Abstract
In Victoria, Australia, children who are reported to authorities to have experienced very recent sexual assault routinely undergo a forensic medical examination and receive psychosocial care. There is very little known about how children and their families experience this process and whether current practices are meeting their needs. This study seeks to understand these experiences by undertaking a thematic analysis of in-depth interviews with 10 children/young people (aged between 4 and 16) and 8 mothers (n = 18). The study draws on constructivist grounded theory methodology and incorporates the contextual-embedded perspective of the clinician/researcher. The study identified three stages participants navigated in the hours following the assault: (a) reaching out for help, (b) hospital processes and procedures, and (c) discharge. Nested within these stages, five key themes emerged: confusion, distress, and minimization when reporting; valuing a caring presence; feeling exposed, vulnerable, and ashamed; being lost in space and time; and going home alone. The need for a sensitive, trauma-informed, accessible, and consistent response to acute sexual assault is discussed; one that acknowledges the experiences and centralizes the priorities and psychosocial needs of the child and their family.
Keywords
Introduction
The primary researcher’s first experience as a social worker in responding to a young person in the hours following a sexual assault, back in 2009, began with being woken by a blaring pager at 2 a.m. She attended the hospital where she worked, turned on the lights in the “Crisis Care Suite” and unlocked the door for two detectives, the forensic pediatrician, and an otherwise unaccompanied 16-year-old young woman. In the hours prior, according to the detectives, she had been raped after being dragged into a public toilet block while she was walking home from school. Despite the hour (by this stage it was close to 3 a.m.), she was still in the school uniform she had been wearing at the time of the assault. The researcher’s only interaction with the pediatrician was being told that she was not required in the examination room, but could she find some clean clothes, please? She made tea for the police. After waiting for about 2 hours, the doctor and the young woman (now clad in an ill-fitting tracksuit) walked by. The doctor said goodbye to her, and she left with the police, her school uniform now in a large brown paper bag tucked under the Detective’s arm. The doctor left and the researcher turned off the lights, locked the door, and went home, wondering, frankly, why she had been there at all. While the initial service response to young victims of sexual assault has changed somewhat in the years since that night, that experience first sparked the questions being asked in this study: What is this like for children, young people, their parents, and carers? How do they experience the professionals they meet and, moreover, how can the service system best respond in the hours after the discovery of the sexual assault of a child?
Locating the Current Study
In metropolitan Melbourne, within the state of Victoria, when a child or young person experiences sexual assault and it is reported to the police within hours or days of the most recent incident, it is routine that they attend one of two large metropolitan hospitals for a forensic medical examination (FME). The purpose of the FME is the collection of any biological material from the victim that may assist the police in the identification and prosecution of an offender. This examination process and the support and assessment that goes along with it is referred to as “Crisis Care.” The term “Crisis Care” has a slightly different meaning in the adult sexual assault sector, but for the purposes of this study, Crisis Care includes an FME. Crisis Care is usually the first point of contact with local services following this kind of traumatic event. The Figure 1 below pictorializes the process. SOCIT refers to the specialist Sexual Offenses & Child Abuse Investigation Team of Victoria Police. The “CCU” refers to the Crisis Care Unit where the FME takes place.
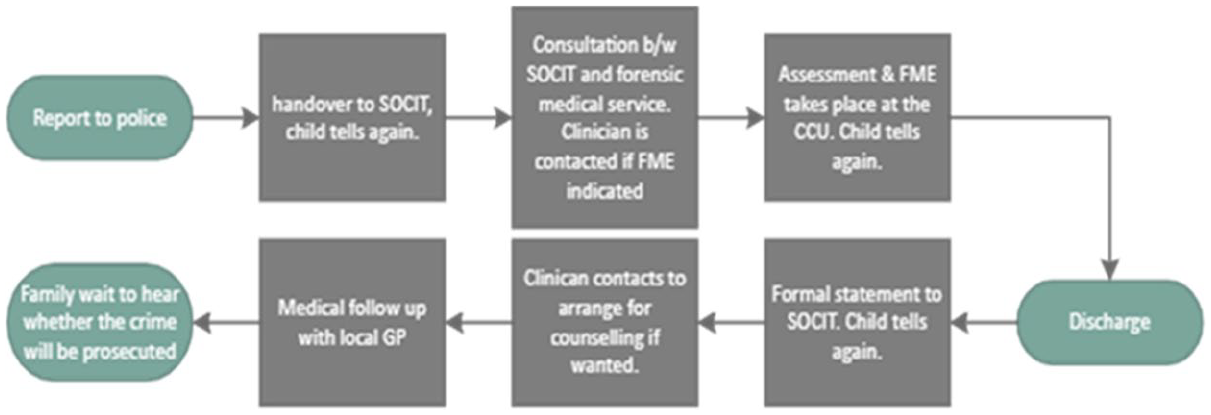
The Process for children after reporting to police.
The Trauma of Sexual Assault
Some children and young people who present for Crisis Care have good attachment relationships (Bowlby, 1969), characterized by supportive families, have not experienced any significant prior adverse life event and are likely to recover without the need for longer-term psychological and social intervention (LaBrocque et al., 2010). However, it is well established that sexual assault can have significant physical, emotional, and psychological short and long-term effects on children and young people (Carrion & Steiner, 2000; Harrison et al., 1997; Herrera & McCloskey, 2003; Rothbaum, et al., 1992).
For most children and young people who receive Crisis Care, abuse occurs within a context that includes one or several compounding vulnerabilities: transgenerational abuse; parental mental health concerns and/or alcohol and other drug misuse; exposure to family and/or community violence; poverty; disability; a traumatic refugee experience; racism; homophobia and transphobia; child protection involvement or living in out-of-home care (Finkelhor et al., 2007; Ford, 2021). Also, the likelihood is that they have experienced abuse at the hands of a loved and trusted family member or friend (Australian Bureau of Statistics, 2021). Crisis Care is not like any other visit to an Emergency Department. Context, history, culture, and connections are all brought into the room with the child.
Intervening Early
Crisis Care is a potentially important intervention, not only because it involves the collection of biological evidence to assist the prosecution of a crime, but also due to the opportunity it affords to decrease the likelihood of the child experiencing longer-term post-traumatic disorders (Berkowitz et al., 2011; Denson et al., 2007) as well as reducing distress after an assault; even by those children and young people who do not go on to develop posttraumatic disorders (Hahn et al., 2016). Crisis Care presents an opportunity to assess which children and families may require further supports, based on their history, as well as current circumstances. It provides an opportunity to alleviate acute stress responses and equip parents and carers to respond to emerging trauma symptoms.
A Trauma Responsive Service System
This assessment and provision of care concords with the notion that health and community services need to be “trauma responsive” or previously, “trauma-informed (Ball et al., 2021).” Trauma-informed services seek to build meaningful partnerships between children and young people, their caregivers, and professionals at an individual and organizational level. They address the intersections of trauma with culture and language, context, gender, and location. They acknowledge the compounding impact of structural inequity and are responsive to the unique needs of diverse communities (National Child Traumatic Stress Network [NCTSN], 2022). In the Crisis Care context, it should seek to not replicate or perpetuate the symptoms or outcomes of acute psychological trauma.
While there is growing activity in exploring the value of trauma-informed care, there is a dearth of research that seeks to understand children and young people’s experience in this context (Quadara & Hunter, 2016). The development of Multi-Disciplinary Centers (MDCs)—a “one stop shop” that includes police, child protection services, and sexual assault support services in one building is an attempt at integrated service response (Victoria Police, n.d.). Like Child Advocacy Centers in the United States, and centers based on the Barnahus model in the United Kingdom and Europe (Cross et al., 2008; Johansson et al., 2017; Shaffer et al., 2018; Williams & Kisiel, 2016), MDCs aim to minimize further trauma to victim/survivors. However, children and young people are not currently able to obtain an FME at an MDC and after-hours crisis appointments with clinicians are likewise not available.
As a clinician, service manager, and leader in the provision of the psychosocial aspects of responding to child sexual assault for over 25 years, in the first author’s experience, while efforts have been made to support families in this circumstance, our youngest clients and their families do not always receive a timely, accessible, consistent, and trauma-informed service response. This research attempts to clarify the validity of this assertion as well as understand and learn from families’ experiences with the service system in the immediate hours after a sexual assault, with the aim of improving practice and ensuring children and young people and their carers receive care that is informed by them, for them.
Methodology
Constructivist Grounded Theory and Embedded Ethnography
The voices and experiences of children, young people, and their families are both important and powerful in understanding the impact of service system interventions (Caldwell et al., 2019). The methodology of this study is based on the constructivist grounded theory (CGT) incorporating an embedded researcher/clinician perspective. CGT differs from the earlier “versions” of grounded theory developed by Glaser (1978), Glaser and Strauss (1967), and later, Strauss and Corbin (1998) in that it positions the researcher as a co-constructor of data with participants (Charmaz, 2014). Incorporating the embedded researcher/clinician takes advantage of this positioning to enhance the co-construction. These approaches together resonate strongly with a focus on privileging child and family voice and how participants and the researcher together construct the findings of the research through their perspectives and interaction. One of the key strengths of CGT is in its flexibility. This method can be used to explore meaning and action in various contexts without necessarily generating a comprehensive theory. The study is not seeking to generate a theory, rather to draw on CGT for its ability to gain an in-depth understanding of the meaning and action that is articulated by people with a shared experience. By utilizing CGT, researchers can capture the complexity of lived experience, explore the processes through which individuals construct meaning, and examine the actions that result from these meanings. This focus is particularly valuable for developing a nuanced understanding of how individuals interpret and respond to their circumstances—and this is especially important when the research focus is on a traumatizing event (Charmaz, 2015).
Given the researcher has been clinically “embedded” in this work for many years, incorporating an embedded ethnographic methodology (Lewis & Russell, 2011) recognizes the value of the researcher/clinician’s perspective as importantly situated contextual knowledge that can also offer of a sense of “thick description” that describes a systemic context for people’s actions and intentions (Ponterotto, 2006). This positioning emerges from the requirement to “immerse him or herself fully in the chosen field of study, learning the day-to-day and extraordinary stuff of social and cultural life by ‘being there,’ Lewis & Russell, 2011 p. 400).”
Together, these two methodologies provide a framework whereby the researcher can be both curious about the Crisis Care phenomenon and its impact on the child and their carers; by allowing questions to be generated from that curiosity, rather than impose preconceived notions of the experience of Crisis Care intervention; as well as reflexively (Buscatto, 2016) draw upon the clinician’s positioning to add local context and systemic insight.
Data Collection
Ethics approval was sought and granted from both the hospital where participants received care and the university affiliated with the researchers.
Semi-structured, in-depth interviews were conducted to capture the experiences and perspectives of the children and young people (aged between 4 and 16) and their parents/carers. The wide age range was a deliberate step by the researchers to capture as many voices as possible. Interviews were conducted either individually or as family dyads/triads or both, as preferred by the participants. Eighteen interviews in total were conducted. Participants were asked, in a developmentally appropriate manner and after a period of “engagement” (e.g., talking about school or hobbies or drawing pictures) to give a narrative account of their experiences when they came to the hospital. Very young children were first asked whether they remembered coming to hospital with their carer and the police, before being asked to talk about what they remembered about the experience.
Navigating the dual roles of researcher and clinician has distinct advantages when speaking with such a vulnerable population. The “embedded ethnographic” methodology was employed precisely due to the interplay between each role. Due to the clinician researcher’s expertise in providing assessment and psychotherapy to children and young people who have experienced sexual assault, she was able to conduct the interviews so that they did not overwhelm the participants and allowed her to speak and listen with extensive knowledge and understanding of the processes being discussed. If any participant was to become overwhelmed, the clinician researcher would be able to support them to manage their distress. Also, the services involved in the research were able to provide immediate crisis sessions to any family who required or requested them.
All participants were keen to share their experiences so that they might be used to improve service provision to other families. Any specific complaints about the care they received were with the consent of the participant, fed back to the providers involved. All participants were given clear pathways if they wished to make a complaint themselves.
Participants
This paper reports on the findings from interviews with children and their parent and is a key section of a larger study that includes interviews with Crisis Care clinicians and pediatricians. The identity of the perpetrator ranged from family member, peer, formal carer, and an online contact. Two assaults were one-off rapes. The rest of the children/young people had experienced on-going sexual abuse. Seven of the children/young people identified as female, two as male and one as nonbinary. They were all born in Australia.
While all carers, guardians, and family members were eligible to participate, all eight parents interviewed were the biological mother of the child/young participant and were the parent who accompanied their child for Crisis Care. One parent identified as being of a refugee background and Arabic was her first language. She was offered an interpreter but declined, being fluent in English. One other parent reported she was born in Türkiye and emigrated to Australia as a child. The rest of the participants identified as being of Australian or western European descent and English was their first language. None of the participants identified as being of Aboriginal or Torres Strait Islander heritage.
Recruitment
The Crisis Care Unit where participants were recruited was located within a large metropolitan hospital that provides forensic medical services to children and young people. Children and young people (aged 4–17) along with the parent/carer that accompanied them during Crisis Care service provision, over the 6-month study period, were eligible to participate. While working within the service, the researcher was independent of the clinical staff who provided or would provide direct care to the family. Written information about the study was provided to families upon discharge from hospital, along with other written materials about responses to trauma, and available supports. As part of the formal clinical follow-up in the days following their presentation to hospital, families received a phone call from the clinician, checking on their well-being. Clinicians then informed families again about the study.
Children, young people, or their parents/carers who were assessed by their Crisis Care clinician or other mental healthcare professional as at risk of suicide or self-harm or was requiring hospitalization for physical or psychological reasons because of the assault were excluded from the study.
If consent was gained during this first call, the study was explained again in a second phone call from the clinician/researcher. Again, if the clinician/researcher assessed a child, young person, or parent to be at risk, they were excluded from the study and follow-up supports arranged instead. If consent was gained the second time, a plain language statement and consent form was sent to the potential participants and an interview time made.
Data Analysis
Interview transcripts and field notes were analyzed thematically, utilizing NVivo software. Following a CGT approach, data analysis entailed: a line-by-line coding of the transcripts with detailed, descriptive codes; key themes and their relationship with the participants narratives were identified; preliminary codes were established; larger thematic constructs were identified. These constructs were scrutinized, and their content carefully read with the research questions in mind. Cross-case comparisons (comparisons between participants) and within-case comparisons (analysis of the content of each individual interview) were applied to gain an in-depth understanding of the coded data and develop the final set of themes.
Along with these narrative accounts, a picture of the local and wider response context was drawn from the clinician/researcher’s embedded knowledge and experience of the professional culture and practices that inform the response/intervention. Memo writing (Charmaz, 2014) took place throughout the process. Finally, the research team came together to discuss conclusions. All interpretations were shared among the team and open for discussion if they felt the interpretations reflected any personal biases as opposed to the participant’s experience.
Findings
In this section, the findings will be structured to align with the narrative accounts given by the participants. While each family’s experience has distinct elements, the processes consistent among participants included reaching out for help (stage 1), entering Crisis Care and their experiences of its requisite processes and procedures (stage 2), and their reflections on what happened after discharge from hospital (stage 3). Nested within these stages are the five emergent themes: Feeling confused, distressed and minimized when reporting; valuing a caring presence; feeling exposed, vulnerable and ashamed; being lost in space and time; going home alone.
Each theme is presented incorporating the words of the participants, the clinician/researcher and then discussed. As a clinician “wholly immersed” in the field of study (Lewis & Russell, 2011, p. 398), memos (Charmaz, 2014) are included within the presentation of the findings.
All participants and individuals referenced in the interviews have been given pseudonyms.
Stage 1: Reaching Out for Help
Of note, even though the first interview question asked about their experience in hospital, all participants began their narrative with a description of reporting to the police.
Feeling Confused, Distressed, and Minimized When Reporting
When a family reaches out for help following the discovery of sexual assault, often their first step is to go to a police station. The decision as to whether an FME will take place is the pediatrician’s decision, made after the police contacts the state-wide forensic medical service by phone. The doctor will not speak directly to the family at this point. This process can have a direct impact on families. For example, Samira (parent) was unclear as to why, at first, it appeared a medical examination would not be taking place and was distressed by this: the reassurance that she believed would come with the exam was the sole reason she reported the assault of her small child to the police.
“I said, look, she hasn’t showered. We still have a chance to get some evidence. I thought if there is any chance they could find something, we should try. At least, I wanted to know what had actually happened to my daughter. But she (the police) said, ‘oh well the doctor said no, we can’t do anything, sorry. . .no medical.’” (Samira, parent)
This examination is for forensic purposes, but of course, a valuable part of the process is the reassurance it offers to young patients and their parents and is a good opportunity for questions. If a FME does not take place in the aftermath of a sexual assault (if there is likely to be little forensic biological material still present) this opportunity is lost.
Another parent, Kathy, was confused and frustrated about being repeatedly told to wait when she felt an urgent response should have occurred.
“After we reported to police, I took my child to our doctor’s clinic, and I text the police saying, ‘I’m just here at the clinic, because I want her seen’ and she said, ‘Look don’t worry about it, go home . . .we’ll call you about taking her to hospital.’ But I wanted something there and then because to me. . . I was just. . . The time was ticking, and I just didn’t want to leave it any longer. . .So then I thought, well okay, I’ll just have to go home and wait. . .And then we didn’t get in (to hospital) until the following day, which left it I think closer to 40 hours or something like that. And it was just too much time to have to wait, to have to let children wait. And I got told I was going to get a call first thing in the morning. And so, I waited, waited, waited and I didn’t get that call. So, I then had to follow up.” (Kathy, parent)
Some of this frustration included a sense that police were minimizing the assault’s seriousness or a sense that they (the participants) were wasting police time or that of being in trouble, feeling like the “perpetrator,” which several participants reported.
“I felt like he (the police) was just trying to dismiss the whole situation because he didn’t want to fill out any paperwork and he just thought, ‘you get what you get,’ and just let it go. It was awful.” (Gemma, young person)
Memo: From my experience of supporting families, this initial stage can easily create a sense of confusion, of having done the wrong thing or of being in trouble; and this might also speak to the issue of an overall lack of clarity and consistency to the reporting process. Families often reported speaking to different people, in different places, both in person, and over the phone. I could also see how it was easy for them to get the impression that no one was really “driving” the response of the system in a way that makes them feel contained and safe. And from my clinical experience, in the crucial initial response period, it is important to give care responses that recognize the impacts of trauma and support recovery. This recognition and support are also important for professionals if they are to gain the trust of victims to collect clear coherent and consistent information that facilitates the justice response.
Some of the participants highlighted the police and SOCIT detectives’ response appeared to them to be uninvolved and passive; by not introducing themselves or being dismissive, as well as the previously discussed procedures where the parents did not feel that the police were doing enough to collect evidence.
“When I got the call that my son had been assaulted, I just went down there, I was in disbelief. . . This detective in charge, what’s her name. . .Amber something. I understand it’s her job, but the way she comes across is a little bit clinical, methodical. I didn’t feel that she should be all soft, but . . .well, she’s just said outright, ‘He’s been raped.’ It wasn’t really said sensitively. . . because if someone doesn’t show that emotion, it concerns me how much effort there is going into this case. You know?” (Margaret, parent).
Other participants felt that the police lack training to deal with the victims, explaining that the police “just don’t seem to understand about trauma and what’s needed” (Kathy, parent). Samira noted that, “I come from a different background, I don’t know what is happening and I don’t know what to ask. I’m not very trusting of police.” Similarly, another mother raised concerns that the police officers did not acknowledge her children’s autism and lacked an understanding of its meaning, which would enable them to deal with her children accordingly.
Stage 2: Entering Crisis Care/Processes and Procedures
Crisis Care, and the examination itself, is one of the earliest parts of the reporting process for families, following within hours of making the first report and is a highly stressful stage. The need for sensitive approaches, clear and situationally relevant information, premised on a sense of consideration of the clients’ experience, which can play a significant role in how the young person and their parent cope with the entire process.
One of the most confronting aspects of the process for the child and their parent was the examination process itself, and how this was experienced was an important factor in shaping the young people and their families’ overall perception of the crisis intervention. The impact of this was by far the most discussed theme.
Valuing a Caring Presence
When first asked about their experience of entering the Crisis Care/examination process, most families initially described their appreciation of the staff’s (both doctors and clinicians) kindness and compassion. Kaye (parent) felt that in communicating with her the clinician involved in her child’s examination “had this incredible demeanor and heart about her.” She acknowledged that they helped her and her child “understand what was going to happen.” Several other participants also saw staff members as “genuinely nice people,” and that they cared and extended their help beyond what they thought was their role. This included staff that “helped me. . . calm down (Dylan, young person),” as well as being good listeners and not rushing the young person. Other participants saw staff going “above and beyond” to make the young person feel comfortable, helped them with their anxiety and “panic attacks,” and generally “made us feel relaxed” (Layla, young person).
It was also noted by participants that some staff also offered the children and young people food, new clothes, and that a clinician lent a young person a phone charger. They “made us feel it was personalized; individuals, unique (Pauline parent).” Taylor (young person) was given a teddy bear by one of the clinicians. She explained that: “I’m a very sentimental person and although it kind of does seem childish. . . it was that emotional support that I needed.”
Memo: As a clinician, I have often made “chickens” out of rubber gloves, made shadow puppets on the ceiling above children during their examination, held the hands of children, young people, parents, and friends during the examination. While such diversions are commonplace during other medical procedures, they are an important part of the, what seems often like unacknowledged or underrated, provision of care.
Feeling Exposed, Vulnerable, and Ashamed
For many participants however, at crucial times, information was not delivered clearly or sensitively, particularly during the examination procedure. Consistently, as the families’ stories unfolded, they revealed more about feeling overwhelmed and finding the experience hard. This was often a result of a lack of sensitivity to their trauma experience, not being clearly and adequately informed about what was going to happen or overwhelmed with information. Several young participants discussed feeling “traumatized,” “intimidated,” and “ashamed” during the examination procedure. Fiona (young person) stated she felt, “really, really, really nervous and scared.”
Both Sasha (aged 7) and her mother Tania described how “the examination lady” was impatient and did the procedure “roughly,” without trying to comfort her young patient: Sasha: She kept saying, “Sit still,” and it was hard for me to just sit still. Then she just, when she did the examination, she. . . (fidgets & appears uncomfortable) Tania: She did it a bit roughly. Sasha: I was crying on the bed, and it hurt me. . . And she just looked at me. Because she’s seen me crying and she just looked at me. She didn’t say anything. . .The other lady (the clinician), she was staring at me a lot.
Gemma (young person) commented that in addition to the examination causing her pain, to the point where she, according to her mother, was “literally crying during the whole thing,” she reported that the clinician was not nice to her, did not respect her privacy, and “didn’t turn around at all,” making the experience even more “awkward.”
Ava (4) told the researcher clinician that she “had a swab in (her) vagina,” unprompted and without context, before being asked anything about her experience in Crisis Care. They interpreted the remark to mean that this element of the process was very much in front of mind for the little girl.
As Kathy (parent) reflected, the experience was overwhelming “because I wasn’t getting a lot of information” and “I didn’t really know what the next step was.” Others thought the roles of some of the professionals were unclear. For example, the pediatrician did not explain what they were doing, what they were writing down in their notes, or what the examination entailed. This was particularly difficult for Tania (parent). “Nothing was explained to me,” and “no one tells me what is actually happening. Not understanding the system makes it hard.”
One parent spoke about the process of needing to hand over clothing to the police at the hospital: “. . .If I’d known that they were going to take his clothes, because I’m not thinking. . . I could’ve. . . so that he felt warm, comforted, maybe, in his own clothes. . .We didn’t have shoes to go walk home in. He had to go out barefoot. He’s just a bit . . .he doesn’t want people looking at him, to wonder why he is walking out of this place without any shoes on. This is a detail, but just to strip someone of their clothes and how that feels to walk out barefoot. . . It’s more of a metaphor. You’re walking out with bare feet, like someone’s taken something fundamental from you. . .” (Margaret, parent)
Memo: There is a supply of clothing kept in the Crisis Care Unit. However, storage space is at a premium (the room is about 3 msq with one small storage cupboard) and there isn’t space for the clothing required (let alone shoes) for every patient of every size, who may be a newborn, a 12-year-old girl, or 17-year-old young man. The floor is already crowded with plastic tubs full of clothing. There are no windows, and it is not soundproof.
Young people also spoke about their concerns for their parents, feeling that they should have been better supported through the process and beyond.
“And it’s not just me that’s going through this, it’s my mum. And I know she just wants to get me the emotional support and I completely agree with that. I 100% need it and need it really quickly but I feel like she should be able to have that support too. None of it was offered to her or anything like that.” (Layla, young person)
Being Lost in Space and Time
Several participants described the Crisis Care spaces as confusing and chaotic, and the procedure as poorly paced. Some reported that everything took too long, while for others the procedures felt rushed, which further contributed to their distress. It was also reported that upon arriving at the hospital, “no one knew where we were supposed to go, (. . .) what was supposed to happen (. . .) or which people that we were supposed to meet (Linda, Parent).” As Kathy also noted, “I had to tell four different people what had happened and every time they say, ‘oh that’s not for us, go here instead.’” Children and young people already tell their story two or three times during this process. These comments indicate they need to explain to strangers yet again, the purpose of their visit. Having to repeat the story again to the pediatrician was “very, very, very stressful” for Fiona (young person). She felt that this further contributed to her trauma experience. Like the initial reporting to the police and the police attitude toward the young person and their family, Layla (young person) commented that when having to repeat her story: “I felt like I was the one in trouble.” The feeling of being in trouble was further exacerbated when the police officer “got a bit mad at me” for trying to call her boyfriend when she was about to be examined.
Several parents mentioned expensive parking and a lack of clear signposting to get to the facility. In addition, what was seen as a poorly designed and unwelcoming space were discussed, with the participants describing the facilities as a “small” (Tania, parent) and “a bit scary” (Ava, child) place that feels “unwelcoming” and “unsafe” (Dylan, young person).
“I mean, it was, like, frightening. You just have all these. . . You’re just walking down a really long corridor, all these white, you know just white ceilings and walls. . . And it was kind of just like a bit. . . Yeah, not welcoming, not nice and hidden away sort of.” (Felicity, young person)
Memo: The Crisis Care Suite where the intervention takes place is not on any of the way-finding maps and is not signposted besides one sign within the Emergency Department, inaccessible to the public. Due to the need for the Suite to be kept forensically clean, there are no pictures on the walls and no soft furnishing to soften the space.
The participant families also reported a range of different perceptions about their experience concerning the time it took to go through the process; some felt it was rushed, others thought it was sufficient, while others found the process interminable.
Memo: A Crisis Care Intervention can take up to 4 hr; sometimes longer if other concerns are uncovered during the process. For example, photographs may need to be taken of injuries, a consultation with colleagues from mental health may be necessary if there are concerns about a young person’s presentation; calls to After Hours Child Protection, Family Violence Services, including Refuges, Out of Home care providers, or the guardians of unaccompanied young people may prolong the process. Of course, these are not the first 4 hr or the last. They don’t include the time taken at the police station prior or if the child or young person first presents to a hospital or clinic that don’t provide forensic services and they don’t include the time following: waiting to make a video and audio recorded evidence—the official statement that can be used in court; waiting for counseling services or waiting for the police and Office of Public Prosecutions to decide whether there is a case to be prosecuted.
Stage 3: Discharge
Going Home Alone
Poor information, support, and follow-up after being discharged was mentioned by many participants. This often led to a sense of “being left on your own.”
Tania (parent) noted that although she was given “a couple little pamphlets” upon their discharge from the hospital, the content was not explained, and she did not feel that this information was clear or useful enough. As she reflected in the following extract: “What am I going to read off there? It’s not going to tell me how to deal with it. What do I do now when I get her home? I have never dealt with anyone that’s been. . . Had anything like that happen so I’m at a loss. All I can think of is, put her to bed, see how she’s in the morning. And then what?” (Tania, parent)
Two participants commented on having been “sent home without any support” (Margaret) and a sense of being “just left there and wondering” (Kathy). As Anna noted, she had to do her own “research” to understand what to do next, and although she had a referral for counseling, the waiting time is long. Kathy also felt that “there’s not a lot of support” and that the waiting time for the counselors is too long. In addition to this, Kathy raised concerns about having to follow up with the police, who never contacted her afterwards to explain what happens next. She was mostly worried about her daughter’s wellbeing, explaining that “I don’t know what to do” and “I don’t know. . . how to protect her.”
Memo: It is interesting to note here, that it is central to the role of the Crisis Care clinician to provide parent/carers with information about the service system, about possible emerging symptoms of trauma and how to support their children in the face of these as well as provide on-going support and referral to whatever support services are indicated. While it is possible that these families did not receive these things from the clinician; it may also point to other dynamics at play. Firstly, it could be indicative of the manifestation of trauma in those particular families that meant that verbal information was not taken on board at the time (this is the reason that written information is also given to families to take home). Alternatively, these families could be gesturing toward broader systemic issues whereby the key service providers, the police, medical response, and the psychosocial response (not to mention a child protection and/or the family violence service system response) are siloed and disconnected.
Summary of Findings
The children, young people, and parents in this study comprise victim/survivors aged between 4 and 16 along with their biological mothers. They all spoke with emotion regarding their experiences with Crisis Care, broadening the original focus of the study, which sought to understand the FME and the experience of coming to hospital, to include their experiences with the police and their feelings of isolation and distress after they were discharged. This is unsurprising, self-evident perhaps, as the story does not begin and end in the Emergency Department but is a snapshot in a series of events that occur within a context, culture, time, and place.
A set of key stages emerged from the data and within the stages, a set of themes. The findings highlight that a child victim/survivor and their mothers are expected to negotiate a path and process that is physically and emotionally overwhelming, and by its very nature, harrowing. They demonstrate the ways in which diversity, polyvictimization, and intersectionality were sometimes ignored in favor of a “one size fits all” approach. They also offer the Crisis Care team ways to mitigate some of children’s distress, through kindness, compassion, and a holistic understanding of the child and their needs.
Discussion
The aim of this qualitative study was to try and understand the experiences of children, young people, and their mothers in the hours following the report of sexual assault so that they may inform practice improvement and potentially, any required overarching systemic change.
Research from the United States, as well as that from the United Kingdom and Europe, has already established the need for timely, streamlined, trauma-informed programs and processes following the report of sexual assault that centralize the wellbeing of the child (Cross et al., 2008; Johansson et al., 2017). Such programs and processes help mitigate emerging trauma symptoms and increase safety as well as gather high quality information to inform a prosecution (Hahn et al., 2016; Shaffer et al., 2018).
This study bears out those findings in an Australian context, highlighting the need for similar reforms. It also uniquely adds and centers the voice of the child and parent and includes the perspectives and procedural knowledge of the embedded clinician/researcher (Lewis et al., 2011), adding depth and richness to the data.
Each stage of the crisis period had its own challenges and mitigating factors, starting with the initial report to the police. The decision to report child sexual assault was seen as a distressing and often confusing one for all the participants of the study. This confusion sometimes stemmed from uncertainty about the legal and medical processes involved, fear of having their experience minimized, or the emotional turmoil associated with recounting a traumatic event. Parents sometimes struggled with self-doubt, questioning their actions or inactions. Young victim/survivors in this study found the process to be scary and the need to talk to strangers about their experience upsetting and stressful.
Also, all the participants in this study reported the assault initially to uniformed police at their local police station. While there are other pathways to seeking support following an assault, by reporting to the police, these families were set on a path of an “outcomes driven” or “justice” response, which includes but is not defined by psychosocial support and/or assessment. Police and medical professionals, while often seen by these participants as caring toward their young victim/survivor, are charged with the collection of evidence and the prosecution of a crime and, to them, this is the purpose and priority of the Crisis Care intervention. Families in this study indicated that while they too were seeking a justice response, this was not their only need or priority when reaching out for help.
This finding, that families have many and varied needs, highlights the potential value of a Crisis Care response that is trauma-informed and embeds psychosocial care (Substance Abuse and Mental Health Services Administration [SAMHSA], 2014). Literature into the provision of trauma-informed care highlights the importance of responding to the whole person, recognizing their context, culture, and prior experiences with the service system (NCTSN, 2022). The way the system currently responds does not have the scope to provide this. Psychosocial assessment and care are also not a core part of the response.
However, the presence of empathetic and caring professionals (or lack thereof) that responded to the individual needs of that family had a significant impact on the experiences of the participants. Doctors, clinicians, and police who demonstrated compassion and patience helped alleviate some of the early emotional burden that accompanied entering the Crisis Care process (Marks et al., 2009). Families valued professionals who provided clear information, were kind, and offered practical as well as emotional support (Quadara & Hunter, 2016). This “caring presence” assisted in making families feel safer and more secure.
The value of the “caring presence” was most pronounced when families discussed the medical examination itself. The FME can leave children and parents feeling exposed and vulnerable (Bersen et al., 1993). Young participants related feeling ashamed and frightened during the FME and several children talked about feeling physical pain. Other studies have focused on whether the FME constitutes a re-traumatization experience, and while many consider that it is not (Allard-Dansereau et al., 2001; Marks et al., 2009), others raise the concern of touching, swabbing, and examining the very area of the body so very recently abused can, if not re-traumatize, then certainly distress young victim/survivors (Bersen et al., 1993). This was the case for some participants in this study. Given the relatively low rates of positive findings from FMEs (Herrmann et al., 2014; Hotton & Raman, 2017), careful consideration of when these examinations occur within the timeline of the service response could be considered.
In addition to the already potentially embarrassing and frightening experience of the FME, not to mention the on-going impacts of the sexual assault itself (Marks et al., 2009), navigating the service response system as a whole made some families feel disoriented and overwhelmed, as if they were “lost” in space and time. The procedural labyrinth—characterized by long waits, repetitive storytelling, and complex bureaucracies—can be disorienting. Participants found themselves in unfamiliar, stark, and sterile environments, facing professionals who use jargon and assume procedural knowledge. The disconnection from their usual sense of time and routine sometimes added to their distress, making it difficult to cope with the process and its aftermath (SAMHSA, 2014).
The researcher/clinician spoke with these families usually within weeks (in some instances days) of their experience. This was a part of the original research strategy; the aim was hearing about people’s experiences soon after the event to optimize recall. However, due to these interviews being conducted shortly after the assault, emotions and responses were still raw. While some participants felt that those they met during Crisis Care were, in fact, caring, they also spoke about being confused by processes and they variably reported that they received either not enough or too much information and that the process was too fast, too slow, or well paced. It seemed that participants spoke about Crisis Care in the context of their individual personalities as well as histories, cultures, and communities and, of course, they spoke about their experience in the context of having recently experienced a sexual assault. The impact of participants speaking about what happened to them while still experiencing the effects of that traumatic event should not be underestimated (Williamson et al., 2020). Their narratives were not a dispassionate recounting of events in isolation of context, and it is possible that expressions of frustration, fear, or confusion could have been reported no matter how well co-ordinated the system or how kind the professionals involved. However, these emotions underscore rather than undermine the themes discussed. They speak directly to the need for service delivery to be as client-centered, trauma-informed, and psychosocially active as it can be and argue for an approach that is conscious of caring, that attends to the whole person, alongside the pursuit of justice for the crime committed.
At the conclusion of the provision of Crisis Care, upon discharge from the hospital, families often felt left to navigate the aftermath on their own. The final theme of “going home alone” represented the transition from structured procedures to self-reliance, which was daunting for some participants. Without adequate follow-up care, guidance, and community resources, some parents struggled to support their child’s emotional and psychological recovery. The lack of a coordinated discharge plan (encompassing all members of the multidisciplinary team) can leave families feeling abandoned and unsure about the next steps, contributing to a sense of isolation and helplessness. Given that families may continue to experience symptoms of posttraumatic distress following discharge from the hospital (Kunst, 2010), effective discharge planning could therefore include clear information, referrals to support services, and reassurance that help is available if needed. Furthermore, professionals could actively outreach to families and, given the inconsistencies in what families say they need in terms of after-care and follow-up, not respond with standardized procedures and materials and then leave them to navigate an unfamiliar system alone.
Recommendations and Implications for the Child Sexual Violence and Abuse Crisis Response Sector
The reported experiences of families in this study give credence to the imperative that the service response to child sexual violence and abuse (CSVA) needs to be timely, coordinated and increase feelings of safety, support, and recovery (NCTSN, 2002). From this sample of children and their mothers’, this study also highlights a lack in the provision of a trauma-informed care approach from the time of first report of sexual assault.
A Crisis Response Service for Children and Young People
A “one-stop shop” whereby already established multidisciplinary response teams could respond to an initial report of CSVA may be a solution to the currently siloed nature of the response, with the police, medical and support personnel often meeting for the first time during the response, in the presence of the child and carer. There is currently little provision for discussion or planning pre-presentation to the hospital.
Like Child Advocacy Centers in the United States and services in the United Kingdom and Europe based on the Barnahus model (Cross et al., 2008; Johansson et al., 2017; Shaffer et al., 2018; Williams & Kisiel, 2016), the establishment of Multi-Disciplinary Centres (MDCs) in Victoria is an attempt at genuine collaboration between services to provide a response to sexual assault that puts the needs of victim/survivors at the center, understanding the imperative of a “victim-centered, integrated and holistic response to victims of sexual crime and child abuse (Victoria Police, 2017).” However, there is still a gap in clear, coordinated service delivery between the time of the assault and any visit to an MDC for children and young people. Currently, children and young people cannot access Crisis Care through an MDC, with FMEs taking place only within hospitals. Consideration could be given to a shift in the role of MDCs in Crisis Care.
Similarly, the Victorian Law Reform Commission, in its 2021 review into the reporting of sexual assault, considered the notion that victim/survivors (adults) be given options into whom they can report their assault (Victorian Law Reform Commission, 2021). For example, being able to make a first report to a support center such as Centre Against Sexual Assault rather than police. This provision would, potentially, set young victim/survivors on a different path to the justice response they currently receive when reporting first to the police. As the participants in this study reported clearly, a justice response is usually necessary but not sufficient in the hours following a report of CSVA. A response that places the needs of the young victim/survivor and their family in the center and responded to their priorities, whether they be making a police statement, undergoing a FME or whether more time needs to be taken and processes embedded that respond to the abused child and their carer’s cultural, emotional, social and psychological needs, the outcome is likely to be better for all.
That the components of trauma-informed care (NCTSN, 2002) mirror the perspectives of what participants in this study discussed, adds weight to notion that the service sector response should make a deliberate undertaking to build a model of service delivery that uses trauma-informed principles as its foundation. To ask children to recount their story, without preparation, to do this repeatedly, and then include an intimate genital examination, not only can exacerbate distress, but decrease trust and impede productive communication. From the initial confusion and distress in reaching out for help, through the vulnerabilities and disorientation during procedures, to the isolation felt upon discharge, the journey is fraught. Ensuring a caring presence, adopting trauma-informed practices, and providing comprehensive plans for follow up are crucial in mitigating these challenges and supporting families through such traumatic experiences.
Generalizability and Diversity Considerations
The findings underscore the need for further research to explore the experiences of underrepresented groups. They demonstrate the need for Crisis Care to directly address the intersections of trauma with culture and language, context, gender, and location (NCTSN, 2022). It would be beneficial if future research gave these aspects further consideration. While this study was open to children and young people of all ages, genders and cultures who would normally attend the hospital for Crisis Care, a case can be made that research that is more assertive to include young people from refugee backgrounds, first nations communities, and those in out-of-home care could provide important information as to the role of Crisis Care for those groups in hospital settings. Such research might offer insights into how these groups navigate Crisis Care services and could potentially identify the specific barriers they face. It could also be valuable to investigate any reasons for non-participation in this current study, such as heightened vulnerability, complexities of child or family circumstances, or other barriers. Further research could illuminate the challenges faced by these populations and guide improvements in research methodologies and Crisis Care services to be more inclusive and responsive to diverse needs.
While acknowledging some potential benefits of future research where diversity is a key variable, CGT methodology significantly enhances the validity of this study by emphasizing the co-construction of knowledge between researchers and participants. This approach allows for an in-depth exploration of participants’ lived experiences and the social processes shaping their interactions with Crisis Care services. By employing constant comparative methods and iterative data collection and analysis, this methodology facilitates the emergence of nuanced, contextually grounded theories that are reflective of participants’ diverse perspectives.
Conclusion
This study attempts to shed light on an often-overlooked aspect of child sexual assault. Through the qualitative lens of interviews with children, young people, and parents, the study highlights the ways in which survivors and their families experience and navigate the initial response system and identify areas where improvements can be made. The study also underscores the importance of putting children, young people, and their families’ experiences at the center of the acute response process and highlights the need for a more holistic, trauma-informed approach to child sexual assault response. By elevating the voices and experiences of survivors and their families, in the aftermath of sexual assault, the study provides valuable insights into the gaps and challenges in current responses and provides some insights into how these systems can be improved to better serve survivors and their loved ones.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interests with respect to the authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research and/or authorship of this article.
