and their current breastfeeding support practices and educational needs, a descriptive cross-sectional online (self-report) survey was conducted. Through social media, pharmacists working in community pharmacies in Jordan were recruited between August 2021 and February 2022. The level of breastfeeding support participants had been provided with was measured using eight items in a 5-point Likert scale ranging from 5 (Always) to 1 (Never). Each participant self-reported the frequency of advice/information given to breastfeeding women in each of these areas. Univariate and multivariable linear regression models were used to identify factors associated with the level of breastfeeding support.
Results:
Participants (N = 381) reported a high level of breastfeeding support, but expressed a need for training and education for further improvement. The breastfeeding support score of female participants was found to be 0.12 higher than that of males (Beta = 0.12, p = .02), 0.16 higher in married participants compared to non-married participants (Beta = 0.16, p = .03), and 0.10 higher in participants working in rural areas compared to those working in urban areas (Beta = 0.10, p = .04).
Conclusion:
While community pharmacists generally report a high level of breastfeeding support, our findings revealed demographic differences. Attention to specific areas of need might enhance what pharmacists could offer; however, additional research would be required to guide the specific educational content.
Keywords
Key Messages
In Jordan, community pharmacists are regarded by parents as accessible and convenient healthcare providers. Little is known about pharmacists’ perceived roles in breastfeeding support.
The self-perceived level of breastfeeding support from community pharmacists in Jordan is high; however, a need for more education and training was identified to enhance breastfeeding support.
Educational and training programs can be advantageous for pharmacists in Jordan to enhance their knowledge and expertise in managing and supporting breastfeeding.
Background
Improving breastfeeding practices is a global priority. Exclusive breastfeeding rates for infants younger than 6 months are low (44%) worldwide (United Nations Children’s Fund [UNICEF], 2021a). The duration of breastfeeding may be influenced by psychosocial factors including social support, breastfeeding intentions, and breastfeeding self-efficacy (Wallenborn et al., 2019). Furthermore, breastfeeding can be a difficult experience for women living in societies that do not fully promote or encourage positive attitudes towards breastfeeding (Blixt et al., 2019). Breastfeeding support is a multidimensional endeavor that includes providing information, practical assistance and supporting self-esteem and emotional wellbeing (Moran et al., 2007). Support services that address some or all of these dimensions include designated lactation support providers, notably International Board Certified Lactation Consultants (IBCLCs; Mercado et al., 2019). Breastfeeding classes and peer support groups can also be very helpful (Demirci et al., 2019). Accommodations in public places, including breastfeeding-friendly areas in workplaces or other care facilities, including pharmacies, can make it easier to breastfeed.
The “breastfeeding friendly pharmacy” is a promising project aimed at providing suitable supportive areas for breastfeeding (Harahsheh et al., 2023). The number of women with an intention to exclusively breastfeed could be increased, especially among first-time mothers, with the help of guided breastfeeding education and breastfeeding support. Appropriate education and support can also enhance breastfeeding skills and have a positive influence on attitudes toward breastfeeding (Al-Radaydah et al., 2022). In 2020, researchers who surveyed community pharmacists using an online survey (N = 63), found that their participants believed they played a critical role in patient care and breastfeeding support (Ceulemans et al., 2020).
Recent advances in practice in the pharmacy profession are shifting community pharmacists’ responsibilities from a traditional product-focused orientation to a patient-oriented approach (Khan et al., 2020). Pharmacists are responsible for providing patients with basic medication information and detailed guidance on drug administration, efficacy, safety, drug–drug interactions, drug–food interactions, medication storage, adverse effects, and the importance of medication adherence (Jordan Pharmaceutical Association [JPA], 2022). Patients can easily obtain a wide range of healthcare services through pharmacies (Basheti et al., 2020). The concept of pharmaceutical care in the United States was generated from continual efforts to enhance patient health outcomes (Hepler & Strand, 1990). The concept was rapidly adopted as “good pharmacy practice” globally (JPA, 2022). The board of the Pharmaceutical Care Network Europe (PCNE) agreed on a PCNE definition for pharmaceutical care, noting that it is “the pharmacist’s contribution to the care of persons in order to optimize medications use and improve health outcomes” (Allemann et al., 2014).
Pharmacists can play a significant role in supporting women throughout preconception, pregnancy, and lactation (Ceulemans et al., 2020). The potential for pharmacist support of breastfeeding women has been reported in the literature, emphasizing their highly visible roles in the community, frequent interactions with soon-to-be and new parents, and knowledge of medication safety (Edwards, 2014). There is evidence that pharmacists have continuous contact with breastfeeding women and that they are seen as easily accessible and trusted health consultants. Thus, breastfeeding counseling and support by community pharmacists can meet a critical care gap.
In Jordan, the JPA health authority has been influential in incorporating community pharmacists into the primary healthcare system. The JPA has launched the Good Pharmacy Practice (GPP) initiative to promote patient-centered healthcare and boost the role of community pharmacists (Basheti et al., 2020). The implementation of GPP in the country has paved the path for new services to become a reality (Asab et al., 2019). Attempts are being made to emphasize the significance of collective efforts to encourage and safeguard breastfeeding for every child under the slogan “Breastfeeding protection: A shared responsibility” (UNICEF, 2021b).
Thus, pharmacists have the potential to play a role in community-level shifts toward breastfeeding as the social norm in Jordan and elsewhere. Pharmacists’ possible roles in supporting breastfeeding have not been evaluated in Jordan. This study was carried out to investigate Jordanian pharmacists’ current breastfeeding support practices and their perceptions regarding their need for education and training in breastfeeding support.
Methods
Research Design
This study followed a descriptive cross-sectional design and was conducted using an online (self-report) survey. Surveys were administered online due to the COVID-19 pandemic, social distancing regulations, and the need to collect confidential data from respondents in a variety of workplaces. Ethical approval for the study was obtained from the Institutional Review Board of King Abdullah University Hospital, University of Science & Technology, Jordan (Reference No. 56/141/2021, July 29, 2021).
Setting and Relevant Context
The healthcare system in Jordan is composed of various service providers, including public, private, international, and charitable sectors. Community pharmacies are part of the private sector. The primary healthcare services in Jordan are administered through a vast network of Ministry of Health (MoH) primary healthcare centers that offer services for maternal, childhood, and dental health, with 448 Motherhood and Childhood Centers. Health insurance in Jordan is available through the public sector and the private sector and can be obtained through a variety of sources. Some individuals have access to health insurance through their employment (Rappel et al., 2020). It is estimated that health insurance is accessible to around 82.3% to 86.0% of people residing in Jordan (United States Agency for International Development [USAID], 2019).
Antenatal, intrapartum, and postnatal care, as well as vaccination coverage and treatment coverage for common childhood illnesses, are the main elements of maternal and child health services in Jordan. During the antenatal period, routine blood pressure checks and tests to detect potential antenatal complications are also considered essential components of antenatal care services. Most of the pregnant women in Jordan give birth in a hospital setting under the supervision of a trained health professional—a physician or a registered nurse. Likewise, postnatal care includes postnatal checkups immediately after delivery and before discharge from the hospital, and often a 2-day postnatal checkup (World Bank, 2008, 2019). Nevertheless, there is a significant gap in the availability of breastfeeding counseling in antenatal care (Khasawneh et al., 2020).
Community pharmacists are regarded by parents in Jordan as the most accessible and convenient healthcare providers (Mukattash et al., 2019). A qualitative exploratory study conducted with 26 parents from various cities in Jordan found that most of the parents trusted pharmacists as medication experts and were comfortable receiving medication and advice from them. This trust was attributed to the perception that local pharmacists had credible educational qualifications and medical expertise (Mukattash et al., 2019). Hence, there is a promising potential for pharmacists to provide support and education about the benefits of breastfeeding to parents, as well as to the general public.
In Jordan, 92% of children aged 2 years and below were nursed at some point in their lives (World Bank, 2019). The Jordanian Ministry of Health, through the Primary Healthcare Administration, is dedicated to promoting breastfeeding as the best start in life for all newborns (UNICEF, 2021b). However, the rate of exclusive breastfeeding for 6-month-old babies is less than ideal, and is gradually declining. According to several Jordanian population and family health surveys, exclusive breastfeeding at 6 months has fallen from 40% in 2007 to 26% in 2018 (World Bank, 2019). Interestingly, attitudes toward breastfeeding among Jordanian women has changed in recent years. In a cross-sectional study conducted in 2015 on 627 young females, it was found that participants held a negative attitude towards breastfeeding, with only 39.3% showing a positive attitude. They perceived it as an old-fashioned feeding practice and believed that formula feeding was more convenient (Al-Domi, 2015). Recently, a questionnaire-based survey showed that 72% of Jordanian women demonstrated a favorable attitude toward breastfeeding, with a high percentage (97%) planning to nurse their infants (Khasawneh et al., 2020). However, there have been some concerning indicators. A review of Jordan’s nutrition situation highlighted the country’s overall suboptimal breastfeeding practices in terms of breastfeeding initiation, exclusive breastfeeding, and duration (Al-Awwad et al., 2021).
Sample
The questionnaire targeted community pharmacists holding at least a bachelor’s degree in pharmacy who were currently working in community pharmacies in Jordan. Recruitment was conducted using a convenience sampling technique. The most recent statistics released by the JPA showed that there were 22,667 registered pharmacists in February 2019 (JPA, 2019). Sample size was estimated using Raosoft® sample size calculator for the online survey. With a margin of error of 5%, a confidence level of 95%, a population size of 22,667, and response distribution of 50%, the recommended sample size was 378 participants.
Measurement
The online survey was developed by reviewing previous surveys in the literature, including those developed by D’Arcy et al. (2019) and Ronai et al. (2009). The 28 items included in the draft questionnaire were reviewed and discussed individually by the research team. In addition, three experts in pharmacy practice, outside of the research team, reviewed the questionnaire for face and content validity. They assessed the relevance of the questionnaire items, specificity, and comprehensiveness. The questionnaire was thus expanded to include a total of 31 items. Following this review, the questionnaire was piloted in a sample of 10 volunteer community pharmacists to verify its comprehension, clarity, and cultural acceptability. The data obtained from the pilot test were not included in the final data analysis. The survey contained multiple-choice questions and was designed to be completed within 10–12 min. The final version of the survey was composed of 18 questions which assessed four main sections:
Demographics
The demographic section included questions about age, sex, marital status, if participants had a child, their years of pharmacy practice, highest pharmacy degree, work location (geographical area and rural/urban), and pharmacy type (independent pharmacy or chain pharmacy). To assess participants’ geographical areas of practice, their self-reported Governorates were used to classify them into three main regions within Jordan. Specifically, the North Region consisted of Irbid, Ajloun, Jerash, and Mafraq, the Middle Region encompassed Balqa, Amman, Zarqa, and Madaba, and the South Region included Karak, Tafilah, Ma’an, and Aqaba. These categories align with well-known geographical divisions within the country.
Personal and work-related breastfeeding experience of study participants
This section measured participants’ personal experiences in breastfeeding and how often participants experienced queries on medication use in breastfeeding. Additionally, participants were asked to rate the level of confidence (being very sure of something) and comfort (physical comfort and ease) they felt while giving advice to women about medication while breastfeeding, on a 5-point scale with answer options ranging from “very confident” to “very unconfident” and “very comfortable” to “very uncomfortable,” respectively. The term “breastfeeding” in the analysis is defined as the child receiving their mothers’ milk (either directly from the breast or expressed; Labbok & Starling, 2012).
Pharmacists perceived need for training and education to provide support to breastfeeding women
Participants were asked to rate their level of agreement on an eight item 5-point Likert-type scale ranging from “strongly agree” to “strongly disagree” to measure their needs for further training and education in breastfeeding support. Internal consistency and reliability was tested by the Cronbach’s alpha coefficient, which was 0.94 for the eight items.
Level of breastfeeding support provided by pharmacists
To measure participants’ breastfeeding support level in their current practice, participants self-rated the frequency with which they gave advice/information in different areas to breastfeeding women in the past 12 months, including medication safety while breastfeeding, types of formula, and treatment of minor conditions in the mother while breastfeeding. The participants indicated the frequency of their support per interaction with breastfeeding women over the specified time frame. This was assessed with eight items on a 5-point Likert scale ranging from “always” to “never.” Internal consistency reliability was tested by the Cronbach’s alpha coefficient, which was 0.93 for the eight items.
Additional breastfeeding support practices in pharmacies
To measure non-pharmacological breastfeeding support practices provided in the pharmacies in which the participants were working, participants were asked to report whether a range of advisory services and a supportive environment were available. Practices considered to support breastfeeding included information on breast pumps and bottles, expression and storage of expressed milk, information on weaning and babies’ nutrition, general information on locally available breastfeeding support, and the presence of a comfortable area for breastfeeding infants. Additionally, we evaluated whether participants proactively or actively promoted breastfeeding as the norm when interacting with breastfeeding mothers about concerns that were related to breastfeeding. A yes/no approach was used to measure the promotion of breastfeeding in a dichotomous manner.
Data Collection
The study was conducted in Jordan from August 2021 to February 2022. The final version of the survey was created using Google Forms. An online link was created. To reach potential participants, social media portals (Facebook and WhatsApp groups) were used to distribute the survey. The inclusion criteria were mentioned at the start of the survey. No incentives were offered. To reach the target sample size, the researchers shared the study’s link multiple times on Facebook and WhatsApp groups dedicated to pharmacists, until they had successfully recruited enough participants. Participants were informed that their participation was voluntary, and the purpose, risks, and benefits of the study were explained in a written introductory online page before accessing the questionnaire. Electronic consent was obtained when participants chose “agree to participate” at the beginning of the questionnaire. Once their consent was given, participants were allowed to proceed to the study questionnaire. For those who selected “disagree to participate,” the survey was submitted automatically without filling out the questionnaire. All participants were informed that they had the right to discontinue their participation at any time. Participants’ names were not requested so the anonymity of respondents was preserved. Google Forms was used as the online survey platform for data collection. The primary investigator maintained collected data. We established password security measures for accessing the online questionnaire to safeguard the confidentiality of participant data.
Data Analysis
The completed surveys were extracted from Google Forms as an Excel sheet and were then exported to SPSS (Version 25.0) for statistical analysis. To describe characteristics of the study sample, frequency and percentages were used for categorical variables, while means and standard deviations were used for continuous variables.
Data was collected from four domains (1) the breastfeeding support level provided, (2) the need for education and training for breastfeeding support, (3) personal and work-related breastfeeding experience, and (4) breastfeeding support practices in pharmacies. For the 5-point Likert scales for both participants’ breastfeeding support level and need for training and education in breastfeeding support, the overall mean of the 8-item domains was computed. Demographic characteristics and having personal breastfeeding experience that were found to be significant on a single predictor level (p < 0.25; Mukattash et al., 2022), were entered into multiple linear regression analyses using univariate linear regression to assess their relationships with breastfeeding support levels. None of the included variables showed multicollinearity; thus, none were eliminated. Variables were selected after checking their independence, using tolerance values > 0.1. Variance Inflation Factor (VIF) values < 10 were checked to indicate the absence of multicollinearity between the independent variables in regression analysis. Statistical significance was considered at p ≤ 0.05. The data analysis included evaluating participants’ personal and work-related breastfeeding experiences, as well as breastfeeding support practices in pharmacies, using descriptive statistics expressed in terms of frequencies and percentages.
Results
Sociodemographic Characteristics and Breastfeeding-Related Experience
After distributing the online questionnaire, a total of 381 completed forms were received and included in the analysis. Most participants were female, single, and 23–30 years of age. Around three-quarters of the participants had less than 5 years of experience as pharmacists and were working in independent community pharmacies (Table 1).
Sociodemographic Characteristic of the Study Participants (N = 381).
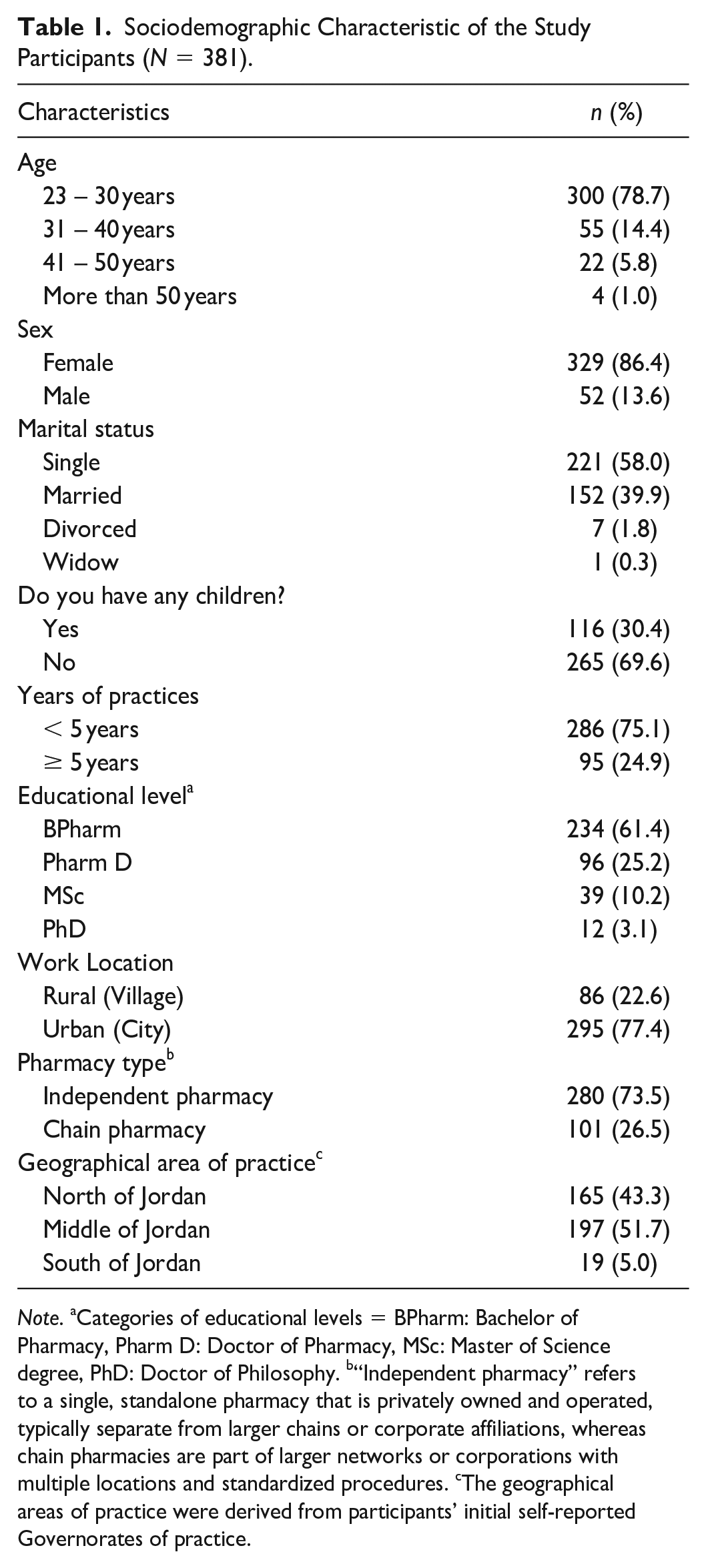

Note. aCategories of educational levels = BPharm: Bachelor of Pharmacy, Pharm D: Doctor of Pharmacy, MSc: Master of Science degree, PhD: Doctor of Philosophy. b“Independent pharmacy” refers to a single, standalone pharmacy that is privately owned and operated, typically separate from larger chains or corporate affiliations, whereas chain pharmacies are part of larger networks or corporations with multiple locations and standardized procedures. cThe geographical areas of practice were derived from participants’ initial self-reported Governorates of practice.
More than half of the participants reported having had a personal experience in breastfeeding (Table 2). About a third reported experiencing queries on medication use during breastfeeding on a daily basis. Most participants reported being somewhat/very comfortable and somewhat/very confident when giving advice to women about medication while breastfeeding.
Breastfeeding-Related Experience of the Study Participants (N = 381).
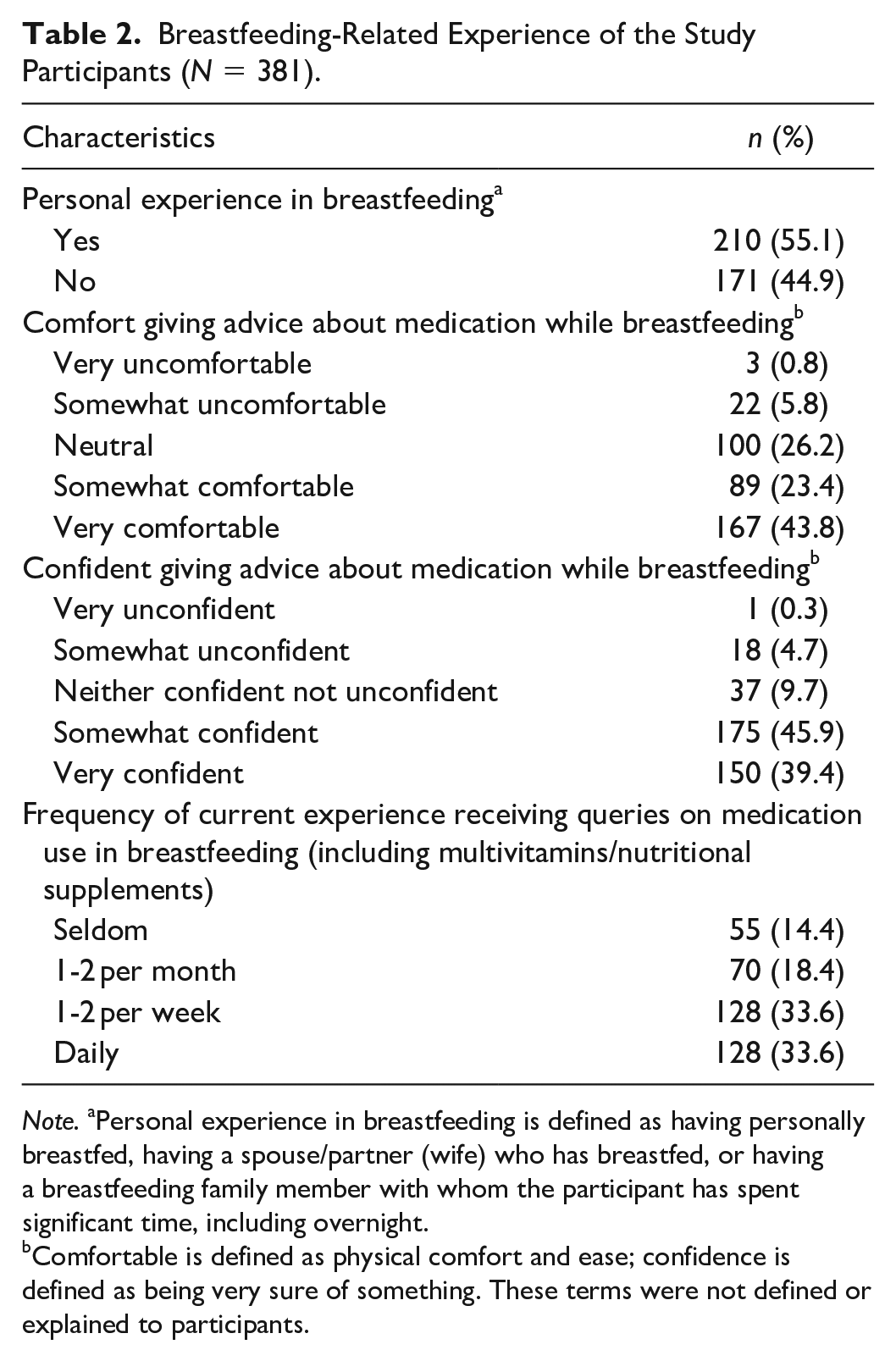
Note. aPersonal experience in breastfeeding is defined as having personally breastfed, having a spouse/partner (wife) who has breastfed, or having a breastfeeding family member with whom the participant has spent significant time, including overnight.
Comfortable is defined as physical comfort and ease; confidence is defined as being very sure of something. These terms were not defined or explained to participants.
Perceived Need for Training and Education
Surveyed participants were evaluated on their needs for further education/training to improve their breastfeeding support practice and confidence in delivering advice/information to breastfeeding women (Table 3). Most surveyed participants (> 80%) strongly agreed or agreed with the need for further education/training to improve their breastfeeding support practices in all eight areas assessed. The most commonly agreed areas for further education/training were: (1) safety of maternal medications while breastfeeding, (2) advice on nutrition while breastfeeding, and (3) advice on the practical aspects of continued breastfeeding while using maternal medication.
Level of Breastfeeding Support Provided by Pharmacists on Different Topics During Encounters With Breastfeeding Women in the Past 12 Months (N = 381).
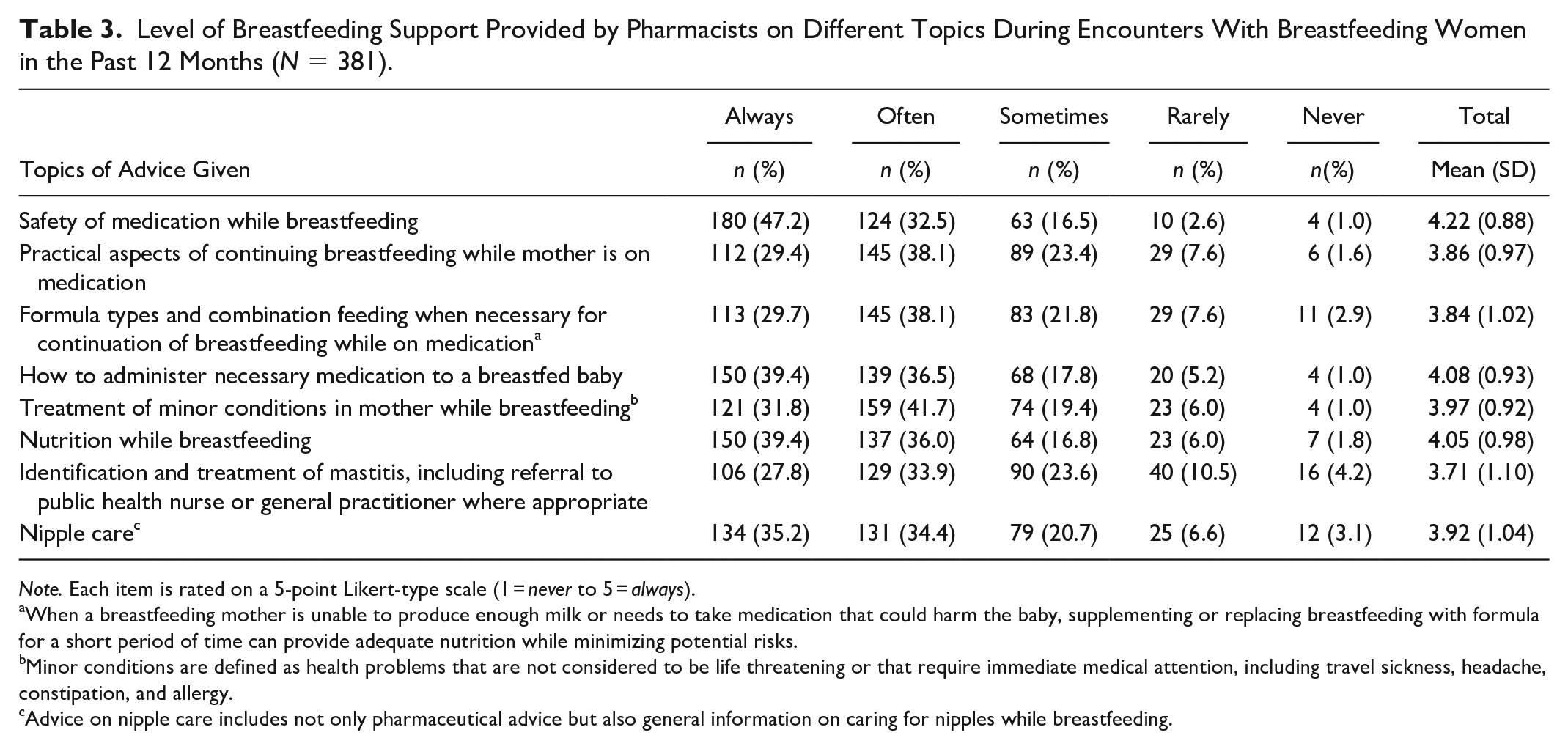
Note. Each item is rated on a 5-point Likert-type scale (1 = never to 5 = always).
When a breastfeeding mother is unable to produce enough milk or needs to take medication that could harm the baby, supplementing or replacing breastfeeding with formula for a short period of time can provide adequate nutrition while minimizing potential risks.
Minor conditions are defined as health problems that are not considered to be life threatening or that require immediate medical attention, including travel sickness, headache, constipation, and allergy.
Advice on nipple care includes not only pharmaceutical advice but also general information on caring for nipples while breastfeeding.
Level of Breastfeeding Support
The majority of participants indicated that they “always” or “often” provided breastfeeding advice or information in encounters with breastfeeding women in all eight areas assessed in the study. The most common advice provided by participants to breastfeeding women was on the safety of medications while breastfeeding, followed by administration of medication to breastfeeding infants, and maternal nutrition while breastfeeding. The least common type of advice was identification and treatment of mastitis, including referral to public health nurses or general practitioners where appropriate (Table 4).
Pharmacists Level of Agreement: on Areas They Would Benefit From Further Education/Training to Improve Their Breastfeeding Support to Breastfeeding Women (N = 381).
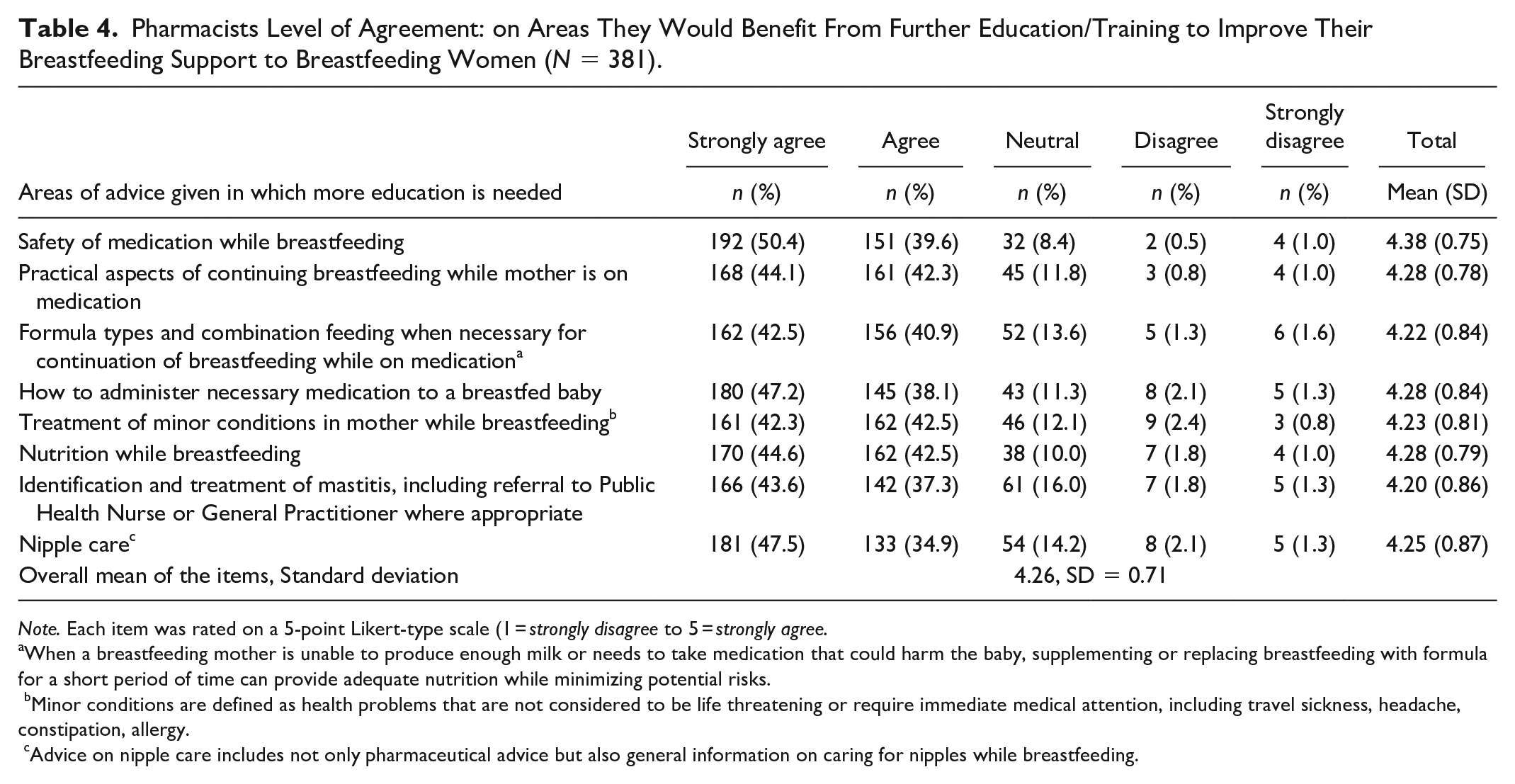
Note. Each item was rated on a 5-point Likert-type scale (1 = strongly disagree to 5 = strongly agree.
When a breastfeeding mother is unable to produce enough milk or needs to take medication that could harm the baby, supplementing or replacing breastfeeding with formula for a short period of time can provide adequate nutrition while minimizing potential risks.
Minor conditions are defined as health problems that are not considered to be life threatening or require immediate medical attention, including travel sickness, headache, constipation, allergy.
Advice on nipple care includes not only pharmaceutical advice but also general information on caring for nipples while breastfeeding.
Lactation support endorsed by participants as being available in the pharmacies in which they worked is presented in Figure 1. The majority of participants reported offering at least one of these services for breastfeeding women, while only 12% (n = 48) did not offer any services. Almost half (44%, n = 165) of the participants reported that they promoted breastfeeding as the norm in all interactions with breastfeeding mothers or individuals accompanying or representing the mother, including family members or partners in their pharmacies.
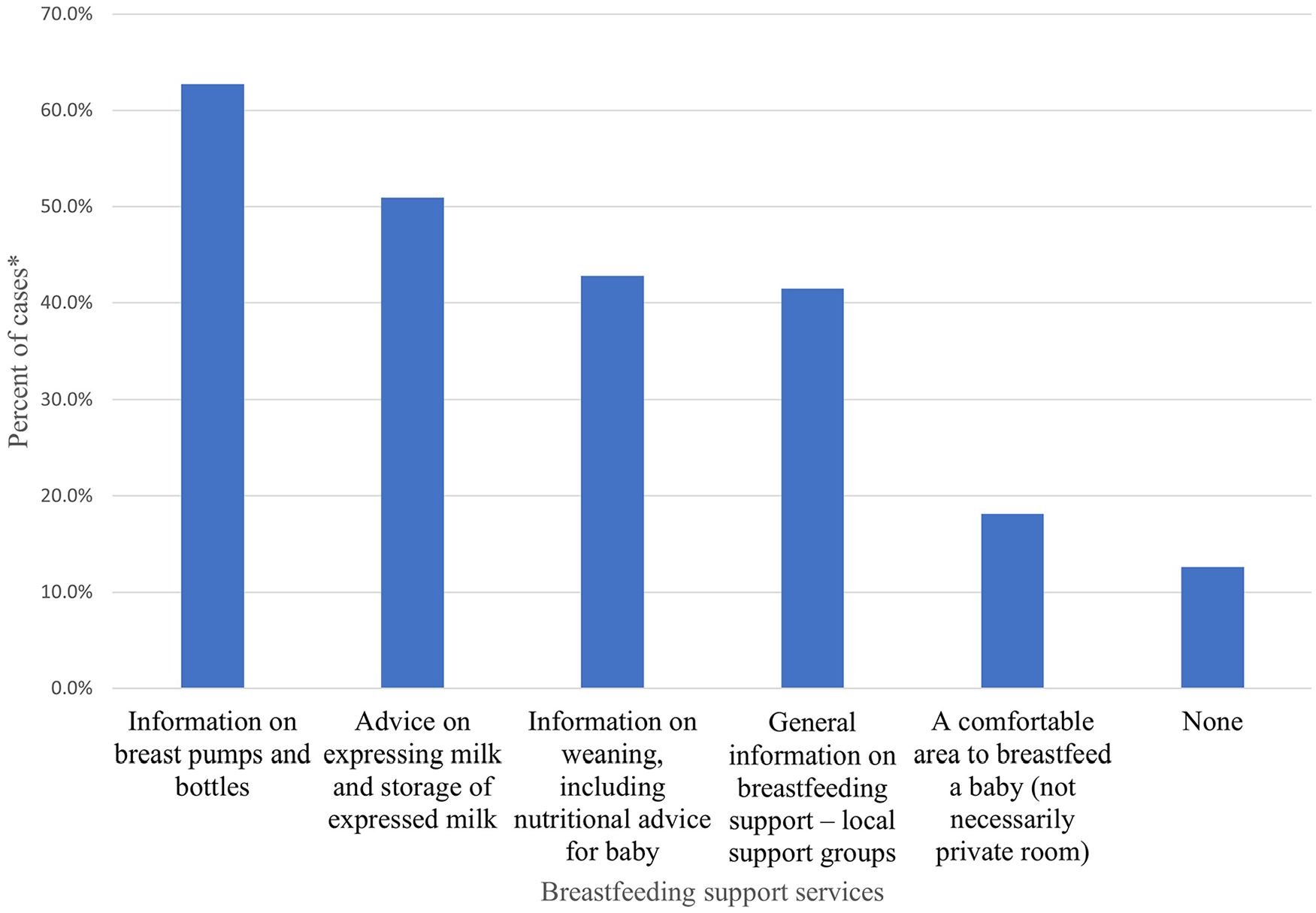
Breastfeeding Support Practices Currently Available in Pharmacies Either From the Pharmacists or Other Personnel With Relevant Training Reported by Participants.
Predictors of the Level of Breastfeeding Support Provided by Pharmacists
Using regression analyses, we found the breastfeeding support score of females to be 0.12 higher than males (p = 0.02), 0.16 higher in married participants compared to non-married ones (p = 0.03), and 0.10 higher in participants working in rural areas compared to those working in urban areas (p = 0.04). The regression model was able to account for 4.4% of the variance in the level of breastfeeding support provided by pharmacists, F (7, 373) = 3.480, p = 0.001. Adjusted R2 = 0.044 (Table 5).
Factors Associated With the Level of Breastfeeding Support Provided by Pharmacists (N = 381).
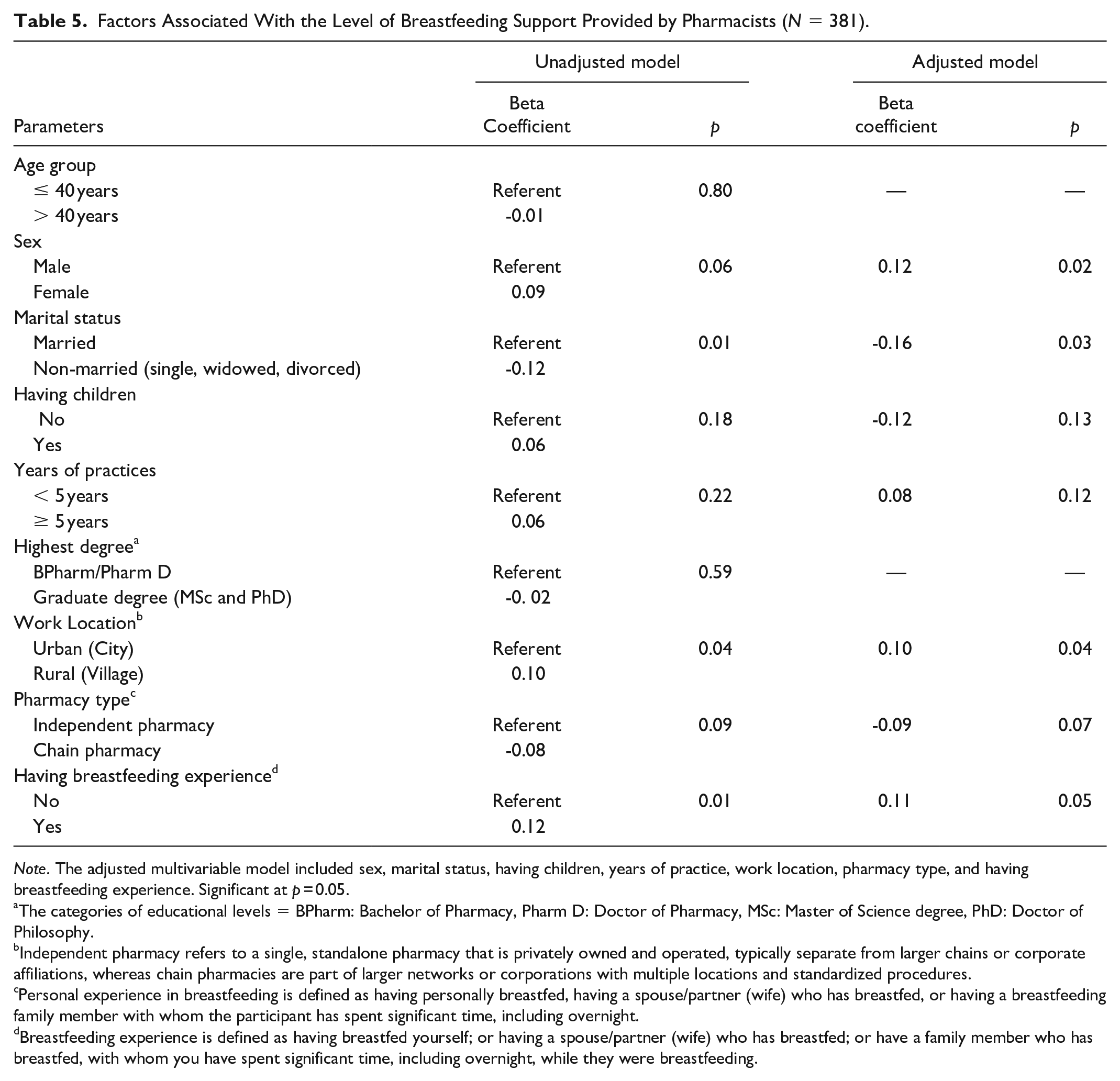
Note. The adjusted multivariable model included sex, marital status, having children, years of practice, work location, pharmacy type, and having breastfeeding experience. Significant at p = 0.05.
The categories of educational levels = BPharm: Bachelor of Pharmacy, Pharm D: Doctor of Pharmacy, MSc: Master of Science degree, PhD: Doctor of Philosophy.
Independent pharmacy refers to a single, standalone pharmacy that is privately owned and operated, typically separate from larger chains or corporate affiliations, whereas chain pharmacies are part of larger networks or corporations with multiple locations and standardized procedures.
Personal experience in breastfeeding is defined as having personally breastfed, having a spouse/partner (wife) who has breastfed, or having a breastfeeding family member with whom the participant has spent significant time, including overnight.
Breastfeeding experience is defined as having breastfed yourself; or having a spouse/partner (wife) who has breastfed; or have a family member who has breastfed, with whom you have spent significant time, including overnight, while they were breastfeeding.
Discussion
There is increasing attention being paid to the influence of health professionals on parents’ decisions to breastfeed (Blixt et al., 2019). It has been recognized by the U. S. Surgeon General that inadequate health professional education and training can be one of the most significant barriers to successful breastfeeding. It was thus recommended that to maintain a satisfactory quality of breastfeeding support, health professionals should have ongoing training and education as well as periodic licensing and certification of their knowledge and skills (CDC, 2011). We found that pharmacists in Jordan had high self-reported breastfeeding support levels in the areas assessed, but also reported a need for further lactation training and education. These findings are in line with those of previous investigators in Belgium, Rome, Australia, and the United States. Pharmacists in these studies also had favorable perspectives and attitudes toward breastfeeding—and a desire to support and advocate for it—but were limited by a lack of information, training, and education (; Hussainy & Dermele, 2011; Prosperi Porta et al., 2019; Ryan & Smith, 2016; Sim et al., 2017). These results were expected because Jordanian community pharmacists, as well as those worldwide, have changed their care models to provide a multitude of clinical services in keeping with pharmaceutical care concepts (Hemberg et al., 2017).
In the current study, the most common areas in which participants were giving advice were medication safety while breastfeeding, how to administer necessary medication to a breastfed baby, and advice on nutrition while breastfeeding. In 2015, an analysis of 20 in-depth semi-structured interviews undertaken with breastfeeding women by Sim et al. (2015) explored the perspectives of breastfeeding mothers on the pharmacist’s role in Australia. Their results suggested that breastfeeding mothers consider pharmacists as medication experts, and the first point of contact for queries about the use of medications during breastfeeding. Researchers have also found that mothers frequently consult pharmacists with inquiries regarding the suitability of medicines while breastfeeding, the influence of a particular medication on their breastfed infants, and nursing performance and milk production (Sim et al., 2017).
Participants in our study expressed a desire for additional training and education in the field of safety of medication use while breastfeeding, as well as breastfeeding in general. Pharmacists’ ongoing training, along with training for pharmacy students in universities, was considered important in semi-structured interviews with 30 community pharmacists practicing in Western Australian, in a study conducted by Sim et al. (2017). In Kuwait, a cross-sectional study undertaken by Albassams and Awads (2018) found that 88.5% of pharmacists agreed that ongoing education programs on giving advice and solving the health and medication problems of lactating women would improve their practice. Currently, in Jordan, there are no educational programs in pharmacy schools at the university level to educate and encourage pharmacists to support breastfeeding, beyond providing counseling on medication safety during lactation. Based on the findings of the current study, there is scope for the Jordanian Pharmacists’ Association and relevant Jordanian universities to lead in the development of education and training resources targeted at improving breastfeeding support, in particular medication safety during breastfeeding and the practical aspects of breastfeeding support.
Sociodemographic characteristics, particularly the type of residence—that is, working in an urban or rural region—are associated with breastfeeding practices (Permatasari & Syafruddin, 2016). In this study in Saudi Arabia, researchers found that residing in a rural region is one of the characteristics associated with a high prevalence and longer duration of breastfeeding (Al Juaid et al., 2014). In an international narrative systematic review analyzing services provided by community pharmacies in urban and rural settings, pharmacists working in rural areas exhibited a greater inclination towards embracing new professional responsibilities and providing an elevated standard of service (Howarth et al., 2020). Rural areas, with limited access to medical facilities and fewer healthcare providers, rely more heavily on community pharmacists to provide needed support. This could provide insight as to why participants working in rural regions reported providing higher breastfeeding support levels than those in urban areas in our study.
Female participants and married participants reported providing higher breastfeeding support levels, more than half of them being parents with personal breastfeeding experience. Therefore, they may have been more aware of the value and necessity of breastfeeding support.
More than half of the participants reported offering information on breast pumps, bottles, and advice on expressing milk and the storage of expressed milk, and more than one third of participants reported providing general information on breastfeeding support, including local support groups. Despite this, it was not common to offer a comfortable area to breastfeed a baby (not necessarily a private room) or to offer any specific breastfeeding services in their pharmacies. These results may be explained by the fact that community pharmacists play an essential yet dual role in Jordan’s healthcare system (JPA, 2022) This is especially relevant when it comes to providing breastfeeding advice and human milk replacements (i.e., commercial infant formula). While pharmacists are one of the most trusted and accessible primary care providers for breastfeeding mothers and their families, pharmacies are also businesses that rely on front-of-store income, potentially through the sale of infant formula. When pharmacists are not compensated for any breastfeeding advice or counseling, this raises the issue of competing interests between optimal practices in providing breastfeeding advice and commercial considerations (Ryan & Smith, 2016). Notwithstanding this apparent conflict of interest, the sale of human milk replacements is not limited to pharmacies and would not necessarily be a significant commercial consideration in all pharmacies.
This study gives first-hand information and insight into Jordanian community pharmacists’ current practices and their needs for training and education to provide breastfeeding support for lactating women in Jordan. It also sheds light on pharmacists’ position as providers of breastfeeding-related services, an area that has received little attention in Jordan. Additionally, this study included pharmacists from all regions in Jordan, therefore results are likely generalizable within the country.
Limitations
The first limitation of this study was the participant self-selection process. The survey was conducted online due to the novel coronavirus pandemic that started around January of 2020. Hence, only people who use the Internet and other social media platforms were able to participate. Moreover, all information in this study was obtained through self-report. There may be inaccurate “social desirability” responses or recall difficulties. However, we surmise that the anonymity of the questionnaire encouraged honesty. Our model explained only 4% of the variance in breastfeeding support, suggesting that other unmeasured factors may play a more influential role in determining participants’ breastfeeding support levels. Finally, the arbitrary categorization of age groups in this study has the potential to introduce residual confounding. This study also represents only the perspective of the pharmacists and not the parents’ perspective.
Conclusion
Community pharmacists in Jordan report providing a high level of breastfeeding support to breastfeeding women; however, they also conveyed a need for more education and training on breastfeeding support and medicine use while breastfeeding. Based on needs, educational programs at university level for pharmacists in training could address safety and management of medications while breastfeeding, the difficulties that mothers may encounter, the treatment of minor ailments, maternal health while breastfeeding, counseling, and communication skills. Ongoing educational and training programs after graduation, including interprofessional collaboration with other healthcare programs, (e.g., nursing or midwifery), might be one way JPA could assist pharmacists in increasing their knowledge and skills in managing and supporting breastfeeding. However, prior to implementation, further research into pharmacists’ preferences for additional breastfeeding support training would be required.
Supplemental Material
sj-docx-1-jhl-10.1177_08903344231206394 – Supplemental material for Community Pharmacists’ Current Practice and Educational Needs in Breastfeeding Support in Jordan: A Cross-Sectional Study
Supplemental material, sj-docx-1-jhl-10.1177_08903344231206394 for Community Pharmacists’ Current Practice and Educational Needs in Breastfeeding Support in Jordan: A Cross-Sectional Study by Mea’ad M. Harahsheh, Tareq L. Mukattash, Samah Al-shatnawi, Rana Abu-Farha, Sawsan Abuhammad, Deirdre D'Arcy and Anan Jarab in Journal of Human Lactation
Footnotes
Author Contributions
Disclosures and Conflicts of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplementary Material may be found in the “Supplemental material” tab in the online version of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
