Abstract
Keywords
Educational institutions rely on nurse preceptors, who are registered nurses, to enhance students’ experimental learning during clinical practice; allowing them to observe and apply their knowledge and to achieve the level of clinical competence required by the profession (Rippie, 2015). Preceptors also engage with students during individualized teaching-learning sessions; while providing quality patient care, they are expected to be role models, teachers, facilitators, guides, and evaluators (Omer et al., 2016). Essentially, they have the responsibility to unite theory and practice, and create effective learning environments, critical for fostering students’ development as competent nurses (Bengtsson & Carlson, 2015). Beyond being a good clinician and demonstrating valuable personal and professional traits, such as self-confidence, leadership skills, and knowledge of their own strengths; evidence exists that academic qualification, experience, and adequate preparation are also key qualities that enable nurses to perform well in their preceptor role (Kamolo et al., 2017; L’Ecuyer, 2019). In order to develop these qualities preceptors require additional training and support from faculty in terms of clinical assessments, feedback skills, and pedagogical strategies to facilitate student learning (Broadbent et al., 2014; McSharry & Lathlean, 2017). However, formal standards for preceptor education programs are lacking, resulting in variability in their content and delivery.
Over the past decade, institutions have replaced the traditional face-to-face nurse preceptor workshops with online programs, as these courses encourage interaction and dialogue, are responsive to nurse preceptors’ schedules, and allow for flexibility in learning (Myrick et al., 2011). Although different instructional design features have been used, results reveal that online preceptor programs are informative, supportive, and highly valued (Wu et al., 2020). Moreover, findings from a systematic review conducted by Wu et al. (2018) showed that these programs enhance preceptors’ knowledge and skills, self-efficacy, and leadership practices (Larsen & Zahner, 2011; Wilkinson et al., 2015). According to Myrick et al. (2011) using online resources to exchange information and knowledge with colleagues is fundamental for preceptors to grow as professionals and develop a stronger sense of self-validation. Similar to classroom curriculums, the development of online programs should be based on current knowledge, and guided by contemporary theories of learning and education. For example, some online preceptor programs have drawn upon different theoretical frameworks, such as Bandura's theory of self-efficacy (Parsons, 2006), Kouzes and Posner's leadership model (Stutsky & Spence Laschinger, 2014), and Benner's model of novice to expert (Zahner et al., 2009). The use of learning theories is contextual, and each one of them supports the student's training.
To our knowledge, no educational online program could be located thand at is aligned with nor based on the Strengths-Based Nursing (SBN) principles. SBN, developed by Dr. Laurie Gottlieb, is a philosophy and value-driven approach that promotes in-person and family-centered care, empowerment, relational care, and innate capacities (Gottlieb, 2013). More specifically, the approach capitalizes on a person and family's strengths required for health and healing (Gottlieb et al., 2021), and consists of eight core values: health & health, uniqueness, holism & embodiment, subjective reality & created meaning, self-determination, person-environment are integral, learning, readiness & timing, and collaborative partnerships (Gottlieb, 2014). These principles and related values have been at the heart of the teaching philosophy at the McGill Ingram School of Nursing (ISoN) since 2016. SBN encourages individuals to use their strengths, capacities, and resources to manage their health problems. In January 2019, the ISoN launched an accredited online course for nurse preceptors using SBN as the theoretical underpinning. The introduction of this new program would permit preceptors to develop new competencies and strengthen current ones.
Purpose
This qualitative study explored the nurse preceptors’ experiences in using a SBN approach to provide clinical teaching to nursing students after completing an online SBN clinical teaching course.
Online course – SBN in clinical teaching
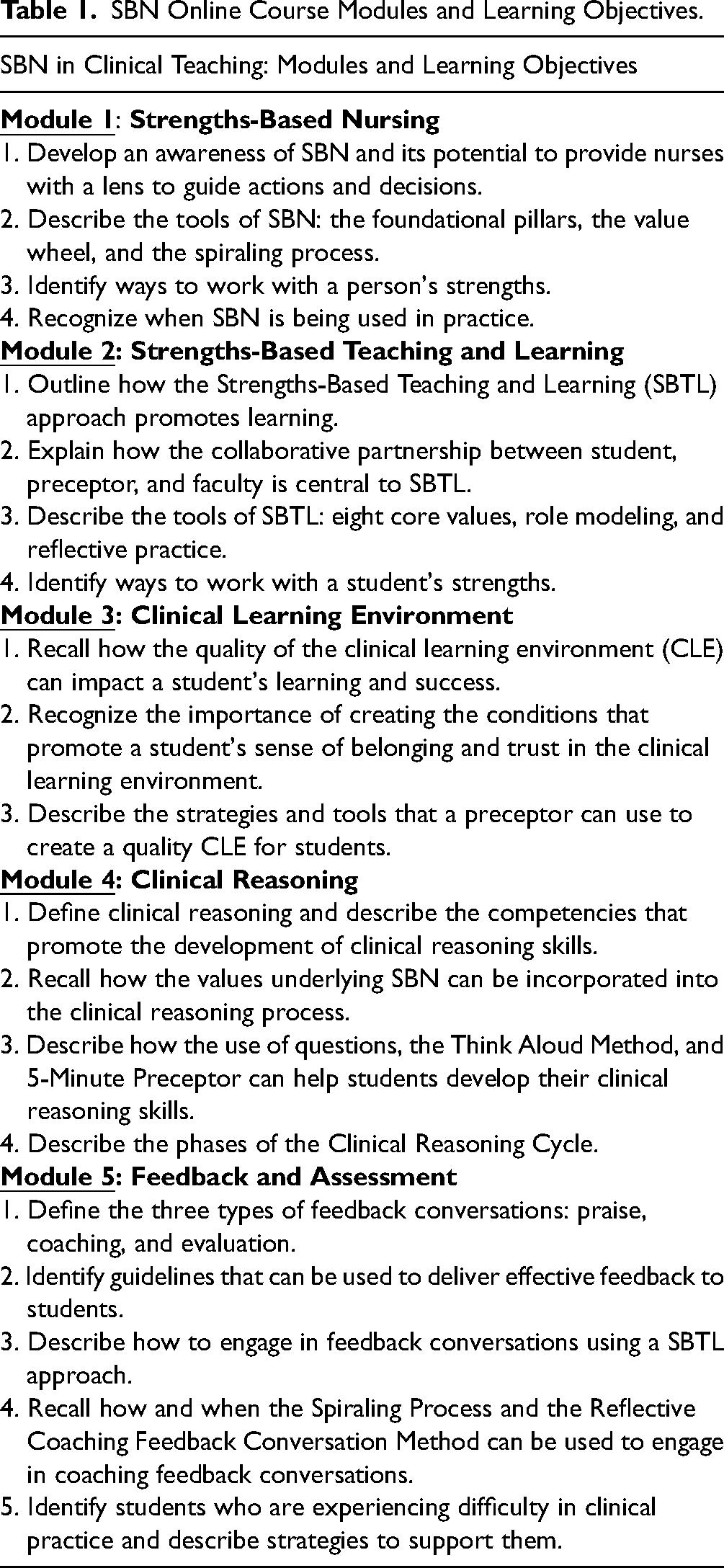
Throughout the course, preceptors learn that SBN involves being student-centered. The preceptors are encouraged to create meaningful learning experiences and to discover and further develop their students’ strengths (Gottlieb & Gottlieb, 2017). The online course consists of five modules: 1) Introduction to SBN; 2) SBN Teaching and Learning; 3) Clinical Learning Environment; 4) Clinical Reasoning; and 5) Feedback and Assessment (see Table 1). The SBN principles and the eight values were integrated throughout the various modules.
SBN Online Course Modules and Learning Objectives.
The online course uses a variety of interactive web-based tools, such as quizzes, videos, animations, narrations, tasks, tips, games, etc. and is offered through the University's computer-aided learning and management system. Each module requires approximately one hour to complete; however, the course design allows the learner to easily navigate through the modules at their own pace, in order to ensure the individual's full understanding before moving forward.
Methods
Design
A qualitative descriptive design was used, and is appropriate to describe nurse preceptors’ experiences. According to Sandelowski (2010), qualitative descriptive studies, which is grounded in the general principles of naturalistic inquiry, provide factual responses to who, what, and where questions of events or experiences (Colorafi & Evans, 2016).
Sample and recruitment
After receiving ethics approval from the University's Institutional Review Board, a purposive sample of six French and English speaking nurse preceptors who obtained professional development credits from the school's office for Continuing Nursing Education (CNE) were recruited. In this primarily French-speaking province of Canada, the nursing association requires that all registered nurses follow 20 h of professional development annually, of which, seven must be accredited (Ordre des infirmières et infirmiers du Québec, 2011). The nurses that participated in the study were preceptors to students during the Winter, Summer and Fall 2019 semesters, and they were employed in various University affiliated hospitals in a primarily French-speaking province of Canada. All participants were women ranging from 27 to 58 years of age (mean of 46 years). Two participants had a college degree, three a bachelor's degree, and one a master's degree. Their years of experience working as nurses ranged from 5 to 39 years (mean of 20 years), and their years of experience related to their work as preceptors ranged from 1.5 to 15 years (mean of 5 years). Two nurses had taken an online preceptor course from another educational institution prior to becoming a preceptor at the ISoN. All participants had completed the online course – SBN in Clinical Teaching.
Data collection
After providing the participants with the course credits, the CNE office sent an email with an information flyer and a consent form as an attachment to all potential preceptors (n = 66) to introduce the study. Semi-structured interviews in English or French, lasting approximately 45 min, were conducted by the 5th author at a convenient time for the participant. These phone interviews were audio-recorded and scheduled in early 2020, approximately 3 to 12 months after completing the course. This allotted time gave participants the opportunity to integrate the SBN concepts when supervising students in clinical practice. The interview guide included questions, such as; After completing the online course, did you modify your approach to precepting students? Were you better prepared for your role as a preceptor? In order to ensure that the interview questions and the study aim corresponded with one another, the guide was pilot-tested and validated with key informants, and further refinements were made after the first few interviews. At the start of each interview, the purpose of the study was re-explained, consent was obtained, and a sociodemographic questionnaire was completed.
Data analysis
Interviews were transcribed verbatim in the language that they were conducted in, interviews conducted in French were translated in English for coding purposes. Each transcript was thematically analyzed using the inductive approach, described by Miles and Huberman (1994), and supplemented with field notes. A process of open coding was used to assign captions to segments of the transcripts. Codes were organized into categories and themes that captured similar concepts, from which descriptive statements were formed and supported with quotes. This process was repeated until consensus was reached between several of the authors. Appropriate steps were taken to enhance the trustworthiness of the study using Lincoln and Guba's (1985) four quality criteria The first two and last authors performed an iterative analysis to reach a consensus in the conceptualization of the data. Trustworthiness was enhanced by conducting mock interviews prior to the data collection. Furthermore, the fourth author wrote reflective notes immediately after each interview, documented personal feelings, insights, possible biases, and preconceptions, and committed to a detailed description of the research methods, participants, and settings. Confirmability was addressed by establishing an audit trail to keep track of decisions made during the analysis. To enhance credibility, informal member checking with participants was performed during the interviews.
Results
Findings revealed that although the levels of familiarity with the SBN approach varied, all nurse preceptors were motivated to learn more about the use of the SBN approach in their clinical teaching, and they acknowledged that using SBN in clinical teaching benefits both students and educators. This led to the overarching theme: Mutual empowerment within the student-nurse preceptor relationship, which consists of five interrelated sub-themes as described below (see Table 2). Getting to know their students helped the preceptors offer tailored learning experiences and also allowed them to provide their preceptees with relevant feedback. Concurrently, it enhanced the preceptor's self-confidence and created opportunities for shared learning.
Overarching Theme and Sub-Themes.

Mixed levels of familiarity with SBN
The first sub-theme related to the different levels of familiarity with the SBN principles and its values varied among the participants. Some nurse preceptors (P1-3, 6) indicated having superficial knowledge of the philosophy, P5 had read the SBN book, while P4 indicated having received SBN resources during former in-person preceptor workshops. Two participants (P1, 2) were aware that SBN is focused on strengths and not deficits; however, they explained not having a real understanding of the approach, as expressed by P2: “I am kind of familiar with that [approach], but [I cannot] put it into words. I think it is unique to the ISoN, even though we use it in our practice”. Nurse preceptor (P3) who is a graduate from another University said: “It was more the McGill Model when I started working. This [SBN] is focused on something else, but the goal is the same. It is just [wearing] other glasses to see things differently”. Participant 6 shared a similar thought: “If I look at the [SBN] values, I think that these are values that we use in our practice. It is not something revolutionary”. P5 however explained that she applies SBN when supervising students. She said: “I apply it [SBN] a lot with my students. There are really great activities that we can develop to motivate students to take on a new approach to better their communication, for example”. Finally, P6 summarized it as follows: “I think that a large majority of nurses practice SBN, but to explain it to a student in the right way is another thing”.
Curiosity and motivation to learn
Although participants expressed knowing and practicing SBN, all were curious and motivated to take part in the online course for a variety of reasons. In this second sub-theme, most of the participants (P1-4, 6) discussed two principle factors that encouraged them to complete the training; the desire to remain informed about the current advancements in teaching at the School and the mere curiosity of wanting to learn new things. This was expressed by P1 as follows: “I wanted to gain more information to match students’ learning experiences and my precepting role to the latest standards. I wanted to learn something new and not miss anything”. P2 voiced this curiosity to learn as having “a little more knowledge about the program to be sure that I was going things right”. This statement was supported by P6: “I want to know what I am doing with the student, and whatever is done at the School. When a student asks ‘Why are you doing that?’ It is easier to explain it if we know their language.” P3 appreciated the work done by the School to formalize the role of the preceptor, and said: “In theory, it is our job as nurse clinicians to train others. We are professionals, but if we can be trained as teachers, so much the better. Personally, I really appreciate the effort that the School makes for its students, and to help us [preceptors] too. We cannot claim to be experienced teachers just because we have nursing experience (…). Everything at the School is improving, including, the science of imparting knowledge”.
Shift towards student empowerment
Being up-to-date with new teaching developments was key for participants to facilitate and support student learning, and foremost, as described in the third sub-theme, the SBN online course helped them to create a shift towards greater student empowerment. Participants (P1, 2, 5) acknowledged that SBN is centred on empowering others, new nurses, or in the case of an educator, empowering students. P1 shared: “I started to focus more on empowering students during evaluations. Before [the course], I said: ‘ok, good’ or ‘that is not good’. People will forget what you did or said, but they never forget how you make them feel. Now I am taking more time to say things like: ‘I really like how you managed your time today’. I started to focus on the good things and saw that it was very beneficial for the student”.
Another participant P2 continued: “[using SBN], we are seeking to validate students’ strengths, because we often tend to correct a lot, but on the negative side. We need to reinforce the positive points; I think it is worth it”. P5 summarized it as follows: “It is positive thinking, positivism, … It is seeing the students'strengths, seeing something constructive”. P1 went on to explain that she would introduce the students to the interdisciplinary team. She stated: “I started to take more into consideration the working environment. Before I did not think it was important to introduce students to the social workers or occupational therapists. It is not only empowerment, but also supporting them to give them a sense of belonging within a team … It is empowering their abilities to connect. They need to know how to communicate, so that they do not feel like strangers”.
Embracing the students’ individuality while creating a supportive environment to empower them was recognized by three participants (P1, 2, 5). One participant P1, who had also reflected on her role as a preceptor on how she supported students in their uniqueness, stated: “Before [the course], it was like you [preceptor] are a professional, you have to demonstrate standards of care and try to train students. But now, we have SBN to help us understand our students’ attitudes, levels of knowledge, and uniqueness”. P2 shared: “One thing that I have learned in this course is to see the person as an integral part”. She continued: “When we do not know the person, we tend to: ‘Ok, the student comes in, we give a lot of information about the clinic, how to interact with the patients, etc. and then they start right away’. Now [I see] students who arrive with different professional and personal backgrounds. It is important to learn these things before you even start and to use them in everyday life as a strength, but also, maybe to better understand when there are weaknesses”.
Using strengths to provide constructive feedback
Creating a supportive environment using the SBN principles not only empowered student, participants also agreed that the online course gave them a different perspective on how to provide constructive feedback to students; which is described in this fourth sub-theme. As expressed by P2: “This [feedback section] was really the most relevant for me. We need to empower students by saying, ‘I like what I have observed, or it is actually a very good point. I like this presentation very much”. P3 embraced this thought: “In order to give feedback, we need to use students’ strengths, and take the time after [the intervention] to evaluate… What did you [the students] do well? What do you need to improve?”. According to P1, focusing on the positive things and acknowledging what was done well, may decrease student stress levels. P6 further elaborated: “[you do not say] You [student] did not do that correctly, [instead you would say]: ‘Ok, you did that. Do you think that is correct? Or, explain to me what has happened, what do you think went well? What went wrong? You try to get more details than just saying ‘yes or no, and then go on to the next patient’. Let the student think, so that he can put his finger on it [on what went wrong], what does he think should be improved?”.
Boosted preceptors’ self-confidence
Participants shared that the SBN approach supported them in providing constructive feedback to students, and simultaneously, as identified in the final sub-theme, it also boosted their self-confidence. All participants, except P5, shared that the online course to a different extent had increased their level of self-confidence and prepared them better for the role of preceptorship. P1 who was categorically convinced that the course boosted her self-confidence, said: “It increased a lot. Before taking the precepting course, I would show the student how I worked, so they could perform well on the job and work safely. But now, I know what I am doing much more than before”. Another participant P3 who is still new to the role of preceptorship, expressed: “Every interaction I have had with my students has helped me a lot, not just the students themselves. They [those interactions] have helped me improve myself in that [preceptor] role”. P6 continued: “It is easier. You do not feel very small in your shoes. I am confident in my practice, I know what I am doing with my patients, but it is also good to be able to come and add the theoretical side that students are always looking for”.
Despite her past experiences as a nurse preceptor, P4 indicated that it helped her perform better at the job: “I learned what to do in my role and how to work with students. I taught them, but they taught me by sharing new material from their courses. It is all about giving and taking, and it makes me a better nurse”. She gave a concrete example: “I had a student who asked: ‘Why are you doing that?’ I answered that I was taught that when you give an IM injection, you aspirate the air bubble. Student replied that this technique was no longer recommended, and she was right. Like I say, it is important to be open and bring change as sometimes we are too comfortable and set in our ways.”
Discussion
Nurse preceptors play a key role in supporting and empowering students transitioning from classroom to clinical practice. The impact of a nurse preceptor's support on a student cannot be underestimated. Our findings are aligned with the existing evidence that preceptors require proper training and communication from academic nurse educators to perform well in their roles (Wardrop et al., 2019). Although the SBN approach was perceived by all participants as being highly appropriate for preparing nurse preceptors, they recommended that the course content be tailored to nurse preceptors’ level of experience. Hence, two points warrant further discussion: 1) The ability to learn is an integral element to the success of a preceptor, and 2) Need for more support and tangible rewards from educational institutions.
Clinical nurse expertise is fundamental to quality patient care; however, becoming a clinical expert does not happen overnight, and according to Benner (1984), not all experienced nurses are experts. In the same vein, not all experienced nurses are interested in being a nurse preceptor or have the attributes and qualifications to become one (Cotter et al., 2018). As indicated by Jackson (2001), it takes more than experience to be an effective preceptor. Beyond specific personal and professional traits, such as effective communication skills and clinical competency, they must be motivated to learn and share clinical experiences, have teaching and leadership skills, have the ability to objectively evaluate students’ performance, and be interested in professional growth and development (Cotter et al., 2018). The nurse preceptors who took part in our study shared those required attributes; however, they also expressed the desire to remain current with new advancements in nursing science and pedagogical approaches to better support students while they learn to apply theory to practice.
Although the ability to learn is a key attribute it is, according to Rebholz and Baumgarter (2015), a trait that is often less investigated in the nurse preceptor literature. Broom (2015) continued by saying that teachers do not “give” their students’ knowledge, instead they “acquire” knowledge through interactions with others. This is similar to what our study participants expressed after having completed the online course; the course led them to appreciate the importance of formal planned interactions with their preceptees. Moreover, nurse preceptors in this study shared that getting to know the students and learning about their strengths allowed them to promote useful learning experiences and give the perceptees the opportunity to address meaningful challenges. Interestingly, these interactions were not only beneficial to students, they also empowered the nurse preceptors; both novice or seasoned participants in this study agreed that it enhanced their self-confidence to precept; a vital quality of a nurse preceptor (Rebholz & Baumgarter, 2015).
As indicated in the literature effective preceptors should possess certain attributes and competencies, therefore, nurse educators have a responsibility to properly prepare nurses for the role of preceptors. Unfortunately, over the decades, a lack of training was found to be a recurrent issue in the nurse preceptor literature (Omansky, 2010). Our current challenging healthcare system, such as limited resources, shortage of nurses, stressful work environment, etc., often has our educational institutions struggling with placing students in various clinical settings; mainly due to the lack of trained and available precepting nurses (Nash & Flowers, 2017). Nurse preceptors need more support, dedicated time, and communication with faculty staff members for them to feel motivated and capable of taking on their role; a key issue to enhance preceptor retention (Kalischuk et al., 2013). The faculty should not underestimate the importance of a nurturing and supportive faculty-preceptor relationship. For example, clinical site visits provide faculty and preceptors, who are guiding nurse practitioner students, an opportunity for face-to-face acknowledgements of the contributions and the nurturing of the preceptor role (Campbell & Hawkins, 2006). Today with the many web-supported tools for online education, those face-to-face discussions may be supplemented with virtual visits; this would lessen the burden on clinicians who serve as preceptors and it would enhance human interaction which was an essential need for some of the study participants (Campbell & Hawkins, 2007).
Another element that may boost a nurse preceptor's continued commitment to the role, and as such their retention, is the offering of tangible rewards (Smith & Sweet, 2019). Our study participants identified the importance of obtaining credits for professional development after completing the online course. Evidence around rewarding nurse preceptors is scarce; however, Stone and Rowles (2002) ranked the top reward choices as follows: 1) Continuing education; 2) Audit a class; 3) Letter of commendation or certification; and 4) Appointment as adjunct faculty. Overall, the development of online preceptor courses requires time, money and human resources from faculty and their respective institutions; however, it is their responsibility to provide the necessary support, recognition, rewards, and resources to sustain preceptors in their role (Viljoen, 2016).
Limitations
The small number of participants enrolled in this study can be seen as a limitation; however, data saturation was achieved, and the results provided a comprehensive picture of the nurse preceptors’ experiences with using a SBN approach to provide clinical teaching to nursing students after completing an online SBN clinical teaching course. A second limitation pertains to the fact that some interviews were conducted with nurse preceptors that took the course approximately 12 months prior can be identified as limitations of this study. The elapsed time between completing the course and the interview may have been important to better understand how preceptors integrated SBN in their interactions with students; however, for a few preceptors it was challenging to remember the course details from an instructional design perspective.
Implications for nursing education and future research
Well-prepared nurse preceptors are essential in order to provide positive clinical learning experiences for students. In addition, it is well-known that the preceptor-preceptee relationship is a major contributing factor for student-learning. However, today many preceptors are inconsistently trained, and existing training programs often do not incorporate the educational institution's nursing philosophy to teaching and learning. As nurse educators, it is our responsibility to both students and preceptors to develop and provide quality training in order to support nurses to become better nurse preceptors. It is also our responsibility to educate preceptors about the school's philosophy of nursing and the school's approach to teaching and learning so that students’ experiences in clinical practice are aligned with what they learn and experience in classroom settings. If faculty do not invest in the training of preceptors, this will impact the quality of nursing education and preparation of future nurses. Future research should, however, further explore the nurse preceptor's experiences with the SBN online course; and it should seek to determine if the course positively impacts students’ performance in clinical settings. In addition, this study should be replicated to include nurse preceptors from different clinical settings as well as include nurses who preceptor nursing students from a variety of nursing programs, such as nurse practitioner.
Conclusion
The results have demonstrated that the offering of an online SBN training program for nurse preceptors was mutual beneficial for both the preceptee and the preceptor. More specifically, using a SBN approach increased the self-confidence of the nurse preceptor in their role and in providing tailored feedback according to the students’ learning needs; hence promoting student empowerment. The SBN online course for preceptors demonstrates the school's commitment to the importance of the preceptor role, and the value of incorporating a strengths based philosophy in clinical teaching and learning.
Footnotes
Authors’ contributions
All authors have contributed to the preparation of this manuscript. More specifically, T.A. conducted all participant interviews. AA, MDF, MLT were involved in the analysis of the qualitative data and documentation of the results. MDF, MLT, MW, and GP developed the original project idea and the research protocol. AA and AC prepared the final manuscript for publication. All authors approved the final manuscript.
Acknowledgements
The authors would like to acknowledge Mrs. Katherine Logue, and Drs. Guylaine Cyr and Laurie Gottlieb.
Conflict of interest disclosure
The authors declare that they have no competing interests.
Funding
This research was supported by the McGill Nursing Collaborative for Education and Innovation in Patient and Family Centered Care (Newton Foundation/McGill Faculty of Medicine).
