Abstract
Objective
This scoping review examined current research on group-based exercise programs for adults with visual impairment (VI) and their outcomes.
Data Source
Searches were conducted using Ovid MEDLINE, Embase, CINAHL Complete, PsycInfo, AMED, and SPORTDiscus.
Study Inclusion and Exclusion Criteria
Included studies were peer-reviewed experimental articles published in English from 2000 to October 2024, reporting group-based exercise programs and outcomes for adults with VI. Studies exploring the experiences of adults with VI in informal group exercise were also included. Excluded were reviews, non-research or unpublished works, theses and dissertations, studies that focused on childhood participation, and those involving professional athletes.
Data Extraction
Data were extracted on program implementation, outcome measures, and key findings. The Template for Intervention Description and Replication (TIDieR) checklist guided reporting on implementation details.
Data Synthesis
The extracted data were analyzed descriptively to identify studies’ patterns and trends. Findings were summarized by study type, with intervention details reported alongside outcomes and assessments.
Results
Thirty-nine studies were included. Programs incorporated various exercise types with adjustments for VI, showing improvements in physical functioning, mental health, and psychosocial well-being.
Conclusions
Group-based exercise programs benefit adults with VI across multiple domains, yet evidence regarding daily functioning, social interaction, and exercise intensity was limited. Addressing these gaps is crucial to developing inclusive and effective programs that support their meaningful participation and well-being.
Introduction
Exercise, a structured and repetitive form of physical activity (PA) performed with a specific purpose, is a key strategy in health promotion. It offers targeted health benefits, such as improved muscle strength through resistance training or enhanced flexibility and relaxation through yoga. 1 Regular participation in exercise contributes to overall physical and mental health, including improved cardiovascular fitness, reduced risk of chronic disease, better mood, and increased longevity. 2 As such, exercise is a widely used and accessible method for supporting population health.
Despite well-established benefits, disparities in exercise participation persist, particularly among individuals with disabilities. People with disabilities face greater challenges in participating in exercise compared to the general population. Barriers such as inaccessible facilities, disability-related health conditions, medication side effects, and social stigma contribute to lower PA levels and poorer health outcomes.3,4 This disparity is especially pronounced for adults with visual impairment (VI), which includes both blindness and low vision. People with VI encounter unique and compounding barriers to exercise. The World Health Organization (2023) identifies VI as associated with restricted mobility, increased fall risk, social isolation, and poor mental health. 5 These challenges often lead to physical inactivity, greater dependence, and elevated risks for chronic conditions such as cardiovascular disease and obesity, all of which contribute to reduced quality of life (QoL).6–8 In addition, adults with VI frequently report both environmental and personal obstacles to participation.9–11 Environmental barriers include inaccessible equipment, transportation difficulties, limited social support, and a lack of inclusive opportunities. Personal factors such as difficulty following visual cues, fear of injury, dependence on others, and the direct impact of vision loss further hinder participation. 12 These challenges reduce motivation and further contribute to withdrawal from exercise. 13 Promoting inclusive, tailored exercise programs is therefore critical to improving engagement, and sustaining exercise participation for this population.
Group-based exercise has gained attention as a promising approach to promote exercise participation. Prior studies have shown that a lack of peer involvement, such as friends and family, can limit exercise engagement among people with disabilities.4,10 Group-based programs that integrate social dynamics can create supportive, enjoyable environments that increase participants’ commitment to the group, thereby reinforcing intrinsic motivation and helping participants adopt more active lifestyles over time.14,15 Peer support within the group can further promote adherence by helping individuals overcome barriers and integrate PA into their routines.3,14 Practices such as assigning group roles—for instance, asking participants to assist or motivate their peers—and establishing inclusive group norms have been shown to strengthen social bonds and enhance belonging. 15 Collectively, these features underscore the potential of group-based exercise to support PA engagement, improve well-being, and address the participation gap among adults with VI.
Research has demonstrated that group-based exercise programs can provide a range of benefits for adults with VI, including improvements in balance, mobility, mental well-being, and health-related QoL.16,17 These outcomes have been observed across various forms of exercise, such as dance and road running. Understanding how these programs are delivered and what outcomes they produce can guide practitioners and service providers in designing more accessible, tailored interventions. 18 However, current reviews offer limited insight into both the outcomes and implementation of group-based exercise programs for this population. For instance, Sweeting et al 19 conducted a systematic review that focused on a small number of randomized controlled trials and pre-post studies, primarily reporting on physical outcomes. Broader impacts—such as psychosocial benefits or changes in attitudes toward PA—were largely overlooked.20,21 Choi and Pionke’s 22 scoping review extended this work by examining the characteristics of exercise programs for adults with VI, such as program durations, frequency, session counts, and accommodation method, yet did not fully report on the outcomes. Moreover, both reviews prioritized studies using quantitative methods that focused on numerically measured outcomes, often overlooking qualitative insights that capture participants’ deeper perceptions. The absence of comprehensive evidence limits our ability to apply group-based exercise effectively as a health-promoting strategy for supporting sustained exercise participation among adults with VI.
The present study addressed this gap, aiming to summarize current research outcomes, including both qualitative and quantitative findings, as well as the implementation of these programs for adults with VI. It examined group-based exercise programs for adults with VI to understand program implementation and outcomes to inform the development of health promotion programs. By doing so, this study can offer valuable insights for developing future exercise programs and strategies that effectively promote exercise participation to improve health and well-being in this population.
Methods
A scoping review is recommended for summarizing and disseminating research findings when there is not yet a universal review on a broad topic.23,24 Therefore, it was a suitable approach to be applied to map the outcomes of group-based exercise programs for adults with VI given current research evidence. The protocol of this scoping review was published previously in Healthy Populations Journal. 25
Data Sources
The search strategy of this scoping review involved both electronic databases and manual searching. The electronic database searching was guided by the Peer Review of Electronic Search Strategies (PRESS) guidelines. 26 We applied the PICO (Population, Intervention, Comparison, and Outcomes) format to derive search terms, 26 and conducted searching using Ovid MEDLINE, Embase, CINAHL Complete, PsycINFO, AMED, and SPORTDiscus on 1st October 2024. Given that “comparison” was not applicable, the search focused exclusively on terms related to “visual impairment” and “exercise”. 25 A complete set of search terms for each database is provided in the Supplemental Table. Manual searching was also conducted by reviewing the reference lists of the studies that were selected for full-text screening. All the identified studies were imported into the online screening application software, Covidence, for review.
Inclusion and Exclusion Criteria
Studies were included if they met the following criteria: (a) published in English, (b) peer-reviewed experimental studies, (c) studies published from 2000 to October 2024, (d) participants aged 18 and over who have a VI, and (e) reporting on the results of group-based exercise programs and interventions for adults with VI. Where studies involved the inclusion of participants younger than 18 years, those with more than 50% of participants aged 18 and over were considered. In addition, studies with adult participants with multiple conditions, which included VI, were also considered. Exclusion criteria were: (a) review papers, text and opinion papers, academic presentations, theses and dissertations, and articles on organizational websites, (b) studies with participants engaged in group-based exercise when they were under 18 but investigated in their adulthood, and (c) studies with participants who were national level or professional athletes.
The search strategy identified 7217 studies for possible inclusion in this scoping review. After 1728 duplicates were removed, two authors independently reviewed the titles and abstracts of the remaining 5489 studies. One author (C-WC) reviewed all the studies, and three authors (AL, NT, and M-DC) reviewed a third of each of the identified studies. A total of 5303 studies were excluded during title and abstract screening. The remaining 186 studies were reviewed by three authors at the full-text stage. To ensure their suitability for inclusion, each study was independently screened by two authors: one author (C-WC) completed a full-text review of all the included studies, and two authors (AL and NT) each completed full-text reviews on half of the included studies (ie, 93 studies each). One hundred and forty-seven studies were excluded during full-text screening. The remaining 39 studies were included in this scoping review. The process and decision making regarding inclusion or exclusion was undertaken using Covidence. Disagreements between authors were resolved through discussions to reach a consensus or with the involvement of an additional reviewer (either AL or NT). The study selection process is outlined in the Systematic Reviews and Meta-analyses extension for Scoping Review (PRISMA-ScR) flow diagram (Figure 1). PRISMA diagram of study selection process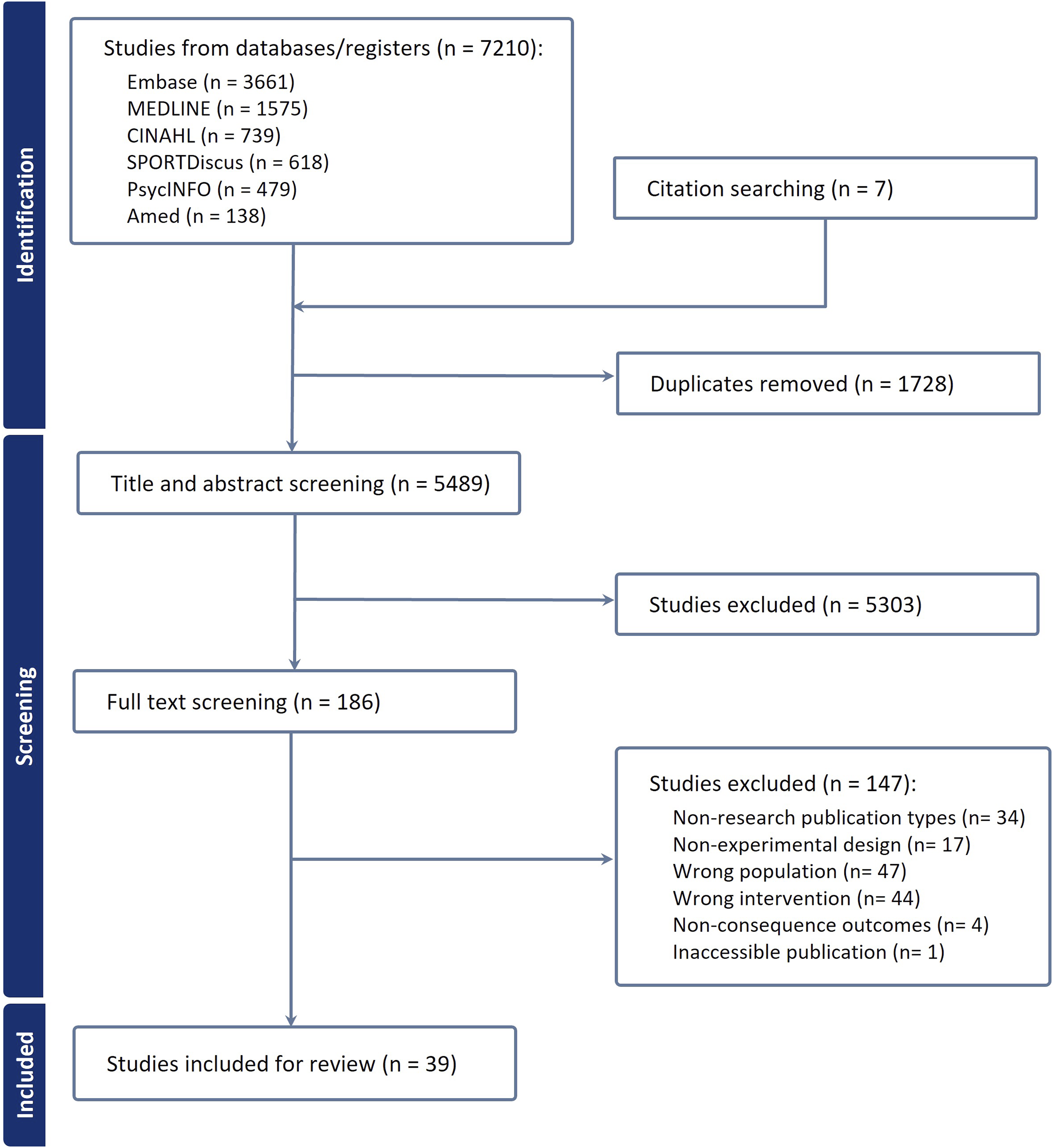
Data Extraction
The included studies were tabulated using information about the study’s outcome(s) and corresponding exercise(s). To ensure the relevancy of information drawn from included studies would help guide future research and practice, the Template for Intervention Description and Replication (TIDieR) checklist was used to develop the charting form. 27 Information regarding the study title, author(s)’ name, year and place of publication, study design, sample size, and participants was also collected alongside information about outcomes, key findings, and measures utilized. Statistical significance of quantitative outcomes was extracted, if available. The selected studies were independently charted by the two authors (C-WC and AL). Disagreements between authors on data charting were resolved by discussion or consultation with a third author (NT).
Data Synthesis
Data were analyzed descriptively to identify patterns and trends across the included studies. The included studies were categorized according to the types of studies (eg, quantitative or qualitative), and analysed with respect to the nature of each study’s intervention and outcomes. Intervention details are presented according to the TIDieR checklist, which includes the name/type of the exercise, materials needed, procedure, intervention/program provider(s), methods/mode of intervention/program delivery, intervention/program location, intervention/program intensity, tailoring required, and modifications. Exercise outcomes were reported along with the corresponding assessment and synthesized narratively according to the study type. Tables were used to present a summary of each study’s intervention, assessments, and key findings, providing a clear overview of patterns across all included studies.
Modification
In conducting this scoping review, two modifications to the study eligibility criteria as specified in the protocol were implemented. 25 The first modification involved only including studies that focused on group-based exercise. Group-based exercise formats are known for their potential to improve health outcomes through increased social interaction, better psychological well-being, and higher levels of motivation.28–30 This is particularly important for visually impaired populations, where psychological issues can hinder engagement in PA.17,19,20 The presence of peers during exercise can also mitigate barriers to participation, as the absence of social interaction often discourages involvement.9,10 The second modification involved considering studies that did not deliver exercise programs for the participants but instead explored the experiences of adults with VI in group exercise settings. During the screening process, we found that some studies focused on participants’ exercise experiences, including their perceived outcomes, even though no program was implemented. As our goal is to provide a comprehensive understanding of exercise outcomes, we decided to include these studies to capture a broader perspective.
Results
Study Information
Characteristics of Included Studies
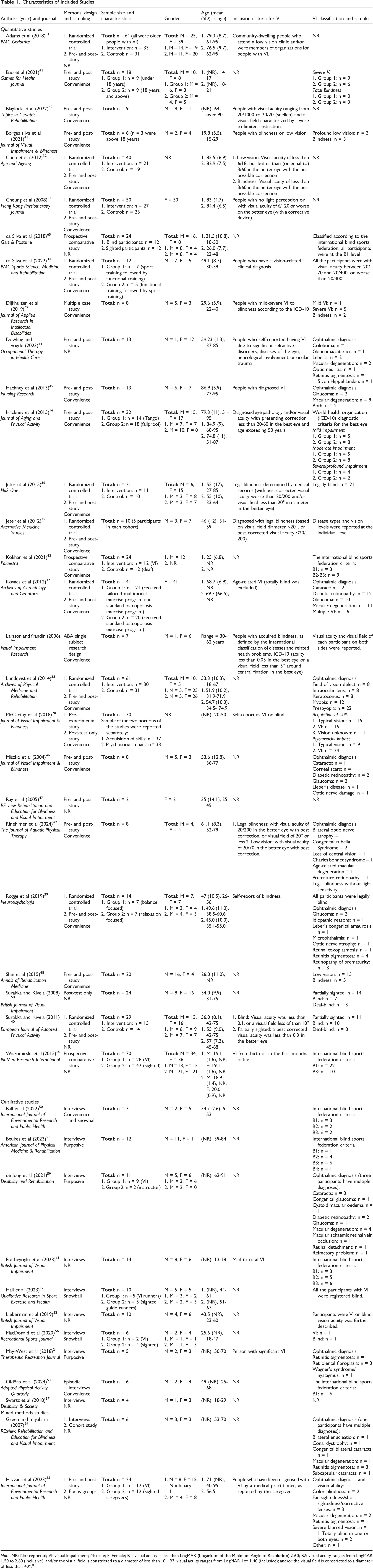
Note. NR: Not reported; VI: visual impairment; M: male; F: Female; B1: visual acuity is less than LogMAR (Logarithm of the Minimum Angle of Resolution) 2.60; B2: visual acuity ranges from LogMAR 1.50 to 2.60 (inclusive), and/or the visual field is constricted to a diameter of less than 10°; B3: visual acuity ranges from LogMAR 1 to 1.40 (inclusive); and/or the visual field is constricted to a diameter of less than 40°. 8
Exercise Programs - TIDieR Checklist
Name, Rationale, Material, Process, Providers, How, and Where Exercise Programs for Adults With VI Were Conducted (TIDieR Checklist)

Note. NR: not reported; VI: visual impairment; MD: Maryland; VA: Virginia; 1RM: one repetition maximum.
When and How Much, Tailoring, Modifications, and How Well Exercise Programs for Adults With VI Were Conducted (TIDieR Checklist)

Note. NR: not reported; 1RM: one repetition maximum.
Brief Name
The majority of the included studies named their group-based exercise programs. Most of the programs’ names were based on the sport or exercise itself, such as “Tai-Chi”32,46,47 and “Yoga”.35,36,44 For those not named, descriptions were provided to clarify the program’s characteristics. For example, a program aimed at improving the QoL and well-being of participants, 55 sports programs including goalball and martial arts, 34 multimodal exercises, 37 standard osteoporosis exercises, 37 and multidimensional physical training programs. 40 Those conducted unspecified exercise programs were labelled based on their contents and purposes.
What was the Rationale for the Program
The included studies implemented and investigated exercise programs based on rationales informed by prior research and population-specific needs. Most studies adopted exercise approaches to address well-documented benefits of PA, such as improved physical function and mental health. For instance, Chen et al. 32 selected Tai-Chi for its known effects on balance and muscle strength, while Jeter et al. 35 designed an Ashtanga yoga program to improve sleep quality and reduce anxiety. Several programs were tailored to meet the unique challenges faced by adults with VI, such as fall prevention and stress reduction.33,37,55 A few studies explored unique delivery methods, such as audio-tactile techniques or running with guide dogs, aiming to support safe and effective participation.43,52 In addition, some research drew on broader concepts such as social inclusion and policy support as foundational elements in their program rationale.42,56,57 These rationales provide valuable insights for informing the development of inclusive and evidence-based interventions.
What Materials and Procedures Were Used
Various materials were employed across the included programs to enhance safety and support participation. Audio and lighting aids were commonly used to compensate for visual limitations and facilitate engagement.16,31,35,36,40,41,43,44,58–60 Large-print handouts were also used in educational programs to improve accessibility.31,42,59 Some studies incorporated music, which served as feedback, background rhythm, or motivational stimulus, particularly in dance-based interventions.41,43,60,61 Additionally, exercise mats and resistance bands were applied to support performance and reduce the risk of injury during the programs.31,37,43 These materials contributed to a more inclusive and supportive exercise environment.
Programs typically included warm-ups and cool-downs, incorporating stretching and breathing exercises.16,35,36,40,43,45,46,48,49,58,61 Exercises targeted strength, balance, and flexibility using bodyweight, resistance, or weighted methods.37,48,62 Activities like Tai-Chi, yoga, and dance emphasized coordination, body awareness, and teamwork.32,35,36,38,41,43,44,46,47,60,61 Some programs also included discussions for participants to ask questions and share insights.31,35,38,42
Who Provided the Programs
The group-based exercise programs were led by a range of professionals, including the researchers,41,42,44,49,55 licensed exercise instructors,16,35,36,44,45 physiotherapists,33,38,43 and specialists like Tai-Chi or dance instructors.16,45,46 Some programs were facilitated by organizations like the Royal New Zealand Foundation of the Blind. 54 Volunteers, including trained undergraduate students and assistants, were common in supporting participants with VI,36,61 however, detailed information about their roles was often lacking.
How Were the Programs Delivered
Most programs were conducted in person, allowing hands-on assistance. Modification to an exercise, verbal instructions, and additional assistance from volunteers or assistant instructors were widely used in these programs. While all the included studies were applied in group format, some studies paired participants with sighted partners for guidance, common in dance and sports programs.16,17,21,45,50–52,57 Few studies delivered computer-based programs, such as PA sessions conducted via Zoom and interactive exercise games.41,44,55
Where the Programs Were Delivered
The group-based exercise programs in the included studies were held in various settings. Some were held in facilities specifically for people with VI, such as schools for the blind or blind rehabilitation centers.41,42 Others targeted older adults and took place in a caring center or senior living communities.16,32 Locations such as local studios and sports centers were also used.36,58,63 Additionally, community venues and local churches were used.31,35,59 Accessibility, particularly regarding transportation, was a key factor in selecting these locations, as noted in a number of studies.35,36,46
Intensity, Frequency, and Length of Programs
Most of the included studies detailed program duration, frequency, and session length. Programs lasted from days to months, with many lasting 12 weeks.16,31,33,38,39,45,59 Sessions ranged from one to five days a week, with twice-weekly sessions being common.16,37,39,42,43,45–47,49,60–64 Session lengths varied from 20 to 120 min, with most lasting 60 to 90 minutes.16,31,32,35,36,40,42,44–47,49,61,63,64
Program Tailoring and Modification
Many studies tailored group-based exercise programs to accommodate participants with varying levels of VI and fitness. Auditory cues, such as verbal guidance and feedback, were commonly used, often paired with tactile instruction for movement feedback and assistance.16,20,32,33,41,43,45,46,58,63 Simple descriptive language and directional terms were integrated into instructions,44,58 while some programs incorporated visual aids like video demonstrations and accessible materials.42,63 Exercise intensity was adjusted based on participants’ fitness levels, starting at 40%-50% of their one-repetition maximum (1RM) and increasing gradually.33,35,48,62
Three studies adapted existing exercise programs originally developed for other populations to better suit the needs of individuals with VI. Hackney et al. adapted a Tango program for individuals with Parkinson’s disease, adding transportation services, clear step descriptions, tactile communication, and longer class durations.16,45 Similarly, Esatbeyoglu et al. adjusted their dance program to prevent eye and head pressure for participants with VI. 61
How Well (Planned): Assessment of Intervention Adherence or Fidelity
Four studies planned to assess program success through adherence and compliance. Adherence was tracked via participants’ attendance (75%-87.5% of sessions) and self-reported home exercise practice.31,35,60,62 Compliance was evaluated based on meeting specific benchmarks, such as training up to 80% of baseline 1RM muscle strength by program end. 62
How Well (actual): How Well Was the Intervention Delivered
The actual success was assessed in twelve studies through adherence measures, including dropout rates (5.7%-14.3%) and program completion rates (60%-100%).16,31,33,35,37,42,44,45 Attendance varied: Dijkhuizen et al reported a training attendance rate of 87.8%, 62 while Jeter et al recorded averages of 7.5 out of 8 weekly sessions for one cohort and 7 out of 8 for another. 35 Overall adherence rates ranged from 64.3% to 77.1%.34,38
Outcomes
Measurement and Findings of the Included Studies (n = 39)

Note. NR: not reported; VI: visual impairment.
Measures Used
The included studies used quantitative and qualitative methods to assess program outcomes. Quantitative approaches employed objective measures and subjective questionnaires. Physical function was evaluated using tools like the Berg Balance Scale,16,33,37,46 one-leg stand test,35,36,64 and the functional reach test.46,64 Lower limb strength was assessed using the chair stand test,33,36,45,49 while flexibility was measured through the sit-and-reach test.34,36 Mobility, on the other hand, was commonly measured using the timed up-and-go test.16,31,33,37,64 Specialized equipment, such as the Cybex Norm dynamometer, 32 Kin-Com isokinetic dynamometer, 46 and Biodex Balance System, 60 was occasionally used. QoL was assessed with tools like the World Health Organization Quality of Life Questionnaire (WHOQOL-Bref), 34 Visual Function Questionnaire-25 (VFQ-25),16,45 and SF-36. 38 Questionnaires also measured self-efficacy, 41 PA levels, 65 and fear of falling.31,65
Qualitative methods primarily involved interviews, with one study employing a focus group. 55 Eight studies used semi-structured interviews to explore participants’ program experiences and perceived outcomes.17,50–52,54,56,59,61 Questions included topics like participation history, feelings about the program, and benefits of exercise, such as “How did you feel about the capoeira dance program?” 61 and “What are the benefits of running with a guide dog?”. 52 May-West et al. 21 conducted in-depth interviews in three sessions, exploring participants’ life histories and program reflections, while Oldörp et al. 53 used episodic interviews to examine insights on blind tennis skills. Two studies used group formats involving people with VI and their assistants. Beukes et al. 51 interviewed VI golf participants and their guides, and Hazzan et al. 55 held a focus group with older adults with VI and caregivers to discuss program effectiveness and QoL.
Findings
The majority of the quantitative findings indicated improvements in participants’ physical functioning and psychosocial outcomes and well-being. Concerning physical functioning, these improvements were notably mobility-related. Studies highlighted enhancements in balance, muscle strength, muscular endurance, risk of falls, flexibility, and gait speed.16,32,33,35–39,45,46,49,58,64,65 However, certain studies noted decreases in mobility-related outcomes, attributed to altered exercise procedures and potential sample bias.31,64 Additionally, improvements were also reported in other aspects of physical functioning, such as enhanced sports performance, pain relief, increased PA levels, and reduced body fat.38,48,54,63 Different from demonstrating the improvements, da Silva et al. 65 observed that participants with VI who participated in group sports demonstrated physical functioning performance comparable to that of individuals without VI. Regarding psychosocial outcomes and well-being, studies highlighted improvements in QoL, mood, mental health, social interaction, sleep quality, and decreased anxiety.16,34,41,43–46,58 Furthermore, exercise knowledge and mastery among participants following their participation were also reported, finding that participants demonstrated a deepened understanding of exercise concepts, including the knowledge of fall prevention strategies and the skill of self-defence.20,42
The qualitative findings from the studies highlighted participants’ perceptions and challenges regarding their participation in a group-based exercise program. Many participants enjoyed the programs and reported improved health and increased social interactions as outcomes.21,50–52,55,56,59,61 These health-related improvements encompassed physical fitness, mental health, psychosocial well-being, and overall well-being, and were attributed to increased PA and socialization opportunities. Social interactions were fostered among peers and instructors, leading to friendships.17,21,55,56,61 These interactions can extend beyond exercise sessions, allowing participants to share experiences and educate others.21,51,54 Furthermore, improvements in body perception and self-confidence were noted, contributing to a reduced sense of disability and enhanced self-esteem in daily life, particularly in areas such as orientation, mobility, and travel.41,51,53,56 However, participants also faced barriers to participation, reporting being unable to access appropriate support. These barriers included difficult to find sighted runners, using unfamiliar software, and risky road conditions.17,50,52 Additionally, feelings of exclusion often stemmed from sighted norms that led to assumptions about the infeasibility of exercise for people with VI. 53 Despite the challenges, participants in the study by Esatbeyoglu et al highlighted the value of consistent practice in overcoming obstacles and enabling their on-going participation. 61
Discussion
This scoping review examined 39 studies featuring 36 group-based exercise programs for adults with VI, highlighting a diverse range of program implementations and outcomes. The variety of exercise types and research focuses led to a broad spectrum of reported benefits, offering valuable insights for future health promotion research and exercise program development for this population. Unlike previous reviews by Sweeting et al. 19 and Choi and Pionke, 22 which focused on limited research designs and outcomes, this review included both quantitative and qualitative studies, capturing a wide range of evidence. By integrating diverse approaches, it offers a more comprehensive understanding of group-based exercise outcomes and implementations for adults with VI.
The findings from the included studies suggest that structured and adaptable program designs are essential for optimizing engagement and outcomes in people with VI. Most programs used verbal instructions and physical guidance to help participants understand and perform exercises correctly. Additionally, there are some key strategies identified in studies with higher adherence and completion rates: family involvement to enhance motivation, 45 tailoring exercises to meet individual needs and abilities,33,37 encouragement from trained instructors to reinforce engagement, 41 and accessible locations or virtual platforms to improve participation.35,44 These strategies align with exercise recommendations for people with VI, and demonstrate their effectiveness in promoting exercise participation.66,67
The programs were commonly structured as twice-weekly sessions lasting 60 to 90 min over a 12-week period. While this format was reported to produce positive outcomes for people with VI, most included studies did not specify the intensity of the exercise (eg, moderate or vigorous). According to the WHO, adults and older adults should engage in 150 to 300 min of moderate-intensity aerobic activity, or 75 to 150 min of vigorous-intensity activity per week, along with muscle-strengthening exercises involving all major muscle groups at least twice weekly. 2 Without consistent reporting on exercise intensity or participants’ total PA levels, it is difficult to determine whether these programs met recommended activity thresholds. Moreover, it remains unclear whether the observed benefits were due to the structured group-based interventions, unreported PA outside the programs, or even sub-threshold exercise intensities that were nonetheless beneficial. More comprehensive reporting of both program intensity and participants’ overall activity levels is needed to clarify the relationship between exercise dosage and health outcomes in this population.
The included studies consistently highlighted improvements in physical function (eg, mobility, balance, strength), psychosocial well-being, and QoL. Quantitative studies primarily focused on measurable mobility-related outcomes, while qualitative research explored social interaction, independence, and psychological resilience. Exercise participation is generally expected to enhance individuals’ functional capacity and independence beyond the exercise setting. 68 Adults with VI often encounter challenges in daily life, such as managing household tasks and navigating their environments. 69
Despite the positive outcomes documented, few studies examined how these improvements translated into their daily activities. For instance, although mobility was frequently assessed through gait and balance measures, its implications for independent travel or community engagement—common challenges for people with VI—were rarely examined. 69 Likewise, although self-efficacy, emotional well-being, and social connectedness were frequently reported as benefits, their roles in supporting sustained PA engagement and daily autonomy were largely underexplored, despite their known significance in promoting health and well-being among individuals with VI.70,71 These gaps limit the applicability of group-based programs as interventions that support functional engagement in everyday life. Future research should further investigate how exercise-related improvements contribute to daily functioning and support greater independence among adults with VI.
Social interaction is a core feature of group-based exercise programs and was frequently associated with positive psychosocial outcomes. Research has shown that exercise programs incorporating social interaction foster psychosocial benefits such as enjoyment, well-being, and a sense of belonging across diverse ages and abilities.66,72,73 These elements are essential for building meaningful social support. 74 The included studies further highlighted that social interaction enabled participants to engage with others, build friendships, and benefit from both PA and socialization. Participants reported high levels of happiness in being part of a group-based program.17,21,41,44,50 While negative psychosocial outcomes from social interactions—such as experiences of prejudice or discrimination—have been shown to hinder engagement, 17 the positive influence of group participation on sustained outcomes remains underexplored among the included studies. Evidence from other populations suggests that group-based exercise fostering cohesion, peer encouragement, and shared responsibility can enhance motivation and long-term participation in PA. For example, for breast cancer survivors, incorporating peer support and group cohesion into exercise programs has been shown to promote continued physical activity after completing structured interventions. 14 How social interaction within the exercise programs influences adherence among people with VI, and whether peer support can promote long-term functional independence, remains an important area for future research.
This scoping review identifies implementations and outcomes that can guide the design of future exercise programs for adults with VI. By applying the TIDieR checklist, it provides detailed descriptions of intervention components. The use of verbal instruction and physical guidance underscores the need for developing accessible exercise environments. Given that sustained participation is critical for achieving health benefits, 2 the findings underscore the value of strategies such as family or peer involvement, individualized modifications, encouragement from trained instructors, and accessible program locations. These insights suggest a need for public policies that support the development of VI-inclusive exercise settings, such as funding and project development for trained staff, adapted facilities, and community-based program delivery. Clinical practice may also benefit from integrating these features into routine rehabilitation and health promotion services to help maintain participation beyond structured programs. The outcomes of the included studies demonstrated the improvement of physical functions, psychosocial health, and QoL of their participants. These domains have been known to be areas of concern for adults with VI.5–8 Policymakers and practitioners can use these outcome areas as meaningful targets when designing or evaluating PA initiatives. The findings also imply research gaps. Limited reporting on exercise intensity and insufficient examination of how functional improvements translate into daily life restrict the ability to make specific recommendations. Future research should therefore clarify the role of exercise dose and explore how gains in physical and psychosocial functioning support daily independence. Standardized monitoring of PA intensity and functional outcomes would enhance the integration of exercise interventions into long-term health management. Additionally, the influence of social interaction on engagement and sustained outcomes remains underexplored; further investigation in this area could strengthen public health initiatives that position group-based programs as an inclusive model for PA promotion among people with VI.
This study has some limitations. First, the inclusion of only English-language studies may have excluded valuable research published in other languages, potentially narrowing the diversity of cultural and regional insights. Second, this review did not explore contextual factors such as environmental accessibility, cultural attitudes, and regional healthcare systems, which may limit the transferability of findings and leave practical applicability and feasibility underexplored. Lastly, reliance on published literature may have introduced publication bias, favoring studies with positive results while excluding unpublished or negative findings, thereby restricting the comprehensiveness of the evidence base.
Conclusion
This scoping review highlights the importance of thoughtful program adaptation and design, as well as the wide-ranging benefits of group-based exercise for adults with VI, including improvements in physical function, mental health, and psychosocial well-being. Verbal instruction and physical guidance were commonly applied strategies to facilitate participation. However, limited reporting on exercise intensity made it difficult to assess whether programs aligned with PA guidelines. Quantitative studies primarily reported improvements in mobility-related outcomes such as balance, strength, and gait, while qualitative findings provided deeper insights into enhanced social interaction, independence, and psychological resilience. Despite these benefits, few studies examined how these improvements translated into everyday life, such as independent travel or household activities. Similarly, although social connection and self-efficacy were frequently discussed in qualitative accounts, the role of social interaction in promoting sustained participation and long-term functional independence was not clearly articulated in the literature. To strengthen the role of group-based exercise in health promotion for people with VI, future research should examine its impact on daily life and clarify how social interaction contributes to outcomes. Clearer reporting on exercise intensity is also needed to guide effective, inclusive program design. Adults with VI face substantial barriers to participating in PA, often leading to sedentary lifestyles and increased health risks. Group-based exercise has shown potential for enhancing motivation, participation, and psychosocial well-being across various populations, including those with disabilities. However, a comprehensive review focusing specifically on adults with VI has been lacking. This scoping review synthesizes findings from both qualitative and quantitative studies on group-based exercise programs for adults with VI, examining program outcomes and implementation strategies. It identifies common program adaptations, such as verbal instruction and accessible environments, that support participation. The review also highlights improvements in physical functioning, psychosocial outcomes, and overall well-being, while revealing key evidence gaps in reporting exercise intensity, assessing daily activity outcomes, and understanding how social interaction facilitates program participation. To improve health outcomes for adults with VI, health promotion practice should incorporate accessible, socially supportive, and adaptable exercise strategies. Future research should focus on exploring how group-based exercise supports daily functioning and independence, clarifying the role of social interaction in promoting sustained participation, and considering reporting of exercise intensity and real-world outcomes to better align with public health guidelines.“So What?’’
What Is Already Known on This Topic?
What Does This Article Add?
What Are the Implications for Health Promotion Practice or Research?
Supplemental Material
Supplemental material - Group-Based Exercise Programs for Adults With Visual Impairment: A Scoping Review of Implementations and Outcomes
Supplemental material for Group-Based Exercise Programs for Adults With Visual Impairment: A Scoping Review of Implementations and Outcomes by Chun-Wei Chang, MSc, Nikos Thomacos, PhD, Ming-De Chen, PhD, Aislinn F. Lalor in American Journal of Health Promotion
Footnotes
Acknowledgments
The authors would like to thank Paula Todd (Liaison Librarian: Medicine, Nursing, and Health Sciences at Monash University, Victoria, Australia) for helping with the development of the full search strategy for Ovid MEDLINE.
Author Contributions
Chun-Wei Chang: Conceptualization, Methodology, Software, Validation, Formal analysis, Investigation, Resources, Data Curation, Writing - Original Draft, Writing - Review & Editing, Visualization, Project administration. Nikos Thomacos: Conceptualization, Methodology, Software, Formal analysis, Investigation, Data Curation, Writing - Review & Editing, Project administration. Ming-De Chen: Conceptualization, Methodology, Software, Formal analysis, Investigation, Resources, Data Curation, Writing - Review & Editing, Project administration. Aislinn Lalor: Conceptualization, Methodology, Software, Formal analysis, Investigation, Data Curation, Writing - Review & Editing, Visualization, Project administration.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
