Abstract

Introduction
The COVID-19 pandemic catalyzed a rapid adoption of virtual healthcare in Canada with a concurrent push toward more patient-centred services that reduce wait times and improve accessibility. Patients receiving medical imaging services in particular have historically expressed feelings of stress and uncertainty. 1 In recent years, radiology consultation clinics have been shown to reduce patient anxiety and improve patient perceptions about their diagnoses and about radiologists in general. 2 The proliferation of telehealth models, and the onset of a new remote work paradigm among radiologists, 3 has created an opportunity for virtual radiology consultation clinics (VRCCs) to become a new standard for patient care. This study aims to assess patient experience and satisfaction after reviewing imaging results online with a diagnostic radiologist, representing the first pilot of VRCCs in Canada and laying the groundwork for an innovative and holistic care model.
Methods
Regional ethics board approval was obtained prior to initiation of this study. Patients receiving computed tomography or ultrasound imaging at an academic hospital were recruited by medical radiation technologists for participation in virtual consultations with a staff or resident (PGY3) radiologist. Consultations were scheduled for 30 minutes at least 1 week after imaging, between October and December 2023. During consultations, radiologists used Zoom to share their screens displaying their PACS software, navigated patients through their most recent images and imaging interpretations, and answered imaging-related questions. Patients then completed a post-consultation survey assessing their experience using 5-point Likert scale, multiple choice, and free-text responses. Quantitative responses were summarized by mean and standard deviation, and free-text responses grouped thematically.
Results
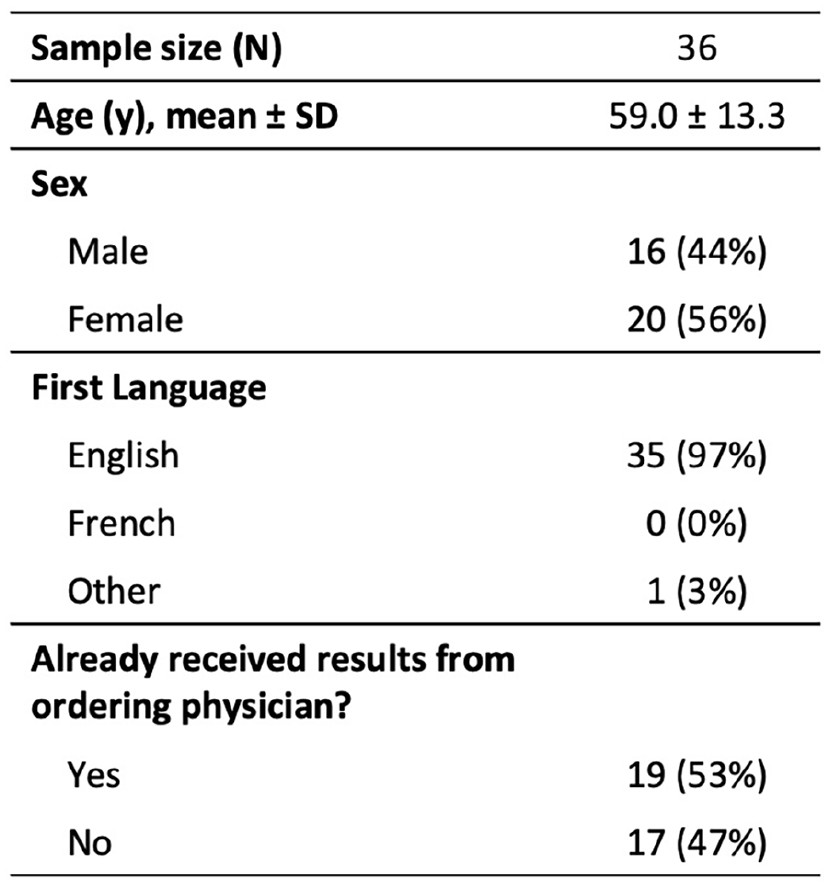
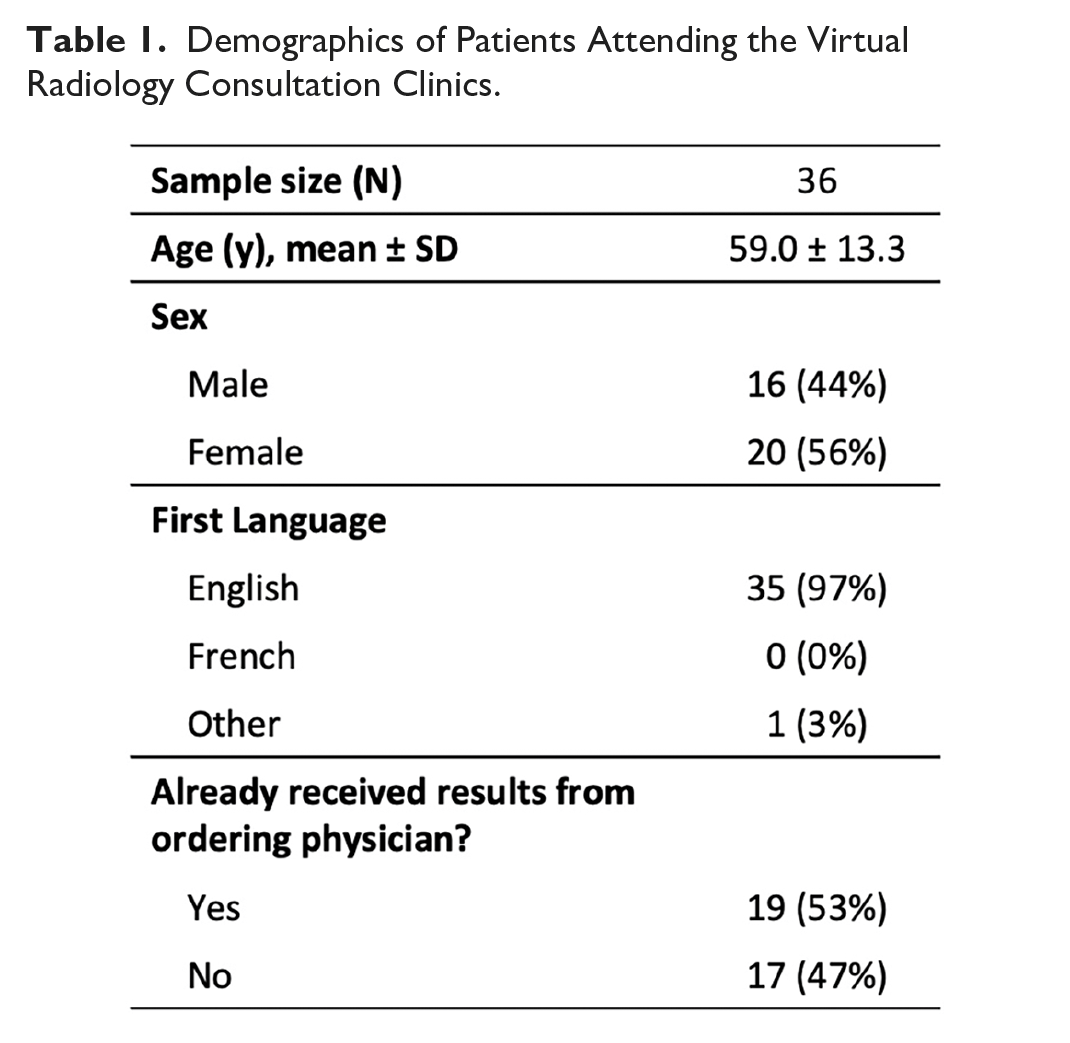
Thirty-six survey responses were collected, with patient characteristics displayed in Table 1. Results indicated a high level of satisfaction (5.0 ± 0.2), improved understanding of their diagnosis due to both the discussion (4.8 ± 0.4) and viewing their images (4.7 ± 0.5), and comfort with the virtual format (4.9 ± 0.3). Response breakdown by question can be found in Figure 1. Patient preference for delivery of future results included 93% via virtual call with imaging-sharing capabilities, 7% in-person at a medical facility, and 0% over the phone. All patients expressed a strong interest in participating in future VRCCs. Free-text responses were overwhelmingly positive, with common themes including enhanced understanding of diagnosis, feelings of reassurance, gratitude, and recommendations for improvement (Figure 2).
Demographics of Patients Attending the Virtual Radiology Consultation Clinics.
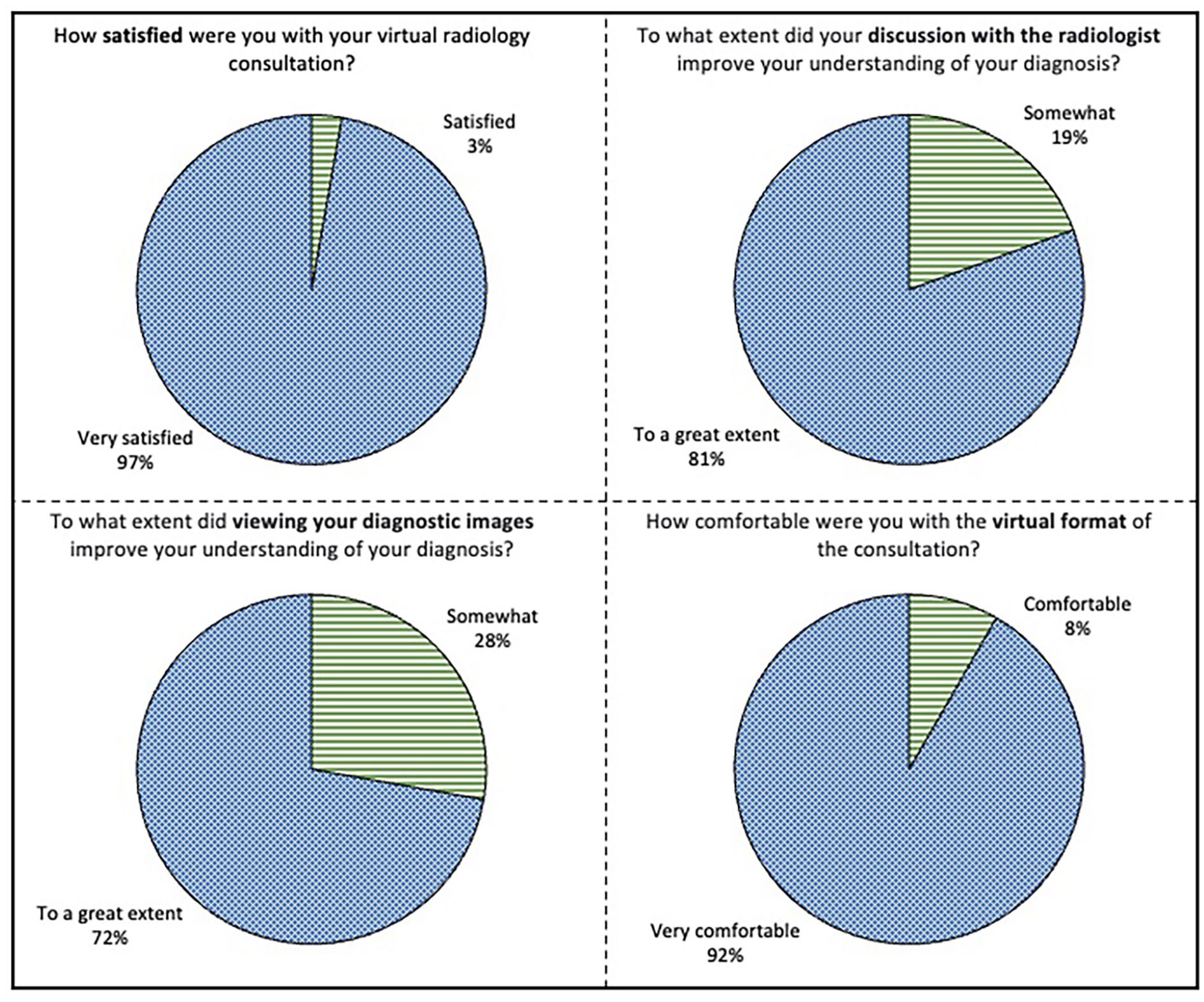
Distribution of patient responses to post-consultation survey questions.
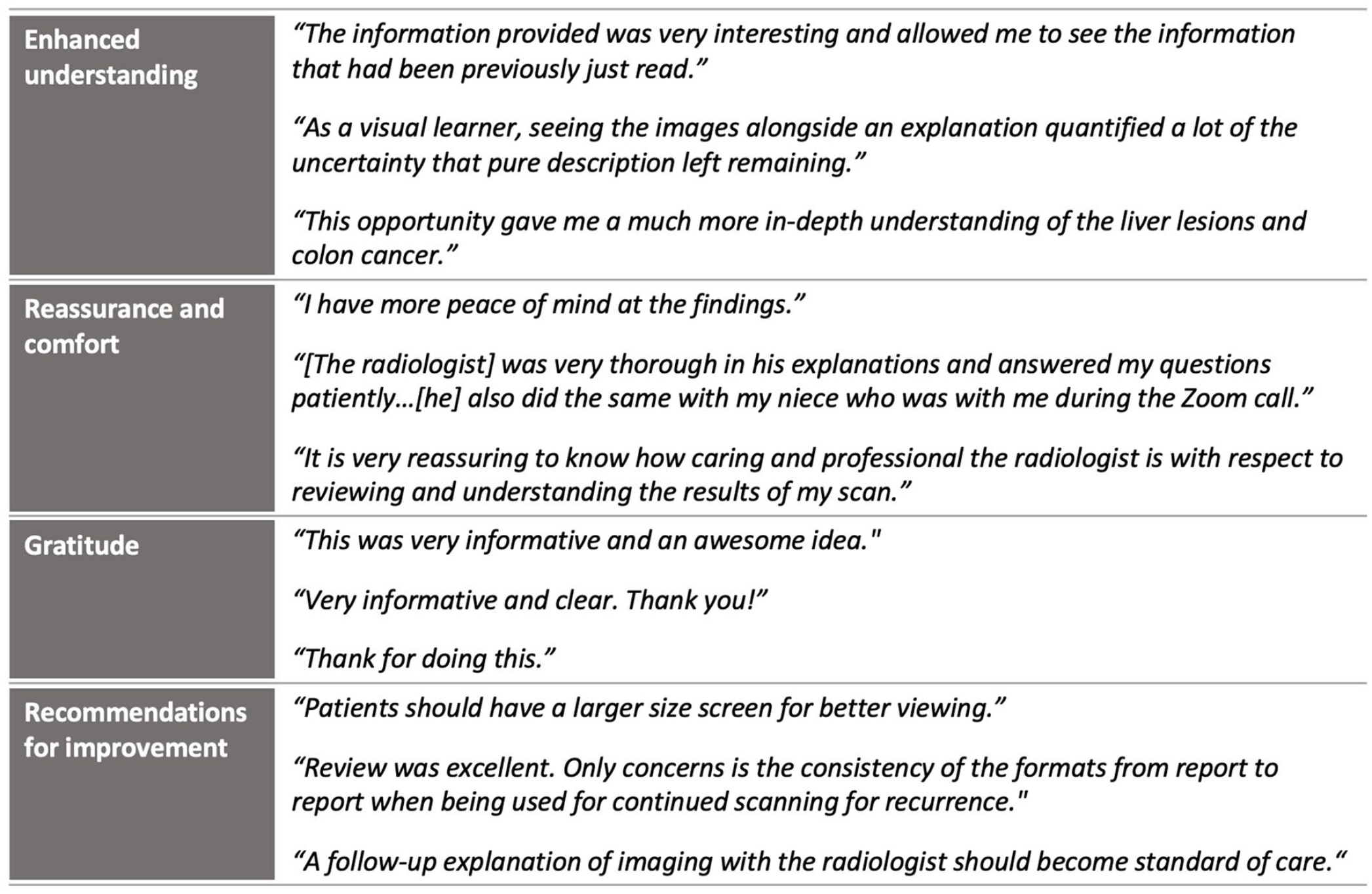
Themes and responses to the following survey question: “Do you have any comments to share about your experience?”
Discussion
Radiology reports traditionally serve as the primary means of conveying the results of diagnostic images between radiologists and referring physicians, often resulting in patients receiving a verbal, rather than visual, description of their condition.4,5 Patient-physician interactions provide an opportunity not only for knowledge translation, but for compassionate and individualized care. The results from this study suggest that VRCCs, which offer expert-guided visual aids, logistical convenience, and valuable patient-radiologist facetime, could significantly improve the patient experience. The enthusiasm evident in our participants’ comments is mirrored by the dramatic increase in appetite for virtual care nationally, 4 and can be contrasted against broader Canadian frustrations with access to primary and specialist care. 5
This study has limitations, including potential bias toward recruiting individuals already comfortable with virtual care, and recruiting radiologists who may be more inclined to provide a positive patient experience. Additionally, participants were not compared with a control group receiving the standard-of-care imaging results from their referring physicians. These limitations were driven largely by the lack of previous patient exposure to VRCCs, and the study’s resource constraints. Nevertheless, the current study provides a promising foundation for incorporating this novel concept across diagnostic imaging departments and radiology residency programs. Future initiatives should focus on recruiting a broader pool of participants, assessing patient outcomes and therapy adherence, and evaluating radiologists’ experience.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.