Abstract
Background
Nurses experience elevated rates of operational stress injuries (OSIs). This can necessitate taking leave from work and subsequently engaging in a workplace reintegration process. An unsuccessful process can have long term impacts on a nurse's career, affecting the individual, their family, and broader community, while contributing to nursing shortages. A knowledge gap regarding the workplace reintegration of nurses experiencing mental health challenges, impedes the development and implementation of initiatives that might increase the success of nurses reintegrating into the workplace. This scoping review explored the existing literature concerning workplace reintegration for nurses experiencing OSIs.
Methods
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) reporting guidelines were utilized. Three key search terms across six databases were employed followed by a qualitative content analysis of the resulting literature.
Results
Eight documents were included. The literature exhibited high heterogeneity in objectives, content, and article types. The content analysis revealed five themes: (1) recognizing stigma, (2) elements of successful workplace reintegration, (3) considerations for military nurses, (4) considerations for nurses with substance use disorders, and (5) gaps in the existing literature.
Conclusion
A paucity of programs, policies, procedures, and research exists regarding workplace reintegration for nurses facing mental health challenges. It is imperative to recognize that nurses may experience OSIs, necessitating mental health support, time off work, and operationally/culturally-specific assistance in returning to work. Innovative and evidence-based approaches to workplace reintegration are needed to enhance the retention of a skilled, experienced, compassionate, and healthy nursing workforce.
Keywords
Background
Nurses are under considerable pressure in a strained healthcare climate (Stelnicki & Carleton, 2021). A global nursing shortage also renders the nursing workforce unable to meet growing service demands. The far-reaching consequences of the nursing shortage includes longer wait times for patients, reduced quality of care, increased workload and stress for existing nurses, and a heightened risk of burnout (Baumann & Crea-Arsenio, 2023). Relative to the general population, nurses experience higher rates of psychological symptoms including those associated with post-traumatic stress disorder (PTSD) (Stelnicki & Carleton, 2021). While the COVID-19 pandemic exacerbated this (Fitzpatrick et al., 2022), potentially psychologically injurious events (PPIEs) and operational stress injuries (OSIs) were affecting nurses prior to this global event (Stelnicki & Carleton, 2021).
OSIs include a broad range of conditions, such as symptoms of PTSD, depression, anxiety, burnout, other comorbid disorders as well as moral injury (Lentz et al., 2021), that interfere with daily functioning (Canadian Institute for Public Safety Research and Treatment (CIPSRT), 2019). Nurses who experience OSIs may need to take leave from work to receive mental health support and rehabilitation (Jones, O’Greysik, et al., 2023). Returning to work after a period of physical or mental unwellness can be a complex process, especially when the workplace and profession involves austere conditions and considerable physical, cognitive, and mental health demands (Jones, Juby, et al., 2023; Jones, O’Greysik, et al., 2023). An unsuccessful workplace reintegration experience can have severe consequences on a nurse's mental health, their career, family, and the broader community while contributing to nursing shortages, and the loss of human capital within healthcare systems (Jones, Juby, et al., 2023; Jones, O’Greysik, et al., 2023). Despite the importance of a successful workplace reintegration of nurses on retention efforts, little is known about what return to work initiatives, policies, procedures, and programs are available and utilized for nurses experiencing OSIs. This poses a significant obstacle to the development and implementation of initiatives that may increase the workplace reintegration success of nurses experiencing OSIs.
The purpose of this scoping review is to explore the existing global literature regarding the return to work and workplace reintegration of nurses after OSIs and addressing the following research questions:
What techniques, interventions, programs, or systems are being utilized to assist with the workplace reintegration of nurses after traumatic work experiences and OSIs? What are the themes, barriers, facilitators, recommendations, and considerations in the evidence-based literature regarding workplace reintegration for healthcare workers affected by OSIs? What are the knowledge gaps and future directions of research that need to be addressed regarding workplace reintegration of nurses/healthcare workers affected by OSIs?
Methods
This scoping review employed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews reporting guidelines (PRISMAScR) (Levac et al., 2010; Tricco et al., 2018). A search strategy was developed based on a broad inclusion and exclusion criteria due to the suspected scarcity of the literature. The search consisted of an extensive list of keywords and subject headings covering three concepts: (1) workplace reintegration, (2) nurses, and (3) operational stress injury (Appendix A). These concepts were arrived at through consultation with key partners involved in the study, including nurses with lived experience, as well as other researchers with expertise of the research topic. The three concepts were then combined with the Boolean operators AND and OR. The researchers expanded the search to include similar terms. To better ensure relevance to the current nursing context, only English language peer-reviewed and gray literature published after 1990 was included (e.g., non-peer reviewed sources, books, journal articles, technical reports, policy articles, theses, etc). The search for literature occurred on December 11, 2022. The full search strategy is available in Appendix B. The searched databases included: MEDLINE (Ovid MEDLINE ALL), Embase (Ovid interface), the American Psychological Association (APA) PsycINFO (Ovid interface), CINAHL Plus with Full Text (EBSCOhost interface), Psych Article (EBSCOhost interface), and Scopus.
The study selection phase utilized Covidence Systematic Review Software (Covidence, 2022). A research team member (CJ) first exported all identified studies to Covidence where the entries were de-duplicated. Researchers (CJ, MV) then review the identified studies based on a broad inclusion and exclusion criteria. Literature that addressed the usability, feasibility, reliability, validity, acceptability, sensitivity, and efficacy of workplace reintegration initiatives and practices for nurses were included. Published work reporting on nurses with comorbid conditions, such as substance use disorders, was also included, as were any and all studies regardless of research method, or presence of positive, negative, or neutral findings. This broad inclusion criteria allowed for the research team to find and include as many relevant articles as possible. Articles were also excluded for some common reasons. This included the population in question being specific to the patients of nurses and not nurses themselves (e.g., non-medical military roles, prisoners of war, or professions including public safety personnel). Articles specific to physical health injuries or medical conditions were also excluded.
Two independent researchers (CJ, MV) evaluated the titles and abstracts of the remaining texts and compared them with the above inclusion/exclusion criteria. Members of the research team (CJ, MV, EO) then met to resolve any differences in decisions to include or exclude studies in the abstract evaluation phase. Due to the limited literature present at this stage, the research team pivoted to selecting those articles that addressed return to work or workplace reintegration related to the mental health of nurses more broadly. This pivot allowed the researchers to include more of what was already returned in the preliminary search.
During the full text read phase, at least two researchers reviewed each of the full texts of selected studies. Four researchers (CJ, MV, EO, KB) independently assessed the studies to determine their suitability for inclusion in the data extraction phase. An article's inclusion or exclusion into the data set for analysis required consensus from the research group. The reference lists of the included full-text studies were also reviewed for texts that the search may have missed. Reasons for exclusion at the full-text phase included the wrong population of study (n = 1), a lack of focus on workplace reintegration or return-to-work (n = 11) which included articles that focused on clinical interventions only. Finally, articles that the researchers were unable to retrieve in English (n = 1) and additional duplicates (n = 1) were excluded. The research team completed the data extraction of relevant details such as study characteristics, research question, methodology, and key findings from each of the final selected documents.
A qualitative thematic analysis of the resulting literature was originally planned by the research team (CJ, MV, EO, KB). Due to the small number of articles found, and the heterogeneous nature of the content, a qualitative thematic analysis was not indicated as the creation of deeper themes was not feasible. The heterogeneity also limited the utility of a narrative synthesis or summary of the articles. The resulting data indicated the need for the research team to pivot to a conventional content analysis with an inductive approach. This method is commonly used in the analysis and reporting with the goal of identifying and understanding themes, patterns, and relationships within the articles (Kleinheksel et al., 2020). This method was noted to be indicated when there is little or no information about the phenomenon under study, consistent with this topic. The analysis was guided by the steps of the Clinical-qualitative Content Analysis technique (Faria-Schützer et al., 2021). This included four researchers becoming familiar with data through in-depth reading, and then inductively identifying the words or phrases that embody the main concepts. Four researchers (CJ, MV, EO, KB) preliminarily coded the texts and assigned codes to content. They then organized axial codes into categories and subcategories based on how they relate or link to one another. Codes were refined through meetings and discussion, with disagreements reconciled through discussion, and a majority vote. The clinical-qualitative analysis presupposes and involves a critical reflection on the processes carried out at each step, with a reflexive lens utilized by researchers throughout the process. Finally, the results of the content analysis were synthesized and reported.
Results
The results of the search are shown in Figure 1. Eight documents were included in the review. Of the included texts, over half (n = 5) focused exclusively on the return-to-work of nurses affected by substance use disorder (SUD) while the remaining (n = 3) focused on the reintegration of nurses in the military context. One of the texts was an edited book (n = 1) while the rest were peer-reviewed journal articles (n = 7). These materials included a scoping review article (n = 1), qualitative studies (n = 2), a quantitative study (n = 1), mixed-methods studies (n = 2) and expert commentaries (n = 2). All literature (n = 8) discussed nurses from the United States although the published scoping review was produced by a Canadian researcher.
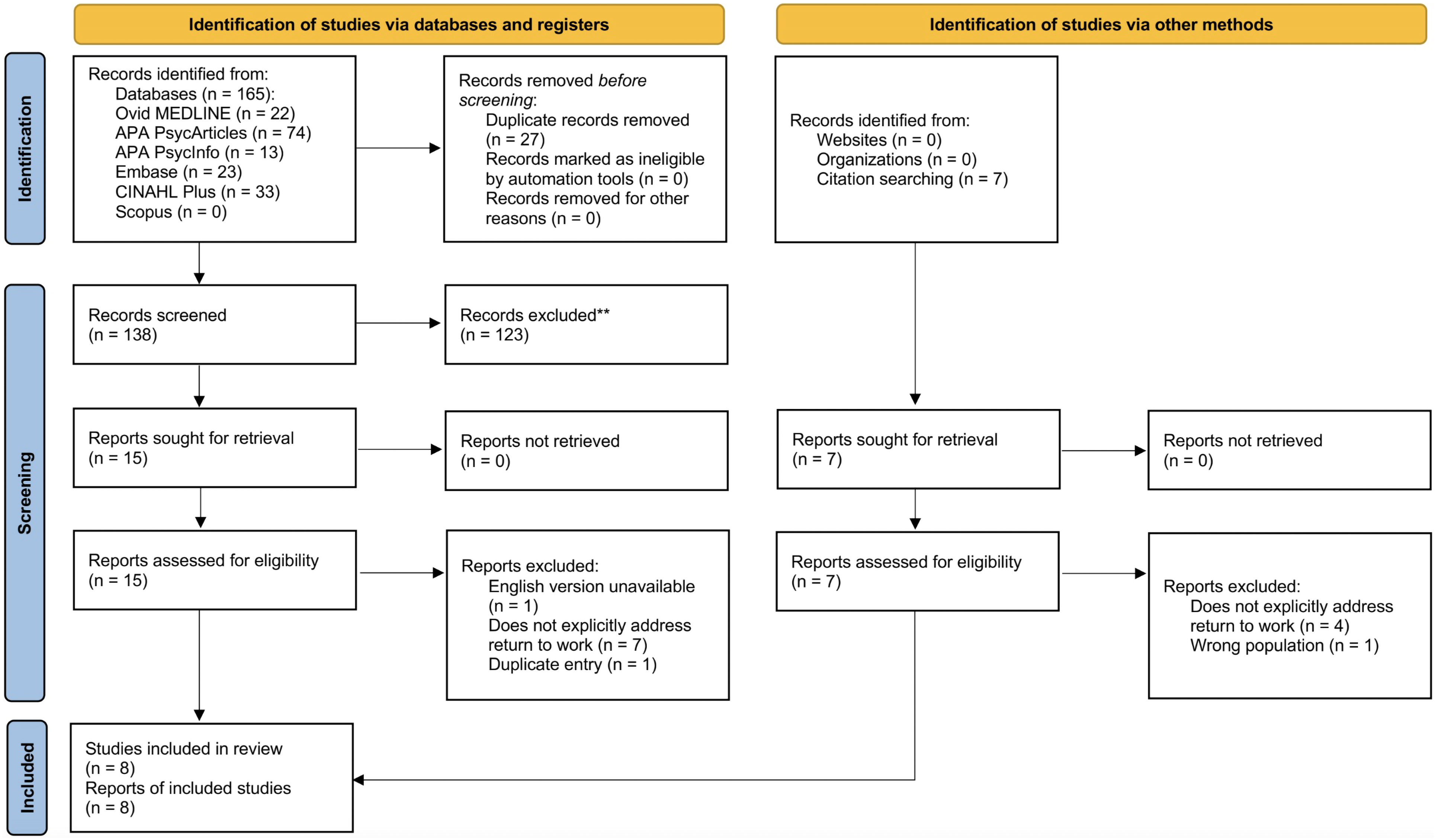
PRISMA 2020 flow diagram for new systematic reviews (Page et al., 2021).
Of the literature that involved original research studies (n = 5), 597 nurses participated with 72.4% identifying as women and sex and gender were similar. The reporting of gender, sex, and ethnicity varied among the studies. See Appendix C for further information on the characteristics of the eight texts, and associated demographic information for study participants.
Content analysis results
The content analysis yielded a number of themes. These included: (1) recognition of stigma, (2) elements of successful workplace reintegration, (3) considerations for military nurses, (4) considerations for nurses with SUD, and (5) gaps in the literature.
Recognition of stigma
Self, perceived, and real stigma affected nurses in their reintegration back to the nursing profession after experiencing mental health challenges (Angres et al., 2010; Bettinardi-Angres et al., 2012; Covell et al., 2020; Doherty & Scannell-Desch, 2015, 2017; Matthias-Anderson, 2016). This was true for both civilian and military nurses, and identified as a major factor for those nurses who experienced SUD (Angres et al., 2010; Bettinardi-Angres, 2020; Bettinardi-Angres et al., 2012; Covell et al., 2020; Doherty & Scannell-Desch, 2015, 2017; Hughes et al., 1998; Matthias-Anderson, 2016). Stigma around emotional labor, compassion fatigue, and PTSD was discussed as possibly leading to less help-seeking behaviors, underdiagnosing of mental health conditions, and, thus undertreating for these conditions (Covell et al., 2020; Doherty & Scannell-Desch, 2015; Matthias-Anderson, 2016). Additionally, stigma from self and others may contribute to affected nurses remaining in the workplace longer than was healthy (Doherty & Scannell-Desch, 2015).
Elements of successful workplace reintegration
Facilitators contributing to a successful return to work for nurses who have experienced mental health challenges were discussed in the literature. The workplace reintegration of nurses was noted to be multidimensional and intertwined with factors such as organizational and workplace support, the demands of the profession and workplace, clinical interventions, home environment and support, as well as relationships with others (Angres et al., 2010; Covell et al., 2020; Doherty & Scannell-Desch, 2015, 2017; Matthias-Anderson, 2016; Rivers et al., 2017). Family support, adequate time away from work, a tailored reintegration approach, widespread education, and peer support were identified as facilitators for workplace reintegration.
Considerations for military nurses
Military nurses had several unique factors that affected their mental health recovery and workplace reintegration after experiencing mental health challenges (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017). Military nurses often experienced the stress of combat zones, witnessed PPIEs, and provided critical care under extreme conditions (Doherty & Scannell-Desch, 2015, 2017). Consequently, their reintegration into the military and/or civilian workplace required specialized support (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017). Military nurses shared concerns that reporting their mental health challenges or asking for time away from their role would negatively impact their chance of promotion and career advancement (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017). One of the texts noted that regular force military members were given time prior to returning to work whereas reservists were expected to return to work immediately with little or no mental health support, highlighting the differences in experiences for nurses within the military context (Doherty & Scannell-Desch, 2015).
Military nurses reported feeling completely changed after deployments in their role as a military nurse (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017). They noted that reintegrating back into civilian nursing was challenging, with a lower level of tolerance for seemingly “trivial” patient complaints after what they had experienced in the austere conditions of deployment (Doherty & Scannell-Desch, 2015, 2017). They described having less patience for civilian nursing concerns, which contributed to feelings of not belonging amongst other nurses (Doherty & Scannell-Desch, 2015, 2017). Military nurses also reported that PTSD and trauma was often not adequately acknowledged during their reintegration back into their nursing role as well as the military at large (Doherty & Scannell-Desch, 2015). Some military nurses cited a lack of support from peers and leadership with a lack of communication. In their reintegration back to working as a nurse, they often had to come to terms with and identify new roles within the profession (Doherty & Scannell-Desch, 2015, 2017).They noted that they needed to be able to self-regulate and be aware of potential triggers and challenges when returning to work as a nurse (Doherty & Scannell-Desch, 2015). They also identified the importance of being self-motivated and insightful enough to seek mental health support as needed (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017). Good communication, consistency and knowing what to expect upon return and reintegration was key in successful return to work. One article noted that those military nurses who have experienced reintegration may also be extremely helpful in helping others prepare for deployment (Rivers et al., 2017).
Considerations for nurses experiencing SUD
There were a number of considerations specific to those nurses who were reintegrating back into the workforce after recovery from SUD. As previously mentioned, stigma regarding those with SUD was identified as a strong barrier to returning to work (Angres et al., 2010; Bettinardi-Angres, 2020; Covell et al., 2020; Hughes et al., 1998; Matthias-Anderson, 2016). In particular, the publications recommended education for peers to reduce stigma and improve reintegration outcomes (Covell et al., 2020; Hughes et al., 1998; Matthias-Anderson, 2016).
Specialized Alternative to Discipline programs were identified as being effective during the rehabilitation and workplace reintegration of nurses affected by SUD (Covell et al., 2020; Matthias-Anderson, 2016). Alternative to Discipline programs enable nurses to avoid disciplinary action and return to work under strict guidance and supervision while still ensuring public safety (Bettinardi-Angres, 2020). While the specifics of these programs vary across the United States (Angres et al., 2010; Bettinardi-Angres, 2020; Covell et al., 2020; Matthias-Anderson, 2016), the after-care monitoring component of these programs was noted to potentially cause some reintegration challenges depending on the workplace environment and type of substance dependance (Covell et al., 2020; Matthias-Anderson, 2016). If the dependence was to a substance that was accessible in the workplace, strict monitoring was more likely to be utilized (Bettinardi-Angres, 2020).
Gaps in the literature
The literature was consistent in noting that further research is required concerning mental health issues among nurses and their reintegration into the workplace. The scarcity of the literature was noted multiple times throughout the manuscripts and text. Gaps included a lack of literature regarding the working mechanisms of facilitators (e.g., peer support), in the reintegration of nurses after mental health challenges (Covell et al., 2020; Matthias-Anderson, 2016). Additionally, although nursing is a profession predominantly composed of women, considerations of gender were noted as not being addressed in the literature (Bettinardi-Angres et al., 2012; Covell et al., 2020; Matthias-Anderson, 2016). An examination of how specific behaviors resulting from SUD affect relationships and reintegration into the workplace was identified as another gap. The recommendations within the literature advocated for the rigorous study of initiatives, programs, policies, and procedures regarding workplace reintegration after mental health challenges (Covell et al., 2020; Matthias-Anderson, 2016). Alternative to Discipline Programs also have had very little evidence-based investigation to determine efficacy and effectiveness compared to other practices as well as across different programs of that type (Covell et al., 2020). Finally, the literature advocated for more research regarding military nursing who cared for injured military and civilians and may have engaged in or been in close proximity to combat scenarios (Doherty & Scannell-Desch, 2017; Rivers et al., 2017).
Discussion
The purpose of this scoping literature review was to explore the existing global literature regarding workplace reintegration initiatives for nurses after OSIs. The research team aimed to answer a series of research questions through the systematic process of locating and evaluating both evidence-based and gray literature. Although the research team was aware prior to initiating the literature review that the resulting search may be scarce, the extreme lack of literature on this topic was surprising. There was little mention within the search results of workplace trauma, PTSD, OSIs, moral injury, or PPIEs. As a result, the research team pivoted to texts that more broadly addressed return to work or workplace reintegration related to any mental health challenges among nurses. Interestingly, PTSD, anxiety, depression, and burnout were commonly combined under “comorbid conditions”, with little mention of how these conditions may affect a workplace reintegration process or if PPEIs may contribute to SUD. All the articles focused on nurses from the United States.
Despite the heterogeneity of the literature, the content analysis yielded some commonalities among the manuscripts and text that were organized into five themes: (1) recognition of stigma, (2) elements of successful workplace reintegration, (3) considerations for military nurses, (4) considerations for nurses with SUD, and (5) gaps in the literature. This allowed the research team to address the research questions as stated below:
What techniques, interventions, programs, or systems are being utilized to assist with the workplace reintegration of nurses after traumatic work experiences and OSIs? What are the themes, barriers, facilitators, recommendations, and considerations in the evidence-based literature regarding workplace reintegration for healthcare workers affected by OSIs?
Return to work policies and processes for military nurses and nurses experiencing SUD were the most represented in the published literature. For civilian nurses specifically experiencing SUD, Alternative to Discipline programs and policies were the only formalized initiatives targeting return to work throughout the included literature. Although these programs were portrayed as favourable in the cited articles, further evaluation of these programs is needed (Covell et al., 2020; Matthias-Anderson, 2016). It is also noteworthy that Alternative to Discipline Programs for nurses experiencing SUD, were inconsistent across jurisdictions (Covell et al., 2020; Matthias-Anderson, 2016). Direct comparison of different types of policies, programs, and procedures was not possible due to the scarcity of information.
Stigma was noted as a significant barrier to returning to work for nurses. Although nurses may be more educated on mental health conditions than non-healthcare personnel, stigma from self, colleagues, organizations, and communities was identified as a major barrier to reintegrating successfully back into the workplace. This is consistent with other publications regarding the workplace mental health of nurses (Jones, Juby, et al., 2023; Jones, O’Greysik, et al., 2023; Stelnicki & Carleton, 2021).
Notably, the literature that discussed workplace reintegration of military nurses acknowledged that their reintegration may have increased complexity and other unique barriers due to past PPIEs. Military nurses have a distinctive career experience that often involves additional barriers such as isolation from social supports, frequent relocation, environmental stressors, and proximity to situations where their safety, or the safety of close others, is compromised (Doherty & Scannell-Desch, 2015, 2017; Rivers et al., 2017).
Multiple facilitators were noted that support the return to work of nurses after mental health challenges. Firstly, the role of family in supporting nurses during their time off work and in the workplace reintegration process was highlighted for both military and civilian nurses alike. This is consistent with existing literature emphasizing the importance of connection with family and support networks for those healthcare personnel experiencing mental health challenges (Di Nota et al., 2021; Jones, Juby, et al., 2023). Secondly, the texts advocated for an adequate amount of time away from the workplace to address mental health challenges, especially when workplace stress may be a contributing factor. Although the amount of time off would vary based on individual needs and contexts, the literature generally advocated for more time off than many of the nurse participants had received. While there is no current consensus in the literature regarding the average or ideal time needed away from the workplace after a PPIE or a mental health challenge for specific professions, research indicates that prolonged time away correlates with a reduced likelihood of successful workplace reintegration (Cancelliere et al., 2016; Killip et al., 2022; Liao et al., 2001). Thirdly, a tailored, individual, and flexible approach to workplace reintegration was identified as an important facilitator in successfully returning to work after challenges with mental health. This is consistent with other publications regarding workplace reintegration of public safety personnel (PSP) and nurses (Jones et al., 2022; Jones, Juby, et al., 2023; Jones, O’Greysik, et al., 2023).
Adaptability around tasks, roles, duration of shifts, hours per week that meet the needs of the individual nurse were noted to facilitate a paced return to the profession while feeling supported by organizations. Additionally, advocacy for widespread education on mental health literacy with the goal of reducing overall stigma was apparent throughout the articles and consistent with recommendations across existing literature regarding workplace reintegration for nurses and PSP (Jones et al., 2022). Lastly, peer support was emphasized and encouraged throughout the literature. Specific to workplace reintegration, some literature exists regarding formalized peer-led return to work programs for other professions such as police, emergency medical services, and firefighters (Jones et al., 2022; Jones, Spencer, et al., 2023; Klose et al., 2017). Whether formal or informal, the importance of peer support was acknowledged and warrants further exploration.
What are the knowledge gaps and future directions of research that need to be addressed regarding workplace reintegration of nurses/healthcare workers affected by OSIs?
Numerous knowledge gaps were identified and emphasized in the literature. Recommendations for future research regarding return to work and mental health include investigation of workplace reintegration initiative delivery including the length and duration of the initiative, effect of facilitator type (e.g., peer to peer versus clinician supported), dropout rates, and other factors such that researchers can begin to build an evidence-based for this specialized area. Study of Alternative to Discipline programs and other initiatives used for nurses with SUD is yet needed to determine their efficacy. Additionally, research is needed regarding military nurses reintegrating into civilian life. We recommend conducting high-quality, mixed-methods research involving nursing participants from diverse countries, cultures, genders, and clinical contexts to ensure comprehensive insights and data. Ultimately, ensuring inclusivity and representation of diverse voices within various professional and operational healthcare settings is crucial for translating research into effective, safe, and efficacious workplace reintegration initiatives for as many nurses as possible.
Practice recommendations
The creation of evidence-guided policies, programs, and practices are recommended to support nurses experiencing mental health challenges in the workplace reintegration process. These initiatives would require context-specific development, design, implementation, fidelity, and evaluation efforts to ensure effectiveness. Initiatives must involve a formalized, well-communicated process that can be individually tailored to be person and profession-specific (Jones, Juby, et al., 2023). The incorporation of formal peer support is also recommended, consistent with the results of the literature review (Angres et al., 2010; Covell et al., 2020; Di Nota et al., 2021; Doherty & Scannell-Desch, 2015; Gamble, 2018; Jones, Juby, et al., 2023; Jones, O’Greysik, et al., 2023; Matthias-Anderson, 2016; Rivers et al., 2017). One of the first steps in the creation of workplace reintegration initiatives is likely the development and implementation of education aimed at partners, such as nurses, nursing students, nurse educators, leadership, administrators and policymakers, workers’ compensation organizations, varying levels of government, unions, and other healthcare providers engaged in the mental health care and rehabilitation of nurses (Jones, Juby, et al., 2023).
Limitations
The main limitation of this study was the low volume of resulting documents. This made analysis challenging, and meant that the original research questions could not be addressed as desired. Although the review process was calculated and rigorous, it is possible that relevant studies were overlooked and that additional research has been published before the release of this scoping review. Finally, the limits of aggregate data and specific nuanced details may have become generalized during the synthesis process.
Conclusions
Nurses may experience OSIs, requiring mental health support, time off from work, and assistance in returning to their profession. Successful workplace reintegration of nurses who have experienced OSIs and other mental health challenges could be a crucial step in their recovery and healing. Neglecting the development of policies, procedures, and initiatives to facilitate this process can lead to reduced retention in the profession, contributing to shortages of experienced healthcare professionals and a decrease in the quality of patient care. Focusing on the workplace reintegration of nurses may prove to be more cost-effective for healthcare systems compared to training and recruiting new staff.
Supplemental Material
sj-docx-1-cjn-10.1177_08445621241255419 - Supplemental material for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review
Supplemental material, sj-docx-1-cjn-10.1177_08445621241255419 for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review by Chelsea Jones, Michelle Vincent, Elly O’Greysik, Katherine Bright, Shaylee Spencer, Amy Beck, Douglas P. Gross and Suzette Brémault-Phillips in Canadian Journal of Nursing Research
Supplemental Material
sj-docx-2-cjn-10.1177_08445621241255419 - Supplemental material for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review
Supplemental material, sj-docx-2-cjn-10.1177_08445621241255419 for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review by Chelsea Jones, Michelle Vincent, Elly O’Greysik, Katherine Bright, Shaylee Spencer, Amy Beck, Douglas P. Gross and Suzette Brémault-Phillips in Canadian Journal of Nursing Research
Supplemental Material
sj-docx-3-cjn-10.1177_08445621241255419 - Supplemental material for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review
Supplemental material, sj-docx-3-cjn-10.1177_08445621241255419 for Workplace Reintegration Programs, Policies, and Procedures for Nurses Experiencing Operational Stress Injury: A Scoping Literature Review by Chelsea Jones, Michelle Vincent, Elly O’Greysik, Katherine Bright, Shaylee Spencer, Amy Beck, Douglas P. Gross and Suzette Brémault-Phillips in Canadian Journal of Nursing Research
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Government of Alberta Supporting Psychological Health in First Responders (SPHIFR) Grant Program (21SPHIFHR24-2) and Alberta Workplace Compensation Board Research Program.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
