Abstract
Objectives
Historically, patients with hematologic malignancies were often declined ICU admission due to anticipated poor outcomes. However, recent publications describe significant improvements in ICU and in-hospital mortality for critically ill patients with hematologic malignancies. It is unclear whether clinicians’ perceptions of outcomes in this patient population have changed, or whether there is consensus on management. This study evaluated intensivist and hematologist perceptions of prognosis in critically ill patients with hematologic malignancies and identified factors that inform their decision-making.
Design
We conducted an electronic cross-sectional survey of Canadian intensivists and hematologists. The survey included 19 questions and a case-based scenario with variations in clinical factors. The survey data were summarized using frequency with percent. Data was compared between intensivists and hematologists using χ2 tests for categorical data. A post-hoc analysis of secondary variables was also conducted using χ2 tests.
Results
A total of 180 clinicians responded to the survey - 63% were intensivists, 36% hematologists and 1% dually trained. Most clinicians reported using a variety of cancer-, patient- and critical illness-related factors for prognostication, and most demonstrated awareness of factors associated with worse prognosis in this patient population. When presented with a hypothetical case, survey results revealed consensus on admitting the patient to ICU but variability in limitations to treatment and goals of care. Additionally, we found wide variability in predicted patient outcomes. There was significant variability in decision-making around withdrawal of life sustaining therapies, but minimal between-group differences between intensivist and hematologist responses.
Conclusions
This study found significant variation among clinicians in predicting prognosis for critically ill patients with hematologic malignancies, although concordance between intensivists and hematologists overall. Further study examining factors affecting prognosis and long-term outcomes for this patient population will help guide clinicians and better inform decisions about medical care.
Introduction
Significant progress in cancer detection, diagnosis and therapy has led to improved survival for patients with hematologic malignancies (HM).1–3 As a direct consequence of improved survival with a heavy burden of treatment and associated side effects, patients with HM commonly face critical illness.4–6 Historically, these patients were considered poor candidates for ICU admission given low survival rates7,8 however recent evidence demonstrates significant improvement in both ICU and in-hospital mortality.1–3,9–12
Clinicians, in conjunction with patients and their families, are often faced with early decision-making around goals of care and the initiation, continuation, or withdrawal of life sustaining therapies. Physicians’ prognostic beliefs significantly influence care decisions and affect mortality more than illness severity scores or organ support needs.13–16 Such prognostic beliefs often guide treatment intensity and discussions with families.
There are currently no clinical guidelines on prognostication, ICU suitability or management of critically ill patients with HM. However, much research has been dedicated to understanding predictive factors for ICU outcomes.11,17–20 Studies suggest clinicians should place more emphasis on patient-related factors such as baseline functional status and comorbidities, and critical illness-related factors such as severity of illness and multiorgan dysfunction, rather than the cancer diagnosis itself.2,10,21 Elements like HM type, remission status, or neutropenia are no longer reliable predictors, while APACHE II scores and need for mechanical ventilation correlate more closely with outcomes.2,18,21–23
It remains unclear whether clinicians apply this evidence in their daily clinical practice. Few studies have looked at physician attitudes toward patients with HM, and whether this differs by physician specialty. It has been shown that oncologists and intensivists have differing views on the role of life support for critically ill oncology patients, 24 however, it is unclear how this specifically applies to patients with HM, and the basis for these differing opinions.
The purpose of this study was to evaluate intensivist and hematologist perceptions of prognosis in critically ill patients with HM, and to identify both knowledge gaps and factors impacting decision-making. We sought to identify whether discrepancies exist between evidence-based predictors of ICU mortality and reported clinician prognostication.
Methods
We conducted a self-administered, electronic, anonymous cross-sectional survey of Canadian intensivists and hematologists who care for critically ill patients with hematologic malignancies. The study was approved by the Research Ethics Board at the University of Calgary (Calgary, AB, Canada; Study ID: REB24-0090).
Survey Development and Validation
We followed a standardized approach for survey development.25,26 Literature review identified the most common reasons for ICU admission, predictors of ICU morbidity and mortality and potential factors that may influence physicians’ perception of prognosis of patients with HM in the ICU. From this literature review, consultation with content experts, and research team discussions, items were grouped into four domains: clinician demographics, knowledge of reasons for ICU admission, reported utilization of prognostic factors, and factors influencing decisions about goals of care and use of life sustaining measures. The survey included 19 questions with multiple-choice and five-point Likert scale options. One scenario was chosen to represent a common presentation to ICU for a patient with HM, and case permutations were described to ascertain factors that would influence clinician perceptions and decision-making. The survey was designed to be completed in under 15 min to minimize respondent burden and optimize survey completion.
The survey was pre-tested by five members of the investigator team to assess for question integrity, survey flow, salience, and administrative ease. The survey was then sent to three hematologists and three intensivists with clinical expertise in this field to assess for clarity, content validity and face validity. We then pilot tested the survey with trainees (five general internal medicine fellows). The trainees were also asked to fill out the clinical sensibility tool. 26
Survey Administration and Population Size
The survey was disseminated through the Canadian Critical Care Society, Canadian Hematology society mailing lists, and to department heads and program directors across Canada. This strategy made it impossible to know the number of individuals who received the survey invitation and to estimate the response rate. Potential respondents received an email invitation with the link to the survey via the Qualtrics software. We sent an electronic reminder after two and four weeks. Participation was voluntary and questionnaire completion implied consent to participate. Partial completion of the survey was allowed.
Statistical Analysis
The survey data were summarized using frequency with percent. Data was compared between intensivists and hematologists using
Results
Respondent Demographics
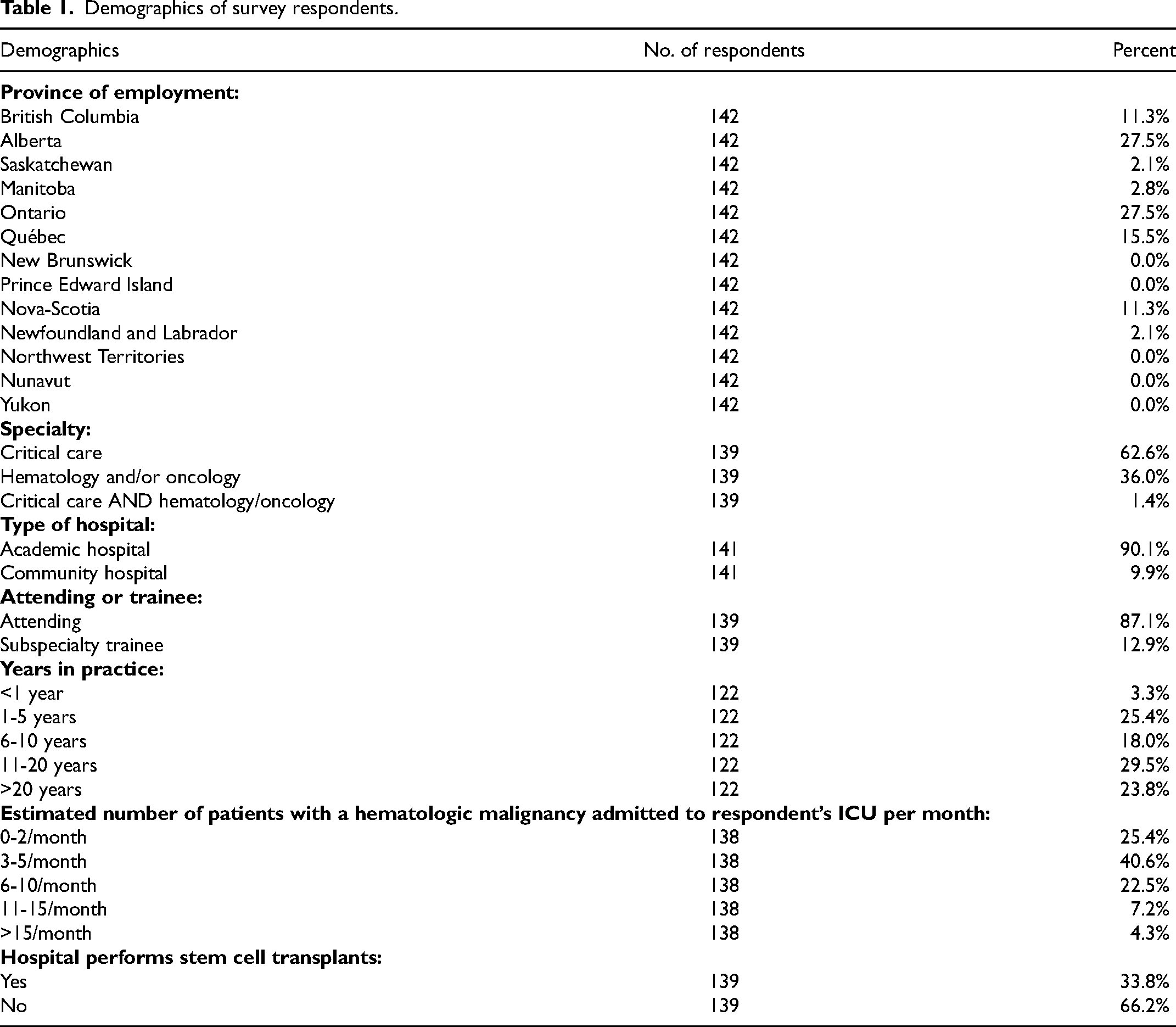
180 clinicians completed the survey: 63% intensivists, 36% hematologists, and 1% dual trained (Table 1). Most worked in academic hospitals (90%) and were attendings (87%). Clinical experience varied broadly, but patient volume ranged from 0–2 to >15 HM ICU cases per month. Most respondents (66%) did not work in a hospital that performed stem cell transplants.
Demographics of survey respondents.

Reported use of Prognostic Factors
Three main categories guided prognostication: cancer-related, patient-related and critical illness-related factors (Figure 1). Factors were considered frequently utilized if >75% of respondents reported ‘often’ or ‘always’. Most clinicians frequently used HM type (94%), treatment line (91%), and malignancy status (98%). Frequently used patient-related factors included patient age (88%), baseline comorbidities (98%), and baseline functional status and frailty (98%). Illness-related factors such as ICU length of stay (77%), goals of care at ICU admission (82%), current infection (80%), mechanical ventilation (88%), vasopressor therapy (84%), and renal replacement therapy (87%) were prominent. Sex and timing from diagnosis to ICU were less utilized; ICU admission APACHE II score, neutropenia, cytopenias, and mucositis were infrequently used (22%, 50%, 19%, 19% and 45% respectively).
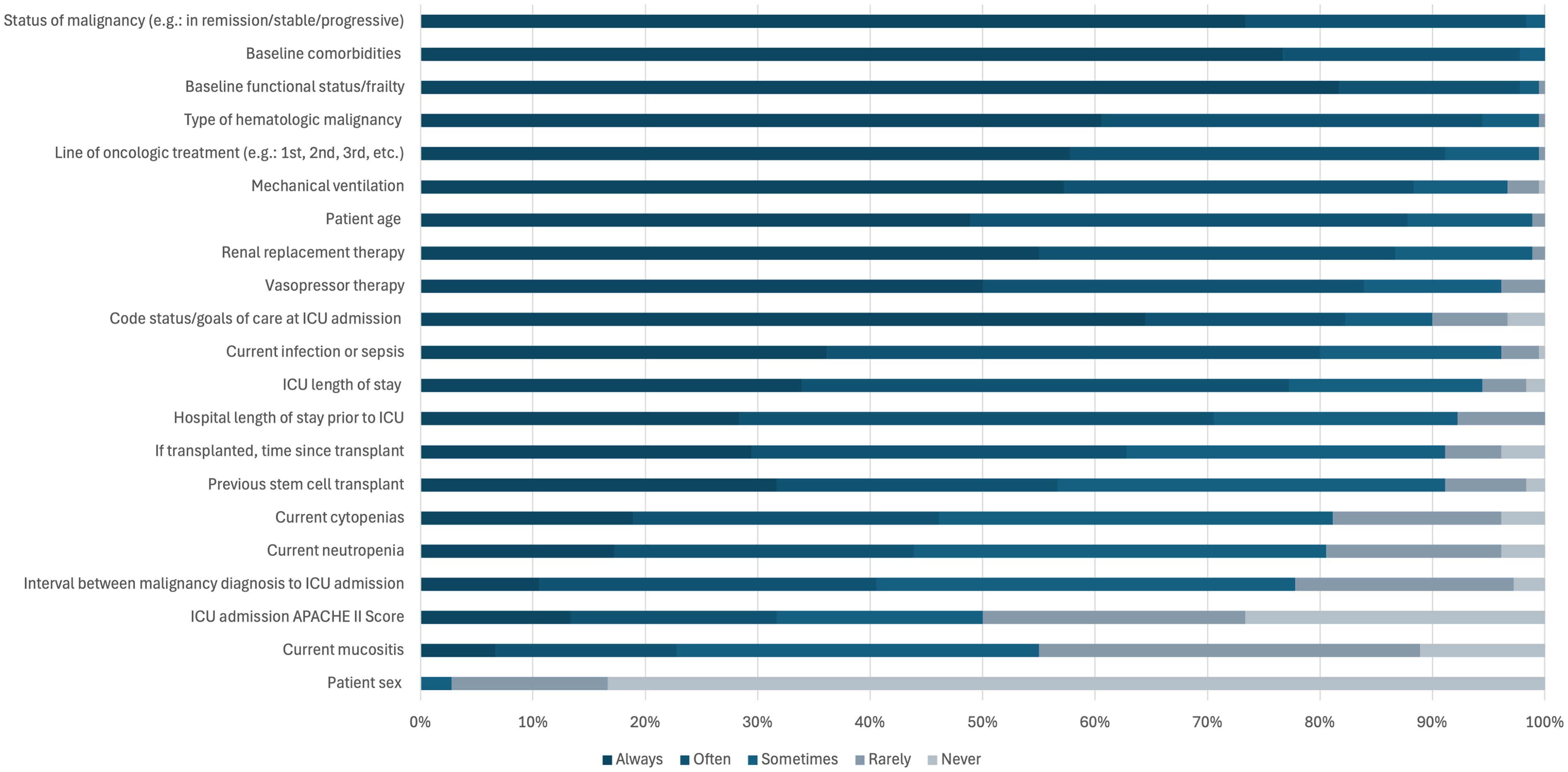
Reported frequency of use of various clinical factors for prognostication in critically ill patients with hematologic malignancies.
Hematologists emphasized time from transplant (74% vs 52%, p = 0.010), while intensivists prioritized hospital length of stay pre-ICU (80.5% vs 52%, p < 0.001). Clinicians who worked in hospitals that did not perform stem cell transplants were more likely to factor in neutropenia (55.3% vs 33.7%, p = 0.014) and cytopenia status (55.3% vs 35.9%, p = 0.028). Clinicians who less frequently treat critically ill patients with hematologic malignancies (
ICU Admission Eligibility and Predicted Patient Outcome
A patient with relapsed myelodysplastic syndrome with graft versus host disease and hypoxemic respiratory failure was presented. 90% recommended ICU admission, but 50% favored treatment limitations during ICU admission. There were no differences in responses between the intensivist and hematologist groups, or other secondary variables (Figure 2). 60% suggested a ‘do not resuscitate’ (DNR) order (Figure 3). Most respondents believed the main responsibility for goals of care discussion at the onset of progression toward critical illness was the hematologists’ (73%). Clinicians assigned prognoses ranging from ICU mortality (30%), in-hospital mortality (23%), mortality within 6–12 months (16%), newly acquired frailty or organ dysfunction (28%) to full recovery (3.5%) (Figure 4).
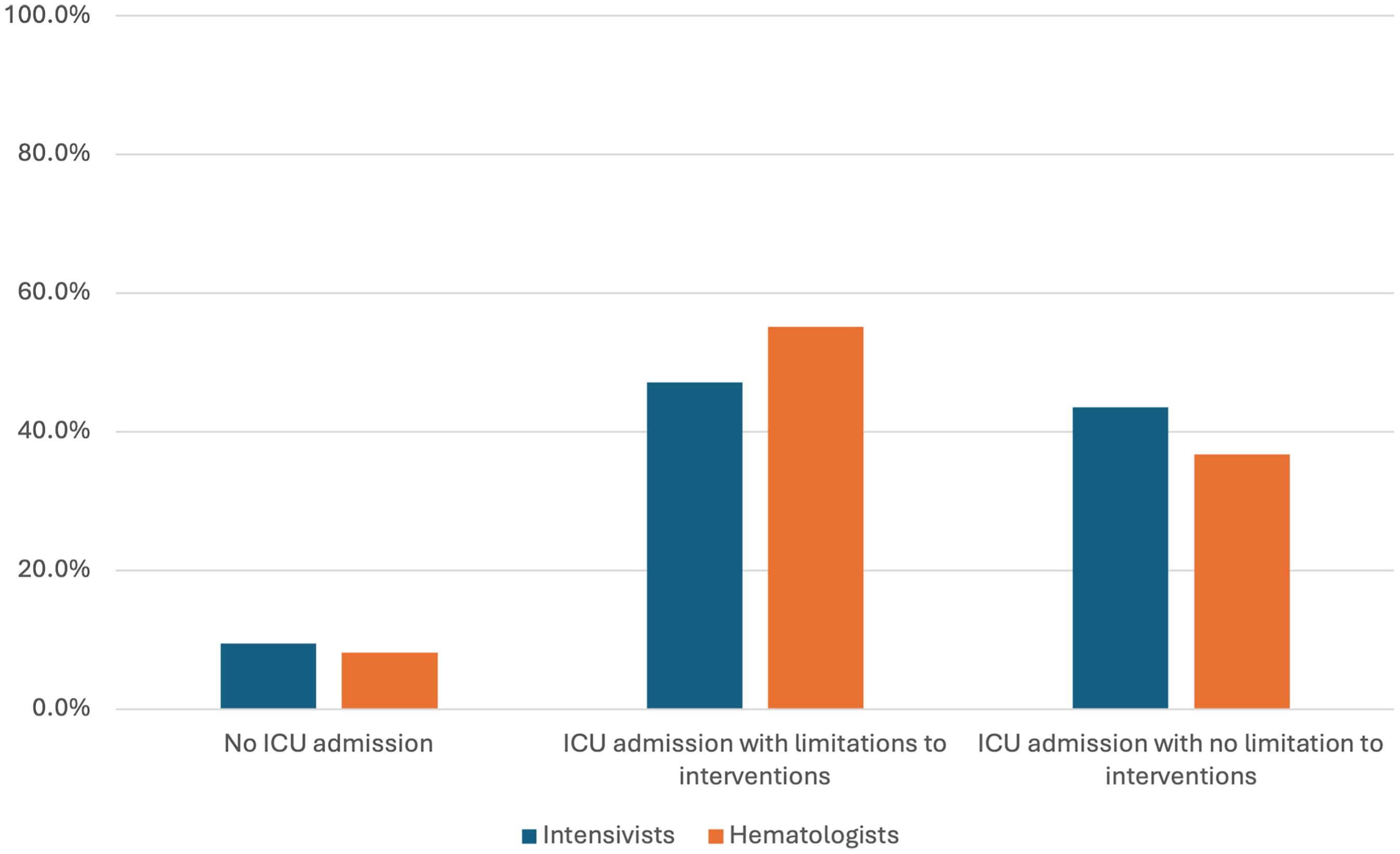
Hematologist versus intensivist recommendation for ICU admission, based on clinical vignette. Examples for limitations to interventions included no intubation, no renal replacement therapy, and/or no CPR.
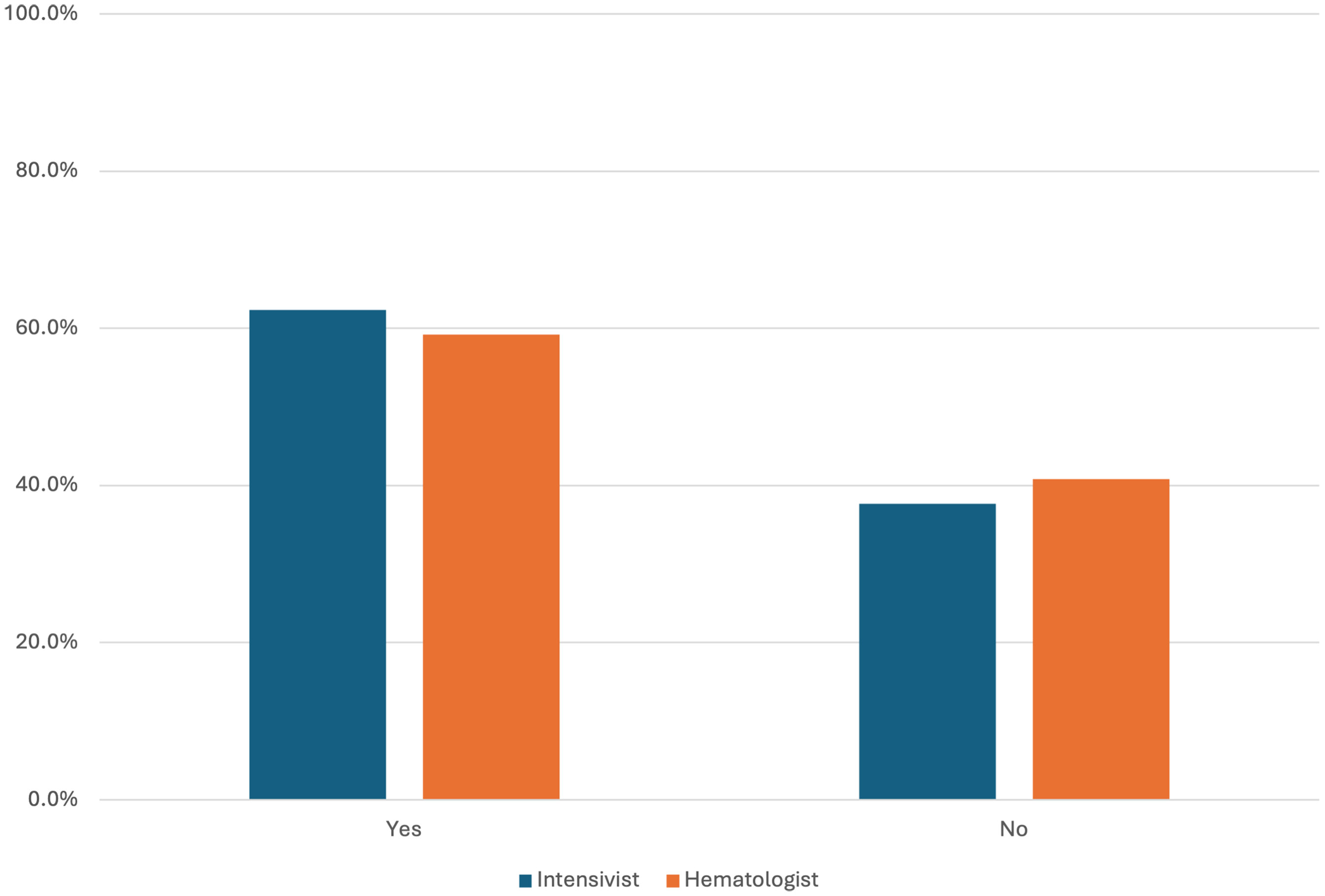
Intensivists and hematologists responses to the question “Based on the information provided, and considering the patient and family's wishes, do you feel this patient should have a “do not resuscitate” order at this point in their hospital admission?”.
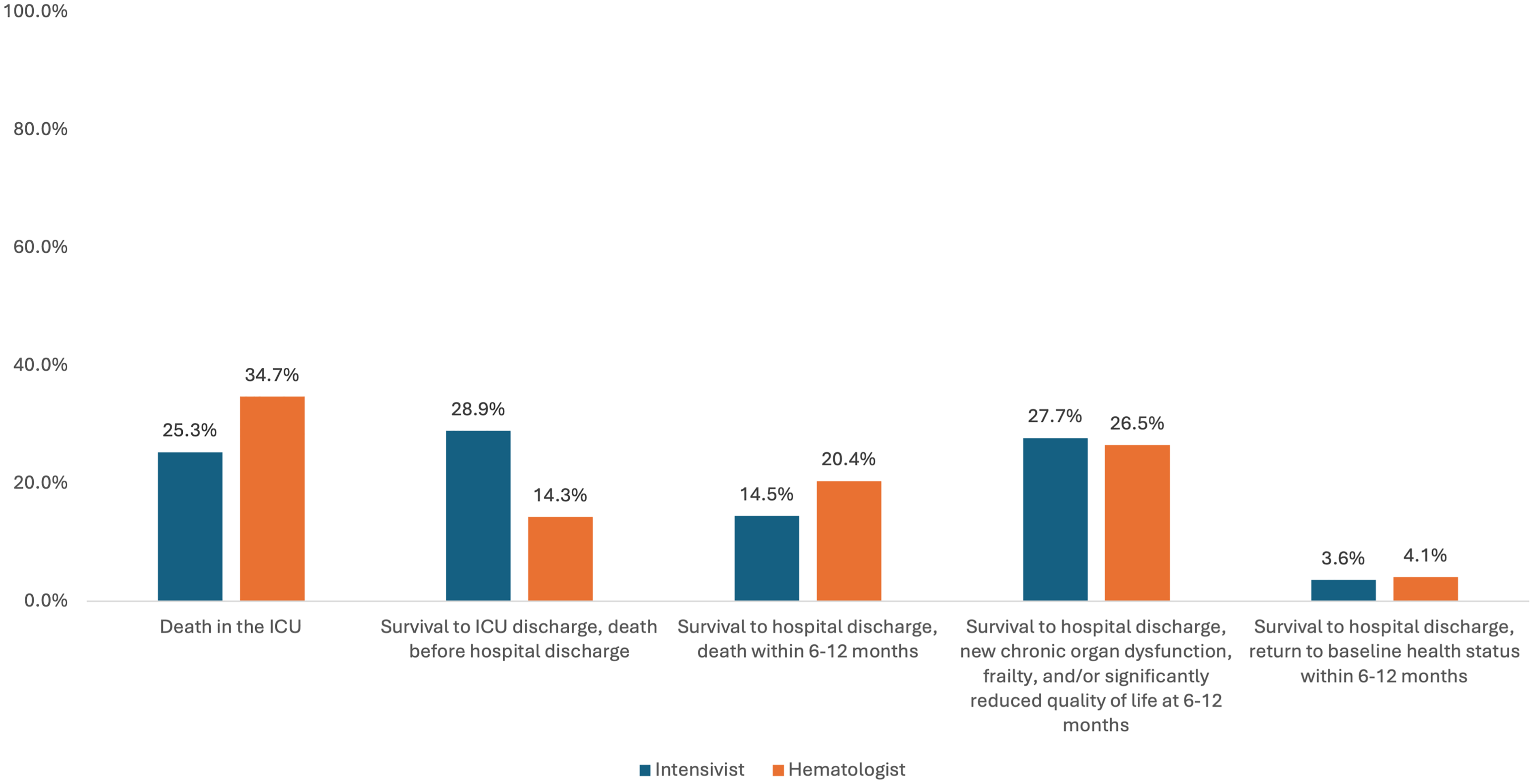
Intensivist and hematologist prediction of expected outcome for patient from clinical vignette, with myelodysplastic syndrome post stem cell transplant with graft versus host disease, admitted to ICU with hypoxemic respiratory failure.
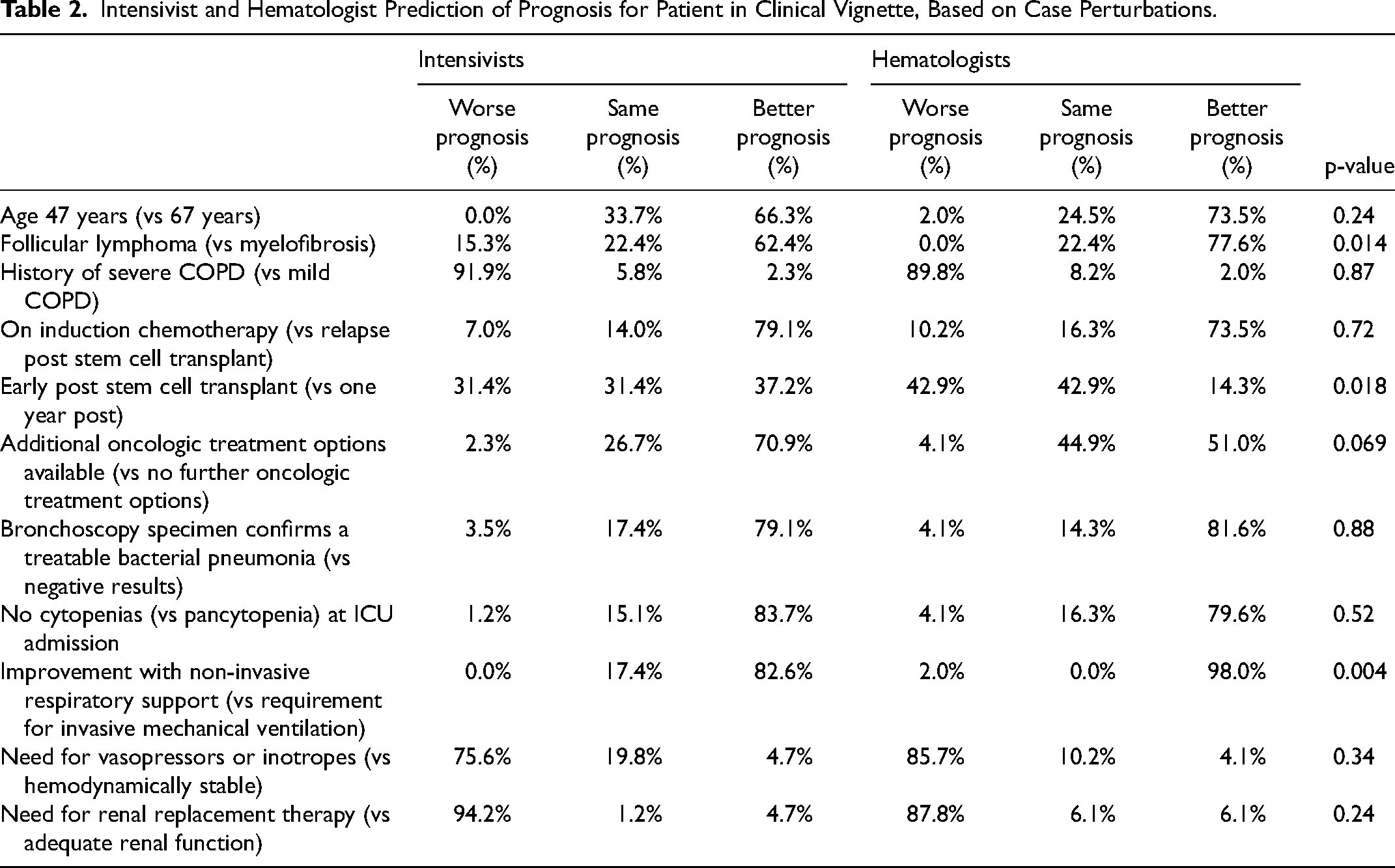
Better outcomes were associated with factors such as being on initial induction chemotherapy, culture-positive results, absence of cytopenias, and improvement with non-invasive mechanical ventilation. Worse outcomes were linked to history of severe COPD, vasopressor use, and renal replacement therapy (Table 2). Clinicians without stem cell transplant experience were more likely to emphasize absence of neutropenia/cytopenias as a positive predictive factor (95.7% vs 76.1%, p = 0.014). Attendings believed an early post stem cell transplant ICU admission conferred a better outcome compared to subspecialty trainees (34.2% vs 5.9%, p = 0.045). Clinicians <10 years in practice were more likely to emphasize early post stem cell transplant ICU admission (42.1% vs 21.5%, p = 0.046) and need for inotropes as negative predictive factors (89.5% vs 67.7%, p = 0.015).
Intensivist and Hematologist Prediction of Prognosis for Patient in Clinical Vignette, Based on Case Perturbations.
Withdrawal of Life Support Measures
Factors prompting comfort-focused care included new organ dysfunction (75%), ventilation beyond one week (55%), persistent GvHD (54%), or unclear etiology of respiratory failure (43%) (Figure 5). Among all respondents, 7% would not withdraw life support measures for such a patient. Hematologists were more likely than intensivists to favor withdrawal of life sustaining therapies if ventilation extended beyond one week (76% vs 48%, p = 0.002). There were no further between-group differences based on secondary variables.
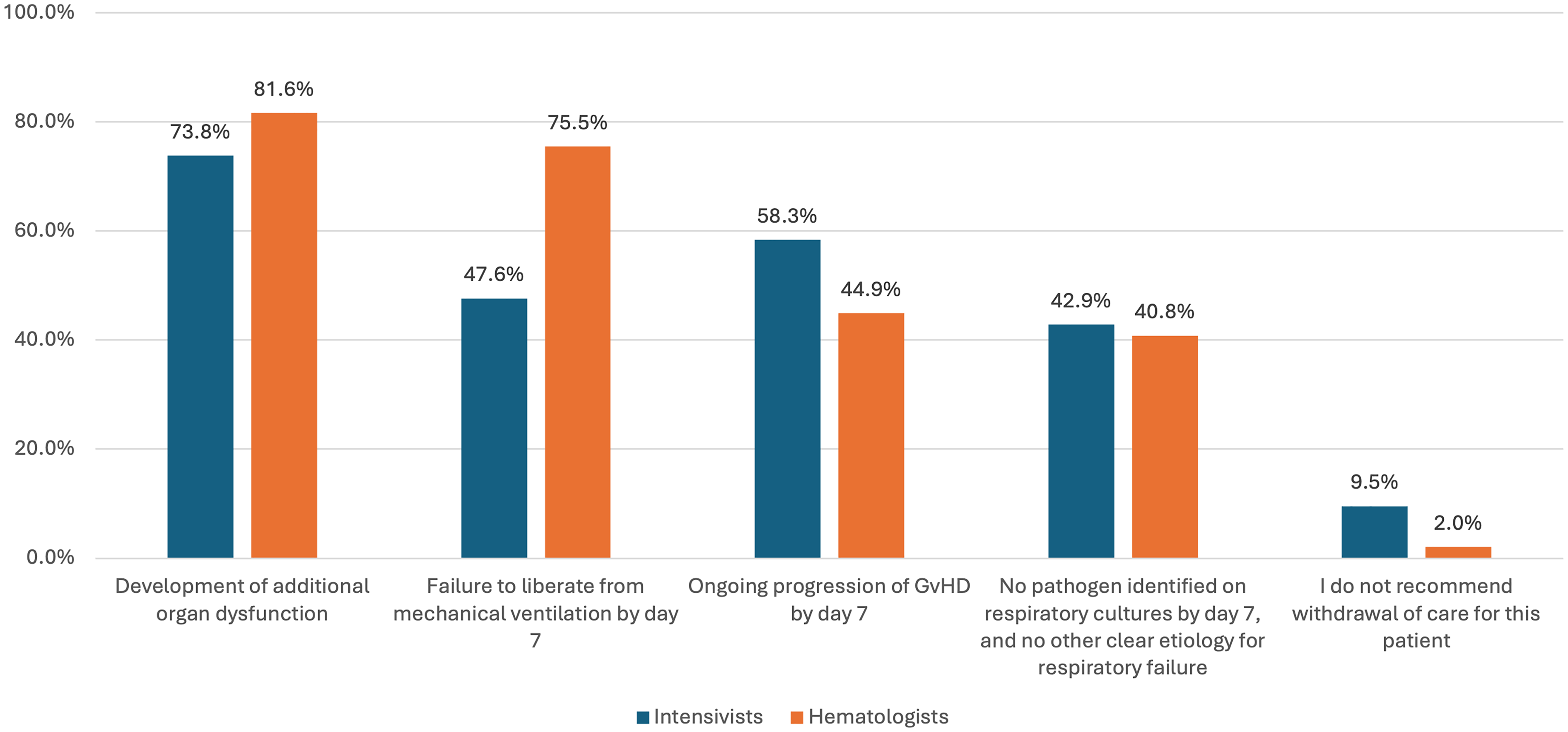
Percentage of intensivists and hematologists in agreement with withdrawal of life sustaining therapies for the patient in the clinical vignette, after one week in ICU, based on various clinical variables; *p =0.002.
Knowledge Gaps
Most clinicians (59%) knew acute leukemias are the most common HM in ICU but underestimated respiratory failure as the leading ICU admission etiology (82% voted sepsis, 15% voted respiratory failure). ICU admission incidence and survival rates for HM patients were frequently underestimated, with most clinicians predicting a 6–10% annual admission rate, and majority predicting a survival rate of 31–50%.2,20,27
Discussion
This survey captured clinician reasoning in the care of critically ill HM patients. There was general concordance among hematologists and intensivists and a broad awareness of prognostic indicators in this patient population. However, discrepancies exist between reported practice and current evidence.
Clinicians recognized high-risk features like significant comorbidities, invasive mechanical ventilation and multi-organ failure, that have been linked to ICU outcomes in HM patients. Cancer-related factors, such as remission status, were overemphasized despite limited predictive value.2,10,21 Conversely, reliable indicators like APACHE II scores were underused.22,28–31 Clinicians also recognized that culture-positive bronchoscopies are associated with better outcomes —consistent with literature showing poorer outcomes when etiology is undetermined.32–37 However, reliance on factors not strongly supported by evidence (eg, cytopenias or treatment phase) highlights gaps in the evidence base and its practical application for this population.2,10,21
There was marked variability in ICU treatment plans and outcome predictions. Most clinicians now favor ICU admission, reflecting improved prognostic optimism. However, outcome projections varied widely, reflecting persistent uncertainty. A near equivalent number of clinicians predicted the patient would not survive ICU admission as those who believed the patient would survive to hospital discharge, albeit with some reduction in their baseline health status. There was a lack of consensus on when to withdraw life sustaining therapies, although general concordance among hematologists and intensivists.
Our survey showed minimal differences between hematologists and intensivists’ perspectives. When transitioning to comfort-based measures, hematologists more often cited duration of mechanical ventilation in impacting their decision, which may be explained by less experience with prolonged ventilator weaning. Intensivists placed more weight on pre- ICU hospital length of stay when prognosticating, perhaps due to less experience with elective admissions for prolonged oncologic treatment. We also found that clinicians with the most experience caring for this patient population, including those that worked in hospitals that performed stem cell transplants, those with increased frequency of HM in their ICUs, as well as those with overall more years in practice, de-emphasized things like neutropenia/cytopenias, time from stem cell transplant and line of oncologic treatment. Interestingly, these secondary variables did not explain differences in predicted prognoses or withdrawal practices.
Survey strengths include a rigorous design and broad specialty inclusion. Additionally, case variations and free text responses enabled better understanding of clinician decision-making. However, limitations include a possible self-report bias, incomplete regional representation, and partial survey responses. As well, real-life practice may differ from stated beliefs. Due to low response rates within some provinces, we were unable to delineate local-regional clustering of data that might have otherwise suggested institution-specific practices that influence decision-making. Additionally, the analysis of secondary variables were post hoc analyses for which our study was not designed to examine, such that secondary variable comparisons were not powered to detect between group differences and the results should be interpreted with caution.
Conclusions
Significant variability exists in clinician approaches to critically ill HM patients. While evidence-based prognostic tools exist, their integration into practice remains inconsistent. The general agreement between intensivists and hematologists underscores the importance of collaborative care. Guidelines and further research are essential to align practice with evolving evidence.
Footnotes
Acknowledgments
We would like to thank Dr Kristina Krmpotic and Molly Ryan for their time and effort reviewing and editing our survey questions and REB proposal. We would also like to thank the program directors and department heads from Hematology and Critical Care across Canada, as well as their associated societies, who helped with survey dissemination.
Author Contributions
HH contributed to the study conceptualization, design of study methodology, data curation, formal analysis, survey dissemination, manuscript preparation and editing. LS contributed to the study conceptualization and survey dissemination. AS contributed to data curation and formal analysis. SM contributed to survey dissemination and manuscript editing. AR contributed to the study conceptualization, supervision, design of study methodology, survey dissemination, and manuscript editing.
Consent for Publication
Not applicable.
Consent to Participate
Participation in the survey was anonymous and free of coercion. Participants were informed that their decision to complete the survey indicated consent and they had the opportunity to withdraw from participation at any time.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Considerations
The study was approved by the Research Ethics Board at the University of Calgary (Calgary, AB, Canada; Study ID: REB24-0090).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
