Abstract
Purpose
The EPIC deterioration index (EDI) and the Sequential Organ Failure Assessment (SOFA) scores are commonly used. However, no studies have examined their performance in hospitalized cancer patients just before intensive care unit (ICU) transfer. We examined the prognostic accuracy of the EDI and SOFA for 48-h ICU mortality.
Methods
This study evaluated consecutive hospitalized medical oncology patients transferred to the ICU from January 1, 2021 to December 31, 2023. Univariable and multivariable logistic regression models examined if EDI scores (EDI-now) and SOFA scores immediately prior to ICU transfer were predictive of 48-h ICU mortality. We assessed the performance of EDI-now, EDI at 24 h before ICU transfer (EDI-24 h), the difference between EDI-24 h and EDI-now (EDI-change) and SOFA using the area under the receiver operating characteristic curve (AUROC).
Results
There were 1987 hospitalizations among 1907 unique patients (mean age = 61, male = 58%); 236 (11.9%) died within 48 hours of ICU transfer. In the multivariable analysis, EDI-Now (OR [95% CI]; 3.11 [2.26,4.27], p < 0.0001) and SOFA (OR [95% CI]; 1.78 [1.31,2.43], p = 0.0002) were significantly associated with 48-h ICU mortality. The AUROC for EDI-now, EDI-24 h, EDI-change and SOFA were 0.657, 0.563, 0.635, and 0.621, respectively. The optimal cut-off threshold for EDI-now was 55 with 73.7% sensitivity, 54.4% specificity, 17.9% positive predictive value (PPV) and 91.5% negative predictive value (NPV). The optimal cut-off threshold for SOFA score was 5 with 63.1% sensitivity, 53.6% specificity, 15.5% PPV and 91.5% NPV.
Conclusion
EDI-now ≥ 54.3 and SOFA ≥ 4 were associated with greater 48-h ICU mortality. High NPVs and low PPVs suggest EDI and SOFA scores could potentially be used to identify patients at lower risk of dying within 48 hours but cannot be used to predict higher risk of 48-h mortality prior to ICU transfer. Better prognostic scores are needed for the medical oncology population.
Introduction
Cancer patients are often hospitalized for complications related to disease progression, treatment related complications or worsening of comorbidities as a result of cancer or its treatment.1,2 In addition, cancer patients are at higher risk of becoming critically ill as a consequence of multiorgan failure in the setting of anti-neoplastic treatments and immunosuppression.3–5 Prior studies report intensive care unit (ICU) mortality rates ranging between 25–50% in the cancer population with a median ICU length of stay (LOS) of 4 days among medical oncology patients who died in the ICU.6–9 ICU mortality within 48 hours may suggest poor quality of end of life care and transferring patients at high risk of 48-h ICU mortality may be costly and ultimately futile.
To identify patients at high mortality risk, EPIC automatically generates the Sequential Organ Failure Assessment (SOFA) score daily in which higher scores have been associated with overall hospital mortality and overall ICU mortality within the medical oncology population.8,10,11 More recently, EPIC developed the EPIC deterioration index (EDI) score which is automatically generated through proprietary machine learning. Because of the lack of evidence and established cutoff, there is high level of variability in how clinicians may interpret and apply the EDI in clinical practice.12–14 Some clinicians have used the EDI score to identify patients at higher risk of mortality and to initiate goals of care discussions or palliative care referrals. However, few studies have evaluated potential predictive value of the EDI for clinical deterioration such as ICU transfer, mechanical ventilation or death in the medical population, COVID, and trauma patients.12,13,15 To our knowledge, there are no validated prognostic scores which predict 48-h ICU mortality, and no studies have examined predictors for 48-h ICU mortality in medical oncology patients. If clinicians are able to accurately identify patients who are at high risk of 48-h ICU mortality and may not benefit from ICU transfer, alternatives to the ICU such as the palliative care unit (PCU) could be considered as life prolonging measures would not be appropriate in this setting. Understanding the prognostic significance of the EDI and SOFA scores can potentially improve resource utilization and promote goal concordant care. In this study, we examine the prognostic accuracy of the EDI and SOFA scores for mortality within 48 hours of ICU transfer among medical oncology patients at a comprehensive cancer center.
Methods
Design
This retrospective study examined the prognostic accuracy of the EDI and SOFA scores in predicting ICU mortality within 48 hours of ICU transfer among medical oncology patients admitted to The University of Texas MD Anderson Cancer Center (MDACC) between January 1, 2021, and December 31, 2023. The Institutional Review Board at MDACC approved this study and provided a waiver for informed consent.
Eligibility Criteria
Consecutive adult patients (aged >18 years old) admitted through the MDACC emergency department to a medical inpatient team in Houston, Texas, United States during the study period were eligible for this study. All patients must have an admission order to the general ward placed at least 24 hours prior to a transfer order to the ICU. If a patient required multiple ICU transfers during one hospital encounter, only the first ICU transfer that occurred after a continuous 24 h LOS on the general ward during the hospital encounter was included for statistical analysis. Patients who were transferred from an outside facility to the general ward at MDACC or directly admitted to the ICU were excluded.
Data Collection
Data was obtained from the electronic health record (EHR). Patient demographics and clinical outcomes were obtained including patient age, sex, race, cancer site, admission type, time to ICU transfer, overall hospital LOS, overall ICU LOS, and discharge disposition.
The EDI was automatically generated every 15 min in the EHR throughout each hospitalization encounter. The total score ranged from 0 to 100. Clinical variables that were contributing factors as well as their weighted contribution were determined through proprietary machine learning and differed among patients. Variables commonly contributing to the total EDI score included but were not limited to the patient age, systolic blood pressure, respiratory rate, oxygen saturation, heart rate, white blood cell count, platelet count, sodium level, and potassium level.
Because it is unclear what timepoint is the most predictive, we selected 3 different variations of the EDI score for analysis. As one prior study showed that the EDI score's predictive value remained high up to 72 h prior to death within the medical population, this study selected the EDI score generated 24 h prior (EDI-24 h) and the most recent EDI score generated prior to the ICU transfer order (EDI-now) being written to evaluate its prognostic accuracy for 48-h ICU mortality. 12 The change in value between EDI-24 h and EDI-now (EDI-change) was also evaluated for its ability to predict mortality within 48 h of ICU transfer as the change in EDI score has been shown to be potentially predictive of other adverse outcomes. 15
The SOFA score was automatically generated in the EHR at midnight every 24 hours throughout each hospital encounter. The total score ranged from 0 to 24. The worst values for each of the 6 clinical variables (respiratory, coagulation, liver, cardiovascular, central nervous system, and renal) that comprise the total SOFA score obtained during the most recent 24 hour period were used to calculate the total SOFA score for each calendar day. 16 The most recent SOFA score generated prior to the ICU transfer order being placed was used for statistical analysis.
Statistical Analysis
We used the Chi-square analysis test to evaluate differences in the distribution of categorical variables and the student t-test to compare differences in continuous variables between groups. Continuous variables were expressed as means and standard deviations (SD) or medians. The Kruskal-Wallis test was used to test whether the median is the same between groups. The level of significance used for all tests was a two-sided P-value less than 0.05. The end point measure, death within 48 hours of ICU transfer from the general ward, was evaluated using multivariable logistic regression models to calculate odds ratios (ORs) adjusting for patient's age, sex, race, cancer type, hospital admission type, time to ICU transfer, EDI-now, and SOFA. Because all three variations of the EDI score were strongly correlated with one another, only the EDI-now was included in the multivariate analysis.
The area under the receiver-operating characteristic curve (AUROC) was used to measure the ability of the EDI score and SOFA score to discriminate the risk of mortality between patients who died and survived within 48 hours of ICU transfer. The AUROC was calculated using EDI-now, EDI-24h, EDI-change and the most recent SOFA score generated prior to the ICU transfer order.
Sensitivity, specificity, positive predictive value (PPV) and negative predictive values (NPV) were calculated across a spectrum of SOFA and EDI thresholds. Youden's J statistic was applied to identify a clinically actionable threshold for both SOFA and EDI.
A P-value of 0.05 or lower was considered to be statistically significant. All statistical analysis was performed by using SAS software version 9.4 (SAS Institute, Cary, NC, USA).
Results
Patient Characteristics
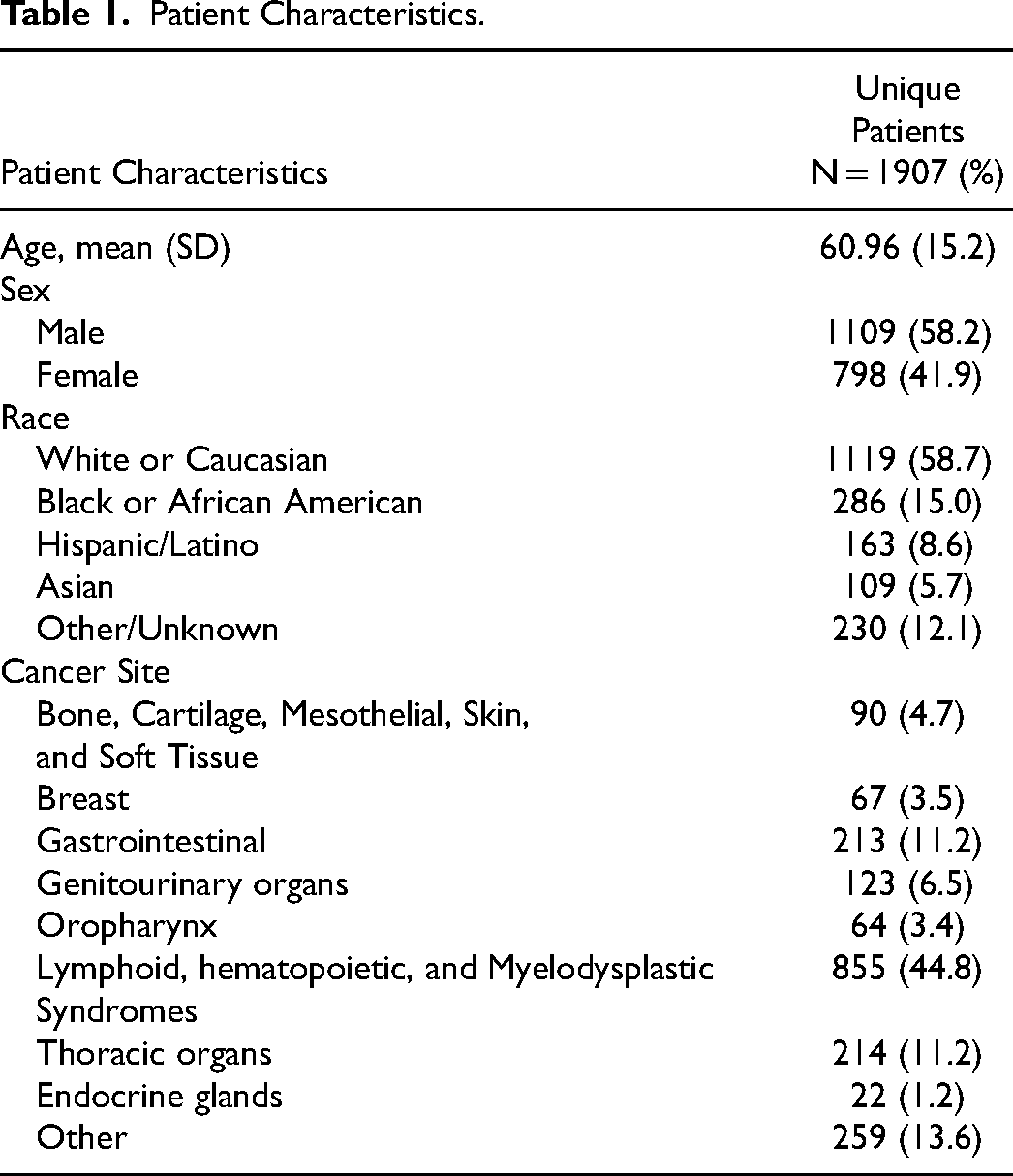
This study included 1987 hospital encounters among 1907 unique medical oncology patients who were admitted to MD Anderson Cancer Center through the emergency department and required ICU transfer during the hospitalization between January 1, 2021, and December 31, 2023 (Figure 1). The mean age during this study period was 61 years (SD 15) (Table 1). The majority of the patient population was male (58.2%) and white (58.7%), and the three most common primary cancer types were lymphoid, hematopoietic, and myelodysplastic (44.8%); gastrointestinal (11.2%) and thoracic (11.2%) (Table 1). There were 236 (11.9%) hospital encounters resulting in death within 48 hours of ICU transfer (Table 2).
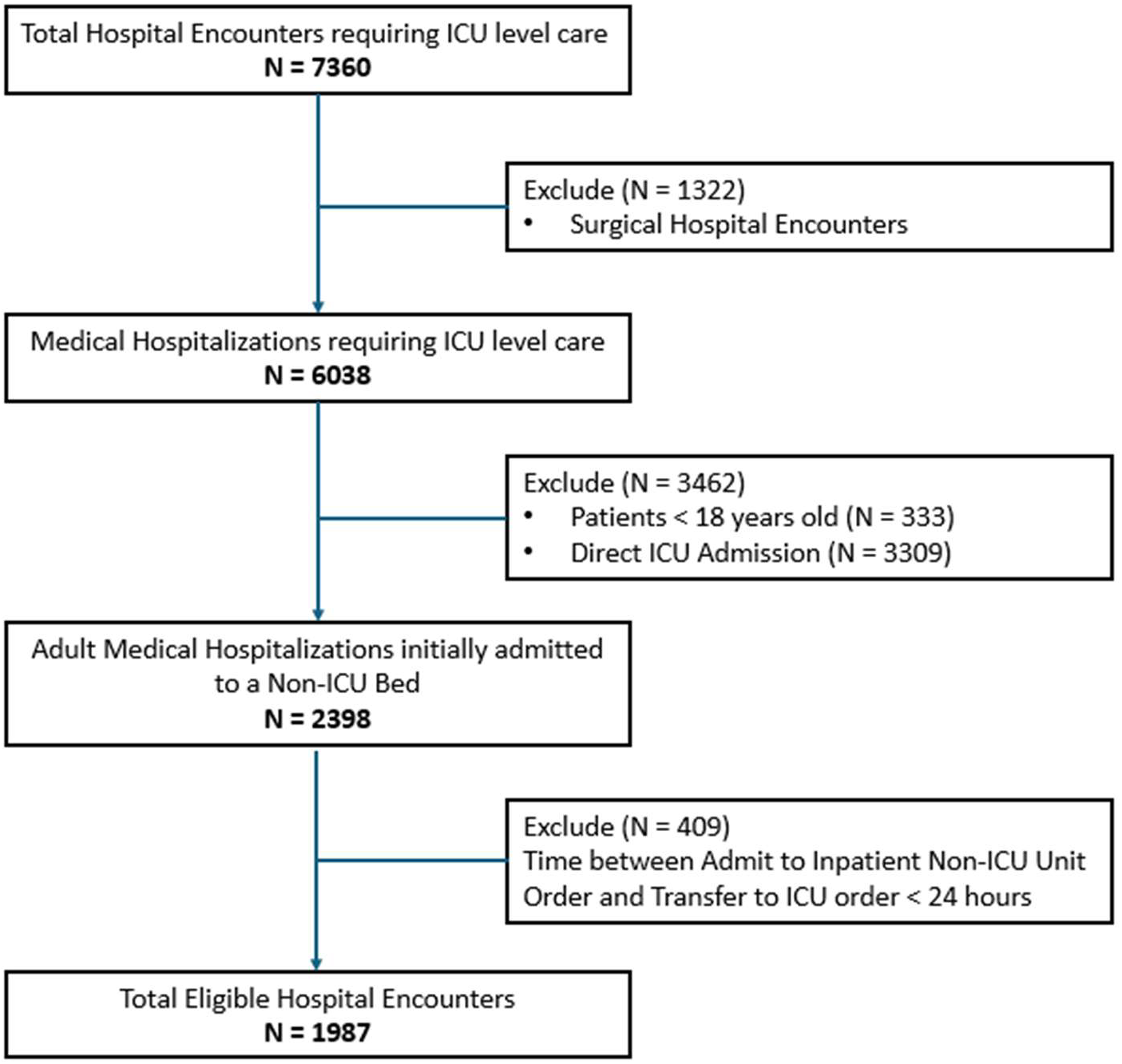
Eligible hospitalization encounters during the study period.
Patient Characteristics.
Clinical Characteristics by 48-h ICU Survival.
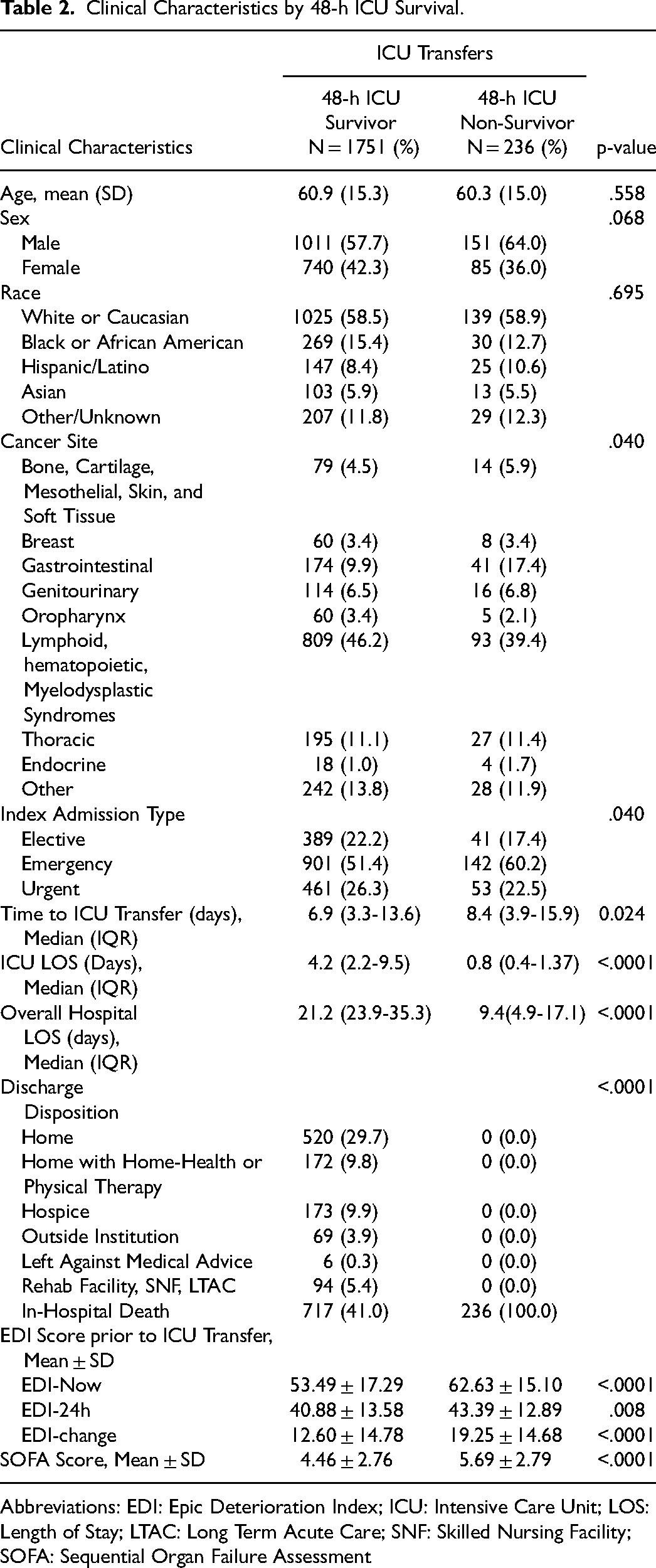
Abbreviations: EDI: Epic Deterioration Index; ICU: Intensive Care Unit; LOS: Length of Stay; LTAC: Long Term Acute Care; SNF: Skilled Nursing Facility; SOFA: Sequential Organ Failure Assessment
EDI Score
The mean EDI-now was 53.5 ± 17.3 versus 62.6 ± 15.1, p < 0.001, and the mean EDI-24 h was 40.88 ± 13.58 versus 43.39 ± 12.9, p = .008, in the 48-h survivor and non-survivor groups, respectively (Table 2). The non-survivors had a significantly larger EDI-change (p < 0.0001) (Table 2). In the multivariate analysis, higher EDI-now remained independently significantly associated with 48-h ICU death (OR [95% CI] 3.11 [2.26, 4.327]) (Table 3).
Predictors of 48-h ICU Mortality.
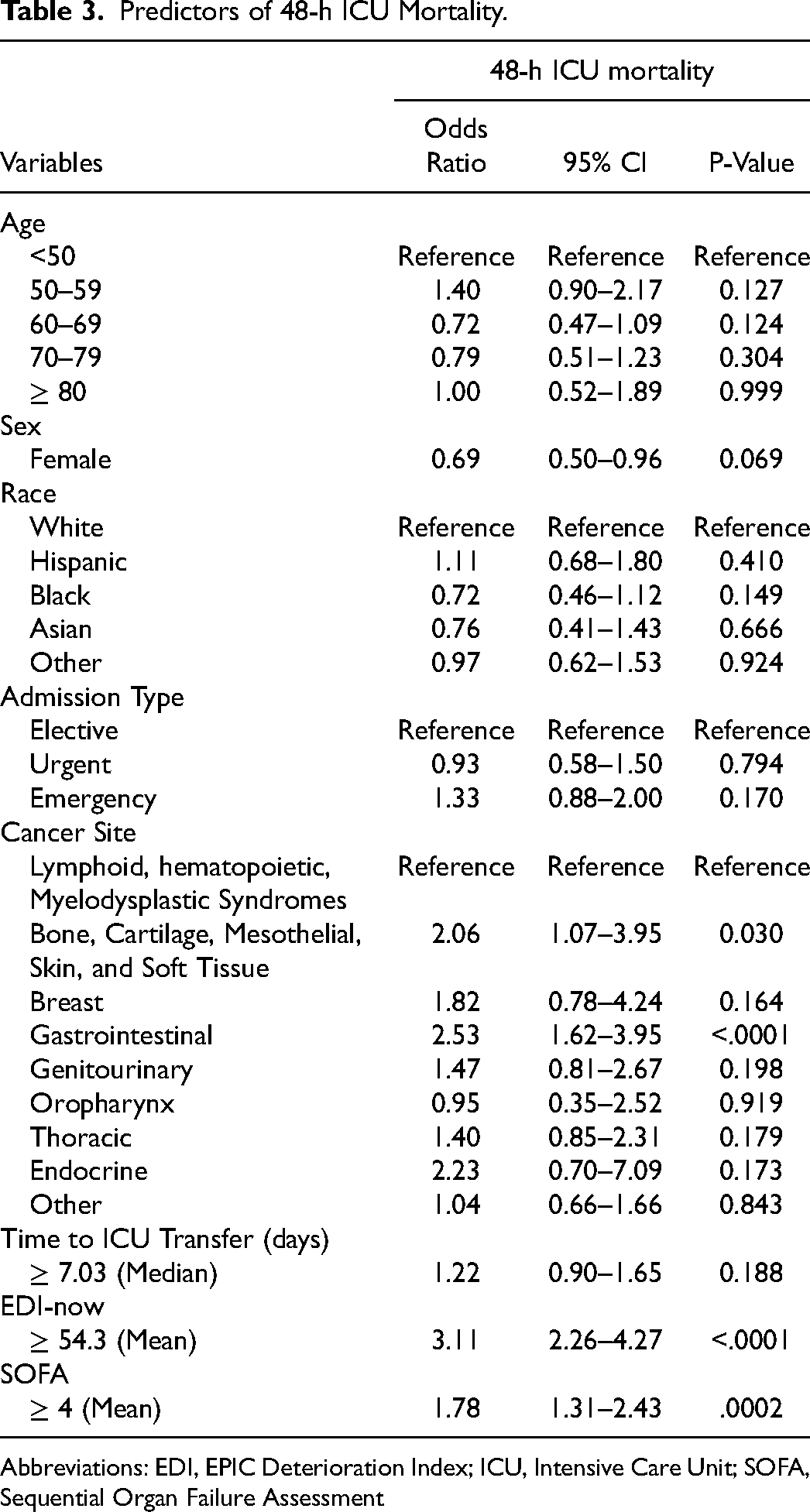
Abbreviations: EDI, EPIC Deterioration Index; ICU, Intensive Care Unit; SOFA, Sequential Organ Failure Assessment
The AUROC of EDI-now and EDI-24h were 0.657 and 0.563, respectively, for 48-h ICU mortality (Figure 2a and b). The AUROC of the EDI-change was 0.635 for 48-h ICU mortality (Figure 2c).
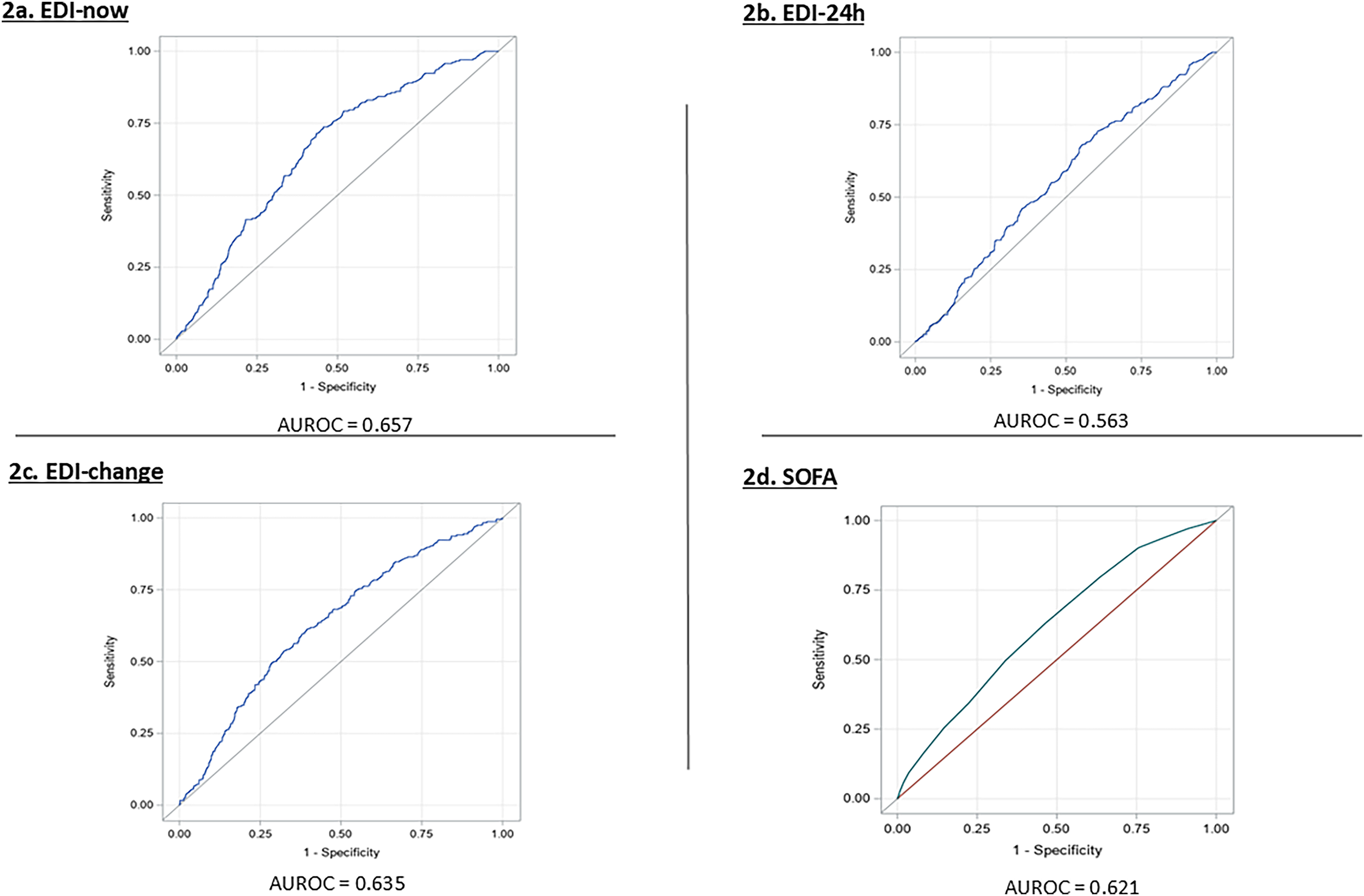
Predictive accuracy of the EDI and SOFA scores for 48-h ICU mortality.
The optimal cut-off threshold identified for EDI-now was 55 with 73.7% sensitivity, 54.4% specificity, 17.9% PPV and 91.5% NPV (Table 4).
Performance of EDI-now and SOFA with Different Cutoff Points.
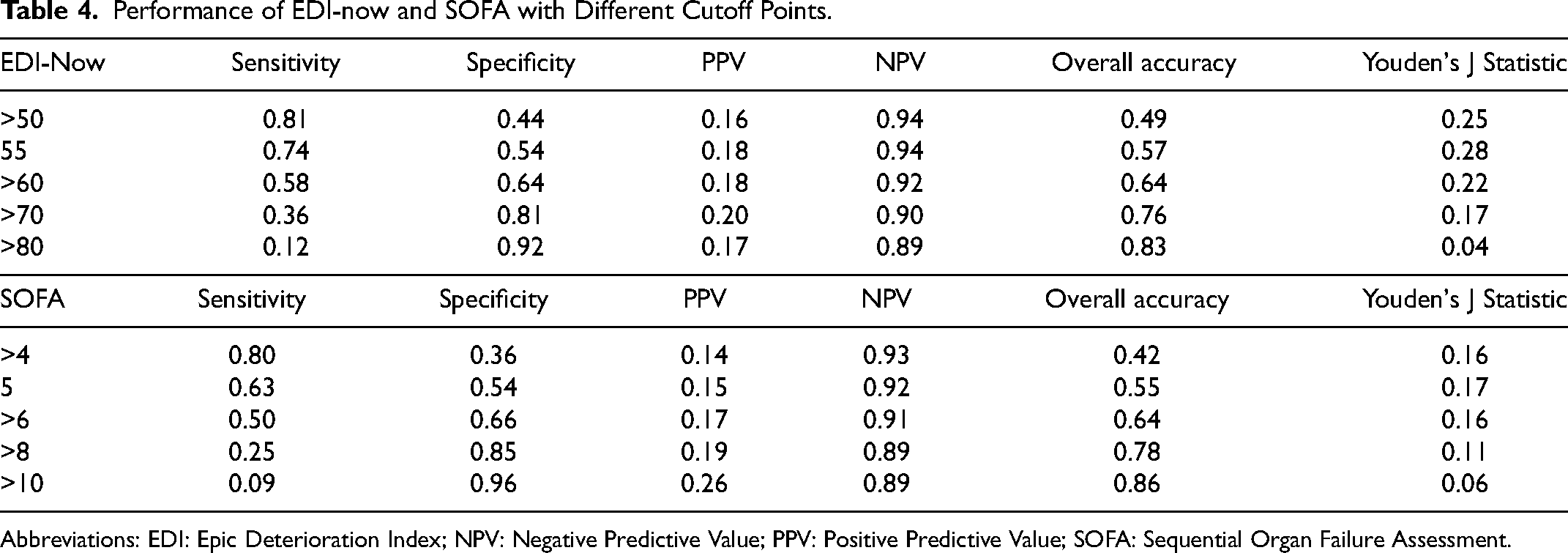
Abbreviations: EDI: Epic Deterioration Index; NPV: Negative Predictive Value; PPV: Positive Predictive Value; SOFA: Sequential Organ Failure Assessment.
SOFA Score
The mean SOFA score was 4.46 ± 2.76 and 5.69 ± 2.79, (p < 0.0001) in the 48-h survivor and non-survivor group, respectively (Table 2). In the multivariate analysis, higher SOFA scores generated just prior to ICU transfer remained independently significantly associated with 48-h ICU death (OR [95% CI] 1.78 [1.31, 2.43]) (Table 3).
The AUROC of the most recent SOFA score generated prior to ICU transfer was 0.621 for 48-h ICU mortality (Figure 2d). The optimal cut-off threshold identified for the most recent SOFA score calculated prior to ICU transfer was 5 with 63.1% sensitivity, 53.6% specificity, 15.5% PPV and 91.5% NPV (Table 4).
Discussion
This study found that a substantial minority (11.9%) of hospital encounters requiring ICU transfer died within 48 h, highlighting the need to identify such patients who may be less likely to benefit from intensive care. We found that higher EDI and SOFA scores were associated with greater 48-h ICU mortality in both the univariable and multivariable analyses; however, their performances were suboptimal with relatively low AUC, low sensitivity, and low positive predictive value, suggesting that it may be difficult to apply these scores in clinical practice to identify at risk individuals. Further research is needed to develop and validate prognostic models to support real-time clinical decision making.
To our knowledge, no prior studies have examined EDI and SOFA scores immediately prior to ICU transfer to identify patients who may not benefit from ICU admission. Existing literature has mostly evaluated prediction models for overall ICU mortality rates based on variables after ICU admission, and few have focused on the medical oncology population. In these studies, 72 hours has been recognized as early ICU death as trends in organ failure during the first 72 hours of an ICU admission have been shown to be predictive of overall death.17–20 One prior study reported a 72-h ICU mortality rate of 17.2% in general medicine patients with septic shock and identified age, malignancy, diabetes mellitus, lack of pathogenic identification and higher SOFA scores upon ICU admission as independent predictors of early ICU mortality. 17 More recently, another study reported a 48-h ICU mortality rate of 5.42% in critically ill patients with sepsis. 21 Our study found a higher 48-h ICU mortality rate than Driessen et al, though this is not surprising as active malignancy was found to be significantly associated with 48-h ICU mortality. 21 As such, the ability to predict early ICU mortality prior to ICU transfer, especially in the medical oncology population, would be beneficial as this can prompt earlier goals of care discussions by providers and allow patients the opportunity to participate in these discussions, to ensure goal concordant care is provided and to potentially avoid futile extraordinary life-prolonging care at the end of life.
This study examined the predictive accuracy of 3 different versions of the EDI score for 48-h ICU mortality in the setting of limited available literature. The EDI-now, EDI-24 h, and EDI-change all performed similarly to the SOFA score in predicting 48-h ICU mortality. However, the EDI-now performed slightly better. Though widely available for use, there have only been 6 studies evaluating the prognostic accuracy of the EDI score within the general medical population, COVID patients and trauma patients.12,13,16,22–24 These prior studies do report acceptable prognostic accuracy of the EDI score in predicting overall in-hospital death and escalation of care including ICU transfer, cardiac arrest, mechanical ventilation with lead times spanning from 3 hours to 72 hours prior to the primary outcome.12,13,15,22–24 Our analysis demonstrated low sensitivity and low positive predictive values indicating that a majority of patients did not die within 48 hours of ICU transfer and that higher EDI scores would not be able to accurately identify the majority of patients at risk of early ICU death. However, high NPVs suggest that clinicians could potentially use low EDI scores to identify patients at lower risk of dying within 48 hours and perhaps more appropriate for ICU transfer. This study highlights that although the EDI score is widely available, clinical utility in predicting 48-h ICU mortality and to ultimately guide decisions regarding ICU transfer remains unclear as this score was not specifically designed for cancer patients or early ICU mortality. Patient and clinical characteristics specific to cancer patients may be unaccounted for in the EDI score, and further study is required to evaluate its utility in other populations and circumstances though this may be difficult given the proprietary machine learning aspect of the EDI score. Other prognostic models may need to be developed and perhaps incorporate physical signs previously shown to occur in advanced cancer patients during the last 3 days of life, including respiration with mandibular movement, peripheral cyanosis, or death rattle. 25
The SOFA score was initially developed to define the severity of multiorgan failure in critically ill patients and has since become a widely used validated prognostic model to predict multiple outcomes including overall mortality in critically ill patients upon admission to the ICU.
16
The use of the SOFA score to assess overall ICU mortality has been validated in adult populations in medical-surgical intensive care units with specific conditions such as sepsis, post cardiac arrest, COVID-19 pneumonia, as well as surgical and trauma patients amongst others.16,26–28 Modified versions have been created to better prognosticate for various patient populations with specific health conditions, including hematologic malignancies (SOFA-HM).
29
Similarly, Nates et al
This study has several limitations. Data was obtained from a single tertiary cancer care center and may not be generalized in other settings. Future studies should consider involving multiple sites to enhance external validity. Due to the retrospective nature of this study, the performance of the EDI and SOFA scores were only evaluated in patients who were transferred to the ICU during their hospitalization. Further studies are needed to further evaluate the prognostic accuracy of the EDI and SOFA scores for 48-h ICU mortality specifically within the surgical oncology, solid tumor and hematologic malignancy population. Though the EDI scores were automatically generated within the electronic health record throughout each hospital encounter, the scores were calculated via proprietary machine learning such that the full list of variables, the parameters of the variables, and the contribution of each of the variables within the prediction model and prior internal validation are not available for review. Additional studies can consider evaluating the predictive value of each component of the SOFA for 48-h ICU mortality. This study did not include prognostic variables such as vital signs, dyspnea or delirium in the multivariable analysis. Reasons for ICU transfer or specific organ failure present on ICU transfer were not included in the analysis, but examination of their predictive value of 48-h ICU mortality can be considered in future studies. Because this study only included patients who were transferred to the ICU, there may be a certain extent of selection bias as patients who were recognized to be actively dying or otherwise deemed inappropriate for ICU transfer were excluded.
Conclusion
In summary, our study highlights the need to examine the utility of predictive models in the medical oncology population prior to ICU level care. Wide availability of the EDI and SOFA scores may tempt reliance among providers. While these scores may have some prognostic utility, the low AUROC and PPV limit their utility to identify medical oncology patients who may not benefit from ICU transfer. Further study is needed to identify variables specific to the medical oncology population and to create a prognostic model with acceptable predictive value for 48-h ICU mortality in cancer patients.
Footnotes
Contributors
Not applicable
Funding
Supported in part by the National Institutes of Health/NCI under award number P30CA016672 and used the Biostatistics Shared Resource. Dr Hui is partly supported by the Dallas Fort Worth Living Legend Professorship.
Conflict of Interest Statement
The authors declared they have no relevant disclosure.
