Abstract
Healthcare waste management is crucial in preventing infections and injuries. However, only an estimated 31% of healthcare facilities in least-developed countries had basic waste management in 2023. We employed multilevel modelling to assess healthcare facility-level and country-level predictors of 6 elements of safe waste management (e.g. having a functional incinerator, having bins for waste segregation) across 2002 healthcare facilities in 14 countries. Eight percent (n = 154) of the surveyed facilities had basic waste management. Facilities with working electricity had higher odds of having a functional waste incinerator (odds ratio (OR): 1.26, p < 0.01), bins for safe waste segregation (OR: 1.28, p = 0.02), and proper sharps waste disposal (OR: 1.48, p < 0.01). Facilities that followed protocols for operations and maintenance had higher odds of having a functional waste incinerator (OR: 1.26, p < 0.01) and proper disposal of infectious waste (OR: 1.34, p < 0.01). At the country level, a higher water, sanitation and hygiene budget as a proportion of GDP was associated with higher average odds of having a functional waste incinerator (OR: 1.17, p < 0.01), proper infectious waste disposal (OR: 1.12, p < 0.01) and adequate sharps waste disposal (OR: 1.12, p < 0.01). Findings underscore the importance of multi-tiered approaches in enhancing healthcare waste management. Strengthening management and operations and maintenance at the healthcare facility level and creating and financing national healthcare waste policies may support healthcare waste management practices.
Introduction
Healthcare facilities in low- and middle-income countries produce a median of 0.7–2 kg of waste per occupied bed per day, including hazardous waste contaminated with chemicals, sharps and infectious pathogens and non-hazardous general waste, based on a systematic review of 136 waste generation points (Cook et al., 2023). The safe management of waste confers several benefits, both within and beyond the healthcare facility. Waste management is crucial in preventing infections from contact with pathogenic waste (Ferreira and Teixeira, 2010; Mol et al., 2016). Proper waste management is essential to prevent injuries from sharps waste and chemical exposures from hazardous waste (Blenkharn and Odd, 2008; Cook et al., 2023). For waste containing pharmaceutical products, safe management and disposal are important for preventing the emergence of antimicrobial resistance in the environment (World Health Organization, 2025). Beyond physical health benefits, proper waste management can contribute to the well-being and morale of healthcare workers (Anderson et al., 2023). Patients may also experience greater satisfaction with care when they observe that waste is safely managed and grounds are free of litter (Fitzpatrick et al., 2025). Finally, healthcare waste management has implications for environmental health that extend beyond the healthcare facility, as safe and environmentally friendly disposal can prevent contamination of water, air and soil (Cook et al., 2023; Vrijheid, 2000).
Despite the importance of healthcare waste management, in 2023, 31% of healthcare facilities in least-developed countries had basic waste management, defined as having safe waste segregation and proper treatment and disposal of sharps and infectious waste (Joint Monitoring Programme, 2024; World Health Organization, 2014). Rural healthcare facilities and non-hospital facilities lagged behind urban facilities and hospitals in waste management service levels (Joint Monitoring Programme, 2024). Prior studies have identified healthcare facility-level drivers of safe waste management practices, including healthcare worker training, the presence of oversight committees and the availability of written guidelines (Assemu et al., 2020; Tilahun et al., 2023; Wafula et al., 2019). Poor knowledge of waste management practices among waste handlers and other facility staff may pose a barrier to improvement (Affordofe et al., 2025). A study of healthcare workers in Nigeria found that better knowledge of waste management was associated with safer practices (Amaike et al., 2025). Facilities require sufficient protocols, budgets, infrastructure and training to implement and sustain waste management services (Omoleke et al., 2021). At the national level, gaps in waste management may arise if countries lack policies and regulations for healthcare waste management or mechanisms for monitoring compliance (Khan et al., 2019).
The international development community has increasingly recognized waste management as an essential environmental health service in healthcare facilities alongside water, sanitation and hygiene (WASH; UN General Assembly, 2023; World Health Organization and United Nations Children’s Fund, 2024). Current international guidelines for healthcare facility quality improvement emphasize the importance of organizational and managerial levers in improving healthcare waste management (Maternal and Child Survival Program and Save the Children, 2016; World Health Organization, 2022b; World Health Organization and United Nations Children’s Fund, 2024). Additionally, guidelines recommend that countries create costed roadmaps and fund national waste management policies as initial steps in their quality improvement approaches (World Health Organization, 2019, 2025; World Health Organization and United Nations Children’s Fund, 2024). Facility-level and national-level interventions may both, therefore, improve access to waste management.
Although prior research has assessed individual-level or facility-level drivers of healthcare waste management practices in low- and middle-income settings (Assemu et al., 2020; Niyongabo et al., 2019; Tilahun et al., 2023; Wafula et al., 2019), most studies focus on a small number of facilities in a single country. There is a lack of investigation into drivers occurring at the regional or national level. Multilevel analysis of waste management determinants can inform guidelines and interventions for effective waste management. The objectives of this study were to determine the proportion of variance in waste management services occurring at the healthcare facility level versus the country level, evaluate administrative and managerial determinants of waste management services in healthcare facilities and assess country-level factors that may determine national trends in healthcare waste management in low- and middle-income settings.
Methods
Data sources
Healthcare facility-level data
We obtained publicly available, de-identified data on waste management and potential determinants from a 2017 evaluation conducted by the Water Institute at UNC-Chapel Hill and the non-governmental organization World Vision (The Water Institute at UNC, 2020; The Water Institute at UNC and World Vision Inc., 2020). Prior publications include an in-depth description of the evaluation’s sampling approach, survey design and data collection procedure (Cronk et al., 2021; Guo and Bartram, 2019). Briefly, the evaluation consisted of a cross-sectional survey completed in 2002 healthcare facilities in 14 low- and middle-income countries: Ethiopia, Ghana, Honduras, India, Kenya, Malawi, Mali, Mozambique, Niger, Rwanda, Tanzania, Uganda, Zambia and Zimbabwe. These countries were selected because they had active World Vision programme areas focused on WASH. In each country, rural geographic clusters were randomly selected from a group of World Vision programme regions and a comparison group of non-programme areas. Researchers compiled a complete list of the healthcare facilities within each cluster’s administrative districts. Then, a simple random sample of 200 small, non-hospital healthcare facilities was selected for the evaluation in each cluster (Guo and Bartram, 2019).Data collection took place from July to October 2017. Trained enumerators visited each healthcare facility and conducted a face-to-face survey with one head doctor, head nurse or other knowledgeable staff member. Survey instruments were translated into local languages and administered using an electronic tool. Surveys included verbal questions and observations to assess the availability and condition of water, sanitation, hygiene, waste management and infection control resources at facilities. Surveys also included questions on facility administrative and training characteristics, including the availability of budgets, protocols, staff members and oversight committees for environmental health and infection control. This study examined survey questions related to waste management and administrative characteristics.
Country-level data
This analysis incorporated policy and development predictors with a hypothesized link to healthcare waste management. We obtained publicly available data from the World Bank, the UN-Water Global Analysis and Assessment of Sanitation and Drinking Water Data Portal (GLAAS) and the World Health Organization (GLAAS Data Platform, 2024; World Bank Group, 2023a, 2023b; World Health Organization, 2023). For this study, we compiled data on country GDP per capita and access to electricity in 2017 from World Bank Open Data. We drew data on official development assistance for WASH in 2020 from the World Bank Global Health Observatory. We obtained data on countries’ annual WASH budgets – encompassing healthcare WASH, waste management, and other WASH domains – in 2016 and 2018 from the GLAAS portal. Government effectiveness and regulatory quality metrics for 2017 were available from the World Bank’s Worldwide Governance Indicators.
Data preparation
To prepare data for analysis, we imported and merged healthcare facility-level and country-level datasets using R statistical software (Version 4.2.2; R Core Team, 2022). We re-coded the continuous variable for reported patient volumes into an ordinal variable with five levels, due to the skewed distribution of this variable. As many countries had data on WASH budgets per capita for either 2016 or 2018, or both years, we created a single variable that averaged the 2016 and 2018 values if both years were available, or used one of the values if only 1 year was available. We used grand mean-centred values for official development assistance for WASH, the WASH budget as a proportion of GDP, the country GDP and population-level access to electricity (Sommet and Morselli, 2017). When a predictor variable is grand mean-centred, the model intercept can be interpreted as the expected outcome when the predictor variable is at its mean value (Enders and Tofighi, 2007). In contrast, in a typical regression model without mean-centring, the intercept is defined as the expected outcome when all predictors are valued at zero. Mean-centring, therefore, aids in the interpretation of model results when a predictor variable value of zero is not meaningful (Enders and Tofighi, 2007; Sommet and Morselli, 2017). We rescaled the country-level variable for WASH development assistance by a factor of 1000, meaning that the model output can be interpreted as the effect of a 1000-dollar increase in WASH development assistance rather than a 1-dollar increase. Rescaling can assist in model interpretation by putting the predictor-outcome relationship on a more meaningful scale (Schielzeth, 2010). For all variables, we coded responses of ‘don’t know’ or ‘decline to state’ as missing.
Measures and analytic approach
We calculated descriptive statistics for facility characteristics and waste management indicators across all countries. To investigate facility-level and country-level determinants of waste management access at healthcare facilities, we created multilevel logistic regression models using Mplus statistical software (Version 8; Muthen and Muthen, 2017). Multilevel modelling is an approach for analysing outcomes influenced by predictors occurring at multiple, nested levels (Sommet and Morselli, 2017). A multilevel logistic regression model partitions outcome variance between the lower-level and higher-level variables and then examines factors contributing to a change in the odds of the outcome at each level. Multilevel modelling has previously been applied in environmental health to evaluate determinants of WASH-related disease and school absenteeism (Dreibelbis et al., 2013; Kumie, 2020; Sahiledengle et al., 2022) and in waste management to evaluate community behaviours related to waste sorting and recycling (De Iaco and Maggio, 2022; Guerin et al., 2001; Tabernero et al., 2015). In this study, we hypothesized that waste management services would be influenced by factors at both the healthcare facility (i.e. lower) and country (i.e. higher) levels (Figure 1).
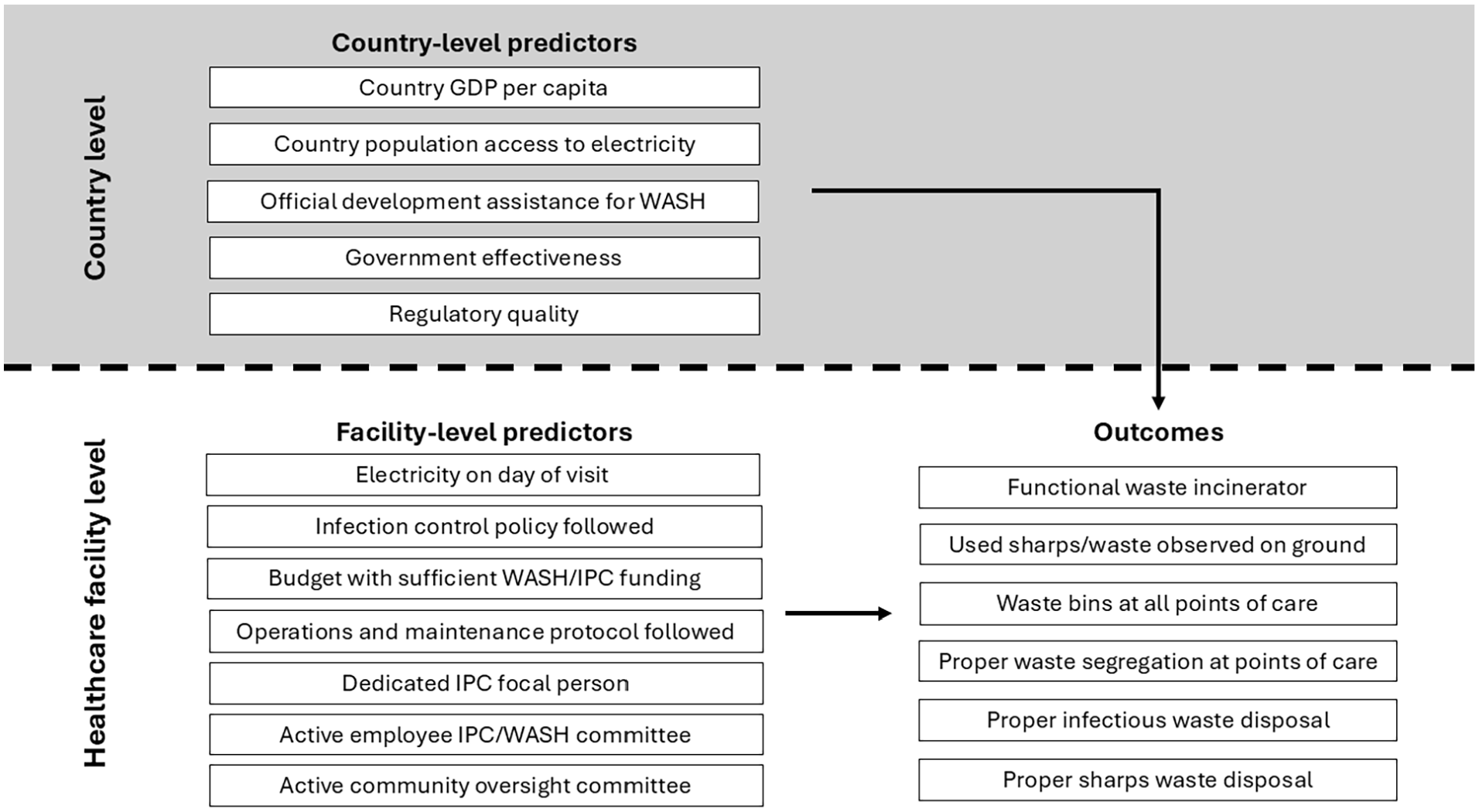
Conceptual model for healthcare facility-level WASH and IPC characteristics and country-level development and governance characteristics hypothesized to influence healthcare waste management.
Each model had a binary outcome measure of healthcare facility waste management services. We created separate models for six outcomes:
Waste incinerator present and working on the day of the survey
Used sharps or other healthcare waste observed on the ground in the facility yard
Three labelled waste segregation bins (for sharps waste, infectious waste and general waste) are available at all points of care
Waste segregation bins used properly at least one point of care, defined as meeting the following criteria: bins are clearly labelled or colour-coded, no more than three-quarters full, do not contain waste other than that corresponding to their label and are appropriate for containing the intended type of waste (e.g. sharps waste bins are puncture-proof)
Infectious waste treated and disposed properly
Sharps waste treated and disposed properly
Unconditional model (model 0)
We used multilevel logistic regression models with no predictor variables to determine the intra-cluster correlation (ICC), defined as the proportion of total outcome variance that is attributable to country-level factors compared to healthcare facility-level factors (Sommet and Morselli, 2017). A higher ICC value indicates that a larger proportion of the variance occurs between countries compared to the variance within countries. We determined the initial ICC for each outcome variable (Supplemental Table 1).
Adding facility-level predictors (model 1)
We used multivariate logistic regression models to assess the associations between seven binary healthcare facility predictors and each waste management outcome. Predictors included in each model were:
The facility had electricity on the day of the visit.
Infection control policy or procedure is followed.
Facility has a budget with sufficient WASH and infection control funding.
Protocol for operations, maintenance and WASH/infection control supply procurement is followed.
Facility has a dedicated infection control focal person.
Employees belong to an active infection control/WASH committee.
The facility has an active community oversight committee.
We added three additional independent variables to the model as covariates: healthcare facility type (a categorical variable with seven levels), average daily patient volume (an ordinal variable with five levels) and number of exam rooms (a continuous variable). These predictor variables and covariates were selected a priori based on a hypothesized relationship with waste management practices. We performed multivariate logistic regression to determine the relationship of all predictors and covariates with each waste management outcome. Results were expressed as log odds and converted to odds ratios (OR) for interpretation. To assess model fit, we reviewed correlation matrices to determine if predictors were highly correlated (i.e. multicollinearity). We determined log-likelihood and model deviance values and calculated the percent change in deviance for each model to measure model fit (Supplemental Table 2).
Adding country-level predictors (model 2)
We added five country-level predictors to evaluate country characteristics that may predict variability in healthcare waste management access. Country-level predictors included in the model were:
Country GDP per capita in 2017 (current US$), grand mean-centred.
Access to electricity in 2017 (percentage of the country population with access), grand mean-centred.
Amount of official development assistance for WASH that was part of a government-coordinated spending plan in 2020 (current US$ millions), grand mean-centred.
Government effectiveness, defined as the perceived quality of government services, quality of policy implementation, and government commitment to upholding policies, measured in units of a standard normal distribution ranging from approximately −2.5 to 2.5.
Regulatory quality, defined as the perceived capability of the government to create and implement policies and regulations for the private sector, measured in units of a standard normal distribution ranging from approximately −2.5 to 2.5.
Using a two-level multivariate logistic regression model, we examined the relationship between these country-level predictors and the country-average odds of each outcome. Associations were expressed as log odds and converted to odds ratios. The statistical significance threshold was set at α = 0.05.
After adding country-level predictors, we re-examined the ICC and model deviance to assess changes from previous models. We calculated the percentage change in these measures compared to the null model (Supplemental Tables 1 and 2). A reduction in the model deviance value indicated a better model fit. In contrast, a lower ICC value indicated that the added predictor variables accounted for a portion of the country-level variance. We did not include random slopes in the model, as we did not hypothesize meaningful variation in slopes of predictor–outcome relationships.
Adding country-level predictor (model 3)
We created additional models incorporating all previous facility-level and country-level predictors, plus an additional predictor for countries’ average amount of WASH development assistance as a proportion of GDP in 2016 and 2018. We rescaled this predictor variable by a factor of 1000 and grand mean-centred it to aid interpretation (Enders and Tofighi, 2007; Sommet and Morselli, 2017). Data for this predictor were available for 12 of 14 countries, leading to a reduction in sample size. As a result, we have included this predictor in a third, separate model. Model associations were expressed as log odds and converted to odds ratios, with a statistical significance threshold for associations set at α = 0.05.
Ethics
The University of North Carolina-Chapel Hill Institutional Review Board and research ethics boards in each of the 14 countries included in this study reviewed and approved the data collection methods. This analysis used a publicly available de-identified dataset (The Water Institute at UNC and World Vision Inc., 2020).
Results
Healthcare facility characteristics
Survey results were available for 2002 healthcare facilities within 75 districts across 14 countries. Forty-six percent of facilities (n = 916) were classified as health centres. Approximately two-thirds (n = 1358) saw 50 or fewer patients per day. Most facilities had a dedicated infection control focal person (53%, n = 1052) and an active community oversight committee for WASH and infection control (52%, n = 1044). Sixty-eight percent of facilities (n = 1351) followed an infection control policy, and 46% (n = 913) followed a protocol for operations, maintenance, and WASH/infection control supply procurement. Fourteen percent of facilities (n = 286) reported having a sufficient WASH and infection control budget. Eight percent (n = 154) of facilities had basic waste management, defined as the safe segregation of waste and proper treatment and disposal of sharps and infectious waste (Joint Monitoring Programme, 2024). Table 1 contains an overview of facility characteristics and waste management characteristics.
Characteristics of 2002 small, rural healthcare facilities in 14 low- and middle-income countries, 2017.
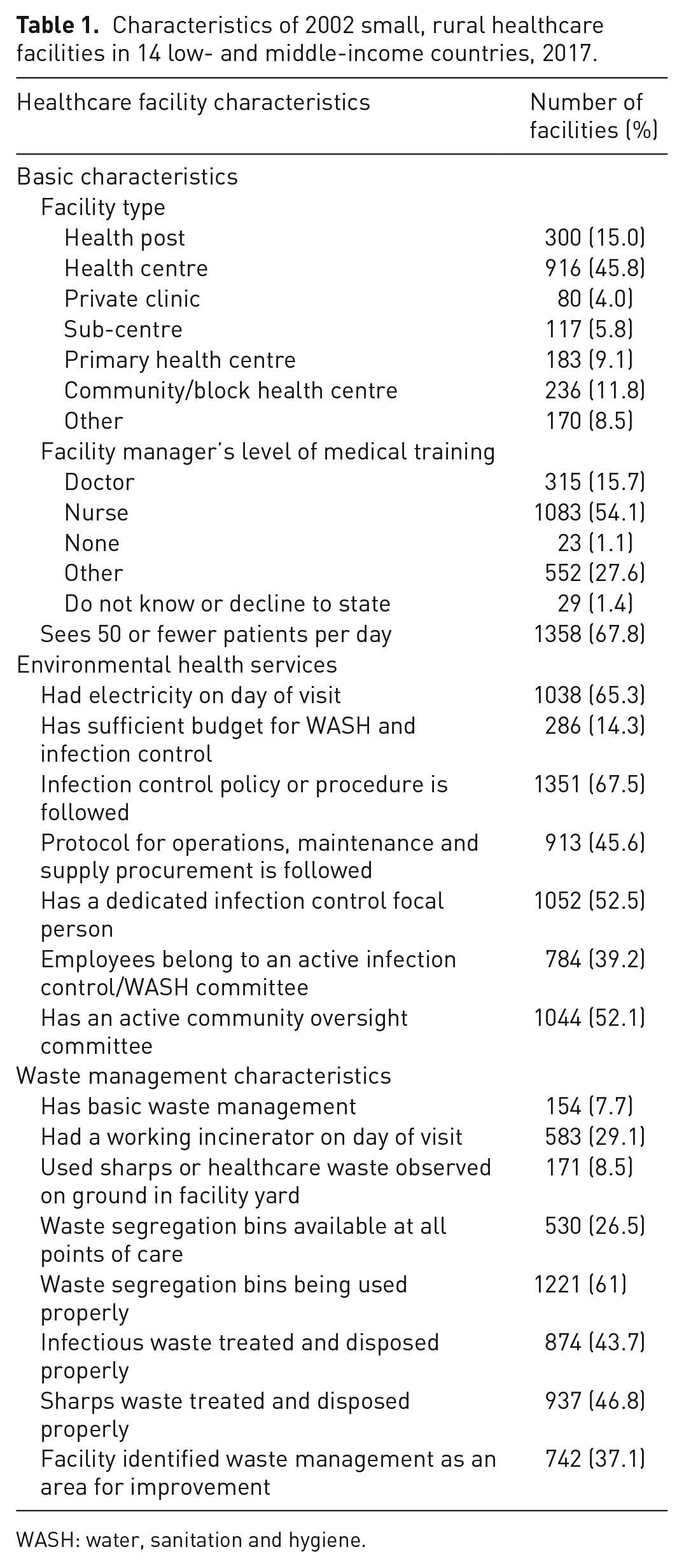

WASH: water, sanitation and hygiene.
Waste management service predictors
Intra-cluster correlation
In models with no predictor variables added, we examined the overall variance in outcomes attributable to facility-level versus country-level factors (Supplemental Table 1). The proportion of variance explained by facility-level factors ranged from 79% (for having a working incinerator) to 92% (for the presence of sharps/healthcare waste on facility grounds and the proper use of waste segregation bins). Country-level factors explained between 8% and 21% of the variance in each outcome. These ICC values indicated that a multilevel statistical approach was suitable for examining sources of outcome variance (Huang, 2018).
Working incinerator
Twenty-nine percent of facilities (n = 583) had a functioning incinerator on the day of the survey. In the multilevel model, following an operations and maintenance policy (OR: 1.41, p = 0.01), having electricity on the day of the survey (OR: 1.26, p < 0.01), and having an active WASH committee (OR: 1.33, p = 0.01) were associated with higher odds of having a working incinerator. Facilities with a higher number of average daily patients (OR: 1.28, p < 0.01) also had higher odds of having a working incinerator. Compared to health centres, there were lower odds of a working incinerator at health posts (OR: 0.50, p = 0.01).
At the country level, facilities in countries receiving a higher amount of WASH development assistance had lower average odds of having a working incinerator (OR: 0.995, p < 0.01). In the model with the country WASH budget predictor variable added, countries with a higher WASH budget as a proportion of GDP had higher average odds of having a working incinerator (OR: 1.17, p < 0.01; Table 2).
Facility-level and country-level factors associated with having a working incinerator on the day of survey.
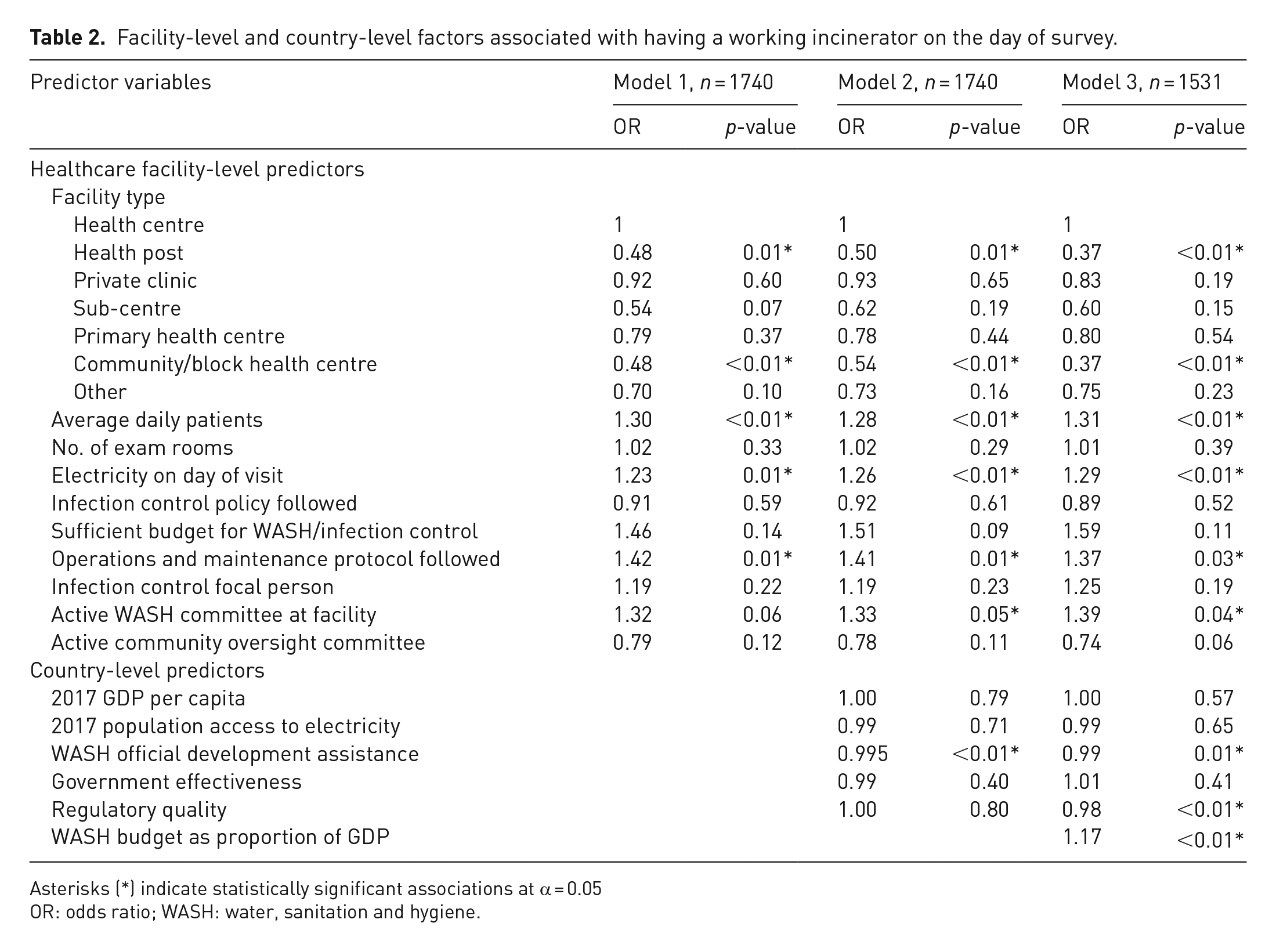
Asterisks (*) indicate statistically significant associations at α = 0.05
OR: odds ratio; WASH: water, sanitation and hygiene.
Sharps/healthcare waste on facility grounds
At 9% of facilities (n = 171), researchers observed used sharps or other healthcare waste on the facility grounds. In comparison to health centres, the odds of observing sharps and healthcare waste on the ground were lower at health posts (OR: 0.56, p < 0.01), sub-centres (OR: 0.16, p < 0.01) and primary health centres (OR: 0.49, p = 0.02). At the country level, higher official development assistance for WASH was associated with increased odds of observing sharps or healthcare waste on facility grounds (OR: 1.01, p = 0.01). In the model with a country-level WASH budget variable added, a decreased WASH budget as a proportion of GDP was associated with a decreased average odds of observing sharps or healthcare waste on the ground at healthcare facilities (OR: 0.99, p < 0.01; Table 3).
Facility-level and country-level factors associated with observing used sharps or healthcare waste on healthcare facility grounds or yard.
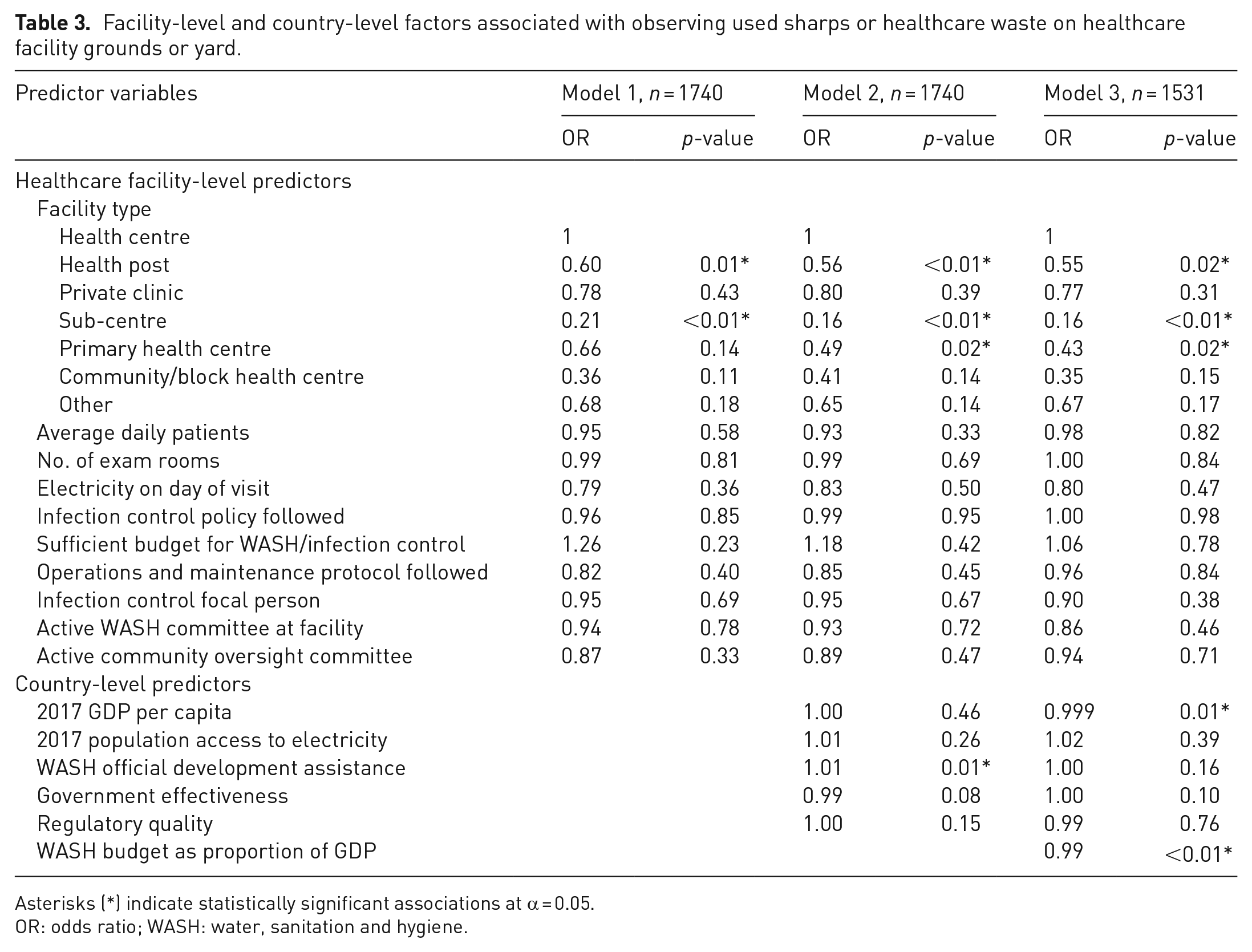
Asterisks (*) indicate statistically significant associations at α = 0.05.
OR: odds ratio; WASH: water, sanitation and hygiene.
Waste segregation bin availability and usage
Surveys assessed whether healthcare facilities had waste segregation bins at all points of care and whether bins were used properly (i.e. whether waste was segregated into the correct bins). At 27% of facilities (n = 530), waste segregation bins were available at all points of care. Healthcare facilities that had electricity on the day of visit had higher odds of having waste segregation bins available at all points of care (OR: 1.28, p = 0.02). At the country level, increased population-level access to electricity was associated with decreased average odds of having waste segregation bins at points of care (OR: 0.96, p = 0.05). An increase in country-level development assistance for WASH was associated with increased average odds of having waste segregation bins (OR: 1.01, p = 0.01; Table 4).
Facility-level and country-level factors associated with having bins for waste segregation at all points of care.
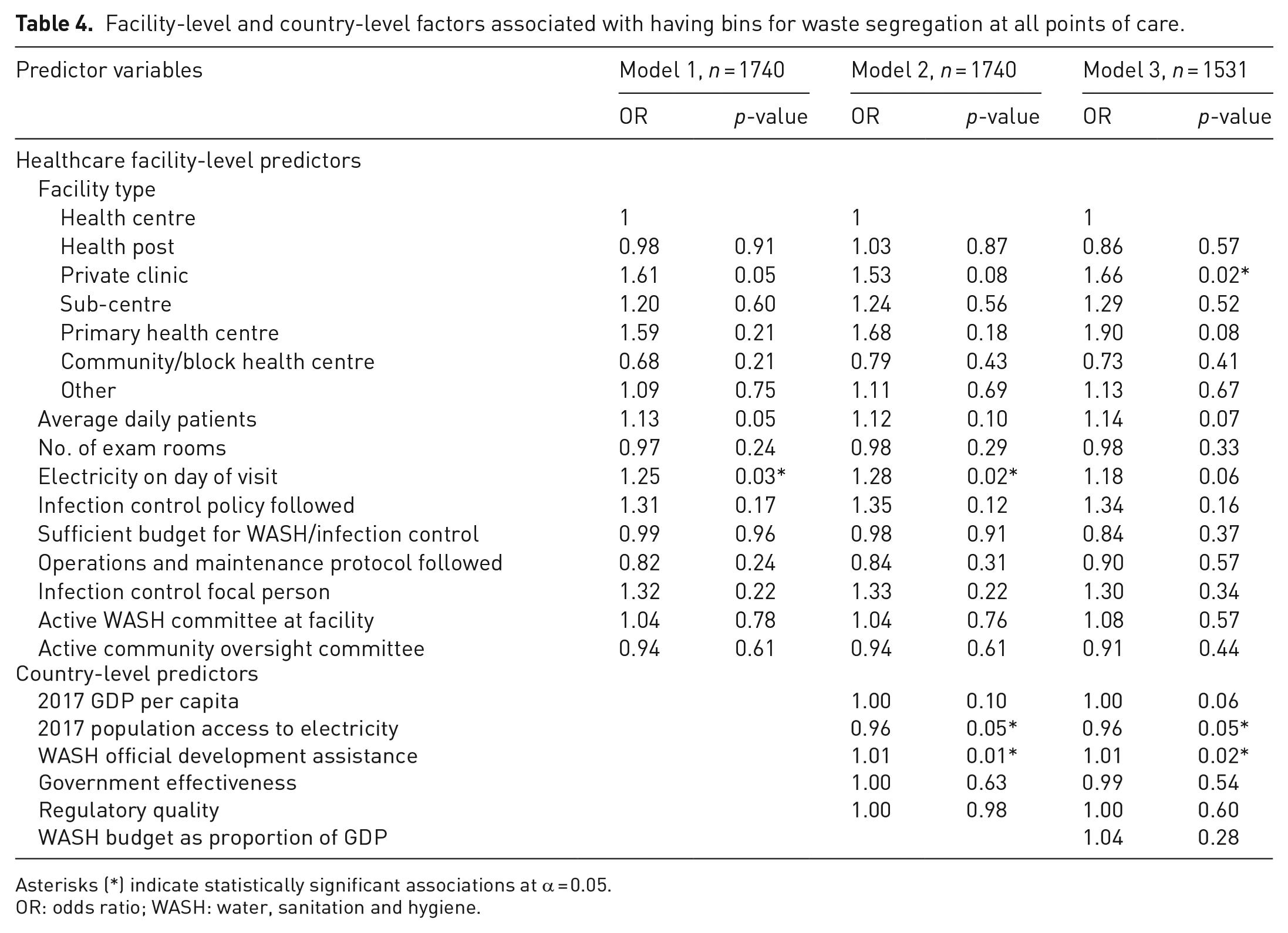
Asterisks (*) indicate statistically significant associations at α = 0.05.
OR: odds ratio; WASH: water, sanitation and hygiene.
Sixty-one percent of facilities (n = 1221) properly segregated waste in bins. Facilities with an active infection control/WASH committee had lower odds of proper bin usage (OR: 0.80, p = 0.04), whereas those with a facility type classified as ‘other’ had higher odds of proper bin usage compared to health centres (OR: 1.56, p = 0.03). No country-level predictors had a statistically significant association with this outcome (Table 5).
Facility-level and country-level factors associated with proper usage of all waste segregation bins.
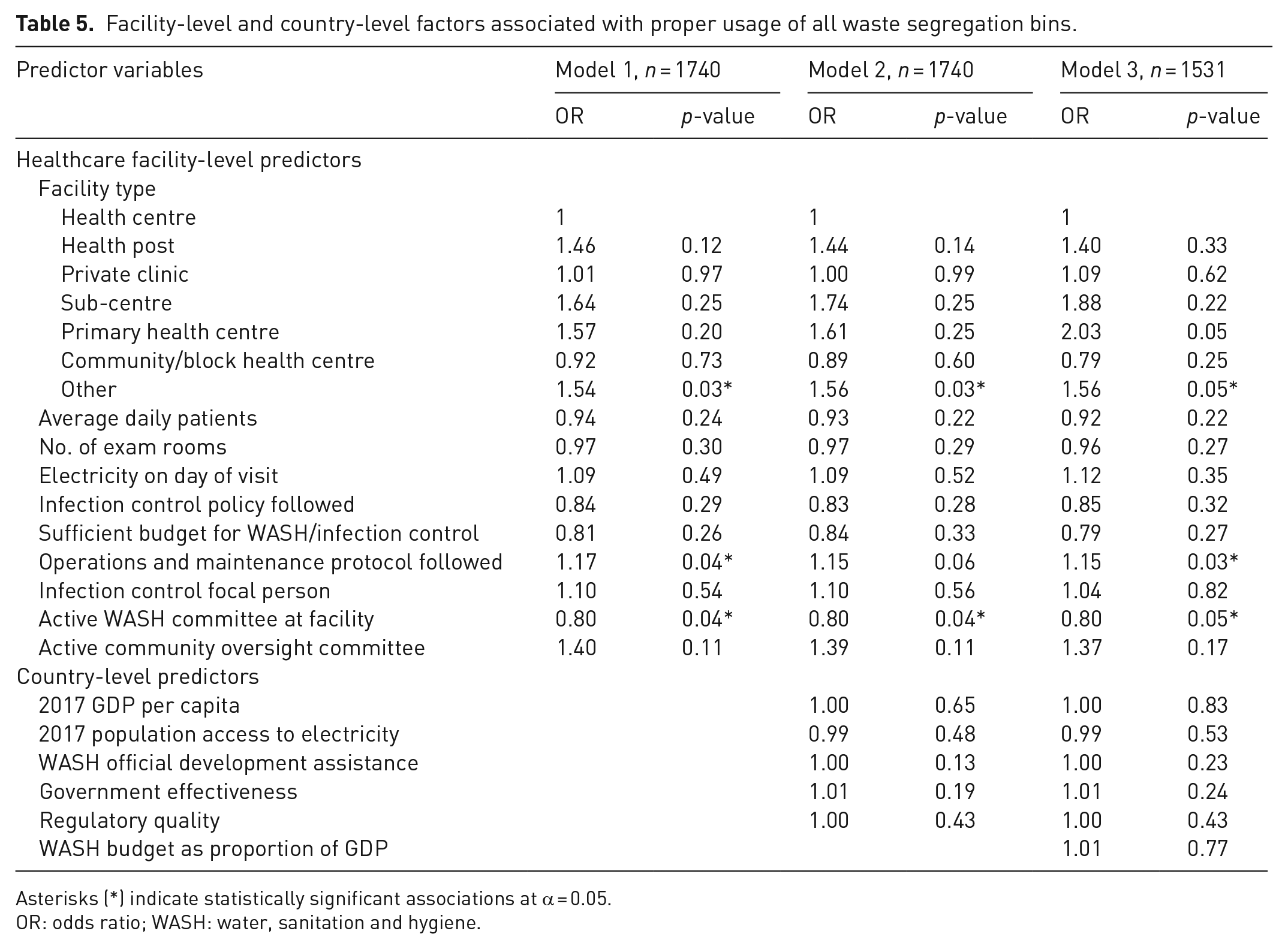
Asterisks (*) indicate statistically significant associations at α = 0.05.
OR: odds ratio; WASH: water, sanitation and hygiene.
Hazardous waste disposal
Forty-four percent of facilities (n = 874) treated and disposed of infectious waste properly. The odds of properly treating and disposing of infectious waste were higher at facilities that followed an operations and maintenance protocol (OR: 1.34, p = 0.04). In the model that included a country-level variable for the annual WASH budget, an increase in the annual WASH budget as a proportion of GDP was associated with increased average odds of practising safe infectious waste disposal (OR: 1.12, p < 0.01; Table 6).
Facility-level and country-level factors associated with proper treatment and disposal of infectious waste.
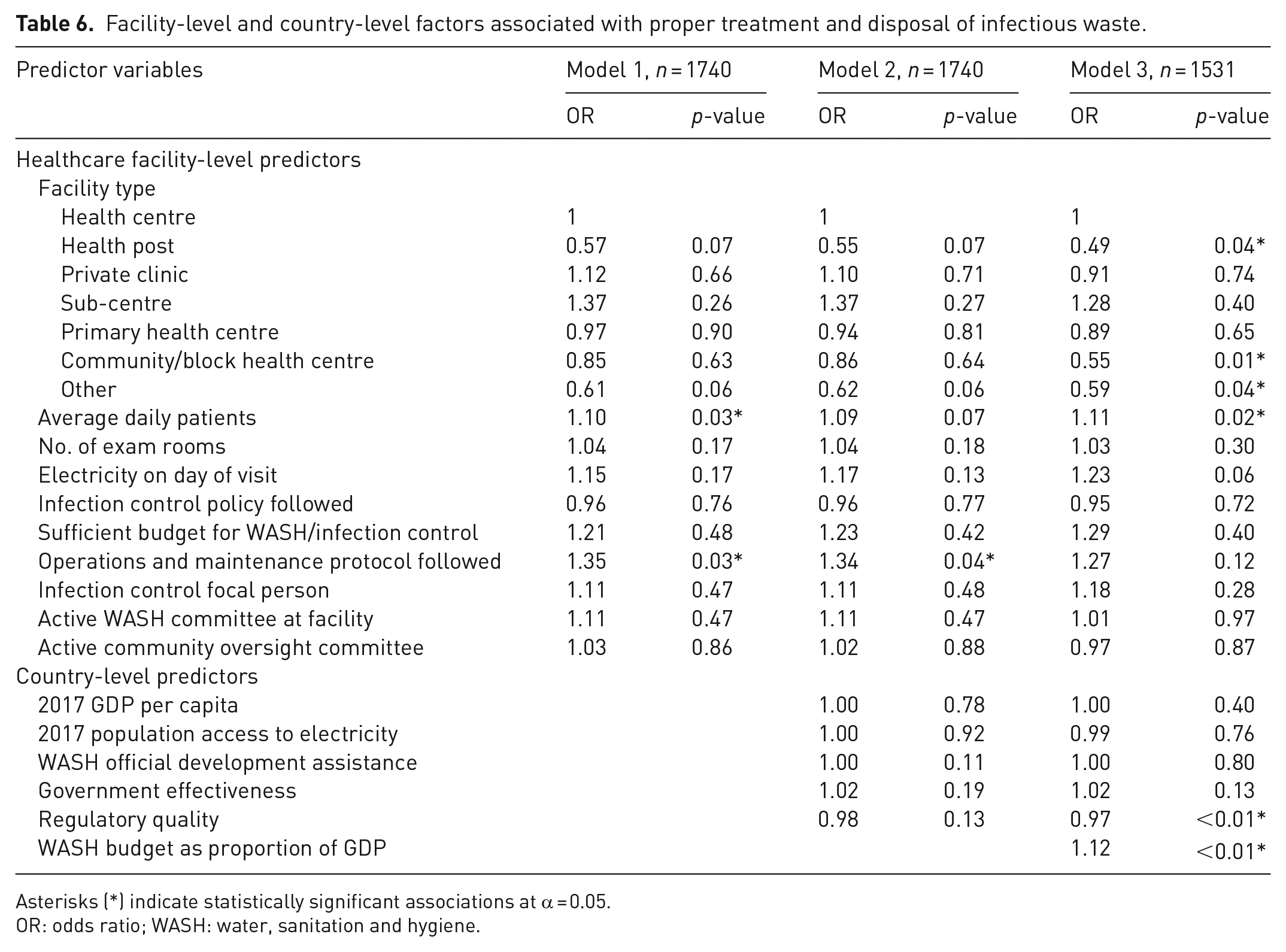
Asterisks (*) indicate statistically significant associations at α = 0.05.
OR: odds ratio; WASH: water, sanitation and hygiene.
Forty-seven percent of facilities (n = 937) treated and disposed of sharps waste properly. The odds of having proper sharps waste disposal were higher at facilities that had electricity on the day of the survey (OR: 1.48, p < 0.01). At the country level, having more official WASH development assistance was associated with higher average odds of having proper sharps waste disposal (OR: 1.002, p = 0.02). When a country-level predictor variable for annual WASH budget was added to the model, an increase in the annual WASH budget as a proportion of GDP was associated with increased average odds of having safe disposal of sharps waste (OR: 1.12, p < 0.01; Table 7).
Facility-level and country-level factors associated with proper treatment and disposal of sharps waste.
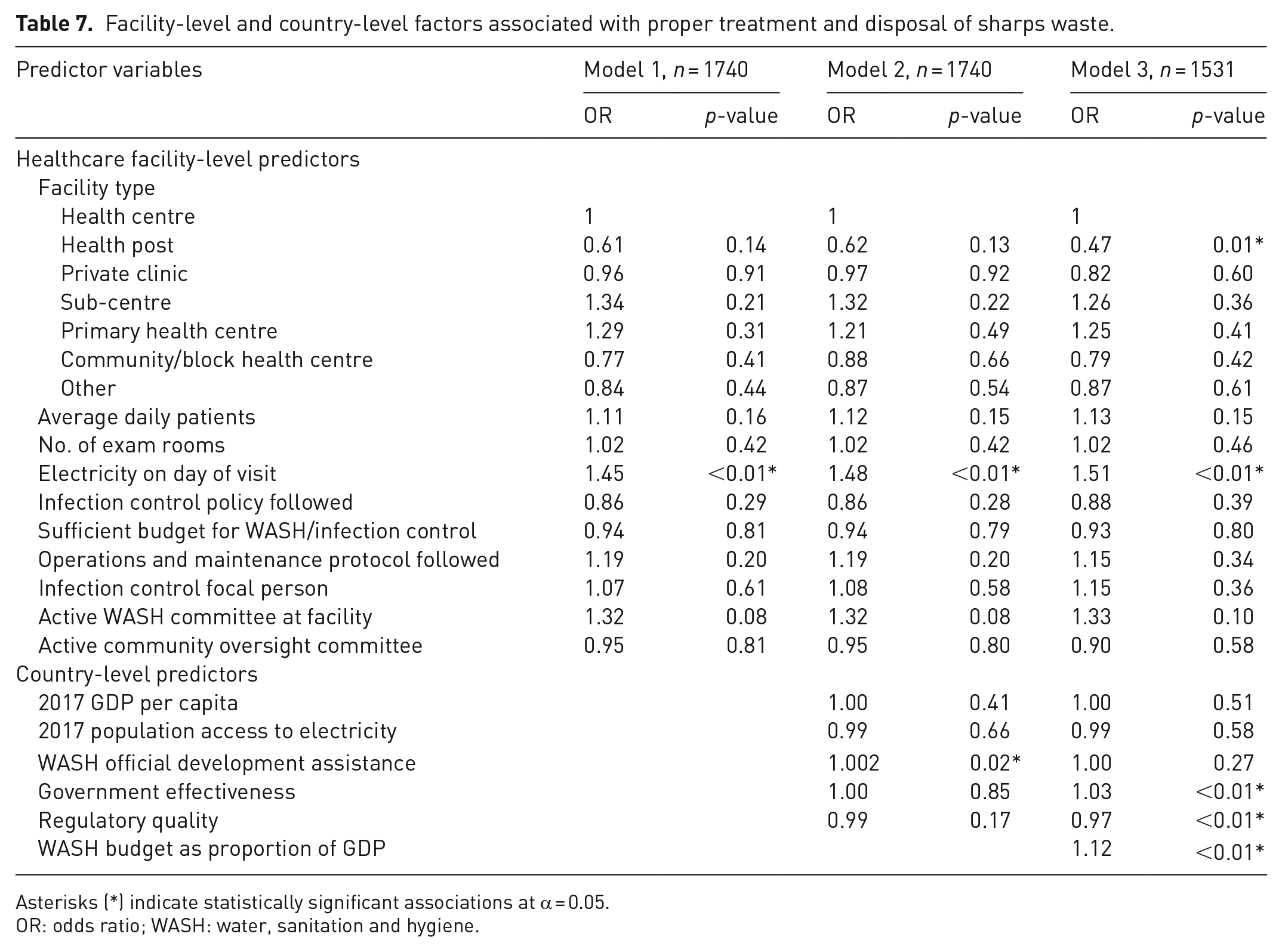
Asterisks (*) indicate statistically significant associations at α = 0.05.
OR: odds ratio; WASH: water, sanitation and hygiene.
Discussion
Waste management is an essential component of safe and high-quality healthcare, yet many healthcare facilities in low-resource settings lack access to essential components of waste segregation, treatment and disposal (Joint Monitoring Programme, 2024). This multilevel logistic regression analysis examined the drivers of healthcare waste management at both the healthcare facility and national levels. Few of the surveyed healthcare facilities had adequate services for segregating, treating and disposing of waste, reflecting trends across global low- and middle-income country settings (Joint Monitoring Programme, 2024). At the facility level, having access to electricity on the day of the survey and following a protocol for infrastructure operations and maintenance were both associated with multiple improved waste management outcomes. The amount of official WASH development assistance and WASH budget as a proportion of GDP for each country were also associated with improved waste management services. These findings highlight multiple targets for interventions to strengthen waste management and improve environmental conditions in healthcare facilities. Key recommendations for improving healthcare waste management include introducing infrastructure maintenance protocols and capacity-building at the facility level, as well as enhancing healthcare costing and budgeting processes at the national level.
This study found that facilities that followed operations, maintenance and WASH supply procurement protocols were more likely to dispose of infectious waste properly and have a working waste incinerator than facilities that did not have or follow such protocols. Prior studies have similarly found that protocols, trained staff and oversight committees are associated with access to waste management in low- and middle-income country healthcare facility settings (Assemu et al., 2020; Tilahun et al., 2023; Wafula et al., 2019). Our study used a survey measure that referred to protocols for WASH and general infection control infrastructure, rather than specifically addressing waste management infrastructure. Maintenance protocols can directly impact waste management by providing instructions for the preventive maintenance of waste-related infrastructure, or they may generate indirect impacts by fostering a culture of accountability and quality. Maintenance protocols can enhance accountability for WASH service delivery by providing information to support planning and clarifying roles and responsibilities (Pu et al., 2022). We recommend that healthcare facilities develop protocols or standard operating procedures for waste management infrastructure maintenance, including considerations for routine preventive maintenance and responding to breakdowns.
Introducing maintenance protocols and improving oversight are low-cost strategies that may be effective in improving healthcare waste management practices, drawing from other WASH maintenance interventions (Buxton et al., 2019). International guidelines for improving WASH and waste management in healthcare facilities, such as the World Health Organization’s WASH FIT tool, recommend identifying staff leaders, assigning responsibilities for quality improvement and integrating operations and maintenance into improvement plans (World Health Organization, 2022b). Beyond protocol development, however, small and rural healthcare facilities may lack the funding, technical expertise and access to supplies required to perform maintenance of waste management infrastructure routinely (Tantum et al., 2024). Researchers and programme implementers should explore strategies to support maintenance in these settings, such as by providing long-term technical maintenance support, circuit-riders or connecting facilities with professional service providers (Sustainable WASH Systems Learning Partnership, 2020).
Healthcare facilities that had electricity on the day of data collection were more likely to have a working waste incinerator and proper disposal of sharps waste. Although electricity access plays a role in many aspects of healthcare delivery – and may affect functionality of some waste management infrastructure, such as autoclaving (World Health Organization et al., 2023) – it is unlikely to have directly impacted the burner-style incinerators that were present at many of the facilities included in our study sample. Instead, electricity access may provide a representation of facility wealth more generally, as facility electrification requires financing for upfront capital costs and ongoing maintenance (World Health Organization et al., 2023). Healthcare facilities with access to more financial resources may be better equipped to purchase and maintain waste management infrastructure.
Financial determinants of waste management also occurred at the regional and national levels in our study. The amount of official development assistance for WASH and country WASH budgets as a proportion of GDP for each country were associated with variations in several outcomes, including having a working incinerator, observing healthcare waste on facility grounds, having segregation bins at all points of care and following proper sharps and infectious waste disposal procedures. National costing and budgeting for WASH and waste management in healthcare facilities is essential for creating and sustaining improvement (World Health Organization, 2019). Global investment is needed to improve WASH and waste management services. By one estimate, achieving full coverage of basic waste management in healthcare facilities in least-developed countries by 2030 requires an overall investment of US$3.7 billion, including a median investment of $10,159 in capital costs and $1750 in recurrent operations and maintenance costs for non-hospital facilities (Chaitkin et al., 2022). However, disparities between policy and available financing undermine improvement: In a 2021–2022 survey of 118 countries, 41% had a formally approved policy and plan for WASH in healthcare facilities, but just 24% had costed their plan, and 3% had sufficient financial and human resources to fund their plan (World Health Organization, 2022a).
International development assistance may support investments in waste management infrastructure. Still, evidence from the WASH sector indicates that poor regulatory quality in low- and middle-income countries hampers the effectiveness of aid (Wayland, 2018). Foreign aid for healthcare waste management can achieve a greater impact when coupled with investment in local capacity building. Programmes to guide policymakers in the process of creating costed roadmaps and budgets may effectively increase and sustain government financing for healthcare waste management (Chettry et al., 2024). Furthermore, advocacy to regional and national decision-makers may help establish healthcare waste management as a priority (Chettry et al., 2024; Hepworth et al., 2022). To improve costing and budgeting, healthcare facilities should track the costs associated with establishing and maintaining waste management services. Facilities and implementing partners should work with policymakers to ensure that these costs are integrated into budgetary allocations.
Limitations
This study has several limitations. At both the healthcare facility and country levels, we included several predictor variables related to WASH and infection control in general, but not specific to healthcare waste management. Although WASH and infection control typically include waste management in healthcare facility settings, the broad nature of these predictor variables could contribute to a misestimation of the effect. Data were collected via cross-sectional surveys, so it is not possible to establish causality of relationships or evaluate seasonal variation and time trends. Country-level predictor variables were derived from different datasets than the healthcare facility-level predictor and outcome variables. Some country predictors were collected in different years than the healthcare facility predictors. Variations in data sources, data collection approaches and timing may contribute to the misestimation of associations between country-level predictors and the outcome.
Conclusions
This study offers novel insights into the factors driving access to healthcare waste management at both facility and country levels. Findings suggest that administration and management, as well as access to electricity, play a role in supporting waste management in healthcare facilities. We recommend implementing protocols, oversight and preventive maintenance for healthcare waste infrastructure to enhance access to safe waste disposal. That said, country characteristics also play a role in waste management, and interventions to strengthen policy and financing mechanisms may contribute to sustained improvement. Waste should be included in healthcare facility WASH interventions at a country level and incorporated into national standards, costed roadmaps and budgets. Country-level monitoring is needed to supervise and implement roadmaps. International aid programmes should consider incorporating capacity-building for costed roadmap development and monitoring into their investments. Further research to collect and analyse data on regional- and national-level determinants of healthcare waste management could guide advocacy and intervention. Strategies to improve management and oversight of waste management at the healthcare facility level, while simultaneously addressing national financing gaps, will improve global access to safe and high-quality healthcare.
Supplemental Material
sj-pdf-1-wmr-10.1177_0734242X251371609 – Supplemental material for Determinants of access to waste management services in healthcare facilities in 14 low- and middle-income countries
Supplemental material, sj-pdf-1-wmr-10.1177_0734242X251371609 for Determinants of access to waste management services in healthcare facilities in 14 low- and middle-income countries by Lucy K Tantum, Darcy M Anderson, Ute Pieper and Ryan Cronk in Waste Management & Research
Footnotes
Acknowledgements
The authors are grateful to the healthcare facility staff who participated in this study. The authors also thank Todd Jensen for his guidance in statistical analysis.
Author contributions
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded in part by World Vision (Federal Way, WA, USA; Grant No. 24925) and was supported by World Vision staff, consulting firms and enumerators in each country. This work was also supported in part by the Wallace Genetic Foundation. LKT was supported by the National Science Foundation Graduate Research Fellowship under Grant No. DGE-2040435. DMA was supported in part by a grant from the National Institute of Environmental Health Sciences (NIEHS; T32ES007018).
Ethics statement
The University of North Carolina-Chapel Hill Institutional Review Board and research ethics boards in each of the 14 countries included in this study reviewed and approved the data collection methods. This analysis used a publicly available de-identified dataset.
Data availability statement
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
