Abstract
Virtual reality (VR) and augmented reality (AR) technology hold potential across many disciplines in medicine to expand the delivery of education and healthcare. VR-AR applications in radiology, in particular, have gained prominence and have demonstrated advantages in many areas within the field. Recently, VR software has emerged to redesign the physical radiology workstation (ie, reading room) to expand the possibilities of diagnostic interpretation. Given the novelty of this technology, there is limited research investigating the potential applications of a simulated radiology workstation. In this review article, we explore VR-simulated reading room technology in its current form and illustrate the practical applications this technology will bring to future radiologists and learners. We also discuss the limitations and barriers to adopting this technology that must be overcome to truly understand its potential benefits. VR reading room technology offers great potential in radiology, but further research is needed to appreciate its benefits and identify areas for improvement. The findings and insights presented in this review contribute to the ongoing discourse on future technological advancements in radiology and healthcare, offering valuable recommendations for further research and practical implementation.
This is a visual representation of the abstract.
Introduction
Medicine is forever undergoing a transformational shift with the implementation of new and revolutionary technology in pursuit of improving medical capabilities and education. Radiology is at the forefront of this shift—adopting and integrating new technology into daily practice. 1 The field has continually evolved to welcome emerging technologies in its pursuit of enhanced diagnostic precision, patient care, and workflow improvements. One emerging technology pioneering this transformation is virtual reality (VR).
Virtual reality is an immersive computer-simulated environment that makes it possible to experience and interact with an artificial, 3-dimensional world in a realistic way. This experience is achieved through a combination of specialized hardware and software. At its core, VR includes hardware for the positional tracking of eye or head movements with a display of virtual elements experienced from the user’s point of view. 2 A head-mounted display (HMD) headset with built-in eye or head tracking software allows for visualization, while handheld controllers track hand movements and provide haptic feedback. Together, this technology produces a realistic 360-degree viewing experience that allows users to participate in simulated real-life tasks, all within a virtual space.
Augmented reality (AR) differs from the immersive VR experience in that it overlays digital content onto the surrounding real-world environment. This can be as simple as the heads-up display features on a car windshield or the appearance of a text notification in one’s visual field while wearing “Smart” glasses. It can be taken a step further such that the digital and real-world environments can interact as if they are a single entity. This can be accomplished through VR headsets with pass-through capabilities, where front-facing cameras create a stereoscopic video feed for the user, which is then superimposed with digital content. 2 Immersive headsets with both AR and VR functionality, combining real and virtual elements, have been termed “mixed reality” HMDs. The latest technology breakthroughs in mixed reality products, such as the Meta Quest 3 (Meta Platforms Inc, Menlo Park, CA) and Apple Vision Pro (Apple Inc, Cupertino, CA), have changed how digital information can be interacted with and displayed in a real-world environment.
These advances in VR-AR bring the technology closer to mainstream adoption with applications in gaming, business, and entertainment. In 2016, investments in VR startups totaled USD 2.3 billion and are expected to reach USD 20.9 billion by 2025. 3 While still in the early stages of adoption, VR-AR has already found diverse applications within the medical field. Notably, this technology has been used to simulate surgical procedures for pre-operative planning and to provide surgeons and trainees with a realistic and risk-free environment to practice their skills. 4 It also has applications in medical education, enabling healthcare professionals to explore anatomical structures through new dynamic and interactive experiences. 5
VR technology has also been adopted in some areas of radiology. Early research has shown the benefit of immersing learners in a simulated environment to better understand complex 3-dimensional anatomical structures. 6 Others have illustrated the benefit of simulated technology for learning foundational skills for interventional procedures. 7
As the technology continues to improve, attempts are now being made to develop an immersive radiology reading room that mimics the physical workstation. Given its novelty, there is a paucity of published research investigating the potential applications of VR reading room technology. In this review article, we explore the initial VR radiology workstation technology and emerging software developments. The potential future applications of this technology will also be discussed through supporting evidence of VR in other avenues. We also shed light on the limitations of adopting this technology in its current form and the hurdles that must be overcome to realize its true potential.
The Radiology Reading Room As We Know It
The radiology workstation, or reading room, can be loosely defined as a specialized area within a medical facility which, at its core, is dedicated to the interpretation and reporting of medical imaging studies. A typical reading room consists of a computer and monitor display system for medical image viewing, hardware and software for reporting, and a telephone for collaboration with consulting medical professionals. Medical images are stored digitally within a Picture Archiving and Communication System (PACS) for efficient retrieval and analysis. 8 PACS is seamlessly integrated into the workstation so radiologists can access patient images from a central database. These medical images are then reviewed on high-resolution monitors and can be manipulated (eg, windowing, leveling, cropping) for better visualization.
The transition to PACS streamlined the radiologist workflow but also disrupted traditional reading room dynamics. As medical images became accessible outside of the radiology department, there was less need for referring physicians to visit the reading room. Similarly, this integration facilitated teleradiology, allowing radiologists to work from home. 9 However, in its current form, the role of the radiology reading room extends far beyond imaging interpretation. It also serves as an area for collaboration among radiologists, resident teaching, patient and physician consultation, and multidisciplinary conferences. 9 As such, the reading room plays a central role in most radiology operations, especially within academic institutions.
Virtual Reality Radiology Reading Room Technology
While VR technology has existed for many years, its integration within radiology remains relatively nascent. Similar to other avenues, VR in radiology provides users with an immersive 3-dimensional experience using wearable technology. The basics of the technology, as it applies to radiology, are as follows: (1) VR hardware, such as head-mounted displays (ie, headsets), haptic feedback devices (eg, handheld controllers), and motion tracking sensors; (2) VR software, such as user interfaces and content display systems; and (3) derived medical data (eg, 3D-anatomy displays, CT scans) that can be displayed within the immersive experience (Figure 1).
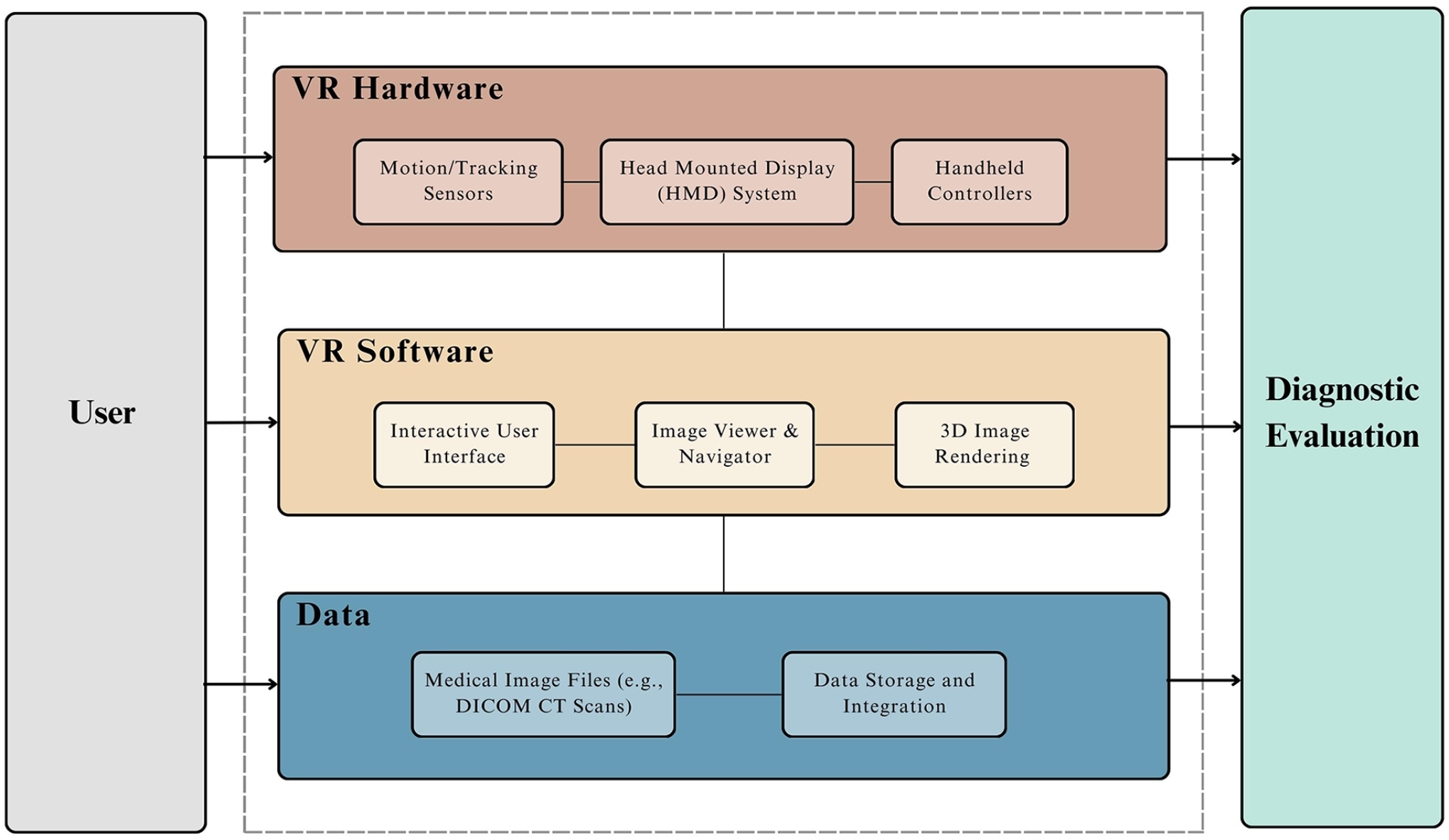
Overview of the standard virtual reality components as they pertain to radiology.
Early pilot models built to mimic reading suite features, such as that used by King et al, 10 used an Oculus Rift HMD system (Oculus VR, Menlo Park, CA) and 3DSlicer (software program) to view multiple individual slices of serial CT scans. Users could interact with the displayed images using a commercial gaming controller and adjust the window width and level. Other more recent attempts, such as VRRRRoom, used similar HMD hardware and a multi-touch frame on a desk surface to create touch-based input. 11 For visualization, 3-dimensional reconstructed models from individual CT slices were displayed on the desk surface and could be manipulated with the user’s touch. Rendering within these models was often deemed insufficient for everyday diagnosis, although this was expected given that these were early prototype models built to explore potential applications of future immersive creations.10,11
Efforts are now being made to create a VR radiology reading room complete with a fully digital PACS workstation. For example, sieVRt (Luxsonic Technologies, Saskatoon, SK) has recently become Canada’s first commercially available VR Digital Imaging and Communications in Medicine (DICOM) viewer. The technology is a web-based software that can be used with commercial high-grade VR HMDs and haptic feedback controllers. Together, it simulates an interactive and personalized 3-dimensional radiology reading room. The software allows users to display stacks of sequential images, adjust window width and level, annotate and mark images, and apply various measurements (eg, lengths, angles, pixel densities). 12 Cases can be retrieved from a local image repository and virtually displayed on a full-featured DICOM viewer with up to 3 virtual monitors. The software can be connected with existing PACS, radiology information system (RIS), and reporting software to integrate with existing workflow practices. The interface also features built-in collaboration tools that allow other users to simultaneously review and discuss cases in the virtual environment. This technology was developed to provide more accessibility to medical imaging and, thus, allow radiologists to take their personalized reading room wherever they go. An example of the virtually displayed reading room environment is shown in Figure 2.
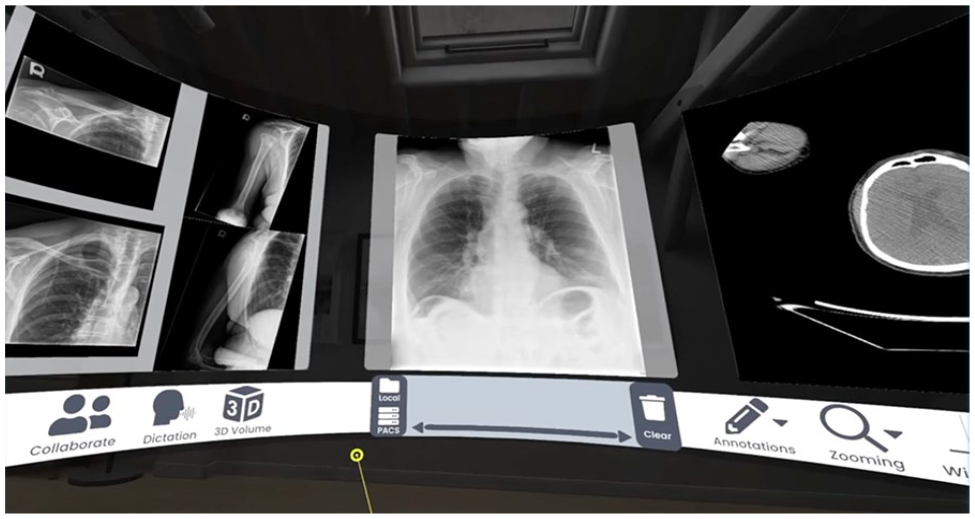
A look inside the SieVRt (Luxsonic Technologies, Saskatoon, SK) virtual reality medical imaging suite. Users can view medical images on 3 virtual display monitors.
Future Applications of VR Reading Room Technology
VR radiology workstation technology holds transformative potential in the realm of medical imaging and diagnosis. A summary of the forthcoming benefits are displayed in Table 1.
Potential Future Applications of Virtual Reality Radiology Workstation Technology.
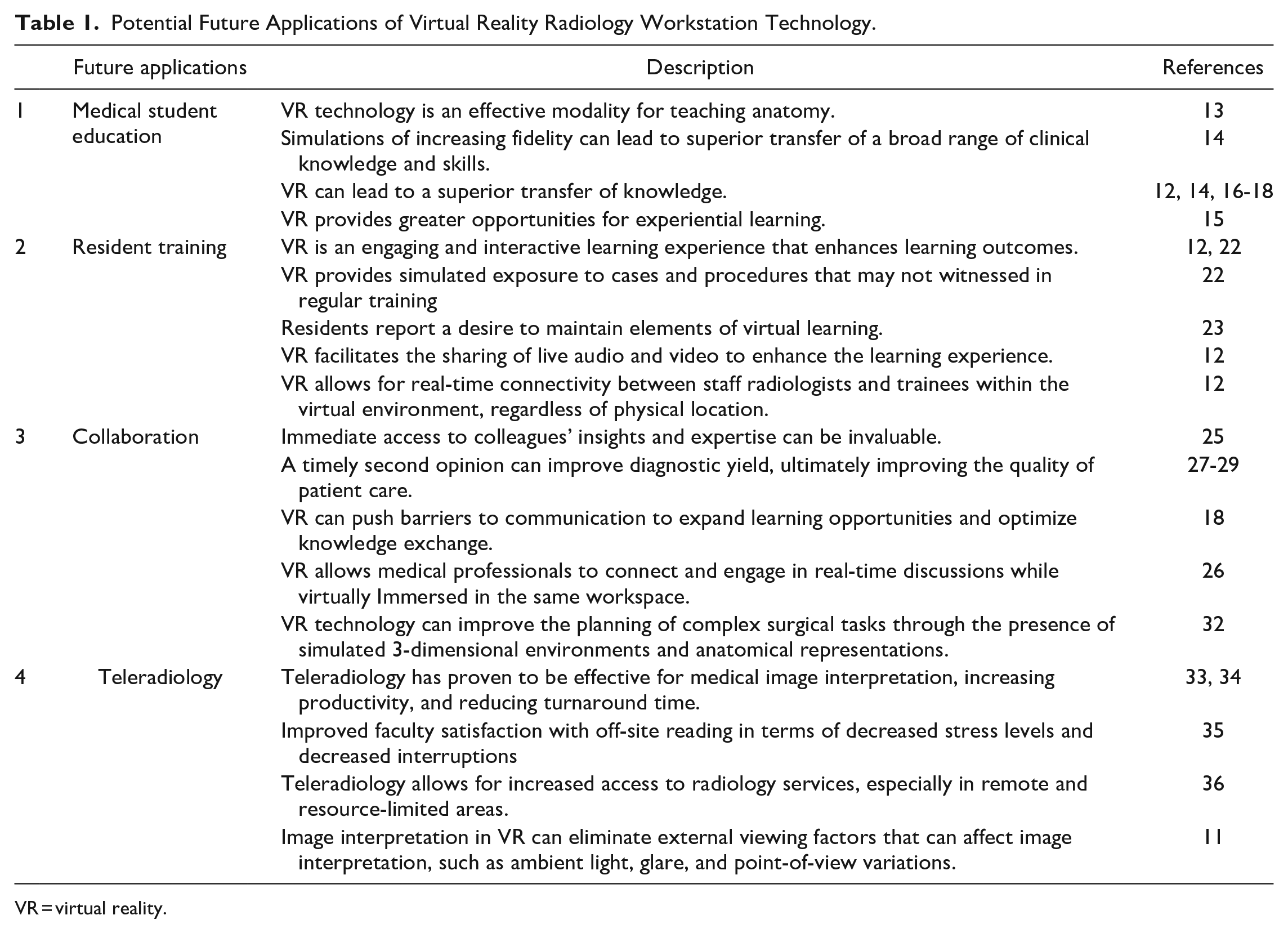
VR = virtual reality.
Medical Student Education
One avenue of exploration for the benefit of integrating VR reading rooms into radiology is its ability to enhance learning experiences and knowledge translation for medical students. The literature has consistently demonstrated that VR technology is an effective modality for teaching anatomy. 13 Similarly, simulations of increasing fidelity lead to superior transfer of a broad range of clinical knowledge and skills. 14 As discussed by Dalgarno and Lee, 15 the educational benefits of VR education include (1) enhanced spatial knowledge representation, (2) greater opportunities for experiential learning, (3) more motivation and engagement, (4) improved contextualization of learning, and (5) richer/more effective collaborative learning. Within radiology, the idea is that this technology’s interactive and dynamic experience can foster a deeper understanding of complex anatomy and pathology. Moreover, offering an immersive and realistic representation of the reading room environment may stimulate greater interest among medical students.
Studies using early VR technology created immersive video game-like experiences for teaching radiologic anatomy to medical students.16,17 These students reviewed single slices of various medical imaging studies (eg, CT, MRI, X-ray) while immersed in the virtual game-like environment. Students objectively performed better at examination after VR radiology anatomy training compared to traditional teaching methods (eg, conferences, seminars, hospital practices). Researchers speculate that the superiority of VR may result from the dynamic and interactive learning experience rather than passive viewing with traditional methods. 18
With current VR reading room technology, a group in Saskatchewan conducted a pilot study to investigate final-year medical students’ radiologic knowledge acquisition and perceptions of VR during their 2-week undergraduate radiology elective. 12 Students underwent interactive teaching and case review sessions with a staff member or resident. They were then asked to individually interpret radiologic cases using a standard PACS-like viewing system, followed by simulated VR reading room case interpretation. Through an objective assessment, students performed better using the VR headset on 2 of the 5 questions and were equivalent to the standard viewer for the remaining 3 questions. Subjectively, the students preferred using VR over the standard viewer and agreed that VR allowed them to find subtle imaging findings more confidently. 12 The immersive nature of VR also allowed for subjectively better concentration and distraction elimination. Although the research is limited, the data suggest that VR-simulated reading room technology can be a beneficial adjunct to conventional teaching methodologies.
Resident Training
Resident learning and teaching are at the heart of developing highly skilled radiologists. Recently, VR technology has been incorporated into many residency program curriculums, allowing trainees to gain medical knowledge, practical skills, and procedural training exposure.7,19 Residents across many specialties value VR as part of their education and believe it is a successful adjunct to current training practices.20,21 It is often seen as an engaging and interactive learning experience that enhances learning outcomes.12,22 VR in residency training has shown potential in addressing the challenges of remote learning and provides simulated exposure to cases and procedures not witnessed in traditional training. 22 During the COVID-19 pandemic, there was an exponential rise in virtual trainee learning, and many radiology residents still report a desire to maintain elements of virtual learning post-pandemic. 23 Thus, VR can be a standardized and engaging method for residents to gain adequate case exposure.
At many institutions, radiology residents spend most of their day performing case interpretation in the reading room and then one-on-one with staff radiologists. Residents highly value this one-on-one teaching with staff and believe it is essential for further developing diagnostic skills. 24 It allows for immediate feedback, direct clarification and discussion of nuanced case findings, and expert insight that may go beyond physical teaching material (eg, textbooks, presentations). The collaborative tools built into current simulated reading room technology can facilitate direct mentorship, regardless of the resident’s or staff member’s physical location. The current software allows simultaneous connectivity between staff radiologists and trainees within the virtual environment, facilitating the sharing of live audio and video to enhance the learning experience. 12 Residents’ demanding schedules and the increased presence of teleradiology may make it challenging to coordinate in-person case reviews. Similarly, many academic centres have a wide geographical spread encompassing many hospitals and imaging centres. 9 Thus, VR reading room technology can provide the flexibility needed to allow residents and staff radiologists to engage in case review at times that best suit their availability, with no barriers to location.
Furthermore, VR may facilitate collaborative learning through resident teaching rounds, which are a standard component of radiology resident curriculum. Residents can present their approach to interpretation as if they were physically present in the reading room and encourage open dialog and knowledge sharing among the group immersed in the simulated environment. Other residents or staff members will then be able to provide immediate feedback or different viewpoints for the case approach while having the ability to annotate and control the simulated workstations themselves.
Collaboration
Radiology reading rooms provide an area for collaboration with other radiologists and consulting healthcare staff. The integration of VR reading room technology has the potential to transcend this collaboration and mitigate geographical limitations.
Collaboration Among Radiologists
At many institutions, seeking second opinions and sharing unique or interesting cases is routine in a radiologist’s workday. For complex cases, immediate access to colleagues’ insights and expertise can be invaluable. 25 With current built-in collaboration tools, this emerging technology will allow radiologists to connect and engage in real-time discussions while virtually immersed in the same workspace. This has been demonstrated using VR technology in other medical fields, such as preoperative planning. 26 Together, radiologists will be able to seamlessly review complex cases and share their thoughts and insights without geographical limitations. This could be beneficial not only for colleagues at the same institution but also for consulting radiologists from other areas. Having a timely second opinion can improve diagnostic yield, ultimately improving the quality of patient care.27-29
Similarly, this technology has the potential to expand collaboration at the global level. VR technology has routinely demonstrated to push barriers to communication to expand learning opportunities and optimize knowledge exchange. 18 This could be particularly beneficial for radiologists to enhance knowledge translation and accessibility of teaching seminars, workshops, and conferences. Through the immersive nature of VR, radiologists from around the world can convene virtually in interactive real-time sessions to share thoughts and explore new and emerging advancements in their field. Additionally, a standard immersive web-based DICOM viewer may facilitate the adaptability of the workstation, allowing radiologists worldwide to interact with the same interface and communicate/interpret in a universal language. Together, this may facilitate the dissemination of knowledge while also promoting a dynamic and unique experience of collaboration among medical professionals.
Collaboration With Other Medical Professionals
Incorporating VR reading room technology further presents an opportunity for improved collaboration with consulting physicians. Clinicians routinely seek explanations of imaging findings from radiologists via telephone or a visit to the radiology reading room. Similarly, radiologists often provide immediate verbal reports to clinicians if imaging findings indicate the need for emergent intervention. With access to VR workstations, consulting physicians can obtain direct one-on-one insight from radiologists if they have questions about complex cases or anatomy. A review of 3-dimensional anatomical images and real-time discussion can result in an improved understanding of the clinical presentation among the physician and patient. 30
This technology may also be particularly helpful with interdisciplinary care rounds. Radiologists can provide their expertise while various medical specialists simultaneously review the medical data together. This will foster collaboration and consensus in diagnostic and treatment planning. Similarly, in the realm of surgical planning, surgeons can review cases with radiologists in real time and seek insight into preoperative planning and anatomical landmarks. 31
In its current state, VR technology can improve the planning of complex surgical tasks through the presence of simulated 3-dimensional environments and anatomical representations. 32 These proposed collaborative capabilities may thus allow radiologists to strengthen their role as essential team members within the broader healthcare landscape.
Teleradiology
In recent years, radiology has seen a significant rise in remote work. The introduction of PACS has enabled radiologists to report medical images outside the hospital, and it has proven to be effective. 33 It can even increase productivity and reduce turnaround times with no change in error rates. 34 A recent survey distributed to US radiology residency program directors revealed improved faculty satisfaction with off-site reading in terms of decreased stress levels, no change in rapport with other physicians, and decreased interruptions. 35 Beyond the benefits of radiologists’ ability to work from anywhere, teleradiology allows for increased access to radiology services, especially in remote and resource-limited areas. 36 For example, a study out of Congo found that implementing teleradiology in an impoverished rural area provided immense clinical value with the potential to change diagnoses and treatment plans. 37 Similarly, it can provide a temporary resolution in areas with reduced staffing by allowing radiologists to provide services remotely.
While the benefits of teleradiology are well documented, physical reading rooms are still the epicentre of image interpretation, especially in academic institutions. The American College of Radiology acknowledges the benefits of teleradiology but also believes the traditional practice model may better serve the overall interests of most communities. 38 This trend and emerging technology illustrate the increased demand for innovative virtual reading room solutions. Current VR workstation technology is built on the premise of owning a portable workflow station that can be used virtually anywhere. With the ability to truly emulate a physical reading room environment, future VR workstations may mitigate some of the criticisms and concerns with current teleradiology practices while preserving the benefits of remote work. Namely, the technology’s ability to incorporate reading room activities beyond examination interpretation, such as the aforementioned potential teaching and collaborative benefits, could improve teleradiology practices, especially at academic institutions.
Limitations
Cost/Accessibility
Although the potential applications for future VR technology are promising, it is essential to acknowledge the challenges and hurdles of future implementation. Adopting VR technology has the potential to save future production costs, but the initial upfront costs can create a financial barrier to acquisition. VR hardware costs thousands of dollars, and current VR reading room software has a current retail price of 600 CAD per license. 12 The aforementioned collaborative benefits of having multiple users immersed in the simulated environment can only work if the technology is acquired and accessible. This high upfront cost may limit its adoption among smaller healthcare facilities. Likewise, one of the biggest hurdles to improving resident training initiatives at academic institutions is funding. 39 As the technology improves, initial costs will likely decrease with time. Still, future research will need to investigate the cost-benefit of acquiring this technology, especially in underserved and resource-limited areas.
Workflow
An efficient workflow is essential for radiologists to stay on top of increasing imaging demand. In its current state, VR reading room technology may pose some workflow challenges. The technology’s initial adaptation and learning curve may cause temporary dips in productivity. Similarly, the initial integration of medical data (eg, DICOM files) into the software may present technological challenges and affect the current seamless transfer of images and reports through PACS. Retrieving medical information on top of the imaging file (eg, patient notes, blood work) may further disrupt workflow. A fully integrated software with access to all required medical data will mitigate this concern. Additionally, the aforementioned collaborative benefit of discussing imaging results with consulting healthcare providers and other “value-added” activities do not directly translate into the ultimate endpoint of radiology workflow—the radiology report. 9 The added time required to discuss these cases virtually can disrupt workflow, and radiologists may see these tasks as more burdensome than a phone call or virtual meeting. If this technology becomes more prominent in the field, institutions will need to carefully plan and manage its implementation to minimize disruptions and avoid hindering the efficiency of clinical operations. As the technology continues to evolve, research assessing the impact of VR technology on workflow outcomes will be beneficial.
Ergonomics
An essential consideration for adopting VR technology is the associated ergonomic limitations, which, despite technological advancements, still pose significant challenges for users. Notably, motion sickness is a common complaint among users of VR headsets, which often results from latency, suboptimal screen refresh rates, and perceived motion within the VR experience that is not often experienced in real life. As the eyes relay information about movement within the experience, the vestibular system, which senses real-time positional movement in space, registers a lack of corresponding activity. This dissonance results in vestibular mismatch, leading to symptoms of disorientation, dizziness, and nausea. 2 To mitigate symptoms of motion sickness, the newest VR headsets use advanced tracking and sensor technology to trace subtle head movements and truly align virtual and real-life motion. Preliminary research using the current VR radiology workstation technology shows promise for avoiding these concerns 12 ; still, the most subtle movements can cause discordance and result in motion sickness. For practical use in radiology, VR technology will also need to ensure that high refresh rates of displays within the screen are upheld to avoid feelings of general discomfort and nausea. It has been reported that a minimum refresh rate of 60 frames per second is needed to avoid these symptoms. 2 Given the significant amount of computing power required to render high-resolution medical images, this may pose a challenge for radiology VR applications.
The general invasiveness and bulkiness of VR headsets, which become more pronounced with prolonged use, also pose a challenge. Radiologists often require extended periods of time for concentrated image analysis, and as a result, the weight and fit of current headsets can hinder their workflow. Similarly, the proximity of the display, combined with its high brightness and pixel density, as well as the need to focus on images that are designed to appear at varying depths, can result in eye strain with extended use. 40 Day-to-day use of VR may exacerbate these ergonomic challenges, ultimately affecting the focus and precision needed for radiologic interpretation. These ergonomic challenges are significant barriers that impede the technology’s widespread adoption within radiology. As the immersive technology industry aims to create more ergonomically friendly environments, future research must explore how these challenges can be mitigated, particularly for extended radiology reading sessions.
Display Fidelity
The application of VR headsets for radiology interpretation faces significant limitations in fidelity. Diagnosis in radiology requires optimal resolution to identify subtle imaging findings. Likewise, consistent presentation of images on workstations is essential for electronic imaging operation. 41 In VR, medical image resolutions differ from those on a physical monitor. Images are fixed in size and resolution on a physical monitor, but in VR, the display adapts dynamically based on the user’s field of view and proximity to the image in the virtual space. 2 For diagnostic purposes, the resolution of the VR display must be significantly higher than that of a typical virtual monitor to simulate an entire workstation, which often includes one or more diagnostic monitors. This high-resolution display must also be duplicated for each eye to create a stereoscopic display. These requirements compound the processing power required for optimal image display, which can be challenging given that the GPU powering VR headsets is often portable and reliant on battery power.
For VR to be recognized and used as a diagnostic tool, it must meet the minimal technical viewing standards set by The American College of Radiology. 41 These standards are in place to ensure that medical images are of sufficient quality for accurate interpretation. In a traditional workstation, diagnostic monitors are calibrated across various elements, including luminance, depth, contrast, and size, to maintain optimal diagnostic parameters. 41 Translating this calibration to VR technology presents unique challenges. It would require the display to replicate the fidelity of regular diagnostic monitors but maintain calibration consistently across different viewing angles and distances within the immersive environment. Thus, while this immersive technology offers an innovative approach to diagnostic imaging, the fidelity and calibration limitations make the technology not quite suitable for routine diagnostic use. Fortunately, the image display quality in VR hardware is continuously improving. 2
Security and Privacy
Radiology services universally prioritize patient data security and privacy. 42 Integrating VR workstation technology, mainly if used remotely, may introduce additional security risks that must be considered. The current technology relies on cloud-based medical data storage, which can expose potential vulnerabilities to data breaches. Similar to a standard PACS viewer, current VR reading room technology requires a password-protected login to access medical images. Still, this technology’s dynamic and collaborative nature may allow for unauthorized user access. Importantly, cybersecurity has been incorporated into teleradiology practices since its inception, and there continues to be considerable research in this area seeking to improve and perfect security features. 43 Going forward, institutions must establish strict security measures to safeguard patient data if this technology is used for remote work.
Virtual or Augmented, Where Does the Future Lie?
It is unclear whether or not this technology will be adopted for everyday use in radiology in the near future. It is certain, however, that the capabilities, functionality, and sophistication of immersive technology will only continue to improve as large technology companies race to develop a winning consumer product. Thus, the drawbacks of current hardware for widespread adoption, namely the ergonomic and fidelity challenges, will likely improve with time. It is also unclear whether the future workstation, if adopted, will welcome an entirely immersive environment (VR) or one that enhances the traditional workstation (AR). In contrast to VR, an AR workstation will allow radiologists to maintain a connection to their physical surroundings and continue to interact with peers and other healthcare professionals in the real world. Such a setup with see-through augmented reality may mitigate symptoms of motion sickness and the unnatural sensations of VR, including feelings of social isolation. Regardless, if the future reflects the trend of emerging technology, the same hardware can be used for both. Mixed reality devices, such as the Meta Quest 3 (Meta, Menlo Park, CA) and Apple Vision Pro (Apple, Cupertino, CA), can serve to create fully immersive environments but are AR-first devices. This would allow a radiologist to immerse in a distraction-free environment irrespective of their physical location or opt for a real-world foothold, tailoring to the specific individual’s needs.
Conclusion
Advancements in technology continue to transform medical education, training, and patient care. Radiology regularly adapts to change, welcoming new and innovative technology for optimized patient care. VR and AR have already proven to be a valuable tool across various medical specialties, including radiology. Now, with new software development, VR has the potential to expand the capabilities of medical image reporting. Although this technology is still a novelty, recent developments demonstrate that it holds promise for transforming how future medical imaging is taught, interpreted, and shared. It is important to note that this novelty has resulted in a lack of comprehensive literature, and this knowledge gap underscores the need for further investigation to truly illustrate the potential benefits of this technology. Adopting this technology in its current state poses several limitations and technological challenges. As the technology improves, the benefits will become more evident; radiology will be at the forefront of that change.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
