Abstract
Purpose
To evaluate the real-world effectiveness of a longstanding community-based National Diabetes Prevention Program (DPP) on participation and weight-loss for Latino(a) adults.
Design
Retrospective cohort analysis.
Setting
The yearlong program was delivered in an urban area of Colorado by a team of Latino(a) community health workers in partnership with a safety-net healthcare organization.
Subjects
National DPP participants between January 2014 and December 2023.
Measures
Outcome measures included National DPP sessions attended and achievement of ≥5% weight loss. Covariates included demographics, body mass index, self-reported physical activity, and health status.
Analysis
Descriptive statistics and multivariable logistic regression analyses evaluated associations between demographic and program-related characteristics with program attendance and ≥5% weight loss.
Results
2377 participants were included; median age 44 years (IQR 37, 52), 86.1% female, 89.8% Latino(a), and 82.0% Spanish speakers. Among 1988 participants who attended ≥8 of 20 sessions within 6 months and had 2 or more weight values, 31.6% achieved ≥5% weight loss. Weight loss of ≥5% was associated with male sex, attendance of ≥16 of 26 sessions, participation in later cohorts, ≥20% sessions with ≥150 minutes per week physical activity, and high self-reported health status.
Conclusion
Community-based National DPP programs can be an effective strategy for increasing program participation and supporting weight loss among Latino(a) adults. Ongoing efforts to engage Latino men in such programs are needed.
Keywords
Purpose
Compared to non-Latino(a) White adults in the U.S., Latino(a) adults have a higher prevalence of type 2 diabetes, worse diabetes control once diagnosed, and higher rates of diabetes complications including kidney failure, depression, cardiovascular disease, and mortality.1,2 Additionally, prediabetes, which carries a 5-10% annual and up to 70% lifetime risk of progressing to type 2 diabetes, affects an estimated 34.6% of Latino(a) adults.1,3 Intensive lifestyle change programs such as the National Diabetes Prevention Program (DPP) are effective in delaying or preventing diabetes among individuals with prediabetes. 4 However, participation and subsequent weight loss has been low among Latino(a) adults, especially those from lower-income households who may be at higher risk. In a previous study of a safety-net clinic-based National DPP intervention, only 15.6% of Latino(a) participants achieved ≥5% weight loss compared to 26.1% of non-Hispanic White participants. 5 These findings raise concerns about the real-world effectiveness of diabetes prevention programs for Latino(a) adults, particularly those with limited English language proficiency and lower income.5,6
Barriers to participation in diabetes prevention programs particularly relevant to low-income Spanish-speaking Latino(a) adults in the U.S. include lack of coverage for the program through health insurance, limited English language proficiency, and low health literacy.7,8 In response to the needs of this high-risk population, multiple culturally tailored diabetes prevention interventions for Latino(a) adults have been developed and tested in the past 2 decades. A systematic literature review of studies published between 2008 and 2016 found that culturally tailored diabetes prevention interventions for Latino(a) adults are modestly effective in decreasing risk for type 2 diabetes through weight loss and lowering of A1c. 9 All 12 of the studies reviewed were offered in Spanish and took place in community locations; 11 studies utilized a peer educator or community health worker (“promotor/promotora” in Spanish); and several studies incorporated modifications for literacy (9 studies), Latino(a) foods and recipes (7 studies), or community input (8 studies). Despite these promising findings, dissemination of culturally tailored diabetes prevention interventions for Latino(a) adults has, until recently, been limited by the lack of adoption of a standardized program and limited availability of culturally tailored curriculum materials.
The National DPP lifestyle change program is an evidence-based program that was selected in 2012 by the Centers for Disease Control and Prevention (CDC) for implementation across the United States.10,11 This program is based on research showing that people with prediabetes can decrease their risk of developing type 2 diabetes by 58% (71% for people over 60 years of age) through weight loss of 5-8% after adopting healthier eating habits and increasing physical activity.11-13 Standardized implementation of the National DPP program is achieved through CDC recognition of participating organizations which are required to deliver the yearlong group program through trained Lifestyle Coaches and using either a CDC-developed curriculum available in English and Spanish or a CDC-approved alternate curriculum. 10 Previous evaluations of National DPP lifestyle change programs have shown that participants who are Latino(a) and uninsured are significantly less likely to achieve 5% weight loss compared with those in corresponding reference groups and that this discrepancy is associated with differences in program attendance.5,14 However, factors associated with program attendance and weight loss among Latino(a) adults with moderate to high attendance rates have yet to be identified.
The primary aim of this evaluation was to investigate the effectiveness of a longstanding community-based CDC-recognized National DPP that utilized culturally tailored materials and community health workers (promotoras) in achieving program completion and 5% weight loss among primarily Spanish-speaking, Latino(a) adults living in low-income, urban neighborhoods in Colorado.
Methods
Design and Sample
The National DPP was implemented by Vuela for Health (Vuela), a community-based non-profit organization, in partnership with a safety-net healthcare organization, in an urban setting. The Vuela DPP was funded by a Colorado Department of Public Health and Environment grant program and was offered at no cost to participants. The Vuela DPP is primarily delivered in Spanish to meet the needs of the local Latino(a) community; however, it is open to all community members, aiming to provide evidence-based diabetes prevention support to all.
Participants were recruited by the community-based organization through outreach in community settings (churches, schools, etc.), word-of-mouth referrals from other participants, or referrals from clinical providers from local healthcare clinics. Adults 18 years and older, at risk for diabetes (based on a diagnosis of prediabetes, history of gestational diabetes, or a high score on the CDC Prediabetes Risk Test which assesses risk based on demographic characteristics) were encouraged to enroll. 15 The Vuela DPP maintained CDC National DPP recognition and utilized the CDC English and Spanish curricula throughout the evaluation period.
The Vuela DPP used the 2012 CDC-developed curriculum for cohorts that started in 2014 through 2016 and the PreventT2 curriculum for cohorts that started in 2017 through 2023.16,17 The program director reviewed culturally adapted program curriculum annually to ensure fidelity to the CDC standard. Group educational sessions were held at community locations including churches, schools, and other community settings. Additional cooking, shopping, and exercise classes were offered and cultural adaptations regarding dietary choices and habits were integrated into the approved curriculum. During the COVID-19 pandemic, classes were quickly transitioned from in-person to distance learning (live remote virtual sessions), followed by a hybrid option once it was safe to return to in-person gatherings. As required for CDC-recognized programs, the Vuela DPP program consisted of 16 hourly sessions held at approximately weekly intervals during the first 6 months, followed by 6 to 8 sessions held bimonthly to monthly during months 7-12. Cohorts of 4 to 6 groups with approximately 10-15 participants each were started at 3 time points each year, throughout the evaluation period of January 2014 – December 2023.
Sessions were conducted by Spanish-speaking promotoras, who were trained on the National DPP curriculum to serve as Lifestyle Coaches. The program director maintained certification as a Master Trainer through the Diabetes Training and Technical Assistance Center and promotoras had monthly continuing education. 18 Additional promotora training topics covered culturally responsive diabetes prevention, motivational interviewing, chronic disease management, mental and sexual health, trauma-informed care, leadership, case management, and community resource navigation. Promotoras received certifications and refreshers to enhance their effectiveness and cultural competency.
This evaluation measured the real-world effectiveness of a National DPP program utilizing the CDC Spanish curriculums on program participation and ≥5% weight loss among Latino(a) adult participants using a retrospective cohort design. Programmatic data (e.g., demographics, weight, height, physical activity, attendance) were collected at intake and at each attended session. Data for the analysis were obtained from program records and stored in REDCap. 19 Any participants under 18 years at the start of the program or participants that had a diagnosis of diabetes or A1c indicating diabetes, were excluded from the analysis.
This evaluation was determined to be non-human subjects research (secondary data analysis) and received IRB Exemption from the Colorado Multiple Institutional Review Board.
Measures
The primary outcome measure was an achievement of at least 5% weight loss (calculated based on weight at intake and weight at the last attended session). Weight loss in the range of 5-7% of baseline body weight is one of the outcome goals recommended for the National DPP.20-24 Predictor variables included the total number of National DPP sessions attended and self-reported weekly minutes of physical activity. The National DPP lifestyle change program guidelines recommend attending at least 8 sessions and achieving an average of 150 min per week of physical activity. The physical activity measure was reported as percent of attended sessions with self-reported “recommended physical activity” defined as ≥150 min per week. Additional covariates included demographic information (collected at intake), and self-reported health status ratings (collected at intake and post-program evaluation). Body mass index (BMI) was calculated from height and weight if both were available. Data on language, formal education, insurance type, and self-reported health status were not collected for participants in cohorts one through 3, which were conducted prior to 2015. As a result, analyses involving these variables were limited to data from cohorts 4 and above.
Analysis
Frequencies and proportions were used to describe the demographic, programmatic, and health outcome characteristics of participants who attended fewer than 8 sessions and those who attended 8 or more sessions in the first 6 months. These same characteristics were also compared between those who did not achieve 5% weight loss and those who did. Chi-square tests were used to detect differences in categorical variables. In addition to being presented categorically, age, weight, and percent of sessions with recommended physical activity were also analyzed as continuous variables and summarized using medians and interquartile ranges (IQR) due to non-normal distribution.
BMI values at program intake and completion were compared using Bowker’s test of symmetry. Bivariate logistic regression analysis was performed to assess the unadjusted odds of having achieved weight loss of 5% or more of initial body weight. Factors that were significant in bivariate analyses or held clinical or programmatic meaning were considered for the multivariable logistic regression model, in which a complete case analysis based on observed data was used. For variables with high missingness, patterns of missing data were assessed by comparing characteristics of participants with and without complete data. Where missingness appeared non-random, variables were excluded from the multivariable model to avoid bias, but retained in descriptive analyses to support transparency and acknowledge their relevance as social determinants of health. Adjusted odds ratios and 95% confidence intervals (CIs) were calculated as the measure of association. An alpha of 0.05 was used as significant for all tests. SAS Enterprise Guide 8.3, R version 4.4.2, and the web-based platform Flourish were used for analyses and data visualization.
Results
Sociodemographic, Programmatic, and Health Outcome Characteristics of Participants in the Vuela Diabetes Prevention Program, Comparing Participants Who Attended Fewer Than Eight Sessions With Those Who Attended at Least Eight Sessions Within the First Six Months (N = 2377)
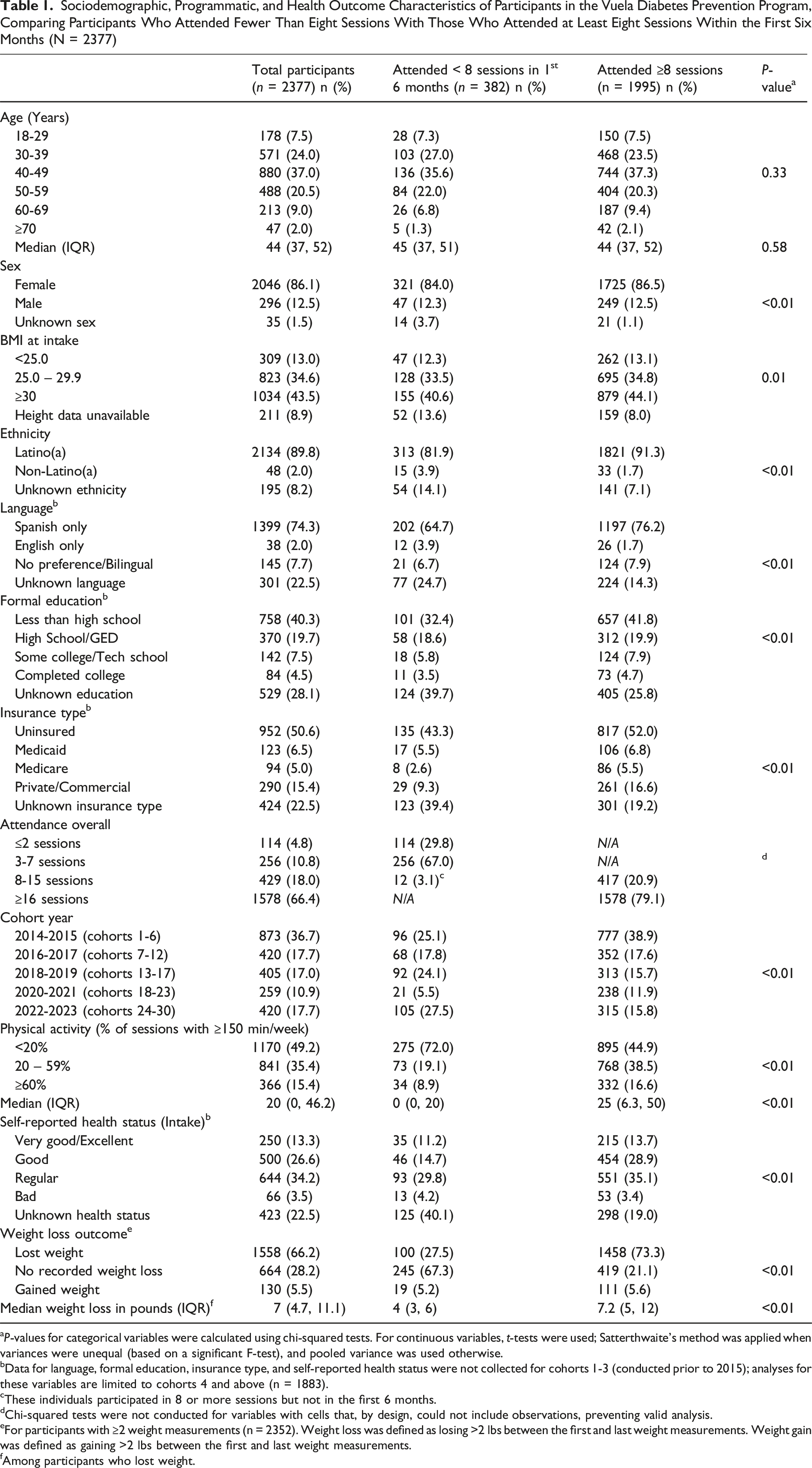
aP-values for categorical variables were calculated using chi-squared tests. For continuous variables, t-tests were used; Satterthwaite’s method was applied when variances were unequal (based on a significant F-test), and pooled variance was used otherwise.
bData for language, formal education, insurance type, and self-reported health status were not collected for cohorts 1-3 (conducted prior to 2015); analyses for these variables are limited to cohorts 4 and above (n = 1883).
cThese individuals participated in 8 or more sessions but not in the first 6 months.
dChi-squared tests were not conducted for variables with cells that, by design, could not include observations, preventing valid analysis.
eFor participants with ≥2 weight measurements (n = 2352). Weight loss was defined as losing >2 lbs between the first and last weight measurements. Weight gain was defined as gaining >2 lbs between the first and last weight measurements.
fAmong participants who lost weight.
The 2014-2015 cohorts, the 2016-2017 cohorts, and the 2022-2023 cohorts had the largest numbers of participants (n = 873, n = 420, and n = 420, respectively), while the 2020-2021 cohorts had the fewest participants (n = 259). Higher participation in 8 or more sessions was observed in earlier cohorts (P < 0.01). Among participants who attended 8 or more sessions, the median percentage of sessions with recommended physical activity reported was 25%, compared to a median of zero for those who attended fewer than 8 sessions (P < 0.01). More than a third of the enrolled participants (39.9%) reported their health status as good or very good/excellent at intake. Participants who reported better health status were significantly more likely to attend 8 or more sessions compared to those who reported “Regular” or “Bad” health status (P < 0.01). Almost 3 quarters of those who attended 8 or more sessions experienced weight loss between the first and the last measurements (P < 0.01) and median weight lost in this group was 7.2 lbs. Compared to 4 lbs. Among those who participated in fewer than 8 sessions.
Sociodemographic, Programmatic, and Health Outcome Characteristics of Participants in the Vuela Diabetes Prevention Program, Comparing Those Who did Not Lose ≥5% of Body Weight Between First and Last Measurement and Those Who Lost ≥5% of Body Weight (N = 2352)
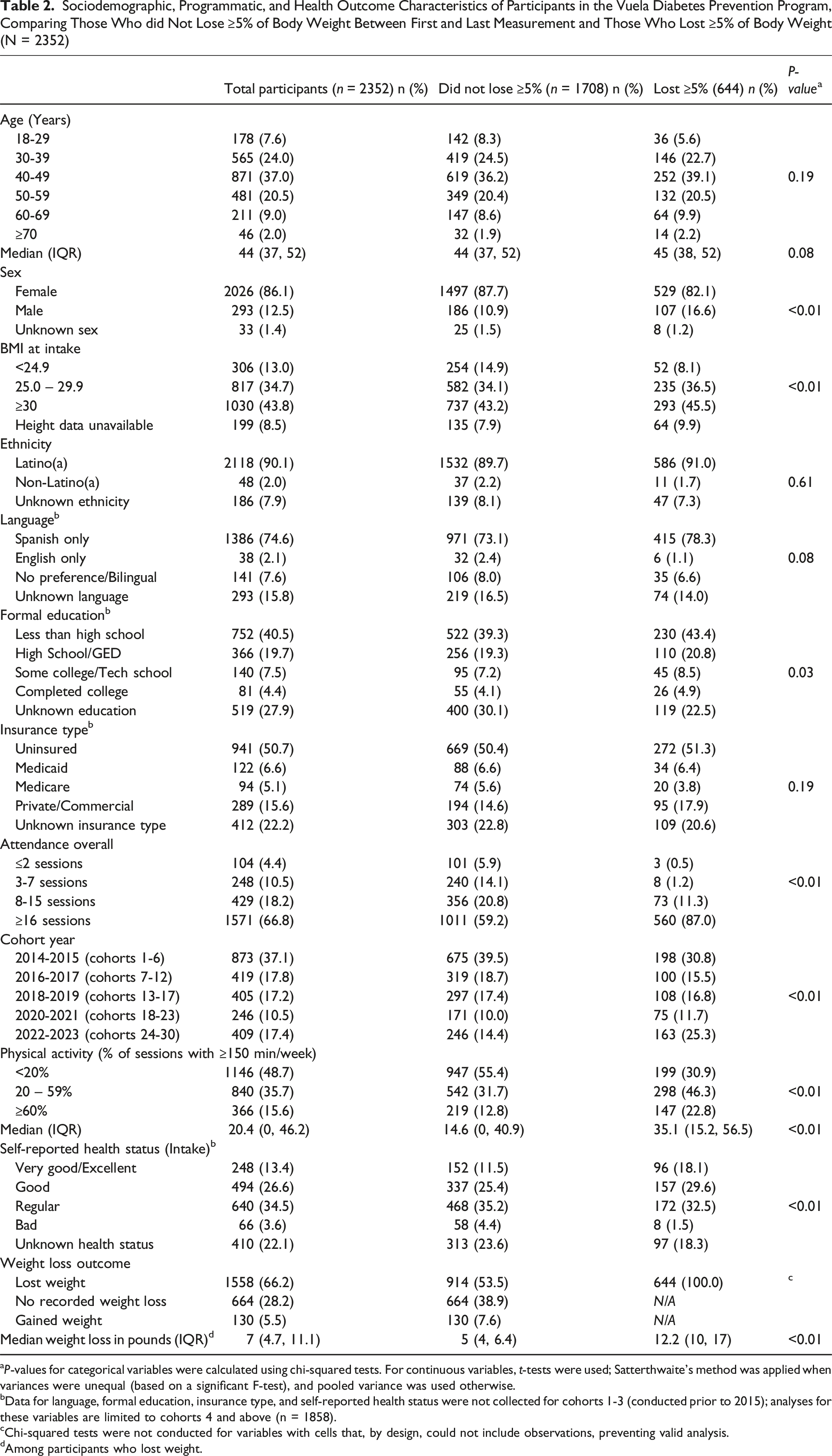
aP-values for categorical variables were calculated using chi-squared tests. For continuous variables, t-tests were used; Satterthwaite’s method was applied when variances were unequal (based on a significant F-test), and pooled variance was used otherwise.
bData for language, formal education, insurance type, and self-reported health status were not collected for cohorts 1-3 (conducted prior to 2015); analyses for these variables are limited to cohorts 4 and above (n = 1858).
cChi-squared tests were not conducted for variables with cells that, by design, could not include observations, preventing valid analysis.
dAmong participants who lost weight.
Among participants who participated in 8 or more sessions in the first 6 months, there were significant improvements in BMI classification over time, particularly reductions in obesity prevalence and increases in the proportion of individuals with normal BMI (Figure 1). Most notably, the proportion of patients with a BMI ≥30 decreased from 48.0% to 39.7%. Additionally, 34.3% of those who had a BMI < 25 at the end of the program (n = 388) had a BMI of ≥ 25 at the beginning. This aligns with the Bowker’s test of symmetry (P < 0.01), indicating the pattern of movement was asymmetric, with more participants moving to a lower rather than a higher BMI category. Transitions in BMI Category From Intake to Final Weight Measurement Among DPP Participants Who Attended at Least Eight Sessions in the First 6 months (n = 1831)a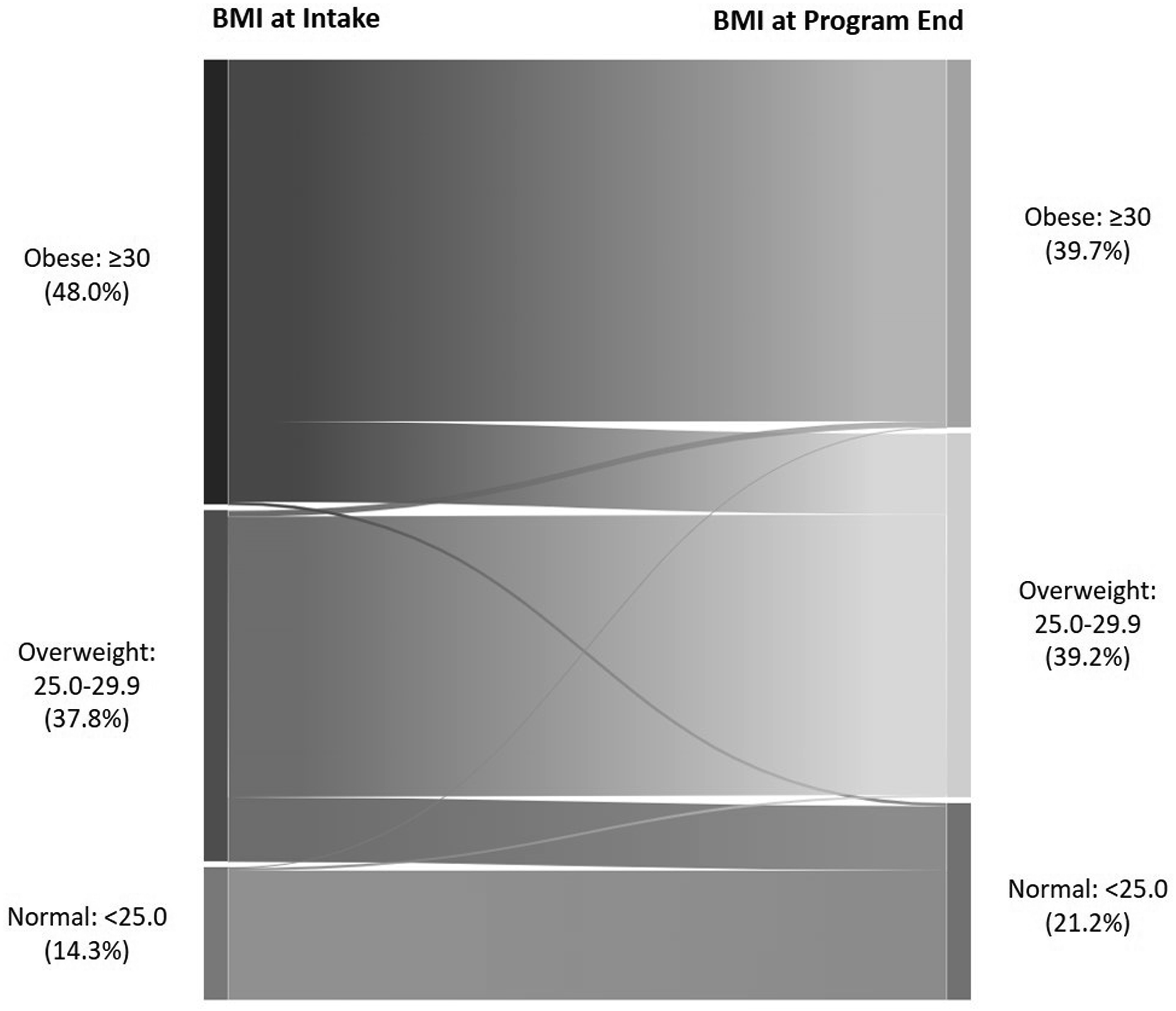
Among the participants who attended at least 8 sessions within the first 6 months and had at least 2 weights recorded (n = 1988), nearly a third (31.6%, n = 628) lost at least 5% of their body weight. Age, sex, BMI at intake, attendance, cohort year, physical activity, and self-reported health status at intake were all statistically significant in the bivariate model (Supplemental Table 1). These factors were included in the adjusted multivariable model (Figure 2). Adjusted Odds Ratios for ≥5% Body Weight Loss Across Covariates (n = 1162)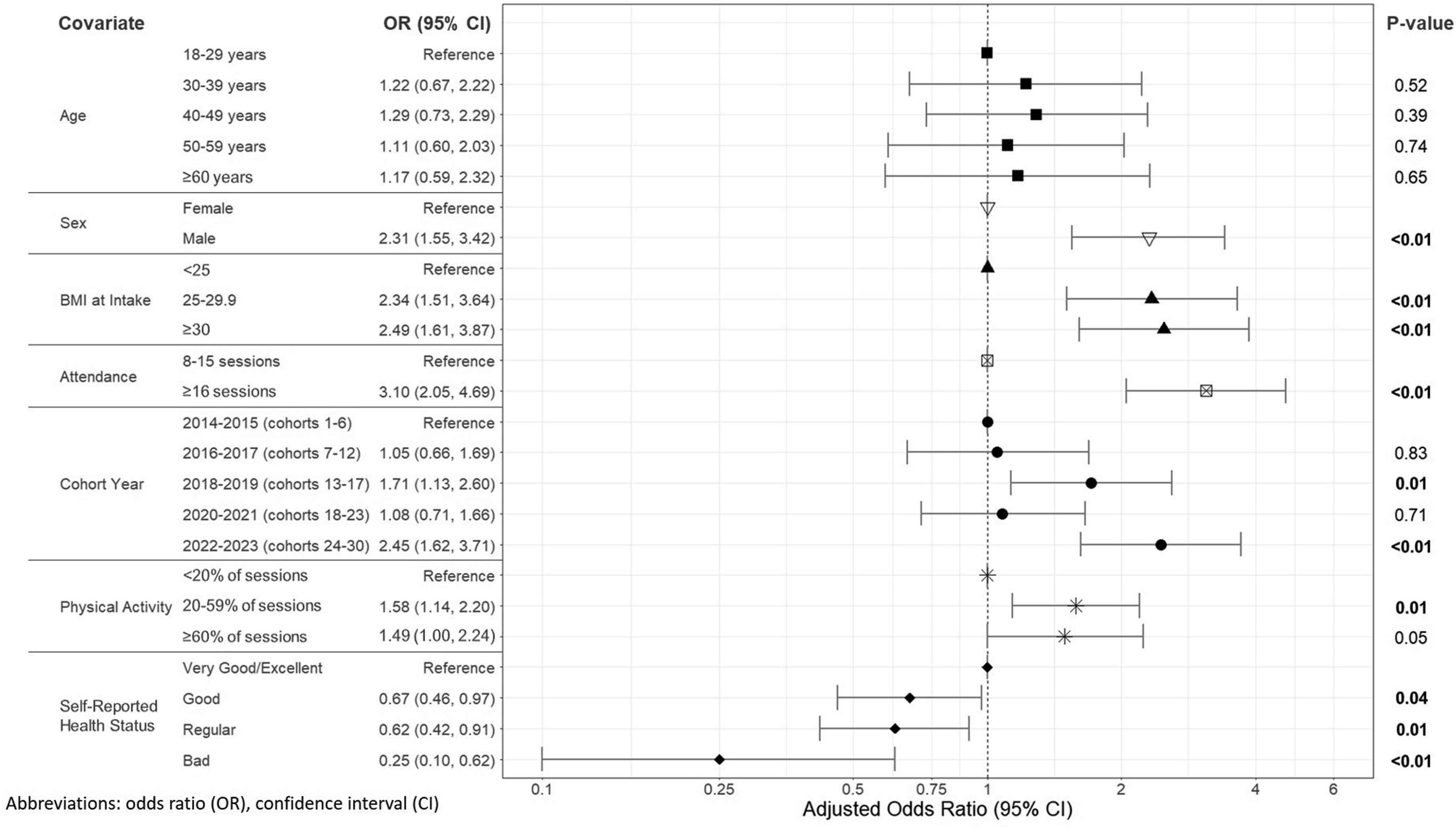
After adjustment, men were 2.3 times more likely than women to achieve a weight loss of 5% or more (95% CI: 1.55, 3.42; P < 0.01). Participants who attended 16 or more sessions were 3.1 times more likely to achieve 5% or greater weight loss compared to those who attended 8 to 15 sessions (95% CI: 2.05, 4.69; P < 0.01). Participants in the 2018-2019 and 2022-2023 cohorts were 1.7 times and 2.5 times more likely, respectively, to lose 5% or more body weight than those in the initial cohorts (95% CI: 1.13, 2.60; P = 0.01; 1.62, 3.71; P < 0.01). Compared to participants reporting recommended physical activity for less than 20% of sessions attended, those who reported this level of physical activity for 20-59% or ≥60% of sessions were around 1.5 times more likely to lose 5% or more body weight, though the association did not reach significance for the latter group (P = 0.05). Individuals who reported “Good”, “Regular”, and “Bad” health status at intake were 33%, 38%, and 75% less likely, respectively, to lose 5% or more weight compared to those with “Very Good” or “Excellent” health status (95% CI: 0.46, 0.97; P = 0.04; 0.42, 0.91; P = 0.01; 0.10, 0.62; P < 0.01). There were no significant differences in odds of weight loss by age group.
Discussion
The Vuela DPP is a successful community-based implementation of the CDC-recognized National DPP, tailored to low-income Spanish-speaking Latino(a) adults. Attendance rates were relatively high, and nearly one-third of participants reached 5% weight loss during the program. Few men participated, but men were more likely than women to achieve 5% weight loss. As expected, participants who attended more sessions were more likely to achieve 5% weight loss. Participants in later cohorts were more likely to achieve 5% weight loss than those in earlier cohorts, suggesting program improvement over time. Another novel finding was an association between self-reported health status, with participants reporting worse health status at intake being less likely to achieve 5% weight loss than participants reporting better health status.
These findings of relatively high rates of participation and achievement of 5% or more weight loss are in contrast to those from other studies showing that Latino(a) adults have low National DPP participation rates and low attainment of 5% weight loss.5,14 In an analysis of National DPP participants from the first 4 years of national implementation, only 10% identified as Hispanic/Latino(a), and 30.8% of Latino(a) participants achieved the weight loss goal of ≥5% compared to 43.2% of non-Hispanic White participants. 4 In a safety-net clinic based National DPP intervention that predominately included adults from low-income households, achievement of ≥5% weight loss was even lower at only 15.6% for Latino(a) participants compared to 26.1% among non-Hispanic White participants. 5 Low achievement of weight loss in that study was attributed to low program participation, with only 47% of enrolled Latino(a) adults vs 64% of enrolled non-Hispanic White adults attending one or more sessions. A cross-sectional state-wide evaluation of National DPP interventions also found that Latino(a), young, and uninsured participants were less likely to achieve 5% or more weight loss. 14
In previous studies, Latino(a) adults reported less physical activity than participants of other races/ethnicities and ethnic/racial weight loss differences were no longer evident after controlling for attendance and physical activity.5,14 In this evaluation, program attendance was also associated with the achievement of 5% weight loss, but there was a weaker association between physical activity and weight loss. It is possible that the weaker association between exercise and weight loss in this evaluation is due to inaccurately reported data (i.e. participants under/over-reporting exercise), or that participants in this program achieved weight loss primarily through dietary changes rather than increased physical activity.
In a previous observational study of National DPP participants, attainment of the recommended 150-minutes weekly physical activity goal was associated with total percent weight loss and achieving ≥5% weight loss at the end of the program, but was not associated with rate of weight loss per session attended. 25 Additionally, in the same study, participants who did not reach the weekly physical activity goal were 25% less likely to attend the next session and attended a lower percent of sessions overall, suggesting that reporting physical activity goals may impact weight loss success in the National DPP indirectly by affecting session attendance. Future studies exploring the association between physical activity goal reporting and subsequent session attendance are warranted. In addition, utilizing objective measures such as those obtained with activity monitoring tools are needed to better assess the impact of physical activity on weight loss in Latino(a) adults participating in the National DPP.
Nationally, men have been less likely to participate in the National DPP than women despite men’s higher prevalence of prediabetes. 1 A cross-site evaluation of National DPP programs reported 19.4% male representation among participants. 14 In a systematic review of culturally tailored programs for Latino(a) adults, most were studies including entirely or largely (>70%) females. 9 A clinic-based National DPP intervention in a Latino(a) cohort of adults reported 16% participation of men. 5 Participation of Latino men in this program was even lower than reported for other programs, with men representing only 13.5% of enrollees and 12.6% of those attending one or more and 8 or more sessions. The drop-off between men enrolling and men attending suggests even men who are interested in participating face barriers to attendance. However, male participants who attended ≥8 sessions were greater than 2 times more likely to achieve 5% weight loss than female participants. Higher weight loss among male compared to female participants in the National DPP has been reported in other studies, highlighting the potential impact of engaging more men in the program.4,14
Possible barriers to participation for men include lack of time due to work outside the home, low sense of belonging due to few male participants, and lack of connection to women National DPP coaches. These barriers might be addressed by increasing access to National DPP in or near work locations, developing programs focused on men, and increasing the number of men certified to serve as National DPP coaches. A translation of the National DPP to engage men in disadvantaged neighborhoods of New York City used community-based participatory methods to develop and test a men-led, men only, National DPP. 26 Though once participants were enrolled, most completed the program and reported they were highly satisfied, recruitment remained a significant challenge and was lower than expected. More studies are needed to identify and disseminate successful approaches to increase male engagement in the National DPP.
We found an association between self-reported health status and achievement of 5% or more weight loss, which remained significant after controlling for attendance. Specifically, individuals reporting worse health status at the beginning of the program were less likely to achieve 5% weight loss than those reporting better health status. These findings could reflect lower self-efficacy for change among individuals reporting “Bad” or “Regular” health status. Further research is needed to understand this association.
Participants in more recent cohorts were more likely to achieve 5% weight loss than participants in the program’s initial cohorts, suggesting improvements in the program over time. Higher rates of weight loss were not observed for the cohorts taking place between 2020 and 2021, which is almost certainly due to pauses in programming and the transition to virtual program delivery during the COVID-19 pandemic. Program adaptations made over time, such as additional classes offered and cultural adaptations of the approved curriculum to make healthy dietary choices and habits more accessible to Latino(a) participants, may explain the observed improvements in weight loss outcomes.
This evaluation was subject to multiple limitations due to its retrospective design and real-world setting without a control group. A large majority of participants were women. Physical activity was self-reported, which may have resulted in over or underestimates or inaccurate reporting. The program was delivered by Latino(a) community health workers and mostly in Spanish, and findings may not be generalizable to implementation by other Lifestyle Coaches, in other languages, or with the use of interpretation services. This evaluation did not explore participant perceptions or experiences that might explain how factors such as self-reported health status influenced weight loss during program participation.
Another key limitation of this study is the extent of missing data for certain variables. Although early cohorts in which these variables were not collected were excluded, the remaining analytic sample still had 22.5%-28.1% missingness. The reasons for this missingness are not fully understood, limiting the feasibility of applying multiple imputation. Missing responses were retained in descriptive analyses for transparency but excluded from the multivariable regression to allow for a complete case analysis. Accordingly, estimates involving these variables should be interpreted with caution due to the potential for bias.
This evaluation found that community-based, culturally adapted National DPP interventions can be effective in decreasing the risk of diabetes among Spanish-speaking adults by facilitating weight loss. Additional research is needed on methods to increase participation among men and to better understand associations between self-reported health status and achievement of weight loss. Future efforts should also focus on the dissemination of successful programs to other geographical regions and other high-risk communities. Low effectiveness of the National Diabetes Prevention Program (DPP) lifestyle intervention for Latino(a) adult participants has been attributed to low attendance rates and low physical activity in this population. Evaluation of a large community-based National DPP for low-income, Spanish-speaking Latino(a) adults showed high attendance and weight loss effectiveness similar to that of all National DPP participants. Dissemination of community-based, culturally adapted National DPP programs can be an effective strategy for decreasing diabetes disparities affecting Latino(a) adults in the US.So What?
What is Already Known on this Topic?
What does the Article Add?
What are the Implications for Health Promotion Practice or Research?
Supplemental Material
Supplemental Material - Effectiveness of a Latino(a) Community Health Worker Led National Diabetes Prevention Program
Supplemental Material for Effectiveness of a Latino(a) Community Health Worker Led National Diabetes Prevention Program by Nancy Wittmer, Abigail Steiner, Karen Uvina, Jayna DeRoeck, Amy Stein, Diana Pineda, Rocio I. Pereira, MD in American Journal of Health Promotion
Footnotes
Acknowledgments
We thank the Vuela for Health promotoras team, without whom this work would not have been possible. Additionally, the authors used ChatGPT (OpenAI) to assist with grammar and phrasing. All edits were reviewed and approved by the authors. The tool did not contribute to the study’s design, analysis, or interpretation.
Ethical Considerations
This program evaluation received IRB Exemption by the Colorado Multiple Institutional Review Board (COMIRB #16-0095).
Consent to Participate
All participants provided written informed consent prior to participation and screening. Program information and consent were provided in Spanish or English depending on the preferred language of the participant.
Author Contributions
Nancy Wittmer drafted the initial manuscript, analyzed and interpreted data, and critically reviewed and revised the manuscript.
Abigail Steiner analyzed and interpreted data and critically reviewed and revised the manuscript.
Karen Uvina performed data collection and critically reviewed and revised the manuscript.
Jayna DeRoeck performed data collection and critically reviewed and revised the manuscript.
Amy Stein analyzed and interpreted data and critically reviewed and revised the manuscript.
Diana Pineda provided subject matter support and critically reviewed and revised the manuscript.
Rocio I. Pereira conceived the work, provided subject matter support, drafted the initial manuscript, and critically reviewed and revised the manuscript.
Funding
The Vuela Diabetes Prevention Program intervention was funded by the Colorado Department of Public Health and Environment (CDPHE) Cancer, Cardiovascular and Pulmonary Disease (CCPD) Grant Program.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated during and/or analyzed during the current evaluation are available from the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
