Abstract
This study identified care and support need profiles for people requiring home-based aged care and explored profile associations with socio-demographic and psychosocial factors. The study utilized cross-sectional aged care assessment data for 94,975 Victorians (mean age 84 [SD = 7.6] years) eligible for Australian Government-funded home-based aged care (Home Care Package) (January 2019–June 2022). Latent class analysis identified seven profiles (P1 to P7). P1, the largest profile (n = 23,487, 24.7%), included those with predominantly basic needs, for example, housework (93%) and shopping (68%). Needs gradually increased from P1 to P7. P7 (n = 9,274, 9.8%) included those with the most advanced needs, for example, showering (99%), medication management (99%), walking (89%), short-term memory loss (99%), and disorientation to time (93%). Individuals living alone were under-represented in higher-need profiles (P4 to P7). The identified profiles provide valuable insights to optimize care management, service-type requirements, and workforce skills tailored to the needs of people within each profile.
Keywords
• Using a population-based routinely collected aged care assessment database containing detailed information about the day-to-day needs of 94,975 people requiring home-based aged care, we identified seven distinct care and support needs profiles (P1–P7). • Care and support needs gradually increased from P1 to P7 and included activities-of-daily-living and cognitive/behavioral/psychological support needs as well as physical/clinical care requirements. • People with an informal carer or with psychosocial complexity were more likely to be classified in higher-need profiles (P4–P7).
• Aged care providers and their workforce could utilize such profiles to inform care planning and tailor service delivery for individuals. • Profiles like these can also highlight workforce skill and skill mix requirements to meet the different care and support needs within each profile, thereby aiding workforce planning at both system and provider levels. • Future research should incorporate data on care outcomes to enhance understanding of which service types and workforce skills best support people within different profiles. In Australia, this information is not yet systematically collected.What this paper adds
Applications of study findings to gerontological practice, policy, and/or research
Introduction
With aging populations around the world (United Nations, 2024), the demand for long-term care is rising to support older adults with day-to-day, social, and healthcare activities that they can no longer manage independently (World Health Organization [WHO], 2022). In most developed countries, governments fund formal long-term care programs, which complement the care provided by informal caregivers (Organisation for Economic Co-operation and Development, n.d.). Most older people prefer to receive long-term care in their home (National Seniors Council, 2024; Ratcliffe et al., 2020). The Australian Government has been providing increasing home-based aged care funding over recent decades to support this preference (Duckett & Swerissen, 2021), and it has also been a policy focus because home-based aged care is viewed as less costly than residential care (Chappell et al., 2004). As of June 2023, approximately 1 million older Australians were receiving government-funded home-based aged care, representing nearly one-quarter of the population aged 65 and over (Australian Bureau of Statistics [ABS], n.d.). Designing contemporary government-funded home-based aged care programs to effectively and efficiently support the day-to-day, social, and healthcare needs of such a volume of people is a complex task (Abdi et al., 2019). However, this challenge must be addressed in the context of increasing demand for care, limited government funding, and shortages of human resources necessary to deliver the required care (Australian Healthcare and Hospitals Association, 2021).
General information about the two current Australian home-based aged care programs
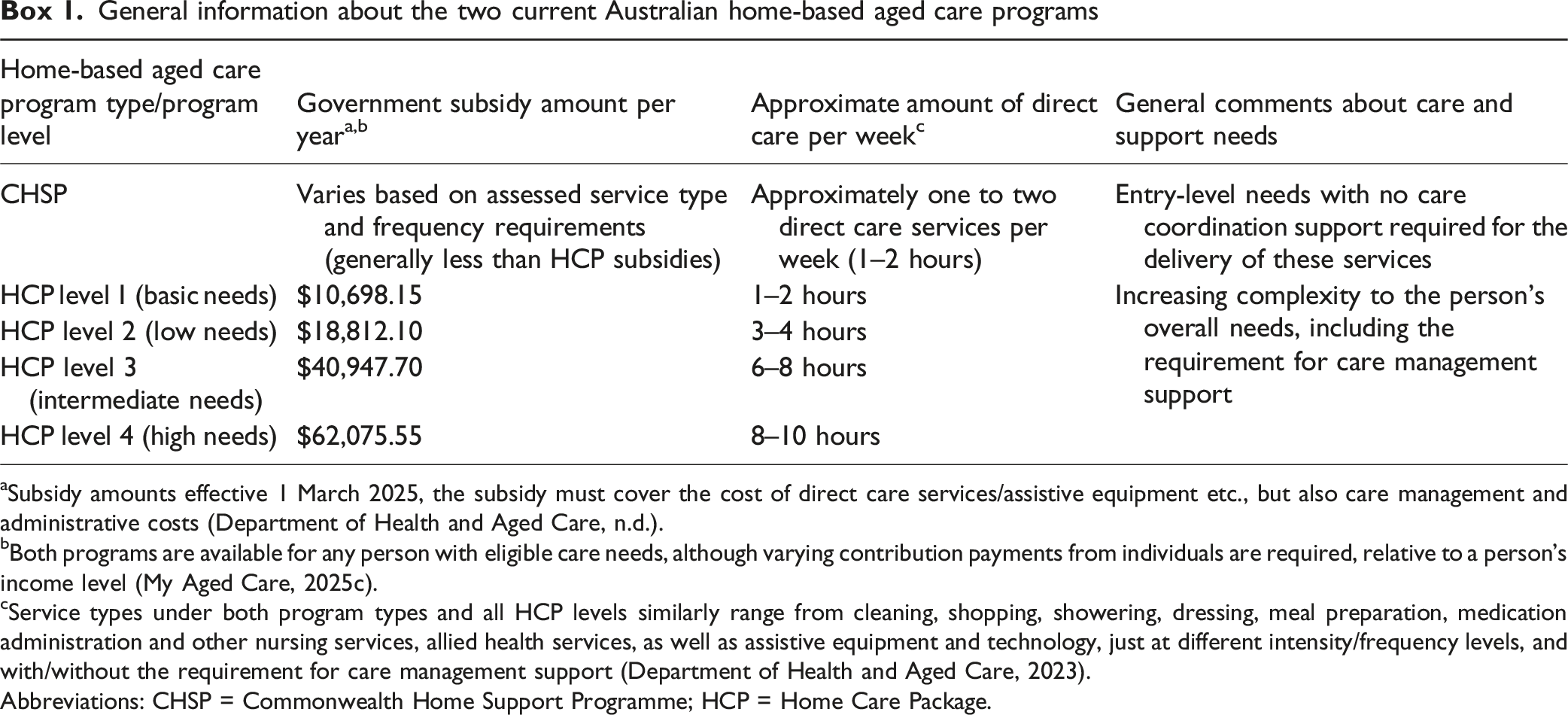

aSubsidy amounts effective 1 March 2025, the subsidy must cover the cost of direct care services/assistive equipment etc., but also care management and administrative costs (Department of Health and Aged Care, n.d.).
bBoth programs are available for any person with eligible care needs, although varying contribution payments from individuals are required, relative to a person’s income level (My Aged Care, 2025c).
cService types under both program types and all HCP levels similarly range from cleaning, shopping, showering, dressing, meal preparation, medication administration and other nursing services, allied health services, as well as assistive equipment and technology, just at different intensity/frequency levels, and with/without the requirement for care management support (Department of Health and Aged Care, 2023).
Abbreviations: CHSP = Commonwealth Home Support Programme; HCP = Home Care Package.
Gaining more detailed insights into the range and prevalence of care and support needs experienced by people requiring home-based aged care, and how these needs group together to form different care and support needs profiles within this population, may assist policymakers and home-based aged care providers to design programs which can efficiently and effectively address care and support needs across such profiles or sub-groups of people (Calver et al., 2004). However, there is limited current knowledge about the range of day-to-day, social, and healthcare needs experienced by older people seeking home-based aged care. Studies using routinely collected, population-based datasets consistently indicate that while domestic and community access needs are common, many people also require assistance for personal care and clinical needs (Chong et al., 2024; McKittrick et al., 2025; Schluter et al., 2016). To date, little research has focused on identifying profiles of people requiring home-based aged care. Saari et al. (2024) recently conducted a study using routinely collected data, identifying six distinct needs profiles among community-dwelling older adults in Ontario, Canada. Liu and Yao (2014) have also developed four needs profiles for recipients of a government home-based long-term care program, also using routinely collected needs data. Authors of both studies suggest that the developed profiles could support an evidence-informed and person-centered approach to health and social care, by better aligning services offered with care and support needs (Liu & Yao., 2014; Saari et al., 2024). These authors argue improved alignment between needs and services to address recognized needs may reduce unmet needs and improve care outcomes, including better quality of life, delayed residential care entry, and fewer hospitalizations (Gilmour, 2018; Saari et al., 2024). No similar research has been conducted in the Australian context.
Using a large, routinely collected aged care assessment dataset for people living in the Australian state of Victoria and requiring an HCP, we previously conducted a study aimed at describing the range and prevalence of socio-demographic characteristics and day-to-day care and support needs of older Victorians approved for an HCP, both within the overall population requiring an HCP and by each HCP level (McKittrick et al., 2025). For the study being reported here, we wanted to explore care and support needs profiles in this population. The rationale was that such profiles would provide more nuanced information to guide the services and workforce requirements that people within the profiles might require. The study specifically aimed to (1) identify profiles of care and support needs for people living in Victoria, approved for an HCP, and (2) explore associations between the profiles, and socio-demographic characteristics and psychosocial factors.
Methods
Study Design, Setting, and Population
This cross-sectional study used a large, routinely collected population-level dataset, containing detailed information about the demographic characteristics and day-to-day care and support needs of 94,975 people living in Victoria (a state of Australia) who were approved for an HCP between January 2019 and June 2022.
Data Source
De-identified NSAF information for all Victorians approved for an Australian government-funded HCP, as contained in the NSAF dataset (2022 version; collated from individual-level NSAF information), was obtained from the Australian Institute of Health and Welfare (AIHW). Of the 94,975 people within the study dataset, 12,060 had undergone more than one assessment. Only the most recent assessment for each individual was retained, as the best reflection of their “current” needs. While most assessments were conducted face-to-face, over some months of 2020 and 2021, for some regions in Victoria, assessments were conducted via phone or telehealth due to restrictions on face-to-face contact in the COVID pandemic context.
Ethics exemption approval to conduct the study using this dataset was provided by Deakin University Human Research Ethics Committee (HREC) in May 2022 (#2022-132). The HREC deemed that use of the de-identified data, incidentally comprising people from a range of population sub-groups, including people identifying as Aboriginal and/or Torres Strait Islanders, did not require specific Aboriginal HREC approval in order to report their data, as part of describing the study population. This is in accordance with the past and current National Statement on Ethical Conduct in Human Research (National Health and Medical Research Council [NHMRC] et al., 2018, 2023) and additional NHMRC guidance (NHMRC, n.d.).
Measures
The full list of variables contained within the NSAF dataset is listed in Supplemental File 1.
The NSAF dataset consists of information on activities-of-daily-living (ADL) support needs (e.g.. walking, showering/bathing, toileting (bladder), and housework) measured on a 3-point Likert scale (“no,” “some,” or “high level” of assistance required); cognitive/behavioral/psychological support needs (e.g., short-term memory loss, impaired judgement, risky behavior, physical aggression, loneliness. and social isolation) measured on a 4-point Likert scale with anchors “never” and “always”; and physical/clinical care requirements (e.g., poor vision, swallowing problems, major skin conditions, and history of falls) measured as “present” or “not present.” For this analysis, ADL and cognitive/behavioral/psychological support needs were re-coded as binary (0 = no needs; 1 = some level of needs).
The dataset also includes information on approved HCP level; demographic characteristics (e.g., age, gender, and living situation); psychosocial considerations including social support situation (e.g., carer status); vulnerability factors (e.g., socially isolated, culturally and linguistically diverse, carer sustainability concerns, and Aboriginal and Torres Strait Islander); and complexity indicators (e.g., significant cognitive changes, self-neglect, mental health issues, and inadequate housing). For this analysis, living situation was re-coded as binary (0 = lives with partner/family/others; 1 = lives alone). The number of vulnerability factors or complexity indicators (multi-vulnerabilities, multi-complexities) was calculated and collapsed to 0, 1, 2, 3+. Please note, the term “vulnerability factors” is used with acknowledgment that it can be regarded as implying inferiority or reduced agency on the part of people/groups of people described in this way, potentially contributing to their stigmatization (Munari et al., 2021). However, within the NSAF dataset used for this study, people identified as experiencing such factors have been defined as at an increased risk of vulnerability and as likely to require additional support to access aged care services (MAC, 2018; see Supplemental File 1 for more details). Accordingly, we have retained the term for consistency with the dataset definitions.
Statistical Analysis
Latent class analysis (LCA) was used to identify classes or profiles of care and support needs within the population of people requiring an HCP in Victoria. LCA is used to identify unobserved (latent) subgroups within a population by analyzing individuals’ responses to observed variables. It assumes that the population is heterogeneous and can be divided into distinct, mutually exclusive “latent classes,” where individuals within each class share similar characteristics or response patterns. This statistical approach estimates the probability of class membership for each individual and the likelihood of specific responses within each class (Aflaki et al., 2022; Weller et al., 2020).
List of 30 indicator variables used for latent class analysis (and their categories)

Modeling: We fitted LC models with 2 to 9 classes. The optimal number of classes was based on statistical criteria and theoretical interpretability (Aflaki et al., 2022; Weller et al., 2020). Each model was fitted 100 times with random starting values for model parameters. We measure the percentage of models with the best fit (measured by log-likelihood), which measures how well a model is identified (Lanza et al., 2007). We also report the Bayesian Information Criterion (BIC), adjusted BIC (ABIC), Akaike Information Criterion (AIC), consistent AIC (CAIC), and the entropy index. Lower BIC, ABIC, AIC, and CAIC values generally indicate a better fit, while an entropy index above 0.80 suggests well-separated classes (Weller et al., 2020).
After selecting the optimal number of classes, item-response probabilities were examined to identify the items characterizing each profile, using 0.4 as a general cut-off value. The item-response probabilities informed the labeling of classes/profiles. Individuals were then assigned to the class with the highest posterior probability, that is, the estimated probability that a person belongs to a given class. Lastly, we explored associations between class membership and selected socio-demographic characteristics, psychosocial considerations, and approved HCP level using the chi-squared test.
SAS Analytical software version 9.4 was used for all analyses; PROC LCA was used to fit LC models (Lanza et al., 2007). Missing data were minimal and had no impact on selection of variables used in the LCA. The 30 items included in the LCA had less than 0.001% missing data each; demographic variables included in this study had less than 0.3% missing data each. This low level of missing data was likely because most NSAF variables are mandatory for assessors to complete.
Results
Prevalence of selected socio-demographic characteristics among people approved for a Home Care Package (HCP) between January 2019 and June 2022, Victoria, Australia
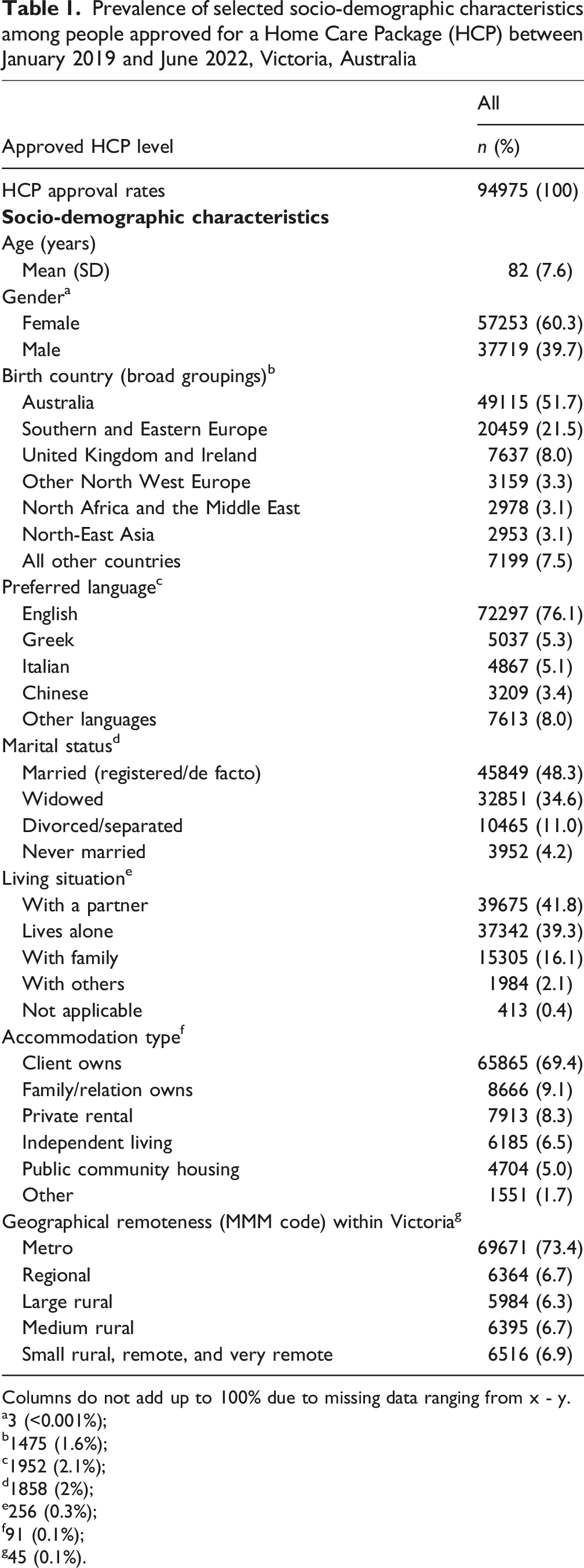

Columns do not add up to 100% due to missing data ranging from x - y. a3 (<0.001%);
b1475 (1.6%);
c1952 (2.1%);
d1858 (2%);
e256 (0.3%);
f91 (0.1%);
g45 (0.1%).
Latent Classes of Care and Support Needs
Fit indices for latent class models with 2 to 9 classes
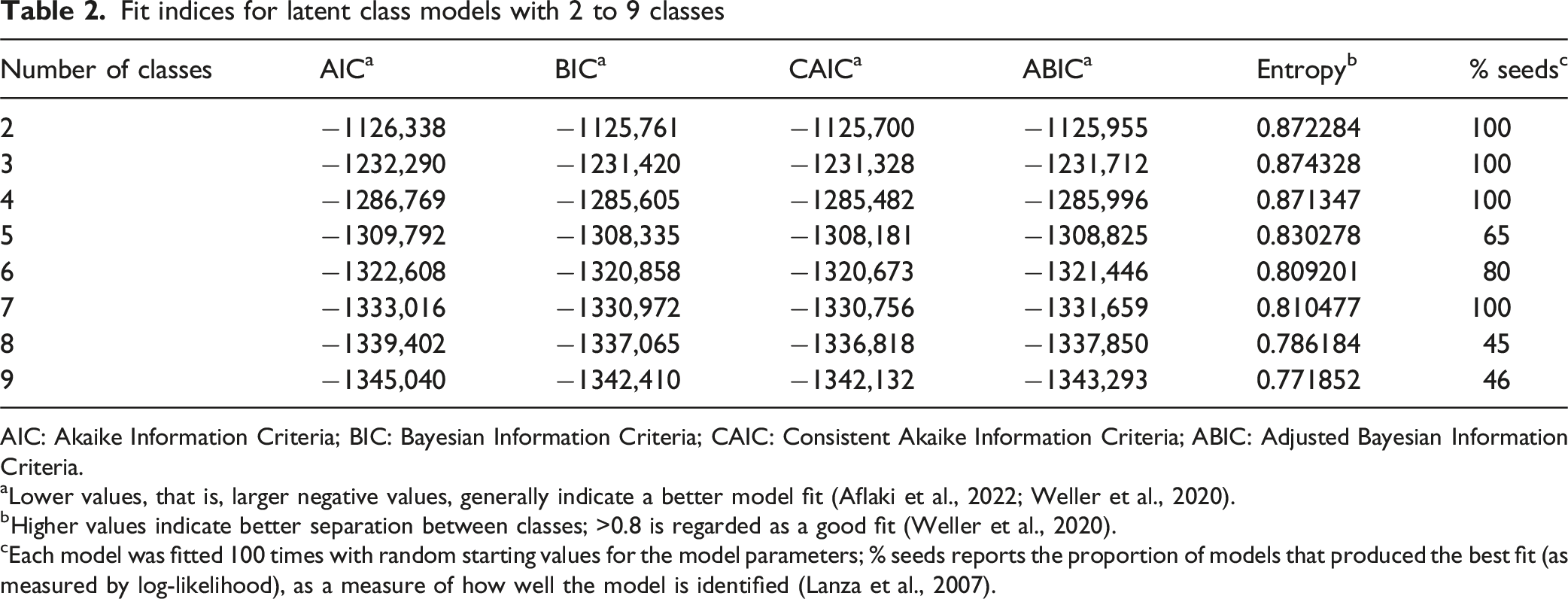
AIC: Akaike Information Criteria; BIC: Bayesian Information Criteria; CAIC: Consistent Akaike Information Criteria; ABIC: Adjusted Bayesian Information Criteria.
aLower values, that is, larger negative values, generally indicate a better model fit (Aflaki et al., 2022; Weller et al., 2020).
bHigher values indicate better separation between classes; >0.8 is regarded as a good fit (Weller et al., 2020).
cEach model was fitted 100 times with random starting values for the model parameters; % seeds reports the proportion of models that produced the best fit (as measured by log-likelihood), as a measure of how well the model is identified (Lanza et al., 2007).
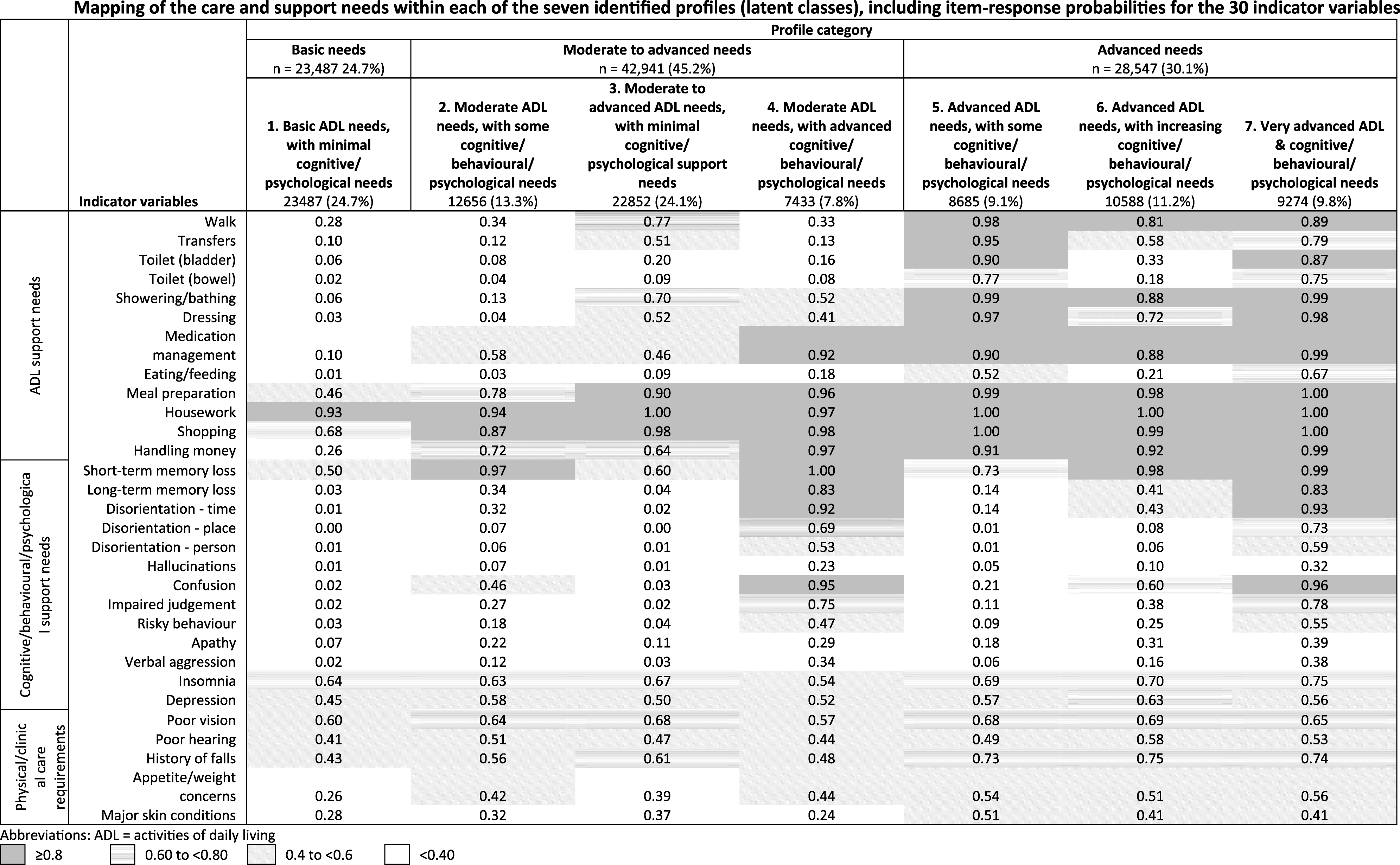
Mapping of the Care and Support Needs Within Each of the Seven Identified Profiles (Latent Classes), Including Item-Response Probabilities for the 30 Indicator Variables. Abbreviations: ADL = Activities of Daily Living
Overall, needs associated with domestic and community ADLs were highly likely in the study population (Figure 1); assistance with housework (>93% across all profiles), assistance with shopping (≥87% in all but profile 1), and assistance with meal preparation (≥90% in all but profiles 1 and 2). From profile 3 up to profile 7, other ADL support needs increased. For example, the need for assistance with personal care ADLs, such as medication management, had a minimum item-response probability of 88% for profiles 4–7 (Figure 1). In addition to ADL support needs, cognitive/behavioral/psychological support needs were present for people in certain profiles. People in profiles 2, 4, 6, and 7 had high likelihood of requiring support for short-term memory loss (≥97%). Profiles 4 and 7 had advanced cognitive/behavioral/psychological support needs, including for confusion (≥95%) disorientation to time (≥92%), disorientation to place (≥69%), and impaired judgement (≥75%). People in these profiles were also somewhat likely to need support for insomnia (≥54%), disorientation to person (≥53%), depression (≥52%), and risky behavior (e.g., dangerous use of kitchen appliances and high levels of impulsivity) (≥47%). Of note, physical/clinical care requirements, for example, history of falls, appetite/weight concerns were present across all profiles, seeming not to relate directly to the degree of ADL or cognitive/behavioral/psychological care and support needs.
The largest class, profile 1 (n = 23,487, 24.7%), included those highly likely to need help with housework (93%) and shopping (68%), and experiencing insomnia (64%), short-term memory loss (STML) (50%), and depression (45%). Even though people within this profile had somewhat basic needs overall, they were still likely to have clinical care requirements such as for poor vision (60%), poor hearing (41%), and a falls history (43%).
Profile 7 (9,274, 9.8%) consisted of people with very advanced ADL and cognitive/behavioral/psychological support needs, as well as other physical/clinical care requirements. Item-response probabilities (Figure 1) for 21 of the 30 indicator variables were >65%. ADL care needs were highly likely to include showering (99%), medication management (99%), dressing (98%), walking (89%), and toileting (bladder) (87%). Highly likely cognitive/behavioral/ psychological support needs were STML (99%), confusion (96%), disorientation to time (93%), and LTML (83%). People in this group were likely to also require help with transfers (79%), toileting (bowel) (75%), and eating (67%). Further, concerns with impaired judgement (78%) and disorientation to place (73%) were likely, and somewhat likely were disorientation to person (59%) and risky behavior (55%).
Associations Between Care and Support Needs Profiles and Socio-Demographic Characteristics, Psychosocial Factors, and HCP Level
Distribution of selected socio-demographic characteristics, psychosocial considerations, and Home Care Package level across care and support needs profiles c
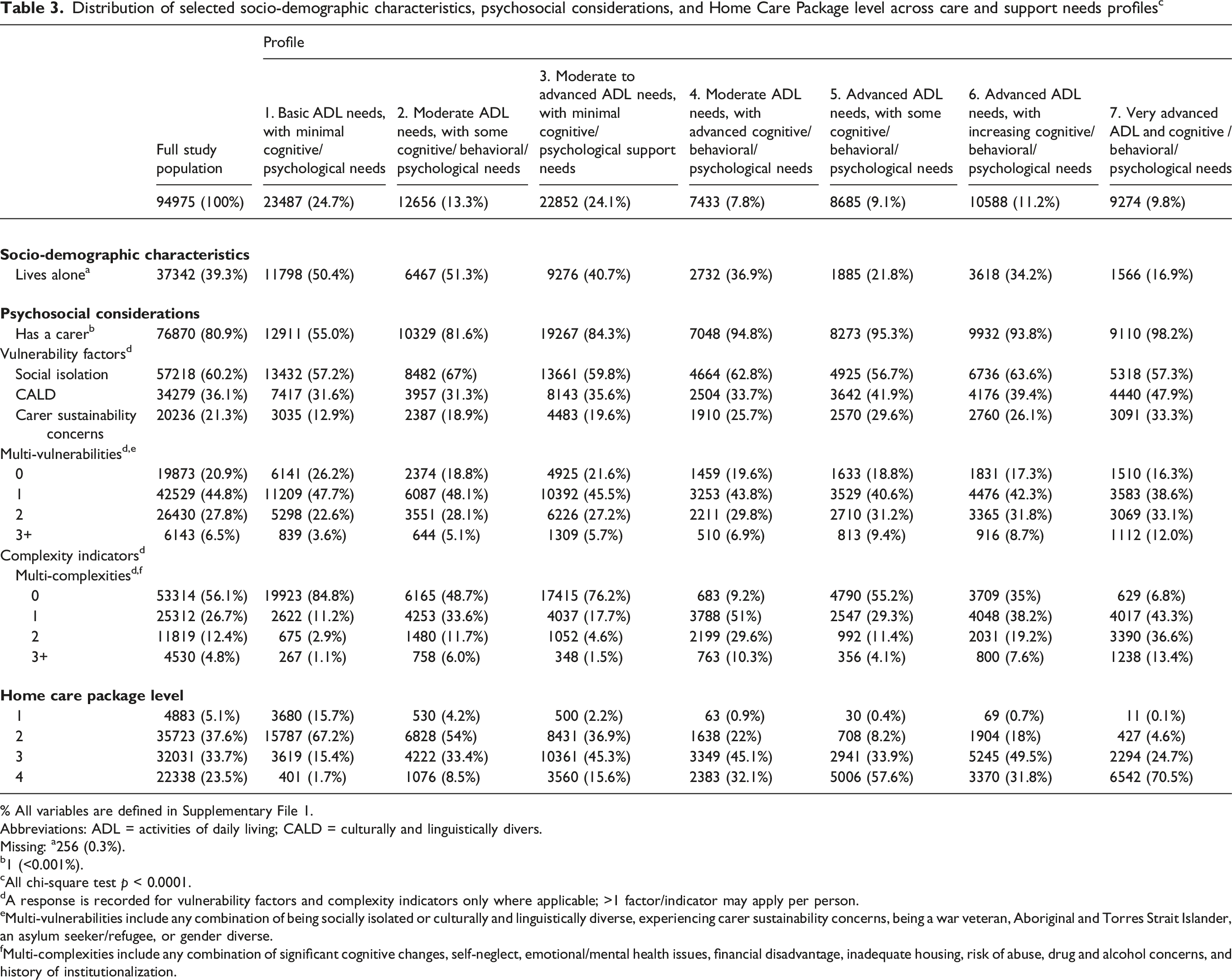
% All variables are defined in Supplementary File 1.
Abbreviations: ADL = activities of daily living; CALD = culturally and linguistically divers.
Missing: a256 (0.3%).
b1 (<0.001%).
cAll chi-square test p < 0.0001.
dA response is recorded for vulnerability factors and complexity indicators only where applicable; >1 factor/indicator may apply per person.
eMulti-vulnerabilities include any combination of being socially isolated or culturally and linguistically diverse, experiencing carer sustainability concerns, being a war veteran, Aboriginal and Torres Strait Islander, an asylum seeker/refugee, or gender diverse.
fMulti-complexities include any combination of significant cognitive changes, self-neglect, emotional/mental health issues, financial disadvantage, inadequate housing, risk of abuse, drug and alcohol concerns, and history of institutionalization.
Individuals living alone were over-represented in profiles 1 and 2 but under-represented in profiles 5 and 7. Those with informal carers were over-represented in profiles 4, 5, 6, and 7. Those with vulnerability factors (social isolation, culturally and linguistically diverse, carer sustainability concerns) were more likely to be present in the more advanced needs profiles, that is, profiles 5, 6, and 7. Those with 2 or 3 vulnerabilities (any combination of being socially isolated, culturally and linguistically diverse, a war veteran, Aboriginal and Torres Strait Islander, an asylum seeker/refugee or gender diverse, or experiencing carer sustainability concerns) were over-represented in profile 7. Similarly, people with one or more complexity indicator (any of experiencing significant cognitive changes, self-neglect, emotional/mental health issues, financial disadvantage, inadequate housing, risk of abuse, drug and alcohol concerns, or history of institutionalization) were over-represented in profiles 4, 6, and 7, which are those consisting of people with advanced cognitive/ behavioral/psychological support needs.
As expected, the profiles were strongly associated with the approved HCP level. The higher the level of Home Care Package an individual had been approved for, the more likely they were to be classified in a more advanced needs profile (Table 3).
Discussion
This study, using latent class analysis, identified seven care and support needs profiles with practical significance and implications. Profiles of this kind, for people with complexity of care and support needs, have not been previously reported for the Australian context. The profiles highlight that people requiring home-based aged care present with a continuum of care and support needs. At one end of the continuum, people have what can be perceived as basic needs, and at the other end, very advanced needs. While such a continuum is expected, the profiles provide novel, nuanced, and detailed information about the day-to-day care and support needs of older people within each profile. Such profiles could help to inform individual-level care planning, including service types and workforce requirements for people within each profile—that is, they could help guide delivery of “the right approach for the right [person]” (Aflaki et al., 2022, p. 168). They could also be of interest for policymakers designing home-based aged care programs by providing insights into which care and support needs may group together at the population-level, which in turn could highlight service-type and workforce planning requirements at the system level. Such approaches to care may lead to people’s needs being more efficiently and effectively addressed.
Few similar studies have been conducted for people requiring home-based aged care. However, a study by Saari et al. (2024) has been located, which similarly aimed to develop groupings of “life care” needs for older people living in Ontario, Canada. Their study used a three-step segmentation process, based on a large routinely collected dataset about people predominantly >85 years of age, requiring long-term home care services. They identified six distinct care and support needs profiles for this group of people. As for the profiles identified in the study being reported here, Saari et al. (2024) found some needs to be common across groups, such as domestic tasks, and that certain needs, for example, for personal care, moderate/severe cognitive impairment, and behavioral support, were concentrated in specific profiles. Liu and Yao (2014) also conducted a similar study using LCA about recipients of a Taiwanese government home-based aged care program to identify needs profiles as a validity check of dependency levels and care planning identified by care managers. The researchers used routinely collected data about a sample very similar to that used for this study in terms of age, gender, and marital status (although more people were living alone in the population for the study being reported here). They identified four profiles with different groupings of needs, ranging from low to severe dependency, and differences in likelihood of belonging to particular profiles based on socio-demographic characteristics (e.g., people in the low and moderate dependency groups were more likely to be living alone). Both studies highlighted that the knowledge about variation in needs across profiles can guide differentiated and person-centered approaches to more effectively and efficiently meet people’s care needs.
The profiles identified here are closely aligned with the HCP levels determined by aged care assessors during the assessment process, adding credibility to the Australian government’s eligibility/rating system. However, the identified profiles provide much more nuanced information about care and support needs than HCP levels, which simply describe a person’s needs as being basic, low, intermediate, or high (DoHAC, 2024). For example, people fitting profile 7 emerged as the group with the most advanced care and support needs. They were likely to have many ADL support needs, significant cognitive/behavioral concerns, and to require support for multi-vulnerabilities and multi-complexities, compared to people fitting most other profiles. Therefore, overall, people in this profile were likely to experience a very high level of dependence and corresponding potential well-being and safety risks. This profile closely aligns with one of Saari et al.’s (2024) profiles consisting of people with advanced cognitive impairment and related behavior changes, potential for abuse, mood changes, and need for help with ADLs due to both physical and cognitive impairments. Caring for people at home with advanced cognitive, behavioral, and psychological needs has a number of implications. This group of people would likely benefit from episodic by specialized clinical assessment, for example, from a dementia nurse, to guide detailed and personalized care planning to optimally manage well-being and safety risks (Dementia Support Australia, n.d.). Ensuring access to adequate funding to implement such assessment and the resulting care plan is important, as is planning for and training the workforce to deliver care with confidence for people with advanced cognitive, behavioral, and psychological needs (Polacsek et al., 2020).
While people fitting profile 7 were most likely of all profiles to have informal carer support, it was also likely that this carer was experiencing difficulty sustaining the caring role, highlighting the potential carer stress which can arise when caring every day for people with advanced and varied care and support needs. This finding aligns with other research identifying that the duration of caregiving and dependency level of the care recipient are key predictors of carer overburdening (Gaugler et al., 2014; Wolff et al., 2016). The finding suggests that depending on the level of support a person’s informal carer can provide, people within this profile would require funding for frequent services to provide ADL and cognitive/behavioral support, as well as center-based and residential respite for people with advanced needs (My Aged, 2025a). Access to carefully considered funding amounts for people with advanced care and support needs is essential, so carers can continue to sustain home-based aged care for this group of people and delay or avoid the need for costly residential care for the care recipient. As Jorgensen et al. (2018, p. 120) modeled in a cohort study using routinely collected client data (n = 1,116), “greater volume and type of home care services are associated with significantly delayed entry to permanent residential care,” with this being a primary aim of home-based aged care (DOHAC, 2023).
In addition to higher funding levels for more frequent services, workforce requirements to provide such a level of service would also need to be considered. It would include ensuring training for direct care workers regarding how to confidently support people with advanced care needs, such as showering and dressing, and managing behavioral concerns related to cognitive decline (Lawn et al., 2017; Polacsek et al., 2020). People within this profile would also likely require active care management to proactively coordinate service provision, as well as to regularly monitor for any gradual or sudden changes in care needs, with such changes being common amongst frail older people (Myhre et al., 2024). The well-being of carers of people fitting this profile should also be monitored by care managers. Accordingly, care managers’ educational background also needs consideration.
At the other end of the continuum of care and support needs, profile 1, comprising 25% of the population, consisted of people likely to have more “basic” ADL support needs, less likely to experience cognitive/behavioral/psychological support needs, and vulnerabilities or complexities. Therefore, this profile would require services far less frequently. Workforce requirements would more simply consist of direct care workers with entry-level training able to provide the more straightforward but also very necessary domestic assistance (e.g., cleaning services), and community access support (e.g., shopping services). This profile aligns with Saari et al.’s (2024) largest of six profiles, where 31% of their sample predominantly needed assistance for domestic and community access tasks, while also exhibiting some mild cognitive impairment.
The most interesting study finding from a socio-demographic perspective was that people living alone or without a carer were less likely to be represented in the more advanced profiles. This suggests that this population sub-group is more likely to find themselves in the position of having to make the decision to move to residential care when their care needs increase beyond a certain point, which could be viewed as care inequity (Hill, 2022). More research is needed to better understand this issue. Nonetheless, the findings suggest that policymakers may need to consider how to differentially support people living alone or without a carer, so they can equitably have the option to remain living at home, along with those living with others or with carer support.
People with vulnerabilities and complexities as measured within the NSAF dataset were more likely to appear in the more advanced needs profiles. Based on this research alone, it is not possible to conclusively comment as to why this is the case. It could be that the accumulated impact over time of experiencing one or more vulnerability or of having to manage one or more complexity, itself results in overall higher care and support needs in older age (WHO, 2015). Alternatively, it could mean that people experiencing vulnerabilities and complexities have difficulty navigating the aged care system, and that by the time they have connected with aged care supports, their overall care and support needs have become advanced. Either way, this finding highlights that people assessed as experiencing vulnerabilities and complexities may benefit from being targeted for earlier intervention, although how this could be managed would need further consideration. There are already “care finders” in place within the Australian aged care system to assist “vulnerable” older people to navigate the system (My Aged, 2025b), so it could be a matter of developing improved approaches for working with these sub-groups of people based on the expertise and input of care finders.
At the time of this research, the CHSP and the HCP program were undergoing reform to create a combined “Support at Home” program. The HCP program is set to reform from 1 November 2025. Information to date indicates an updated aged care assessment process will assign people, via an aged care assessment process, to a “classification scale” which might be akin to the seven profiles we have identified. Interestingly, the Australian Government DoHAC has proposed eight ongoing classifications (DoHAC, 2025b). Details about the likely care and support needs of people within each of these classifications were not publicly available at the time of reporting this study. Of note, the CHSP will not combine with the new program until at leave 2027 (DOHAC, 2025b).
The key strength of this study is the utilization of a population-based dataset comprising nearly 100,000 Victorians who had sought eligibility assessment for and been approved for a government-funded HCP between January 2019 and June 2022. Since the whole population of Victorians approved for this care type was included, no sampling bias is likely. Limitations include that information bias during data collection could have contributed to under- or over-reporting of care and support needs, for example, people might have under-reported their care issues during data collection to avoid being assessed as requiring aged-care, or some assessors might have been more attuned to identify certain needs, dependent on their experience. Additionally, although this was a population-level study, self-selection bias cannot be ruled out, since those from vulnerable population groups may have been less likely to seek assessment and, therefore, be under-represented in the study population. Lastly, while the study findings cannot be generalized across the whole of Australia, they could be informative for states with similar socio-demographic characteristics (e.g., New South Wales, South Australia (Australian Bureau of Statistics, n.d.)), especially with the aged care assessment process being nationally consistent (MAC, 2018).
There are other limitations of this study. First, the dataset did not include people assessed as requiring entry-level CHSP services only. Had his group been included, it is likely they would be either part of profile 1 or generate a new profile with even lower-level care and support needs. Also, with aged care assessments having been more routinely completed by phone over 2020 and 2021 in some regions of Victoria due to the COVID pandemic, while assessments were still completed according to standardized assessment processes, it is possible assessors missed certain care and support need for some people, which they would otherwise have detected via direct observation, even if not reported by the older person themselves. This could have led to under-reporting of some needs within the NSAF, potentially resulting in fewer people within the higher needs profiles.
Additionally, services use data and outcome measures for home-based aged care in Victoria or Australia are not yet routinely measured at the system-level, and any measures taken at the provider level are not readily accessible for researchers. Therefore, evaluation of the impact of particular approaches to home-based aged care delivery via particular service or workforce models is not currently possible. However, there is still merit in conducting observational studies utilizing population-based routinely collected datasets about people requiring home-based aged care, to inform system improvements and provide insights for policymakers and aged care providers about the fundamental needs of people requiring home-based aged care, to contribute to continued improvement of this type of long-term aged care. When such data becomes available, research should be designed to explore associations between care and support needs, care inputs and care outcomes.
Conclusion
This study, conducted with a population-level dataset about Victorians requiring an HCP, a form of government-funded home-based aged care, has identified seven distinct care and support needs profiles. Other home-based aged care populations with similar demographics within Australia and internationally are likely to have similar predictable care and support needs groups. The profiles provide detailed and nuanced information that can inform the specific service requirements, care inputs, and workforce skill, including the appropriate skill-mix, needed to optimally address the needs of older people within each profile. Similarly, it could inform the education requirements for home-based aged care workers.
Supplemental Material
Supplemental Material - Identifying Care and Support Needs Profiles for Home-Based Aged Care: A Latent Class Analysis Using Routinely Collected Aged Care Assessment Information
Supplemental Material for Identifying Care and Support Needs Profiles for Home-Based Aged Care: A Latent Class Analysis Using Routinely Collected Aged Care Assessment Information by Rachel McKittrick, Alison M. Hutchinson, Elizabeth Manias, Martin Hensher, and Liliana Orellana in Journal of Applied Gerontology
Footnotes
Ethical Considerations
Ethics approval to conduct the study using this dataset was provided by the Deakin University Human Research Ethics Committee on 20 May 2022 (#2022-132).
Author Contributions: Credit
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The first author was supported to undertake this research by a Deakin University Postgraduate Research Scholarship; the Australian College of Nursing, Centaur Nurses Memorial Scholarship 2022; and the Australian Nursing and Midwifery Federation (Victorian Branch), Annual Higher Education and Research Grant 2023.
Declaration of Conflicting Interest
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: We declare the following: MH is a board director of Glenview Community Services, a Tasmanian not-for-profit residential and home-based aged care provider; RM is an Assessment Clinician with the Monash Health Aged Care Assessment Team/Southern Metropolitan Region in Victoria. LO/AH/EM have no conflicts of interest to declare.
Data Availability Statement
The dataset used for this study, the National Screening and Assessment Form (NSAF) dataset (2022 version), was provided by the Australian Institute of Health and Welfare (AIHW) under a confidentiality agreement and cannot be made publicly available. The data are housed in the National Aged Care Data Clearinghouse, managed by the AIHW. To request access to these data, please contact the AIHW through their “data on request” processes (![]() ).
).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
