Abstract
Background
Caring for older adults is among the most challenging issue of public health and social care systems in modern societies. By enhancing the nursing curriculum, nursing students will be qualified to provide gerontology care, and they will be acknowledging and working to eliminate ageism from the health care system.
Purpose
This study explores nurses’ and nursing students’ knowledge and attitudes in caring for older adults and addresses the factors contributing to nurses’ perspectives. It also examines the nursing curriculum's contributions to nurses’ knowledge and attitudes and provides suggestions aimed at reconfiguring the nursing curriculum for comprehensive gerontology nursing care.
Methods
A mixed-method research design was utilized, and quantitative and qualitative data were collected from 90 nurses and nursing students through an online questionnaire. Data were analyzed via SPSS and NVivo 12 software programs.
Results
The results revealed that most nurses possess neutral attitudes toward caring for older patients, and their knowledge ranged from average to above-average levels. Statistical analysis revealed no statistically significant difference between gender and nurses’ attitudes or between gender and knowledge. Similarly, there was no statistically significant difference between work status and nurses’ attitudes. Results showed a statistically significant positive correlation between nurses’ attitudes and knowledge level. This study demonstrated the positive impact of the Canadian nursing curriculum on nurses’ knowledge and attitudes.
Conclusion
The current study recommends providing gerontology nursing courses as a mandatory separate course in nursing education to enhance nursing students’ knowledge and skills for high-quality gerontology nursing care.
Keywords
Background and purpose
Statistics of older adults and their health problems
The world population is rapidly ageing, and individuals’ life expectancy is increasing due to medical advances and lifestyle improvements. The World Health Organization [WHO] (2018) indicated that from the year 2015 to 2050, people are and will continue to age throughout the world, and the percentage of people over 60 years of age will increase from 12% to 22%. Similarly, the Canadian Institute for Health Information (2017) reported that over the last 40 years the older adults who are 75 years old and older are rising at a faster rate. Additionally, Statistics Canada reported that Canadian older adults aged 75 or more are expected to increase dramatically in each province and territory between 2017 and 2037 (e.g., Ontario 2.1 times, Quebec 2.0 times, Alberta 2.8 times, Yukon 2.9 times, and British Columbia 2.1 times) (Ministry for Seniors and Accessibility, 2017). Furthermore, King et al. (2013) estimated that currently, individuals over 65 years of age comprise 65% of hospital patients and have four times the rate of hospitalizations relative to many younger people. Also, 26% of all outpatient appointments and 38% of all emergency room admissions are older people, while the older adults register for 85% of home-care trips, and 90% of nursing home-use stays—this statistic is expected to rise as the population continues to grow.
As the aging population increase, these individuals can present with numerous health problems (Vann, 2016). The WHO (2017) reported that physical, neurological, and psychological diseases among older population account for 6.6% of all illness in this age group and around 15% of the older people aged 60 and over complain of a mental disability such as depression and dementia. Moreover, Vann (2016) affirmed that cerebral vascular stroke, hypertension, asthma, pneumonia, cardiovascular disorders, obesity, respiratory diseases, osteoporosis, Alzheimer's, influenza, and neurovascular disorders are the most common chronic health issues among the older adults. According to the WHO (2020), people 65 years of age or older are more likely to have a severe infection of coronavirus (COVID-19), as their immune systems are changing with age, and it is more challenging to control pathogens and viruses. Therefore, older people are more likely to have chronic health problems such as acute pneumonia that make it more challenging to live with and recover. In addition, WHO (2020) and Centers for Disease Control and Prevention (CDC) (2020) stated that individuals of all ages can be infected with the latest COVID-19 but, older patients and those with pre-existing medical problems such as asthma, hypertension, diabetes, and cardiac disease are most vulnerable to severe complication or death from the virus. As per recent Statistics Canada reports, Canadians aged 85 and up account for more than half of the excess deaths recorded during the COVID-19 pandemic (Neustaeter, 2020). Therefore, it is apparent that older people require close monitoring for their health status to reduce the complexity of their chronic illness and to remain safe from communicable diseases (Vann, 2016).
Role of nurses
Nurses have a vital role in caring for various categories of individuals in society as they provide care and support to children, adolescents, adults, and older adults. In addition, the education of patients, families, and the community is a nurse's primary function (International Council of Nurses, 2002). Nurses have been described as the primary health care resource ideally prepared to fulfill the demands of an aging population in the health care system (King et al., 2013). Deasey et al. (2014) also contended that nurses play a crucial role in providing medical services for older patients with a supportive environment and positive outcomes. The WHO report (2017) stipulates that the well-being and mental health of older people is essential, similar for any other lifetime, and nurses should be aware of older adults’ health needs and health problems. According to Wagner et al. (2014), because older people are the most frequent users of the Canadian healthcare system, it is vital that nurses be educated to fulfill this population's health care needs. Similarly, Rush et al. (2017) stated that well-prepared gerontological nurses are essential for providing high-quality care for older patients.
Nurses’ attitudes, knowledge and perception toward older adults
According to the literature, caring for the older adults is among the most challenging issue of public health and social care systems in modern societies. For example, Liu et al. (2012) reported that nurses view older people as a burden, as they found caring for older adults annoying. Dikken et al. (2017) asserted that some nurses have a negative attitude towards older patients, while King et al. (2013) claimed that new studies found that even in situations where nursing graduates have positive attitudes, they usually tend not to deal with older patients. As a result, there is a severe lack of caregivers with experience in gerontological nursing care. Consequently, older people may suffer from different forms of discrimination from society in general, and in particular, from the health care sector. Wyman et al. (2018) also revealed in their study that nursing students showed a common lack of interest in working with older adults. These researchers observed that in addition to the communication quality, care provided to older individuals is accompanied by undesirable attitudes against old age. To clarify, the nurses did not engage the older persons in their treatment plan, and nurses spoke in a patronizing tone when communicating with older patients. Congruently, Çelik et al. (2010) indicated that some Turkish nursing students have negative attitudes toward the older people; however other students mentioned that they were sympathetic and treated older patients kindly while caring for them, but they had language barriers and relationship difficulties with them. Another study conducted in Iran confirmed that nurses possess negative attitudes toward older patients at public hospitals in Ilam city (Arani et al., 2017). Topaz and Doron (2013) argued that nurses’ attitudes are changeable and vary from country to country. For instance, they discovered in their research that nurses’ positive reactions toward older adults’ care are reported by several researchers in the United States, Jordan, and Australia. Nevertheless, negative attitudes toward the older patients were recorded in many hospitals in Sweden and Ireland. Deasey et al. (2014) revealed from their study that culture, religion, social structures, and the beliefs of individual nurses affect the care of older patients.
It is noteworthy to mention that the literature did not mention the leading causes behind this discrimination and negative attitude towards older patients among health care providers. Rush et al. (2017) affirmed that nurses’ attitudes towards gerontological nursing care are complex and contradictory, and more research on the attitudes of nurses are required to establish a solid evidence base. They also added that a review of studies on the attitude of nurses toward caring for older adults is essential for identifying the needs of nursing staff and improving the quality of care. As well, Dikken et al. (2017) argued that “identifying positive and negative attitudes toward older patients is very important to improve the quality of care provided to them” (p. 6). Liu et al. (2012) contended that healthcare practitioners’ attitudes influence the standard of care provided. Based on recent studies, nursing students had a positive perception of older adults and aging; however, most nurses possess negative attitudes concerning the characteristics and complexities that come with aging. There is a need for comprehensive training of nurses and nursing students on how to care for the older population, possibly in separate courses, to improve older individuals’ quality of life (Attafuah et al., 2022). According to Alsenany (2007), student nurses lack fundamental knowledge of aging, have misconceptions about caring for older people, and have little interest in working in long-term care facilities. Similarly, according to a cross-sectional study of registered nurses (RNs) and registered practical nurses (RPNs) in Ontario, many Canadian nurses had a positive attitude toward older individuals. Meanwhile, most Ontarian nurses had no plans to specialize in gerontological nursing or work in long-term care facilities (Smith et al., 2022). In addition, Wagner et al. (2014) revealed that gerontological content in the Canadian baccalaureate nursing school curricula remains relatively low across the country. Canadian research shows that nurses have less accurate knowledge about aging than other health professionals, and nursing students are not reluctant to learn about older adults. Thus, gerontological content should be thoroughly and adequately included in the Canadian nursing curriculum (Hirst & Lane, 2016). Baumbusch and Andrusyszyn (2006) stated a deficit in the Canadian nursing curriculum since only 8% of clinical hours focused on caring for older individuals, and only 5.5 percent of students decided to care for older adults. Another Canadian study revealed that despite gerontological nursing standards and competencies, nurses dealing with older patients frequently adopt ageist ideas, and nursing curriculums do not include enough anti-ageism content (Dahlke et al., 2021a, 2021b). Therefore, it is essential to assess nurses’ attitudes toward older patients to identify their perceptions and actions toward the older population. As well, it is important to obtain nurses’ assessment of the nursing curriculum to identify knowledge and skills deficits. In that way, reforming nurses’ attitudes can be a focus of the curriculum, thus resulting in an improved standard of health care for older people.
The nursing curriculum
Nursing curriculum is described as all the learning that is developed and supervised by the nursing school, whether it is done inside or outside of school, individually or in groups. Traditionally, it has been skill-based and test-driven, with a strong emphasis on behavioral objectives to assess techniques and processes. Curriculum objectives have developed throughout time, and nurses are today trained and prepared to make critical decisions and practice innovatively (Wright & Wosinski, 2017). To ensure safe, competent, and ethical nursing, all Canadian provinces mandate entry-to-practice competencies before a nurse practice nursing (The College of Nurses of Ontario (CNO), 2019).
Gerontological competencies for entry to practice
The Canadian Association of Schools of Nursing (CASN) (2017) developed the entry-to-Practice Gerontological Care Competencies for Baccalaureate Programs in Nursing. These competencies describe the fundamental knowledge, skills, and attitudes that new registered nurses in Canada should have while caring for older adults and their families. The competencies’ objective is to guide nurse educators and curriculum development. Nursing graduates should acquire these competencies during their studies. According to Dahlke et al. (2021a, 2021b), Canadian competencies frameworks for health and social service education have not been incorporated into accreditation processes or curriculum revision plans due to insufficient faculty expertize in gerontology nursing. In addition, Canadian health educators are unaware of the published gerontological competencies that could help them evaluate and improve curricular content.
Reforming nursing curriculum
Curriculum development has a broader perspective because it is not just about students, educators, and schools but also about the community's growth (Mary, 2014). As the curriculum significantly impacts students’ academic performance, reforming nursing education by incorporating the requisite knowledge and skills specific to gerontological care and nurses’ training is essential to improve nurses’ beliefs and reduce ageism. By enhancing the nursing curriculum, nursing students will be qualified to provide care for older adults, and they will be acknowledging and working to eliminate ageism from the health care system (Wyman et al., 2018). Deasey et al. (2014) asserted that nurses’ attitudes are strongly related to their perception of the aging process. Increased knowledge and understanding of nursing students about aging processes will help them identify deterioration in older individuals, deal with older adults’ physical and psychological problems, and promote supportive attitudes towards older adults.
Additionally, Topaz and Doron (2013) also affirmed that nursing curricula should integrate information about healthy aging and prevent focusing mainly on age-based illnesses. Within our contemporary health care systems, increased aging awareness along with modern pedagogical approaches are required to enhance nursing students’ knowledge and perceptions toward older people care to reduce the ageism rate within the health care system and society. According to Cary et al. (2017), ageism is a multifaceted stereotype that includes positive and negative perceptions of older people. Some of the positive perceptions of older individuals could, in fact, be benevolent ageism. For example, high warmth or helping behavior can be passive harm or benevolent ageism as hostile ageism. So, it is essential to teach nursing students how to differentiate between positive perception and benevolently ageist action to remove ageism from the health care system and community.
Based on Bandura's self-efficacy theory (1977), nursing instructors can inspire, encourage, and direct their students and empower them with the information and practices related to gerontology care through role modeling approaches. Deasey et al. (2014) claimed that supportive instructions, encouragement, feedback, and recommendations from nursing educators about the practice of nursing students might increase their self-confidence, thus leading to positive older adults’ care experiences. Nurses must be qualified with gerontological knowledge and skills to decrease or avoid further deterioration in older adults’ health status. Furthermore, nursing students should be trained to deal with older people's health needs. Hands-on experience and brief on-site training sessions are the most significant ways to learn how to care for older persons (Fox et al., 2016). According to Every Nurse (2019), gerontology nursing programs should provide nursing students with knowledge and skills that allow them to deal with stressful events such as patients’ deaths and enable them to recover from depression quickly. Likewise, the nursing profession's development is a primary aim of nursing education, and the nursing profession's enhancement depends on the advancement of nursing education (Carson-Newman University Online, 2018). Hence, reforming the nursing curriculum can improve nursing beliefs and the nursing profession. Assessment of nurses’ attitudes may help to direct curriculum designers in developing nursing curricula to provide society with highly qualified nurses. Older people are vulnerable and need more love and attention together with more knowledgeable and skillful healthcare providers.
Dillon (2009) noted that the curriculum consists of multiple elements such as students, content, and pedagogy that educators and curriculum designers should consider and follow when developing a curriculum. Curriculum designers need to place the programmatic and implemented curriculum content into context to carefully bring the teaching-learning process to students’ realities, including the cultural, historical, political, and geographical nature of the society. Dillon (2009) also stated that curriculum contextualization is essential, as contextualization of the curriculum connects all the elements which make up the curriculum, such as the content, pedagogy, teacher, student, milieu, activities, and students’ evaluation methods. Thus, curriculum developers need to contextualize the three levels of the curriculum—institutional, programmatic, and implemented—because, without contextualization, the curriculum becomes challenging to understand. Contextualization helps students apply concepts and skills they studied while engaging with older patients. Mouraze and Leite (2013) asserted that the curriculum's contextualization allows teachers and students to connect theory to practice and give students meaning and value to what they learn in school. Besides curriculum contextualization, the accountability of nursing instructors for students’ performance is crucial. Tilley and Taylor (2013) contended that accountability and standardization are required for clearly understood curriculum conceptualizations such as text, ministry documents, and materials that teachers are responsible for implementing in the neo-liberal age. Moreover, from my perspective, nursing students should also learn about social justice, human rights, and the disadvantages of discrimination, especially ageism. I trust that equity should be present first at school, and the primary function of the nursing educator and the curriculum designer is to teach students about fairness and the benefits of social justice for individuals and society. Through the learning process, students can learn unintended undesirable attitudes from their educators, curriculum contents, or school policies—or through what is referred to as a hidden curriculum. Alsubaie (2015) defined the concept of the hidden curriculum as “the unspoken or implicit values, behaviors, procedures, and norms that exist in the educational setting” (p. 125). For example, when the nursing curriculum lacks information related to gerontology nursing care or nursing instructors allocate their students to younger adults in the clinical areas and ignore aged people, this sends the students implicit messages that older people are not as significant as youngsters.
Consequently, this will negatively influence the nursing students’ beliefs and behaviors toward the older population. Thus, there is a need to change the educational policies, pedagogical methods, and educators’ teaching strategies and modify curriculum content to enhance students’ performance and attitudes. Tilley and Taylor (2013) argued that social justice education should be reflected in the curriculum's content and pedagogy used by teachers. Besides, it is not enough to reform the current curriculum or the students’ background and teachers to achieve social justice and equality. Instead, social justice in education is an active movement to examine the curriculum, educational policy, and administrative strategies that maintain inequities in classrooms. Deng (2010) also argued that “significant curricular change requires systems change which entails impacting change across the institutional, programmatic, and classroom levels of the curriculum” (p. 9). By adding new curricular goals and expectations, curricular reform may help develop the gerontology course structure, content criteria, pedagogy, and evaluation methods. Therefore, this study aims to (a) assess current nurses’ and nursing students’ knowledge and attitude toward gerontology nursing care, (b) examine the nursing curriculum's contributions to nurses’ knowledge and attitudes, (c) explore the needed knowledge and skills for older adults’ care, (d) identify gap(s) in the nursing curriculum, and (e) provide suggestions to reform the nursing curriculum.
Significance of the study
This study's findings contribute to the current body of literature related to the knowledge, and attitudes of Canadian nurses and nursing students toward gerontological nursing care. This study addresses the gap in attitudes toward older adults’ care among Canadian nurses and nursing students. The research also enriches the existing literature on Canadian nursing curriculum's impact on nurses and nursing students’ attitudes and knowledge. Based on the results, nursing students’ attitudes and knowledge may be enhanced for high-quality gerontology nursing care through recognizing knowledge, practical skills, and communication skills gaps in the nursing curriculum. This study also contributes insights into nursing programs by providing information and data to curriculum developers, nursing instructors, and nursing administrators that can guide them through designing the appropriate nursing curriculum.
Methods and procedures
Research design
A mixed-method research design (convergent parallel design) was utilized to achieve the purpose of the study. According to Creswell (2013), a mixed-method approach is a research method used in the social, behavioral, and health sciences in which researchers gather, examine, and integrate quantitative and qualitative data into a single analysis to address their research questions. Quantitative and qualitative data were collected simultaneously and independently from ninety nurses and nursing students through an online questionnaire using a convergent parallel design and then results were analyzed, giving equal weight to the quantitative and qualitative data. Data sources for the study entailed three main surveys that measured nurses’ practical experience, knowledge, general opinion, and attitudes towards caring for aging populations. The research tools effectively gathered both quantitative (Likert scale questionnaire) and qualitative (open-ended questions) data. Qualitative data provided more details about the quantitative data and helped inform the interpretation of the quantitative data. Both data were compared to highlight similarities or inconsistencies in order to gain deeper insights and perspectives. Using different methods allows for triangulation or confirmation of findings (Creswell et al., 2003; Sauro, 2015).
Data source
Data were collected online utilizing the following tools: (1) Demographic questionnaire was used to collect data related to nurses’ characteristics such as age, gender, current work status, educational qualifications, and years of experience, as well as any formal training in caring for the older patients; (2) The Older Patient in Acute Care Survey—United States (OPACS-US), which contains two sections—section A measures nurses’ practical experience, and section B measures nurses’ general opinions of caring for older patients. This tool was tested for validity and reliability in the USA by Dikken et al. (2017). Scoring system for (OPACS-US): Items with a star * should be reverse coded (5 = 1, 4 = 2, 3 = 3, 2 = 4, 1 = 5), Sum all scores on the OPACS-US section A, and divide the sum score of section A by 28 (is average score on a scale from 1–5); sum all scores on the OPACS-US section B and divide the sum score section B by 34 (is average score on a scale from 1–5). Interpretation: 1 = Very negative, 2 = Negative, 3 = Neutral, 4 = Positive, 5 = Very positive. (3) Knowledge-about-Older-Patients Quiz (KOP-Q) for nurses is designed to measure nurses’ knowledge regarding caring for the older adults and was tested for validity and reliability in the USA by Dikken et al. (2017); and (4) Open-ended questions designed by the researcher to explore participants’ source of knowledge and attitude in terms of geriatric care. These include: How has the nursing curriculum contributed to nurses’ knowledge in caring for geriatric patients? and How has the nursing curriculum contributed to nurses’ attitudes in caring for geriatric patients?
Participants
Ninety participants, including nurses and nursing students with different work experiences were recruited for the study. Forty-three nursing students and 47 nurses (82 females, 8 males), ages ranging from 20 to 40+ participated in this study. Most participants (63.3%) had received training for older patient care. Criteria for the participants’ inclusion in this study were: (1) undergraduate nursing students from universities and colleges, (2) new nursing graduate with less than one year of work experience, (3) new nursing graduate with 1 to 5 years of work experience, and (4) nurses with extensive work experience (more than five years).
Setting
Participants were recruited from different nursing programs (colleges and universities), long term care facilities, the Canadian Nursing Students’ Association, and hospitals all over Canada. Given the context of the COVID-19 pandemic, participants were recruited online via their organizations and affiliations. I chose to include nurses in practice in hospitals, long-term care homes, and nursing students in training in colleges and universities, as well as those belonging to professional organizations. These locations were selected as they provided a range of participant experiences, nursing program curriculums, and are representative of the population of nurses and nursing students.
Procedure
Following ethical approval, the administration of different nursing programs including universities and colleges, hospitals, Canadian Nursing Students’ Association, and long-term care homes for older adults in Canada were contacted via publicly available email to recruit study participants. Administrators were located and selected using the public websites of universities, colleges, and hospitals in Canada. The nature and importance of the study were explained, as well as a letter of information with an introduction about the research and its potential contribution. All information about the study was forwarded by administrators, and potential participants were instructed to contact the researcher regarding questions about the study. Participants were invited to complete the survey through Qualtrics, a secure online survey platform. Participants’ privacy and confidentiality were protected as survey responses were collected anonymously. Recruitment of study participants was also facilitated through social media and snowball sampling. The study link was posted on WhatsApp and Facebook groups, requesting voluntary nurses and nursing student participants. Nurses and nursing students who were interested in participating were able to access the link, the letter of information and the surveys. Upon completion of data collection, data was computed and analyzed.
Data analysis
Likert scale survey responses were imported and tabulated in Microsoft Excel and analyzed via SPSS software program using descriptive, and inferential statistical analysis. Frequency distribution and percentages, arithmetic mean as an average that describes the central tendency of observations, standard deviation as a measure of dispersion of results around the mean, T-test and Chi-square were used to analyze the obtained data. In addition, the Pearson correlation coefficient test was used to measure the strength and direction between variables. The level of significance was considered at the 5% level (p = .05). Qualitative data obtained from open-ended question were analyzed using descriptive themes, and coding using NVivo 12 data analysis software to address the study's purposes (Miles et al., 2014). Using the themes identified by the NVivo analysis, participants’ responses to the open-ended questions were thematically analyzed. The themes were examined for frequency of occurrence among participants to illustrate similar comments, opinions, concerns, and suggestions.
Results
Part A: quantitative survey findings
In total, ninety participants completed the surveys. Table 1 (nurses’ demographic data) lists the participants’ age, gender, marital status, work status, years of experience, and whether they received gerontology care training. Study participants consisted of 90 nurses, with ages ranging from 20 up to 40+ years old, with more than half of the study group (59.9%) between 20 to 25 years old. Females comprised 91.9% of the participants. Most of the sample were either single (60%) or married (40%). In relation to their current work status, more than half of the participants were working (52.2%), while (47.8%) were studying, and two-third of all participants (63.3%) received training for gerontology care. In terms of work experience, 43.3% of participants had no work experience, while the rest had varying years of work experience with a mean + SD of 8.4 + 9.6.
Nurses’ Demographic Data, Grand Total the Older Patient in Acute Care Survey (Attitudes)and Knowledge About Older Patients Frequencies and Percentages among the Study Group (n = 90).
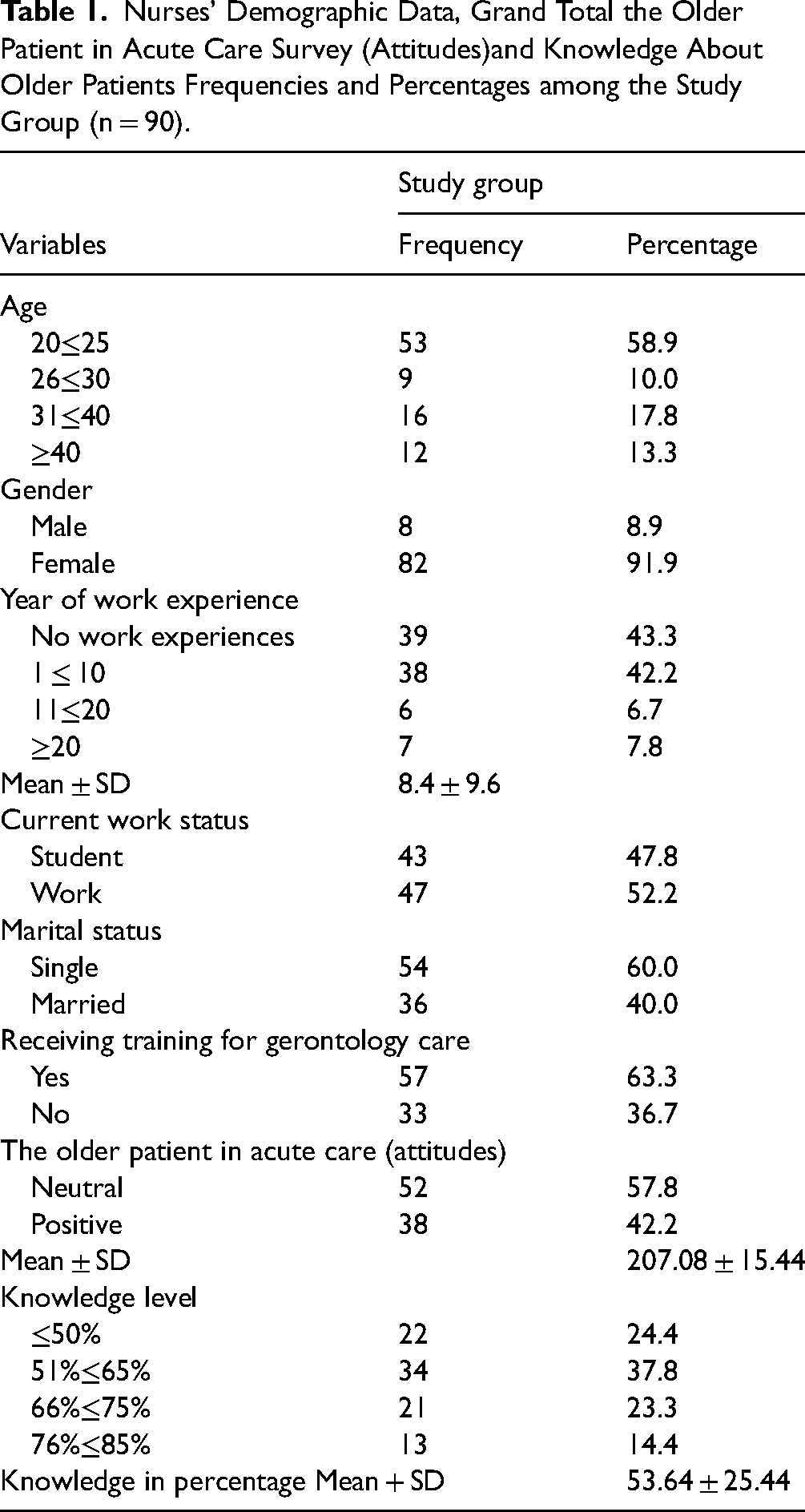
Table 1, which illustrates findings from Section A and B of the OPASCS-US and KOP-Q, shows that 57.8% of the study participants have neutral attitudes toward caring for geriatric patients, while 42.2% have positive attitudes with a mean + SD of 207.08 + 15.44. In gauging participants’ knowledge about older patients, less than half of the study participants (37.8%) had an average level of knowledge regarding gerontology care. In contrast, the remaining participants had relatively high, above average, or limited levels of knowledge (14.4%, 23.3%, and 24.4%, respectively) with knowledge in percentage mean score + SD of 53.64 + 25.44.
In exploring relationships between variables—age group, gender, work status, attitudes, and level of knowledge—a statistically significant relationship between age group and level of knowledge with p = .01, and a statistically significant relationship between work status and level of knowledge with p = .02 were noted. There was no statistically significant relationship between gender and knowledge level with p = .38 and no statistically significant relationship between work status and nurses’ attitudes, with p = .77. Additionally, there was no statistically significant relationship between age and attitudes with p = .52 (Table 2). Finally, findings revealed a statistically significant positive correlation between nurses’ attitudes and total knowledge level with r = 0.219 at p = .04. However, there was no statistically significant correlation between nurses’ attitudes and the number of years of experience with r = 0.09 at p = .39, and no statistically significant correlation between nurses’ knowledge level and the number of years of experience with r = 0.194 at p = .07 (Table 3).
Relationship among Participants’ Age Group, Gender, Work Status and Knowledge Level and Older Patient in Acute Care Categories (Attitudes) (N = 90).
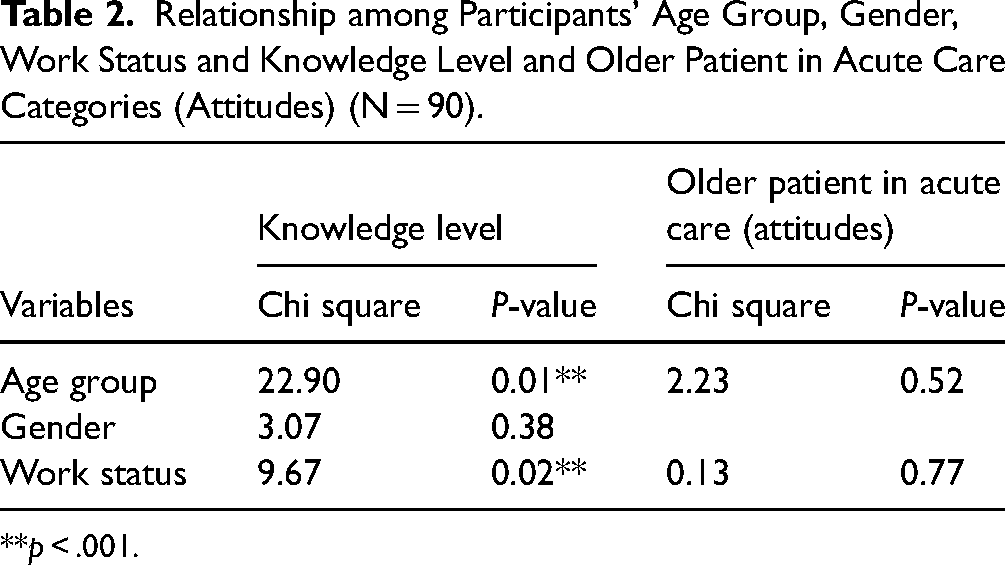
**p < .001.
Correlation Between Total Score of the Older Patient in Acute Care, Knowledge Level, and Number of Years of Experience (N = 90).
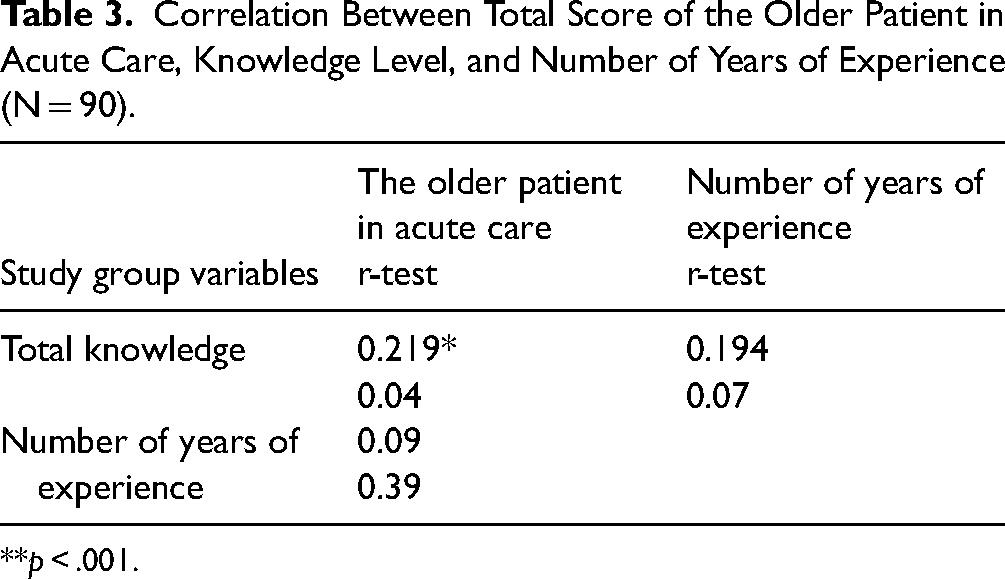
**p < .001.
Part B: findings—open-ended questions
Findings from the contribution of the nursing curriculum to the knowledge of nurses in caring for older patients highlighted that most nurses (62%) reported that the nursing curriculum is helpful and had a significant influence on their knowledge in terms of providing them with the required knowledge and skills that empowered them to provide comprehensive nursing care to the aging population (Figure 1). Nurses commented: “I feel more equipped to handle geriatric problems due to the nursing curriculum” and “The nursing curriculum has prepared me for the care of the elderly by shedding light on the normal aging process, and common health challenges among the elderly”.
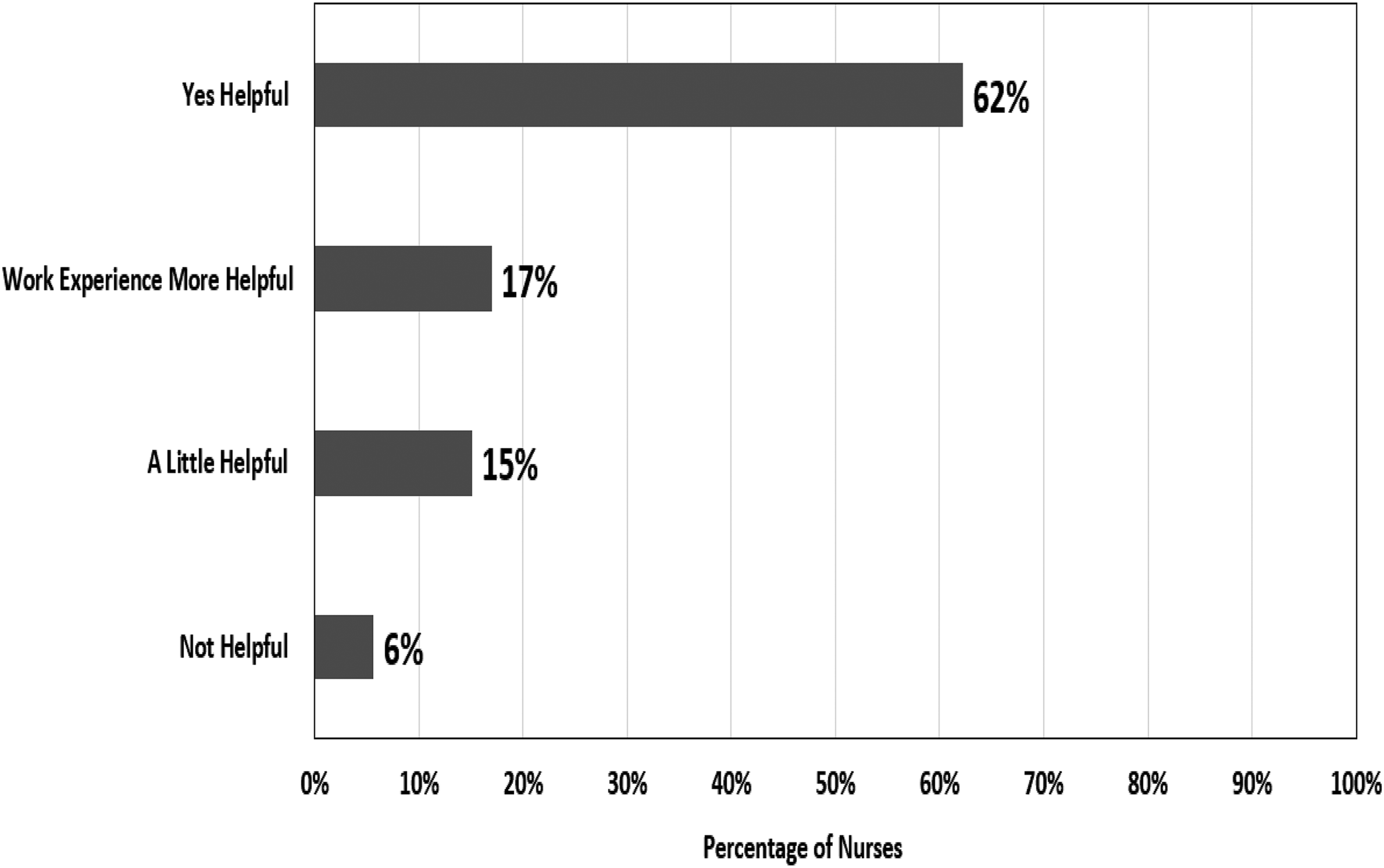
Nurses’ opinions of the contribution of the nursing curriculum to their knowledge.
However, some nurses reported that the nursing curriculum was either a little helpful or not helpful, and that their work experience provided them with the knowledge and skills and helped them more in terms of positively engaging with older patients. Nurses commented: “Nursing curriculum doesn't help me much but my experience as a nurse for past 8 years helped me a lot” and “Not enough knowledge when you are newly graduated, learn process start when you are hands-on”.
In terms of the contribution of the nursing curriculum to nurses’ attitudes toward older people care, study findings reveal that for most nurses (74%), the nursing curriculum positively impacted their attitudes. Nurses commented: “Education on geriatric patients influences my attitude and gives me more empathy”, and “The nursing curriculum contributed to my attitude in the care of geriatric patients as we have been educated on treating all patients with dignity”. In contrast, a small percentage of nurses (14%) said that the nursing curriculum had a minor influence on their attitudes, and other nurses (12%) reported that clinical work experience had more impact on their attitudes toward caring for older adults (Figure 2). Nurses commented: “I honestly think the nursing program focuses too much on geriatric deficits, and not enough on their strengths, a lot of seniors will not fit the standard mold that we have been taught”; and “Practical experience helps more, I think attitudes are formed more once working with the population”.
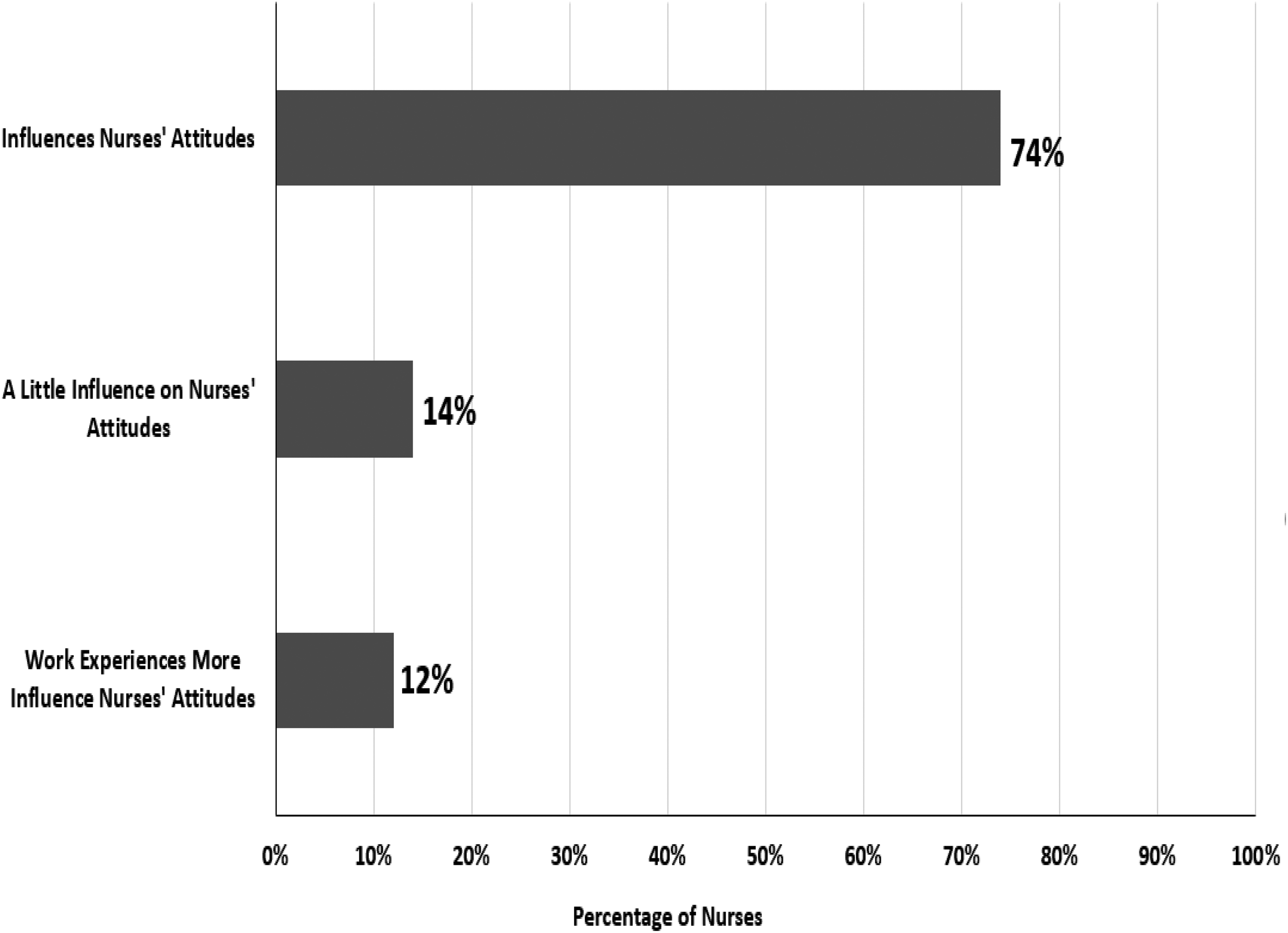
Nurses’ account of the contribution of the nursing curriculum to their attitudes towards the elderly.
Figure 3 illustrates how the nursing curriculum contribute to nurses’ attitudes. The most significant theme identified by nurses (39%) is that the nursing curriculum had a positive impact on nurses’ attitudes by increasing nurses’ empathy, compassion, and respect toward older people. This was followed by increasing nurses’ awareness about older adults’ personalities and cognitive impairment (34%), followed by reducing bias and stereotypes (15%), and finally, a small group of nurses (12%) stated that work experience helped them more to deal positively with older patients.
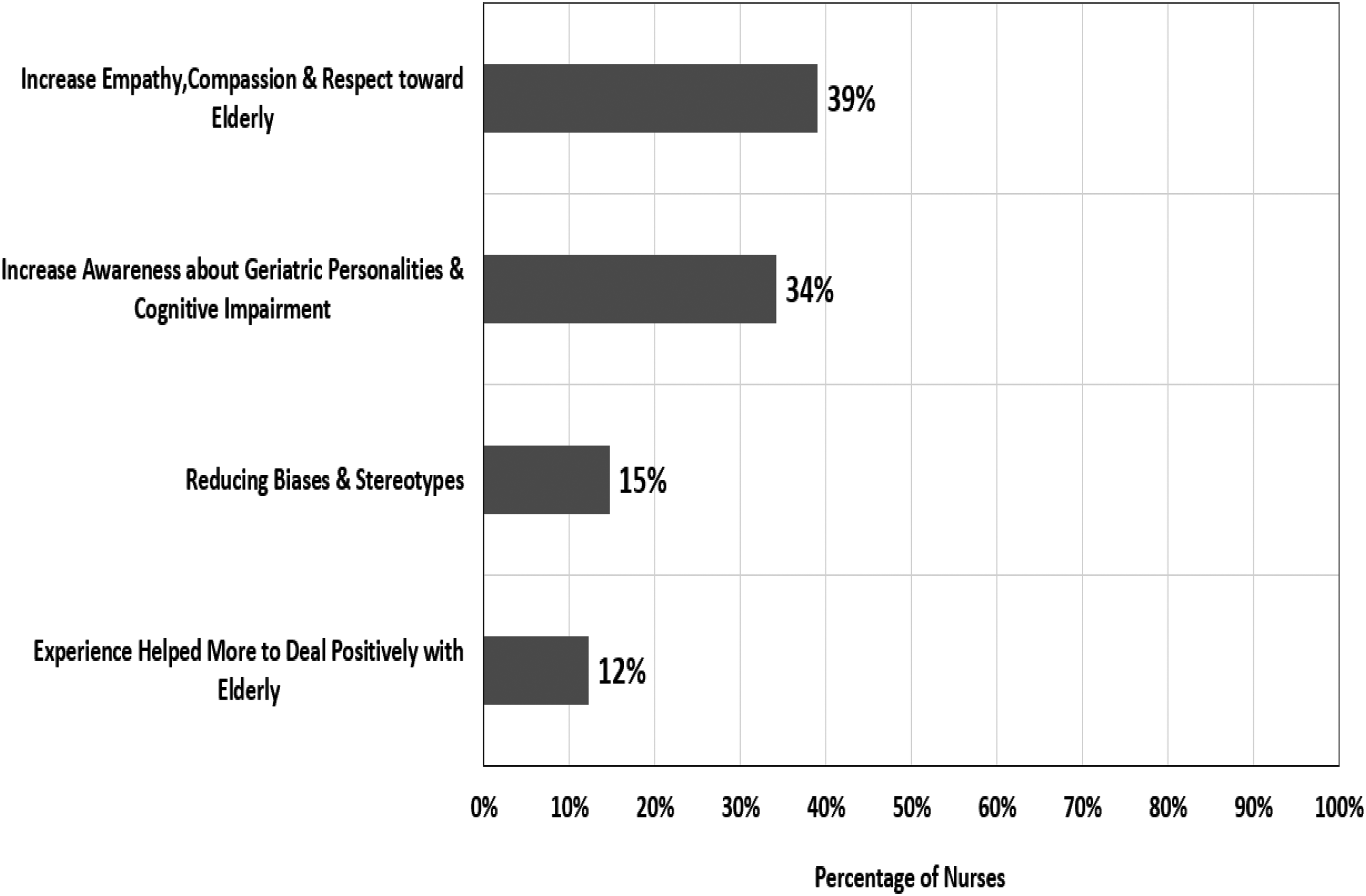
Nurses’ account of how the nursing curriculum contribute to their attitudes.
Nurses commented: “After learning how to properly care for geriatric patients I became more understanding and sympathetic with the patients”; “Education on geriatric patients influences my attitude and gives me more empathy”. One nurse stated that “My experience more than school has contributed to my attitude toward geriatric patients. It takes additional patience and knowledge to care for this population which is not always recognized during learning”.
Discussion
Nurses’ attitudes toward caring for older patients
Based on findings of this study and Table 1, more than half of the total participants held neutral attitudes toward caring for older patients, while the remaining participants held positive attitudes. Nurses expressed their attitudes toward gerontology care through their opinion and nursing practice experience. It became apparent that there were no negative attitudes among Canadian nurses toward caring for aging populations. Based on previously discussed literature about nurses’ attitudes toward older adults’ care, findings from this study are to some extent congruent with Zhang and Sun (2019), and Gould et al. (2015), which revealed that nursing students who were prepared had positive behaviors when it came to caring for the older adults, at least where there is no dementia. Correspondingly, Capezuti (2011) found that the most positive attitude toward older people is amongst Canadian nurses in long-term care facilities. Topaz and Doron (2013) also reported that nurses with supportive attitudes towards older adults stated that they listen attentively, assist with compassion, and develop a friendly relationship with their patients. According to Hsu et al. (2019), Neville and Dickie (2014), and Hweidi and Al-Obeisat (2006), nursing students had positive perceptions and attitudes toward gerontology care. Likewise, Chi et al. (2016) declared that “Taiwanese undergraduate nursing students had neutral to slightly favorable attitudes toward working with older adults” (p.172). Findings of this study contradict Dikken et al. (2017), who asserted that nurses negatively affect older patients. Alike, Abozeid (2015) revealed that most of the nurses have negative behaviors towards older patients. Several nursing studies have shown that nurses and nursing students have negative attitudes towards the aged. For example, in the United Kingdom and Iran, there were ageist views expressed by nurses, which negatively influence the dignity and autonomy of older patients (Arani et al., 2017; Gallagher et al., 2006). According to Liu et al. (2012), the attitudes of registered nurses and nursing students towards the older adults varied from positive to negative to neutral. Dahlke et al. (2021a, 2021b) revealed that ageist attitudes are common among nurses and many Canadian nurses believe that caring for older people is a low-skilled occupation.
Nurses’ knowledge level in terms of providing gerontological nursing care
The present study illustrated that less than half of the participants possessed some knowledge about caring for older patients, while the remaining participants possessed relatively high, average, or low knowledge levels. These findings are congruent with Topaz and Doron (2013) who reported that Israeli nurses had limited knowledge and understanding of elderly care. The current study findings parallel those of Zhang and Sun (2019), who found that most of the nurses in their research had a low level of knowledge about elderly care in Chinese nursing homes. According to some Canadian scholars, nurses are graduating with insufficient knowledge of how to care for the older population (Dahlke et al., 2021a, 2021b).
Overall, study findings highlighted in Table 2 demonstrate that on one hand there is a statistically significant relationship between nurses’ work status and their knowledge level for older adult care, and a statistically significant relationship between nurses’ age and their knowledge level. In addition, there was a statistically significant positive correlation between nurses’ attitudes and their total knowledge level (Table 3). These findings coincide with Hirst et al. (2012), who analyzed the attitudes of Canadian nursing students and nursing curriculum content across Canada, and noted that knowledge, attitudes, and interest in caring for the older population are all interrelated. Moreover, they found that nursing students who interacted more with older patients may develop relatively positive attitudes as a result. The researchers also indicated that some existing research had linked insufficient knowledge and nursing practice regarding older adults to the unfavorable attitudes towards older patients. Similarly, Thai nurses had a high level of knowledge and possessed a positive attitude toward older adults’ care (Prasomsuk et al., 2020). Moreover, Kotzabassaki et al. (2002) confirmed a statistically significant correlation between Greek nursing students’ attitudes and their level of knowledge. In the same way, Topaz and Doron (2013) demonstrated that nurses’ attitudes are strongly affected by their age, cultural background, educational level, and knowledge level regarding gerontology care. In the same context, Wells et al. (2004) indicated that Australian nurses have less understanding about gerontology care than other health providers. They were anxious about caring for older adults, and they agree that working with older people was correlated with low self-esteem and negative behaviors. On the other hand, findings from the current study are inconsistent with Mellor et al. (2007) who indicated that Australian nurses have very positive attitudes toward older people despite their lack of knowledge of the socio-economic condition of the aging population and essential clinical skills of gerontology nursing. Similarly, Ryan and McCauley (2005) noted that nursing students have a strongly favorable view toward older citizens and a knowledge deficit regarding gerontology nursing care. Correspondingly, Brabham (2018) and Alsenany (2009) stated that while nursing students lacked understanding of the aging process and physiological and psychological features, they held mainly positive attitudes toward older patients. Finally, this study revealed that there was no statistically significant correlation between nurses’ attitudes and their years of experience. These results are congruent with Abozeid (2015), who found no statistical variation between nurses’ attitudes and work experience. Likewise, there is no statistical relationship between age group and nurses’ attitudes and no statistical relationship between gender and nurses’ attitude were noted (Table 2). In addition, as highlighted in Table 2, there was no statistically significant relationship between gender and knowledge level of nurses. Furthermore, as demonstrated in Table 3, there was no statistical correlation between work status and nurses’ attitudes. It is apparent that study findings are congruent with Abozeid (2015), who revealed no statistically significant relationship between age and attitudes. As well, Liu et al. (2012) demonstrated that nurses’ attitudes are influenced by their work experience, knowledge, and understanding of the aging process, and there was no statistically significant difference between attitudes of registered and student nurses and their ages, gender, or educational level. Meanwhile, these findings are inconsistent with those of Gallagher et al. (2006), which indicated that age, gender, education level, spending time with an elderly adult, and areas of experience tend to have a significant impact on changing attitudes about gerontology care. Abozeid (2015) noted that female nurses reported more negative attitudes toward older people than male nurses. Zhang and Sun (2019) also demonstrated that female nurses with extensive work experience had negative attitudes towards older adults. Correspondingly, Hweidi and Al-Obeisat (2006) found that nursing students’ behaviors were strongly associated with their age and social background and noticed that male and older nursing students showed positive attitudes toward the aged group compared to their female peers.
The influences of the nursing curriculum on nurses’ knowledge and attitudes
Specific trends are highlighted in Figures 1–3, when examining the impact of the nursing curriculum on nurses’ knowledge and attitudes. Most nurses “agreed” with many of the statements related to the importance of the nursing curriculum, especially with comments that discussed how the nursing curriculum helped provide them with the required knowledge and skills about older adults’ needs, problems, the aging process, common diagnosis, and medications. In particular, statements such as: “The nursing curriculum has prepared me for the care of the elderly by shedding light on the normal aging process, and common health challenges among the elderly”; and “The nursing curriculum has contributed to my knowledge in the care of geriatric patients by teaching us about the normal process of aging” corroborate and support the identified themes. Study findings, to some extent, is in accordance with Hsieh and Chen (2018) who revealed in their systematic review that incorporating gerontology and long-term care courses into undergraduate nursing curricula could help students improve their nursing knowledge and skills. Equally, Hsu et al. (2019) asserted that Macao nursing students’ positive attitudes toward Chinese older adults were associated with their clinical experience, knowledge level, and religion. A study of nurses in Greece (Kotzabassaki et al., 2002) revealed that nursing students believe that their nursing curriculum equipped them with appropriate knowledge and skills to deal with older patients, and they expressed their willingness to work with them after graduation. Study findings indicate that another group of nurses “agreed” that the nursing curriculum was not helpful, and that they acquired their practical experience from working in the hospital setting. Examples of statements include: “Nursing curriculum doesn't help me much but my experience as a nurse for past eight years helped me a lot”, and “Not enough knowledge when you are newly graduated, learn process start when you are hands-on”. These findings are corroborated by the literature on clinical practice being essential for the development of nursing students in gerontology care, as clinical practicum is needed to prepare students with problem-solving, clinical experience, clinical judgment, and administration skills (Hsieh & Chen, 2018). These results are also compatible with a Saudi study which revealed that training and working experience with older patients help improve nurses’ attitudes, abilities, and interests (Alsenany, 2009).
In the same line, Figures 2 and 3 indicate that nurses strongly agreed that the nursing curriculum positively impacted their attitudes toward older patients by increasing their empathy, compassion, and respect toward older people. The nursing curriculum also helped raise nurses’ awareness about older people's personalities and cognitive impairment and reduce bias and stereotypes. These notions are captured in participants’ statements such as “Education on geriatric patients influences my attitude and gives me more empathy”; “The nursing curriculum contributed to my attitude in the care of geriatric patients as we have been educated on treating all patients with dignity”; and “The curriculum also teaches you to treat the elderly with respect and to avoid stereotypes”. The aforementioned findings align with those of Kotzabassaki et al. (2002), which indicated that nursing students felt the nursing curriculum had supported them in being more positive about gerontology care. In conjunction with Hsieh and Chen (2018) on the importance of the inclusion of the gerontology program in the nursing curriculum to increase student knowledge, awareness, attitude, and skills in gerontology nursing care, it is not surprising that most nurses in the current study found the nursing curriculum plays a crucial role in the development of their attitudes toward older people. Topaz and Doron (2013) also emphasized that nurses discriminate against older patients in various ways; this result is unsurprising as gerontology content is missing the fundamental knowledge and skills in all Israeli nursing education. According to Wagner et al. (2014), Canadian nursing curriculum lacks knowledge about caring for aged people. In contrast, a small group of nurses reported that the nursing curriculum had a minor impact on their attitudes, as highlighted in comments such as: “It is good but needs to be better when approaching unforeseen problems that students might encounter”. The remaining participants agreed that clinical work experience had a significant impact on their attitudes toward older people care, as they learned to deal positively with older patients while working with them in the hospitals. For example, statements such as “My experience more than the school has contributed to my attitude toward geriatric patients. It takes additional patience and knowledge to care for this population which is not always recognized during learning”, and “I think attitudes are formed more once working with the population” support these findings. Kotzabassaki et al. (2002) stated that research findings haven't always been constant. On the one hand, some results suggested that the nursing curriculum had no impact on nurses’ attitudes. On the other hand, some research studies reported that the nursing curriculum positively affects nurses’ opinions and attitudes regarding older adults’ nursing care. Congruent with the current study findings, Kotzabassaki et al. (2002) revealed that interactions with older patients in long-term care settings improved nursing students’ attitudes. Likewise, these findings resonate with Hsieh and Chen (2018) and Alsenany’s (2009) findings which indicated that clinical work experience in long-term care helps develop nurses’ positive attitudes.
Based on participants’ self-reporting of various nursing curriculum in Canada, it is apparent that gerontology nursing is not a stand-alone course; it is included in the overall nursing curriculum. One standard nursing curriculum does not exist as every nursing program creates its own curriculum; therefore, nurses had different learning experiences. Congruent with this study findings, Baumbusch and Andrusyszyn (2006) claimed that Canadian gerontological nursing is being included into the general adult care curriculum and the impact of this method is still unknown. Dahlke et al. (2021a, 201b) also revealed that nursing curriculum lacks care for older people with dementia, and nurses are graduating unprepared to cope with the aging population. Equally, Hirst et al. (2012) pointed out that nursing students, according to some studies, have negative attitudes towards older adults and dislike working with them; although, recent evidence shows that student attitudes are not standardized and can vary based on the learning environments. The authors concur with Brabham (2018), who stated that the nursing curriculum is necessary to ensure that nurses and nursing students obtain the required knowledge, skills, experience, and attitudes to provide specific care to older adults. According to King et al. (2013), nursing education significantly impacts nurses’ knowledge and attitudes; a gerontology nursing curriculum is essential for equipping nursing students with the knowledge and practical skills in older adult care. In the same line, Wells et al. (2004) asserted that gerontology curriculum improvement is crucial to enhancing nurses’ attitudes and perception toward caring for the older adults. In addition, Canadian nursing schools should integrate content concerning older adults’ care into their curriculum and create learning activities that eliminate negative perceptions about ageing population (Dahlke et al., 2021a, 2021b).
Nursing implications and recommendations
Based on the study findings, it is recommended that gerontological nursing courses be mandatory separate course in nursing education to enhance nursing students’ knowledge and skills. It is also suggested that more concentration be given to the gerontological curriculum, including topics regarding healthy aging, rather than focusing only on the dysfunctions and mental illness associated with aging. Likewise, some suggestions for improving nursing students’ attitudes include increasing students’ practical training with older patients by inspiring them to act independently and under close supervision. Finally, nursing educators and curriculum developers should be aware of and follow the Canadian entry-to-practice gerontological care competencies to develop the Canadian nursing curriculum and improve the nursing students’ knowledge and attitudes toward older people's care.
Limitation
One limitation of this study is the difficulty recruiting participants. Due to the COVID-19 pandemic, hospitals were overwhelmed, and some nursing administrators were challenged in distributing the study among nurses. Similarly, different nursing programs apologized in advance for not sending study materials to their students, and justified their decision based on online learning. Another limitation is the lack of access to the nursing curricula across the programs. As a result, there could be self-reporting biases in participants’ accounts of the role of curriculum in nursing education.
Conclusion
This study has provided the opportunity to reflect on the attitudes and knowledge of nurses and nursing students toward older adults’ care. The current study findings revealed that most Canadian nurses and nursing students possess average knowledge levels and neutral attitudes toward caring for the older population. It is essential to remember and ultimately recognize that the nursing curriculum positively impacted most nurses’ attitudes, perceptions, and understanding. While more comprehensive and well-defined studies may yield more accurate and valid results, we recommend that future studies should aim to analyze the curriculum content in different nursing programs to identify the knowledge deficits. Finally, gerontological nursing courses should be mandatory separate courses in nursing education to enhance nursing students’ knowledge and skills.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
